Introduction to Health Change Methodology How to get































































- Slides: 88

Introduction to Health. Change® Methodology: How to get better satisfaction and patient outcomes without adding time to consults for Presented by Health. Change Australia Janette Gale www. healthchange. com Please switch your mobile phone to silent © 2016 Health. Change Australia Slide 1

Workshop essentials • Who is Health. Change Australia? • Housekeeping, OH&S and timings • Health. Change® Handouts • Terminology & Glossary • Interaction, questions, comments • Power. Point and learning styles • Introductions © 2016 Health. Change Australia Slide 2

What topics will we cover? 1. Best practice and person-centred care 2. What health service clients need to follow health, medical, social or other recommendations and what stops them from doing this 3. What health service providers can do to increase readiness, willingness and confidence in following these recommendations using Health. Change® Methodology © 2016 Health. Change Australia Slide 3

Topic 1: Best practice and person-centred care © 2016 Health. Change Australia Slide 4

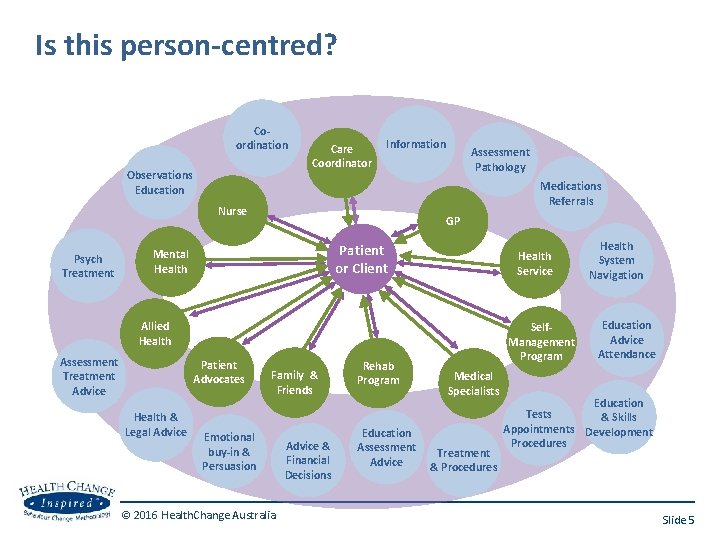
Is this person-centred? Coordination Observations Education Care Coordinator Information Medications Referrals Nurse Psych Treatment Assessment Pathology GP Patient or Client Mental Health Service Allied Health Assessment Treatment Advice Patient Advocates Health & Legal Advice Family & Friends Emotional buy-in & Persuasion © 2016 Health. Change Australia Advice & Financial Decisions Rehab Program Education Assessment Advice Self. Management Program Medical Specialists Treatment & Procedures Health System Navigation Education Advice Attendance Education Tests & Skills Appointments Development Procedures Slide 5

Why is person-centred service delivery important? ‘Don’t tell me what to do!’ ‘Yes, tell me what to do’ …because it engages clients to do what they need to do © 2016 Health. Change Australia Slide 6

Evidence-based Best Practice Evidence-based assessment, diagnosis, treatment, advice and care Evidence-based person-centred service delivery © 2016 Health. Change Australia Slide 7

Client Reflections Video - Geoff • Back injury (medical discharge from Navy) • Chronic pain • PTSD, depression & other psychosocial • Diabetes type 2 • Prostate cancer previously • High cholesterol • Weight management issues • Resistance from previous experiences © 2016 Health. Change Australia Slide 8

Health. Change® Methodology A health service delivery methodology used to provide person-centred care and promote health literacy, shared decision making, behaviour change and self-management to support adherence to evidence-based recommendations for improved health and quality of life outcomes Visit healthchange. com for short videos on Health. Change® Methodology and to download other resources © 2016 Health. Change Australia (HCM Mini Guide p. 1) Slide 9

Australian and Overseas programs and services Primary Care • • Prevention • GP & Allied Health consultations ACT Health/Medicare Local/Heart Foundation Heart. Link Program Practice Nurse Care Planning NSW Get Healthy Telephone Coaching NSW Live Life Well Diabetes Prevention VIC Work. Safe Work. Health Coach Program • • • Clinical Research • • Chronic Condition Management • • • NSW CDM Connecting Care Home & Community Care (HACC) VIC Early Intervention (EICD) VIC HARP programs Heart failure & Cardiac rehab Diabetes, HIV, Disability, Aged Care Mental health QLD Health Call Centre Cardiac Triage QLD Disease Management Services TAS Diabetes services Deakin University – HIPP/Healthy Pregnancy Study Melbourne University – Knee Osteoarthritis, Diabetic Retinopathy, Lung Cancer Wollongong University – Practice Nurse Care Planning Studies Monash University – Positive Ageing with HIV Ottawa Regional Cancer Foundation • Survivorship support coaching Alberta Health Services • Chronic Disease Management Services © 2016 Health. Change Australia Denmark - Copenhagen • Metropolitan University College Slide 10

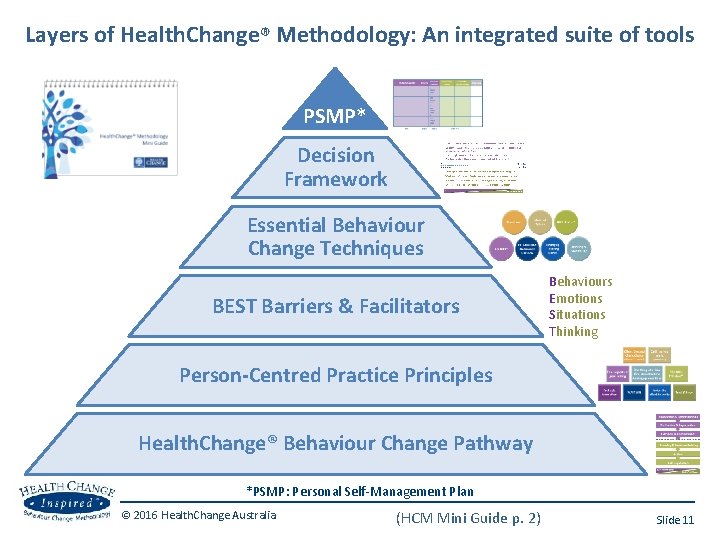
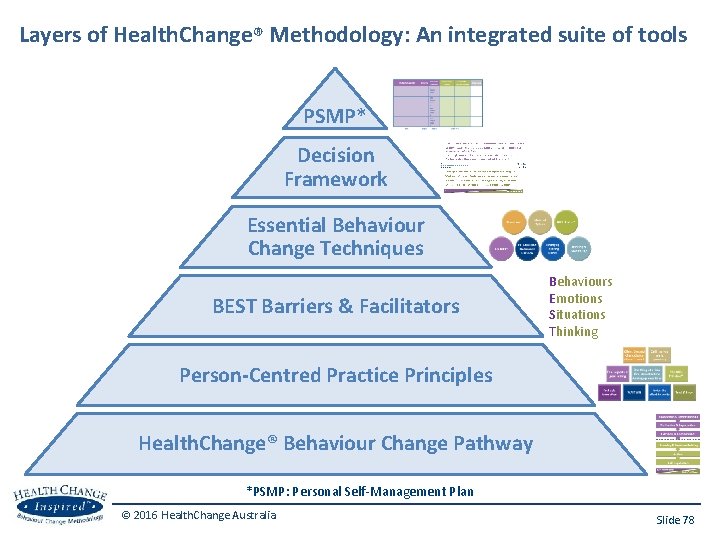
Layers of Health. Change® Methodology: An integrated suite of tools PSMP* Decision Framework Essential Behaviour Change Techniques BEST Barriers & Facilitators Behaviours Emotions Situations Thinking Person-Centred Practice Principles Health. Change® Behaviour Change Pathway *PSMP: Personal Self-Management Plan © 2016 Health. Change Australia (HCM Mini Guide p. 2) Slide 11

Health. Change® Methodology is like an ice cream cone! © 2016 Health. Change Australia Slide 12

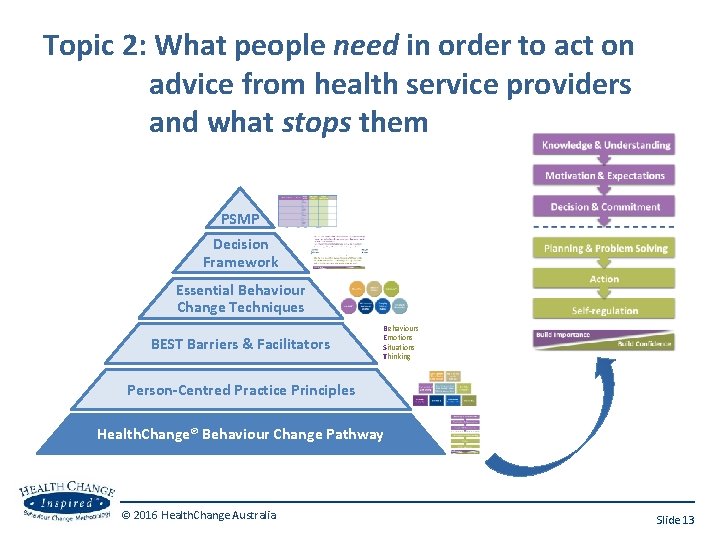
Topic 2: What people need in order to act on advice from health service providers and what stops them PSMP Decision Framework Essential Behaviour Change Techniques BEST Barriers & Facilitators Behaviours Emotions Situations Thinking Person-Centred Practice Principles Health. Change® Behaviour Change Pathway © 2016 Health. Change Australia Slide 13

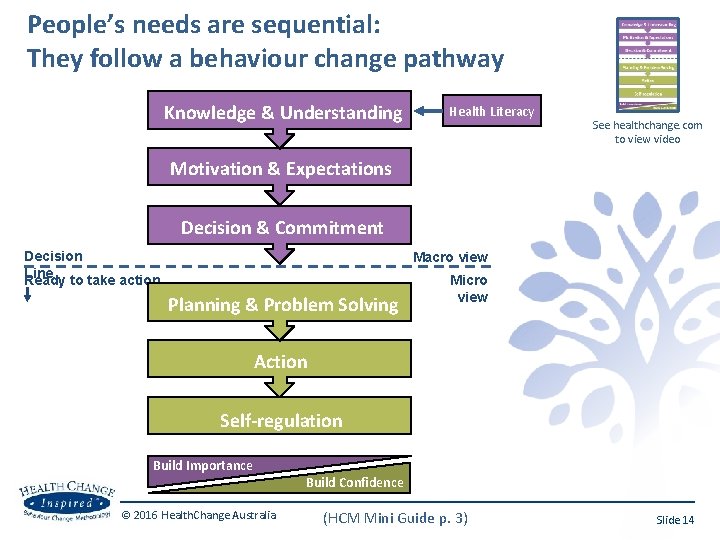
People’s needs are sequential: They follow a behaviour change pathway Knowledge & Understanding Health Literacy See healthchange. com to view video Motivation & Expectations Decision & Commitment Decision Line Ready to take action Macro view Planning & Problem Solving Micro view Action Self-regulation Build Importance Build Confidence © 2016 Health. Change Australia (HCM Mini Guide p. 3) Slide 14

Health. Change Health Literacy What (Information) Why (Motivation) Health Condition What can be done to manage this condition Elements required to make a fully informed decision © 2016 Health. Change Australia Slide 15

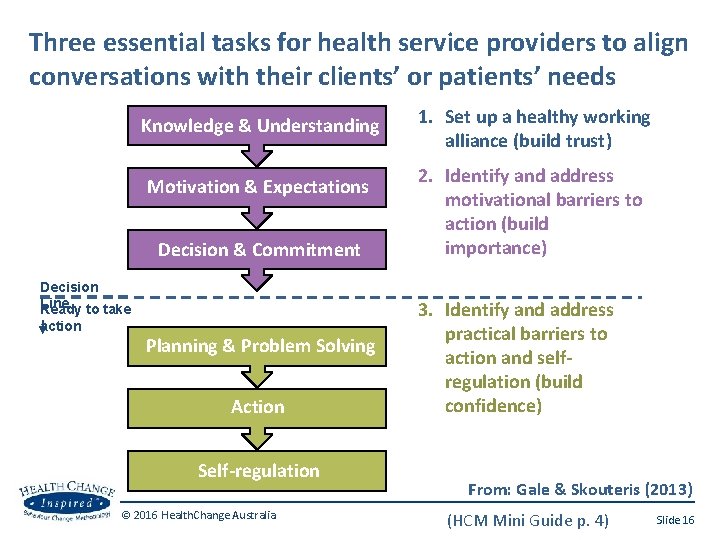
Three essential tasks for health service providers to align conversations with their clients’ or patients’ needs Knowledge & Understanding Motivation & Expectations Decision & Commitment Decision Line Ready to take action Planning & Problem Solving Action Self-regulation © 2016 Health. Change Australia 1. Set up a healthy working alliance (build trust) 2. Identify and address motivational barriers to action (build importance) 3. Identify and address practical barriers to action and selfregulation (build confidence) From: Gale & Skouteris (2013) (HCM Mini Guide p. 4) Slide 16

What service providers need to ask themselves to help clients Does the client know and understand their health issues and clinical targets? Do they know and understand the broad treatment, lifestyle and referral categories applicable to these? Have they been assisted to collaboratively prioritise these categories? Are they ready, willing, able and committed to taking action? Decision Line Ready to take action Macro view What options do they have for taking action in particular categories? Micro view What are their personalised goals/plans for achieving category goals? Are they confident they can do these things? What might stop them? Will I review the client? What other support might they need? Build Importance © 2016 Health. Change Australia Build Confidence (HCM Mini Guide p. 5) Slide 17

Client case demonstration Video - Terry • • • CAD, heart attack Hypertension Diabetes T 2 Obesity, Lap banding Gall bladder removed © 2016 Health. Change Australia Slide 18

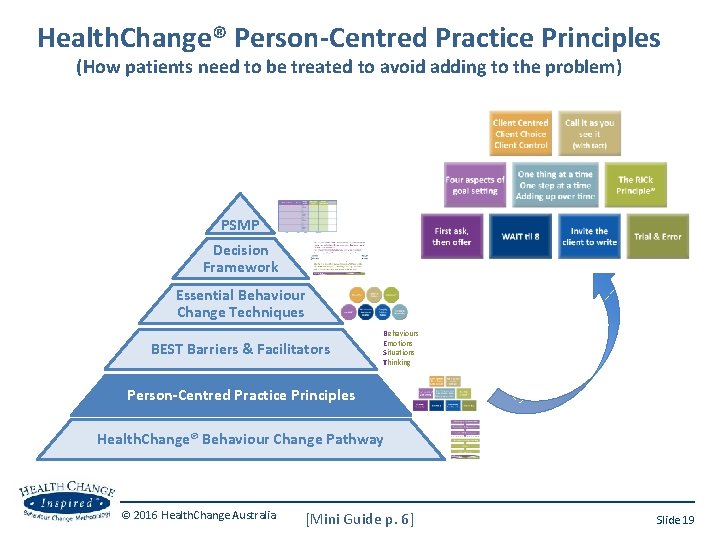
Health. Change® Person-Centred Practice Principles (How patients need to be treated to avoid adding to the problem) PSMP Decision Framework Essential Behaviour Change Techniques BEST Barriers & Facilitators Behaviours Emotions Situations Thinking Person-Centred Practice Principles Health. Change® Behaviour Change Pathway © 2016 Health. Change Australia [Mini Guide p. 6] Slide 19

Health. Change® Methodology requires health service providers to balance their duty of care with their client’s right to make fully informed, conscious decisions about what they will do. If you feel like all your consultations sound the same, you are probably not being personcentred © 2016 Health. Change Australia (HCM Mini Guide p. 7) Slide 20

How to turn clients into elks or polar bears…. . • ‘Tell’ people what to do • Argue the point • Use scare tactics with people who are low in confidence • Using judgmental language • Overwhelm people by expecting them to do too much • Overwhelm them with too much information/education Service providers need alternative strategies to be built into their consultations and service delivery © 2016 Health. Change Australia Slide 21

Use honest and open dialogue to avoid playing the ‘practitioner-patient’ game! Acknowledge the elephant in the room © 2016 Health. Change Australia (HCM Mini Guide p. 8) Slide 22

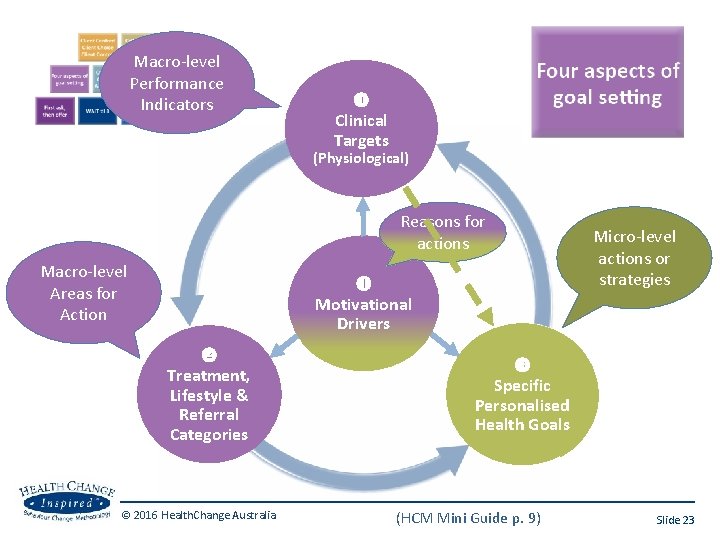
Macro-level Performance Indicators Clinical Targets (Physiological) Reasons for actions Macro-level Areas for Action Micro-level actions or strategies Motivational Drivers Treatment, Lifestyle & Referral Categories © 2016 Health. Change Australia Specific Personalised Tasks Health Goals (HCM Mini Guide p. 9) Slide 23

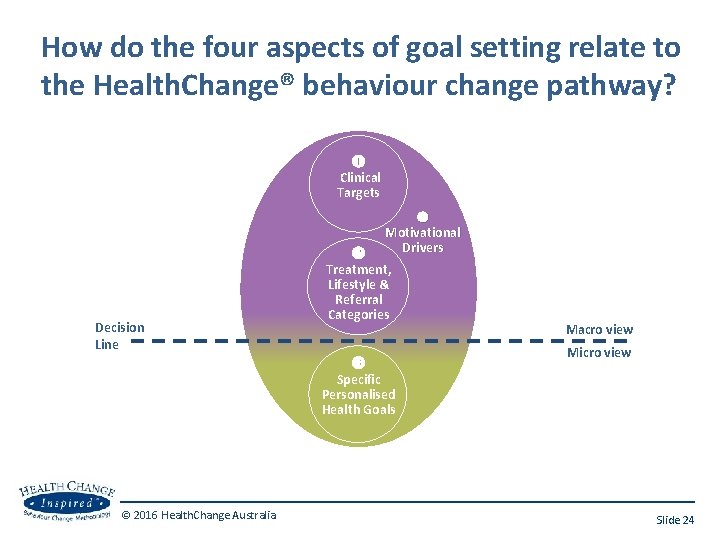
How do the four aspects of goal setting relate to the Health. Change® behaviour change pathway? Clinical Targets 2 Decision Line Motivational Drivers Lifestyle & Treatment, Treatment Lifestyle & Categories Referral Categories Macro view Micro view Specific Personalised Health Goals © 2016 Health. Change Australia Slide 24

Health. Change Health Literacy What (Information) Health Condition What can be done to manage this condition What I will do to manage this condition (How? ) © 2016 Health. Change Australia Why (Motivation) Decision Macro view Line Micro view (HCM Mini Guide p. 9 & 10) Slide 25

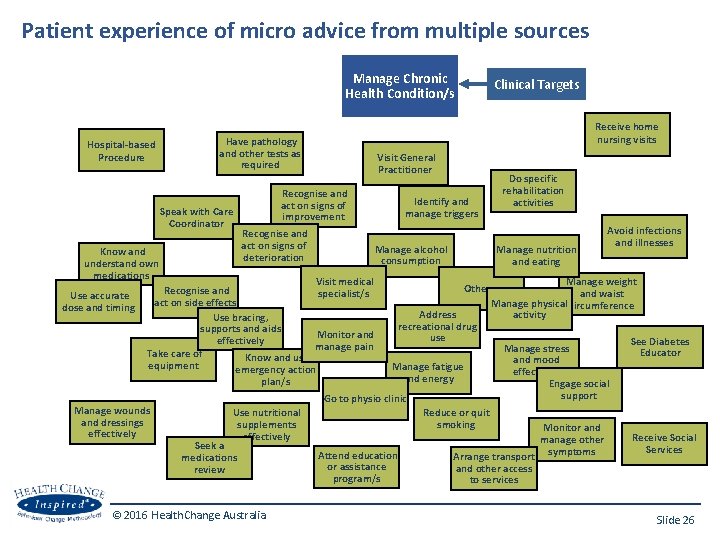
Patient experience of micro advice from multiple sources Manage Chronic Health Condition/s Hospital-based Procedure Know and understand own medications Use accurate dose and timing Receive home nursing visits Have pathology and other tests as required Speak with Care Coordinator Clinical Targets Visit General Practitioner Recognise and act on signs of improvement Recognise and act on signs of deterioration Identify and manage triggers Manage alcohol consumption Do specific rehabilitation activities Manage nutrition and eating Avoid infections and illnesses Visit medical Recognise and specialist/s act on side effects Use bracing, supports and aids Monitor and effectively manage pain Take care of Know and use equipment emergency action plan/s Manage wounds and dressings effectively Use nutritional supplements effectively Seek a medications review © 2016 Health. Change Australia Manage weight Other. . . and waist Manage physical circumference Address activity recreational drug use See Diabetes Manage stress Educator and mood Manage fatigue effectively and energy Engage social support Go to physio clinic Reduce or quit smoking Monitor and Receive Social manage other Services symptoms Attend education Arrange transport or assistance and other access program/s to services Slide 26

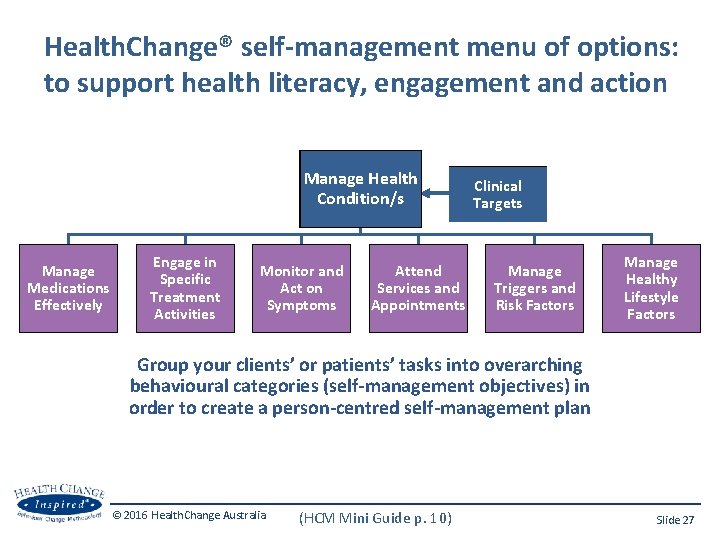
Health. Change® self-management menu of options: to support health literacy, engagement and action Manage Health Condition/s Manage Medications Effectively Engage in Specific Treatment Activities Monitor and Act on Symptoms Attend Services and Appointments Clinical Targets Manage Triggers and Risk Factors Manage Healthy Lifestyle Factors Group your clients’ or patients’ tasks into overarching behavioural categories (self-management objectives) in order to create a person-centred self-management plan © 2016 Health. Change Australia (HCM Mini Guide p. 10) Slide 27

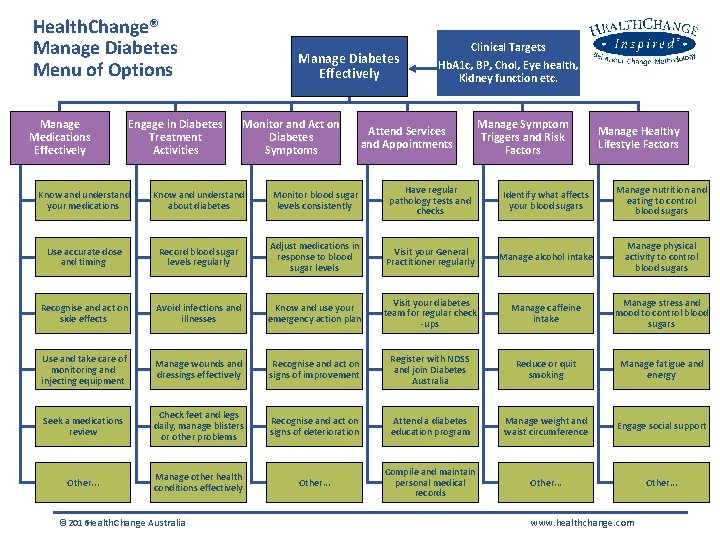
Health. Change® Manage Diabetes Menu of Options Manage Medications Effectively Engage in Diabetes Treatment Activities Manage Diabetes Effectively Monitor and Act on Diabetes Symptoms Clinical Targets Hb. A 1 c, BP, Chol, Eye health, Kidney function etc. Attend Services and Appointments Manage Symptom Triggers and Risk Factors Manage Healthy Lifestyle Factors Know and understand your medications Know and understand about diabetes Monitor blood sugar levels consistently Have regular pathology tests and checks Identify what affects your blood sugars Manage nutrition and eating to control blood sugars Use accurate dose and timing Record blood sugar levels regularly Adjust medications in response to blood sugar levels Visit your General Practitioner regularly Manage alcohol intake Manage physical activity to control blood sugars Recognise and act on side effects Avoid infections and illnesses Know and use your emergency action plan Visit your diabetes team for regular check -ups Manage caffeine intake Manage stress and mood to control blood sugars Use and take care of monitoring and injecting equipment Manage wounds and dressings effectively Recognise and act on signs of improvement Register with NDSS and join Diabetes Australia Reduce or quit smoking Manage fatigue and energy Seek a medications review Check feet and legs daily, manage blisters or other problems Recognise and act on signs of deterioration Attend a diabetes education program Manage weight and waist circumference Engage social support Other. . . Manage other health conditions effectively Other. . . Compile and maintain personal medical records Other. . . © 2016 Health. Change Australia www. healthchange. com

This is a principle, not a rule! © 2016 Health. Change Australia (HCM Mini Guide p. 11) Slide 29

Readiness Importance Confidence knowledge } Action Listen to your intuition, but when in doubt, ask the client! © 2016 Health. Change Australia (HCM Mini Guide p. 12) Slide 30

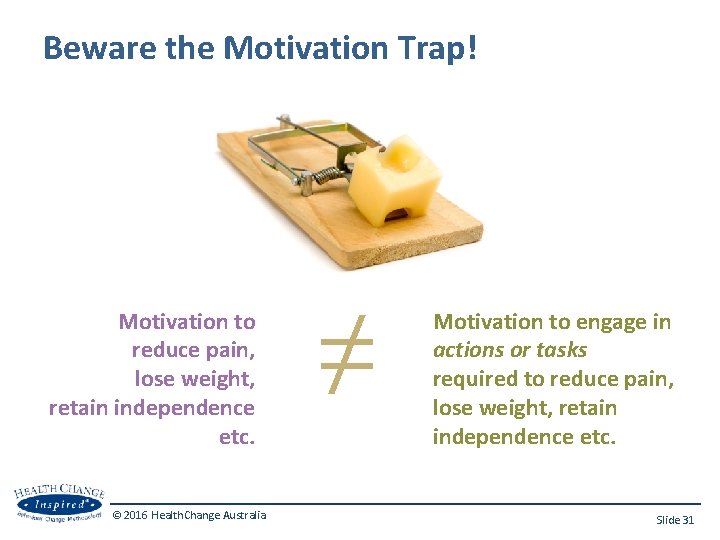
Beware the Motivation Trap! Motivation to reduce pain, lose weight, retain independence etc. © 2016 Health. Change Australia ≠ Motivation to engage in actions or tasks required to reduce pain, lose weight, retain independence etc. Slide 31

Elicit information from the client prior to offering your own information, education or suggestions to find out: Prior knowledge, knowledge gaps, misinformation 1. What do they already know? 2. What don’t they know? 3. What misinformation do they have? 4. What are they already doing? © 2016 Health. Change Australia (HCM Mini Guide p. 13) Slide 32

WAIT for a response Why Am Am I I Talking? Taking Notes? © 2016 Health. Change Australia 8 seconds is a common response time (HCM Mini Guide p. 14) Slide 33

Provide pens and paper and invite every client to write themselves some notes during your conversation if they wish to It’s a very practical way to help patients and clients! © 2016 Health. Change Australia (HCM Mini Guide p. 15) Slide 34

When you don’t succeed…. . . try a different strategy! Discuss trial and error and reduce the number of your ‘no show’ clients © 2016 Health. Change Australia (HCM Mini Guide p. 16) Slide 35

Sample phrasing for encouraging trial and error • We have discussed a number of things today that you can do to manage your health and we have agreed on what you will begin with. • If for some reason you are unable to do these things in the timeframe that we discussed, don’t worry. • Take note of the things that got in the way for you. We can discuss these at our next appointment and potentially come up with some solutions for you. • How does that sound? © 2016 Health. Change Australia (HCM Mini Guide p. 43) Slide 36

Activity: How are you using these Practice Principles currently? 1. Rate yourself your use of each of the Practice Principles using the PPET form in your workbook 2. Small group discussion - Consider a challenging client who is not progressing – Where is the client on their behaviour change pathway? – Which Practice Principles might help you? © 2016 Health. Change Australia Slide 37

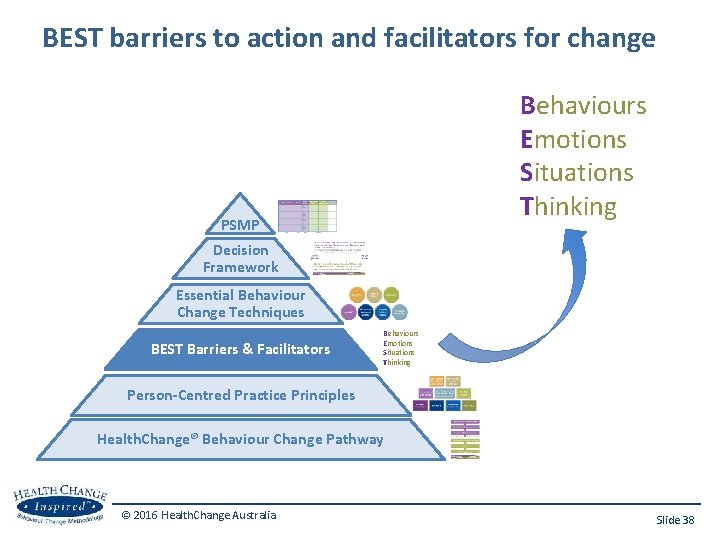
BEST barriers to action and facilitators for change Behaviours Emotions Situations Thinking PSMP Decision Framework Essential Behaviour Change Techniques BEST Barriers & Facilitators Behaviours Emotions Situations Thinking Person-Centred Practice Principles Health. Change® Behaviour Change Pathway © 2016 Health. Change Australia Slide 38

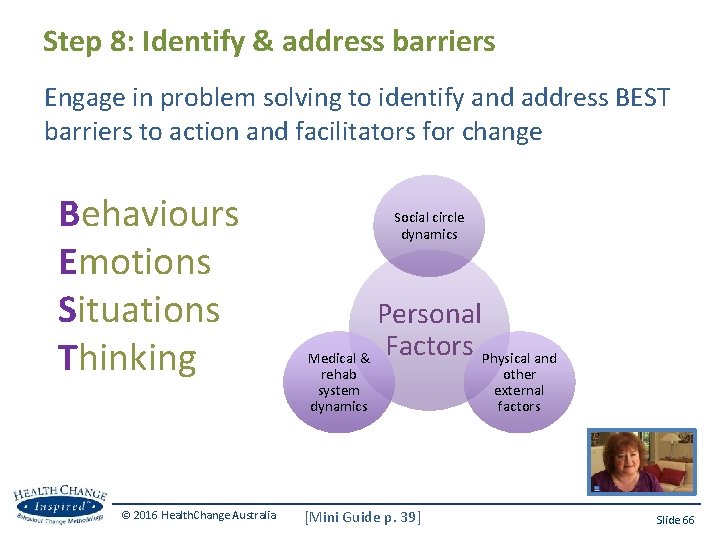
BEST barriers to action and facilitators for change Behaviours • Actions, everyday habits, planning or lack of planning Emotions • Emotional reactions to things that happen to us, mood states Situations • Medical, physical, cognitive, social, cultural, access, $, changes in circumstance, clinicians Thinking • Beliefs, attitudes, expectations & habitual thinking patterns, readiness, importance, confidence, knowledge (RICk) © 2016 Health. Change Australia (HCM Mini Guide p. 17) Slide 39

What gets in the way for you? What are the recommended activity levels for adults? Does your own activity level meet the guidelines? If No: What stops you from achieving this? If Yes: How do you manage to achieve this? What gets in the way for your clients? © 2016 Health. Change Australia Slide 40

Topic 3: What health service providers can do to Click to client edit master style and increase readiness, title willingness confidence to follow referral, treatment and lifestyle recommendations using Health. Change® Methodology © 2016 Health. Change Australia Slide 41

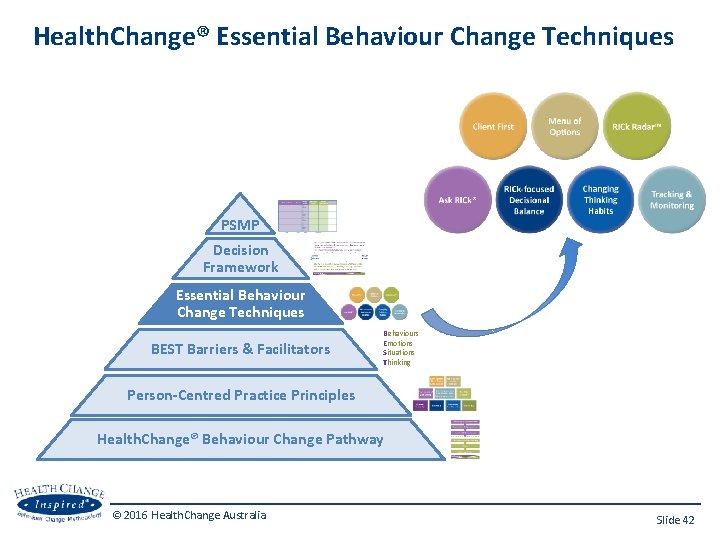
Health. Change® Essential Behaviour Change Techniques PSMP Decision Framework Essential Behaviour Change Techniques BEST Barriers & Facilitators Behaviours Emotions Situations Thinking Person-Centred Practice Principles Health. Change® Behaviour Change Pathway © 2016 Health. Change Australia Slide 42

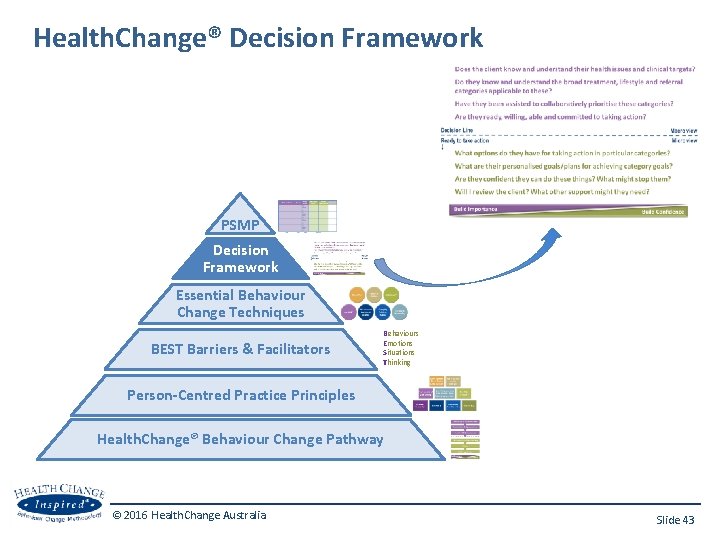
Health. Change® Decision Framework PSMP Decision Framework Essential Behaviour Change Techniques BEST Barriers & Facilitators Behaviours Emotions Situations Thinking Person-Centred Practice Principles Health. Change® Behaviour Change Pathway © 2016 Health. Change Australia Slide 43

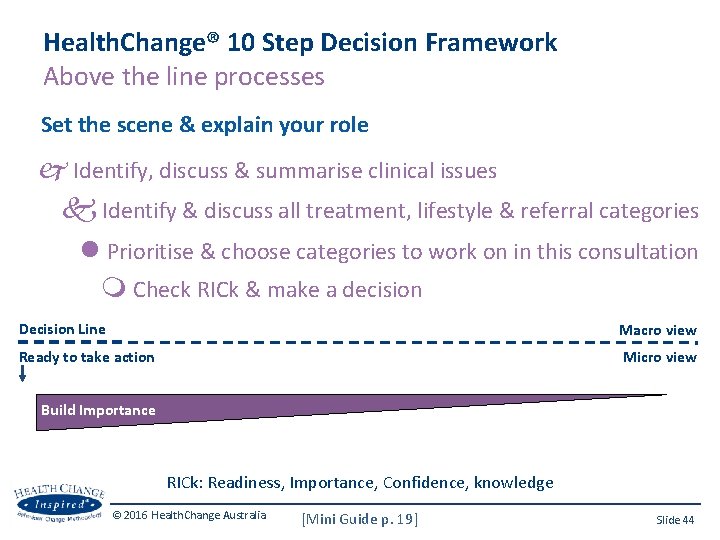
Health. Change® 10 Step Decision Framework Above the line processes Set the scene & explain your role Identify, discuss & summarise clinical issues Identify & discuss all treatment, lifestyle & referral categories Prioritise & choose categories to work on in this consultation Check RICk & make a decision Decision Line Macro view Ready to take action Micro view Build Importance RICk: Readiness, Importance, Confidence, knowledge © 2016 Health. Change Australia [Mini Guide p. 19] Slide 44

Set the scene and explain your role Create a comfortable environment and Set up positive and accurate expectations © 2016 Health. Change Australia Slide 45

Activity: Explain your role Elements: 1. Who you are and how you work • Collaborative approach 2. What you won’t do (address negative expectations) 3. What’s in it for them (state the benefits and create positive expectations about your service and their role in their care) 4. State how long the consult will take (and ask permission to proceed if relevant) © 2016 Health. Change Australia (HCM Mini Guide p. 20) Slide 46

Step 1: Identify, discuss & summarise clinical issues • Gather clinical data and/or conduct clinical or other objective assessment • What are the relevant clinical issues? • Summarise these issues for the patient or client • Check their knowledge and understanding • Why are these clinical issues a potential problem for them? First ask, then offer! © 2016 Health. Change Australia [Mini Guide p. 21] Slide 47

Sample phrasing for checking a person’s knowledge and understanding of their clinical issues • What is your understanding of (your condition/s)? • Are you comfortable that you know enough about how (your condition/s) impacts on a person’s body and quality of life? • Would you like to spend a little time talking about this? © 2016 Health. Change Australia (HCM Mini Guide p. 22 and 23) Slide 48

What is the critical information for people to know so that they understand enough about their clinical condition/s to be motivated to take action? 1. Usual course of the condition over time and how it can impact on people 2. What will make the symptoms or prognosis better or worse 3. Common misconceptions about either of the above © 2016 Health. Change Australia Slide 49

Step 2: Identify & discuss all relevant treatment, lifestyle & referral categories • What does anyone with these particular clinical or other issues need to do over time to get the best results? • Summarise the general recommendations for the client • Check their broad knowledge and understanding of each general recommendation • Establish why taking action on these recommendations might be beneficial for this client or patient • Acknowledge current actions (what they are already doing) First ask, then offer! © 2016 Health. Change Australia [Mini Guide p. 24] Slide 50

Activity Step 2: How do you first ask, then offer advice about referral, treatment and lifestyle categories? • Can you tell me what you already know about managing (your condition/s) so that it has the minimum effect on your health and quality of life? • What are you already doing to manage (your condition/s)? • There are some other things that people with (your condition/s) really need to do over time to get the best outcomes and avoid complications. Do you mind if we discuss these as well? © 2016 Health. Change Australia [Mini Guide p. 25] Slide 51

Step 3: Prioritise and choose categories to work on in this consultation • • • Prevent the client from becoming overwhelmed Prioritise broad lifestyle and treatment categories Balance duty of care with client fully-informed choice Clarify what the client is already doing to manage their health Set the agenda for the current consultation Messy Head Syndrome © 2016 Health. Change Australia [Mini Guide p. 27] Relief Slide 52

Client case demonstration Video – Darren low back pain Promoting health literacy and prioritising long and short-term areas for patient action © 2016 Health. Change Australia Slide 53

Do the first few steps right and the rest will follow! © 2016 Health. Change Australia Slide 54

Step 4: Check RICk & make a decision Readiness, Importance, Confidence, knowledge Client decision: a) ‘yes’ b) ‘no’ c) ‘maybe’ Service provider decision: a) Client ‘yes’ Proceed below the decision line b) Client ‘no’ Revisit Step 3 or invite the client to opt out c) Client ‘maybe’ Use RICk-focused decisional balance, and/or Determine if the client needs more information to make a decision © 2016 Health. Change Australia [Mini Guide p. 28] Slide 55

Use your intuition to observe body language, tone of voice and other verbal and non-verbal cues to detect low RICk or ambivalence Don’t fall into the Motivation Trap! © 2016 Health. Change Australia When in doubt ask the client! But, be careful how you ask your questions (HCM Mini Guide p. 29) Slide 56

Activity: How many different ways can you think of to ask about importance and confidence without actually using these words? Words related to Importance: • Value, priority, desire, motivated, committed, reasons, outcomes, benefits you hope to achieve, personally important, want to do, feel you need to do, happy to do. . . Words related to Confidence: • Ability, able, capable, manageable, comfort zone, likelihood of being able to, think you can do, will do successfully. . . © 2016 Health. Change Australia (HCM Mini Guide p. 30) Slide 57

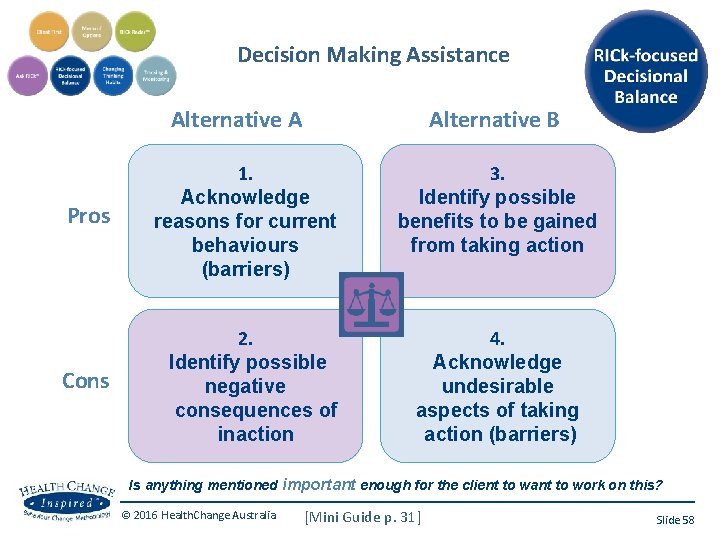
Decision Making Assistance Alternative A Alternative B Pros 1. Acknowledge reasons for current behaviours (barriers) Cons 2. Identify possible negative consequences of inaction 3. Identify possible benefits to be gained from taking action 4. Acknowledge undesirable aspects of taking action (barriers) Is anything mentioned important enough for the client to want to work on this? © 2016 Health. Change Australia [Mini Guide p. 31] Slide 58

RICk-focused decisional balance sample questions • What are the benefits of what you are currently doing? • What’s the downside of what you are currently doing? What are the possible long-term consequences for you and the things/people that are important to you? * • Why might you consider doing things differently? What benefits could you expect from this? * • What is unappealing about doing things differently? What might stop you from taking action? • From what you have said, the reasons why you have not taken action before are [mention barriers], but if you did take action then you may be able to avoid [negative consequences] and gain [benefits]. * • Is anything that you have mentioned important enough to make you want to work on this issue? * Questions and reflections that may increase Importance © 2016 Health. Change Australia [Mini Guide p. 32] Slide 59

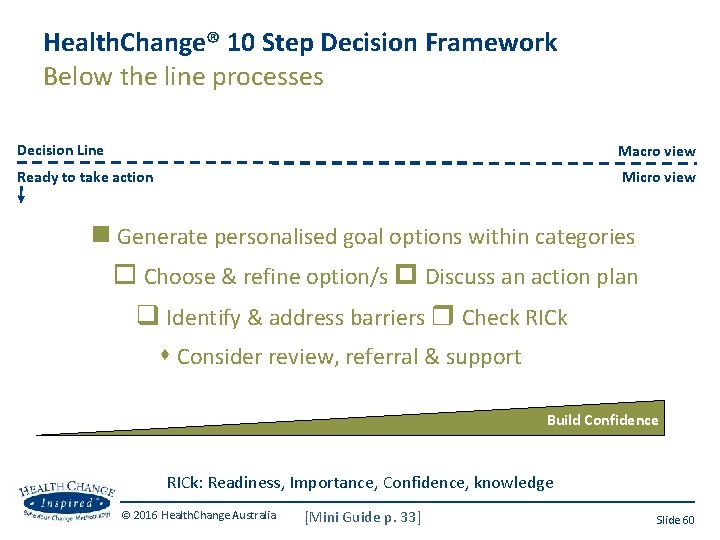
Health. Change® 10 Step Decision Framework Below the line processes Decision Line Macro view Ready to take action Micro view Generate personalised goal options within categories Choose & refine option/s Discuss an action plan Identify & address barriers Check RICk Consider review, referral & support Build Confidence RICk: Readiness, Importance, Confidence, knowledge © 2016 Health. Change Australia [Mini Guide p. 33] Slide 60

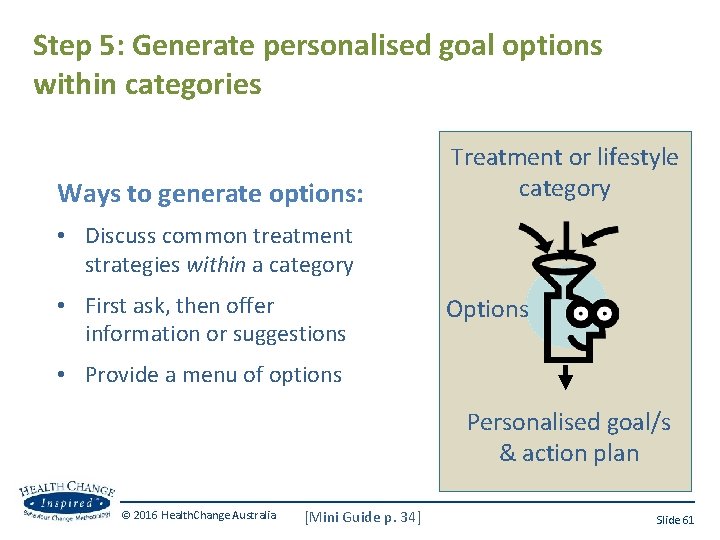
Step 5: Generate personalised goal options within categories Ways to generate options: Treatment or lifestyle category • Discuss common treatment strategies within a category • First ask, then offer information or suggestions Options • Provide a menu of options Personalised goal/s & action plan © 2016 Health. Change Australia [Mini Guide p. 34] Slide 61

Sample phrasing for offering a menu of options It often helps to have a number of different ideas of how you can tackle an issue, so that if one strategy doesn’t work, you can try one of the others. I can offer some suggestions if you like, based on what has worked for other people. However, ultimately you will be the best judge of what will work for you and what won’t. Would you like to hear my ideas or are you confident that you already have your own solutions? © 2016 Health. Change Australia (HCM Mini Guide p. 35) Slide 62

Step 6: Choose & refine personalised goal option/s Help the client to choose and personalise specific short term goals for achieving longer-term broad category goals. State personalised goals in one or two sentences: • What action will they take? • How much? • How often? • When will they start? • When will they complete or review? © 2016 Health. Change Australia [Mini Guide p. 36] Slide 63

Step 7: Discuss an action plan Discuss as much detail as necessary for the client to feel confident. Invite the client to write down their plan if necessary: • Actions or tasks • Memory prompts • Support mechanisms • Thinking strategies to support actions • Emotion management strategies • Backup plans • Tracking and monitoring strategies • Time frames for completing sub-tasks © 2016 Health. Change Australia [Mini Guide p. 37] Slide 64

Track actions and monitor outcomes • • • Pen and paper methods Visual, graphical or mapping methods Electronic diaries and smart phones Accumulating objects Subjective scales • Record physical measurements Reward systems • Record symptoms • Use pedometers, accelerometers or GPS • Use the Health. Change® Habit Change Diary • Others? © 2016 Health. Change Australia (HCM Mini Guide p. 38) Slide 65

Step 8: Identify & address barriers Engage in problem solving to identify and address BEST barriers to action and facilitators for change Behaviours Emotions Situations Thinking © 2016 Health. Change Australia Social circle dynamics Personal Medical & Factors Physical and rehab system dynamics [Mini Guide p. 39] other external factors Slide 66

Common everyday thinking barriers… © 2016 Health. Change Australia Slide 67

Sample phrasing for discussing thinking strategies 1. Do you ever procrastinate or talk yourself out of doing things you had planned to do? 2. What excuses do you usually give yourself for not taking action? 3. What do you need to say to motivate yourself instead, to make sure you do what you are planning to do? 4. How will you practise these thoughts so that you can say them to yourself when you need them? © 2016 Health. Change Australia (HCM Mini Guide p. 40) Slide 68

Client case demonstration Video – Terry Identifying and addressing thinking barriers © 2016 Health. Change Australia Slide 69

Step 9: Check RICk again To check whether the client’s personalised goals are workable and that the client is likely to succeed RICk tips: Don’t fall into the Motivation Trap! Motivation to get outcomes ≠ motivation to act If importance is low: Check knowledge, build motivation, raise priority If confidence is low: Identify and address BEST barriers Adjust personalised goals and/or add necessary strategies to action plans © 2016 Health. Change Australia [Mini Guide p. 41] Slide 70

Step 10: Consider review, referral and support • Review consultation scheduling: the lower the client’s overall confidence, the sooner the next consult should be • Discuss other supports for the client • Check RICk for attending referral appointments • Track client actions and clinical or other objective measures to review progress over time • Encourage a trial and error approach © 2016 Health. Change Australia [Mini Guide p. 42] Slide 71

Sample phrasing for encouraging Trial and Error • We have discussed a number of things today that you can do to manage your health and we have agreed on what you will begin with. • If for some reason you are unable to do these things in the timeframe that we discussed, don’t worry. • Take note of the things that got in the way for you. We can discuss these at our next appointment and potentially come up with some solutions for you. • How does that sound? © 2016 Health. Change Australia [Mini Guide p. 43] Slide 72

What service providers need to ask themselves to help clients Does the client know and understand their health issues and clinical targets? Do they know and understand the broad treatment, lifestyle and referral categories applicable to these? Have they been assisted to collaboratively prioritise these categories? Are they ready, willing, able and committed to taking action? Decision Line Ready to take action Macro view What options do they have for taking action in particular categories? Micro view What are their personalised goals/plans for achieving category goals? Are they confident they can do these things? What might stop them? Will I review the client? What other support might they need? Build Importance © 2016 Health. Change Australia Build Confidence (HCM Mini Guide p. 5) Slide 73

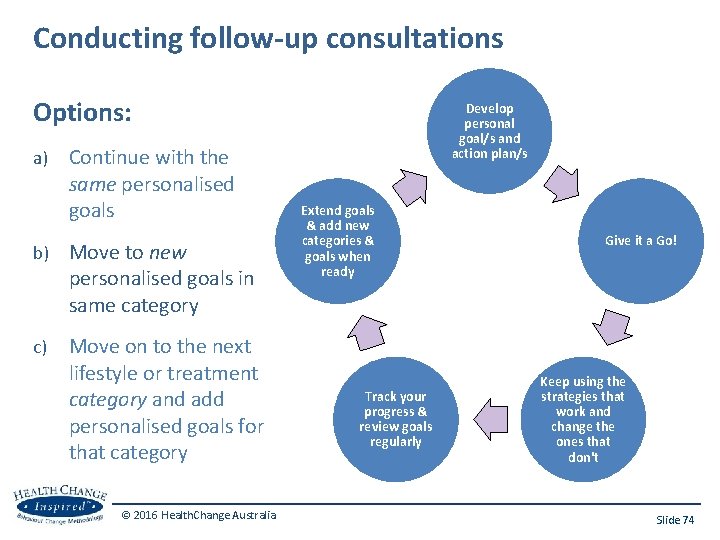
Conducting follow-up consultations Options: a) Continue with the same personalised goals b) Move to new personalised goals in same category c) Move on to the next lifestyle or treatment category and add personalised goals for that category © 2016 Health. Change Australia Develop personal goal/s and action plan/s Extend goals & add new categories & goals when ready Track your progress & review goals regularly Give it a Go! Keep using the strategies that work and change the ones that don't Slide 74

Health. Change® Personal Self-Management Plan PSMP Decision Framework Essential Behaviour Change Techniques BEST Barriers & Facilitators Behaviours Emotions Situations Thinking Person-Centred Practice Principles Health. Change® Behaviour Change Pathway © 2016 Health. Change Australia Slide 75

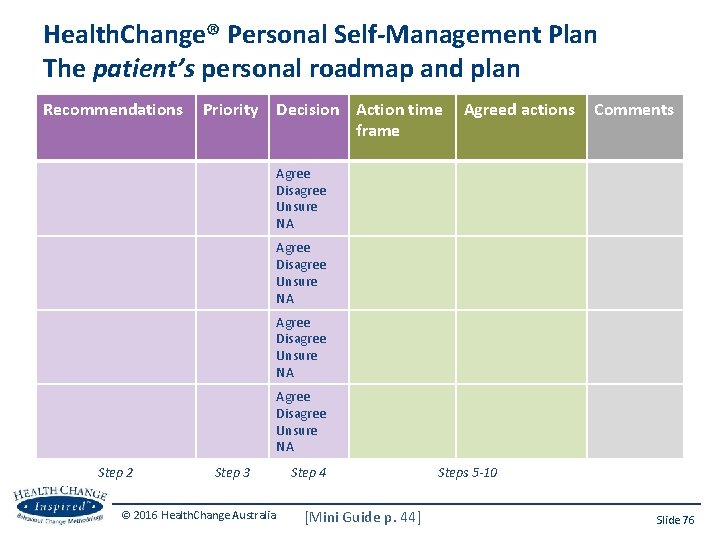
Health. Change® Personal Self-Management Plan The patient’s personal roadmap and plan Recommendations Priority Decision Action time frame Agreed actions Comments Agree Disagree Unsure NA Step 2 Step 3 © 2016 Health. Change Australia Step 4 [Mini Guide p. 44] Steps 5 -10 Slide 76

Client case demonstration Video – Darren low back pain Identifying and addressing potential barriers and documenting patient self-management information and intended actions © 2016 Health. Change Australia Slide 77

Layers of Health. Change® Methodology: An integrated suite of tools PSMP* Decision Framework Essential Behaviour Change Techniques BEST Barriers & Facilitators Behaviours Emotions Situations Thinking Person-Centred Practice Principles Health. Change® Behaviour Change Pathway *PSMP: Personal Self-Management Plan © 2016 Health. Change Australia Slide 78

How Health. Change® Methodology saves time 1. Clean, targeted assessment 2. Targeted and individualised education 3. Targeted questions 4. Quickly identifying and addressing barriers to adherence to referral, treatment and lifestyle recommendations Avoids discussing things that other clinicians have already covered Quickly builds rapport and trust Avoids discussing things the patient does not want to do Avoids irrelevant and nonproductive conversations Avoids discussing things the patient is already doing Keeps the conversation focused & on track © 2016 Health. Change Australia Slide 79

HCM Implementation Levels or Stages Language Person-centred Practice Principles Complementary Behaviour Change Skills © 2016 Health. Change Australia Health Literacy Decision Framework Evaluation Slide 80

Activity: From what we have covered today, what are you going to do to refine your service delivery to be more person-centred? Write down 3 things that you are going to do as a result of attending this workshop © 2016 Health. Change Australia Slide 81

Thank you for your participation! Find videos, case studies and practice tools at www. healthchange. com Health. Change® tools can be used freely in clinical practice and programs as long as Health. Change® Australia intellectual property is visibly acknowledged by displaying the Health. Change® Inspired logo Contact us for more information Use of any of the content contained in this workbook for training purposes outside of Health. Change® workshops and without written permission from Health. Change® Australia is a breach of Copyright and Intellectual Property Laws and legal action may be taken against persons or organisations that engage in this activity © 2016 Health. Change Australia Slide 82

© 2016 Health. Change Australia Slide 83

Workshop essentials • Who is Health. Change Australia? • Housekeeping, OH&S and timings • Health. Change® Handouts • Terminology & Glossary • Interaction, questions, comments • Power. Point and learning styles • Introductions © 2016 Health. Change Australia Slide 84

Getting to know you 1. Your name 2. Your role 3. The common conditions you/your team helps patients to manage 4. The biggest challenges that you face in working with your patients, clients or service users • Managers or administrators may like to the service users associated with their organisation and/or their other stakeholders (staff, management, colleagues etc. ) © 2016 Health. Change Australia Return Slide 85

© 2016 Health. Change Australia Slide 86

Health. Change® Menu of Options © 2016 Health. Change Australia www. healthchange. com
