INTRODUCTION TO CLINICAL MYCOLOGY Mgr Kateina Svobodov Ph

INTRODUCTION TO CLINICAL MYCOLOGY Mgr. Kateřina Svobodová, Ph. D. LABORATORY OF MYCOLOGY, INSTITUTE OF MEDICAL BIOCHEM & LAB DIAGNOST, CLINICAL MICROBIOLOGY & ATB CTR, GENERAL UNIVERSITY HOSPITAL IN PRAGUE
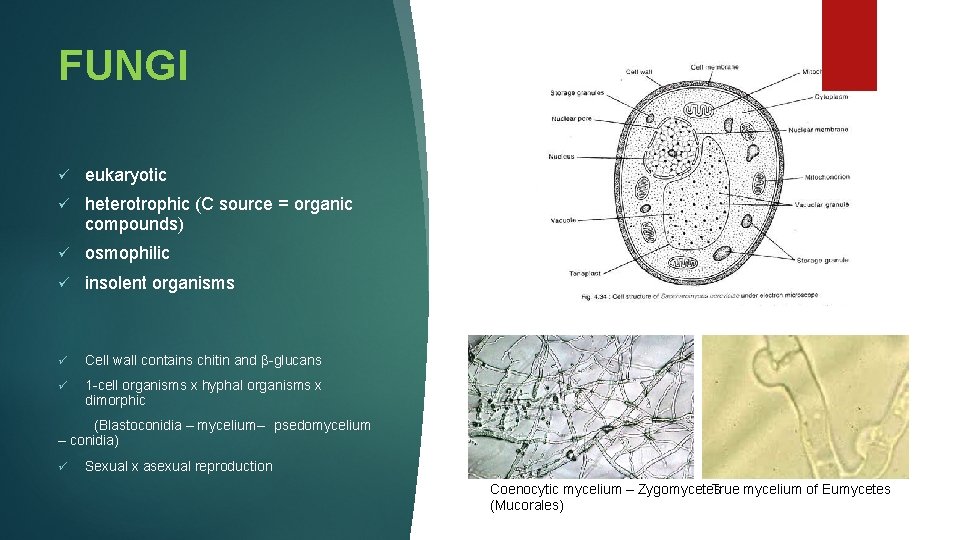
FUNGI ü eukaryotic ü heterotrophic (C source = organic compounds) ü osmophilic ü insolent organisms ü Cell wall contains chitin and β-glucans ü 1 -cell organisms x hyphal organisms x dimorphic (Blastoconidia – mycelium– psedomycelium – conidia) ü Sexual x asexual reproduction Coenocytic mycelium – Zygomycetes True mycelium of Eumycetes (Mucorales)

Taxonomic classification Eukarya – kingdom OPISTHOKONTA subkingdom EUMYCOTA division ZYGOMYCOTA Estimated number of species Known species division ASCOMYCOTA 1 500 000 120 000 = 10% division BASIDIOMYCOTA
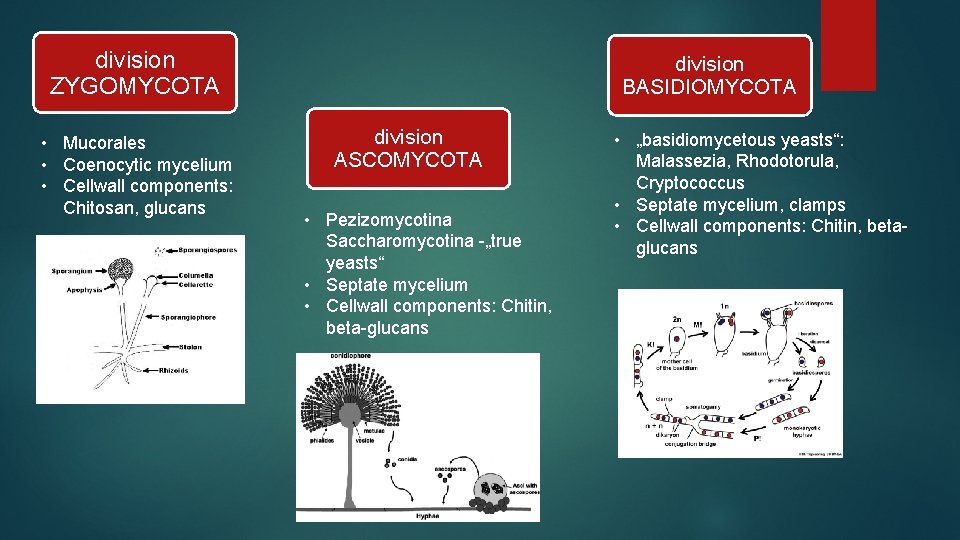
division ZYGOMYCOTA • Mucorales • Coenocytic mycelium • Cellwall components: Chitosan, glucans division BASIDIOMYCOTA division ASCOMYCOTA • Pezizomycotina Saccharomycotina -„true yeasts“ • Septate mycelium • Cellwall components: Chitin, beta-glucans • „basidiomycetous yeasts“: Malassezia, Rhodotorula, Cryptococcus • Septate mycelium, clamps • Cellwall components: Chitin, betaglucans

FUNGI – strategy of life ü Saprophytic fungi living on dead organic matter Most fungal infections are caused by saprophytic species ü Parazitic fungi of living plants and animals ü Symbiotic fungi living in symbiosis with fototrophic organisms (eg. lichens, mykorhiza) Claviceps purpurea

Health problems caused by fungi ü Fungal infections ü Intoxication by toxins eaten with mushrooms by toxins released by fungi into the environment (eg. aflatoxins) ü Allergic reactions to fungal metabolites/fungal elements ü Mycetisms = fungal elements mechanically irritates human tissues, fungi do not grow in the human body

Take home message Fungi = oportunistic pathogens Mycotic infections are common in immunodeficient people!

Risk factors age – low gestation age – age extremes ATB therapy Diabetes mellitus pregnancy Oncology- haematooncological diseases, tumors, neutropenia Radiotherapy, chemotherapy Immunodeficiency (HIV/AIDS) Corticotherapy
Extensive surgery Hospitalization Catethers, Diet at intensive care units dialysis, artificial ventilation (Fe, B 12, folic acid, malnutrition. ) Smoking Foreign (growth factors of C. albicans) materials in the body (piercing in tongue, cardiostimulator, catheters, joint implants, artificial heart valve)

Factors of pathogenicity Angioinvasivity – typical for hyphal fungi, like Aspergillus spp. and zygomycetes Dimorphic growth Adhesivity Production of acidic proteinases, keratinolytic enzymes
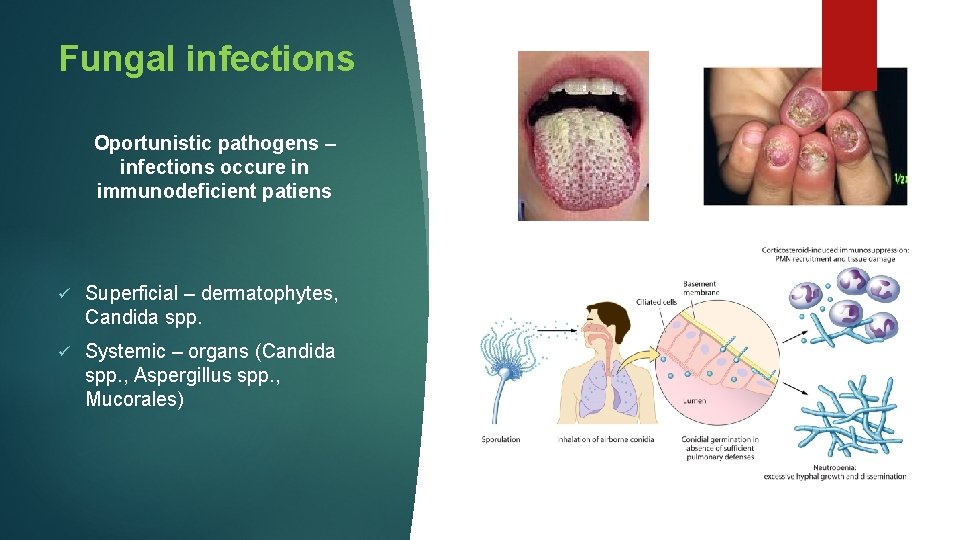
Fungal infections Oportunistic pathogens – infections occure in immunodeficient patiens ü Superficial – dermatophytes, Candida spp. ü Systemic – organs (Candida spp. , Aspergillus spp. , Mucorales)
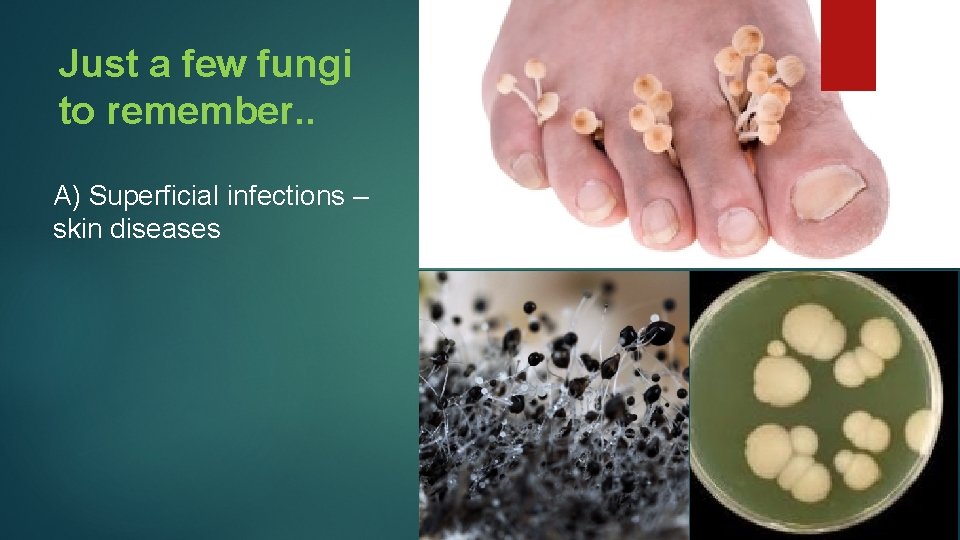
Just a few fungi to remember. . A) Superficial infections – skin diseases
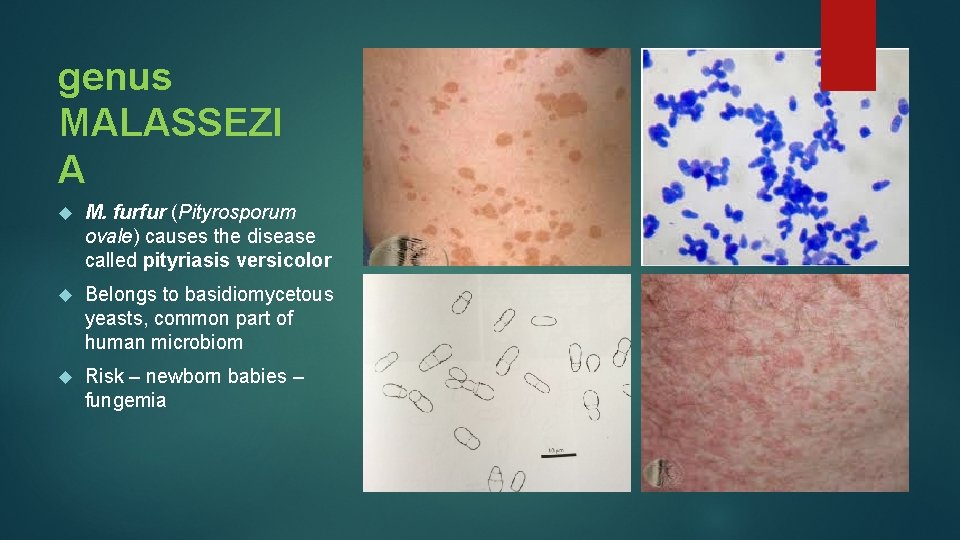
genus MALASSEZI A M. furfur (Pityrosporum ovale) causes the disease called pityriasis versicolor Belongs to basidiomycetous yeasts, common part of human microbiom Risk – newborn babies – fungemia
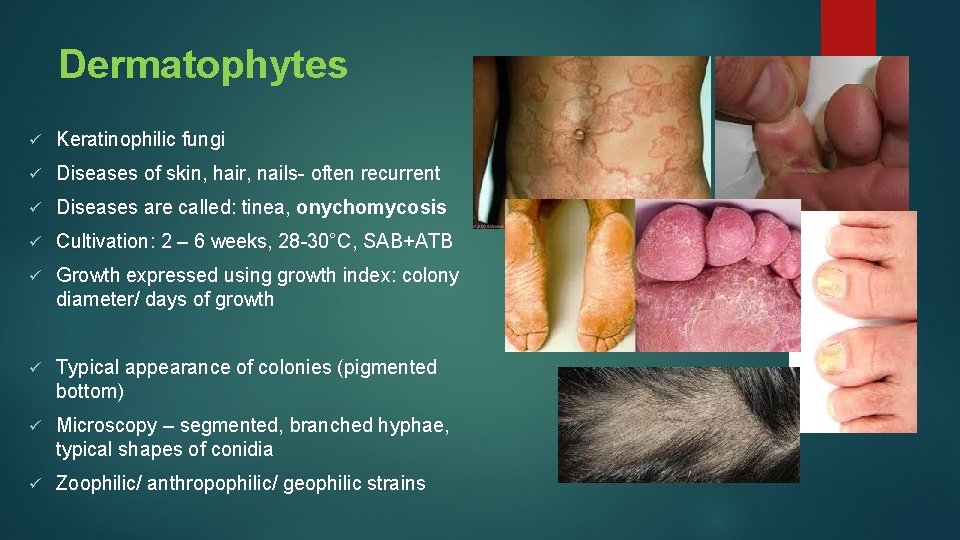
Dermatophytes ü Keratinophilic fungi ü Diseases of skin, hair, nails- often recurrent ü Diseases are called: tinea, onychomycosis ü Cultivation: 2 – 6 weeks, 28 -30°C, SAB+ATB ü Growth expressed using growth index: colony diameter/ days of growth ü Typical appearance of colonies (pigmented bottom) ü Microscopy – segmented, branched hyphae, typical shapes of conidia ü Zoophilic/ anthropophilic/ geophilic strains

genus EPIDERMOFYTO N E. floccosum ü nails, skin, NOT hair ü khaki color of colonies ü club-shaped macroconidia – 3 -5 in a bunch ü chlamydospores, no microconidia

genus TRICHOPHYTON ü colonies of various color ü producing microconidia T. rubrum - growing 2 -3 weeks T. equinum – growing fast – 1 week T. verrucosum, T. megnii, T. schenleinii, T. violaceum - growing 3 -4 weeks
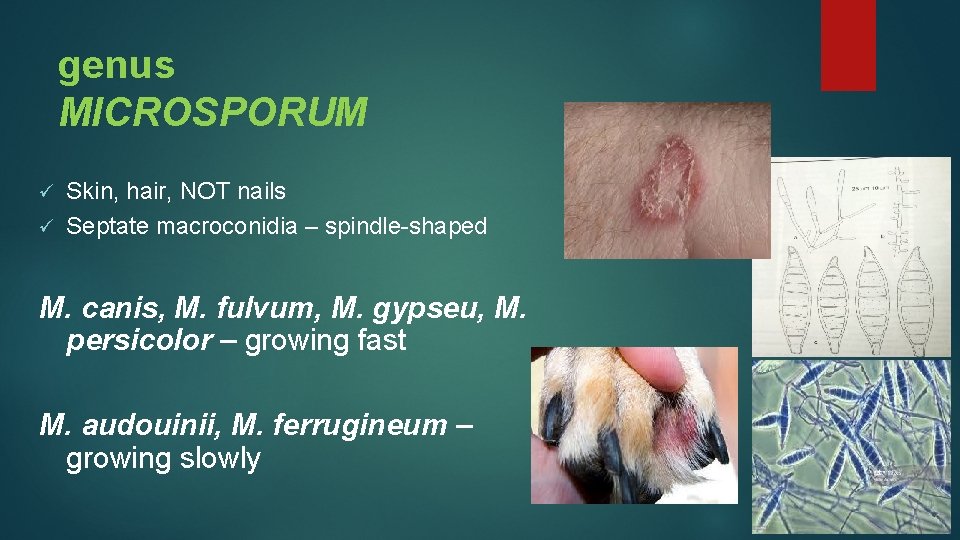
genus MICROSPORUM Skin, hair, NOT nails ü Septate macroconidia – spindle-shaped ü M. canis, M. fulvum, M. gypseu, M. persicolor – growing fast M. audouinii, M. ferrugineum – growing slowly
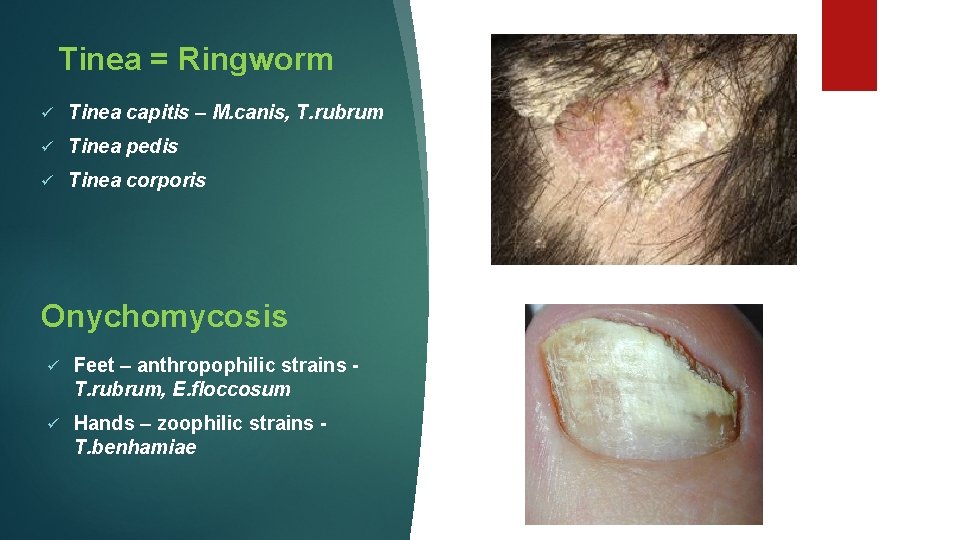
Tinea = Ringworm ü Tinea capitis – M. canis, T. rubrum ü Tinea pedis ü Tinea corporis Onychomycosis ü Feet – anthropophilic strains T. rubrum, E. floccosum ü Hands – zoophilic strains T. benhamiae

„Dark mycosis“ Common in tropical and subtropical areas Infection through contaminated soil and skin wounds long-term fungal infection of the skin and subcutaneous tissue (1) Ø Exophiala spp. , Fonsecaea sp. = „black yeast“ (1) (dimorphic, extremophilic, producing melanin) Ø Sporotrichosis (2) – Sporothrix schenckii (2) (dimorphic, living on plants, animals, afinity to lymphatic system) Ø Chromoblastomycosis (3) - Fonsecaea pedrosoi, Phialophora verrucosa, Cladosporium carrionii (3)
Just a few fungi to remember. . B) Systemic infections
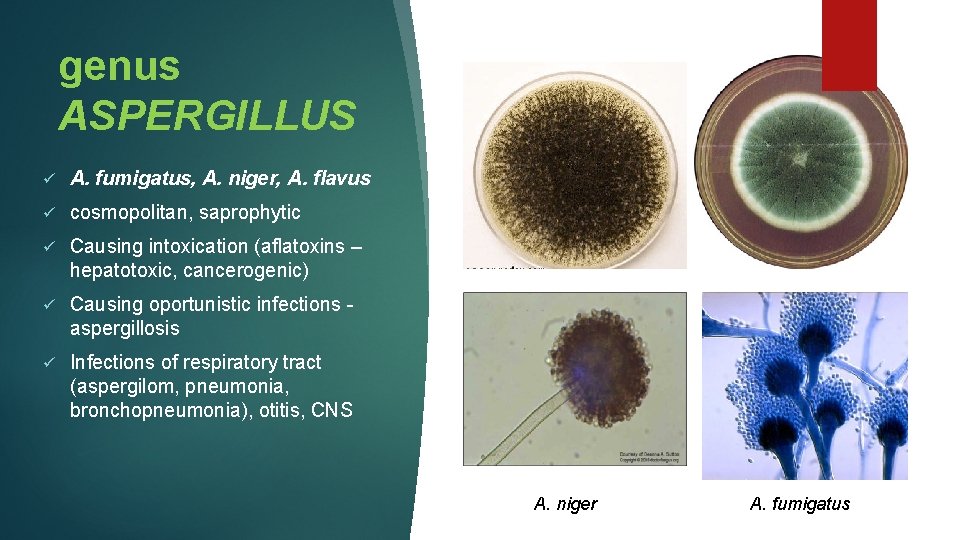
genus ASPERGILLUS ü A. fumigatus, A. niger, A. flavus ü cosmopolitan, saprophytic ü Causing intoxication (aflatoxins – hepatotoxic, cancerogenic) ü Causing oportunistic infections aspergillosis ü Infections of respiratory tract (aspergilom, pneumonia, bronchopneumonia), otitis, CNS A. niger A. fumigatus
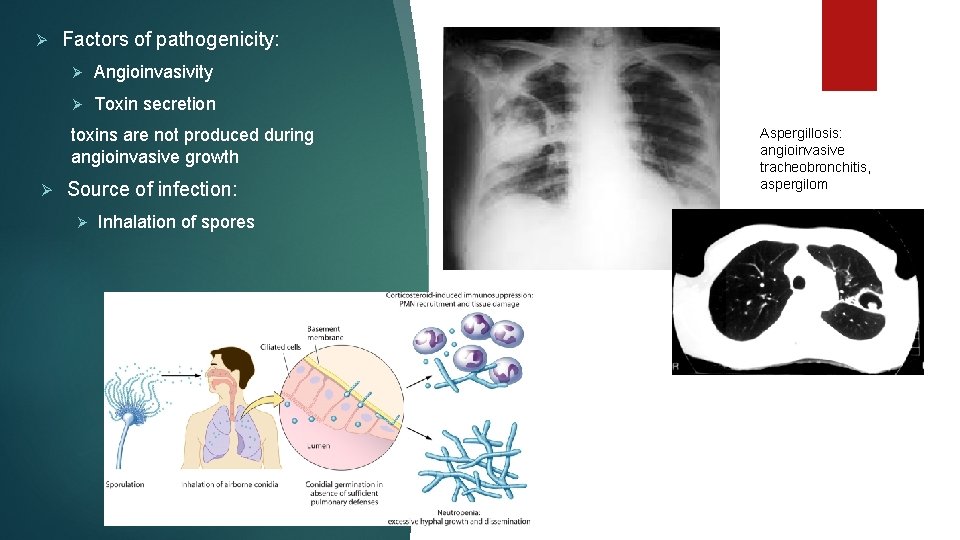
Ø Factors of pathogenicity: Ø Angioinvasivity Ø Toxin secretion toxins are not produced during angioinvasive growth Ø Source of infection: Ø Inhalation of spores Aspergillosis: angioinvasive tracheobronchitis, aspergilom

div. ZYGOMYCOTA Mucormycosis ü Mucorales: Mucor, Rhizomucor, Absidia, Rhizopus ü cosmopolitan, saprophytic ü Local infection of wounds, otitis ü Systemic infection – orofacialis, rhinocerebralis, lungs, GIT ü Diabetes mellitus – rhinocerebralis ü Leukemia - lungs ü Angioinvasive, causing trombosis – necrosis – fast and agressive ü High mortality ü Risk factor – immunosupresion ü Therapy – POSA, Amp. B + drastic surgery!! Rhizopus sp.
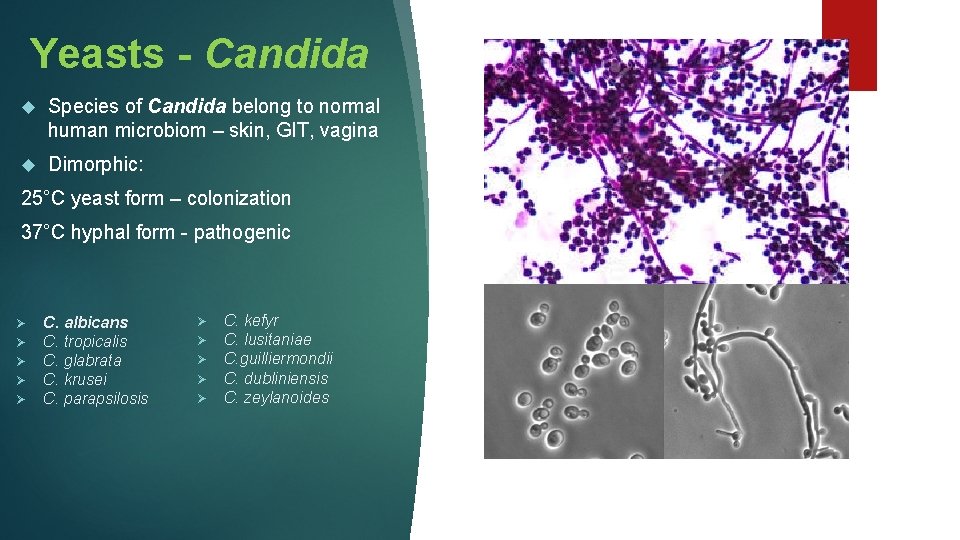
Yeasts - Candida Species of Candida belong to normal human microbiom – skin, GIT, vagina Dimorphic: 25°C yeast form – colonization 37°C hyphal form - pathogenic Ø Ø Ø C. albicans C. tropicalis C. glabrata C. krusei C. parapsilosis Ø Ø Ø C. kefyr C. lusitaniae C. guilliermondii C. dubliniensis C. zeylanoides
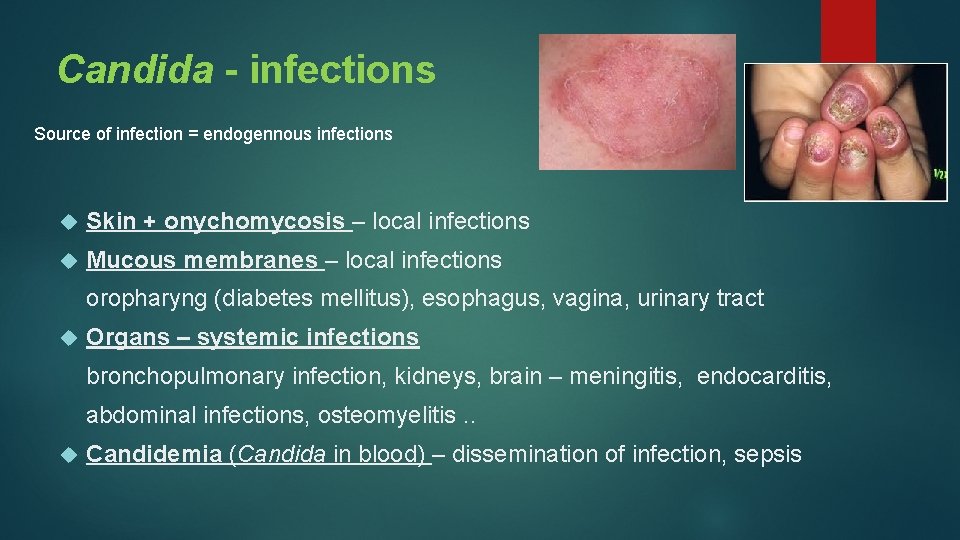
Candida - infections Source of infection = endogennous infections Skin + onychomycosis – local infections Mucous membranes – local infections oropharyng (diabetes mellitus), esophagus, vagina, urinary tract Organs – systemic infections bronchopulmonary infection, kidneys, brain – meningitis, endocarditis, abdominal infections, osteomyelitis. . Candidemia (Candida in blood) – dissemination of infection, sepsis

Candida - epidemiology 97% of infections – caused by C. albicans+C. glabrata+C. parapsilosis+C. krusei+C. tropicalis Decrease in C. albicans incidency x increase in the incidency of nonalbicans strains (40 -55%) C. tropicalis – neutropenic patients C. glabrata, C. krusei – after profylactic treatment with FLU (haematooncology) C. parapsilosis – newborn babies C. lusitaniae – after polyene treatment C. krusei – high mortality (57%)
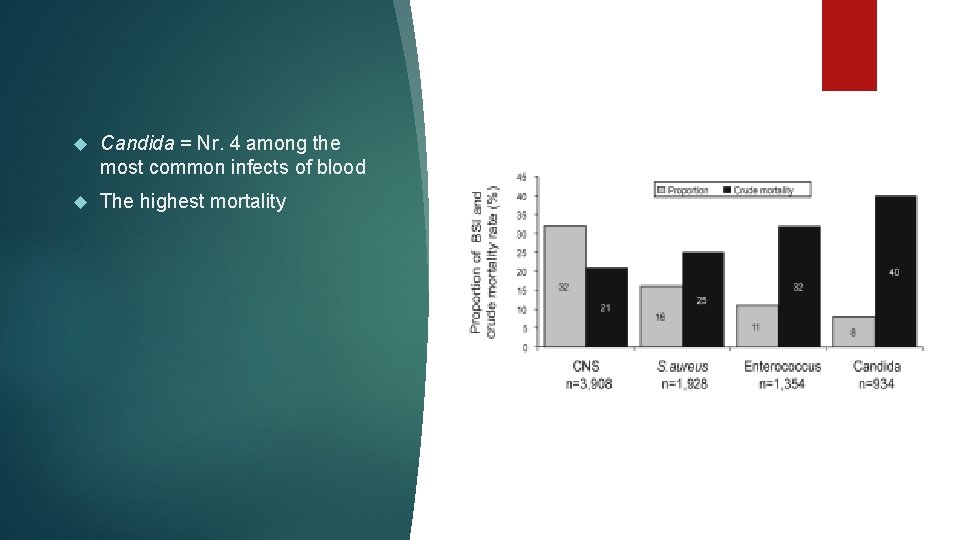
Candida = Nr. 4 among the most common infects of blood The highest mortality

Candida-infection of newborns Risk factors: Low weight Low gestational age Hospitalization – intensive care units Source of infection: mother hands of hospital staff

SOOR 2 weeks after birth white plaques on tongue, in oral cavity – cannot be easily removed – pain while sucking can disseminate further into GIT CNS – meningitis endocarditis marker of sepsis = interleukin therapy: liposomal Amphothericin B, fluconazole micafungin – low doses depending on the gestation age
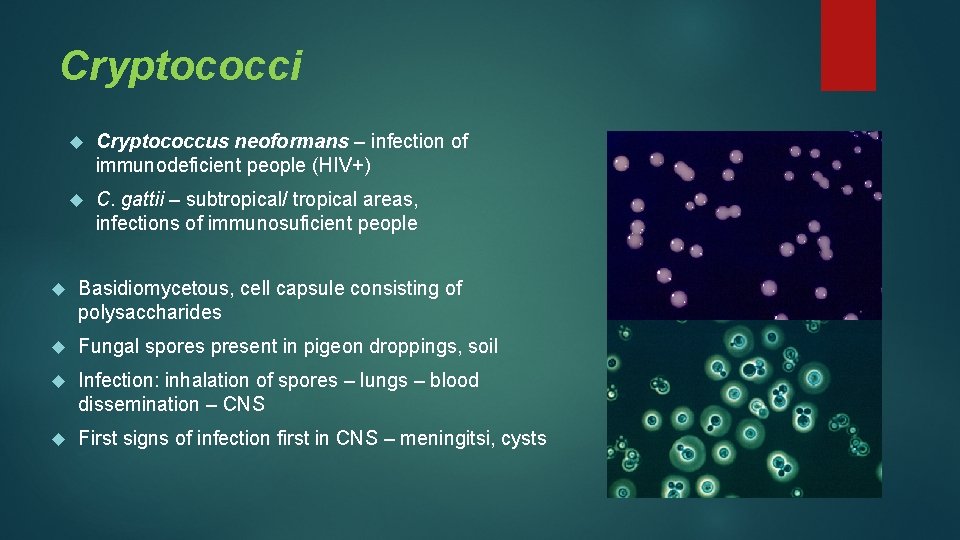
Cryptococci Cryptococcus neoformans – infection of immunodeficient people (HIV+) C. gattii – subtropical/ tropical areas, infections of immunosuficient people Basidiomycetous, cell capsule consisting of polysaccharides Fungal spores present in pigeon droppings, soil Infection: inhalation of spores – lungs – blood dissemination – CNS First signs of infection first in CNS – meningitsi, cysts
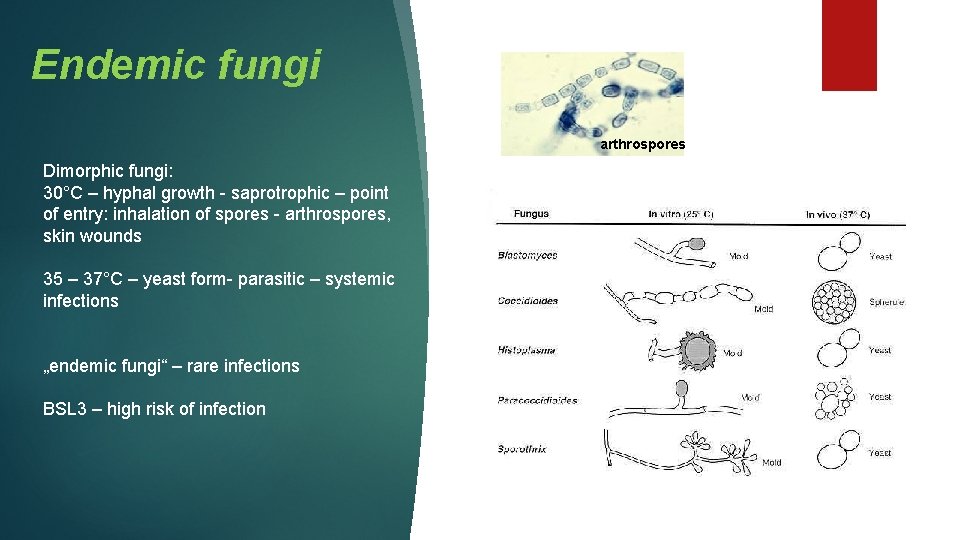
Endemic fungi arthrospores Dimorphic fungi: 30°C – hyphal growth - saprotrophic – point of entry: inhalation of spores - arthrospores, skin wounds 35 – 37°C – yeast form- parasitic – systemic infections „endemic fungi“ – rare infections BSL 3 – high risk of infection
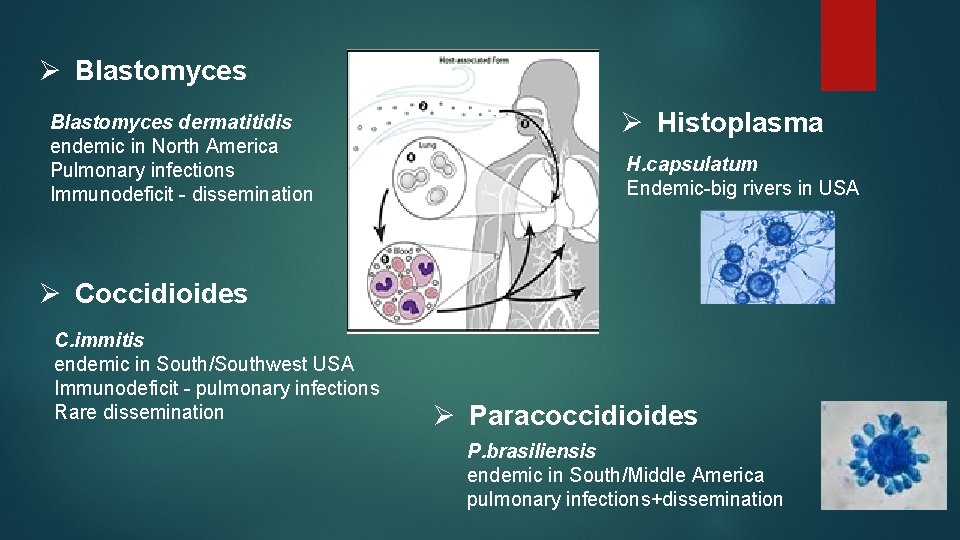
Ø Blastomyces dermatitidis endemic in North America Pulmonary infections Immunodeficit - dissemination Ø Histoplasma H. capsulatum Endemic-big rivers in USA Ø Coccidioides C. immitis endemic in South/Southwest USA Immunodeficit - pulmonary infections Rare dissemination Ø Paracoccidioides P. brasiliensis endemic in South/Middle America pulmonary infections+dissemination

PNEUMOCYSTIS JIROVECII Known since 1951: found in lungs of childern with pneumonia Formerly: Protozoa - Now: Ascomycetes Cosmopolitan, Causing infection – air pneumonia Risk factors: immunodeficites, transplantations, premature newborns Therapy: cotrimoxazol, pentamidin
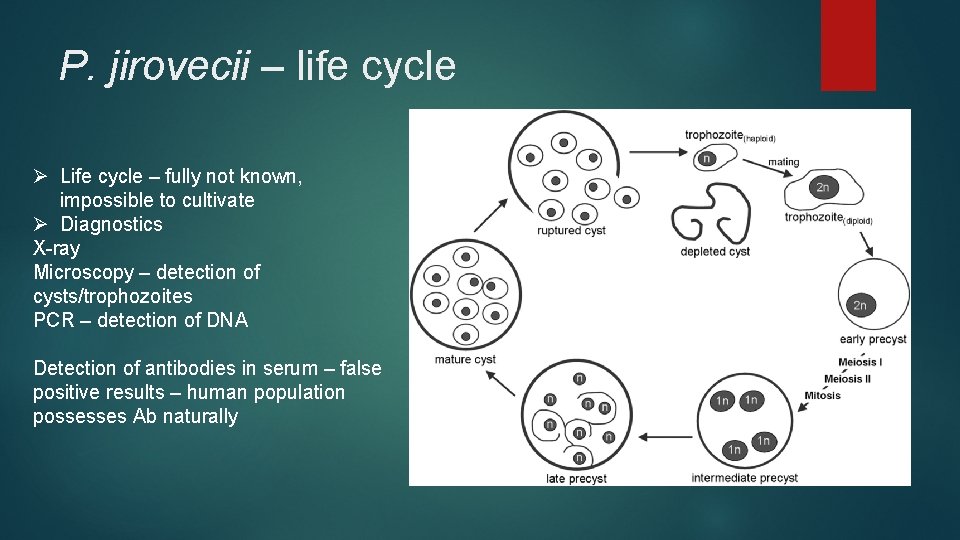
P. jirovecii – life cycle Ø Life cycle – fully not known, impossible to cultivate Ø Diagnostics X-ray Microscopy – detection of cysts/trophozoites PCR – detection of DNA Detection of antibodies in serum – false positive results – human population possesses Ab naturally

HIV+ associated fungal infections Pneumocystis jirovecii – pneumonia, extrapulmonary localization after ATB profylaxis Candida spp. incetions in esophagus Cryptococcus neoformans – pneumonia, CNS

THERAPY - Antimycotics Polyenes: amphotericin B, lipid-Amp. B, nystatin Azoles: fluconazole, itraconazol, ketoconazole, voriconazole, posaconazol, econazol, klotrimazol, oxiconazol, … Antimetabolites: flucytosin Echinocandines: caspofungin, anidulafungin, micafungin Others- systemic ATBs: griseofulvin, terbinafin
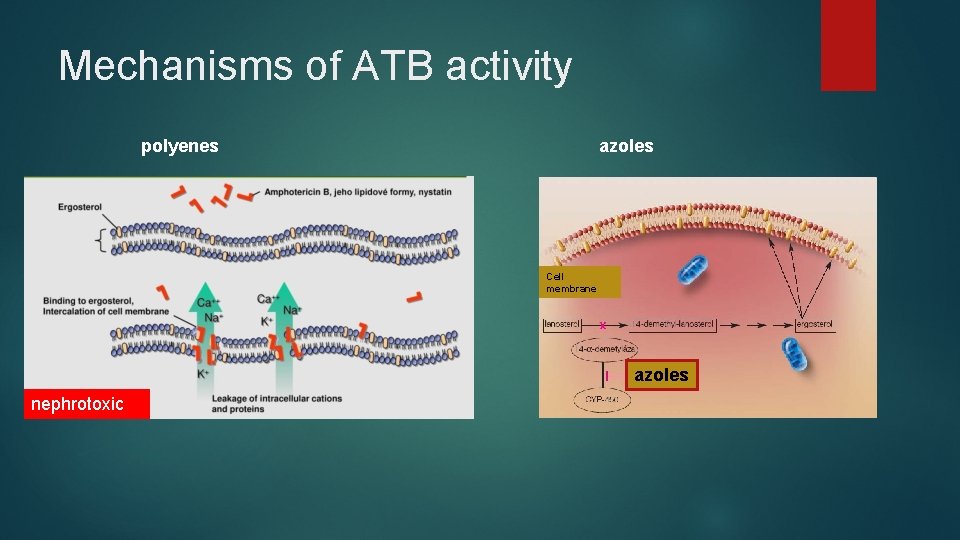
Mechanisms of ATB activity polyenes azoles Cell membrane azoles nephrotoxic
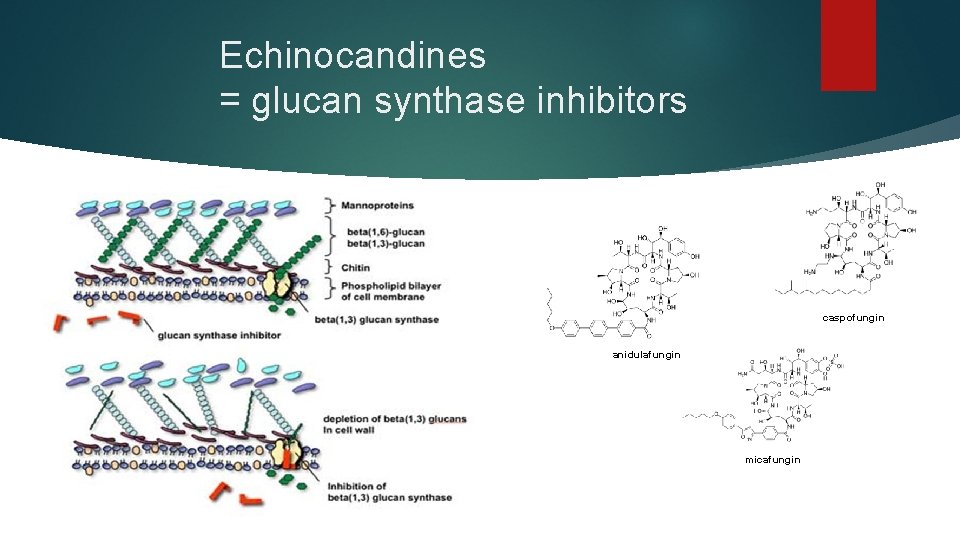
Echinocandines = glucan synthase inhibitors caspofungin anidulafungin micafungin
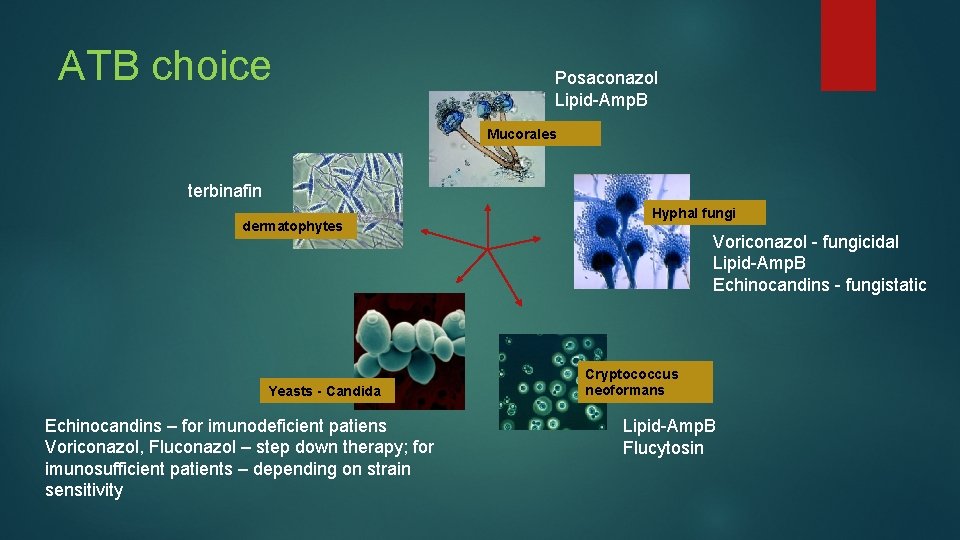
ATB choice Posaconazol Lipid-Amp. B Mucorales terbinafin dermatophytes Yeasts - Candida Echinocandins – for imunodeficient patiens Voriconazol, Fluconazol – step down therapy; for imunosufficient patients – depending on strain sensitivity Hyphal fungi Voriconazol - fungicidal Lipid-Amp. B Echinocandins - fungistatic Cryptococcus neoformans Lipid-Amp. B Flucytosin

Laboratory diagnostics What samples to take What to do with them to get results…. A set for sampling and shipping the samples in Amies medium
Samples… Upper/lower respiratory tract (throat, nose, sputum, bronchoalveolar lavage BAL) Gastrointestinal tract (stomach, gall, stool) Urogenital tract (urine, vagina) Blood (haemoculture) Cerebrospinal fluid Primarilly sterile materials

Sampling… dermatophytes Skin • Wash with 70% ethanol • Scrape skin from the edge of the affected area • in case of local ATB therapy – sampling first after 14 days Hair, nails – extract, do not cut/scrape nails Ship in a sterile tube – without any media – dermatophytes are oxygen demanding

Investigation methods in clinical mycology Microscopy –gram staining Cultivation –sabouraud agars antigen detection – beta-D-glucan, mannan, galactomannan – ELISA tests Molecular methods – PCR, MALDI-TOF
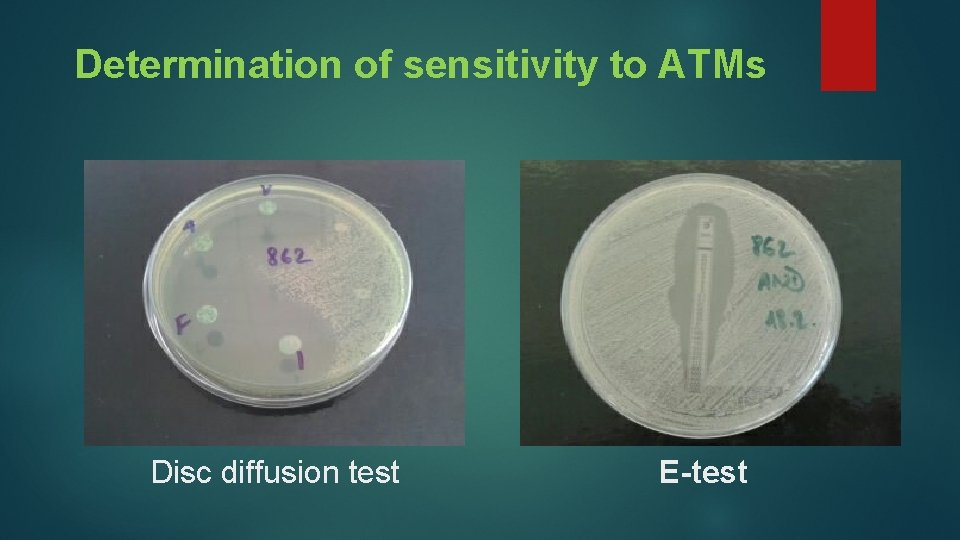
Determination of sensitivity to ATMs Disc diffusion test E-test

Thanks for your attention In case of any question do not hasitate to contact me. My email is: katerina. svobodova 3@vfn. cz
- Slides: 45