Introduction to CBT for Psychosis CBTP An Evidencebased

Introduction to CBT for Psychosis (CBT-P): An Evidence-based Treatment Robert Reiser, Ph. D: Licensed Psychologist, Kentfield, CA. Academy of Cognitive Therapy Certified Cognitive Therapist Website: www. robertreiser. com Email: robert. reiser@gmail. com Tel. 415 297 1016 (c) Robert Reiser, 2013, All Rights Reserved NAMI Marin General Meeting

Plan for tonight Introduction Brief review of evidence for CBT-P: Why evidence is important! Reassessing schizophrenia Basic CBT-P techniques with video and examples Training & implementation issues Your questions

(c) Robert Reiser, 2013, All Rights Reserved Brief review of evidence for CBT-P: Why evidence is important!

“. . . (the) mental health field must expand its efforts to develop and test new treatments and practices, to promote awareness of and improve training in evidence-based practices, and to better finance those practices” (Page 73) (c) Robert Reiser, 2013, All Rights Reserved The President’s New Freedom Commission on Mental Health Report: Transforming Mental Health Care in America (Final Report July, 2003)

“Evidence-based treatments” (EBTs) or “empirically-supported treatments” are treatments that have been determined to be effective based on research and a “gold standard” of science. Evidence based practice is defined by the Institute of Medicine: “the integration of bestresearched evidence and clinical expertise with patient values” [Institute of Medicine] (c) Robert Reiser, 2013, All Rights Reserved What is “evidence-based treatment”?

“…. the very first step in improving the quality of treatment for schizophrenia is stemming the tide of therapeutic nihilism which still flows far too strongly, with iatrogenic consequences. Evidence-based optimism is one obvious strategy and these guidelines document current evidence-based knowledge and recommendations. ’ Royal Australia and New Zealand College of Physicians guidelines, p 8 (c) Robert Reiser, 2013, All Rights Reserved “Evidence-based Optimism”

Therapeutic nihilism, pessimism, past disappointments, errors Over-reliance on a medical model understanding of schizophrenia Divisions between biological and psychosocial approaches Lack of training Lack of resource commitment Lack of a national scheme, plan (c) Robert Reiser, 2013, All Rights Reserved Some problems pointed out by researchers

Why psychotherapy is important in addition to medicine “Pharmacologic therapy can leave as many as 60% of psychotic patients with persistent positive and negative symptoms, even when the patients are compliant with their medication instructions. Furthermore, medication compliance remains a major problem despite the introduction of modern atypical antipsychotics. Studies have shown treatment discontinuation in an estimated 74% of patients in both outpatient and inpatient settings. ” Taken from: http: //www. psychiatrictimes. com/schizophrenia/abcscognitive-behavioral-therapy-schizophrenia/page/0/1 (c) Robert Reiser, 2013, All Rights Reserved

“NICE is an independent organisation responsible for providing national guidance on promoting good health and preventing and treating ill health. ” National Clinical Practice Guideline, Number CG 82 � (Slides taken directly from NICE guidelines) � Retrieved from: http: //www. nice. org. uk/ (c) Robert Reiser, 2013, All Rights Reserved National Institute for Clinical Excellence (NICE)

Psychological and psychosocial interventions: Offer cognitive behavioural therapy (CBT) to all people with schizophrenia. This can be started either during the acute phase or later. Offer family intervention to all families of people with schizophrenia who live with or are in close contact with the service user. This can be started either during the acute phase or later. *Nice Guidelines, National Clinical Practice Guideline, Number CG 82, update 2009, p. 21: www. nice. org. uk (c) Robert Reiser, 2013, All Rights Reserved NICE Guidelines- Effective psychosocial treatments*

NICE Guidelines- Summary (c) Robert Reiser, 2013, All Rights Reserved www. nice. org. uk

CBT should be delivered on a one-to-one basis over at least 16 planned sessions and: • follow a treatment manual − people can establish links between their thoughts, feelings or actions and their current or past symptoms, and/or functioning so that: − the re-evaluation of people’s perceptions, beliefs or reasoning relates to the target symptoms • also include at least one of the following components: − people monitoring their own thoughts, feelings or behaviours with respect to their symptoms or recurrence of symptoms − promoting alternative ways of coping with the target symptom − reducing distress − improving functioning. (c) Robert Reiser, 2013, All Rights Reserved Delivering psychological interventions, NICE guidelines

Family intervention should: • include the person with schizophrenia if practical • be carried out for between 3 months and 1 year • include at least 10 planned sessions • take account of the whole family's preference for either single- family intervention or multi-family group intervention • take account of the relationship between the main carer and the person with schizophrenia • have a specific supportive, educational or treatment function and include negotiated problem solving or crisis management work. (c) Robert Reiser, 2013, All Rights Reserved

CBT versus ‘Befriending therapy’ (c) Robert Reiser, 2013, All Rights Reserved Effectiveness of CBT

Sensky, T. , Turkington, D. , Kingdon, D. , Scott, J. L. , Siddle, R. , O'Carroll, M. , & Barnes, T. R. E. A RANDOMIZED CONTROLLED TRIAL OF COGNITIVE-BEHAVIOURAL THERAPY FOR PERSISTENT SYMPTOMS IN SCHIZOPHRENIA RESISTANT TO MEDICATION. i Archives of General Psychiatry 2000, 57, 165 -172. Note: slides 15 -24 taken from Turkington, CIMH workshop, May, 2013.

‘BEFRIENDING’ Focus on neutral non-threatening topics No active formulation No active techniques taught or used Non-confrontational Non-colluding Empathic Supportive Accepting Note, taken from Turkington, CIMH workshop, May, 2013 ’ (Samarasekera et al, 2007)

RESULTS: Ninety patients received a mean of 19 individual treatment sessions over 9 months, with no significant between-group differences in treatment duration. Both interventions resulted in significant reductions in positive and negative symptoms and depression. At the 9 -month follow-up evaluation, patients who had received cognitive therapy continued to improve, while those in the befriending group did not. These results were not attributable to changes in prescribed medication. CONCLUSION: Cognitive-behavioral therapy is effective in treating negative as well as positive symptoms in schizophrenia resistant to standard antipsychotic drugs, with its efficacy sustained over 9 months of follow-up. (c) Robert Reiser, 2013, All Rights Reserved Sensky et al. (2000) A randomized controlled trial of cognitive-behavioral therapy for persistent symptoms in schizophrenia resistant to medication.
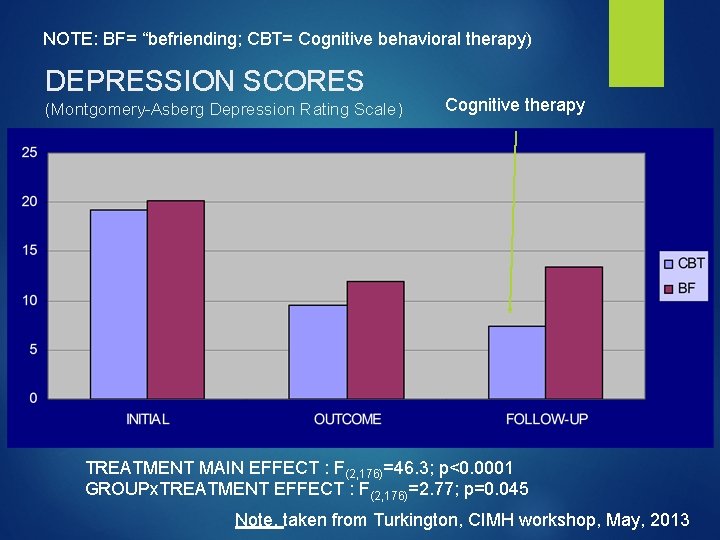
NOTE: BF= “befriending; CBT= Cognitive behavioral therapy) DEPRESSION SCORES (Montgomery-Asberg Depression Rating Scale) Cognitive therapy TREATMENT MAIN EFFECT : F(2, 176)=46. 3; p<0. 0001 GROUPx. TREATMENT EFFECT : F(2, 176)=2. 77; p=0. 045 Note, taken from Turkington, CIMH workshop, May, 2013
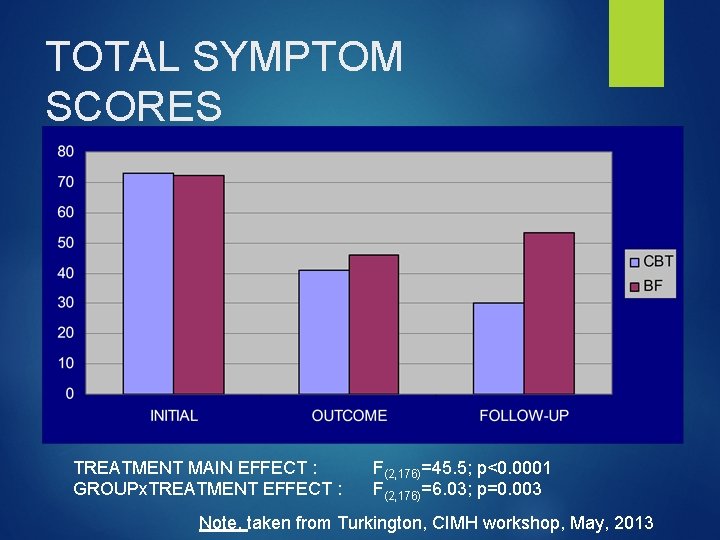
TOTAL SYMPTOM SCORES (Comprehensive psychopathological rating scale) TREATMENT MAIN EFFECT : GROUPx. TREATMENT EFFECT : F(2, 176)=45. 5; p<0. 0001 F(2, 176)=6. 03; p=0. 003 Note, taken from Turkington, CIMH workshop, May, 2013
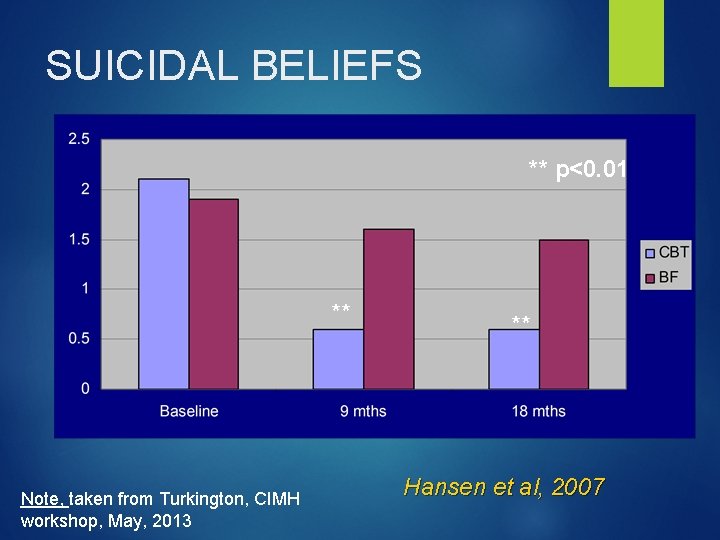
SUICIDAL BELIEFS ** p<0. 01 ** Note, taken from Turkington, CIMH workshop, May, 2013 ** Hansen et al, 2007
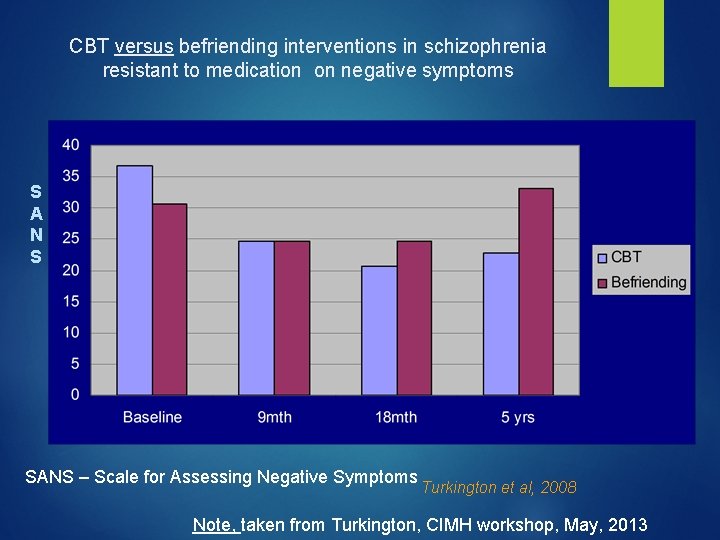
CBT versus befriending interventions in schizophrenia resistant to medication on negative symptoms S A N S SANS – Scale for Assessing Negative Symptoms Turkington et al, 2008 Note, taken from Turkington, CIMH workshop, May, 2013

Befriending vs CBT Study Results Positive, negative, and depressive symptoms including suicidal thoughts decreased with CBT Number showing greater than 50% improvement: 63% in CBT group v 39% with befriending (on CPRS) Enduring effect at 5 years Befriending effect on severe persecutory paranoia and none on hallucinations. Note, taken from Turkington, CIMH workshop, May, 2013

Evidence for CBT for Psychosis Note, Slide taken from Turkington, CIMH workshop, May, 2013 • Average effect size for target symptom (33 studies) =. 40 • Average effect size for “rigorous” RCTs (12 studies) =. 22 • Significant effects (ranging from. 35 –. 44) for: • Positive symptoms (32 studies) • Negative symptoms (23 studies) • Functioning (15 studies) • Mood (13 studies) • Social anxiety (2 studies) Wykes et al, 2008 – also Pilling et al 2002 & Zimmerman et al 2006 • Further evidence of cost effectiveness Peters et al, 2012 • Equivalence between CBTP & supportive therapies? Cochrane Review, 2013: Lynch et al, 2009

Current Evidence (psychosis) Note, taken from Turkington, CIMH workshop, May, 2013 Under 16 16 -65 Over 65 White No substance misuse Non-White Substance misusers Substance abusers Prodromal Early Persistent Acute wards Community Forensic None Case studies 1 -2 RCTs Meta-analyses/ RCTs

Psychoanalytic or psychodynamic therapy Therapy based on the double-bind hypothesis of schizophrenia (1970 s) Low level, stand alone case management Mega vitamin therapy Other? (c) Robert Reiser, 2013, All Rights Reserved Some ineffective or harmful treatments for schizophrenia

(c) Robert Reiser, 2013, All Rights Reserved Reassessing schizophrenia

Demographics, Risk Factors Social outcome poorer in developed countries Ø High morbidity and mortality rates “The excessive mortality of patients with schizophrenia has been reported to be two to four times that of the general population. About 4%– 10% of persons with schizophrenia die by suicide, and the rate are highest among males in the early course of the disorder and in industrialized countries. ” APA Practice Guidelines for the Treatment of Psychiatric Disorders, 2004. (c) Robert Reiser, 2013, All Rights Reserved Ø

“The long-term outcome of schizophrenia varies along a continuum between reasonable recovery and total incapacity. About 10%– 15% of persons with the disorder are free of further episodes but the majority display exacerbations and remissions in the context of experiencing clinical deterioration, and about 10%– 15% remain chronically severely psychotic. ” APA Practice Guidelines for the Treatment of Psychiatric Disorders, 2004), p. 316) (c) Robert Reiser, 2013, All Rights Reserved Course of Illness, traditional view

Ø The International Study of Schizophrenia (World Health Organization, 2001) provided a long-term follow-up study of 1, 633 people diagnosed with schizophrenia. 75% were available for follow-up � 50% had a favourable outcome � 16% had a delayed recovery after an early unremitting course. � Source: A Report From the WHO Collaborative Project, the International Study of Schizophrenia. 2007. Eds. Kim Hopper, Glynn Harrison, Aleksandar Janca, and Norman Sartorius. Oxford: Oxford University Press (c) Robert Reiser, 2013, All Rights Reserved But, how certain are we on the course of schizophrenia

According to the UK’s Royal College of Psychiatrists, for every five people who develop schizophrenia: 1 in 5 will get better within five years of their first episode of schizophrenia. 3 in 5 will get better, but will still have some symptoms. They will have times when their symptoms get worse. 1 in 5 will continue to have troublesome symptoms. Taken from: http: //www. helpguide. org/mental/schizophrenia_treatment _support. htm (c) Robert Reiser, 2013, All Rights Reserved Course and prognosis, continued

“Heterogeneity of outcome, both in terms of symptoms and functioning, is the signature feature, an observation that has profound implications for our understanding and management of the condition. “ Ø Good outcome was evident in more than 50% of the International Study of Schizophrenia subjects. Ø 60+% of patients found to be recovered Ø (criteria: no long term disability, full time work). Source: Am J Psychiatry 164: 1444 -1445, September 2007 Book Review A Report From the WHO Collaborative Project, the International Study of Schizophrenia. 2007. Eds. Kim Hopper, Glynn Harrison, Aleksandar Janca, and Norman Sartorius. Oxford: Oxford University Press. (c) Robert Reiser, 2013, All Rights Reserved Recovery From Schizophrenia: An International Perspective (WHO)

Outcome-Revisited This 5 -year study found that 62% of people at follow-up showed overall improvement on a composite measure of clinical and functional outcomes* * Source: Harvey CA, Jeffreys SE, Mc. Naught AS, Blizard RA, King MB (2007). "The Camden Schizophrenia Surveys III: Five-Year Outcome of a Sample of Individuals From a Prevalence Survey and the Importance of Social Relationships". International Journal of Social Psychiatry 53 (4): 340– 35 (c) Robert Reiser, 2013, All Rights Reserved Ø

Predictors of Course of Illness “…better outcomes are associated, on average, with: female gender, family history of affective disorder, lack of family history of schizophrenia, good premorbid social and academic functioning, higher IQ, …” (c) Robert Reiser, 2013, All Rights Reserved APA Practice Guidelines for the Treatment of Psychiatric Disorders, 2004, p. 316.

Predictors of Course of Illness “married marital status, later age of onset acute onset with precipitating stress, fewer prior episodes (both number and length), a phasic pattern of episodes and remissions, advancing age, minimal comorbidity, paranoid subtype, and symptoms that are predominantly positive (delusions, hallucinations) and not disorganized (thought disorder, disorganized behavior) or negative (flat affect, alogia, avolition)” (c) Robert Reiser, 2013, All Rights Reserved (APA Practice Guidelines for Treatment of Psychiatric Disorders, 2004, p. 316 -318)

Familial pattern “It appears that the course is influenced by cultural factors and societal complexity, with better outcomes in developing countries. ” (APA, 2004) Ø ~10 X risk in first degree biological relatives Ø “lifetime risk is 13% for a child with one parent with schizophrenia and 35%– 40% for a child with two affected parents” (APA Practice Guidelines for Treatment of Psychiatric Disorders, 2004) Ø But Kingdon notes that even in studies of identical twins the rate of concordance is only 36%. (Kingdon, 2005, p. 5) (c) Robert Reiser, 2013, All Rights Reserved Ø

(c) Robert Reiser, 2013, All Rights Reserved Basic techniques with video and examples

(c) Robert Reiser, 2013, All Rights Reserved CBT: General approach

CBT, general approach Structured Collaborative Problem oriented Time effective (but not necessarily time limited) Practical-oriented to current problems, improving functioning Uses guided discovery, a non confrontational method for exploring problems, symptoms (c) Robert Reiser, 2013, All Rights Reserved

People with severe mental disorders can connect deeply with others …. can live purposeful, value driven, committed lives The purpose of therapy is to help people live richer, fuller lives, as they define it, in the face of ongoing symptoms and problems Respect limitations: foster realistic hope Taken from: Fowler, D. (2004) San Jose Presentation (c) Robert Reiser, 2013, All Rights Reserved Underlying philosophy of treatment

“Gentle engagement”- start where the person is in terms of their understanding of the illness - avoid jargon Normalizing (but not minimizing distress, symptoms)and educating Destigmatizing illness and instilling hope Start out with ‘guided discovery ‘ - a low key conversational exploration of the distressing problems (c) Robert Reiser, 2013, All Rights Reserved Specific Treatment Approach

Setting goals for treatment Client centered Reducing distress and disability is a key goal Target area(s) of functioning affected by symptoms (voices, delusions, negative symptoms) Start with small, manageable goals Encourage willingness and commitment Taken from: Fowler, D San Jose Presentathion (c) Robert Reiser, 2013, All Rights Reserved

CBT stages of treatment Engaging, developing an alliance II. Normalizing, remoralizing, destigmatizing III. Developing a collaborative understanding -explaining problems in a more helpful way IV. Helping with distressing and disabling behavior using the ABC model V. Help with distressing beliefs, meanings of the symptoms (hallucinations, delusions) (c) Robert Reiser, 2013, All Rights Reserved I.

“Columbo” Style (c) Robert Reiser, 2013, All Rights Reserved Therapist is careful not to make confrontational statements, does not want to contradict the client (avoid confrontation!) Therapist might appear confused or slow-witted, apologizing for not understanding Therapist should then follow client explanations w/questions for clarification & details

Normalizing, destigmatizing (c) Robert Reiser, 2013, All Rights Reserved Example of CBT:

Exercise: Try to find an explanation for this problem that is normalizing A 16 year old high school junior is afraid to go to school because she is afraid that other people are talking about her. Sometimes she sees other groups of friends laughing and she thinks they might be laughing at her. She feels very anxious and embarrassed. (c) Robert Reiser, 2013, All Rights Reserved

Illness is produced by a combination of environmental stressors and problematic responses (distress) and innate vulnerability conferred by biology, genes, etc. The message is: ‘We can work on things that are bothering you in a helpful way to reduce distress and disability associated with distress or poor coping skills (c) Robert Reiser, 2013, All Rights Reserved Using the Vulnerability. Stress Model

Vulnerability-stress model (Kingdon, D. , San Jose Presentation, 2004) S t r e s s WELL Decompensate family attitudes, self-esteem loss of job, home, friends Vulnerability (c) Robert Reiser, 2013, All Rights Reserved ILL

Problem-solving, improving coping strategies (c) Robert Reiser, 2013, All Rights Reserved Example of CBT:

EMOTIONS THOUGHTS BEHAVIOR

EMOTIONS: Feel angry, upset attacked. THOUGHTS: The voice is criticizing me again BEHAVIOR: Scream back at the voice And shake my fist
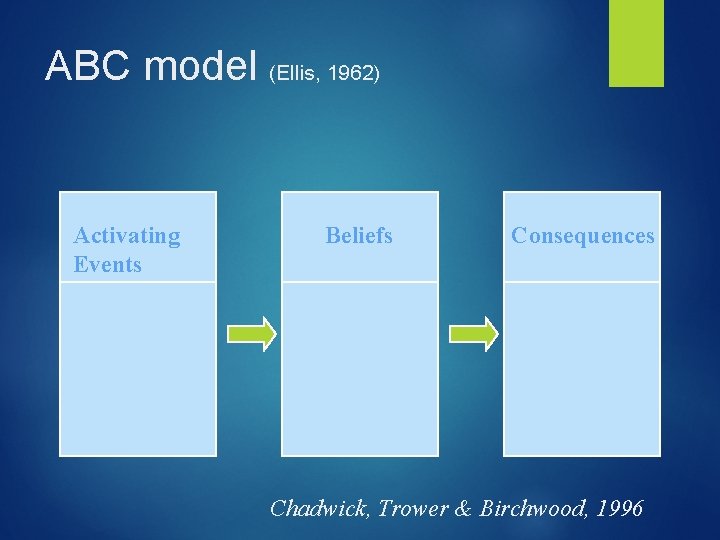
ABC model (Ellis, 1962) Activating Events Beliefs Consequences Chadwick, Trower & Birchwood, 1996
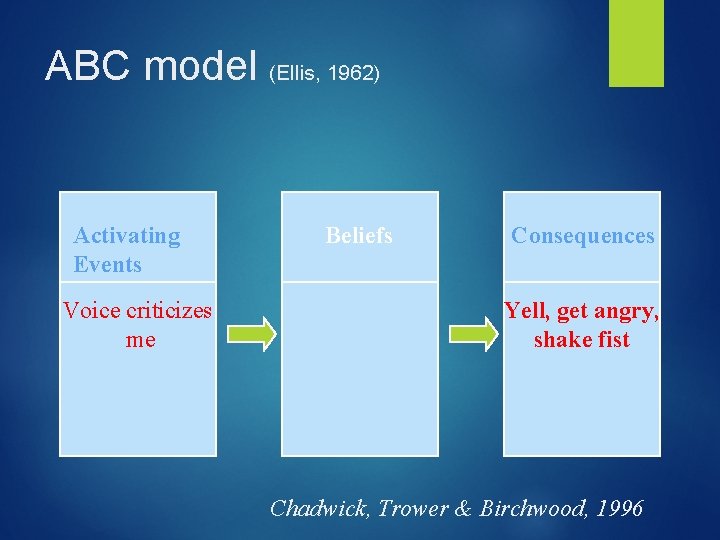
ABC model (Ellis, 1962) Activating Events Voice criticizes me Beliefs Consequences Yell, get angry, shake fist Chadwick, Trower & Birchwood, 1996

Goal: Improving Client’s Coping Strategies Can we control any of the antecedents(As) (what comes before…problems sleeping, medication, self care, stressors, improving awareness of mood states, feelings, interpersonal problems and conflicts) Can we change any of the consequences (Cs), what comes after (feeling angry, yelling, shaking fist) Using attentional distraction techniques (headphones, refocusing, getting engaged) Suggesting alternate responses, behaviors-talking back silently, postponing response Note that we don’t have to change beliefs to improve behaviors. Later we will discuss dealing with B’s (beliefs) (c) Robert Reiser, 2013, All Rights Reserved

Using Distraction Humming Talking to yourself Listen to music Engage in a pleasant activity Meditation or prayer Phone a friend Exercise Adapted from: List of 60 Coping Strategies for Hallucinations, Turkington, CIMH, May 2013 workshop materials (c) Robert Reiser, 2013, All Rights Reserved Possible coping strategies for voices

Focusing, or refocusing or engaging Use a normalising or more compassionate explanation Subvocalisation, talk back quietly Use rational responses to reduce anger Remind yourself that no one else can hear the voice Phone a voice buddy and tell them the voice is active Remember to take antipsychotic medication Adapted from: List of 60 Coping Strategies for Hallucinations, Turkington, CIMH, May 2013 workshop materials (c) Robert Reiser, 2013, All Rights Reserved Possible coping strategies for Voices

(c) Robert Reiser, 2013, All Rights Reserved Understanding cognitive vulnerabilities, explanatory models

Externalizing- making external causal attributions to protect sense of self/self-esteem Personalizing Making arbitrary inferences Chadwick et al (1996): a vulnerability to view self negatively: ‘poor me’, ‘bad me’ (c) Robert Reiser, 2013, All Rights Reserved What creates additional psychological vulnerability for individuals with schizophrenia

• A very specific cognitive deficit that results in difficulty appropriately distinguishing between internal stimuli and external stimuli • There is a specific deficit in the internal monitoring system and sense of conscious experience and effort associated with our internal thoughts, intentions, goals • This leads to a misinterpretation that our thoughts, feelings, sense of self are ‘alien’ or unintended (c) Robert Reiser, 2013, All Rights Reserved Alternate Explanatory Models (Firth, 1987)

Deficits in social understanding and accurately understanding the intentions of others (theory of mind)might complement this resulting in a basis for developing delusions (c) Robert Reiser, 2013, All Rights Reserved Alternate Explanatory Models (Firth, 1987)

• The automatic assessment of significance (or lack of significance) is impaired – • Non-relevant stimuli might be seen as ‘important ‘ and might be attended to- including thoughts and memories This could account for the delusional conviction that irrelevant events have great significance – This theory would predict that people with schizophrenia might rapidly jump to conclusions on the basis of weak or irrelevant evidence (c) Robert Reiser, 2013, All Rights Reserved Alternate Explanatory Models (Hemsley, 1986)

Problem-solving, improving coping strategies (c) Robert Reiser, 2013, All Rights Reserved Example of CBT:

EMOTIONS THOUGHTS BEHAVIOR

THOUGHTS: I’m no good EMOTIONS: Feel depressed BEHAVIOR: Stay in bed
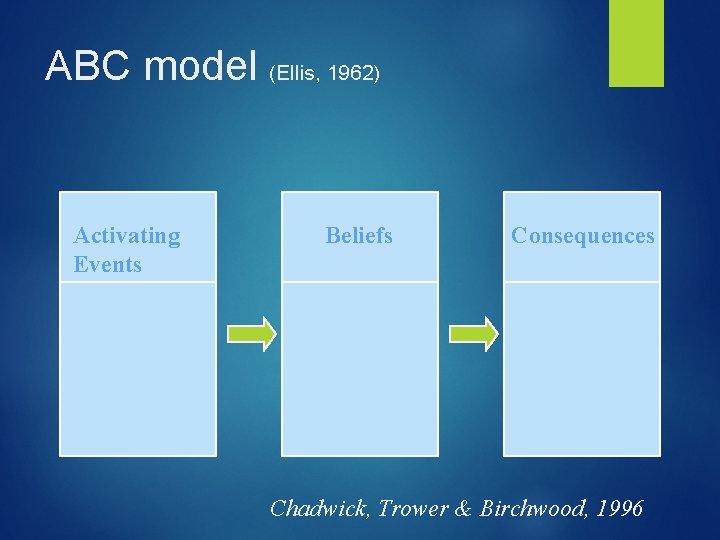
ABC model (Ellis, 1962) Activating Events Beliefs Consequences Chadwick, Trower & Birchwood, 1996

ABC model (Ellis, 1962) Activating Events Voice tells me I’m rotten, no good Beliefs Consequences This must be true The voice is Powerful. Feel depressed, Stay at home Chadwick, Trower & Birchwood, 1996

Improving coping strategies we alter some of the consequences (staying in bed) to help the person feel better. We might use behavioral activation, gradually moving towards increasing enjoyable behaviors, activities associated with a sense of accomplishment or mastery. (c) Robert Reiser, 2013, All Rights Reserved Can
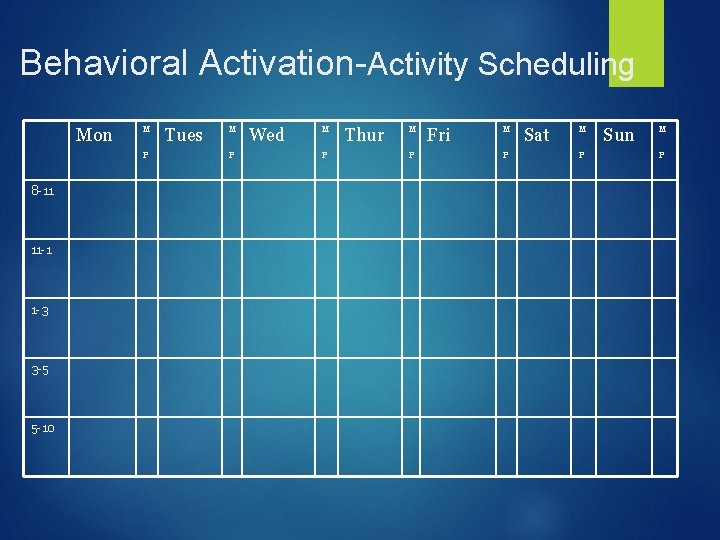
Behavioral Activation-Activity Scheduling Mon M P 8 -11 11 -1 1 -3 3 -5 5 -10 Tues M P Wed M P Thur M P Fri M P Sat M P Sun M P

Enhancing Client’s Coping Strategies: Summary (c) Robert Reiser, 2013, All Rights Reserved Select distressing symptoms Assist client in identifying antecedents & consequences & their usual way of coping with the symptoms Suggest ways of improving client’s coping strategies or suggest ones that have not been attempted Coping strategies should be practiced in session & eventually assigned as homework Review & assess effectiveness of newly practiced strategies

Working with problematic beliefs (delusions) (c) Robert Reiser, 2013, All Rights Reserved Example of CBT:

(c) Robert Reiser, 2013, All Rights Reserved Video Example-Working with delusions

(c) Robert Reiser, 2013, All Rights Reserved Training & implementation issues

(c) Robert Reiser, 2013, All Rights Reserved Summary: Where we are with improving treatment for people with schizophrenia and their families?

Drake et al, 2009* “Over the last decade, a consensus has emerged regarding a set of evidence-based practices for schizophrenia that address symptom management and psychosocial functioning. Yet, surveys suggest that the great majority of the population of individuals with schizophrenia do not receive evidencebased care. ” Drake, Robert E. ; Bond, Gary R. ; Essock, Susan M. ; Schizophrenia Bulletin, Vol 35(4), Jul, 2009. pp. 704 -713. (c) Robert Reiser, 2013, All Rights Reserved

Current services are not routinely evaluated for evidence for effectiveness Ø The system is married to providing services based on the status quo Ø Ø Ø (“We have always done it this way”, “Everyone does it this way”) Practice often lags behind research Source for Slides: Corrigan, P. et al. 2001. Strategies for Disseminating Evidence-Based Practices to Staff who Treat People with Serious Mental Illness. Psychiatric Services, 52, 1598 -1604 (c) Robert Reiser, 2013, All Rights Reserved Why is there a gap in implementing evidencebased practices?

Difficulty in implementing new practices at the administrative level: 2. 3. 4. 5. 6. Threat to the status quo (“We’ve been doing this for years”-- the “sunk costs” of bad investments” principle) Need to change system priorities at high administrative level and at service level Demoralization of staff and limited resources Crisis oriented management Difficulty “getting the word out” Costs of retraining staff (c) Robert Reiser, 2013, All Rights Reserved 1.

Individual clinicians lack of knowledge and skills Limited staff time for training Leadership, organizational structure and provider team dynamics that does not actively support implementation of new practices (c) Robert Reiser, 2013, All Rights Reserved Difficulty in implementing new practices at the clinician level

(c) Robert Reiser, 2013, All Rights Reserved Resources


Resources for Families Think You're Crazy? Think Again: A Resource Book for Cognitive Therapy for Psychosis By Anthony P. Morrison, Julia Renton, Paul French, Richard Bentall Overcoming Paranoid and Suspicious Thoughts: A self -help guide using cognitive behavioral techniques by Daniel Freeman, Jason Freeman, and Philippa Garety. Back to l. Ife, Back to normality: Recovery, cognitive therapy and Psychosis. Turkington, D et al (2009) Cambridge University Press: Cambridge. (c) Robert Reiser, 2013, All Rights Reserved

Suggested resources The Complete Family Guide to Schizophrenia: Helping Your Loved One Get the Most Out of Life (Paperback) “Authors Kim T. Mueser, Ph. D, and Susan Gingerich, MSW, walk readers through a range of treatment and support options that can lead to a better life for the entire family. …Families learn to help their loved ones manage day-to-day tasks, develop friendships, and set personal life goals. Like no other book, this powerful, practical resource helps families stay connected to the individual behind the disorder so they can work together toward recovery. ” Taken from: http: //schizophrenia. com/media/ (c) Robert Reiser, 2013, All Rights Reserved

Resources on the web Hearing Voices Network http: //www. mind. org. uk/Information/Booklets/Ot her/The+voice+inside. htm (A practical guide to understanding voice hearing. ) (c) Robert Reiser, 2013, All Rights Reserved Academy of Cognitive Therapy http: //www. academyofct. org (How to find a cognitive therapist, recommended reading, new research)

Resources on the web www. hearingvoices. org. uk/info_resources 11. htm (Website that gives over 20 examples of good advice on coping with voice hearing) www. paranoidthoughts. com (Helpful advice on coping with paranoia; based on “Overcoming Paranoid and Suspicious Thoughts” book by Freeman, and Garety (c) Robert Reiser, 2013, All Rights Reserved

The PART Program at UCSF Close monitoring of symptoms Comprehensive clinical feedback and provided with treatment recommendations Paid participation for some assessment procedures Collaboration with treatment providers Free consultation with psychiatrist

PREP/PART Referrals Call: (415) 476 -7278 Visit: www. prepwellness. org

(c) Robert Reiser, 2013, All Rights Reserved Your questions
- Slides: 85