Introduction to ANS Pharmacology Dr Kaukab Azim Dr

Introduction to ANS Pharmacology Dr. Kaukab Azim + Dr. Hanin Osama

NS • Central – Brain – Spinal cord • Peripheral – Afferent (sensory) – Efferent (motor, autonomic )
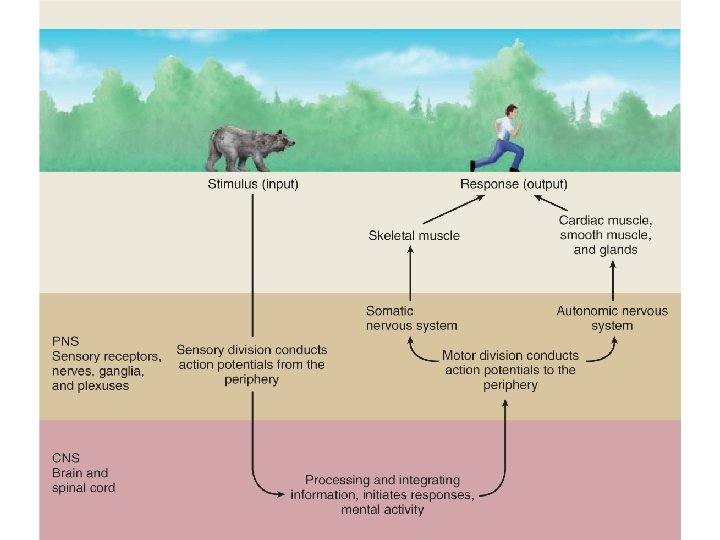
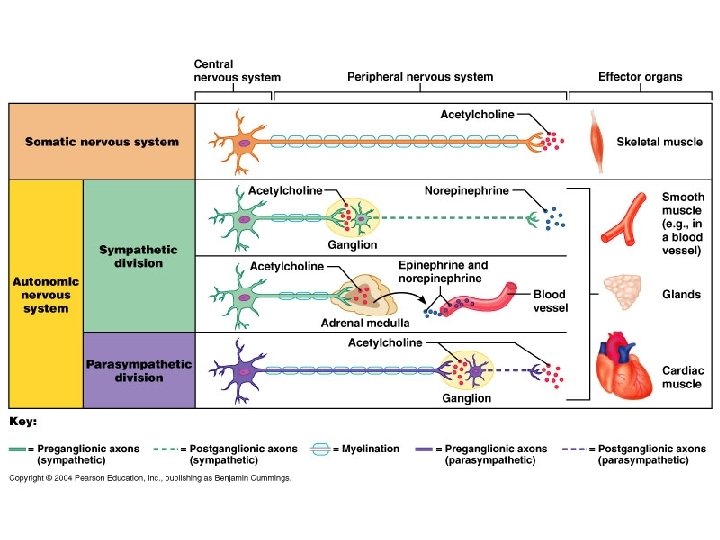

ANS Regulates Involuntary Functions • • Blood pressure Heart rate Respiration Body Temperature Glandular Secretion Digestion Reproduction

• The ANS facilitates immediated physical reactions associated with a preparation for violent muscular action. • Acceleration of heart and lung action • Paling or flushing, or alternating between both. • Inhibition of stomach and upper intestinal action (digestion slows down or stops) • Liberation of nutrients for muscular action • Dilation of blood vessels for muscles • Inhibition of Lacrimal gland salivation • Dilation of pupil
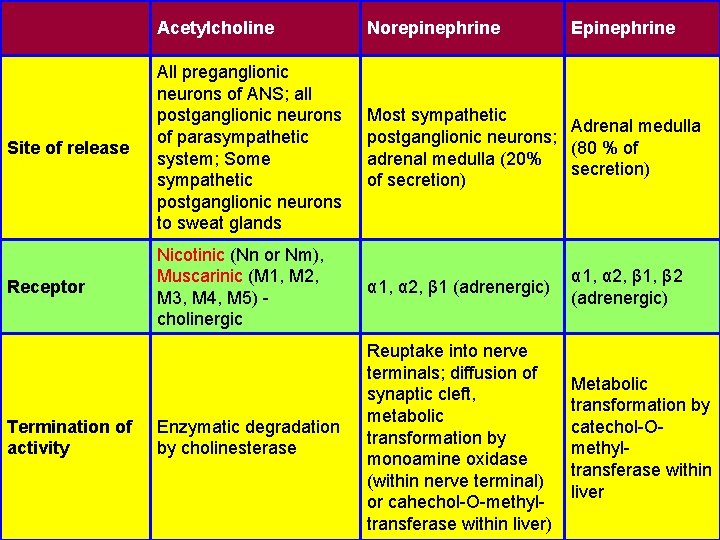
Acetylcholine Norepinephrine Site of release All preganglionic neurons of ANS; all postganglionic neurons of parasympathetic system; Some sympathetic postganglionic neurons to sweat glands Most sympathetic Adrenal medulla postganglionic neurons; (80 % of adrenal medulla (20% secretion) of secretion) Receptor Nicotinic (Nn or Nm), Muscarinic (M 1, M 2, M 3, M 4, M 5) cholinergic α 1, α 2, β 1 (adrenergic) α 1, α 2, β 1, β 2 (adrenergic) Enzymatic degradation by cholinesterase Reuptake into nerve terminals; diffusion of synaptic cleft, metabolic transformation by monoamine oxidase (within nerve terminal) or cahechol-O-methyltransferase within liver) Metabolic transformation by catechol-Omethyltransferase within liver Termination of activity Epinephrine

Location of cholinergic transmission • • • All autonomic ganglia Voluntary muscles (neuromuscular junction) Adrenal medulla (secretion of adrenaline) Post ganglionic parasympathetic Post ganglionic sympathetic to sweat glands

Sympathetic System Parasympathetic System Originates in thoracic and lumbar regions of the spinal cord (T 1 – L 2) Originates in brainstem (cranial nerves III, VII, IX, and X) and sacral region of spinal cord (S 2 – S 4) Ganglia located in paravertebral sympathetic ganglion chain Terminal ganglia located near or embedded within target tissue Short pre-ganglionic fibers Long postganglionic fibers Long pre-ganglionic fibers Short postganglionic fibers Ratio of pre-ganglionic fiber to postganglionic fibers is 1 : 20 Ratio of pre-ganglionic fibers to postganglionic fibers is 1 : 3 Activity often involves mass discharge of entire system Activity normally to discrete organs Primary neurotransmitter of postganglionic neurons is norepinephrine Primary neurotransmitter of postganglionic neurons is acetylcholine Predominates during emergency “fight-orflight” reactions and exercise Predominates during quiet resting conditions Divergence coordinates activity of neurons at multiple levels of spinal cord Limited divergence
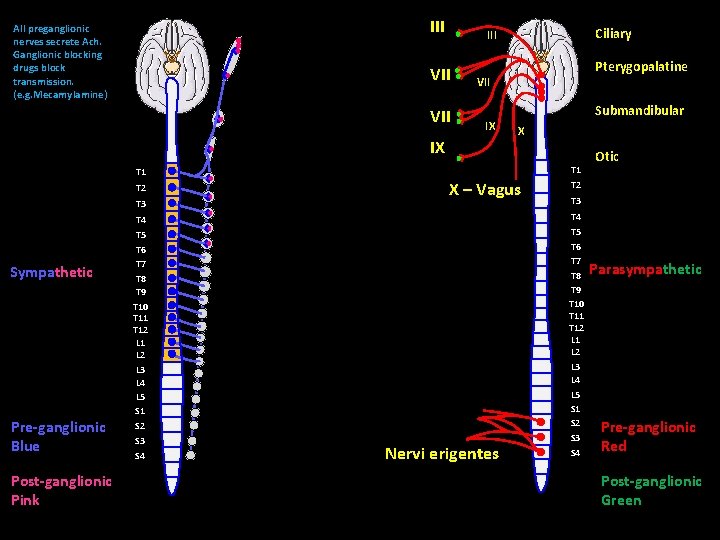
III All preganglionic nerves secrete Ach. Ganglionic blocking drugs block transmission. (e. g. Mecamylamine) Ciliary III VII Pterygopalatine VII Submandibular IX IX X T 1 T 2 T 3 Sympathetic Pre-ganglionic Blue Post-ganglionic Pink X – Vagus T 2 T 3 T 4 T 5 T 6 T 7 T 8 T 9 T 10 T 11 T 12 L 1 L 2 L 3 L 4 L 5 S 1 S 2 S 3 S 4 Nervi erigentes Otic S 4 Parasympathetic Pre-ganglionic Red Post-ganglionic Green

Acetyl Choline (Ach) Synthesis: • At the nerve terminals • CAT (choline acetyl transferase), From Choline • 50% of it, is recaptured by nerve terminals
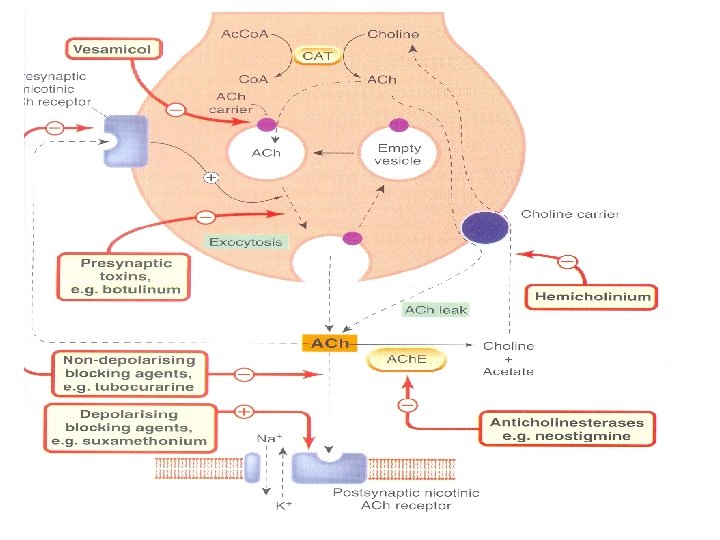

Potential targets for drugs Five key features of neurotransmitter function provide potential targets for pharmacologic therapy: • synthesis, • storage, • release, • termination of action of the transmitter, • functions of the receptor.

Parasympathomimetic

Effects of Muscarinic agonists A. Cardiovascular system • Slow heart rate (negative chronotropy) • Decreases conduction velocity and increases refractory period • Bradycardia and vasodilatation lead to drop in BP • Vasodilatation of arteries and veins due to stimulation of M 3 receptors in the endothelium, releasing NO

Continue… B. RESPIRATORY • Bronchio-spasm • increase secretion C. GIT • Increase peristalsis • Increase secretions mainly salivary and gastric • Sphincters are relaxed

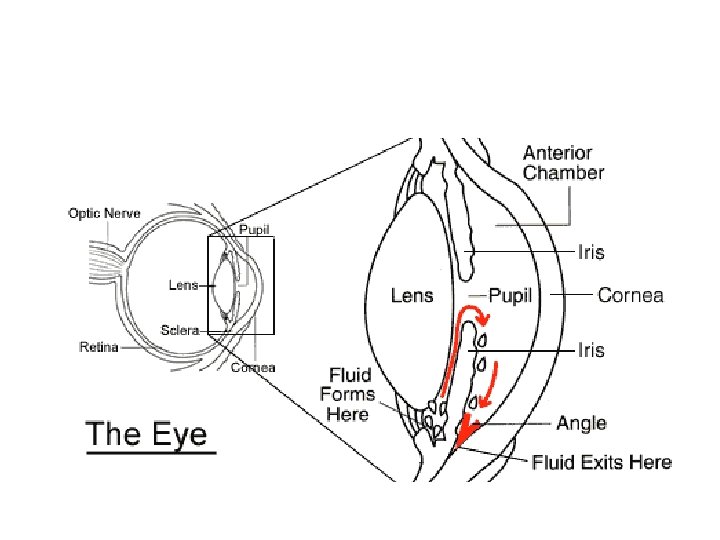
Continue… D. GU • Stimulation of detrusor muscle and Relaxation of the trigone and sphincter of the bladder thus promote micturition. E. Eye • Causes contraction of the smooth muscle of the iris causing miosis and of the ciliary muscle (accommodation of near vision) • It will facilitate the outflow of aqueous humor into the canal of Schlemn which drains the anterior chamber

Continue… F. Exocrine gland • Increased their secretion, sweating, lacrimation and salivation G. CNS • Ach is widely distributed in the brain • It is a excitatory neurotransmitter in the basal ganglia • Its effect include; increased locomotor activity tremor

Nicotinic agonists A. Peripheral nervous system • Activation of nicotinic receptors in the autonomic ganglia result in firing action potential in postganglionic neurons • The action is same on both sympathetic and parasympathetic ganglia

B. NMJ • Application of nicotine agonist in NMJ leads to depolarization of the endplate • The response vary from fasciculation of independent motor units to a strong contraction of entire motor unit.

MUSCARINIC ANTAGONIST • • Atropine Scopolamine Ipratropium Pirenzepine

Pharmacological action Muscarinic antagonist 1 - CNS: • Atropine in therapeutic doses has a minimal stimulant effect on CNS and a slower-long lasting sedative effect on the brain • Scopolamine has more marked CNS effects producing drowsiness in recommended doses • In high doses scopolamine and to a lesser extent atropine causes agitation, excitement, hallucination and coma

2 - eye: • Mydriasis • Cycloplegia leads to loss of accommodation of near vision (eye can not focus on near objects) • Reduction of lacrimal secretion, dry eyes

3 - CVS: • The initial effect is bradycardia followed by tachycardia • The initial bradycardia is often with lower doses and is due to blockade of presynaptic M 1 muscarinic receptors on vagal nerve, thus facilitate Ach release • The tachycardia is due to blockade of M 2 receptors in the SAN • Therapeutic doses of atropine is abolishes peripheral vasodilatation induced by cholinomimetics.

4 - Respiratory system: • Antimuscarinic drugs are added to general anesthetics to reduce secretion in the trachea 5 - GIT • marked reduction in salivary secretion (dry mouth) • Gastric secretion is blocked less effectively.

6 -GU: • Smooth muscle of the uterus is relaxed • Bladder wall is relaxed and voiding is slower 7 - sweat glands • Sweat gland secretions are blocked by antimuscarinic drugs, thermoregulation is suppressed leading to increase in body temperature.

Nicotinic antagonists A) neuromuscular blockers : 1 - depolarizing NMJ blocking drugs; the depolarizing blockers first depolarize the motor end -plate and then prevent further depolarization. E. g. Succinylcholine 2 - non-depolarizing NMJ blocking drugs; compete with acetylcholine for receptors at the neuromuscular junction and clinical relaxation begins when 80– 85% of the receptors on the motor end-plate are blocked. tubocurarine

Ganglion blocking drugs B. Ganglion blocking drugs can occur by several mechanisms: – By interfering with Ach release – By prolonged depolarization due to large dose of stimulation – By interfering with postsynaptic action of Ach.

ADRENERGIC AGONIST & ANTAGONIST

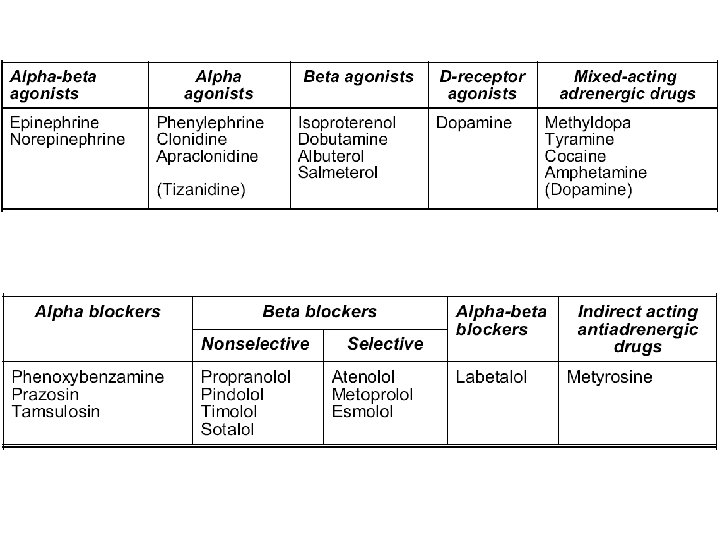
SYMPATHOMIMETICS Classification: A- According to the source: 1. Natural; NE, EP, DA 2. Synthetic; isoproternol, ephedrine, amphetamine B- chemically: 1. Catecholamines; NE, EP, DA and isoproternol 2. Non catecholamines; ephedrine, amphetamine, tyramine

PHARMACOLOGYCAL EFFECTS OF SYMPATHOMIMETIC 1 - Cardiovascular system • The overall effects on blood vessels depend on the relative activities of the sympathomimetics at α or β receptor. • α 1; increase arterial resistance • β 2 receptors promote smooth muscle relaxation • Activity of both normal (SAN) and abnormal (purkinje fibers) is increased (positive chronotropic effects). • Contractility is increased (positive inotropic effects)

2. eye: • Activation by α 1 agonist causes mydriasis • α 1 - agonists increases the outflow of aqueous humor from the eye, while β antagonists decreases the production of the aqueous humor. These effects are beneficial in treatment of glaucoma. 3. Respiratory • Activation of β 2 receptors in the bronchial muscle results in bronchiodilatation.

4. GU • In human uterus the β 2 receptors mediate relaxation that might be useful during pregnancy. • The bladder base, urethral sphincter and prostate contain α receptors that mediate contraction and therefore promote urinary continence. 5. effects on endocrine function • Insulin secretion is stimulated by β receptors and inhibited by α 2 • Renin secretion is stimulated by β 1 and inhibited by α 2

6 - Metabolic effect • Activation of β 3 receptors in fat cells leads to increased lipolysis. • Sympathomimetics enhances glycogenolysis in the liver that leads to increased glucose release into the circulation (mediated mainly by β 2) • Activation of β 2 receptors promotes uptake of potassium into cells, leading to fall in extracellular potassium. . • Carbohydrates metabolism in the muscle and liver is enhanced

α-blocker • Selective α 1 (prazosin): – Vasodilation – Hypotension • Selective α 2 (yohimbine) – Increase nor adrenaline release and cause sympathomimetic effect – Can block α 2 in blood vessel and cause vasodilatation

• α 1 found in the smooth muscle of many organs and they cause contraction of the blood vessels, relaxation of the GIT and glycogenlysis • α 2 found in presynaptic neuron , CNS, blood vessels , it inhibit transmitter release, in addition they cause platelets aggregation and blood vessel contraction • β 1 mainly in the heart , stimulation result in an increase cardiac out put and heart rate • β 2 present in the smooth muscle of many organs and its stimulation lead to bronchodilation, perpherial vasodilation, relaxation of the visceral smooth muscle and skeletal muscle tremor

• Non selective α-blockers – Phenoxybenzamine, phentolamine – Vasodilatation – Reduce blood pressure

β-blocker • Non selective: – Propranolol, labetalol • Selective – Atenolol, metoprolol – Reduce HR (-ve chronotropic) – Reduce force of heart contraction (-ve ionotropic)
- Slides: 40