Introduction Habitat Morphology Life cycle Pathogenesis Clinical diseases


• Introduction • Habitat • Morphology • Life cycle • Pathogenesis • Clinical diseases • Lab diagnosis • Treatment Topics

Introduction: E. granulosus tapeworm formally called “Tenia echinococcus”, causes hydatid disease or echinococcosis. History: Hydatid cyst is recognised since the time of Hippocrates. ü Adult worm was discovered by Hartmann in 1965, Goez described larva in 1782.
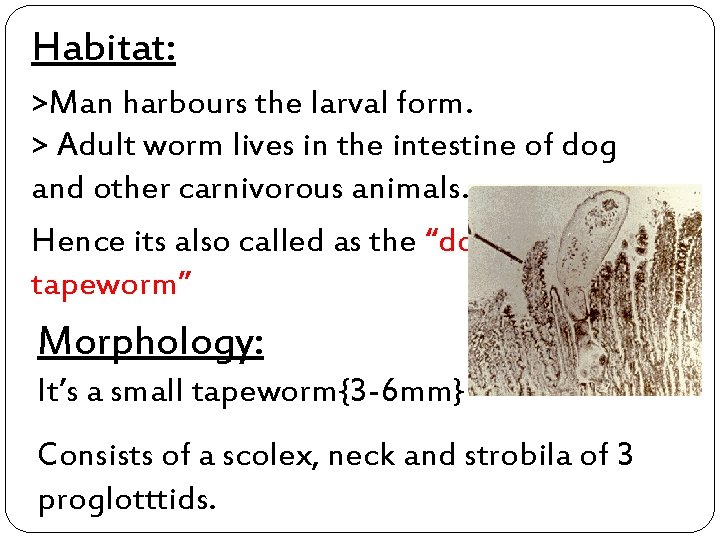
Habitat: >Man harbours the larval form. > Adult worm lives in the intestine of dog and other carnivorous animals. Hence its also called as the “dog tapeworm” Morphology: It’s a small tapeworm{3 -6 mm} Consists of a scolex, neck and strobila of 3 proglotttids.
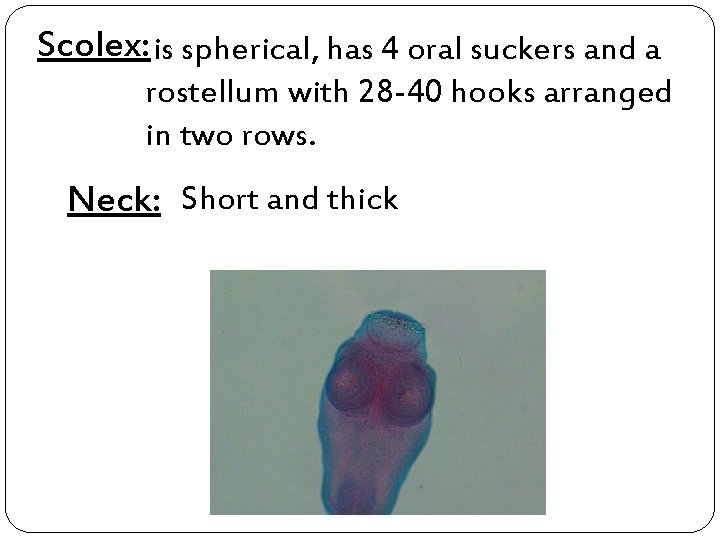
Scolex: is spherical, has 4 oral suckers and a rostellum with 28 -40 hooks arranged in two rows. Neck: Short and thick
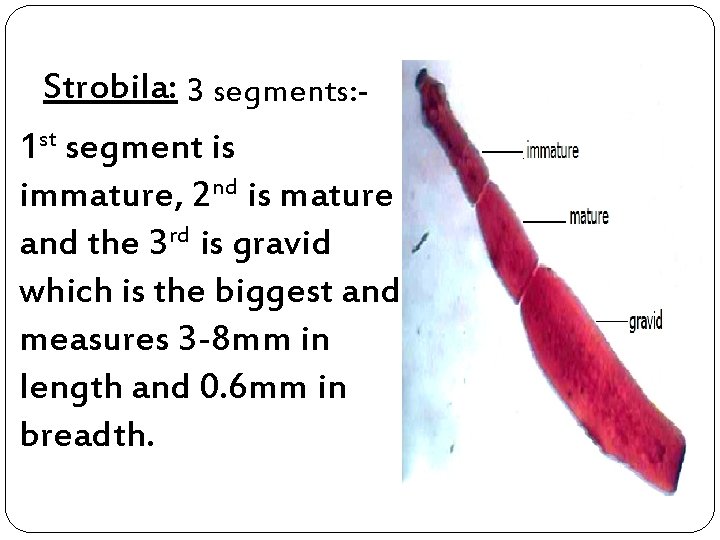
Strobila: 3 segments: 1 st segment is immature, 2 nd is mature and the 3 rd is gravid which is the biggest and measures 3 -8 mm in length and 0. 6 mm in breadth.

Egg: Morphologically similar to Taenia > Ovoid, 32 to 36 um long and 25 -32 um >wide. Has 2 layers, an outer shell surrounding the inner embryophore. Fully developed egg has 3 pairs of hooklets within the embryophore. Eggs are excreted in the faeces of canine animals [dog, fox, jackal]
![Larval form: Embryos develop into cyst [hydatid] in the intermediate host, which contain many Larval form: Embryos develop into cyst [hydatid] in the intermediate host, which contain many](http://slidetodoc.com/presentation_image_h/0238c1f79421507cfae222c037679569/image-8.jpg)
Larval form: Embryos develop into cyst [hydatid] in the intermediate host, which contain many brood capsules and small protoscolices. Protoscolex contains a scolex which represents future head of worm, remains invaginated within vesicular body. After entering into definitive host, scolex evaginates, attaches to mucosa with rostellar hooklets and develops into an adult worm.
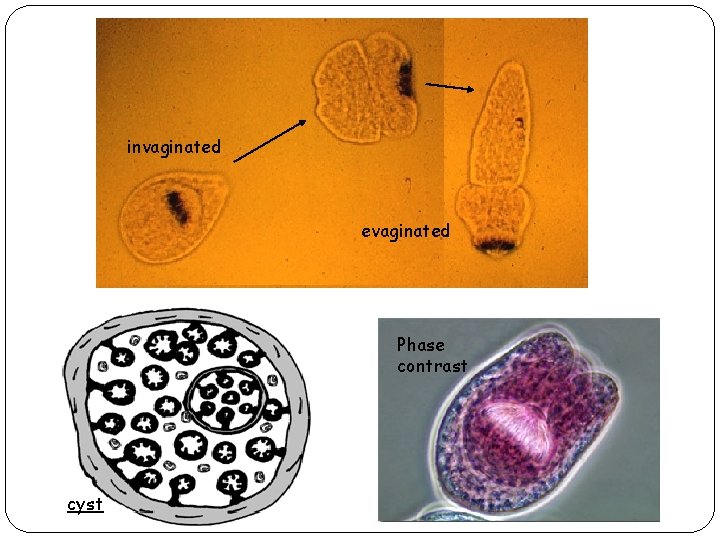
invaginated evaginated Phase contrast cyst
![Epidemiology: 1. Host: dogs are definitive hosts and herbivores [man, cattle, sheep] are intermediate Epidemiology: 1. Host: dogs are definitive hosts and herbivores [man, cattle, sheep] are intermediate](http://slidetodoc.com/presentation_image_h/0238c1f79421507cfae222c037679569/image-10.jpg)
Epidemiology: 1. Host: dogs are definitive hosts and herbivores [man, cattle, sheep] are intermediate hosts. Tranismission: definitive host get infected by eating contaminated meat. Humans get infected by ingestion of eggs passed in dog faeces. 3. Distribution: Latin america, Arab, North Africa, Middle east and South east asia. Andra Pradesh and Tamil Nadu in India. 2.


Pathogenecity: 1. In dogs: no disease 2. In humans: hydatid cyst or disease, grows slowly and several years[5 -20 yrs]. 10% of cases terminate fatally. • most cysts occur in liver[70%] and lungs[20%] • cysts in other sites[10%] include: Spleen[3 -4%] brain[3%] bones[1%] Pelvic organs[2%] -3%] head and muscles[1
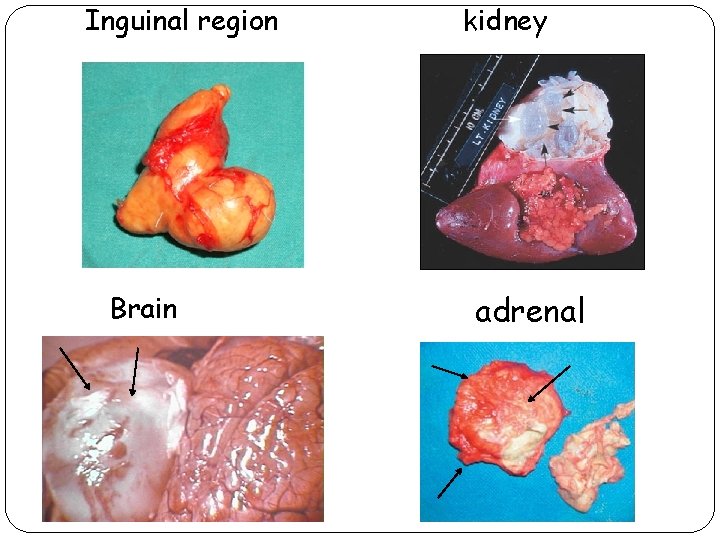
Inguinal region Brain kidney adrenal

Evolution of hydatid cyst: the wall of cyst consists of 3 layers, 2 inner layers are secreted from embryo and outer layer is produced by host. 1. Germinal layer [endocyst]: Innermost vital thin layer, consisting of a number of nuclei embedded in protoplasmic mass. Functions: • formation of outer laminated layer • production of brood capsule with protoscolices
![2. Laminated layer [ectocyst]: Cuticle layer, laminated hyaline membrane. Derived from parasite and composed 2. Laminated layer [ectocyst]: Cuticle layer, laminated hyaline membrane. Derived from parasite and composed](http://slidetodoc.com/presentation_image_h/0238c1f79421507cfae222c037679569/image-15.jpg)
2. Laminated layer [ectocyst]: Cuticle layer, laminated hyaline membrane. Derived from parasite and composed of mucopolysaccharide material which is tough, elastic[1 mm thick]. Looks like white of “hard boiled egg”. 3. Adventitial layer [pericyst]: Fibrous layer that results from cellular reaction with host. May become calcified or sclerosed.

Development of brood capsules: small knob-like excrences protude into the lumen of the. cyst from germinal layer Excrescencs enlarge , become vacuolated & filled with fluid to form “ Brood capsule” Protoscolices arise from inner layer of brood capsule Brood capsule detaches from germinal layer, escapes free into the fluid filled cyst cavity.

Mature cyst contains about 1 million protoscolices & v may detach from germinal membrane and float free in the cyst together with the brood capsule to form the “hydatid Thesand” cyst may further form “daughter and grand daughter cysts”, Or may rupture into tissues or circulation, the spilled protoscolices may produce “secondary cysts”.
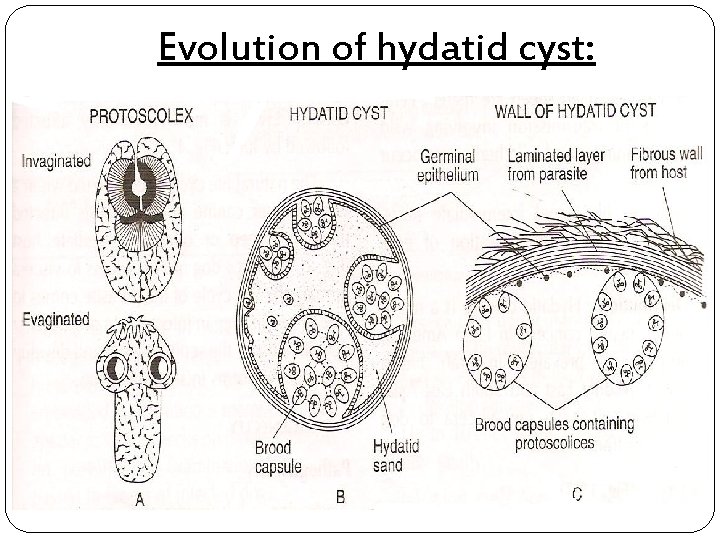
Evolution of hydatid cyst:

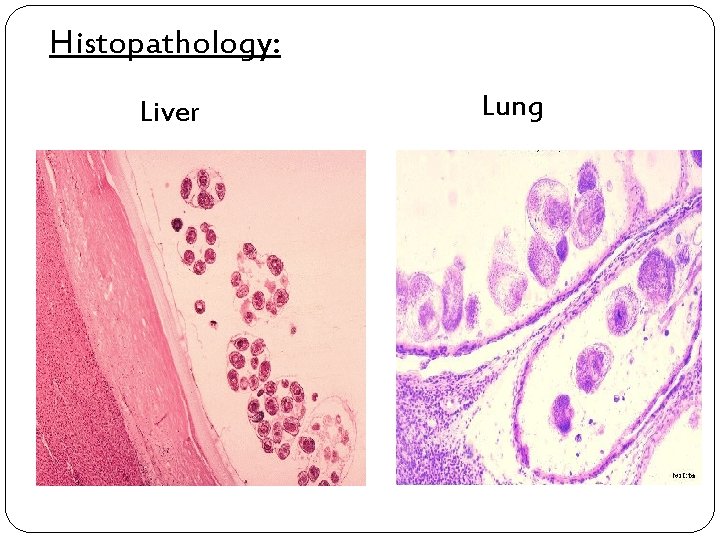
Histopathology: Liver Lung

Hydatid fluid: secreted by germinal layer of cyst • colour: clear colourless or pale yellow • specific gravity: low varies from 1. 005 -1. 010. • reaction: slightly acidic, p. H 6. 7 • chemical composition: Na. Cl, sodium sulphate, sodium phosphate, sodium and calcium salts of succinic acid. • antigenicity: antigenic, used for immunological tests. • toxicity: highly toxic, when comes out causes

Fate of hydatid cyst: 1. spontaneous recovery in some patients. Scolies die and fluid is gradully absorbed. 2. cyst may get calcified following injury to its wall 3. spontaneous evacuation of cyst may occur following inflammation reaction 4. cyst of liver may rupture into pleural cavity or lungs producing disseminated hydatid lesions. 5. may rupture to body cavity leading to disseminated and widespread growth of hdatid

Clinical syndromes: Cyst grows slowly to 4 cm diameter at end of 1 st year, brood capsules and scolices begin to appear. Most remain symptomless for many years. 1. Hepatic liver cyst: hepatic enlargement, more frequent in right lobe of liver. Rupture of cyst may lead to severe symptoms and allergic manifestations. 2. Lungs cysts: cough dysponea and chest pain, rupture can cause haemomptysis, pneumonia pneumothorax. 3. In vital organs[ spleen, heart, brain] or bones, fatal!
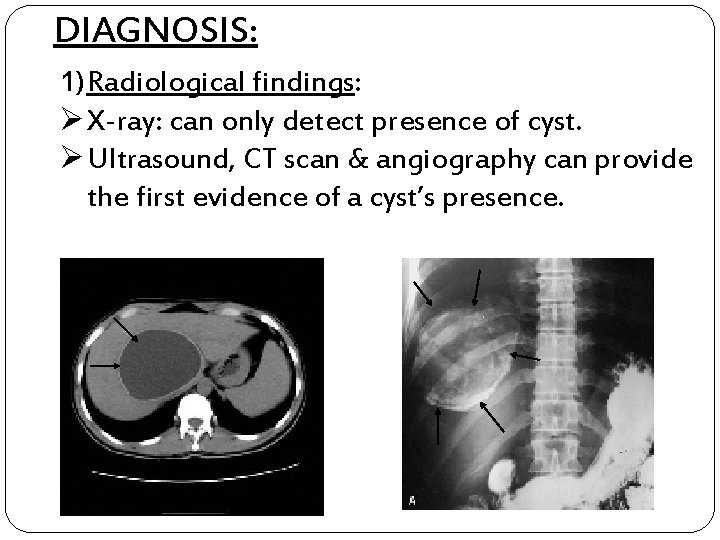
DIAGNOSIS: 1) Radiological findings: Ø X-ray: can only detect presence of cyst. Ø Ultrasound, CT scan & angiography can provide the first evidence of a cyst’s presence.

2) Exploratory cyst puncture: aspiration of cyst contents may reveal the presence of protoscolices [hydatid sand]. Ø contraindicated due to accidental spilling of contents 3) Serologic tests: Antibody detection: ELISA, indirect immunoflorescence test, latex agglutination, IHA. Antigen detection: double diffusion and counter immunoelectrophoresis technique.
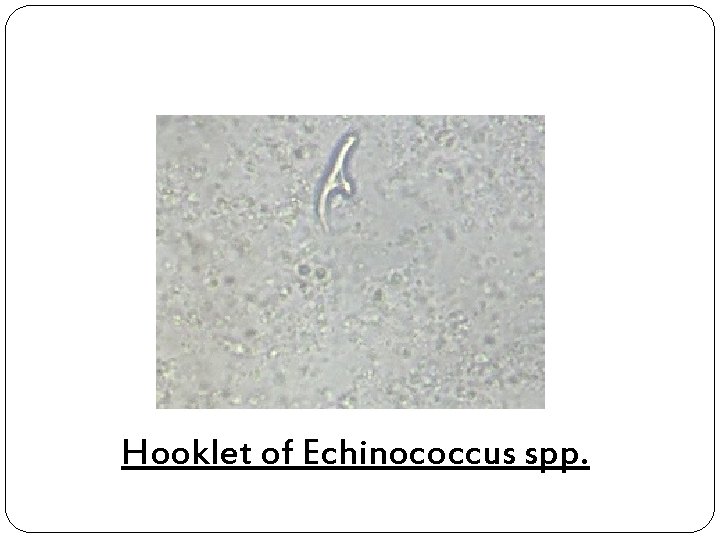
Hooklet of Echinococcus spp.
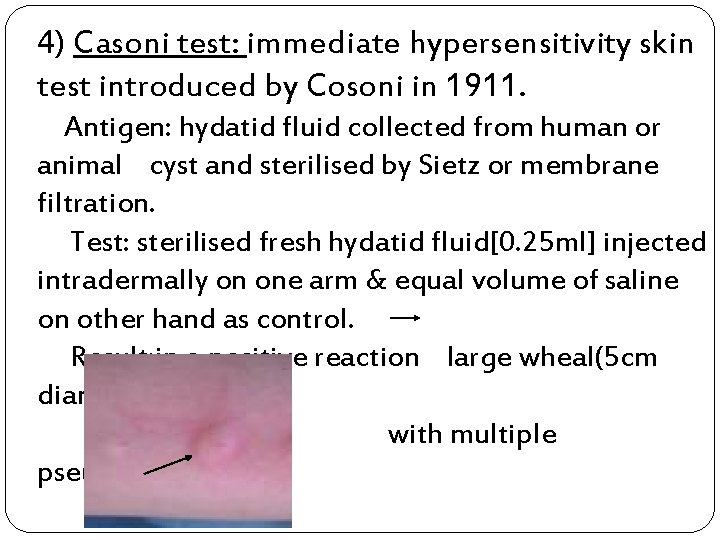
4) Casoni test: immediate hypersensitivity skin test introduced by Cosoni in 1911. Antigen: hydatid fluid collected from human or animal cyst and sterilised by Sietz or membrane filtration. Test: sterilised fresh hydatid fluid[0. 25 ml] injected intradermally on one arm & equal volume of saline on other hand as control. Result: in a positive reaction large wheal(5 cm diameter) with multiple pseudopodia

Remarks: i) False positive and false negative cases may occur. Nonspecificity being the major limitation. ii) Diagnostic sensitivity is limited in patients having intact or hyaline cysts. iii) The antigen may sensitize the patient leading to production of antibody and anaphylactic reaction. > therefore rarely used these days for diagnosis.

TREATMENT SURGERY CHEMOTHERAPY CYST PUNCTURE PAIR

Prevention: i) Education: regarding transmission of infection and role of canines in life cycle. ii) personal hygiene: washing of hands and utensils in areas inhabited by dogs iii) Dogs should not be fed viscera of slain animals


TOPICS CLASSIFICATION EPIDEMIOLOGY TRANSMISSION MORPHOLOGY LIFE CYCLE MODES OF INFECTION CLINICAL SYNDROMES DIAGNOSIS TREATMENT PREVENTION MCQ’S
CLASSIFICATION Kingdom: Animalia Phylum: Platyhelminthes Class: Cestoda Order: Cyclophyllidea Family: Hymenolepididae Genus: Hymenolepis Species: Hymenolepis nana

EPIDEMIOLOGY DISTRIBUTION: Worldwide Infection more in warmer climates S. AMERICA & AFRICA Crowded areas, such as India and China More common in children than in adults.

TRANSMISSION : Ingestion of eggs from contaminated hands. Ingestion of infected rat fleas , beetles as they contain cysticercoid in their haemocele.

MORPHPLOGY ADULT WORM: Small thread like worm. 1 -4 cm long; max. 1 mm width. Often found in large numbers(1000 to 8000) Life span is 4 – 6 weeks. Dwarf tape worm
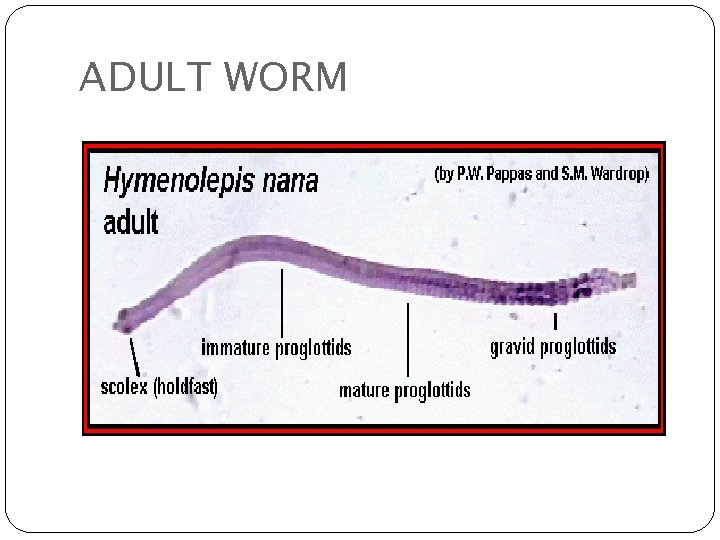
ADULT WORM

SCOLEX Ø Shows a knob like rostellum Ø Bears a ring of hooklets. Ø They possess 4 suckers.
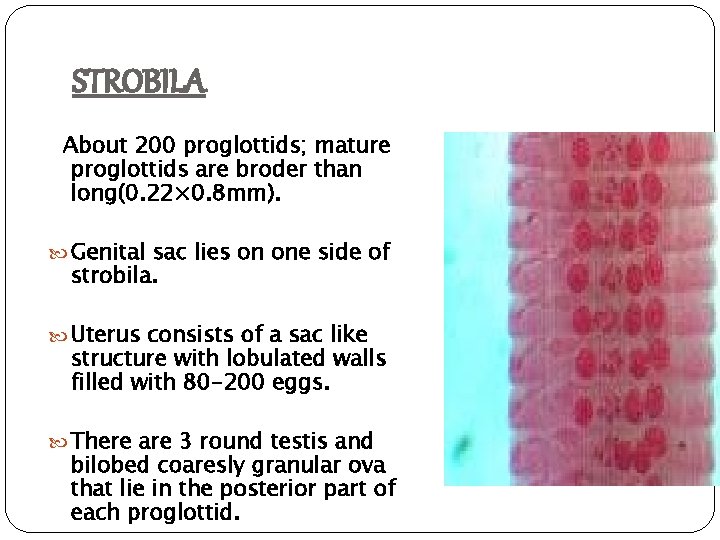
STROBILA About 200 proglottids; mature proglottids are broder than long(0. 22× 0. 8 mm). Genital sac lies on one side of strobila. Uterus consists of a sac like structure with lobulated walls filled with 80 -200 eggs. There are 3 round testis and bilobed coaresly granular ova that lie in the posterior part of each proglottid.

EGGS Colorless, oval or sub spherical 45*35 mm. Egg , has two membranes : a. outer thin and colorless. b. inner embryophore. q Space b/w them has –. yolk granules. polar filaments. q Oncosphere 3 pairs of hooklets q Egg floats in salt solution



MODES OF INFECTION H. nana has 3 modes of infection: (1) Indirect 2 -host cycle involving rodents as primary definitive hosts and grain beetles, fleas, or other insects that feed on contaminated rodent droppings as intermediate hosts. (2) Oral-anal cycle in which eggs are passed from one human to another or recycle externally in a single host.

3) INTERNAL AUTOINFECTION: Eggs hatch within the gut and initiate a 2 nd generation without ever exiting the host. This results in massive numbers of worms nausea vomiting diarrhea abdominal pain weight loss and nonspecific systemic symptoms.

CLINICAL SYNDROMES Ø Ø Ø Asymptomatic H. nana causes HYMENOLEPIASIS/ HYMENOLIPIDOSIS. Heavy infections : abdominal discomfort diarrhoea anorexia pruritis Hyper infection : autoinfection in immuno compromised pts. With heavy worm burden

DIAGNOSIS v Adult worm or proglottids are rarely seen in stools. v Demonstration of typical eggs with 6 hooked embryo & polar filaments.
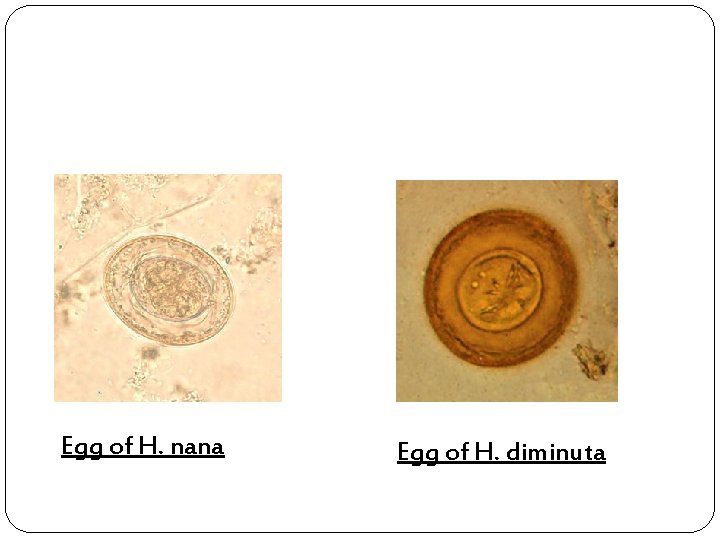
Egg of H. nana Egg of H. diminuta

TREATMENT DRUG OF CHOICE : PRAZIQUANTEL single dose of 25 mg/kg. body weight. ALTERNATIVE : Niclosamide Nitazoxanide

PREVENTION & CONTROL Improved sanitation & proper Personal hygeine. Control of arthropod vectors disposal.

- Slides: 50