INTRODUCING DEPRESCRIBING TO SINGAPORE Brought to you by

INTRODUCING DEPRESCRIBING TO SINGAPORE Brought to you by Pharmaceutical Society of Singapore (PSS) as part of Pharmacy Week 2015 Supported by: • Society of Geriatric Medicine, Singapore • Singapore Nurses Association • Association of Diabetes Educators (Singapore) 1

What is Polypharmacy? �Traditionally defined by the number of drugs a patient is taking ◦ No consensus on how many drugs constitutes polypharmacy ◦ Varies from ≥ 2 drugs, all the way up to ≥ 10 drugs �Defined as taking at least one drug that is not clinically indicated Clin Geriatr Med 2012; 28: 173 -86 Copyright of PSS 2

Prevalence of Polypharmacy in Singapore � At least half of all discharged patients from a Singapore restructured hospital had > 5 chronic medications; 27. 7% were discharged with > 8 chronic medications. 1 � Among 454 geriatric nursing home residents, more than half were on > 5 medications, and inappropriate medication use was seen in 70% of the residents. 2 1. In-hospital data for discharges (Jan 2013 – Dec 2014), a Singapore restructured hospital. 2. Ann Acad Med Singapore. 2004 Jan: 33(1): 49 -52. Copyright of PSS 3

Causes of Polypharmacy �Disease-specific clinical practice guidelines 1 ◦ Targets are disease-specific, not holistic enough ◦ Patients with multiple co-morbidities can end up on many drugs and complicated regimen �Focus on pharmacologic treatment options when lifestyle modifications can suffice 2 �“Prescribing cascade” 3 ◦ Drugs are added to treat unrecognised side effects of other drugs J Am Geriatrics Soc 2011; 59: 376 -7 1. 2. Clin Geriatr Med 2012; 28: 173 -86 � 3. Expert Opin Drug Saf 2007; 6: 695 -704 Patient or caregiver expectation Copyright of PSS 4

Consequences of Polypharmacy �Increased risk of adverse drug events �Increased non-compliance due to complex drug regimen �Increased pill burden �Increased unnecessary expenditure �Increased risk of drug-drug interactions �Increased hospitalizations �Increased risk of falls and fractures in the elderly Clin Geriatr Med 2012; 28: 173 -86 Copyright of PSS 5

“Success” case study - LYL, Female 71 years old PMHx: HTN, DM, HLD, depression and cervical spondylosis. Before: (Taking BD instead) 1) Gabapentin 300 mg TDS 2) Insulin Aspart Flex Pen 14 units BD 3) Metformin 850 mg TDS 4) Atenolol 50 mg OM 5) Amlodipine 10 mg OM (Disturbing Cough) 6) Enalapril 10 mg BD 7) Aspirin 100 mg OM (Taking 20 mg BD) 8) Omeprazole 40 mg BD 9) Simvastatin 20 mg ON 10) Calcium Vit D 1 OM 11) Glargine 56 units ON 12) Diclofenac 50 mg TDS PRN Y N A M 13) Neuroforte 1 OM TOO TAKIN ! S E N I C I D E M Y L G N O R W G Copyright of PSS 6

“Success” case study After: 1) Gabapentin 300 mg TDS 2) Insulin Aspart Flex Pen 14 units BD 3) Metformin 850 mg TDS 4) Atenolol 50 mg OM 5) Amlodipine 10 mg OM 6) Irbesartan 150 mg BD 7) Aspirin 100 mg OM 8) Simvastatin 20 mg ON 9) Glargine 56 Units ON & T N A I L P M O C E R R E I MO P P A H S FEEL Copyright of PSS 7

What can we do to reduce polypharmacy and its adverse patient outcomes? Copyright of PSS 8

Concept of Deprescribing Systematic process of identifying and discontinuing drugs in instances in which existing or potential harms outweigh existing or potential benefits within the context of an individual patient’s care goals, current level of functioning, life expectancy, values, and preferences. Part of the prescribing continuum JAMA Intern Med 2015; 175: 827 -34 Copyright of PSS 9
Deprescribing…. . Patient-centred Associated with inherent uncertainties Is Shared decision-making Informed patient consent It is NOT denying effective treatment to eligible patients Close monitoring of effects Considers cumulative risk from multiple drugs Copyright of PSS 10

Benefits of Deprescribing �Reduced risk of adverse drug events �Improved compliance �Reduced risk of drug-drug interactions �Improved quality of life and sense of well-being JAMA Intern Med 2015; 175: 827 -34 Copyright of PSS 11

Barriers to deprescribing �Time limitations �Patient refusal to stop medications �Fear of worsening conditions or concern about withdrawal effects from drug cessation �Poorly communicated or fragmented care among multiple specialists �Disagreement between healthcare professionals on which medication should be discontinued Drugs and Aging 2013; 30(10): 793 -807. Copyright of PSS 12
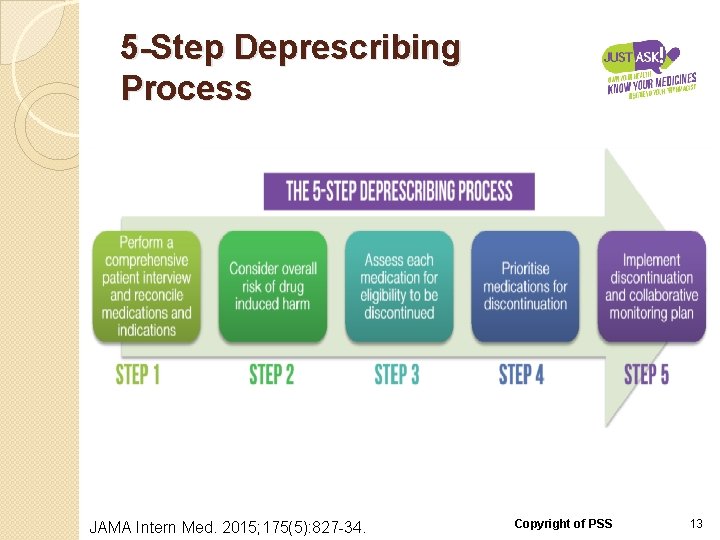
5 -Step Deprescribing Process JAMA Intern Med. 2015; 175(5): 827 -34. Copyright of PSS 13

5 -Step Deprescribing Process Step 1: Perform a comprehensive medication-indication reconciliation �Include prescription and nonprescription drugs �Document indication for each drug �Identify ADRs and non-compliance JAMA Intern Med. 2015; 175(5): 827 -34. Med J Aust. 2014; 201(7): 386 -9. Copyright of PSS 14

5 -Step Deprescribing Process Step 2: Consider overall risk of druginduced harm �Drug factors ◦ Number of drugs ◦ History of toxicity/ADRs ◦ Use tools e. g. . BEERS list, STOPP criteria �Patient factors ◦ Age ◦ Multiple comorbidities ◦ Multiple prescribers JAMA Intern Med. 2015; 175(5): 827 -34. Med J Aust. 2014; 201(7): 386 -9. Copyright of PSS 15

5 -Step Deprescribing Process Step 3: Assess each medication for eligibility to be discontinued �Jointly consider life expectancy and treatment goals �Identify medications used for ◦ Unconfirmed diagnosis ◦ Confirmed diagnosis but no evidence for choice of treatment ◦ Counteracting ADR of other medications JAMA Intern Med. 2015; 175(5): 827 -34. Med J Aust. 2014; 201(7): 386 -9. Copyright of PSS 16

5 -Step Deprescribing Process Step 4: Prioritise medications for discontinuation �Discontinue medication with greatest harm and least benefit first �Taper dose of medications that cause withdrawal �Ensure patient/caregiver is comfortable with decision �Discontinue one at a time JAMA Intern Med. 2015; 175(5): 827 -34. Med J Aust. 2014; 201(7): 386 -9. Copyright of PSS 17

5 -Step Deprescribing Process Step 5: Implement drug discontinuation plan and monitor adverse withdrawal effects �Monitor for adverse withdrawal reactions or return of symptoms �Counsel patient/caregiver on steps to take �Implement non-pharmacological measures �Document process and outcome, communicate to other healthcare providers JAMA Intern Med. 2015; 175(5): 827 -34. Med J Aust. 2014; 201(7): 386 -9. Copyright of PSS 18

Deprescribing in Action �Projects ongoing in Australia and Canada to develop deprescribing guidelines ◦ E. g. , PPI’s, benzodiazepines �Singapore – start with proton pump inhibitors (PPI’s) Copyright of PSS 19
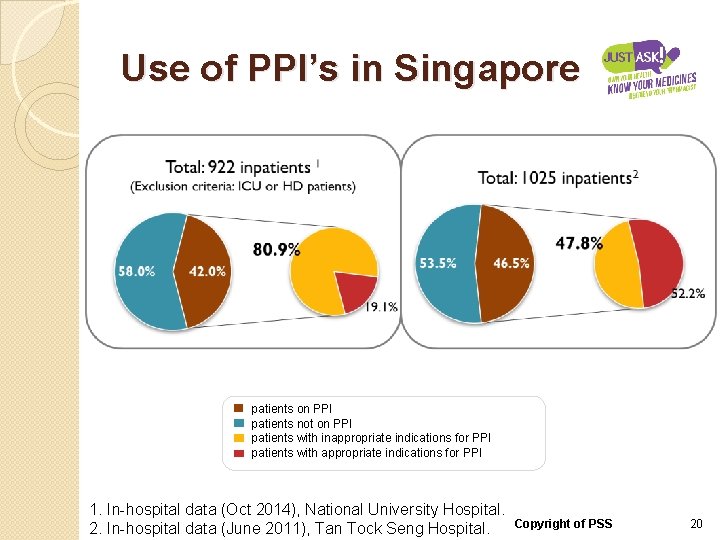
Use of PPI’s in Singapore patients on PPI patients not on PPI patients with inappropriate indications for PPI patients with appropriate indications for PPI 1. In-hospital data (Oct 2014), National University Hospital. 2. In-hospital data (June 2011), Tan Tock Seng Hospital. Copyright of PSS 20

Use of PPI’s in Singapore �Criteria used for inappropriate indications of PPIs: ◦ Prophylaxis of gastrointestinal bleeding in LOW risk patients using antiplatelets, anticoagulants, steroids and NSAIDs (non-selective and COX-2 selective) ◦ Anaemia ◦ Lower GI bleed ◦ Malignancy 1. In-hospital data (Oct 2014), National University Hospital. 2. In-hospital data (June 2011), Tan Tock Seng Hospital. Copyright of PSS 21
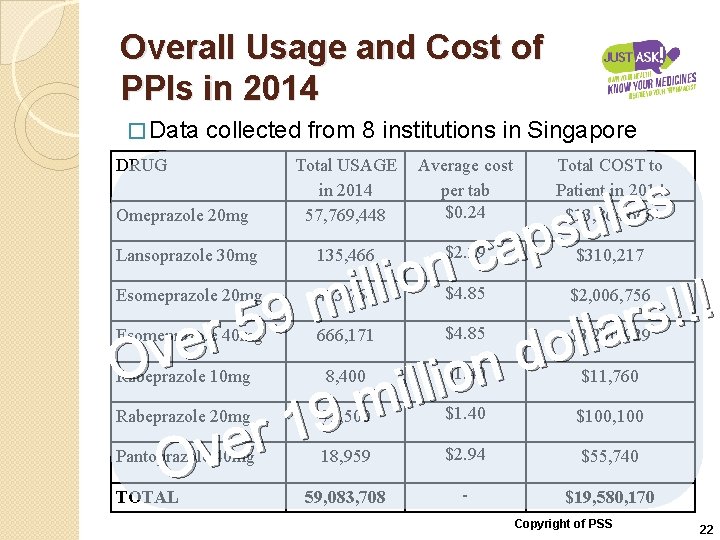
Overall Usage and Cost of PPIs in 2014 � Data collected from 8 institutions in Singapore DRUG Omeprazole 20 mg Total USAGE in 2014 57, 769, 448 Average cost per tab $0. 24 Total COST to Patient in 2014 $13, 864, 668 Lansoprazole 30 mg 135, 466 $2. 29 $310, 217 Esomeprazole 20 mg 413, 764 $4. 85 $2, 006, 756 Esomeprazole 40 mg 666, 171 $4. 85 $3, 230, 929 Rabeprazole 10 mg 8, 400 $1. 40 $11, 760 Rabeprazole 20 mg 71, 500 $1. 40 $100, 100 Pantoprazole 40 mg 18, 959 $2. 94 $55, 740 59, 083, 708 - $19, 580, 170 s e l u s p a c n o i l l i ! m ! ! s 9 r 5 a l r l e o v d O n o i l l i m 9 1 r e v O TOTAL Copyright of PSS 22

Appropriate Indications of PPI’s �Gastro-esophageal reflux disease (GERD) �Peptic ulcer disease �Helicobacter pylori eradication �Zollinger-Ellison Syndrome �Uninvestigated dyspepsia PPI approved indications. http: //www. cms. gov/Medicare. Medicaid-Coordination/Fraud-Prevention/Medicaid. Integrity-Education/Pharmacy-Education. Materials/Downloads/ppi-adult-dosingchart. pdf. Accessed August 15, 2015. Copyright of PSS 23

Appropriate Indications of PPI’s �Prevention of NSAID-induced ulcers in patients with risk factors 1 ◦ Age > 65 years ◦ History of PUD or GI bleed ◦ Concurrent use of low dose aspirin, antiplatelets, anticoagulants or steroids �Patients on dual antiplatelet therapy with risk factors 2 ◦ ◦ History of PUD or GI bleed Age > 75 years Concurrent use of anticoagulants or steroids H. pylori infection 1. Am J Gastroenterol 2009; 104(3): 728 -38. 2. Am J Gastroenterol 2010; 105(12): 2533 -49. Copyright of PSS 24

Common Inappropriate Uses of PPI’s �Dual Anti-platelet Therapy (DAPT) ◦ GI events occurred despite prophylaxis in patients with aspirin + clopidogrel 1 ◦ 57/250 (22. 8%) received GI prophylaxis when not indicated. ◦ PPI-related adverse events accounted for 6/22 (18. 0%) of readmissions. �Patients without risk factors for GI bleeding receive little if any absolute risk reduction from a PPI 2 1. J Manag Care Pharm. 2014 Feb; 20(2): 187 -93. 2. Am J Gastroenterol. 2010 Dec; 105(12): 2533 -49. Copyright of PSS 25

Common Inappropriate Uses of PPI’s � NSAIDs ◦ Patients with high GI risk (e. g. history of previously complicated ulcer or > 2 GI risk factors) should avoid NSAIDs 1 (1 B) ◦ Patients with low GI risk should not be given PPI for GI prophylaxis with NSAIDs 1 (1 A) ◦ No randomized, prospective, controlled outcome trials till date have evaluated efficacy of PPIs in preventing the occurrence of complications (e. g. . , bleeding, perforation, obstruction, death) resulting from NSAIDs-induced ulcers 1 ◦ (NSAIDs + PPI) vs COX-2 inhibitors alone demonstrated similar rates of symptomatic ulcer recurrence in high risk patients. 2 1. Am J Gastroenterol 2009; 104: 728– 738; 2. Scheiman Arthritis Research & Therapy 2013, 15(Suppl 3): S 5. Copyright of PSS 26

Recommendations for prevention of NSAID-related ulcer complications 2 1. Table adapted from : Am J Gastroenterol 2009; 104: 728 – 738 2. Lancet. 2007 May 12; 369(9573): 1621 -6 Copyright of PSS 27

Common Inappropriate Uses of PPI’s �COX-2 inhibitors ◦ No strong evidence for routine prescription for COX 2 Inhibitors + PPI ◦ Only ONE study conducted in high risk patients concluded PPI should be prescribed 1: �Single-centre, prospective, randomized double blind trial over 13 months (n=441) �Celecoxib 200 mg BD + Esomeprazole 20 mg BD was more effective than Celecoxib alone for the prevention of ulcer bleeding in patients with arthritis and history of GI bleed. �Cumulative incidence of recurrent GI bleed was 0% in the combined-treatment group and 12 (8. 9%) in the controls (95% CI difference, 4. 1 to 13. 7; p=0. 0004) 1. Lancet. 2007 May 12; 369(9573): 1621 -6 Copyright of PSS 28

Common Inappropriate Uses of PPI’s �Corticosteroids ◦ Routine prophylaxis with short term steroids is not indicated. ◦ Incidence of peptic ulcer is rare (0. 4 - 1. 8%)1 ◦ Large prospective trials to determine the most efficacious prophylactic regimen (e. g. , H 2 RAs, PPIs or misoprostol) for corticosteroidinduced ulcerations are not available. 2 ◦ PPIs can be considered when NSAIDs and systemic corticosteriods are used concomitantly (increased risk of ulcers and a poorer recovery from these complications). 1 1. Ned Tijdschr Geneeskd. 2013; 157(19): A 5540. (Only Abstract in English) 2. Ann Pharmacother 1996 Jul-Aug; 30(7 -8): 870 -2 Copyright of PSS 29

Adverse Effects of Long Term PPI Use 1. Clostridium difficile infection ◦ US FDA safety alert 2012: 1. 4 to 2. 75 times higher risk of C. difficile diarrhoea 1 ◦ Meta-analysis including 313, 000 patients 2 �Increased risk of incident C. difficile infection (odds ratio [OR] 1. 7; 95% CI 1. 5 -2. 9 ) �Increased risk of recurrent C. difficile infection (odds ratio [OR] 2. 5; 95% CI 1. 2 -5. 4) 1. http: //www. fda. gov/Drugs/Drug. Safety/ucm 290510. htm [accessed June 13, 2015] 2. Am J Gastroenterol. 2012; 107(7): 1011. Copyright of PSS 30

Adverse Effects of Long Term PPI Use 2. Community acquired pneumonia ◦ Meta-analysis: use of PPI increased risk of pneumonia (adjusted OR 1. 27, 95% CI 1. 111. 46) � Higher doses of PPI more strongly associated with pneumonia (adjusted OR 1. 52 vs 1. 37) CMAJ. 2011 Feb 22; 183(3): 310 -9. Copyright of PSS 31

Adverse Effects of Long Term PPI Use 3. Fractures ◦ Meta-analysis �Increased risk of any fracture (adjusted OR 1. 30, 95% CI 1. 15 -1. 48) and hip fracture (adjusted OR 1. 34, 95% CI 1. 09 -1. 66) with PPI use for longer than a year �Increased risk of hip fracture for both high dose (adjusted OR 1. 53, 95% CI 1. 18 -1. 97) and usual dose PPI (adjusted OR 1. 42, 95% CI 1. 31 -1. 53) Ann Fam Med. 2011 May-Jun; 9(3): 257 -67 Copyright of PSS 32

Adverse Effects of Long Term PPI Use 4. Hypomagnesemia ◦ US FDA safety alert 20111: �Hypomagnesemia reported in patients taking PPIs after a year ~25% of these cases required Mg supplementation and discontinuation of PPI ◦ Cross-sectional analysis 2: �Significant association between PPI use and hypomagnesemia risk after multivariable regression analyses 1. http: //www. fda. gov/Drugs/Drug. Safety/ucm 245011. htm [accessed 13 th June 2015] 2. Int J Clin Pract. 2014 Nov; 68(11): 1352 -7 Copyright of PSS 33

Conclusions � Polypharmacy is prevalent amongst patients on chronic medications and this can potentially lead to avoidable adverse drug events and readmissions � Systematic deprescribing can alleviate polypharmacy through tapering with a plan to take off eligible medications. It can also involve optimising necessary medications in order to take off some others. � Deprescribing is part of the prescribing continuum and it involves compiling, evaluating, assessing, prioritising and monitoring � A drug class of great deprescribing potential is the proton pump inhibitors, and evidence was presented for its removal from a patient’s drug list where warranted. � Doctors, pharmacists and nurse educators are enablers to promote medication safety and well-being of patients with chronic conditions. Copyright of PSS 34

Thank You! Pharmacy Week 2015 IPE Committee: � Grant Sklar, NUS � Soong Jie Lin, SGH � Chuang Shen Hui, TTSH � Kelvin Xu, KKH � Loke Ek Theng, Mt. Alvernia � Chee Enqing, SGH � Dennis Chua, NTFGH � Veronica Teo, NTFGH � Koh Tsing Yi, NUH Chairperson: Doreen Tan, KTPH Copyright of PSS 35
- Slides: 35