Introduce the Topic Pilon Fracture Fixation Joseph Borrelli

Introduce the Topic Pilon Fracture Fixation: Joseph Borrelli, Jr. MD Professor and Chair Department of Orthopaedic Surgery University of Texas – Southwestern Medical Center Dallas, TX

Objectives: 1 - Briefly review radiographic and clinical findings of high energy pilon fractures, 2 - Describe the ‘Two-Stage Approach’ for the treatment of high energy pilon fractures, 3 - Review surgical options and approaches for these fractures,
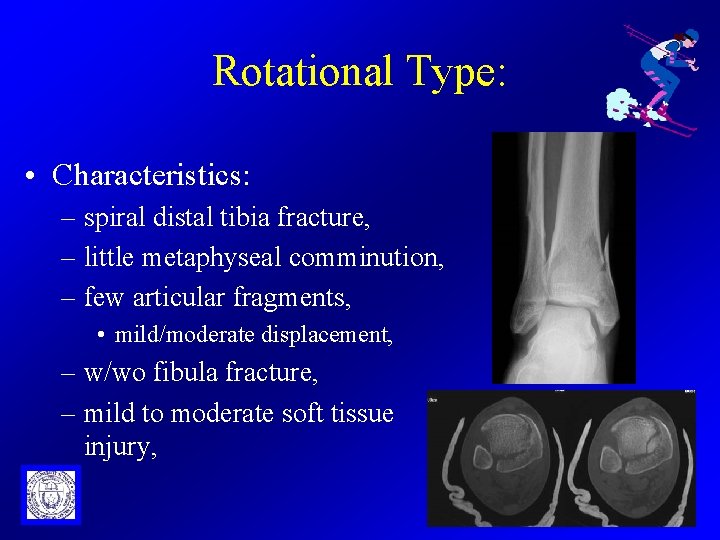
Rotational Type: • Characteristics: – spiral distal tibia fracture, – little metaphyseal comminution, – few articular fragments, • mild/moderate displacement, – w/wo fibula fracture, – mild to moderate soft tissue injury,

Axial Compression Type: • Characteristics – articular impaction, – metaphyseal and articular comminution, • moderate to major displacement, – severe soft tissue injury/open – associated with fibula fracture (85%),

Recognize the Difference ! • Timing of treatment, – earlier vs delayed, • Type of treatment, – approach, – ORIF vs limited IF and EF, • Complications, • Outcome,
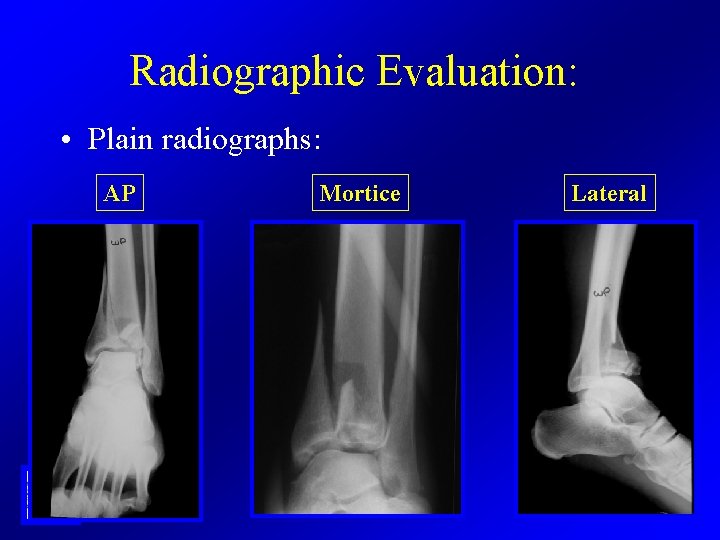
Radiographic Evaluation: • Plain radiographs: AP Mortice Lateral
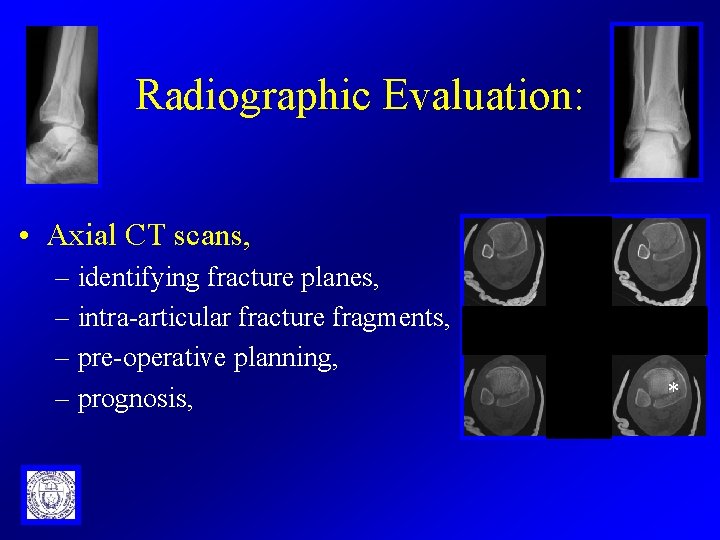
Radiographic Evaluation: • Axial CT scans, – identifying fracture planes, – intra-articular fracture fragments, – pre-operative planning, – prognosis, *
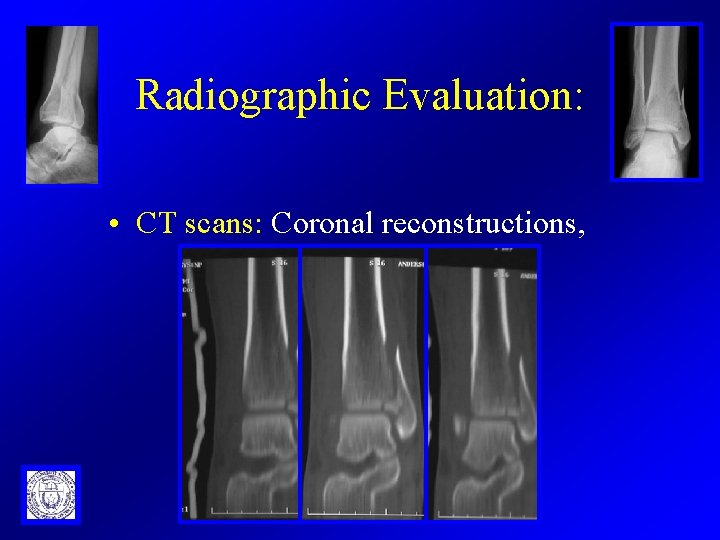
Radiographic Evaluation: • CT scans: Coronal reconstructions,
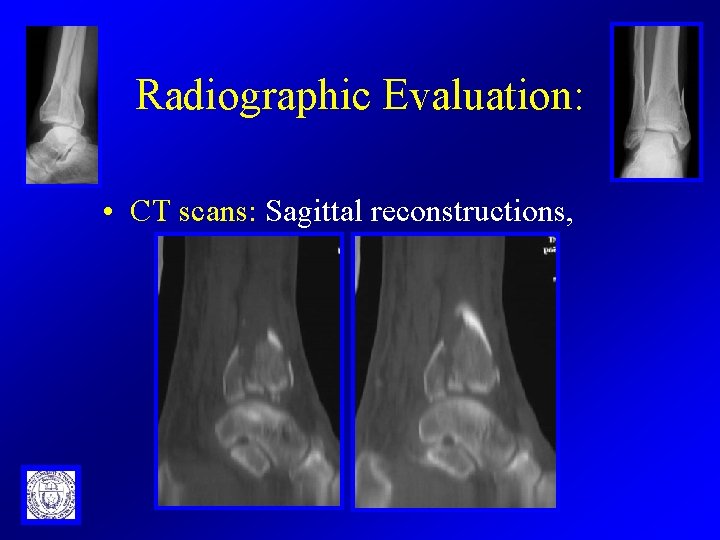
Radiographic Evaluation: • CT scans: Sagittal reconstructions,

Goals of Treatment • • Biological exposure Articular surface restoration (1) Bone graft metaphyseal defect (2) Buttress plate fixation (3) Atraumatic closure Early active ROM (4) Protected weightbearing RÜEDI - ALLGÖWER
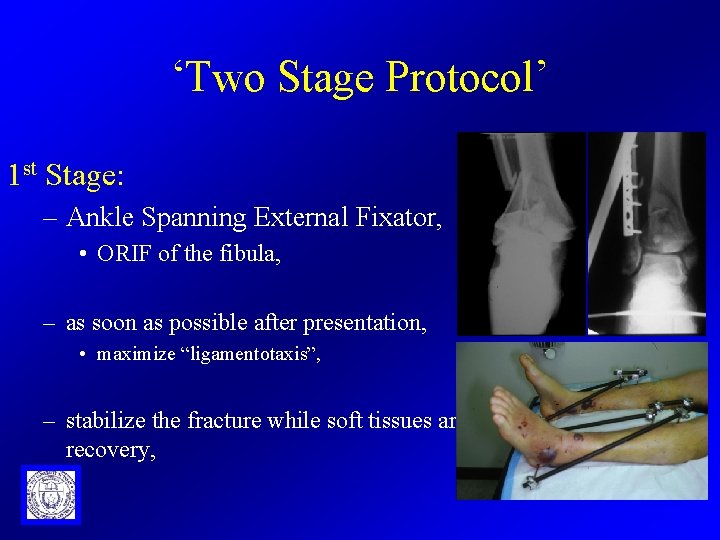
‘Two Stage Protocol’ 1 st Stage: – Ankle Spanning External Fixator, • ORIF of the fibula, – as soon as possible after presentation, • maximize “ligamentotaxis”, – stabilize the fracture while soft tissues are recovery,

‘Two Stage Protocol’ Interim: • ice, elevation, pre-operative plan, • physical therapy, • TIME to allow swelling to resolve,
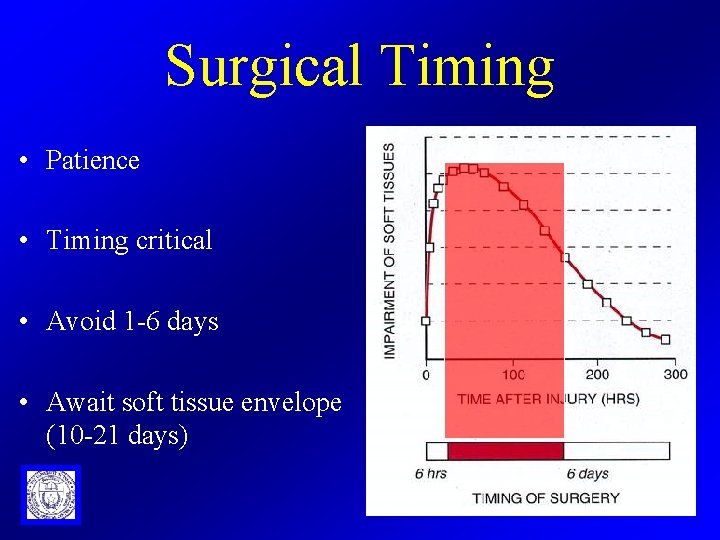
Surgical Timing • Patience • Timing critical • Avoid 1 -6 days • Await soft tissue envelope (10 -21 days)
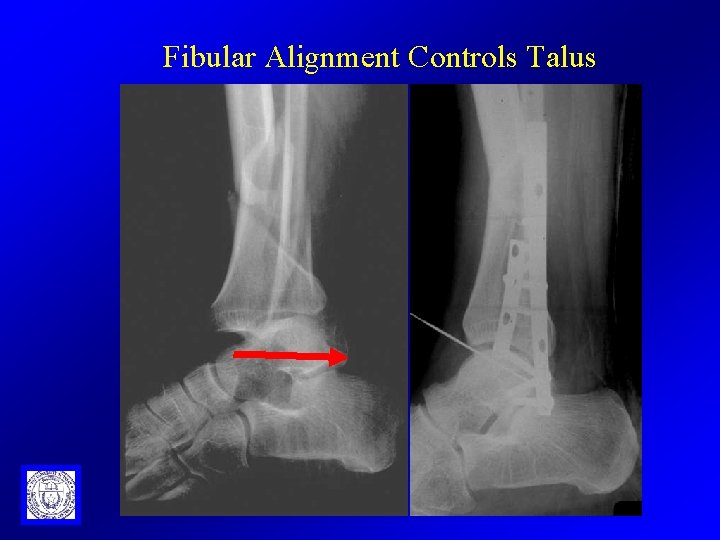
Fibular Alignment Controls Talus
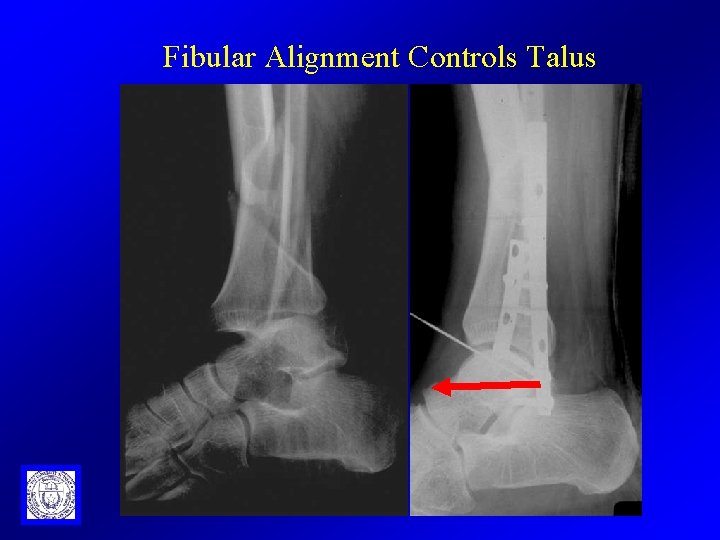
Fibular Alignment Controls Talus
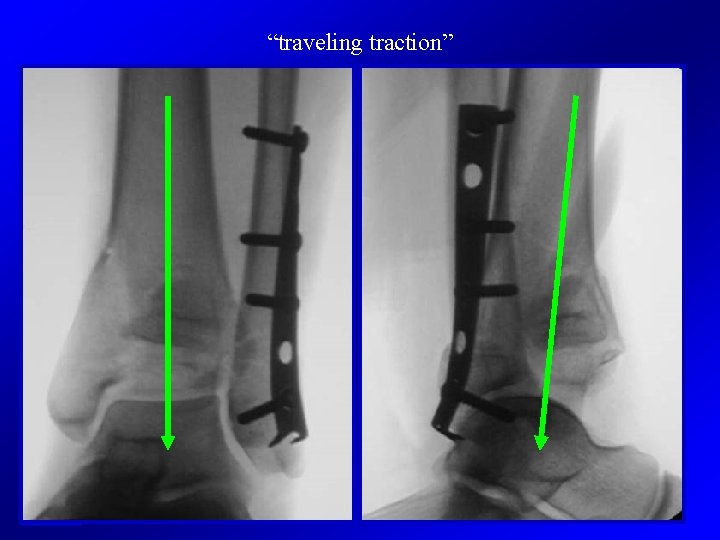
“traveling traction”
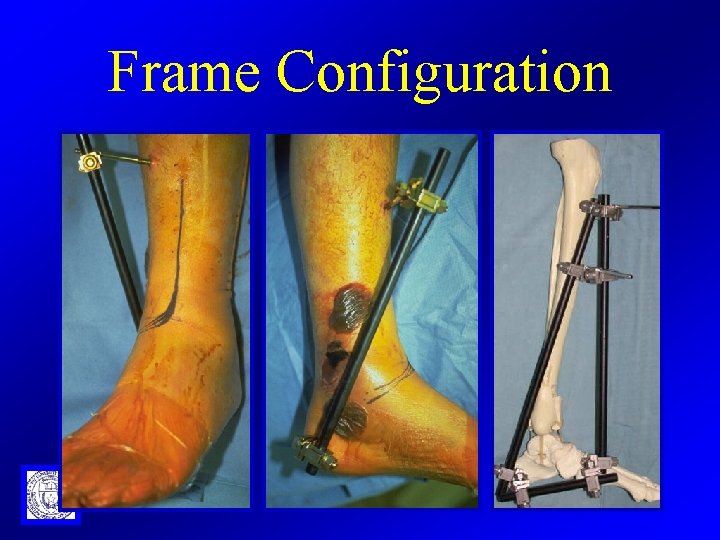
Frame Configuration
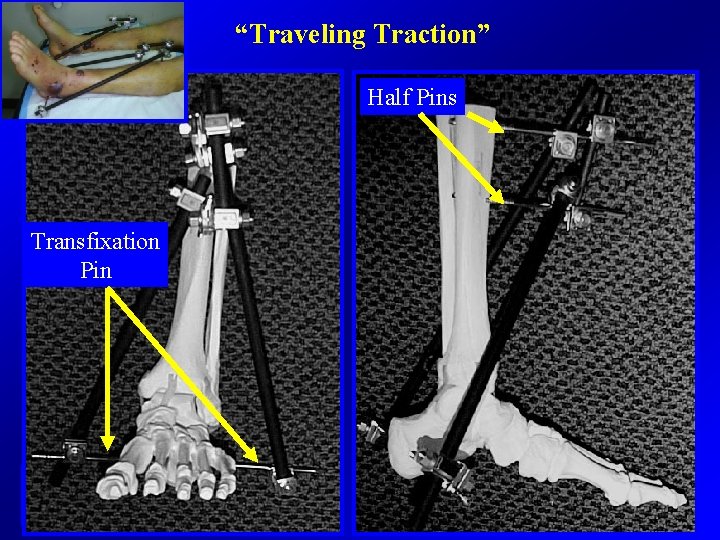
“Traveling Traction” Half Pins Transfixation Pin
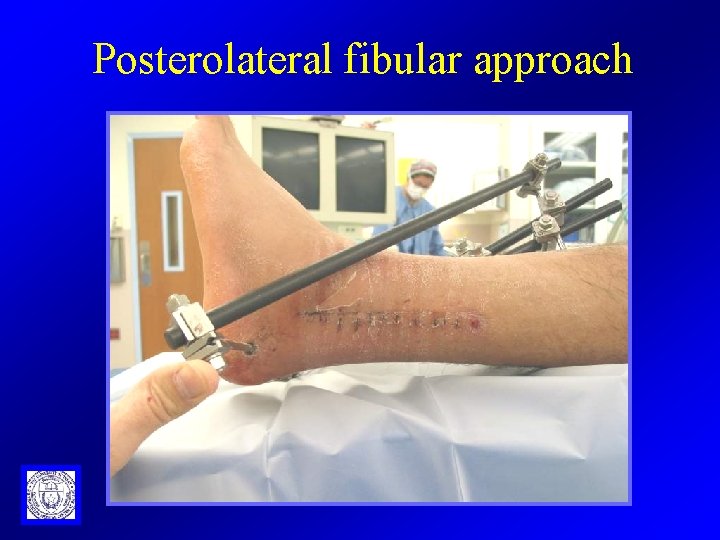
Posterolateral fibular approach
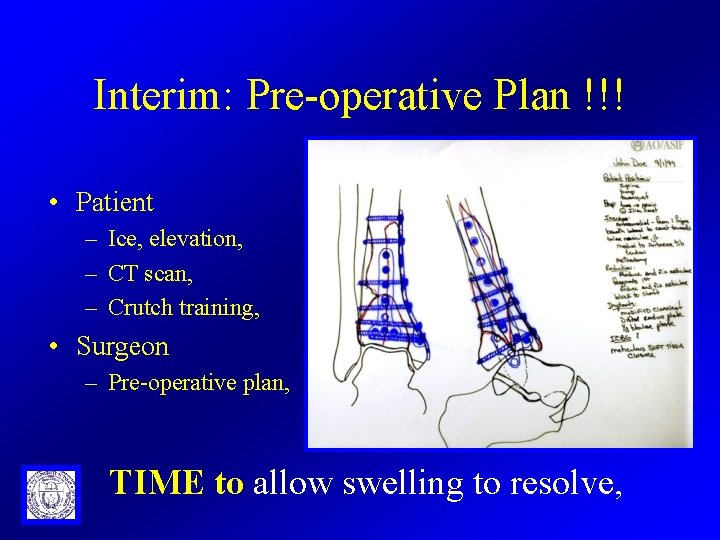
Interim: Pre-operative Plan !!! • Patient – Ice, elevation, – CT scan, – Crutch training, • Surgeon – Pre-operative plan, TIME to allow swelling to resolve,
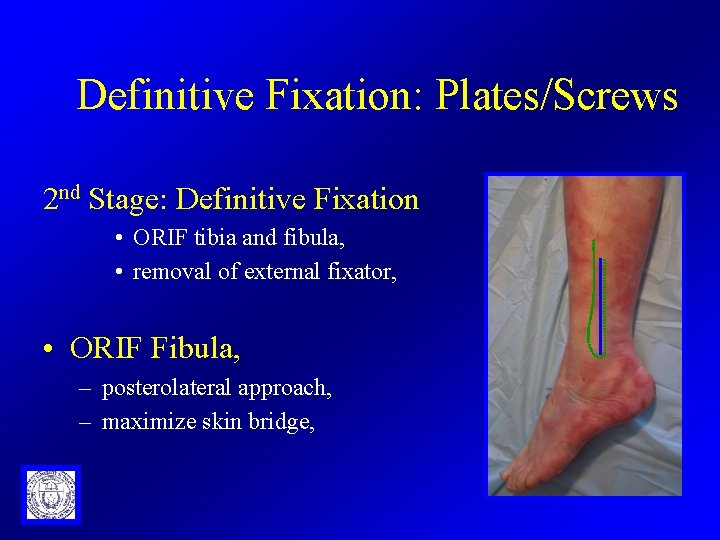
Definitive Fixation: Plates/Screws 2 nd Stage: Definitive Fixation • ORIF tibia and fibula, • removal of external fixator, • ORIF Fibula, – posterolateral approach, – maximize skin bridge,
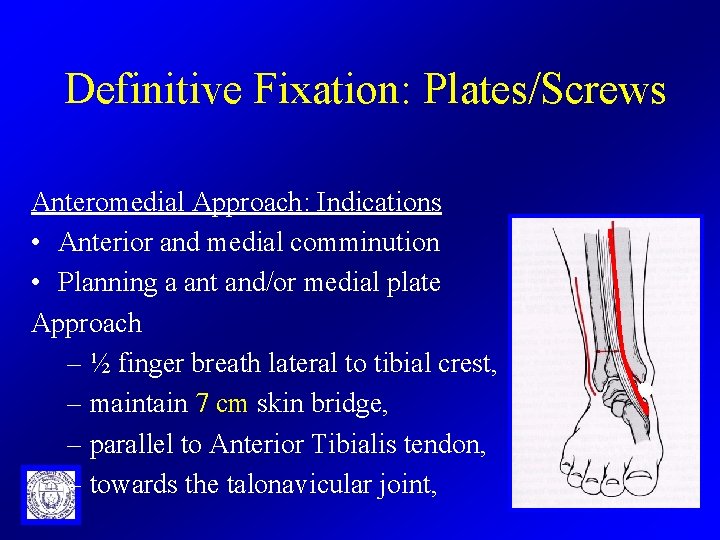
Definitive Fixation: Plates/Screws Anteromedial Approach: Indications • Anterior and medial comminution • Planning a ant and/or medial plate Approach – ½ finger breath lateral to tibial crest, – maintain 7 cm skin bridge, – parallel to Anterior Tibialis tendon, – towards the talonavicular joint,
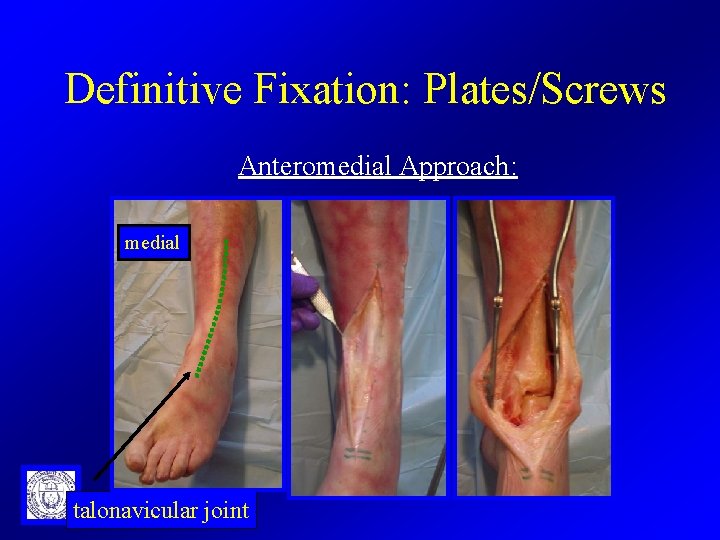
Definitive Fixation: Plates/Screws Anteromedial Approach: medial talonavicular joint

Definitive Fixation: Plates/Screws Articular Reduction: – largest, least displaced fragments first, • posterior fragment, – reduce fragments and hold, • K-wires (1. 6 mm), • pointed reduction forceps, – definitive fixation, • lag screws, cannulated screws, – reduce articular bloc to shaft, • definitive fixation,

Definitive Fixation: Plates/Screws DON’T make medial a incision !!! – incision is directly over the bone/plate, – difficult to close, – increased wound complications, • deep infection, • soft tissue loss, • free flap only bailout, – burns bridges for later reconstruction, NO !!

Definitive Fixation: Plates/Screws Anterolateral Approach (Bohler): • Indications: – open medial wound, – displaced Chaput fragment, – lateral articular comminution, • Advantage: – good soft tissue coverage, – uninjured skin, – single incision for ORIF of the tibia and fibula, Wolinsky, P, & Lee, M J Ortho Trauma 2008
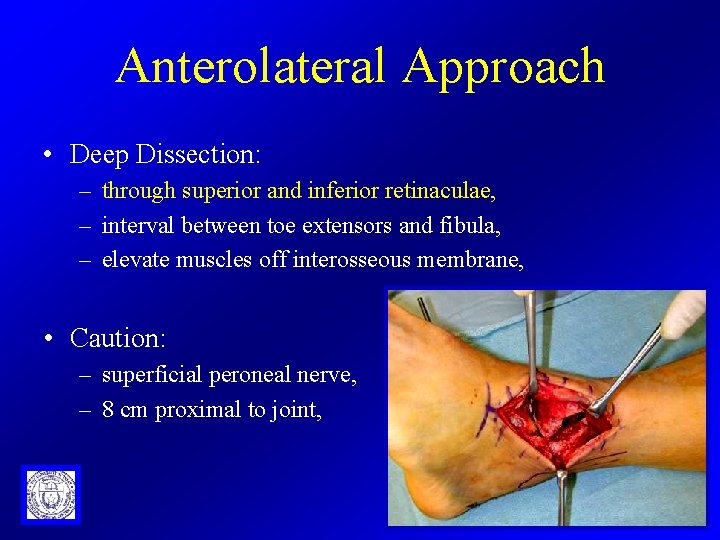
Anterolateral Approach • Deep Dissection: – through superior and inferior retinaculae, – interval between toe extensors and fibula, – elevate muscles off interosseous membrane, • Caution: – superficial peroneal nerve, – 8 cm proximal to joint,
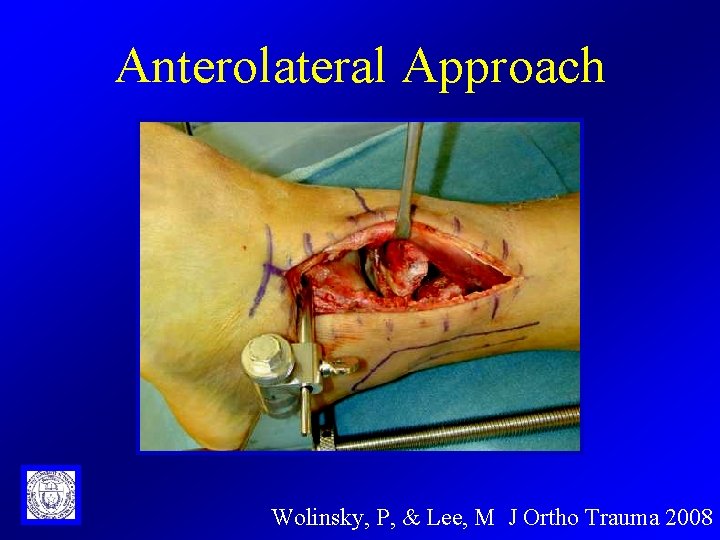
Anterolateral Approach Wolinsky, P, & Lee, M J Ortho Trauma 2008
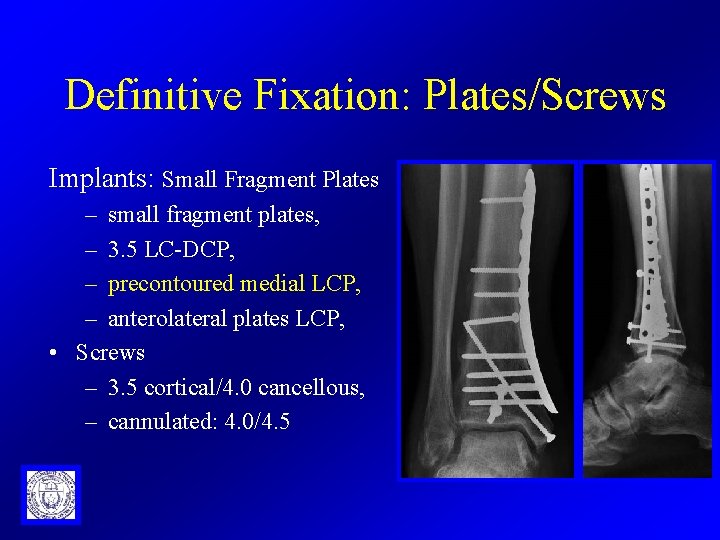
Definitive Fixation: Plates/Screws Implants: Small Fragment Plates – small fragment plates, – 3. 5 LC-DCP, – precontoured medial LCP, – anterolateral plates LCP, • Screws – 3. 5 cortical/4. 0 cancellous, – cannulated: 4. 0/4. 5
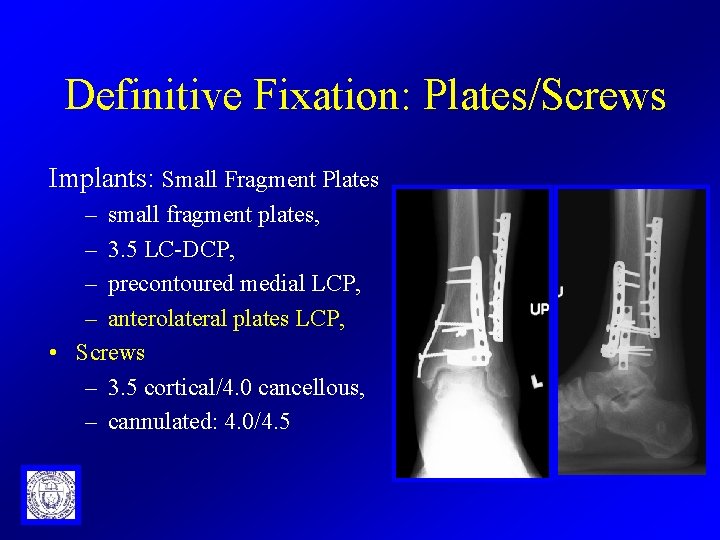
Definitive Fixation: Plates/Screws Implants: Small Fragment Plates – small fragment plates, – 3. 5 LC-DCP, – precontoured medial LCP, – anterolateral plates LCP, • Screws – 3. 5 cortical/4. 0 cancellous, – cannulated: 4. 0/4. 5

Definitive Fixation: Plates/Screws Bone Graft: Theory – support articular fragments, – augment healing, – fill cancellous defects, • ICBG, • Allograft, • Synthetic – Calcium putties,

Definitive Fixation: Plates/Screws Meticulous Wound Closure – Deep closure, • 1 -0 vicryl for capsule, • 2 -0 vicryl for subcutaneous tissue, – Skin closure • 3 -0 nylon, AllgÖwer’s modification of the Donati stitch,
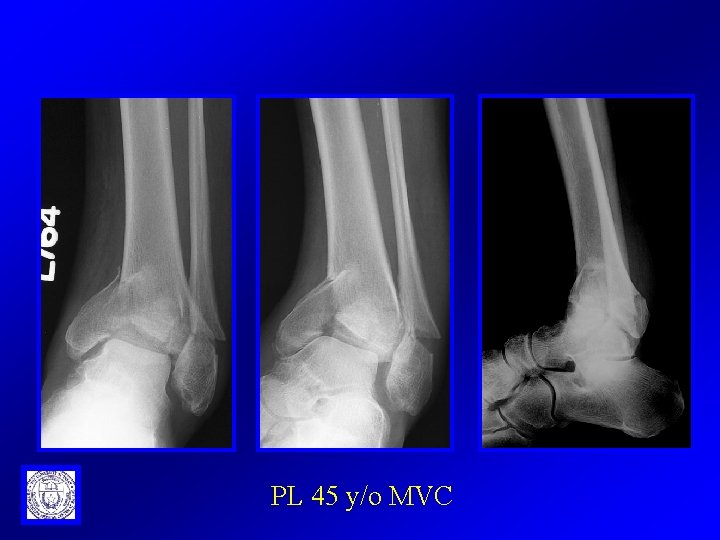
PL 45 y/o MVC
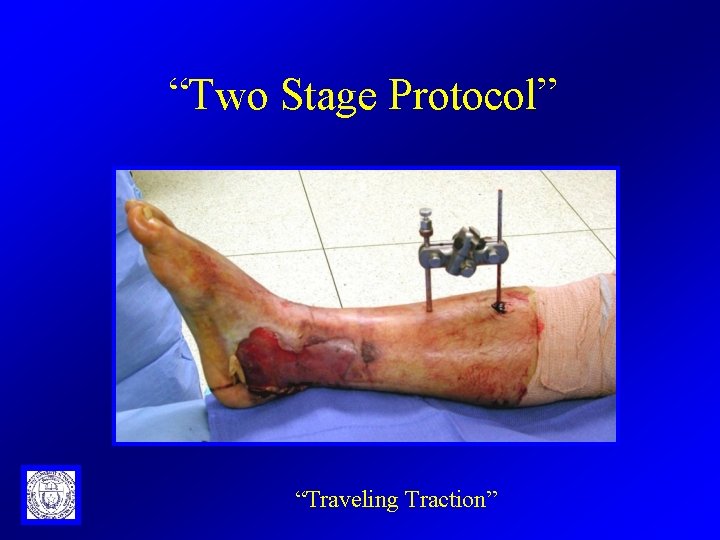
“Two Stage Protocol” “Traveling Traction”
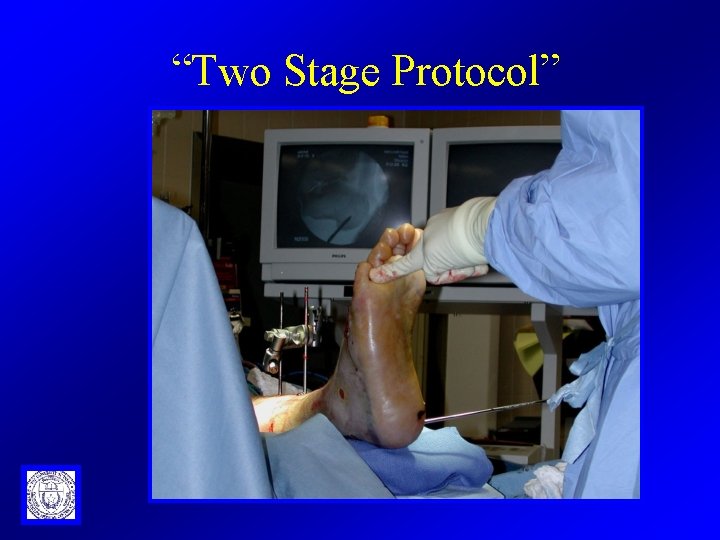
“Two Stage Protocol”
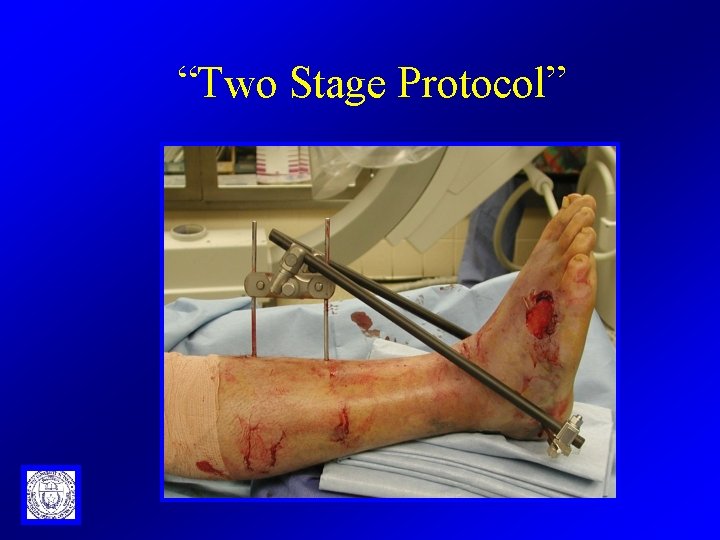
“Two Stage Protocol”
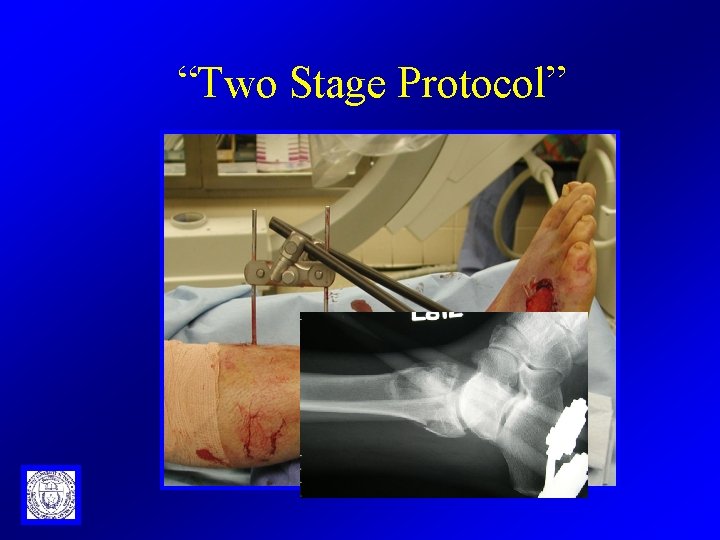
“Two Stage Protocol”
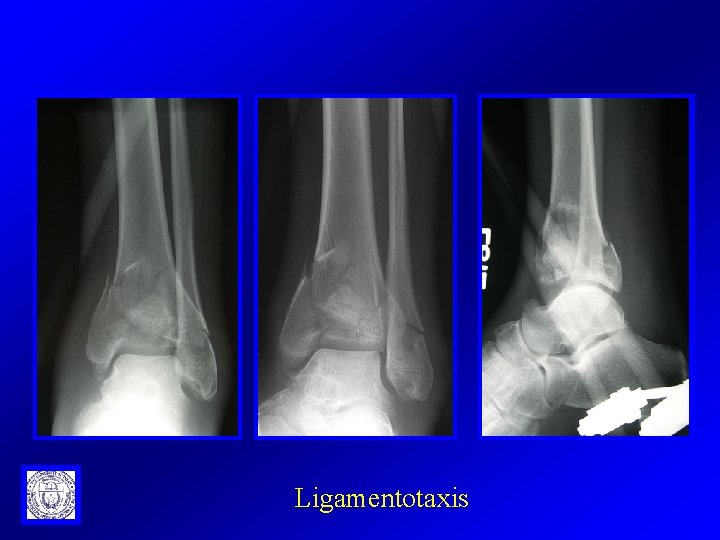
Ligamentotaxis
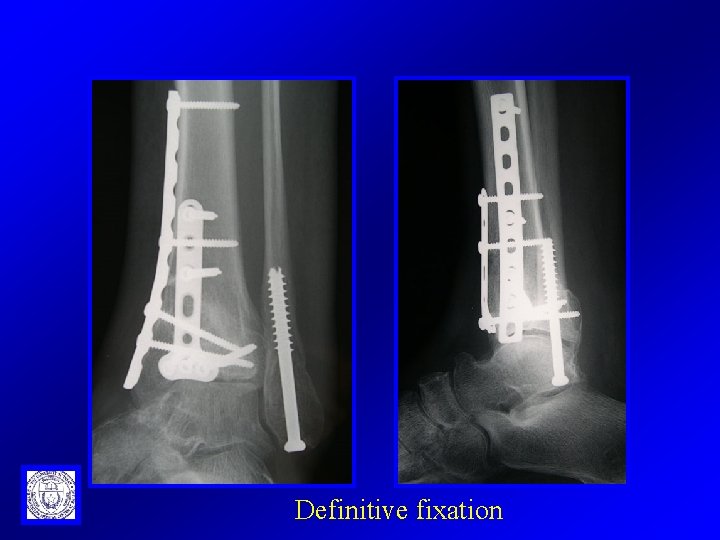
Definitive fixation

Summary • Tibial Plafond Fractures are challenging injuries, • Represent both a bony and soft tissue injury, – AO principles have remained the same: • • articular reduction, stable fixation, early mobilization of the patient and ankle, meticulous soft tissue handling,
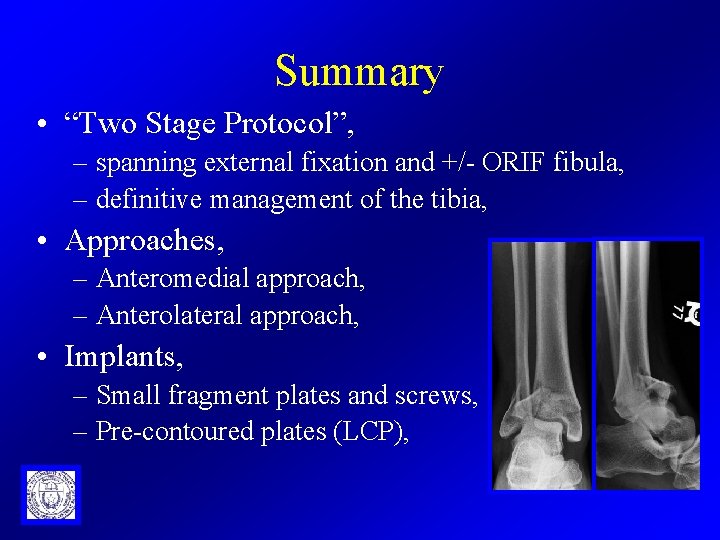
Summary • “Two Stage Protocol”, – spanning external fixation and +/- ORIF fibula, – definitive management of the tibia, • Approaches, – Anteromedial approach, – Anterolateral approach, • Implants, – Small fragment plates and screws, – Pre-contoured plates (LCP),

- Slides: 42