Intraventricular Hemorrhage John Baier MD Incidence of IVH

Intraventricular Hemorrhage John Baier MD

Incidence of IVH Late 1970’s- 80’s n Late 1980’s n – < 34 weeks – <1501 g n 39 -49% 16% Still large problem – 1. 24% of 4 million births are < 1500 g – 7400 infants per year sustain IVH

Incidence of IVH

Developmental Anatomy Bleeds originate in the subependymal germinal matrix n Site of neuronal and glial proliferation n – cerebral neuroblasts 10 -24 weeks – after 24 weeks cerebral astrocytes and oligodendroglia n Size decreases as fetus matures – 2. 5 mm at 23 -24 weeks – 1. 4 mm at 32 weeks – disappears at 36 weeks
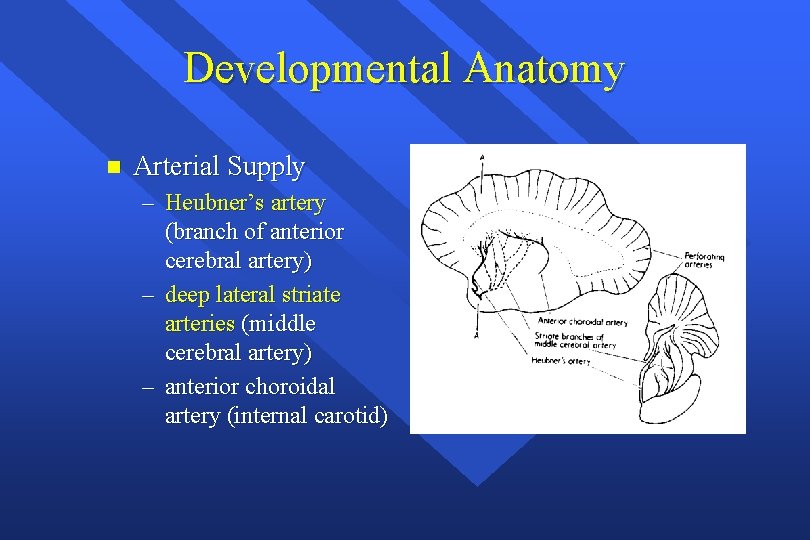
Developmental Anatomy n Arterial Supply – Heubner’s artery (branch of anterior cerebral artery) – deep lateral striate arteries (middle cerebral artery) – anterior choroidal artery (internal carotid)
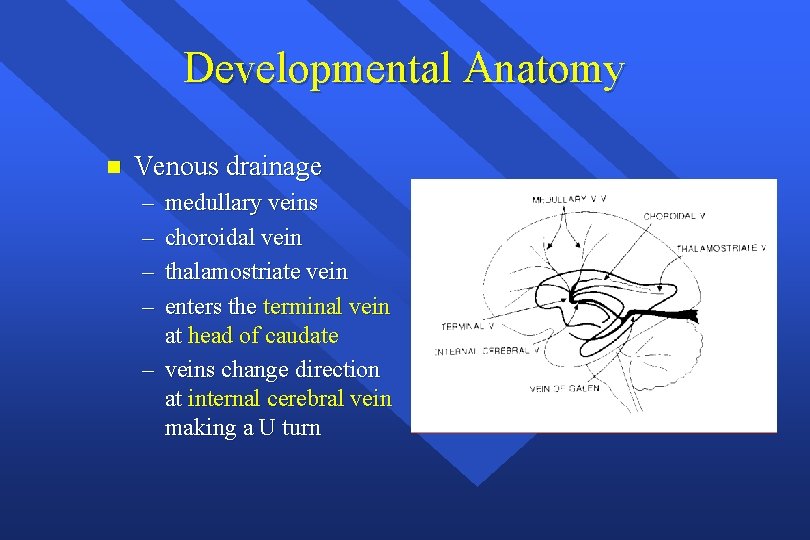
Developmental Anatomy n Venous drainage – – medullary veins choroidal vein thalamostriate vein enters the terminal vein at head of caudate – veins change direction at internal cerebral vein making a U turn

Developmental Anatomy n Capillary Network – large irregular vessels – lined only with endothelium – gelatinous matrix – as term approaches these vessels develop adventia

Why is this region prone to bleeding ?

Pathogenesis of IVH Fluctuating cerebral blood flow n Increase in cerebral venous pressure n Decrease in cerebral blood flow and reperfusion injury n Platelet and coagulation defect n Vascular factors n
Fluctuating cerebral blood flow n Normal – even arterial pressure wave » peak to peak systolic < 10% difference – cerebral blood flow parallels arterial wave n Fluctuating – systolic and diastolic pressure vary beat to beat – cerebral blood flow parallels arterial wave
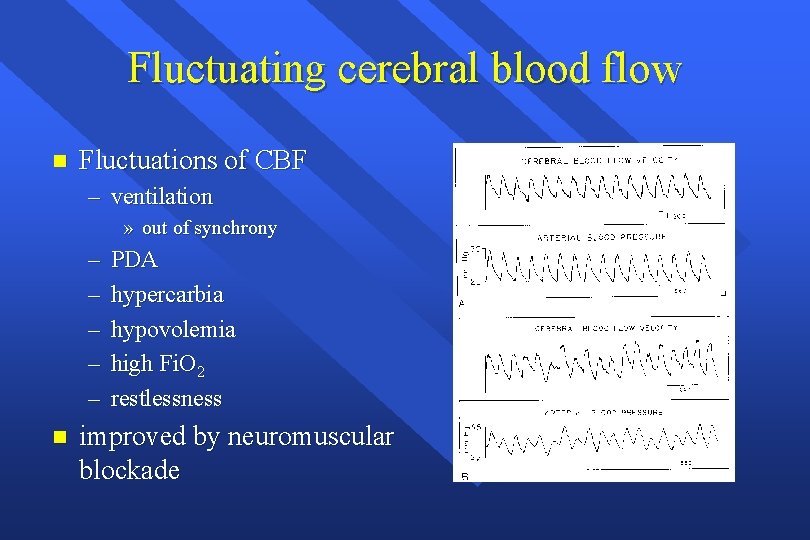
Fluctuating cerebral blood flow n Fluctuations of CBF – ventilation » out of synchrony – – – n PDA hypercarbia hypovolemia high Fi. O 2 restlessness improved by neuromuscular blockade

Increase in cerebral blood flow intact cerebral autoregulation in term infants n pressure passive cerebral autoregulation in sick preterm infants n
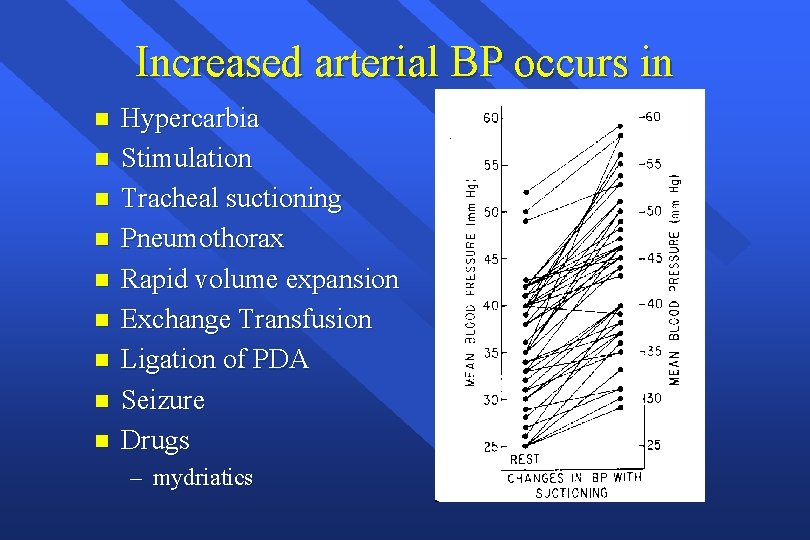
Increased arterial BP occurs in n n n n Hypercarbia Stimulation Tracheal suctioning Pneumothorax Rapid volume expansion Exchange Transfusion Ligation of PDA Seizure Drugs – mydriatics

Increased Cerebral Venous Pressure n Caused by – asphyxia – labor and delivery – respiratory » pneumothorax » high PIP » tracheal suction » respiratory mechanics

Decreases in Cerebral Blood Flow n Caused by asphyxia or hemorrhage – may be the required precedent for IVH – may be caused by less obvious factors » taking temperature » chest auscultation » suctioning n Ischemic changes in germinal matrix – free radical production – can be reduced by superoxide dismutase in animal models

Platelets and coagulation Uncertain role in IVH n Platelet-capillary function n – 40% of VLBW infants have platelets < 100, 000 – IVH rate is greater in thrombocytopenic infants – increased PGI may interfere with platelet function n Coagulation – common in VLBW infants – FFP may decrease IVH without changing coagulation

Vascular Factors n Tenuous capillary integrity – Remodeling capillary bed – Deficient vascular lining » absent muscle and collagen – Large vascular and luminal area n Vulnerability of matrix capillaries – Vascular border zone » Between striate and thalamic arteries – High metabolic activity

Extravascular Factors Deficient vascular support n Increased fibrinolytic activity n Postnatal decrease tissue pressure n

Changes in CBF with Asphyxia n Initially hypotension with decreased CBF – ischemia to germinal matrix – generation of free radicals – injury of endothelia n Resuscitation (PPV, Bicarbonate, volume etc) – loss of cerebral autoregulation – hypercarbia Increase in blood pressure and CBF n Fluctuation of CBF n
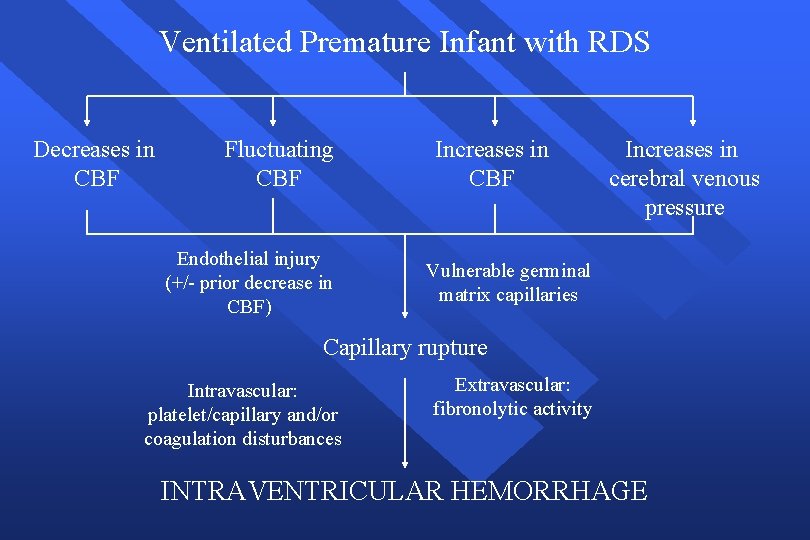
Ventilated Premature Infant with RDS Decreases in CBF Fluctuating CBF Endothelial injury (+/- prior decrease in CBF) Increases in CBF Increases in cerebral venous pressure Vulnerable germinal matrix capillaries Capillary rupture Intravascular: platelet/capillary and/or coagulation disturbances Extravascular: fibronolytic activity INTRAVENTRICULAR HEMORRHAGE
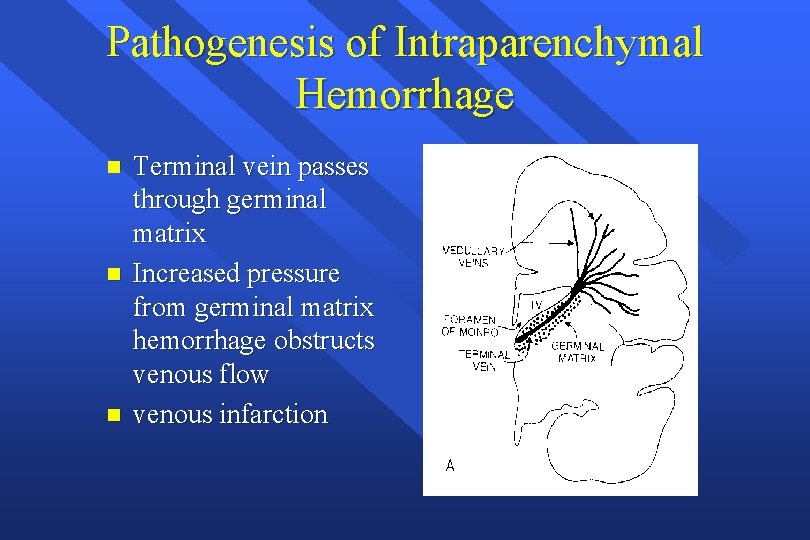
Pathogenesis of Intraparenchymal Hemorrhage n n n Terminal vein passes through germinal matrix Increased pressure from germinal matrix hemorrhage obstructs venous flow venous infarction

Timing of IVH Postnatal Day 1 2 3 4+ % infants with IVH 50 25 15 10

Clinical features of IVH n 3 clinical presentations – catastrophic – saltatory – silent

Clinical features of IVH n Catastrophic Syndrome (least common) – evolution over minutes to hours – Stupor or coma – arrhythmias, hypoventilation and apnea – Generalized seizures and “Decerebrate posturing” – Fixed Pupils, eyes fixed to vestibular stimulation – Flaccid quadriparesis

Clinical features of IVH n Catastrophic syndrome – falling hematocrit – bulging anterior fontanelle – hypotension and bradycardia – temperature changes – SIADH and very rarely DI – Outcome generally poor because of associated large intraparenchymal bleeds

Clinical features of IVH n Saltatory – more subtle – alteration in level of consciousness – change in movement (decrease) – hypotonia – minor changes in eye movements – decreased popliteal angle – outcome more favorable » depends of degree of underlying IVH

Clinical features of IVH n Clinically silent – symptoms may not be detected on routine exam – 50% of cases of IVH – unexplained fall in hematocrit

Clinical Staging of IVH Papile n I bleeding confined to subependyma n II intraventricular bleed without dilation n III intraventricular bleed with dilation n IV parenchymal bleed n

Clinical Staging of IVH I bleeding confined to subependyma n II intraventricular bleed without dilation n III intraventricular bleed with dilation n Periventricular Intraparenchymal Echodensity (IPE) n

Outcome of IVH n Acute – seizures – acute hydrocephalus – intracranial hypertension – death

Outcome of IVH n Long Term – neurologic impairment » motor » sensory – developmental impairment » cognitive » related to sensory deficits – hydrocephalus

Neurologic Impairment in IVH Incidence of impairment related to degree of IVH Incidence of Severity Neurological sequelae Mild 5% Moderate 15 % Severe 35 % Severe + IPE 90 % n

Neurologic Impairment in IVH Outcome is also related to extent of IPE Outcome Extensive IPE Localized IPE Mortality 81 % 37 % Major Motor abn 100 % 80 % IQ < 80 85 % 53 % “Normal” 0 10 % n
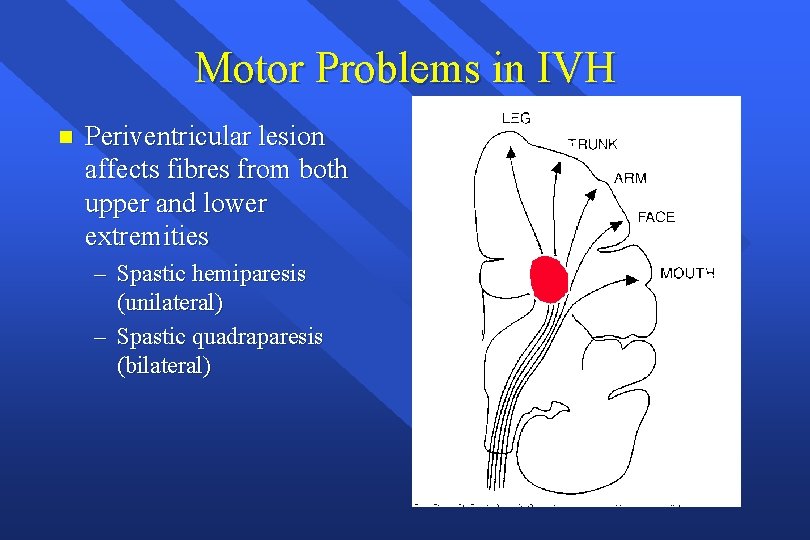
Motor Problems in IVH n Periventricular lesion affects fibres from both upper and lower extremities – Spastic hemiparesis (unilateral) – Spastic quadraparesis (bilateral)

Pathogenesis of Brain Injury in IVH n Preceding hypoxic-ischemic injury – PVL – pontine hemorrhage n Destruction of glial precursors in germinal matrix – effects on mylenation – cerebral organization n Destruction of periventricular white matter – infarction – intraventricular blood » » » potassium glutamate vasoactive compounds

Pathogenesis of Brain Injury in IVH Arterial vasospasm with focal brain ischemia n Hydrocephalus n

Hydrocephalus Progressive ventricular dilation secondary to alteration in CSF dynamics n Distinguish from ventriculomegaly with normal CSF dynamics n – atrophy “hydrocephalus ex evacuo” » PVL » IPE

Pathophysiology of Hydrocephalus n most are communicating – chronic obliterative arachnoiditis (most common) – obstruction of aqueduct by blood, clot and debris (infrequent)

Clinical Aspects of Hydrocephalus onset 1 - 3 weeks after IVH n rapidity of progression relates to degree of IVH n Head growth and signs of increased ICP follow ventricular dilation n – days to weeks n Posterior horn dilate earlier and greater than anterior horns

Management of Hydrocephalus n Medical – acetazolamide with or with out furosemide – serial lumbar punctures – serial ventricular punctures n Surgical – ventriculostomy – Rickham reservoir – VP or subgaleal shunt

Prevention of Hydrocephalus Intraventricular injection of t. PA may reduce the incidence of hydrocephalus n only a single small pilot study n

Prevention of IVH n Antenatal and Perinatal – PREVENTION OF PREMATURE BIRTHS – Maternal Transfer to high risk facility – Maternal Phenobarbital – Maternal Vitamin K – Maternal Steroids – Management of Labor and Delivery » breech delivery or prolonged labor » ? CS

Prevention of IVH n Maternal Phenobarbital – controversial (now largely abandoned) » treated infants were more ill » lower BP required increased fluids – may decrease incidence of severe IVH – may increase need for ventilation at birth – may increase RDS

Prevention of IVH n Maternal Vitamin K – vitamin K administered 4 hours prior to delivery – vitamin K administered to all infants at birth – PT normal in treated (67% normal in controls) » IVH was not related to PT – incidence of IVH was decreased in two studies

Prevention of IVH n Antenatal glucocorticoids – currently in favor – significant reduction in IVH – reduction in degree not incidence of HMD – may relate to brain maturation » glucocorticoids mature other organ systems » gut and respiratory tract

Prevention of IVH n Neonatal – Resuscitation must be prompt and adequate » avoid hypercarbia and hypoxemia – Avoid rapid infusion of volume expanders and hypertonic solutions – Correction of fluctuation in cerebral blood flow velocity » paralysis » however not easy to identify which infants have this fluctuation

Prevention of IVH n Neonatal – Prevention and treatment of hemodynamic aberrations » apnea » acute hypercarbia (CO 2) > 60 mm Hg » pneumothorax » suctioning » rapid transfusions » inotrope use » exchange transfusions

Prevention of IVH n Neonatal – Correction of abnormal coagulation » unclear data – Phenobarbital – Indomethacin – Ethamsylate – Vitamin E

Prevention of IVH n Phenobarbital – not currently used – largest controlled study showed worse outcome in treated infants

Prevention of IVH n Indomethacin – effect first noted in studies to prevent symptomatic PDA – decreases baseline cerebral blood flow – attenuates cerebral hyperemia in asphyxia – may be deleterious if hypotension occurs » decreased oxidized cytochrome oxidase » decreased cerebral intracellular oxidation – inhibits free radical formation – may accelerate maturation of germinal matrix

Prevention of IVH n Ethamsylate (not available in US) – inhibits prostaglandin synthesis distal to cyclo-oxygenase » inhibits prostacyclin predominately » does not affect cerebral blood flow – polymerization of hyaluronic acid in basement membranes – promotes platelet adhesiveness – placental transfer » ? ? ? antenatal use

Summary IVH remains a significant problem in the NICU despite recent improvements in care n Pathogenesis include anatomical susceptibility and pathologic changes in CBF n Incidence varies with gestational age n Prognosis depends on clinical stage n Current therapies are unsatisfactory and prevention remains the best way to reduce the incidence and impact of IVH n
- Slides: 52