INTRAVENOUS THERAPY Blood transfusions Central venous access Special
INTRAVENOUS THERAPY • Blood transfusions • Central venous access • Special care patients Lecture #3

BLOOD • Called Hematopoietic System • Hematopoiesis means – Manufacture and development of blood cells • System consists of: – Bone marrow – Lymphatic system, which includes the • Thymus gland • Spleen • Lymph; tonsils
BLOOD Facts about your Blood: - Actual p. H range is 7. 35 -7. 45 - Blood is considered a connective tissue - Is made up of RBC, WBC, Platelets, Plasma - Comprises about 8% of total body weight - Produced in the Red bone marrow - Divisions of blood: - Solids - Liquids

PLASMA Facts about your Plasma – Liquid portion of blood is plasma – More than half of total volume of blood is plasma – Plasma itself is 90% water. – Plasma content varies because substances are removed and added as blood circulates. – Next largest percentage of material in plasma is protein – Nutrients are found in plasma. – Helps in distribution of body heat

BLOOD • Purpose of Blood transfusion – Restore and maintain blood volume • Blood loss due to trauma, surgery, shock, or failure of the mechanism that produces RBC – Improve the oxygen carrying capacity of blood – Replace deficient blood components and improve coagulation

“WHEN IS A BLOOD TRANSFUSION NEEDED? ” • Acute and massive blood loss will empty blood vessels of the needed nutrient so that the heart cannot maintain enough pressure to pump blood and 02 to the tissues • In severe anemia where there are not enough red blood cells to carry enough 02 to the tissues

“ARE THERE OPTIONS TO A BLOOD TRANSFUSION? ” • During massive hemorrhage (loss of blood), a blood transfusion is the only practical way to keep the system working and to prevent death • Pressure of the system can be maintained by infusing plasma or certain artificial materials

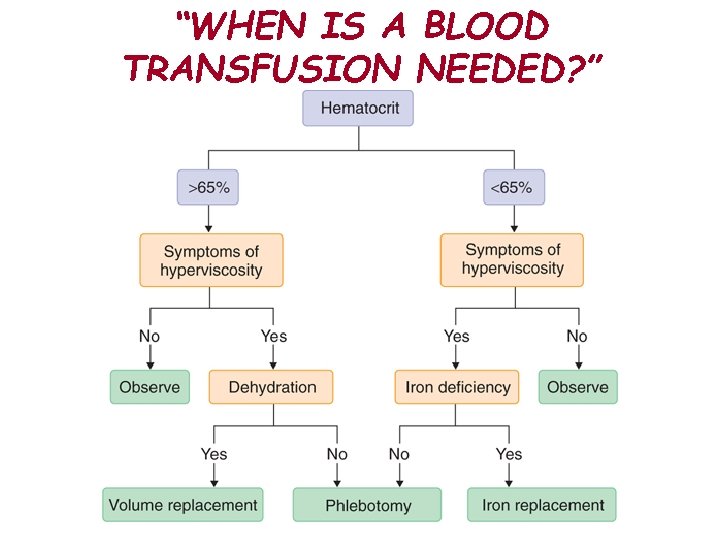
“WHEN IS A BLOOD TRANSFUSION NEEDED? ”

“ANY DANGERS TO A BLOOD TRANSFUSION? ” YEP! • Accumulation of fluid in the lungs if administered to rapidly • Damage to kidneys if incorrectly typed • WBC may clump together to release chemicals causing lung disease and severe fever • Blood may be contaminated by bacteria causing infections • Viruses and other parasites may be present in the donor and cause illness to recipient

NURSE’S RESPONSIBILITY • Most common cause of transfusion reactions is receiving the wrong blood – Check that you have the right blood/components, Rh factor, and right patient – Check that type and crossmatch done – Check that informed consent has been signed – Have another licensed person verify all information – Inspect the blood for abnormalities

BLOOD TYPES • Blood group A Blood has A antigens on surface of RBC and B antibodies in blood plasma. • Blood group B Blood has B antigens on surface of RBC and A antibodies in blood plasma. • Blood group AB Blood has AB antigens, then both A and B antigens are on the surface of RBC and no A or B antibodies at all in blood plasma. • Blood group 0 Blood has neither A or B antigens on the surface of RBC but have both A and B antibodies in blood plasma.

BLOOD TYPES • The Rh factor or D antigen, refers to the presence or absence of a specific antigen in the blood. (An antigen is a substance capable of stimulating an immune response. ) • People are either Rh positive or Rh negative, meaning they either have the antigen or they do not.

NURSING ALERT!!! If anthing abnormal is observed with the blood or blood product, return to the blood bank with explanation and … DO NOT USE!!!

GUIDE TO BLOOD PRODUCTS and COMPONENTS • Whole blood – volume 500 ml – Type and cross-match necessary – Given to restore blood volume in hemorrhage, trauma or burn patients – Seldom administered except in emergency situations • Packed red blood cells – volume 250 ml – Type and cross-match necessary – Same RBC mass as whole blood with 80% plasma

GUIDE TO WHOLE BLOOD AND PRODUCTS • Leukocyte poor–RBC’s – Type and cross-match necessary – To restore/maintain 02 carrying capacity – To correct anemia and surgical blood loss – To treat immunosuppressed patients


GUIDE TO WHOLE BLOOD AND PRODUCTS • White blood cells – Type and cross match necessary – To treat patient with life-threatening low granulocyte count • Platelets – ABO compatibility not necessary but is preferred – To treat thrombocytopenia and acute leukemia; to restore platelet count

GUIDE TO WHOLE BLOOD AND PRODUCTS • Fresh frozen plasma – To expand plasma volume; To treat post-surgical hemorrhage and shock; To replace/correct deficiency a specific factor • Albumin – volume varies – To replace circulatory volume in burns, trauma; to treat hypoproteinemia

GUIDE TO WHOLE BLOOD AND PRODUCTS • Factor VIII – volume varies – To treat Hemophilia A; to control bleeding associated with factor VIII deficiency; to replace fibrinogen or factor VIII – Type and cross matching not necessary but recommended
BLOOD TRANSFUSIONS • Two kinds of transfused blood – Autologus • From recipient himself – Homologus • From donor • Plasmapheresis – Removal of plasma from blood with retransfusion of the formed elements into the donor • Hemapheresis – Collecting and removing specific blood components and return the remaining to the donor

TRANSFUSION PROCEDURE A blood transfusion is the transfer of blood or blood products from one person into another person’s bloodstream

PRIOR TO INFUSION • Prior to infusing blood, patient should have these tests done – ABO Blood typing – Rh typing – Cross matching of blood – Direct antiglobulin blood test (also called the direct Coombs test)- determines whethere is an immune etiology. – Antibody screening; screening for diseases

ALERT!!! Two licensed health care professionals must check the unit of blood to be transfused to be sure the correct match is made.

“READY… • Take patient’s vital signs – Prior to infusion - To establish a baseline – Recheck every 15 minutes for the first hour; more frequently if warranted • If patient does not have an IV in place – Perform a venipuncture using a 20 G or larger needle – Use only Normal Saline
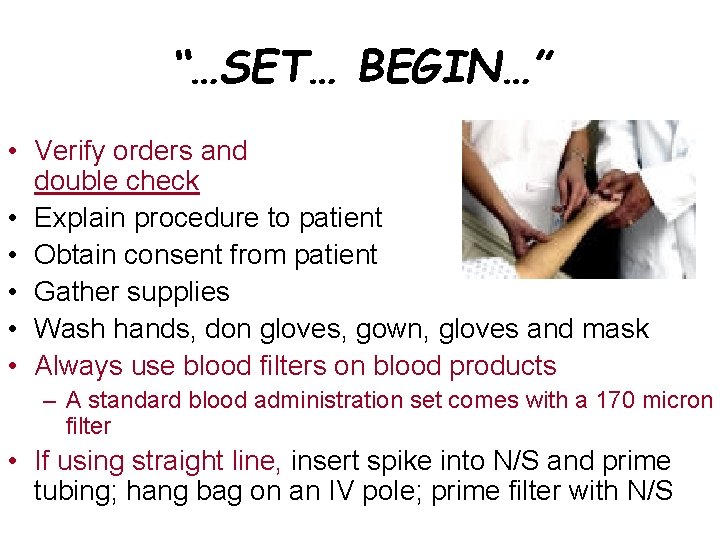
“…SET… BEGIN…” • Verify orders and double check • Explain procedure to patient • Obtain consent from patient • Gather supplies • Wash hands, don gloves, gown, gloves and mask • Always use blood filters on blood products – A standard blood administration set comes with a 170 micron filter • If using straight line, insert spike into N/S and prime tubing; hang bag on an IV pole; prime filter with N/S

“…AND GOING…” • If using a “Y”-type” blood administration set – Close all clamps on the set – Blood and normal saline are connected and can be clamped without opening the system – Insert the spike of the line you are using for normal saline solution into that bag and prime tubing – Then open the port on the blood bag and insert the spike into the blood or cellular component into the port.
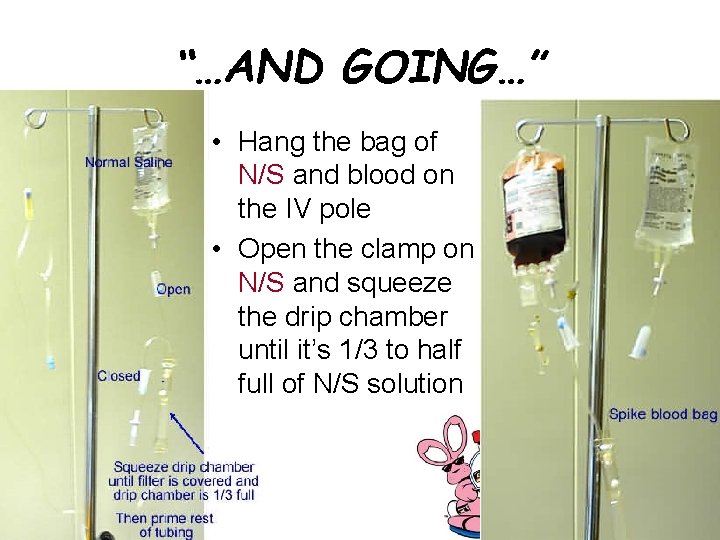
“…AND GOING…” • Hang the bag of N/S and blood on the IV pole • Open the clamp on N/S and squeeze the drip chamber until it’s 1/3 to half full of N/S solution

NURSING TIP Blood and blood products are transfused only with normal saline. No other medications or solutions may be given through the same line

“…AND GOING…” • Flush with N/S • When using a Y-type set, open the clamp on the N/S line and the main flow clamp • When administering whole blood or white blood cells, gently invert the bag several times during the procedure to mix the cells • During the administration gently agitate the bag to prevent the viscous cells from settling

“AND ADJUSTING THE FLOW. ” • After having flushed the venous access device, the blood can be transfused • Adjust the flow clamp closest to the patient to deliver a slow rate – Usually 20 gtts/min for the first 10 to 15 minutes

TERMINATING A TRANSFUSION • When transfusion is complete – Flush the blood tubing with an adequate amount of N/S • Reassess the patients condition and vital signs • Discard blood bag and tubing according to facility policy • If IV is to continue – use the N/S and replace tubing

DOCUMENT, DOCUMENT • Be sure this is done following transfusion start: – Date/time of transfusion; ID number on blood bag – Type and amount of blood transfused – Volume of N/S infused – Status of venous access site – Patient’s vital signs and how tolerated – If reaction occurred

CONSIDER THIS… • The type of blood product being given and the patient’s condition determines the rate • Most reactions occur within the first 15 minutes, but… • A unit of Red blood cells may be given over a period of 1 to 4 hours • A transfusion should not take longer than 4 hours because of the risk of contamination and sepsis increases after that. • Discard or return to the blood bank any blood or blood products not given in that time.

MONITORING TRANSFUSION • To help recognize a reaction – Record patient’s vital signs before transfusion and 15 minutes after starting and right after completion – More often if patient’s condition warrants • Most hemolytic reactions occur during the first 15 minutes • Always have N/S hanging as the primary line

TRANSFUSION REACTION • If reaction occurs - Stop transfusion • Change IV tubing; Administer NSS • Take vital signs (Pulse, b/p, resp, temp) • Maintain IV site and Infuse with normal saline using new tubing • Notify primary care provider • Send blood, tubing, UA, blood sample to lab • Monitor I & O &
SYMPTOMS OF TRANSFUSION REACTION • • • Bronchospasm Flank pain/back pain Bloody urine Fainting Rash Fainting

TYPES OF REACTIONS • Hemolytic – destroys transfused blood – Life threatening; result of incompatible blood/improper storage of blood; clerical error – Can progress to shock and renal failure – Monitor vital signs; treat for shock • Nonhemolytic reaction – Febrile – does not destroy transfused blood – Fever as result of transfusion – Relieve symptoms with antipyretic/ antihistamine

TRANSFUSION REACTION for these signs of a FEBRILE transfusion reaction – Fever, malaise – Chills – Headache; low b/p; dyspnea – Nausea – Chest pain

TYPES OF REACTIONS • Allergic – 2 nd most common transfusion reaction – Administer antihistamines – Monitor for anaphylactic reaction; administer epinephrine and steroid if ordered • Circulatory overload – occur more with those who have diminished cardiac function – Stop the transfusion – Maintain the IV with NSS – Administer 02; elevate the patient’s head

REACTIONS FROM MULTIPLE TRANSFUSIONS • Hemosiderosis – Accumulation of iron containing pigment – may destroy RBC • Elevated ammonia levels – Acquired from stored blood • Hypothermia – Rapid infusion can lower body temperature – May experience shaking chills, low b/p, cardiac arrhythmias

REACTIONS FROM MULTIPLE TRANSFUSIONS • Potassium toxicity – Some cells in stored RBC’s may leak potassium into the plasma; usually occurs with large volumes of blood transfused • Citrate toxicity – also called hypocalcemia – If blood transfused to rapidly (citrate is used to preserve blood) – Monitor potassium and calcium levels

TRANSMISSION OF DISEASE • Hepatitis C – Can go undetected days/wks/months later – Prevention – laboratory testing; careful screening of potential donors • HIV – HIV screening determines the presence of antibodies and antigens to HIV – Thorough screening of potential donors • Syphilis – Routine screening still done – Refrigeration of blood kills the syphilis organism

SPECIAL NEEDS PATIENT PEDIATRIC GERIATRIC

PEDIATRIC PATIENTS • Keep this in mind: – A child’s normal circulating blood volume determines the amount of blood to be transfused – Blood units for pediatrics are prepared in half units – Usually a 24 gauge or 22 gauge thin walled catheter is used – Must use an electronic infusion device

PEDIATRIC PATIENTS • Closely monitor especially in the first 15 minutes; reactions are more likely • Blood warmers may be used if indicated. • Fluid overload is a major danger and must be avoided.

GERIATRIC • A Geriatric patient who has a preexisting heart conditon may be unable to tolerate a rapid transfusion of an entire unit of blood; may exhibit signs of SOB or heart failure • More at risk for delayed blood transfusion reaction due to slowing of immune system • Geriatric patients are usually less resistant to infections
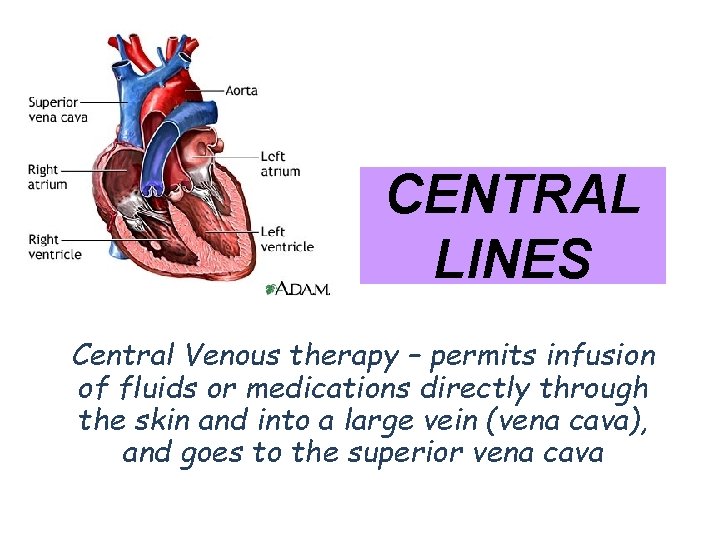
CENTRAL LINES Central Venous therapy – permits infusion of fluids or medications directly through the skin and into a large vein (vena cava), and goes to the superior vena cava

WHAT IS A CENTRAL VENOUS INFUSION? • Infusions that deliver solutions into a large central vein, such as the vena cava • The catheter is inserted through the skin into a vein often in the neck or chest. – Subclavian vein, – Jugular vein, – Femoral vein

CENTRAL LINES • After insertion, location of the catheter must be checked by x-ray • Advantages? – Ability to deliver irritating or concentrated medications – Rapid onset of action – When peripheral veins have collapsed – Ability to measure central venous pressure – For long term therapy

CENTRAL LINES • Disadvantages – Can become infected – Higher risk of bleeding – Higher risk of bacteremia – High risk of air embolism – Require greater skill to insert and are costly to maintain – usually done by a physician

TYPES OF CENTRAL VENOUS CATHETERS • • Single-lumen Multi-lumen Groshong – tunneled catheter Hickman - “ “ Broviac “ “ Hickman-Broviac Long-line catheter Peripherally inserted central catheter
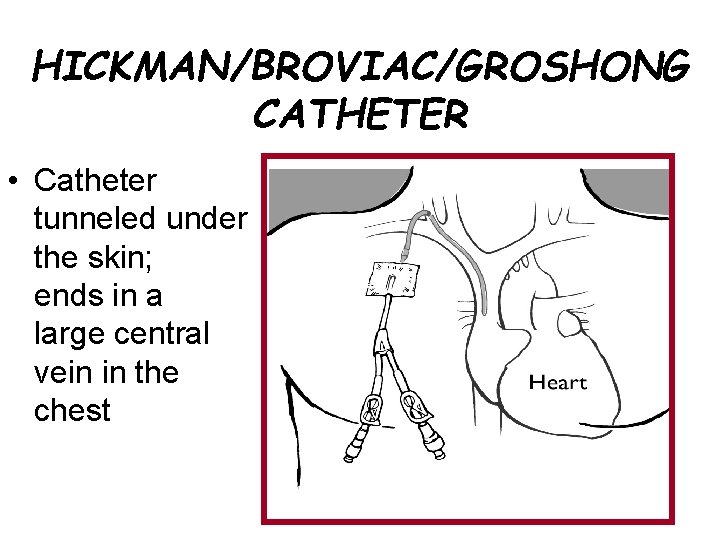
HICKMAN/BROVIAC/GROSHONG CATHETER • Catheter tunneled under the skin; ends in a large central vein in the chest
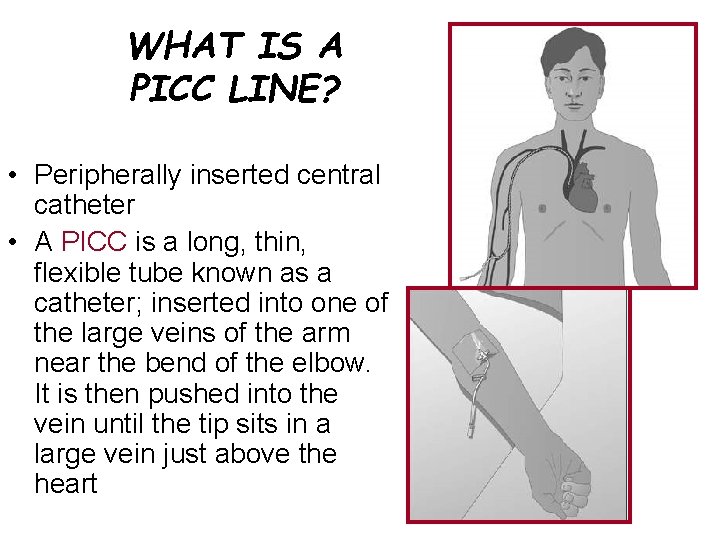
WHAT IS A PICC LINE? • Peripherally inserted central catheter • A PICC is a long, thin, flexible tube known as a catheter; inserted into one of the large veins of the arm near the bend of the elbow. It is then pushed into the vein until the tip sits in a large vein just above the heart

IMPLANTABLE PORTS • A port – Referred to as Port-a-Cath or Medi-port – Does not have an external connector – Has small reservoir implanted under the skin – Medication can be administered by placing a small needle through the skin into the reservoir – Has low risk of infection – Commonly used for patients on long term treatments
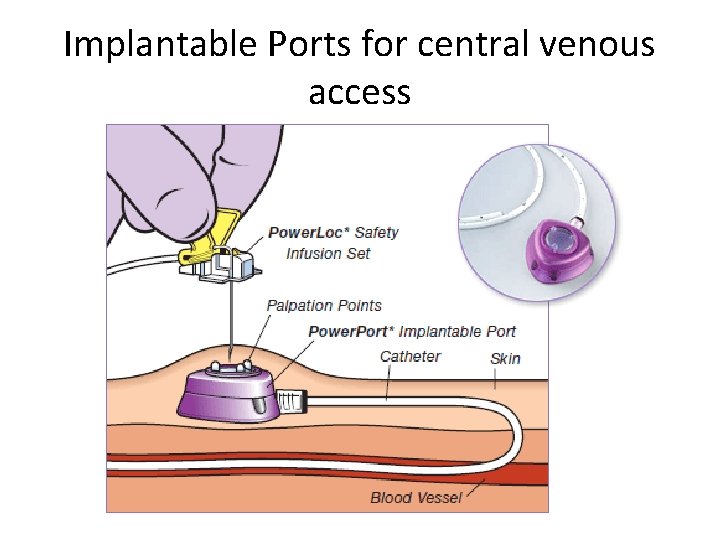
Implantable Ports for central venous access

DRESSING MANAGEMENT of CENTRAL LINES This reduces the risk of infection and requires meticulous care

DRESSING CHANGES in GENERAL • Patients who receive IV therapy for more than 24 hours need to have their insertion site, tubing, fluid and dressing changed at certain intervals • Standards as set by the Infusion Nurse’s Society – Peripheral IV sites are changed every 72 hours – Tubing is changed every 72 hours with the site change – A gauze dressing is changed every 48 hours – A transparent semi-permeable membrane dressing is changed every 72 hours – The solution is changed every 24 hours

DRESSING CHANGES • Central Venous Infusions – In general, gauze dressings on Central Venous access sites are changed every 48 hours – Semi-permeable transparent dressings are changed every 3 -7 days – Whenever the site dressing is loose or sterility is compromised, the dressing should be changed

NURSING TIP Always wear gloves and a mask when changing the central venous access dressing. The patient should also wear a mask if possible

EQUIPMENT for DRESSING CHANGE of CENTRAL LINES • Some facilities provide a preassembled dressing change tray that contains all the necessary equipment – Chlorhexidrine swabs – Transparent semi-permeable tape – Sterile drape – Sterile gloves and masks – Clean gloves – Bag to dispose of old dressing

READY… • • Gather all equipment Wash hands Explain procedure to patient Place patient in comfortable position – Head turned away from catheter insertion site – Place mask over patient’s mouth, nose • Organize supplies and equipment • Prepare a sterile field; Don mask; gown • Don pair of clean gloves

SET… • Remove present dressing carefully • Discard soiled dressing • Visually inspect skin and catheter site for signs of infection/leakage/other problems • Removed soiled gloves and discard; wash hands; don sterile gloves • Working in circular motion from insertion site outward, cleanse skin with ANTI-MICROBIAL wipes 30 seconds; allow to dry

…G 0 • Redress the site with transparent semipermeable dressing • Loop and secure IV tubing to dressing on arm or chest • Label dressing with time, date of dressing change and insertion and initials • Discard supplies used • Wash hands • Document the dressing change, the condition of the insertion site; document any problems

FLUSHING CENTRAL LINES Observed by the LVN • Flushing the Central line catheter with saline solution routinely is done according to the facilities policy • Why? – Maintains patency of line • Amount? – Amount of solution varies; per Infusion Nurse’s Society states to “flush at least 2 times the volume capacity of the catheter and add on devices” – Facilities recommend using 3 -5 ml of solution – Some facilities allow for as much as 10 ml of solution

FLUSHING CENTRAL LINES • How often? – Varies from every 8 hours to once per day • Follow these steps – Wash hands – Put on gloves – Clean cap with alcohol swab – Allow cap to dry – Inject prescribed type and amount of solution.

BLOOD WITHDRAWAL Observed by the LVN • Management and care of Central Venous Catheters (CVC) may only be undertaken by licensed nurses accredited to give intravenous medication • Procedure should be carried out under strict asepsis. • The Central Venous Catheters is not an ideal site for drawing blood samples but may be used in conditions where other access is not available.

REMOVAL OF CENTRAL CATHETER • This procedure is governed by the Nurse Practice Act. • Long term catheters and implanted devices are always removed by physician • PICC lines may be removed by a licensed nurse who is certified to do so.

CENTRAL LINE COMPLICATIONS As with any invasive procedure, central venous therapy can pose risks

RISKS OF CENTRAL VENOUS THERAPY • Problems – Pneumothorax • Hemothorax – collection of blood in pleural cavity • Chylothorax – presence of chyle in pleural cavity • Hydrothorax – presence of noninflammatory serous fluid within the pleural cavity – Air Embolism – Thrombosis – Local infection
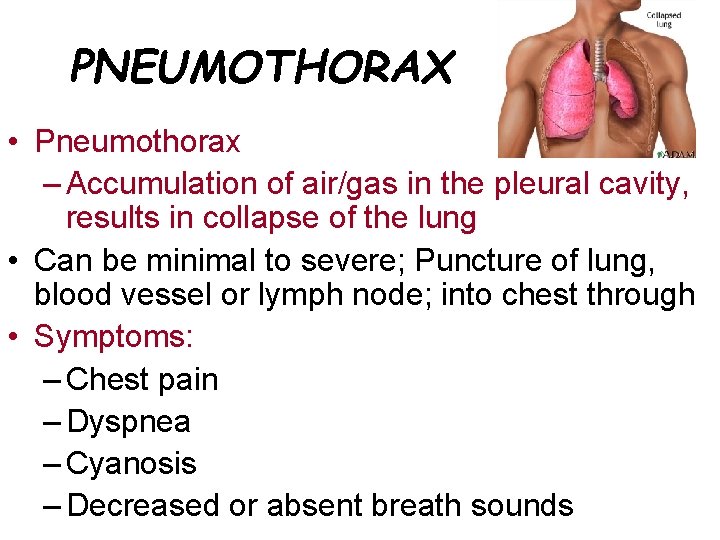
PNEUMOTHORAX • Pneumothorax – Accumulation of air/gas in the pleural cavity, results in collapse of the lung • Can be minimal to severe; Puncture of lung, blood vessel or lymph node; into chest through • Symptoms: – Chest pain – Dyspnea – Cyanosis – Decreased or absent breath sounds

PNEUMOTHORAX • Prevention – Proper positioning of patient during insertion – Assess for sign of early fluid infiltration • Swelling of neck, shoulder and arm areas – Immobilize patient during insertion – Explain procedure – Sedate if necessary – Confirm placement with x-ray

AIR EMBOLISM • Air embolism – The sudden blocking of an artery by an air bubble • Causes – Intake of air into system • During insertion; or During tube change – Inadvertently • Opening • Removal • Cutting; or Breaking catheter
AIR EMBOLISM • Symptoms – Respiratory distress – Unequal breath sounds – Weak pulse – Increased central venous pressure – Decreased blood pressure – Churning murmur over precordium – Change in level of consciousness

AIR EMBOLISM • Nursing Interventions – Clamp the catheter immediately – Cover the exit site – Turn patient’s head to the left side, head down; air can enter the right atrium, rather than pulmonary artery – Don’t perform the valsalva maneuver – Administer 02 – Notify MD – Document, document

AIR EMBOLISM • Prevention – Purge all air from the system before hook-up – Patient taught to perform the valsalva maneuver during insertion – Use air eliminating filters – Use infusion control device with air detection – Use luer lock tubing and tape connections
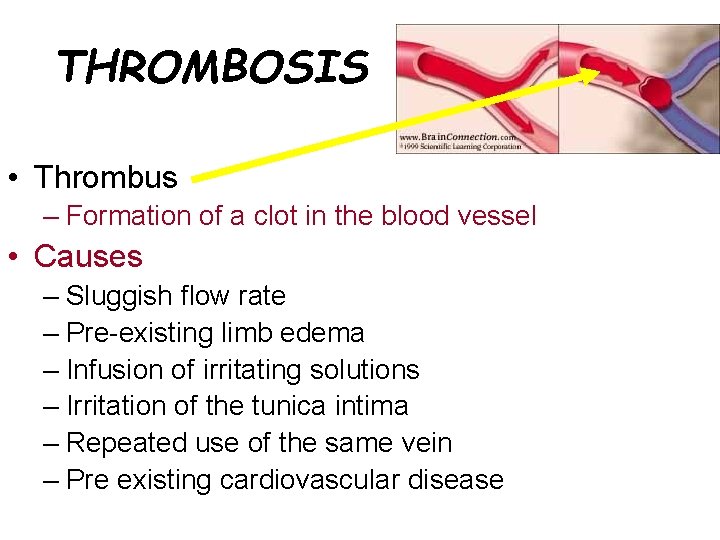
THROMBOSIS • Thrombus – Formation of a clot in the blood vessel • Causes – Sluggish flow rate – Pre-existing limb edema – Infusion of irritating solutions – Irritation of the tunica intima – Repeated use of the same vein – Pre existing cardiovascular disease
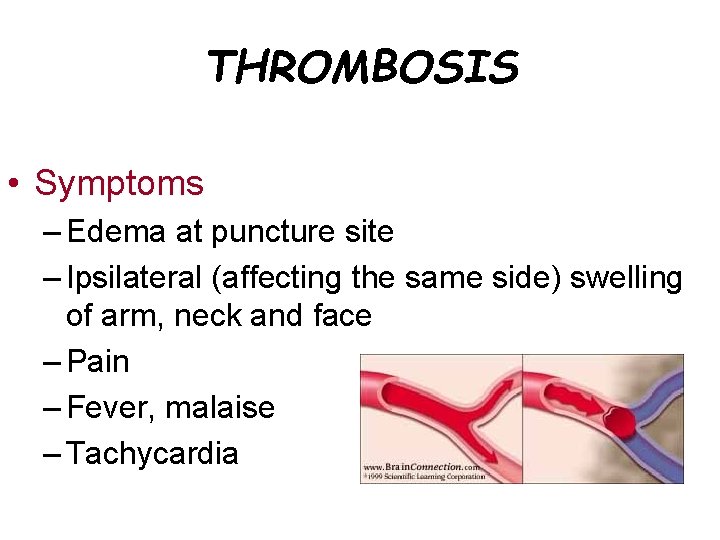
THROMBOSIS • Symptoms – Edema at puncture site – Ipsilateral (affecting the same side) swelling of arm, neck and face – Pain – Fever, malaise – Tachycardia

THROMBOSIS • Interventions – Notify MD – Infuse a thrombolytic to dissolve clot if ordered – Verify thrombosis with diagnostic studies – Don’t use limb on affected side for subsequent studies – Document

THROMBOSIS • Prevention – Maintain flow through catheter at a steady rate with an infusion pump – Flush at regular intervals – Verify that the catheter tip is in the superior vena cava before using the catheter

INFECTION • Local – Redness, warmth, tenderness & swelling at insertion site – Possible exudate – Rash, pustules – Fever, chills, malaise • Systemic – Fever, chills for no apparent reason – Leukocytosis – N&V; malaise – Elevated urine glucose level

INFECTION • Causes – Failure to maintain aseptic technique during insertion – Contaminated equipment – Wet/soiled dressing remaining on site – Failure to comply with dressing change protocol – Irritated suture line – Immunosuppression

INFECTION – Nursing interventions • Monitor temperature • Cultural site; central and peripheral blood cultures • Assess for other sources of infection • Redress aseptically; possibly with antibiotic ointment • Systemic antibiotics • Possible catheter removal; culture tip • Document

INFECTION • Prevention – Strict aseptic technique – Adhere to dressing protocols – Do tracheostomy care after catheter care – Examine solution to double check is clear – Keep system closed as much as possible – Teach patient aseptic technique

GERIATRIC PATIENTS • The aging process means many elderly patients have decreased functioning in several of their biological systems. • Be aware: – Administering IV analgesic observe for signs of resp depression or CNS depression, confusion – When giving a drug that can cause renal toxicity, monitor the patient closely

“WHAT DO YOU THINK? ” • When doing a venipuncture where should you place the tourniquet in proximity to the intended venipuncture site? • • A. B. C. D. About 2” above the venipuncture site About 12” above the venipuncture site Just above the venipuncture site About 6” above the venipuncture site

“WHAT DO YOU THINK? ” • Which of the following is a cause of thrombophlebitis? (may be more than 1 answer) – 1. – 2. – 3. – 4. Irritation of vein by catheter Infection Chemical irritation of medicines Slow rate of infusion – KVO (keep vein open)

THE END!!!
- Slides: 88