Intrapartum Physiology How the baby enters this world

Intrapartum Physiology How the baby enters this world

The 5 P’s of Labor n Passage • Birth canal n Passenger • Fetus n Powers • “Forces of labor” n Position • Fetal engagement and position n Psyche • Maternal behaviors

Passageway n n Passage (birth canal) consists of the pelvic inlet, midpelvis, and outlet The size and type of the passageway affects the labor and delivery process and outcome

n Four types of Passageway • Gynecoid n Adequate pelvic outlet n Round, slightly oval, 50% of women n Most favorable for delivery • Android n Normal male pelvis n Heart shaped, 20% of women n Not favorable for delivery • Higher risk of c-section, arrest of labor, forcep delivery • Anthropoid n 25% of women, narrow arch n Favorable for labor • Platypoid n Flat pelvis, 5% of women n Favorability for labor ? due to outlet capacity
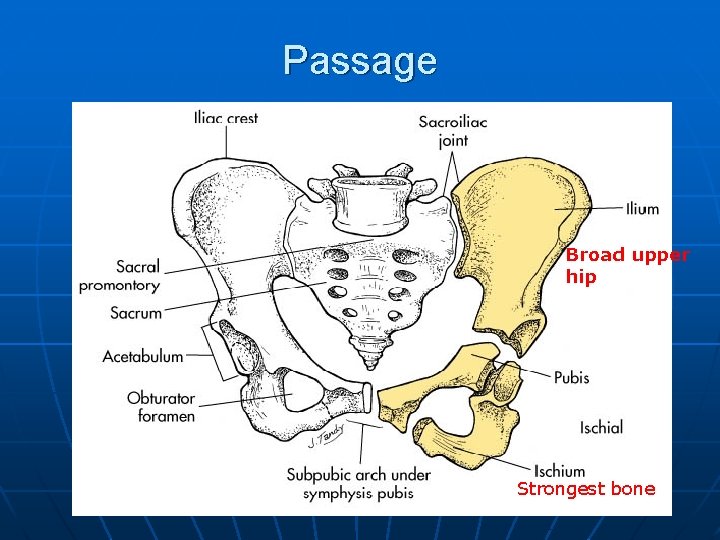
Passage Broad upper hip Strongest bone
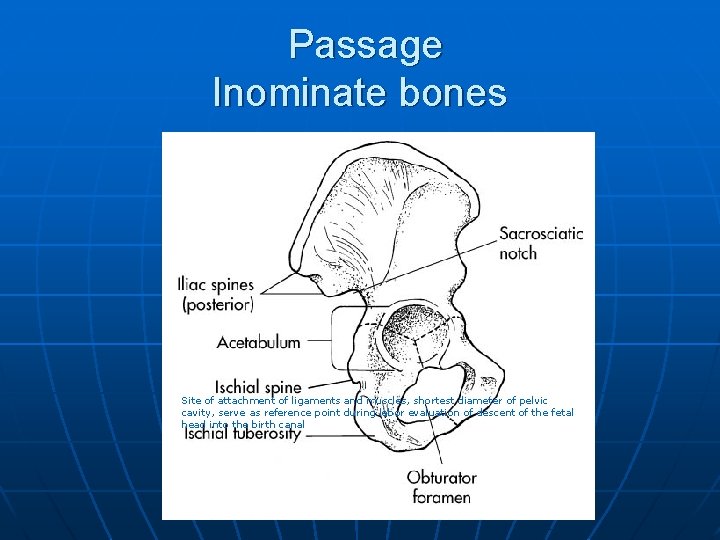
Passage Inominate bones Site of attachment of ligaments and muscles, shortest diameter of pelvic cavity, serve as reference point during labor evaluation of descent of the fetal head into the birth canal
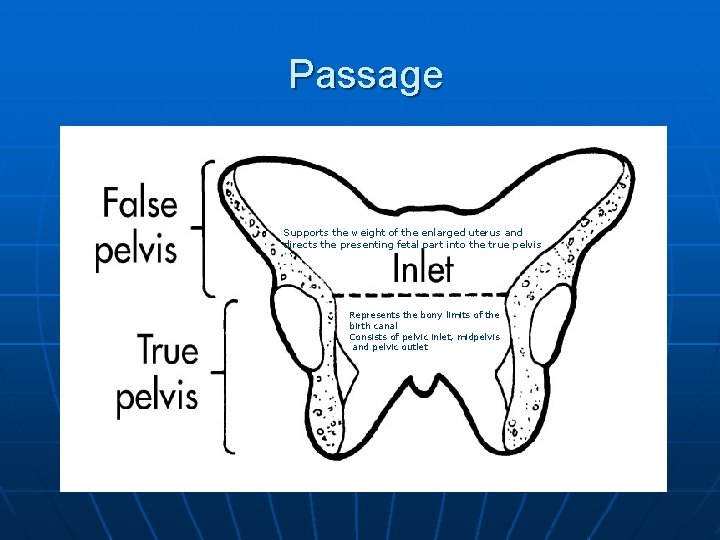
Passage Supports the weight of the enlarged uterus and directs the presenting fetal part into the true pelvis Represents the bony limits of the birth canal Consists of pelvic inlet, midpelvis and pelvic outlet
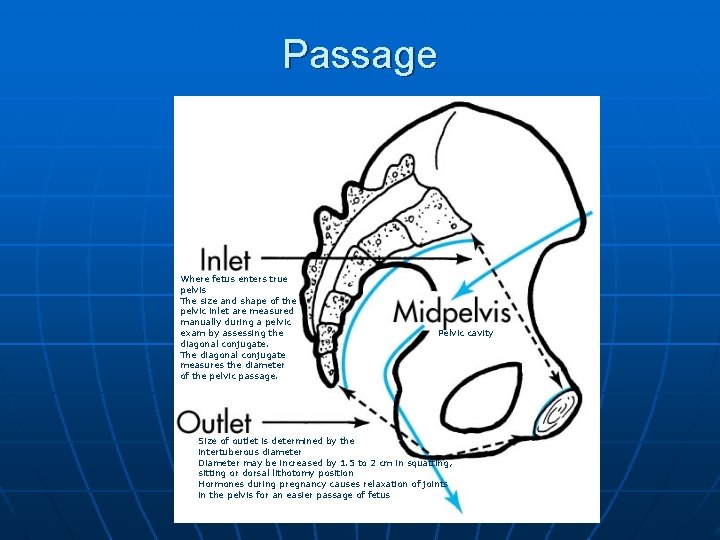
Passage Where fetus enters true pelvis The size and shape of the pelvic inlet are measured manually during a pelvic exam by assessing the diagonal conjugate. The diagonal conjugate measures the diameter of the pelvic passage. Pelvic cavity Size of outlet is determined by the intertuberous diameter Diameter may be increased by 1. 5 to 2 cm in squatting, sitting or dorsal lithotomy position Hormones during pregnancy causes relaxation of joints in the pelvis for an easier passage of fetus
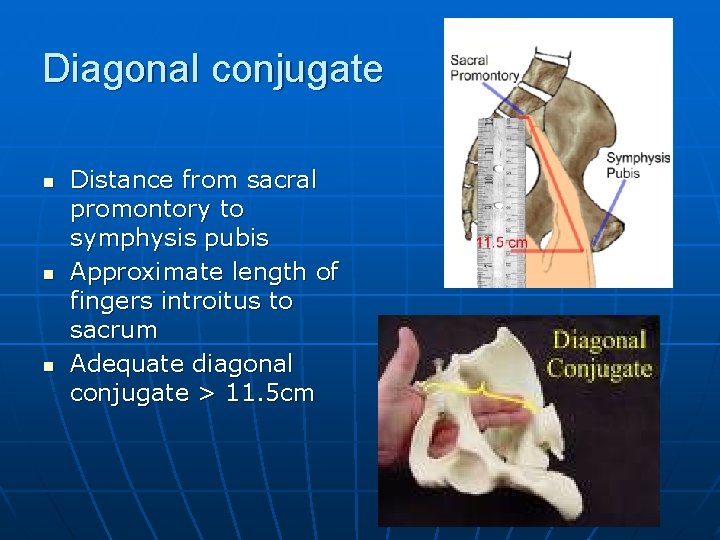
Diagonal conjugate n n n Distance from sacral promontory to symphysis pubis Approximate length of fingers introitus to sacrum Adequate diagonal conjugate > 11. 5 cm
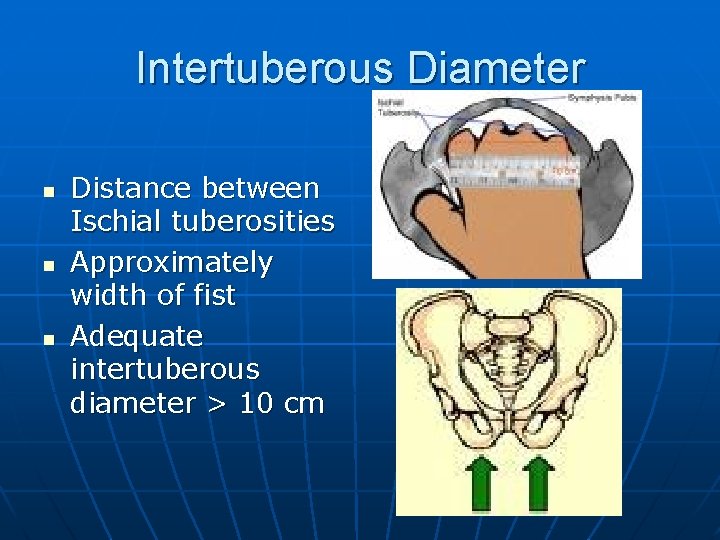
Intertuberous Diameter n n n Distance between Ischial tuberosities Approximately width of fist Adequate intertuberous diameter > 10 cm
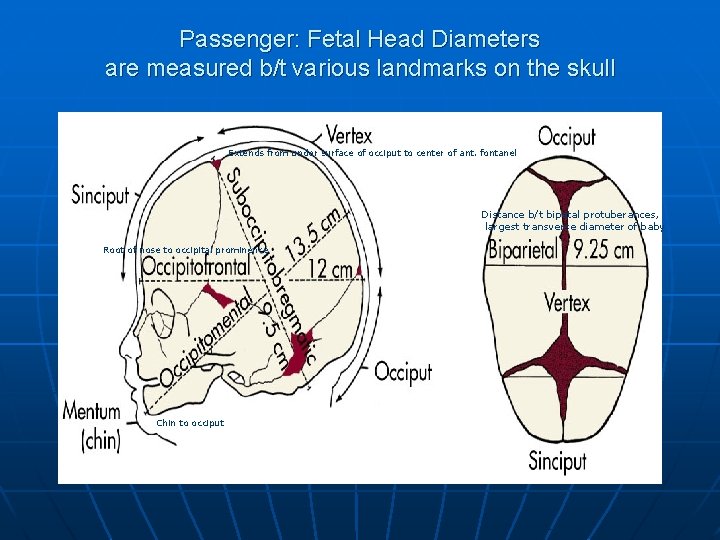
Passenger: Fetal Head Diameters are measured b/t various landmarks on the skull Extends from under surface of occiput to center of ant. fontanel Distance b/t bipatal protuberances, largest transverse diameter of baby Root of nose to occipital prominence Chin to occiput
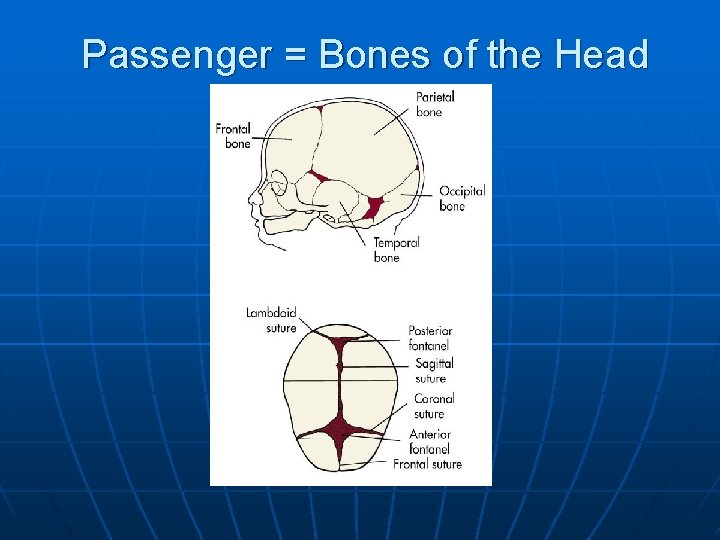
Passenger = Bones of the Head

Passenger n n Fetal skull consists of three major parts, face, cranium, and vault • Vault consists of 2 frontal bones, 2 parietal and the occipital bones (these are not fused) • Overlapping of these bones to allow for delivery is called molding Sutures are membranous joints that unite the cranial bones, sutures allow for molding of the fetal head and in identifying position of fetal head in the birth canal • Frontal suture b/t frontal bones • Saggital suture b/t parietal bones divides the skull into L and R halves, connects 2 fontanelles • Coronal suture b/t frontal and parietal • Lambdoidal suture located b/t parietal and occipital
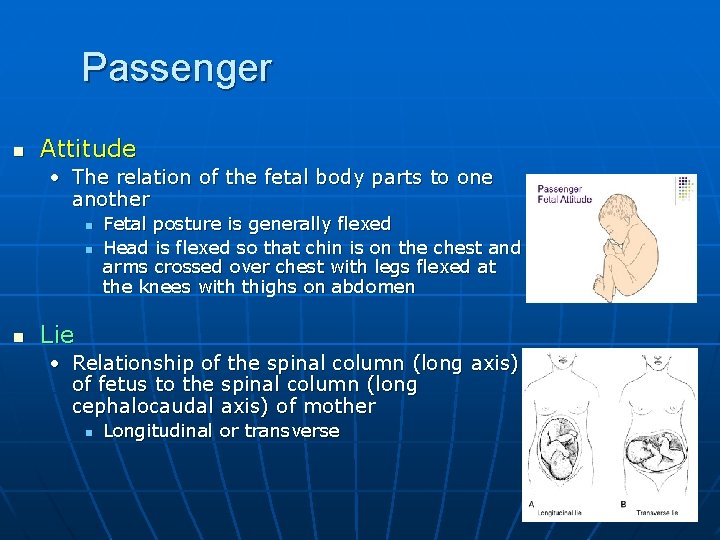
Passenger n Attitude • The relation of the fetal body parts to one another n n n Fetal posture is generally flexed Head is flexed so that chin is on the chest and arms crossed over chest with legs flexed at the knees with thighs on abdomen Lie • Relationship of the spinal column (long axis) of fetus to the spinal column (long cephalocaudal axis) of mother n Longitudinal or transverse
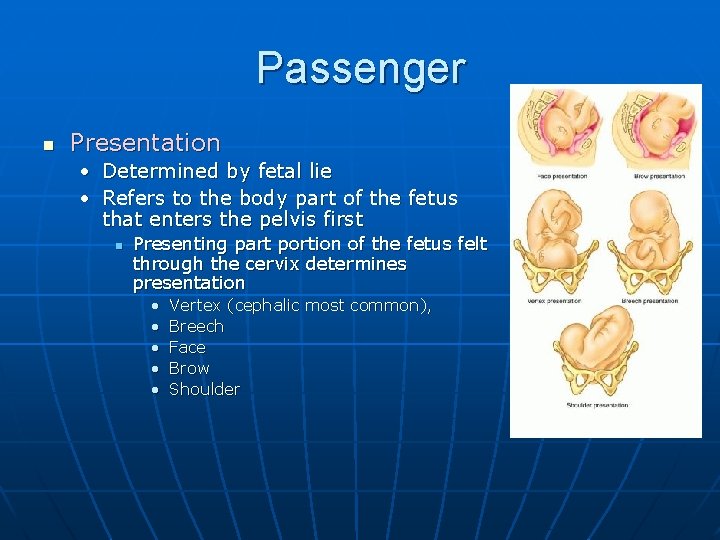
Passenger n Presentation • Determined by fetal lie • Refers to the body part of the fetus that enters the pelvis first n Presenting part portion of the fetus felt through the cervix determines presentation • • • Vertex (cephalic most common), Breech Face Brow Shoulder

n Descent Passenger • Assesses relationship of pelvis and presenting part n n Ballotable--Floating or freely movable above pelvic inlet Engagement of the presenting part occurs when the largest diameter of the presenting part passes through the pelvic inlet • Determined by VE, occurs 2 weeks before term • Multiparas may experience several weeks before term
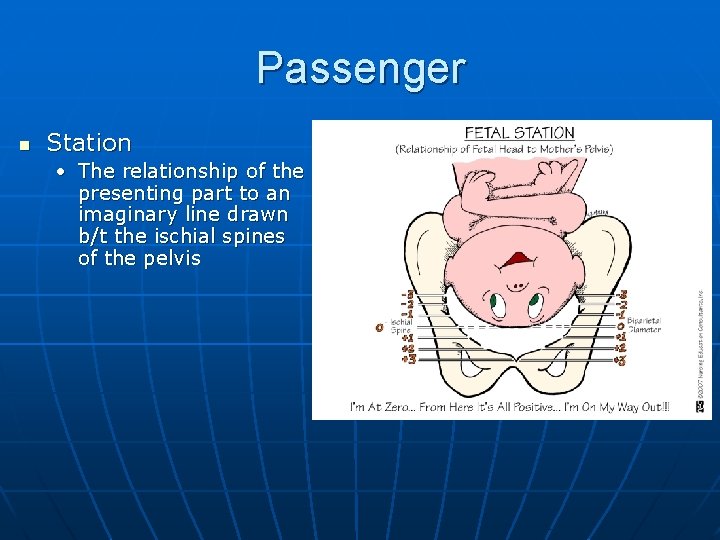
Passenger n Station • The relationship of the presenting part to an imaginary line drawn b/t the ischial spines of the pelvis

Fetal Position n Parts of notation • • • n Bony prominence Anterior or posterior Left or right side of maternal abdomen Bony parts presenting • Occiput (cephalic presentation, vertex) • Mentum (chin, face presentation, hyperextended fetal head) • Sacrum (breech) • Acromium process (shoulder presentation)

Passenger: Position n Position refers to the relationship of a landmark on the presenting fetal part to the anterior, posterior or sides left or right of pelvis. • Draw four imaginary quadrants left anterior, right anterior, left posterior and right posterior this designates where the presenting part is directed. Next note the n Landmarks n Occiput n Mentum n Sacrum n Acromion process
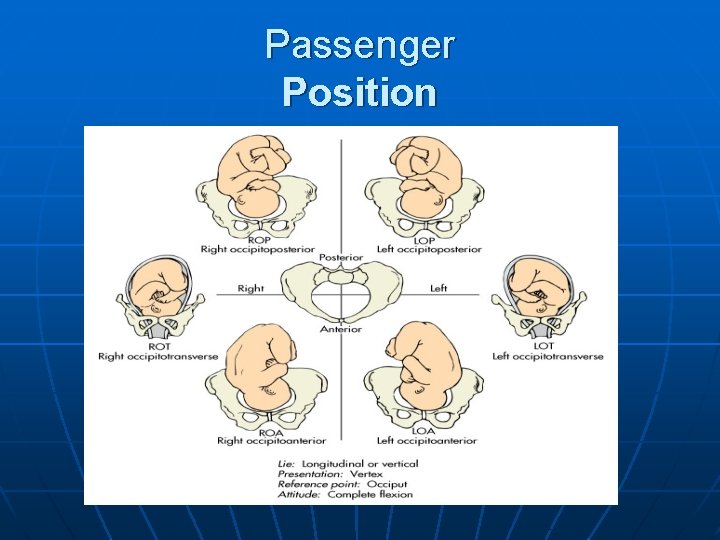
Passenger Position
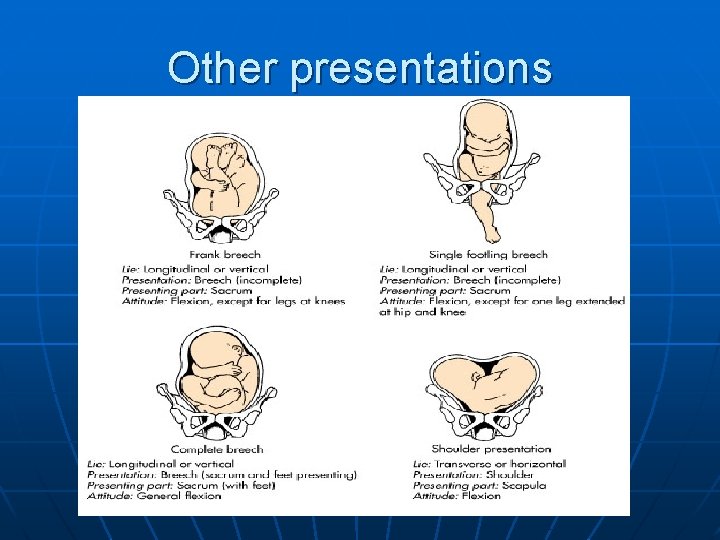
Other presentations
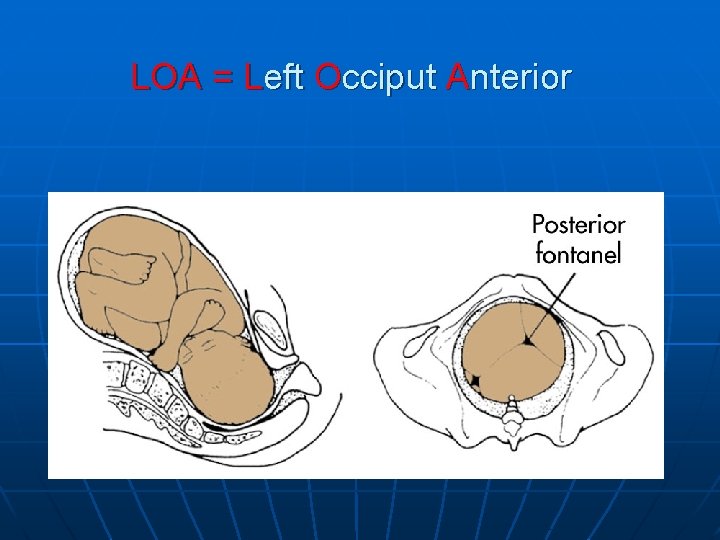
LOA = Left Occiput Anterior
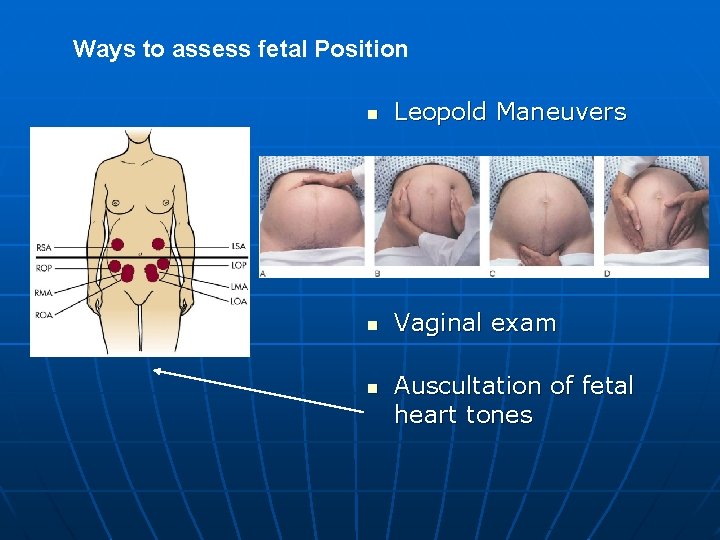
Ways to assess fetal Position n Leopold Maneuvers n Vaginal exam n Auscultation of fetal heart tones

Assessing Fetal Position n Leopold Maneuvers helps in assessing fetal heart tones • four assessment parameters n Fundal exam n Fetal exam (lie) n Pelvic palpation for vertex presentation n Position of fetal body Vaginal exam • Helps to determine presentation and position Auscultation of fetal heart tones • Heard best thru fetus back in vertex and breech position, heard thru chest in transverse lie

Powers—Phenomena of Labor n Causes of Labor unknown (several theories) • Progesterone theory n Progesterone produced by the placenta relaxes uterine smooth muscle by interfering with conduction of impulses from one cell to the next • By the end of pregnancy progesterone availability decreases this is associated with a yet unknown antiprogesten that inhibits the relaxant effect on the uterus • Oxytocin theory n Oxytocin stimulates uterine contractions by acting directly on the myometrium (increasingly sensitivity to oxytocin) and indirectly increases production of prostaglandins initiating labor

Powers—Phenomena of Labor • Fetal cortisol n Corticotropin releasing hormone (CRH) • CRH concentration increases throughout pregnancy with sharp increase at term gestation • CRH stimulates synthesis of prostoglandin F and E by amnion cells n Secretion of cortical steroids triggers mechanism of labor by slowing production of progesterone by the placenta and stimulates the release of prostoglandins • Prostaglandin n Acts on uterine muscle to initiate labor and can also stimulate oxytocin and the response to oxytocin

n Power—Uterine Contractions Parts of a contraction n • Primary force is uterine muscular contraction which causes the changes in the 1 st stage of labor n Uterine contractions are rhythmic tightenings and shortenings of the uterine muscles during labor • Each ctx has 3 phases n Increment-the building up (longest phase) n Acme (peak) n Decrement-the letting up n The relaxation b/t ctx restores uteroplacental circulation Duration n • Is measured from beginning of ctx to completion of ctx Frequency • Refers to the time b/t the beginnings of one ctx to the beginning of the next ctx

Power—Uterine Contractions n n n Intensity • Refers to the strength of the ctx during the acme of the ctx n Examined by palpation • Mild, moderate, or strong n Measured directly with IUPC External monitoring measures frequency and duration • Variables affecting external monitoring include maternal weight, and position of monitor Internal monitoring measures frequency, duration, and intensity

Stages of Labor n Duration of labor • Primipara—Gravida 1 (up to 20 hours total) n 1 st stage • Latent phase lasts 8. 6 hours • Active phase lasts 4. 6 hours • Transition lasts 3. 6 hours n 2 nd stage lasts up to 3 hours n 3 rd stage lasts 10 min • Multipara—>1 pregnancy (6 hours less than first pregnancy labor experience) n 1 st stage • Latent 5. 3 hours • Active 2. 4 hours • Transition variable n 2 nd stage 30 min to 0 min n 3 rd stage 3 min.

Stages of Labor n Terms related to labor • Effacement n The drawing up of the internal os of the cervical canal into the uterine side walls • The cervix changes progressively from a long and thick structure to a structure that is tissue or paper thin n Primip effacement usually preceeds dilation

Terms related to labor • Dilatation n Cervical os and cervical canal widen from < 1 cm to approx 10 cm allowing for delivery • The pt. is complete or 10 cm when the cervix is no longer palpable • Station n The ischial spines mark the narrowest diameter through which the fetus must pass. n The ischial spines are used as a landmark to establish a station of zero. n If the presenting part is higher than the ischial spines a negative number is assigned, beginning with -5 at the inlet of the pelvis and going through +4 at the outlet, moving from a negative station to zero to a positive station
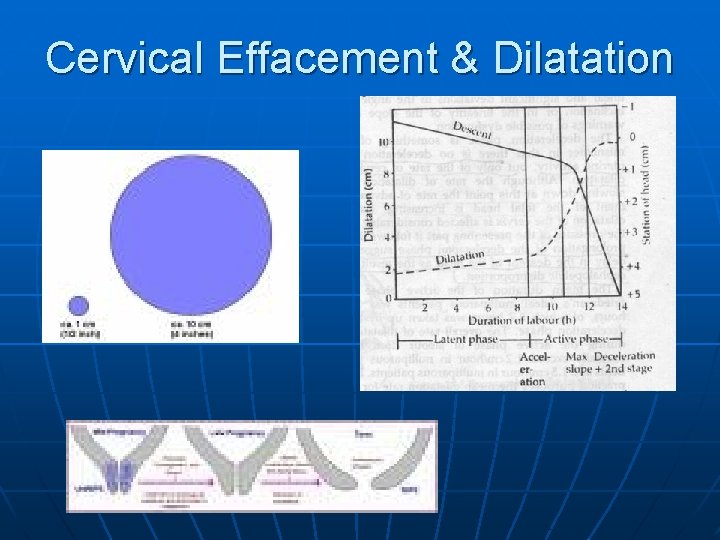
Cervical Effacement & Dilatation

Psyche n How is mom coping with labor? n What is her pain threshold? n What kind of support does she have? n What is her level of knowledge about the labor and delivery process?

Premonitory signs of Labor n What sx might mom exhibit that say labor is imminent? • Lightening (descent of fetal head into the pelvis) n n Primip 10 -14 days before delivery Multip during labor • Cervical ripening (the softening of the cervix) • Bloody show (pressure of baby on cervix causes microcapillaries to rupture) n Blood mixes with mucus • Braxton Hicks Contractions (ctx that do not cause cervical change) • SROM (gush of fluid collects in the vagina) • energy/nesting syndrome (24 -48 hours before labor) • Weight loss of 1 -3 kg (2. 2 -6. 6 lbs) • frequency of urination • diarrhea
True vs. False Labor (p. 541, Olds) True Contractions Cervix Fetus False

Stages of Labor n Stage 1 (closed complete) • Latent phase (0 3 cms) n Ctx every 5 -30 min, mom feels anxious excited n Ctx every 2 -5 min, mom focused on self n Ctx every 2 -3 min, mom is irritable, feels urge to push • Active phase (4 7 cms) • Transition phase (8 10 cms) n Stage 2 (complete birth) • Expulsion stage, baby crowns, stronger urge to push, feels good to push n Stage 3 (birth placenta) • Placental stage n n Rise of uterus in abdomen descent of cord outside vagina, sudden gush of blood, takes 5 -30 min. Stage 4 (recovery phase 1 hr p birth) • Blood loss 250 -500 cc • Potential time for post partum hemorrhage, assess vitals, lochia and fundal height every 15 min, then 30 min x 2, then 60 min x 2.

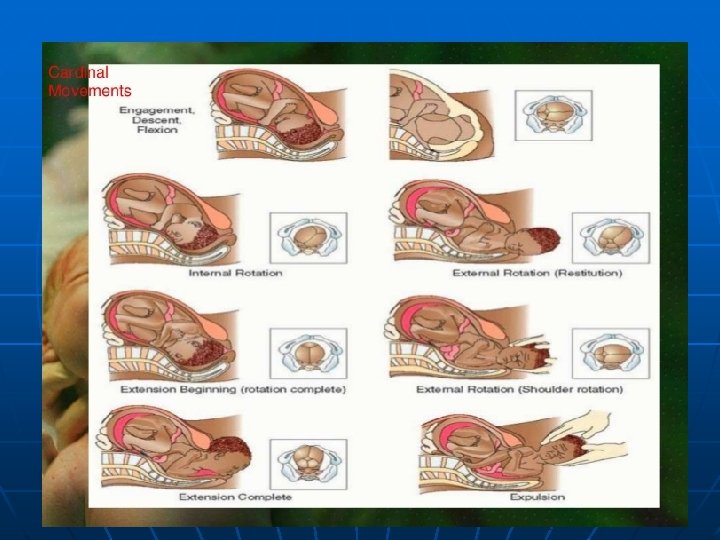
Mechanisms of Labor n also known as Cardinal Movements (pp. 458 -462; 10 th edition) Engagement & descent • 4 forces n n n Pressure of amniotic fluid Direct pressure of the fundus of the uterus on the breech of the fetus Contraction of the abdominal muscles Extension and straightening of the fetal body Flexion • Fetal head meets resistance from pelvic floor causing chin to flex downward to chest n Internal rotation to OA position • Head rotates to fit pelvic cavity by rotating the occiput from left to right and sagittal sutures align with the anteriorposterior pelvic diameter.

Mechanisms of Labor also known as Cardinal Movements n Extension • Crowing occurs as the fetal head meets resistance from pelvic floor allowing fetal head to pass under symphysis pubis n Restitution • neck is twisted (b/c of internal rotation) once free turns head to one side n External rotation • Shoulders in anteroposterior position, the head is turned farther to one side to assist in birth n Expulsion • After external rotation the anterior shoulder meets the undersurface of pubis and slips under, shoulders are born then body.

Systemic Response to Labor n Cardiac output 10 -15% in 1 st stage, 30 -50% in 2 nd stage • Position change affects co, side lying increases co by 22% n n n BP: systolic during contraction in 1 st stage; systolic & diastolic during contractions in 2 nd stage WBC 25 -30000 during labor due to increase in neutrophils resulting from a physiologic response to stress Respiratory rate due to increase in oxygen demand consumption • Metabolic acidosis uncompensated by resp. alkalosis occurs b/c of pushing (balance is reversed in 4 th stage)

Systemic response (cont’d) n n Temperature may slightly, especially if pt. is dehydrated. Proteinuria of 1+ may occur • Occurs in 1/3 of women in labor n Gastric motility is • Emptying is delayed (risk for aspiration)

Causes of Pain in Labor n First stage • Pain arises from dilation and stretching of cervix • Hypoxia of uterine muscle cell during ctx • Stretching of the lower uterine segment • Pressure on adjacent structures n Second Stage • • Hypoxia on contracting uterine muscle cells Distention of the vagina and perineum Pressure on back, buttocks, thighs Pudendal nerve transmits nerve impulses for pain
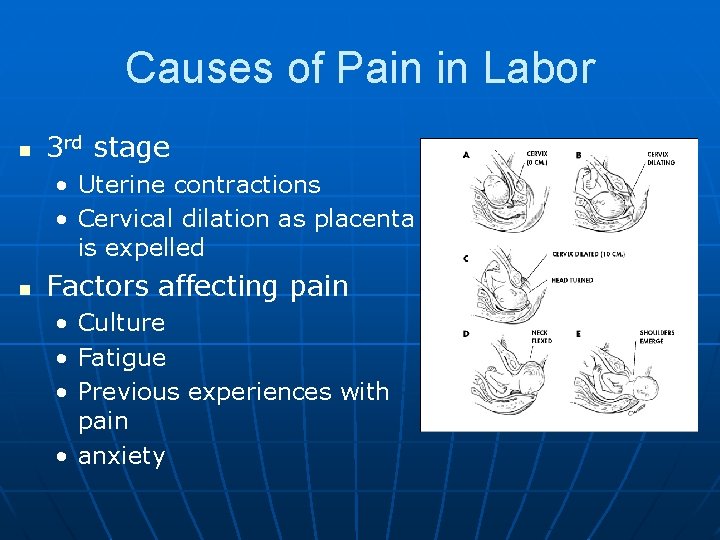
Causes of Pain in Labor n 3 rd stage • Uterine contractions • Cervical dilation as placenta is expelled n Factors affecting pain • Culture • Fatigue • Previous experiences with pain • anxiety

Every new birth is truly a miracle!
- Slides: 44