Intracranial Pressure Chapter 57 Copyright 2014 by Mosby

Intracranial Pressure Chapter 57 Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Case Study • A. T. is a 68 -year-old male brought to the ED with confusion, lethargy, and headache. • He was in a car accident 2 days ago where he hit his head on the windshield. Creatas Images/Creatas/Thinkstock Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Case Study Creatas Images/Creatas/Thinkstock • He felt fine at the time and did not seek medical care. Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Case Study Creatas Images/Creatas/Thinkstock • The health care provider suspects A. T. ’s symptoms may be caused by increased intracranial pressure (ICP). • What causes increased ICP? Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
Intracranial Pressure • Skull has three essential components: 1. Brain tissue 2. Blood 3. Cerebrospinal fluid (CSF) Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
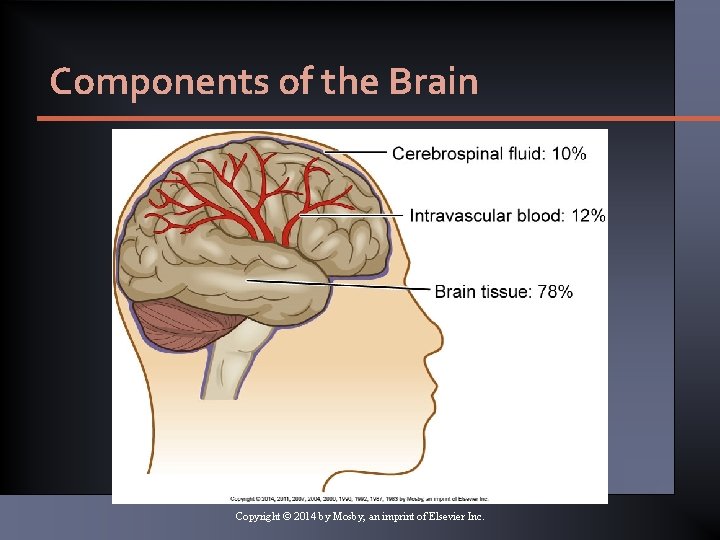
Components of the Brain Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
Intracranial Pressure • Factors that influence ICP • Arterial pressure • Venous pressure • Intraabdominal and intrathoracic pressure • Posture • Temperature • Blood gases (CO 2 levels) Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Regulation and Maintenance • Monro-Kellie doctrine • If one component increases, another must decrease to maintain ICP. • Normal ICP 5 to 15 mm Hg • Elevated if >20 mm Hg sustained Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Case Study Creatas Images/Creatas/Thinkstock • What compensatory mechanisms may have been at work in A. T. ’s body over the last few days in response to increased ICP? Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Regulation and Maintenance • Normal compensatory adaptations • Changes in CSF volume • Changes in intracranial blood volume • Changes in tissue brain volume • Ability to compensate is limited. • If volume increase continues, ICP rises → decompensation Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
Cerebral Blood Flow • Definition • The amount of blood in milliliters passing through 100 g of brain tissue in 1 minute • About 50 m. L/min per 100 g of brain tissue Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
Cerebral Blood Flow • Autoregulation • Adjusts diameter of blood vessels • Ensures consistent CBF • Only effective if mean arterial pressure (MAP) 70 to 150 mm Hg Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
Cerebral Blood Flow • Cerebral perfusion pressure (CPP) • CPP = MAP – ICP • Normal is 60 to 100 mm Hg. • <50 mm Hg is associated with ischemia and neuronal death. • Effect of cerebral vascular resistance • CPP = Flow x Resistance Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
Cerebral Blood Flow • Pressure changes • Compliance is the expandability of the brain. • Impacts effect of volume change on pressure • Compliance = Volume/Pressure Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
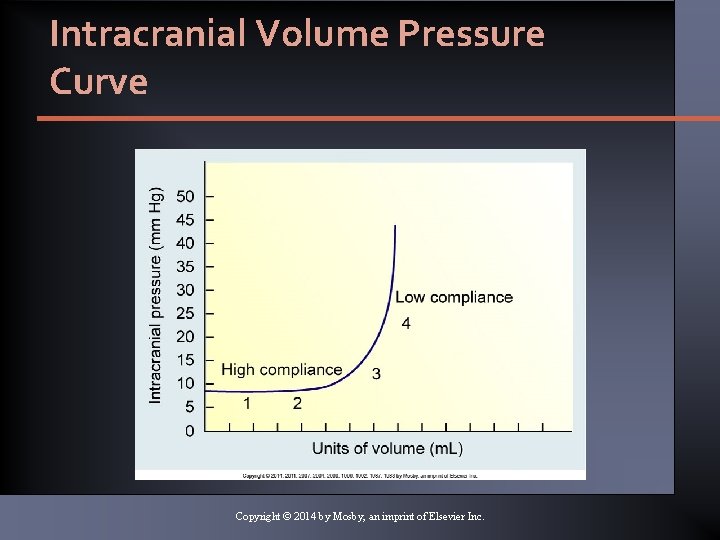
Intracranial Volume Pressure Curve Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Case Study Creatas Images/Creatas/Thinkstock • A. T. ’s BP is 144/54 mm Hg, HR 76 bpm, RR 12 breaths/minute, and Temp 98. 9 F. • His CT scan reveals a subacute subdural hematoma. • What stage of increased ICP is A. T. displaying? Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
Cerebral Blood Flow • Stages of increased ICP • Stage 1: total compensation • Stage 2: ↓compensation; risk for ↑ICP , • Stage 3: failing compensation; clinical manifestations of ↑ICP (Cushing’s triad) • Stage 4: Herniation imminent → death Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
Cerebral Blood Flow • Factors affecting cerebral blood vessel tone • CO 2 • Hydrogen ion concentration Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
Increased ICP • Life-threatening • Increase in any of three components • Brain tissue • Blood • CSF • ↑ cerebral edema Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Increased Intracranial Pressure Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
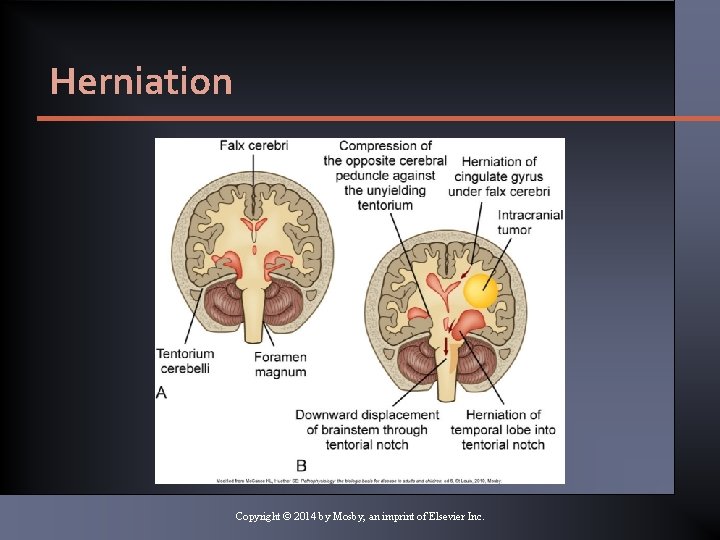
Herniation Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Cerebral Edema • ↑ Extravascular fluid in brain • Variety of causes • Three types of cerebral edema 1. Vasogenic 2. Cytotoxic 3. Interstitial Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Cerebral Edema • Vasogenic cerebral edema • Most common type • Occurs mainly in white matter • Fluid leaks from intravascular to extravascular space. • Variety of causes • Continuum of symptoms → coma Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Cerebral Edema • Cytotoxic cerebral edema • Disruption of cell membrane integrity • Secondary to destructive lesions or trauma to brain tissue • Fluid shift from extracellular to intracellular Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Cerebral Edema • Interstitial cerebral edema • Usually result of hydrocephalus • Excess CSP production, obstruction of flow, or inability to reabsorb • Treat with ventriculostomy or shunt Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Case Study • For what additional clinical manifestations will you assess A. T. ? Creatas Images/Creatas/Thinkstock Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Clinical Manifestations • Change in level of consciousness • Change in vital signs • Cushing’s triad • Ocular signs Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Clinical Manifestations • Change in level of consciousness • Flattening of affect → coma • Change in vital signs • Cushing’s triad (widened pulse pressure, bradycardia, irregular respirations) • Change in body temperature Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Clinical Manifestations • Compression of oculomotor nerve • Unilateral pupil dilation • Sluggish or no response to light • Inability to move eye upward • Eyelid ptosis Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Clinical Manifestations • Other cranial nerves • Diploplia, blurred vision, EOM changes Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Clinical Manifestations • ↓ In motor function • Hemiparesis/hemiplegia • Decerebrate posturing (extensor) • Indicates more serious damage • Decorticate posturing (flexor) Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Decorticate and Decerebrate Posturing Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Clinical Manifestations • Headache • Often continuous • Worse in the morning • Vomiting • Not preceded by nausea • Projectile Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
Complications • Inadequate cerebral perfusion • Cerebral herniation • Tentorial herniation • Uncal herniation • Cingulate herniation Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Diagnostic Studies • CT scan / MRI / PET • EEG • Cerebral angiography • ICP and brain tissue oxygenation measurement (LICOX catheter) • Doppler and evoked potential studies • NO lumbar puncture Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Measurement of ICP • Guides clinical care • Indications • Glasgow Coma Scale of ≤ 8 • Abnormal CT scans or MRI Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Case Study Creatas Images/Creatas/Thinkstock • A. T. ’s health care provider decides to insert a device to measure and monitor his ICP levels. • What types of monitoring devices are used to measure ICP? Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
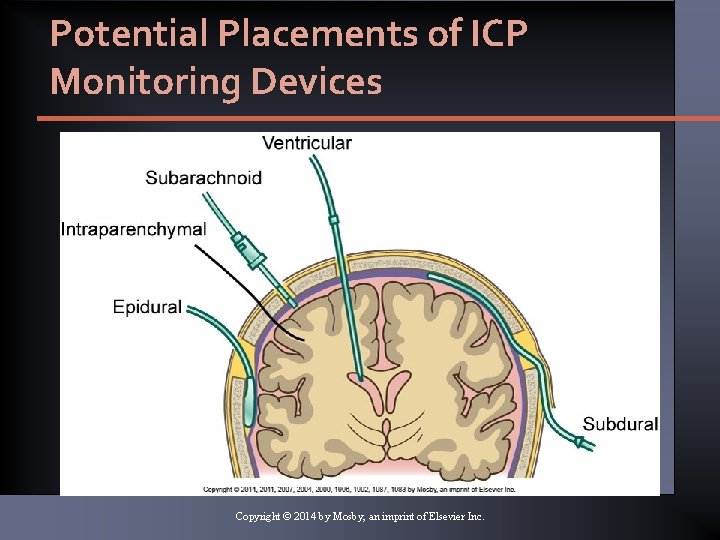
Potential Placements of ICP Monitoring Devices Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Measurement of ICP • Ventriculostomy • Catheter inserted into lateral ventricle • Coupled with an external transducer Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
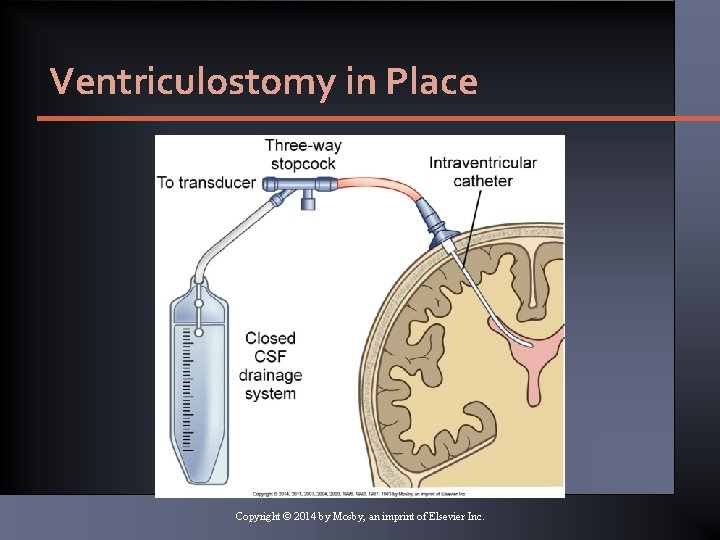
Ventriculostomy in Place Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
Leveling a Ventriculostomy Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Measurement of ICP • Fiberoptic catheter • Sensor transducer located within the catheter tip • Subarachnoid bolt or screw • Between arachnoid membrane and cerebral cortex Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Measurement of ICP • Prevent and monitor for infection. • Measure as mean pressure. • Waveform should be recorded. • Normal, elevated, and plateau waves Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
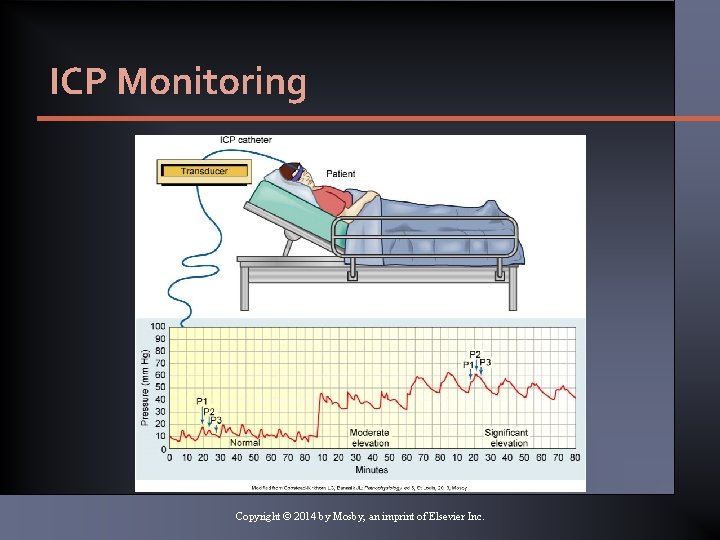
ICP Monitoring Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
Measurement of ICP • Evaluate changes with patient condition. • Inaccurate readings caused by • • • CSF leaks Obstruction in catheter/ kinks in tubing Differences in height of bolt/transducer Incorrect height of drainage system Bubbles/air in tubing Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Measurement of ICP • Can control ICP by removing CSF (with ventricular catheter). • Intermittent or continuous drainage • Careful monitoring of the volume of CSF drained is essential. • Prevent infection and other complications. Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
Measurement of Cerebral Oxygenation and Perfusion • LICOX catheter • Measures brain oxygenation (Pbt. O 2) and temperature. • Placed in healthy white brain matter. • Jugular venous bulb catheter • Measures jugular venous oxygen saturation (Sjv. O 2). Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

LICOX Catheter Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
Collaborative Care • Treat underlying cause. • Adequate oxygenation • Pa. O 2 > 100 mm Hg • Pa. CO 2 35 -45 mm Hg • Intubation • Mechanical ventilation • Surgery Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Case Study Creatas Images/Creatas/Thinkstock • A. T. undergoes a craniotomy with burr holes to evacuate his hematoma. • He returns to the ICU with a venticulostomy in place. Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Case Study Creatas Images/Creatas/Thinkstock • Although his ICP is currently stable, you review potential drug therapies that could be used if his ICP rises again. Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Case Study • Name five classifications of drugs that might be used to treat increased intracranial pressure. Creatas Images/Creatas/Thinkstock Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Collaborative Care • Drug Therapy • Mannitol (Osmitrol) • Plasma expansion • Osmotic effect • Monitor fluid and electrolyte status. • Hypertonic saline • Moves water out of cells and into blood. • Monitor BP and serum sodium levels. Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Collaborative Care • Drug Therapy • Corticosteroids • Vasogenic edema • Monitor fluid intake, serum sodium and glucose levels. • Concurrent antacids, H 2 receptor blockers, proton pump inhibitors Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Collaborative Care • Drug Therapy • Antiseizure medications • Antipyretics • Sedatives • Analgesics • Barbiturates Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Collaborative Care • Nutritional Therapy • Hypermetabolic and hypercatabolic state ↑ need for glucose • Enteral or parenteral nutrition • Early feeding (within 3 days of injury) • Keep patient normovolemic. • IV 0. 9% Na. Cl preferred over D 5 W or 0. 45% Na. Cl Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Case Study • How would you monitor A. T. ’s neurologic status postoperatively? Copyright © 2014 by Mosby, an imprint of Elsevier Inc. Creatas Images/Creatas/Thinkstock

Nursing Assessment • Subjective data • Level of consciousness (LOC) • Glasgow Coma Scale • Eye opening • Best verbal response • Best motor response Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Pupillary Check for Size and Response Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Assessment • Cranial nerves • Eye movements • Corneal reflex • Oculocephalic reflex (doll’s eye reflex) • Oculovestibular (caloric stimulation) Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Assessment • Motor strength • Squeeze hands • Palmar drift test • Raise foot off bed or bend knees • Motor response • Spontaneous or to pain • Vital signs Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
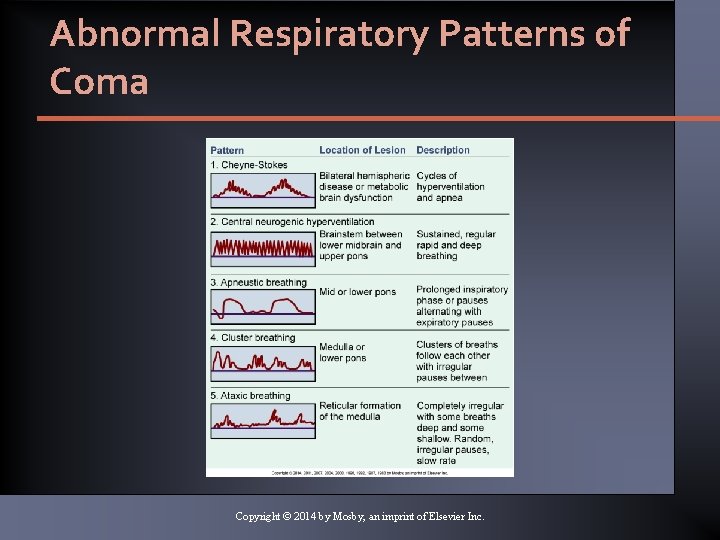
Abnormal Respiratory Patterns of Coma Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Case Study Creatas Images/Creatas/Thinkstock • What would be some priority nursing diagnoses for A. T. ? Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Diagnosis • Decreased intracranial adaptive capacity • Risk for ineffective cerebral tissue perfusion • Risk for disuse syndrome Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Planning • Overall Goals • Maintain a patent airway. • ICP within normal limits • Normal fluid and electrolyte balance • Prevent complications secondary to immobility and decreased LOC. Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Implementation • Respiratory function • Maintain patent airway. • Elevate head of bed 30 degrees. • Suctioning needs • Minimize abdominal distention. • Monitor ABGs. • Maintain ventilatory support. Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Implementation • Pain and anxiety management • Opioids • Propofol (Diprivan) • Dexmedetomidine (Precedex) • Neuromuscular blocking agents • Benzodiazepines Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Implementation • Fluid and electrolyte balance • Monitor IV fluids. • Daily electrolytes • Monitor for DI or SIADH. • Monitor and minimize increases in ICP. Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Case Study Creatas Images/Creatas/Thinkstock • What nursing measures can you use to prevent further increases in A. T. ’s ICP? Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Implementation • Interventions to optimize ICP and CPP • HOB elevated appropriately • Prevent extreme neck flexion. • Turn slowly. • Avoid coughing, straining, Valsalva. • Avoid hip flexion. Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Case Study • A. T. continues to be somewhat confused even after evacuation of his subdural hematoma. • What nursing interventions would be appropriate to prevent further injury? Creatas Images/Creatas/Thinkstock Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Implementation • Minimize complications of immobility. • Protection from self-injury • Judicious use of restraints; sedatives • Seizure precautions • Quiet, nonstimulating environment • Psychologic considerations Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Evaluation • Expected Outcomes • Maintain ICP and CPP within normal parameters. • No serious increases in ICP during or following care activities • No complications of immobility Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Audience Response Question A patient with a head injury has an arterial BP of 92/50 mm Hg and ICP of 18 mm Hg. The nurse uses the assessments to calculate the cerebral perfusion pressure (CPP). How should the nurse interpret the results? a. b. c. d. The CPP is so low that brain death is imminent. The CPP is low, and the BP should be increased. The CPP is high, and the ICP should be reduced. The CPP is adequate for normal cerebral blood flow. Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Audience Response Question A patient with increased ICP is positioned in a lateral position with the head of the bed elevated 30 degrees. The nurse evaluates a need for lowering the head of the bed when the patient experiences a. b. c. d. ptosis of the eyelid. unexpected vomiting. a decrease in motor functions. decreasing level of consciousness. Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
- Slides: 75