Intra Uterine Growth Retardation Dr B Khani MD

Intra Uterine Growth Retardation Dr. B Khani MD

Case 1 v 27 Y G 2 L 1 36 w CC: VB & LP PMH: Iron deficiency anemia (no treatment) Spotting in 24 w pregnancy v PH: The patient was pale FH: 32 cm V /E: 4 cm The newborn birthed after 3 h v N: female APGAR: 7/10 & 8/10 (1′ & 5′) v BW: 1590 g HC: 29. 5 cm Height: 45 cm v DX: IUGR The newborn was Hospitalized and managed v BS was normal HB: 23. 9 After 2 days bilirubin was 16 and phototherapy was started CXR: normal blood culture: WNL v After one Week the infant was discharged 12 October 2002 IUGR - Prof. S. N. Panda 2

Intra Uterine Growth Retardation n Intra Uterine Growth Restriction n Small for gestational age (SGA) n Foetal growth restriction n 'wasted' and 'stunted' Please also see notes pages for more details in most of the slides 12 October 2002 IUGR - Prof. S. N. Panda 3

Definition v Intrauterine growth retardation (IUGR) occurs when the unborn baby is at or below the 10 th weight percentile for his or her age (in weeks). The foetus is affected by a pathologic restriction in its ability to grow. n Low birth weight (LBW) means a baby with a birth weight of less than 2500 Gms, which could be due to IUGR or Prematurity Please also see notes pages for more details in most of the slides 12 October 2002 IUGR - Prof. S. N. Panda 4
Classification Symmetricl the baby's head and body are proportionately small. may occur when the foetus experiences a problem during early development. Asymmetrical baby's brain is abnormally large when compared to the liver. may occur when the foetus experiences a problem during later development In a normal infant, the brain weighs about three times more than the liver. In asymmetrical IUGR, the brain can weigh five or six times more than the liver. 12 October 2002 IUGR - Prof. S. N. Panda 5

Classification Newer Classification: 1. Normal small fetuses- have no structural abnormality, normal umbilical artery & liquor but wt. , is less. They are not at risk and do not need any special care. 2. Abnormal small fetuses- have chromosomal anomalies or structural malformations. They are lost cases and deserve termination as nothing can be done. 3. Growth restricted fetuses- are due to impaired placental function. Appropriate & timely treatment or termination can improve prospects. 12 October 2002 IUGR - Prof. S. N. Panda 6

Aetiology v The foetal growth is dependent on multiple factors. v IUGR resulting in SGA babies can result from many factors known and unknown either acting alone or in conjunction or in association. v The aetiologic determinants of IUGR have two measures of effect: relative risk and etiologic fraction. v Most of the evidence on aetiologic determinants is based on observational studies and systematic overviews or meta-analyses of such studies. v In a majority of cases (40%) the cause is unknown– probably due to placental insufficiency (idiopathic). 12 October 2002 IUGR - Prof. S. N. Panda 7

Aetiology 1. General- Racial / Ethnic origin, Small maternal / paternal height / weight, Foetal sex. 2. 3. 4. 5. Maternal causes. Foetal causes. Placental causes. Idiopathic- In a majority of cases (40%) the cause is unknown– probably due to placental insufficiency. 12 October 2002 IUGR - Prof. S. N. Panda 8

Maternal Risk Factors v v Has had a previous baby who suffered from IUGR. Extremes of age. Is small in size (Ht & Wt). Has poor weight gain and malnutrition during pregnancy. v Is socially deprived. v Uses substances (like tobacco, narcotics, alcohol) that can cause abnormal development or birth defects. v Has a low total blood volume during early pregnancy. 12 October 2002 IUGR - Prof. S. N. Panda 9

Maternal Risk Factors v v v v Is pregnant with more than one baby. High altitude. Drugs like anticoagulants, anticonvulsants. Has a cardio-vascular disease-preeclampsia, hypertension, cyanotic heart disease, cardiac disease Gr III & IV, diabetic vascular lesions. Chronic kidney disease Chronic infection- UTI, Malaria, TB, genital infections Has an antibody problem that can make successful pregnancy difficult (antiphospholipid antibody syndrome, SLE). 12 October 2002 IUGR - Prof. S. N. Panda 10

Fetal Risk Factors v Exposure to an infection-German measles (rubella), cytomegalovirus, herpes simplex, tuberculosis, syphilis, or toxoplasmosis, TB, Malaria, Parvo virus B 19. v A birth defect (cardiovascular, renal, anencephally, limb defect, etc). v A chromosome defect- trisomy-18 (Edwards’ syndrome), 21(Down’s syndrome), 16, 13, xo (turner’s syndrome. v A primary disorder of bone or cartilage. v A chronic lack of oxygen during development (hypoxia). v Developed outside of the uterus. v Placenta or umbilical cord defects. 12 October 2002 IUGR - Prof. S. N. Panda 11

Placental Factors v Uteroplacental insufficiency resulting from -. § Improper / inadequate trophoblastic invasion and placentation in the first trimester. § Lateral insertion of placenta. § Reduced maternal blood flow to the placental bed. v Foetoplacetal insufficiency due to-. § Vascular anomalies of placenta and cord. § Decreased placental functioning mass-. » Small placenta, abruptio placenta, placenta previa, post term pregnancy. 12 October 2002 IUGR - Prof. S. N. Panda 12

Diagnosis Intrauterine v IUGR can be difficult to diagnose. v Presence of risk factors. v Inadequate growth detected by serial measurement of Wt. , abdominal girth and fundal Ht. v Ultrasound to evaluate the foetal growth. § Inadequate foetal growth. § Reduced AFI. § Placental calcification. 12 October 2002 IUGR - Prof. S. N. Panda 13

Diagnosis Neonatal v Low ponderal index (Wt. /Fl). v Decreased subcutaneous fat. v Presence / appearance of – § Hypoglycemia, § Hyperbilirubinemia, § Narcotizing enterocolitis, § Hyper viscosity syndrome 12 October 2002 IUGR - Prof. S. N. Panda 14

Neonate and Placenta in IUGR v Normal & IUGR Newborn babies v Normal & IUGR Placentas 12 October 2002 IUGR - Prof. S. N. Panda 15

Prevention v Strategies include § prenatal care modalities, § protein/energy supplementation, § treatment of anaemia, § vitamin/mineral supplementation, § fish oil supplementation § prevention and treatment of » hypertensive disorders, » foetal compromise » infection. 12 October 2002 IUGR - Prof. S. N. Panda 16

Prevention v Strong evidence of benefit only for the following interventions: § balanced protein/energy supplementation, § strategies to reduce maternal smoking, § antibiotic administration to prevent urinary tract infections and § antimalarial prophylaxis. v Few statistically significant reductions in the risk of IUGR have been demonstrated with other interventions. 12 October 2002 IUGR - Prof. S. N. Panda 17

Surveillance v Unless delivery occurs, once treatment begins the foetus must undergo surveillance. v The purpose - to identify further progression of the disease process that would jeopardize the foetus to a point that it would be better to be delivered than to remain in utero. v There are four testing modalities which are helpful -Non-Stress Test, Amniotic Fluid Index, Doppler of the Umbilical Artery & Biophysical Profile, each of which addresses different aspects of surveillance. v Combination of tests are better than an isolated test. 12 October 2002 IUGR - Prof. S. N. Panda 18

Surveillance n Non- Stress Test (NST) This simplest to perform test should b used first in the surveillance of IUGR foetuses. With the help of a heart rate monitor, the changes in the foetal heart rate with foetal movement are to be determined. If the heart rate increases more than 15 beats for more than 15 seconds, this is considered to be a reactive test. If the heart rate does not accelerate, remains flat, or decreases, then this is an abnormal test. The problem with this test is that it changes late in the course of the disease and is not an early predictor of adverse outcome. 12 October 2002 IUGR - Prof. S. N. Panda 19

Surveillance n Amniotic Fluid Index (AFI) The vertical depth of four pockets of amniotic fluid are measured by USG, to obtain a total AFI. This method allows for comparison of changes in amniotic fluid with time. In the normal foetus the AFI remains relatively constant. In the foetus with IUGR, it may decrease slowly, or decrease abruptly with time. A decrease in AFI may occur before there are changes in the non-stress test. 12 October 2002 IUGR - Prof. S. N. Panda 20
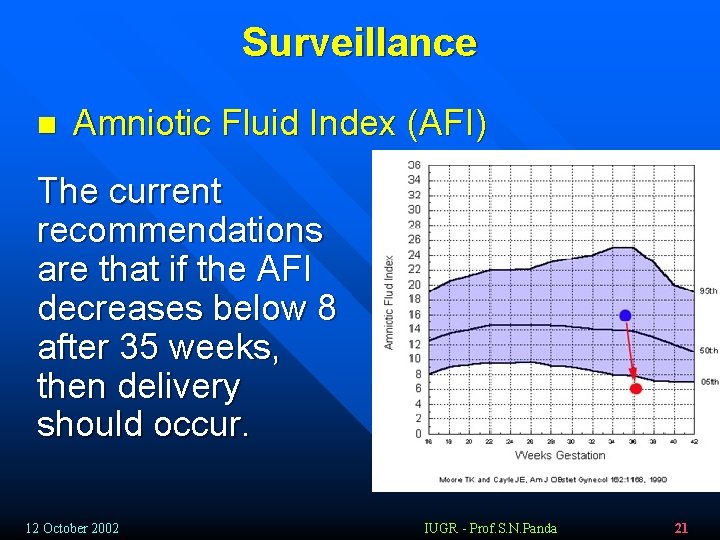
Surveillance n Amniotic Fluid Index (AFI) The current recommendations are that if the AFI decreases below 8 after 35 weeks, then delivery should occur. 12 October 2002 IUGR - Prof. S. N. Panda 21
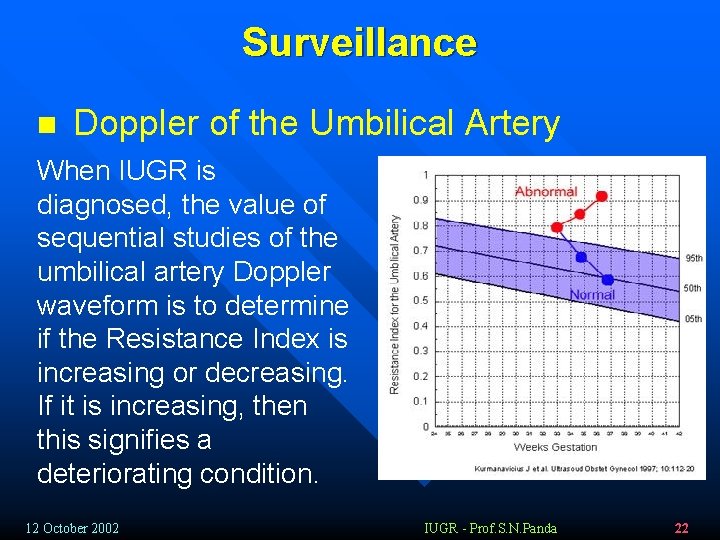
Surveillance n Doppler of the Umbilical Artery When IUGR is diagnosed, the value of sequential studies of the umbilical artery Doppler waveform is to determine if the Resistance Index is increasing or decreasing. If it is increasing, then this signifies a deteriorating condition. 12 October 2002 IUGR - Prof. S. N. Panda 22

Surveillance n Biophysical Profile v This test combines the NST and the AFI with foetal movement, breathing, and muscle tone. § If each of the tests are normal they are given a score of 2. If abnormal, a score of 0. § A score of 6 or less suggests the foetus is at risk for adverse outcome. v While the biophysical profile is an useful test, when it becomes abnormal the foetus may have already suffered some damage 12 October 2002 IUGR - Prof. S. N. Panda 23

Treatment n IUGR has many causes, therefore, there is not one treatment that always works. 12 October 2002 IUGR - Prof. S. N. Panda 24

Treatment v Although there are many causes of IUGR, the treatment consists of either delivery or remaining in utero and improving blood flow to the uterus. v When blood flow is improved, the delivery of oxygen and other nutrients to the foetus occurs. If the foetus is lacking in these substances, their increased availability may result in improved growth and development. v If IUGR is caused by a problem with the placenta and the baby is otherwise healthy, early diagnosis and treatment of the problem may reduce the chance of a serious outcome. v There is no treatment that improves foetal growth, but IUGR babies who are at or near term have the best outcome if delivered promptly. 12 October 2002 IUGR - Prof. S. N. Panda 25

Treatment n Maternal bed rest This is the initial approach for the treatment of IUGR. The benefit of bed rest is that it results in increased blood flow to the uterus. Studies have shown, however, that in most cases bed rest at home is just as effective as bed rest in the hospital environment. 12 October 2002 IUGR - Prof. S. N. Panda 26
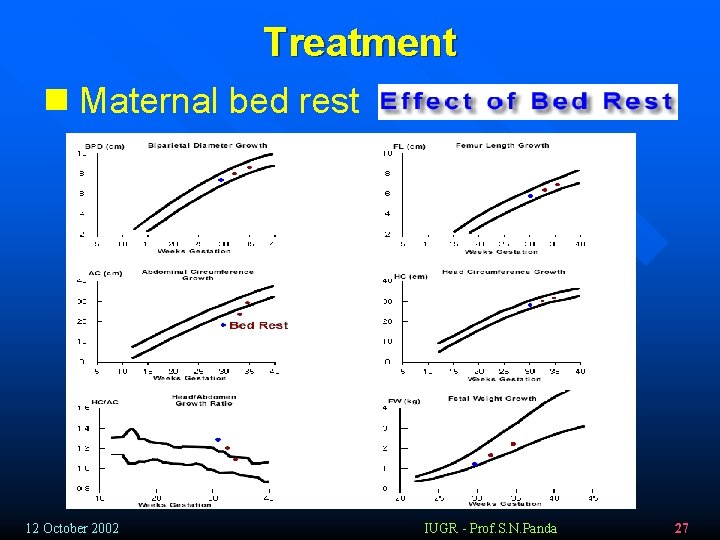
Treatment n Maternal bed rest 12 October 2002 IUGR - Prof. S. N. Panda 27

Treatment n Aspirin Therapy v The use of aspirin to treat foetuses with IUGR is still controversial. v If aspirin is used, it may be advantageous if given to patients before 20 weeks of gestation. It is minimal to limited benefit if given at the time of diagnosis (third trimester). v At the present time it is not recommended as a form of prevention for low risk patients. 12 October 2002 IUGR - Prof. S. N. Panda 28

Treatment n Other Forms of Treatment v Other forms of treatment that have been studied are nutritional supplementation, zinc supplementation, fish oil, hormones and oxygen therapy. v Limited studies are available regarding the use of these modalities in the treatment of IUGR. 12 October 2002 IUGR - Prof. S. N. Panda 29

Treatment Judge Optimum Time Of Delivery RISK OF PREMATURITY v DIFFICULT EXTRA UTERINE EXISTENCE 12 October 2002 RISK OF IUD v HOSTILE INTRA UTERINE ENVIRONMENT IUGR - Prof. S. N. Panda 30

Short Term Risks of IUGR v Increased perinatal morbidity and mortality. § Intra uterine / Intrapartum death. § Intrapartuum foetal acidosis characterized by-. » Late deceleration. » Severe variable deceleration. » Beat to beat variability. » Episodes of bradicardia. § Intrapartum foetal acidosis may occur in as many as 40 % of IUGR, leading to a high incidence of LSCS. § IUGR infants are at greater risk of dying because of neonatal complications- asphyxia, acidosis, meconium aspiration syndrome, infection, hypoglycemia, hypothermia, sudden infant death syndrome. § IUGR infants are likely to be susceptible to infections because of impaired immunity 12 October 2002 IUGR - Prof. S. N. Panda 31

Long term Prognosis v Babies who suffer from IUGR are at an increased risk for death, low blood sugar, low body temperature, and abnormal development of the nervous system. These risks increase with the severity of the growth restriction. v The growth that occurs after birth cannot be predicted with certainty based on the size of the baby when it is born. v Infants with asymmetrical IUGR are more likely to catch up in growth after birth than are infants who suffer from prolonged symmetrical IUGR. v If IUGR is related to a disease or a genetic defect, the future of the infant is related to the severity and the nature of that disorder. 12 October 2002 IUGR - Prof. S. N. Panda 32

Long term Prognosis v IUGR infants are more likely to remain small than those of normal birth weight. They will need the special attention of primary health, nutrition and social services during infancy and early childhood. v Implication of IUGR can be life long affecting: § Body size growth, composition and physical performance. § Immunocompetence. v It appears to predispose to adult-onset, degenerative diseases like maturity onset diabetes and cardiovascular diseases. v Each case is unique. Can not reliably predict an infant's future progress. 12 October 2002 IUGR - Prof. S. N. Panda 33

syndrome

v “mekonionarion” – “opium like” (Aristotle) v Meconium stained amniotic fluid – 8 -15 % of all deliveries. v 5% of them – meconium aspiration syndrome v 5% mortality 12 October 2002 IUGR - Prof. S. N. Panda 35

Origin and composition v Meconium is recognized – 70 -85 d of gestation v Composition: » Water, Mucopolysaccharides, Cholesterol and sterol precursos, Protein, Lipid, Bile acids and salts, Enzymes, Blood group substances, Squamous cell, Vernix caseosa v No bacteria! 12 October 2002 IUGR - Prof. S. N. Panda 36

In utero passage v Risk factors associated with in utero passage of meconium: § § § § Postterm pregnancy Little/no amniotic fluid at amniotomy Oligohydramnion by US IUGR/ placental insufficiency Maternal HTN Preeclampsia Maternal drug abuse (tobacco, cocaine). v Gestational age > 34 w – increasingly present with advancing gestational age. 12 October 2002 IUGR - Prof. S. N. Panda 37

Pathophysiology v As the GI tract matures: vagal stimulation peristalsis+ rectal sphincter relaxation meconium v Etiology not well understood: § Fetal response to intra-uterine stress: hypoxia increased vagal tone § Transient compression of umbilical cord/head increased vagal tone § Maturation of of fetal intestinal function 12 October 2002 IUGR - Prof. S. N. Panda 38

Timing of the initial insult: v Traditional belief: immediately after birth v Several investigations: Most cases occur in utero when fetal gasping is initiated before delivery. 12 October 2002 IUGR - Prof. S. N. Panda 39

Effects of meconium: v Reduce antibacterial activity (perinatal bacterial infection) v Irritating to fetal skin ( erythema toxicum) v The most severe complication of meconium passage in utrro is aspiration of stained amniotic fluid before, during, and after birth 12 October 2002 IUGR - Prof. S. N. Panda 40

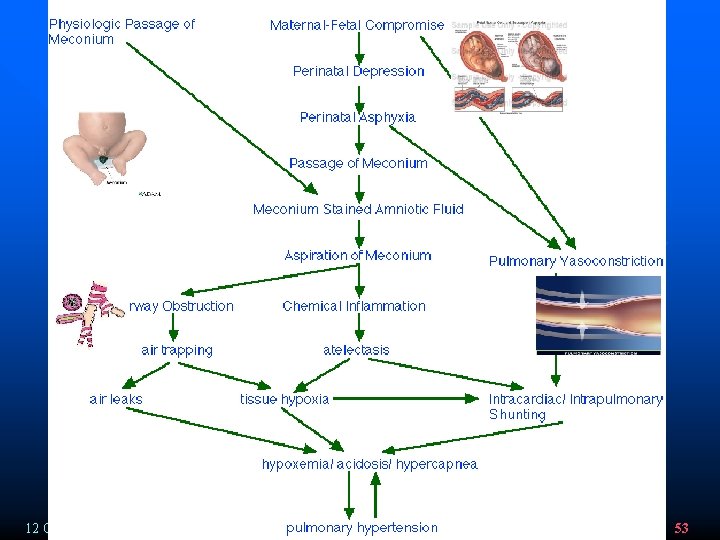
Meconium aspiration syndrome pathophysiology v Airway obstruction: v Chemical pneumonitis: v Surfactant dysfunction: v Umbilical vessel damage v Persistent pulmonary hypertension of the newborn 12 October 2002 IUGR - Prof. S. N. Panda 41

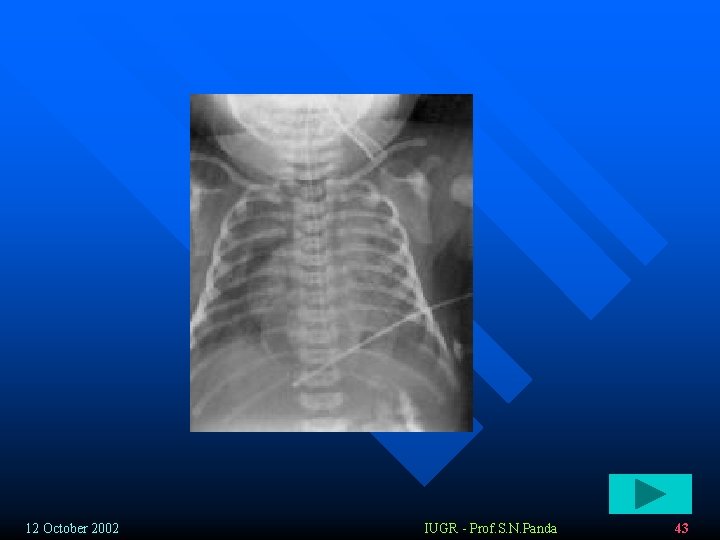
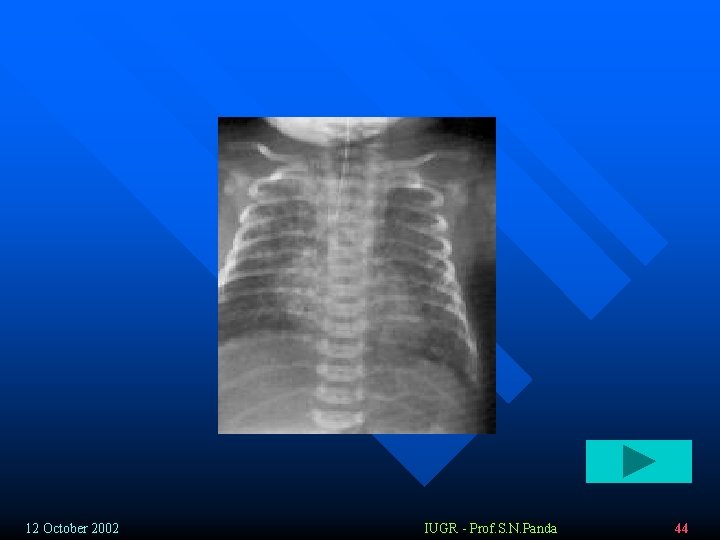
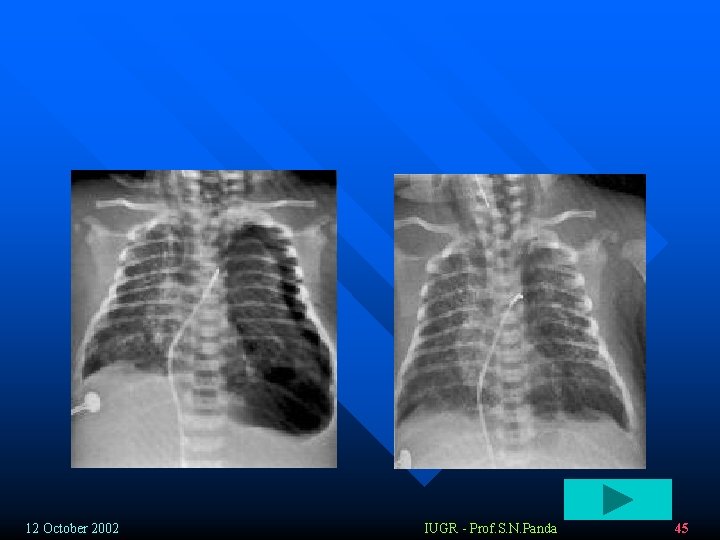
Airway obstruction: v Immediate : obstruction of large airways: (volume dependent ): hypoventilation => hypoxemia, hypercapnea, acidosis v Central clearing – obstruction of small airways: § Complete athelectasis § Partial air trapping (ball valve phenomenon) hyperdistention of alveoli increaesed lung resistance during exhalation § pneumothorax, pneumomediastinum , pneumopericardium. 12 October 2002 IUGR - Prof. S. N. Panda 42
12 October 2002 IUGR - Prof. S. N. Panda 43
12 October 2002 IUGR - Prof. S. N. Panda 44
12 October 2002 IUGR - Prof. S. N. Panda 45

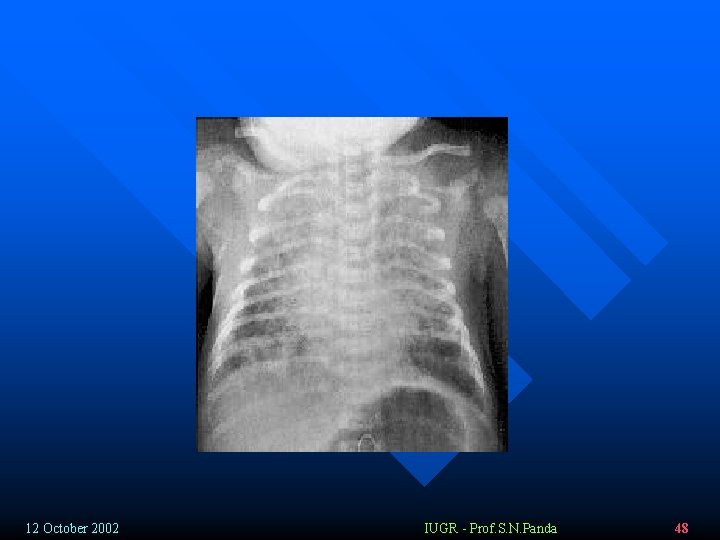
Chemical pneummonitis: v 50% of cases v Enzemes, bile salts, fats – irritants PMN, MQ, inflammatory mediators. v Chemical pneumonitis, edema (6 h) inflamation (24 h) v Hyalin membranes, hemorrhage, vascular necrosis can occur. v Bacterial superinfection. v Activated Vasoactive mediators play a role in the develipment of PPHN. 12 October 2002 IUGR - Prof. S. N. Panda 46

Chemical pneummonitis: v 50% of cases v Enzemes, bile salts, fats – irritants PMN, MQ, inflammatory mediators. v Chemical pneumonitis, edema (6 h) inflamation (24 h) v Hyalin membranes, hemorrhage, vascular necrosis can occur. v Bacterial superinfection. v Activated Vasoactive mediators play a role in the develipment of PPHN. 12 October 2002 IUGR - Prof. S. N. Panda 47
12 October 2002 IUGR - Prof. S. N. Panda 48

Surfactant dysfunction v Free fatty acids (paimitic, stearic, oleic) – higher minimal surface tention than surfactant (striping effect) v decreased lung compliance v concentration dependent 12 October 2002 IUGR - Prof. S. N. Panda 49

Umbilical vessel damage v Umbilical vessels exposed to meconium may cause severe focal inflammation injury. v Spasm and necrosis fetal hypoperfusion v 1% meconium induced umbilical vascular necrosis among meconium stained placentas. 12 October 2002 IUGR - Prof. S. N. Panda 50

Persistent pulmonary hypertension of the newborn v Final common pathway for the severe morbidity and mortality in infants with MAS. § Hypoxia Pulmonary arterial vasoconstriction. § Abnormal pulmonary arterial muscularization m/p chronic change v Association between MAS and PPHN : § Direct pathogenic cause of lung damage § Simple marker of chronic intrauterine hypoxia 12 October 2002 IUGR - Prof. S. N. Panda 51

Risk factors of MAS developing into PPHN v “Risk factors of meconium aspiration syndrome developing into persistent pulmonary hypertension of newborn. Acta Paediatr Taiwan. 2004 Jul-Aug; 45(4): 2037” – 362 cases of MAS (17% with PPHN). v Pneumothorax, change in FHR base line, asphyxia most important risk factors 12 October 2002 IUGR - Prof. S. N. Panda 52
12 October 2002 IUGR - Prof. S. N. Panda 53

Risk and severety of MAS: v Degree of contamination of the amniotic fluid and Presence of meconium in the airway at delivery is meconium itself a direct primary cause of morbidity mortality? v MAS is commonly associated with chronic hypoxia is meconium a marker of fetal maturation of chronic fetal hypoxia? v Asphyxia, pneumothorax, PPHN – the most important risk factors of mortality in MAS. 12 October 2002 IUGR - Prof. S. N. Panda 54

Clinical presentation: v Depressed at birth v Early onset of respiratory distress (within 2 h) » » » Mild tachypnea cyanosis Dyspnea: granting, ala nazi, intercostal retraction Barral chest (presence of air trapping) respiratory failure v Auscultayion: “wet” inspiratory crackles, occasional expiratory noises v Severe Mas: » Hypoxemia – R L shant » Persistant fetal circulation » PPHN – hypoxic pulmonary arterial vasoconstriction – acidosis, hypercapnea, hypoxemia (prenatal & perinatal maladaptation) » Cardiopulmonary failure » acidosis 12 October 2002 IUGR - Prof. S. N. Panda 55

Complication: v PPHN v AIR LEAK v PULMONARY HEMORRAGE v ASPHYXIA COMPLICATIONS 12 October 2002 IUGR - Prof. S. N. Panda 56

Laboratory: v Hypoxemia (R L shunt) v Hypercarbia (in significant obstruction) v Respiratory alkalosis (hyperventilation) v Combined respiratory and metabolic acidosis (severe disease – respiratory failure) 12 October 2002 IUGR - Prof. S. N. Panda 57

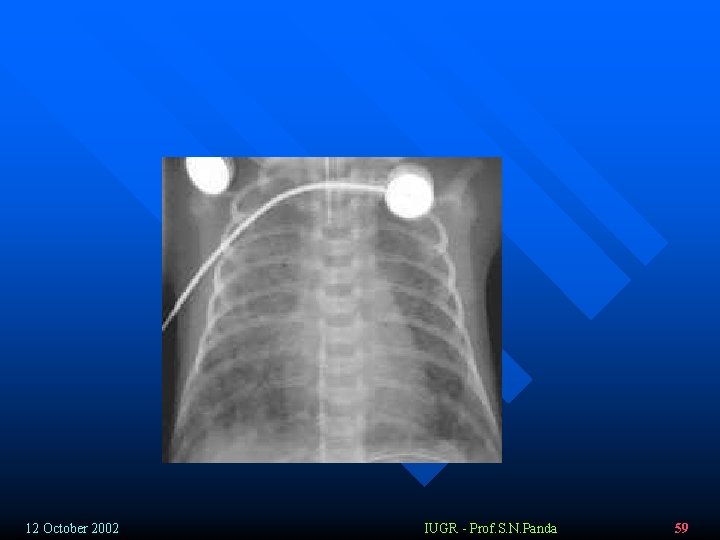
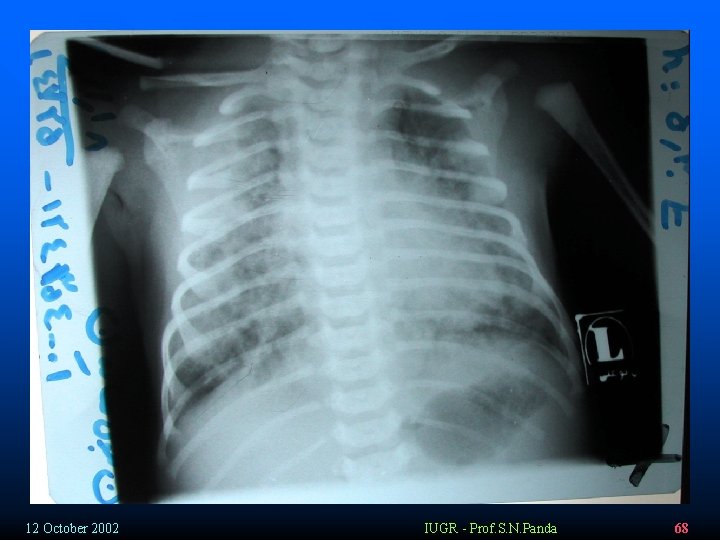
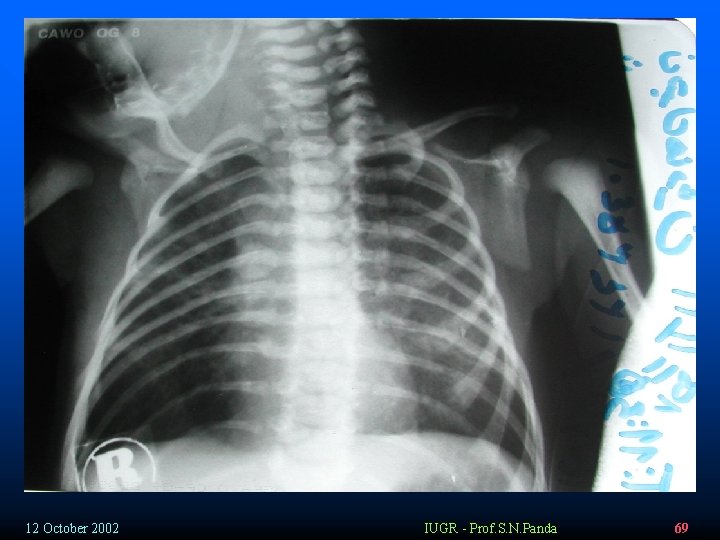
Chest x-ray v 73% - positive x-ray findings v Global atelectasis – early § Patchy dense opacifications (decreased vantilation) accompanied by areas of hyperinflation § Widespread infiltrates § Consolidations § Small pleural effusion (30%) § Pneumothorax/ pneumomediastinum (25%) 12 October 2002 IUGR - Prof. S. N. Panda 58
12 October 2002 IUGR - Prof. S. N. Panda 59

Prenatal diagnosis and prevention: v Diagnosis of fetus “at risk” – monitoring fetal status. v Thick VS thin meconium v Meconium and FHR abnormalities v Amnioinfusion during labor v Nasopharyngeal suctioning 12 October 2002 IUGR - Prof. S. N. Panda 60

Upon delivery intervention: v “combined approach” : nasopharengeal suctioning + neonatal trachea suction. v Thick meconium + depressed infant tracheal suction - marked reduction in morbidity and mortality. v The American Academy of pediatrics Neonatal Resuscitation Program Steering Guidelines 12 October 2002 IUGR - Prof. S. N. Panda 61

management v Minimize agitation (prevent additional acidosis and hypoxemia) – optimal thermal environment, minimal handling, muscle relaxation. v NGT v Respiratory care v Maintain systemic blood pressure (R L shunt) v Antibiotics. 12 October 2002 IUGR - Prof. S. N. Panda 62

v MAS treatment – ventilation Main target: oxigenation! – Pa. O 2 60 -90 mm. Hg support: v difficulty with oxigenation positive airway pressure (CPAP) – improves ventilation, stabilizes small airways. v Respiratory acidosis/severe respiratory distress mechanical ventilation – s. PO 2> 50 mm Hg with Fi. O 2 – 100% & p. H< 7. 2. sedation! Relaxation! v Surfactant v i. NO v failed conventional ventilation – HFJV, HFO v ECMO 12 October 2002 IUGR - Prof. S. N. Panda 63

SURFACTANT v Lung lavage using sufractant in MAS is currently being investigated “Treatment of severe meconium aspiration syndrome with porcine surfactant: a multicentre, randomized, controlled trial” Acta Paediatr. 2005 Jul; 94(7): 896 -902. “ Pulmonary function after surfactant lung lavage followed by surfactant administration in infants with severe meconium aspiration syndrome”. J Matern Fetal Neonatal Med. 2004 Aug; 16(2): 125 -30. 12 October 2002 IUGR - Prof. S. N. Panda 64

Steroids v Pathophysiology: anti-infalammatory properties. v Corticosteroid treatment, started early, show some improvement in oxigenation and pulmonary hemodynamics durind acute phase. v Effect on morbidity and mortality Cochrane Database Syst Rev, 2003 insufficient evidence. v Further research: clinucal significant, optimal timing, dosing. 12 October 2002 IUGR - Prof. S. N. Panda 65

!!! תי 12 October 2002 IUGR - Prof. S. N. Panda 66

v v v v Case 2 25 Y G 1 42 W Single CC: LP PNC: (-) PMH: opiate abuser FH: Term V/E: 3 – 4 cm & me conium stained Amniotic fluid The new born birthed by C/S The vernix , umbilical cord and nails was me conium – stained endoteracheal suction was performed The new born had respiratory distress with marked tachypnea and cyanosis. APGAR: 3/10 & 6/10 (1′ & 5′) Auscultation reveals rales The new born was hospitalized in NICU Because of Eyes Discharged Gentamicin and cefotaxim was started After 6 days the infant was discharged 12 October 2002 IUGR - Prof. S. N. Panda 67
12 October 2002 IUGR - Prof. S. N. Panda 68
12 October 2002 IUGR - Prof. S. N. Panda 69

- Slides: 70