INTESTINAL PERMEABILITY LEAKY GUT SYNDROME Adan Sanchez MD


INTESTINAL PERMEABILITY/ LEAKY GUT SYNDROME Adan Sanchez, MD

The stomach has a controlling power upon the health of the entire body. —Anything which is taken into the stomach and converted into blood becomes a part of the being. —

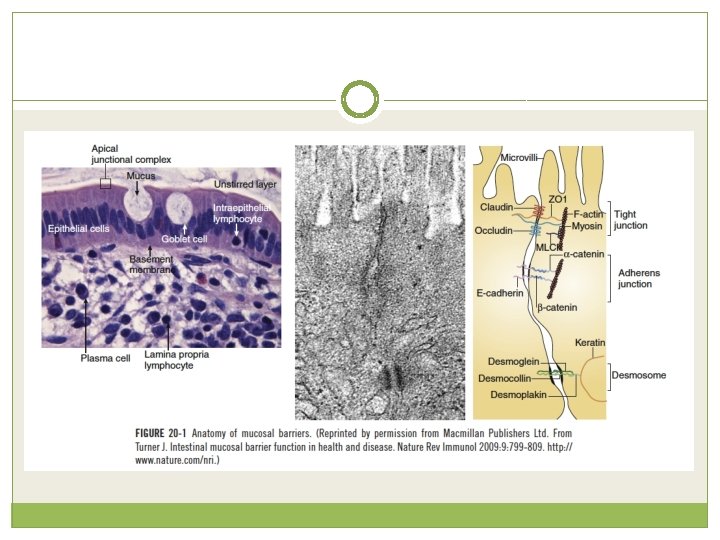
Natural Physiologic Barrier � A key function of healthy gut mucosa is to prevent bacteria and their endotoxins from reaching portal circulation. For this purpose, a natural physiologic barrier is formed by the mucous layer, the epithelial cells and apical junctional complex, and the lamina propria. When one or more of these components is impaired, damage to the intestinal barrier may result, allowing luminal toxins to translocate from the gut into the systemic circulation.


Facts of a gut barrier � It prevents against loss of water and electrolytes and entry of antigens and microorganisms into the body while allowing exchange of molecules between host and environment and absorption of nutrients in the diet. �The immune system of the gastrointestinal tract also helps prevent the translocation of harmful molecules across the gut mucosa. Gut associated lymphoid tissue comprises approximately 25% of the mucosal mass of the intestine. It is considered the body’s largest immune organ, containing 40% of its immune effector cells.

GALT �The immune system of the gastrointestinal tract also helps prevent the translocation of harmful molecules across the gut mucosa. Gut associated lymphoid tissue comprises approximately 25% of the mucosal mass of the intestine. It is considered the body’s largest immune organ, containing 40% of its immune effector cells.

Gut Brain Axis/Second Brain. � The CNS communicates with the enteric nervous system, the gut muscle layers, and the intestinal mucosa through bidirectional (ie, afferent and efferent) autonomic pathways, thus modulating permeability, mucus secretion, motility, and immunity. � Inputs from the CNS can modify gut functions, while inputs from the gut to the CNS can modulate specific symptoms. Alterations of these bidirectional communications may contribute to neuroinflammation and the pathogenesis of CNS disorders.


�The brain and nerves are in sympathy with the stomach. Erroneous eating and drinking result in erroneous thinking and acting. " Ibid. , p. 134 � You are a nervous dyspeptic. The brain is closely connected with the stomach, and its power has so often been called to aid the weakened digestive organs that it is in its turn weakened, depressed, congested.

�The brain and nerves are in sympathy with the stomach. �The diseased stomach affects the entire nervous system, brain, and mind… the nerves of the brain are diseased by the abuse heaped on the stomach. �The success of acquiring a good memory and a calm, uniform temper depends not upon circumstances, but very much upon the way in which the stomach is treated.

Disrupting Intestinal Barrier �Environmental stress �Pathogens �HFD/Western Diet �Drugs and antibiotics �Genetic susceptibility


Pathogens, as well as usage of antibiotics, might disturb the intestinal mucus layer, either by enhancing mucus degradation, or by inhibiting the normal commensal triggers for mucus production. Rotavirus is the most common cause of diarrhea in children and is associated with an increase in gut permeability. Repeated rotaviral infections during infancy may also increase the risk of allergy and atopy later on in life.

HFD/Western Diet �Energy rich high fat diets increased intestinal permeability resulting in metabolic endotoxinemia. �Among dietary sugars fructose plays a particular role with regard to the intestinal barrier �Consumption of 30% fructose solution for eight weeks was associated with the loss of the tight junction proteins occludin and ZO 1 in the duodenum and a subsequent increase of bacterial endotoxin in the portal vein.

Drugs and antibiotics NSAIDs are the most commonly prescribed antirheumatic drugs, and NSAID enteropathy is estimated to occur in 65% of longterm users. Even short term NSAID therapy has been shown to cause changes in intestinal permeability similar to those seen in patients with active IBD.
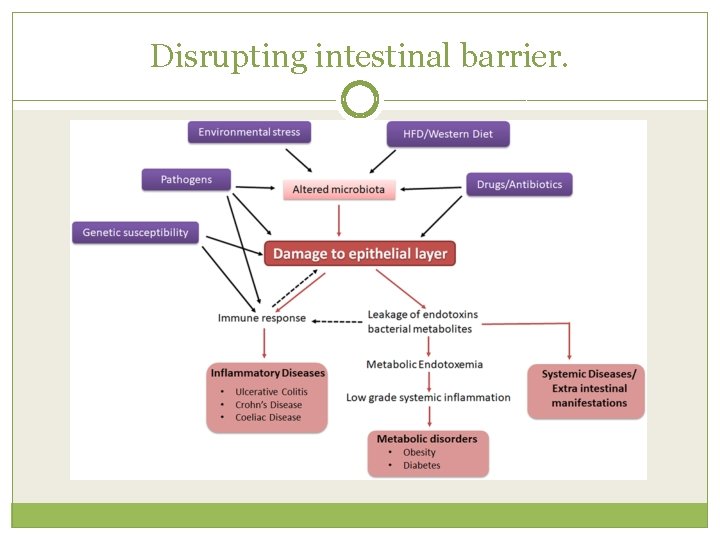
Disrupting intestinal barrier.
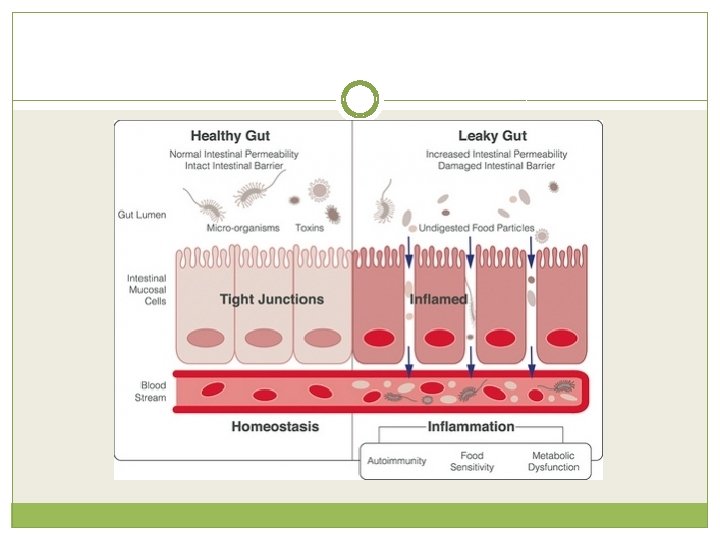

Intestinal Microbiota. �The microbiota is important for the maintenance of barrier integrity, immunologic tolerance and certain metabolic activities. In contrast, intestinal dysbiosis plays a critical role in diverse pathological processes, such as inflammatory bowel diseases, diabetes and obesity.

Intestinal Microbiota Importance �Gut microbial metabolites such as short chain fatty acids (SCFAs) and succinate, which are derived from the fermentation of dietary fiber, have important metabolic functions. �SCFAs and succinate might prevent obesity by increasing energy expenditure, increasing anorexic hormone production and improving appetite regulation. �SCFAs have a crucial role in gut homeostasis, adipose tissue and liver substrate metabolism and function, through which they can prevent the progression of type 2 diabetes mellitus (T 2 DM) and nonalcoholic fatty liver disease (NAFLD).

Intestinal Microbiota Importance �The microbial metabolites derived from protein fermentation, which are mainly produced in the distal colon, are most often considered detrimental for gut integrity and metabolic health. �Providing mixtures of dietary fibers to increase distal colonic microbial carbohydrate fermentation and thereby inhibit protein fermentation might be a putative target to ameliorate obesity, T 2 DM and NAFLD. �

Dysbiosis � Dysbiosis and alterations of the gut microbiome composition have been shown to contribute to the development of several diseases in humans, such as inflammatory bowel disease, type 2 diabetes, metabolic syndrome, obesity, allergies, colorectal cancer, and Alzheimer disease (AD).
SIBO �Abnormal colonization within the small bowel by bacteria normally found in the colon, mouth, or pharynx. Also called bacterial overgrowth of the small intestine (BOSI), “blind loop, ” or “stagnant loop, ” �SIBO is a potentially serious disorder that leads to problems such as malabsorption, anemia and weight loss, malnutrition, increased intestinal permeability, and bone loss.

L/M Test � In healthy individuals, there is a 20% to 30% recovery of mannitol and less than a 1% recovery of lactulose over a 6 hour period. 12 Under pathologic conditions, the amount of lactulose permeating the intestinal barrier increases and the amount of mannitol does not change or decrease. Th is results in a rise is the L/M ratio, which refl ects disturbances in the integrity of the small bowel.

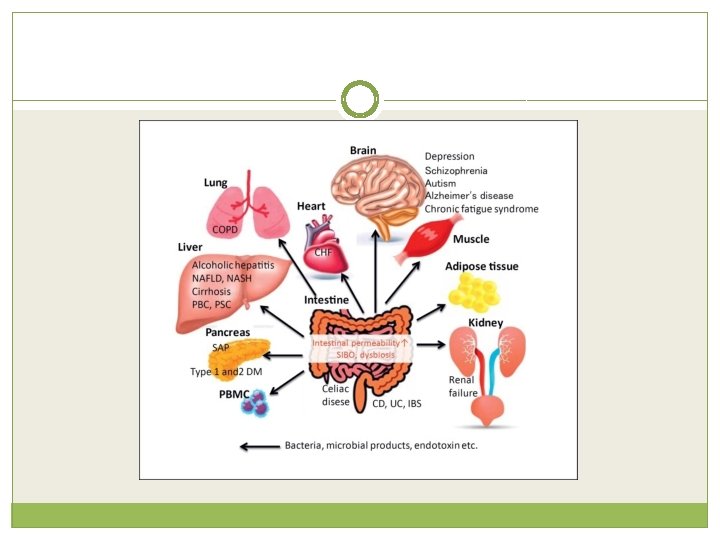
Clinical Applications � Because the intestinal mucosa plays a pivotal role in immune defense and nutrient absorption, a wide variety of diseases and conditions are associated with abnormal bowel permeability.

Inflammatory Bowel Diseases �Disrupted barrier function comprises alterations in epithelial TJ, . These barrier defects are attributed to the enhanced activity of proinflammatory cytokines like TNF α, IL 1β and IL 13, which are highly expressed in the chronically inflamed intestine. �Systemic endotoxemia was reported to be present in 28∼ 88% of patients with UC and 48∼ 94% with CD during clinical relapse. �Patients with Crohn's disease (CD) exhibit marked increases in intestinal permeability assessed by the lactulose mannitol (L/M) test.

Inflammatory Joint Diseases � Numerous studies have shown a correlation between different types of arthritis and increased intestinal permeability. � It is estimated that between 30% and 60% of such patients have occult intestinal inf ammation. � However, it has not been fully determined whether this correlation results from the disease process itself or is due to mucosal damage caused by treatment with nonsteroidal anti infl ammatory drugs (NSAIDs).

Food Allergies � When there is a breach of gut barrier function, dietary antigens and other luminal toxins can also be translocated across the intestinal wall. �For food allergies to manifest, intraluminal antigens must first penetrate the intestinal epithelial barrier before gaining access to mast cells in the subepithelial compartment and triggering hypersensitivity reactions.

Nonalcoholic Fatty Liver Disease/NAFLD � Through a meta analysis of five such studies, Luther et al found that almost 40% of patients with NAFLD had increased intestinal permeability. � A subgroup analysis of NASH patients showed a stronger association with altered intestinal permeability, with nearly 50% affected, suggesting that the necroinflammatory changes seen in NASH may be more closely associated with increased gut permeability. � Injury to the intestinal epithelium led to increased permeability and passage of bacterial products to the portal vein, leading to enhanced liver injury. � They suggest that an initial liver injury may lead to the release of inflammatory cytokines, which in turn affects the intestinal tight junctions and increases intestinal permeability passage of bacterial elements into the portal circulation propagating the preexisting liver injury.

GUT–BRAIN AXIS � CNS communicates with the enteric nervous system, the gut muscle layers, and the intestinal mucosa through bidirectional (ie, afferent and efferent) autonomic pathways, thus modulating permeability, mucus secretion, motility, and immunity. � Alterations of these bidirectional communications may contribute to neuroinflammation and the pathogenesis of CNS disorders

AD, Parkinson’s disease, Huntington’s disease, Amyotrophic lateral sclerosis. � Increasing evidence suggests that clumping of proteins with prion like behavior might be a phenomenon shared by many of the major CNS diseases, like AD, Parkinson’s disease, Huntington’s disease, and amyotrophic lateral sclerosis. � Protein degradation pathways are normally able to degrade small amount of prions; however, when prions accumulate and exceed a certain threshold, they are able to self propagate thereby compromising CNS functions. � In particular, the gut has been shown to play a role in the transmission of prionic proteins. � Interacting with follicular dendritic cells, prion like proteins might move to the enteric nervous system, which governs gastrointestinal functions, finally spreading to the CNS.

Prevention and Treatment �A day or two of fasting per week. �Plant based diet. �Avoid snacks. �Eliminate all those foods known to give you a sensitivity. �Take one teaspoon slippery elm in water or mixed with 3 oz of Aloe Vera, half an hour before each meal. �Quercetin is a naturally occurring flavonoid with antioxidant, anti inflammatory, and anticancer properties. Quercetin has been shown to enhance intestinal barrier functions in human intestinal cells.

�Anxiety has been found to increase permeability and make it so that your intestine cannot keep partly digested nutrients out so well. Avoid anxiety with the meals. If the brain is burdened, reduce the amount of food that you take. Let food stay a long time in the mouth. �Ginkgo biloba extract (GBE) has antioxidant and free radical–scavenging properties with cytoprotective effects on cells of the gastrointestinal mucosa. �Essential fatty acids such as those found in walnuts and flaxseed can be most helpful to protect your body from toxins produced in the digestive tract.

� Vitamins C and E play essential roles in protecting intestinal mucosal cells from oxidative damage and free radical pathology. � If abnormal bacteria are present (dysbiosis), use herbal antibacterials as indicated. Most bacteria are sensitive to gentian, and particularly to grapefruit seed extract. If a hidden infection is a probability, use goldenseal, echinacea, artemisia, and garlic as anti germ agents. � Glutathione (GSH) and N acetyl cysteine are considered extremely good supplements to use in the leaky gut syndrome. Do not take these if you are taking artemisia or any other parasite medicine. Use two pills of NAG (N acetyl glucosamine) three times a day for one year to help heal the leaky gut.

�L glutamine is an important energy source for cells of the intestinal mucosa and has been shown to be conditionally essential for normal mucosal structure and function �Dietary fiber.

�"The brain and nerves are in sympathy with the stomach. Erroneous eating and drinking result in erroneous thinking and acting. " Ibid. , p. 134.

�"Peace of mind is lost. There is dissension, strife, and discord. Impatient words are spoken, and unkind deeds are done; dishonest practices are followed, and anger is manifested—and all because the nerves of the brain are disturbed by the abuse heaped on the stomach. . The affliction of the stomach afflicts the brain. " Ibid. , p. 578.

�"It is impossible for the brain to do its best work when the digestive powers are abused. Many eat hurriedly of various kinds of food, which set up a war in the stomach, and thus confuse the brain.
- Slides: 40