Interpretive Skills Introduction to Abdominal Ultrasound Before You

Interpretive Skills Introduction to Abdominal Ultrasound

Before You Begin This module, intended for pre-clinical medical students transitioning to the clinical years, assumes familiarity with fundamental anatomy and pathology concepts. Please review our website sections: • “Anatomy” • “Radiology-Pathology” If you need to learn or review these core concepts prior to initiating this interpretive skills module If material is repeated from another module, it will be outlined as this text is so that you are aware

General Concepts

Why Ultrasound? • Because it’s portable • Because it’s cost-effective • Because it’s non-invasive • Because you can do it anywhere • Because it answers your clinical question quickly

What can I use ultrasound for? Ultrasound is your visual stethoscope: • Chest: • Dull to percussion on physical exam? • US can evaluate for possible effusion • Abdomen: • Palpable or pulsatile mass on physical exam? • Fluid Wave? • Pain? • In all of these circumstances, US can assist in diagnosis
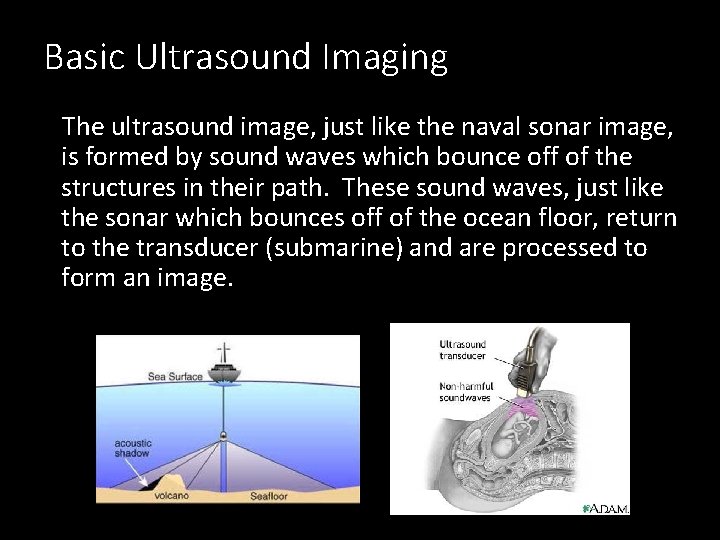
Basic Ultrasound Imaging The ultrasound image, just like the naval sonar image, is formed by sound waves which bounce off of the structures in their path. These sound waves, just like the sonar which bounces off of the ocean floor, return to the transducer (submarine) and are processed to form an image.

Basic Ultrasound Principles • Sound waves bounce off of the structures in their path. • These sound waves return to the transducer and are processed to form an image. • Differences in adjacent structures generate organ-specific images.

The only basic concept in ultrasound physics which you need to remember: Acoustic impedance – The degree to which a sound wave is impeded as it travels through a medium (i. e. through air, water, and bone, etc. )
Basic Ultrasound Imaging Principles When traveling sound waves in the body hit a structure or a surface with a dramatically different acoustic impedance, those sound waves can essentially go no farther. THE RESULT: NO USEFUL IMAGE IS FORMED For example, due to bone’s high acoustic impedance relative to surrounding tissue, there is complete obstruction of sound waves; thus, ultrasound cannot image through it

Understanding differences in acoustic impedance tell us what structures and disease processes can and cannot be imaged

Is ultrasound viable across these tissues? Test yourself, keeping acoustic impedance in mind Abdominal wall – Liver – Gallbladder? Liver – gas-filled small bowel? Abdominal wall – fluid-filled bowel or ascites? Lung abnormality? Chest wall – pleural effusion? Bone abnormality?

Answers: Abdominal wall – Liver – Gallbladder = Yes, image Liver – gas-filled small bowel = Image stops at bowel surface Abdominal wall – fluid-filled bowel or ascites = Yes, image Lung abnormality = Image stops at lung surface Chest wall – pleural effusion = Yes image, which stops when it hits aerated lung Bone abnormality = No image. Image stops below skin surface, as soon as it hits bone.

Will Ultrasound Image the Target? In addition to acoustic impedances, an acoustic window is imperative when considering the viability of ultrasound (and which test to order) An acoustic window is the are selected by an operator to introduce sound waves; for example, the uterus can be imaged via pelvic or transvaginal ultrasound windows Some pathology may only be visualized using one specific window
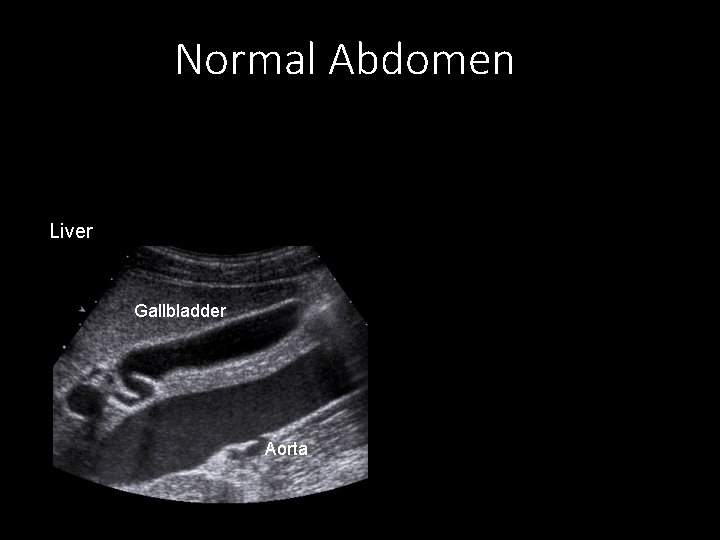
Normal Abdomen Liver Gallbladder Aorta
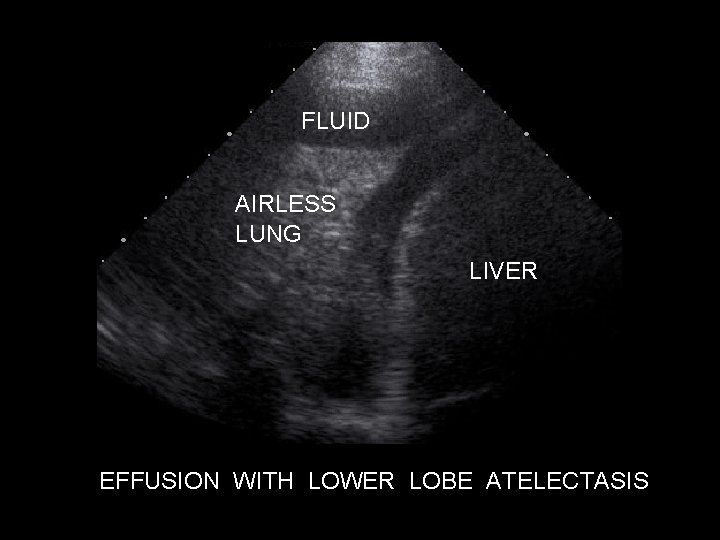
FLUID AIRLESS LUNG LIVER EFFUSION WITH LOWER LOBE ATELECTASIS
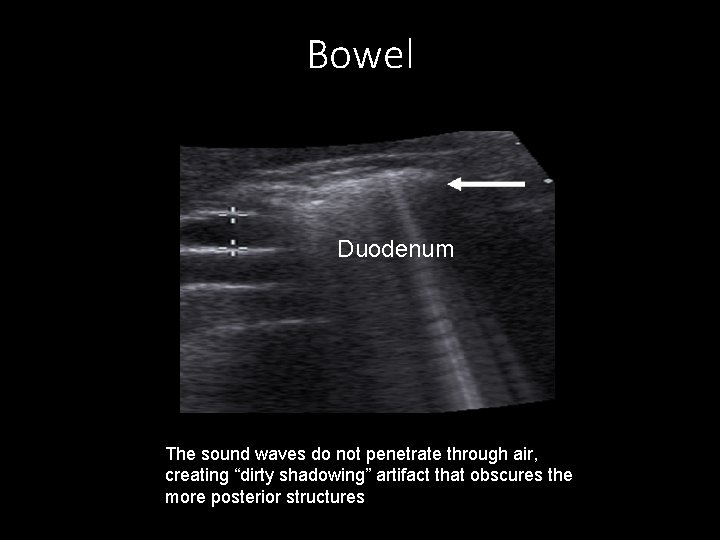
Bowel Duodenum The sound waves do not penetrate through air, creating “dirty shadowing” artifact that obscures the more posterior structures

Approach to Ultrasound Acquisition

Transducers Which one do I use?

Ultrasound Transducers (probes): Basic Facts • They both send out and receive the image-forming sound waves • They are very expensive. i. e. Don’t drop them!!! • They are labeled with one or more numbers. These numbers describe the frequency or range of frequencies that the transducer uses to form the image. • The useful range for abdominal imaging is 2 to 8 MHz.

The rule of thumb for selecting a transducer is……. (assuming you have a choice) THINK OPPOSITES!

Think opposites……. Small (thin) patient or a child: high number (5 -8 MHz) Heavy patient: low number (2 -5 MHz) Why? Low frequency = high penetration (think submarines!) but low resolution High frequency = less penetration, high resolution
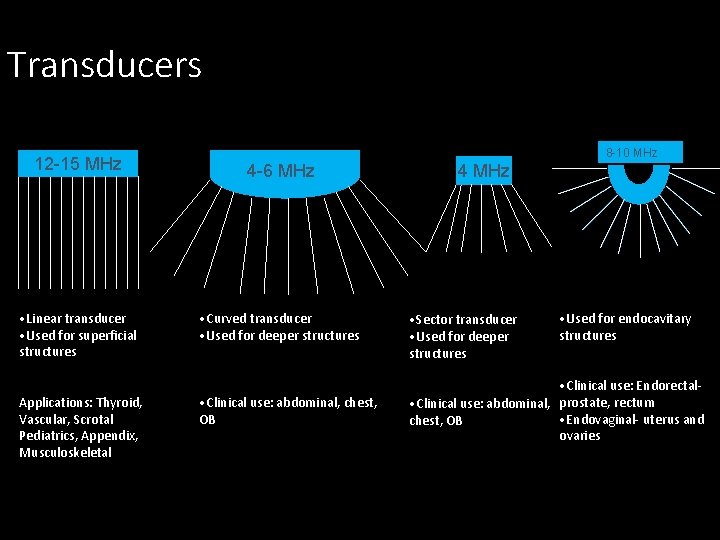
Transducers 8 -10 MHz 12 -15 MHz 4 -6 MHz • Linear transducer • Used for superficial structures • Curved transducer • Used for deeper structures Applications: Thyroid, Vascular, Scrotal Pediatrics, Appendix, Musculoskeletal • Clinical use: abdominal, chest, OB 4 MHz • Sector transducer • Used for deeper structures • Used for endocavitary structures • Clinical use: Endorectal • Clinical use: abdominal, prostate, rectum • Endovaginal- uterus and chest, OB ovaries
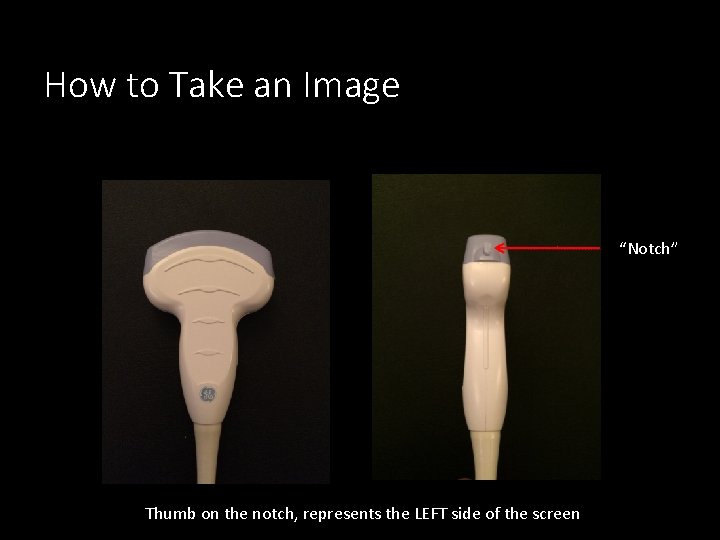
How to Take an Image “Notch” Thumb on the notch, represents the LEFT side of the screen
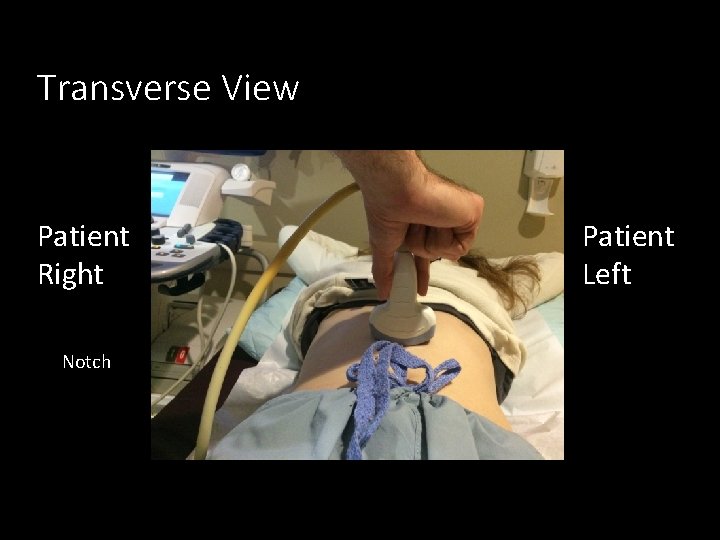
Transverse View Patient Right Notch Patient Left
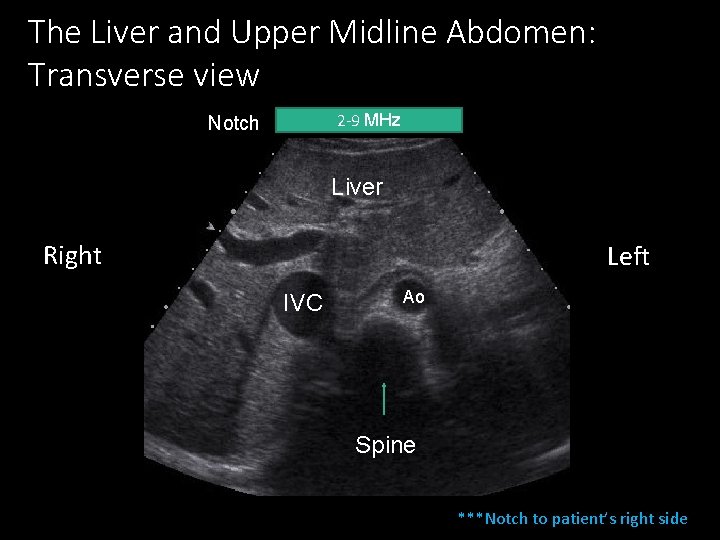
The Liver and Upper Midline Abdomen: Transverse view 2 -9 MHz Notch Liver Right Left IVC Ao Spine ***Notch to patient’s right side
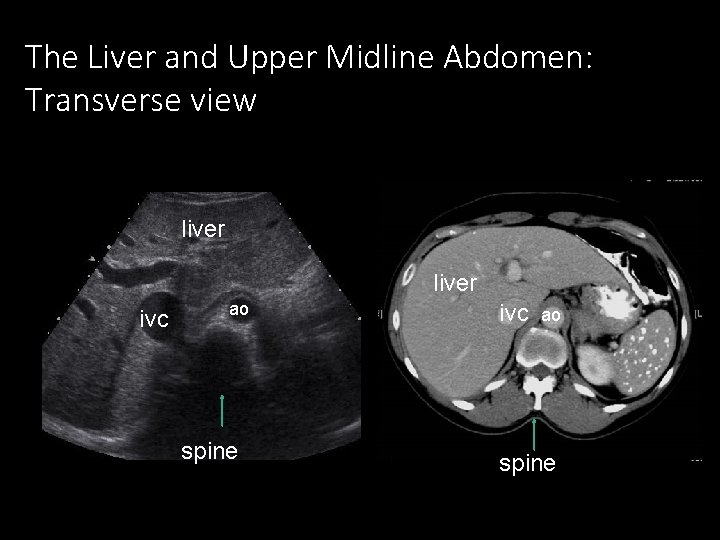
The Liver and Upper Midline Abdomen: Transverse view liver ivc ao spine
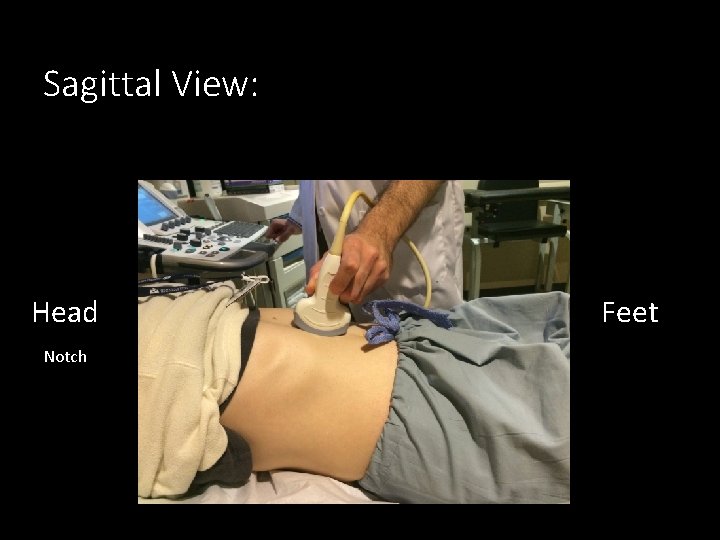
Sagittal View: Head Notch Feet
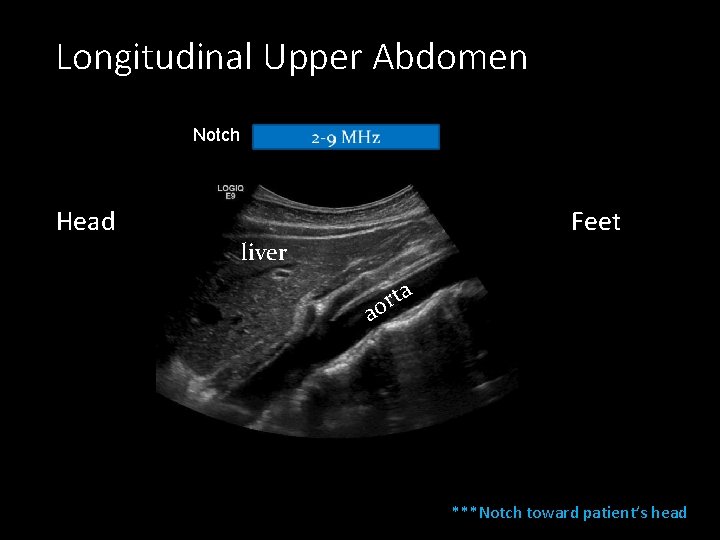
Longitudinal Upper Abdomen Notch Head Feet liver ta r o a ***Notch toward patient’s head

Ultrasound Terminology
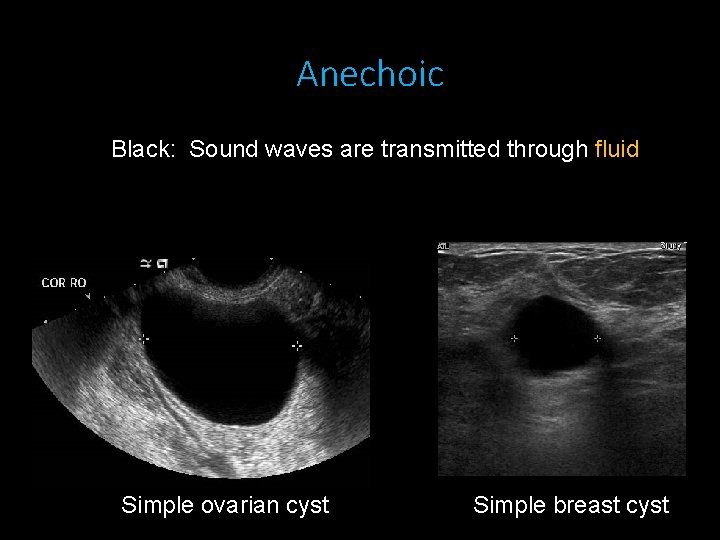
Anechoic Black: Sound waves are transmitted through fluid Simple ovarian cyst Simple breast cyst
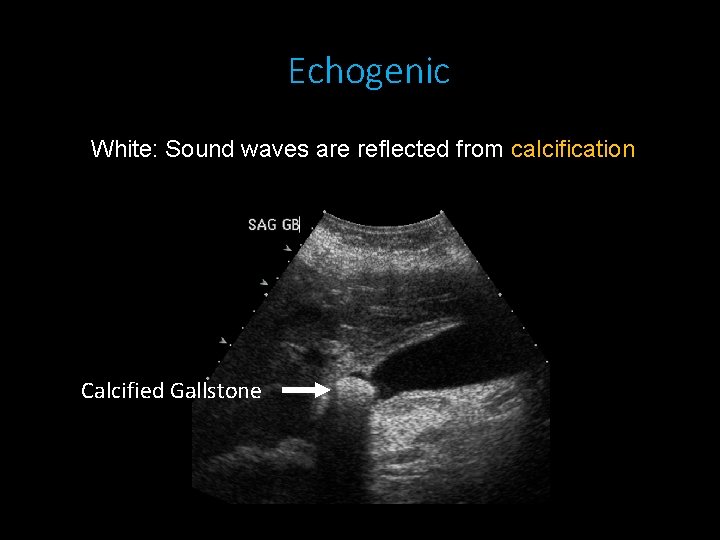
Echogenic White: Sound waves are reflected from calcification Calcified Gallstone
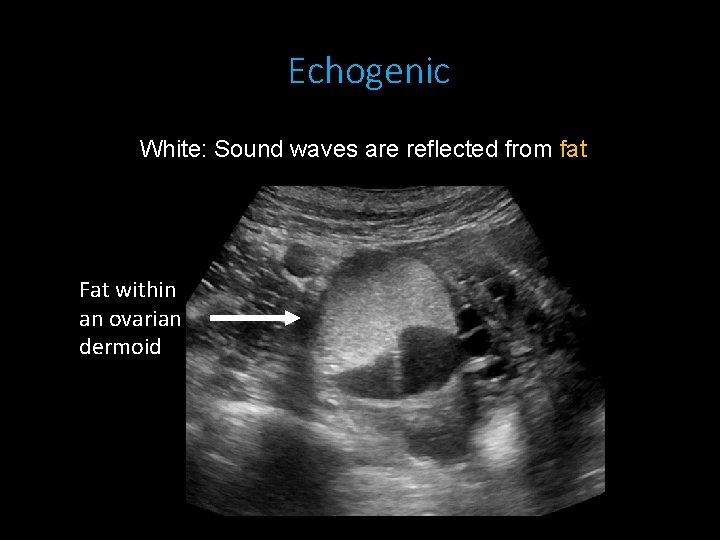
Echogenic White: Sound waves are reflected from fat Fat within an ovarian dermoid
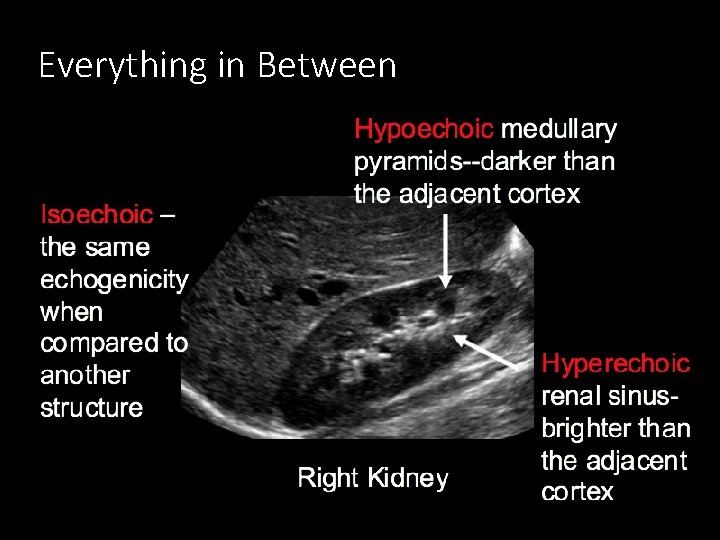
Everything in Between

Abdominal Ultrasound Components Routine • Liver • Gallbladder • Bile ducts • Kidneys • Spleen • Pancreas • Aorta/IVC As needed • Check for ascites • Targeted scan of bowel/appendix • Doppler interrogation of vasculature (renal vasculature, portal veins, superior mesenteric/celiac arteries)

Identifying Normal Anatomy on Ultrasound
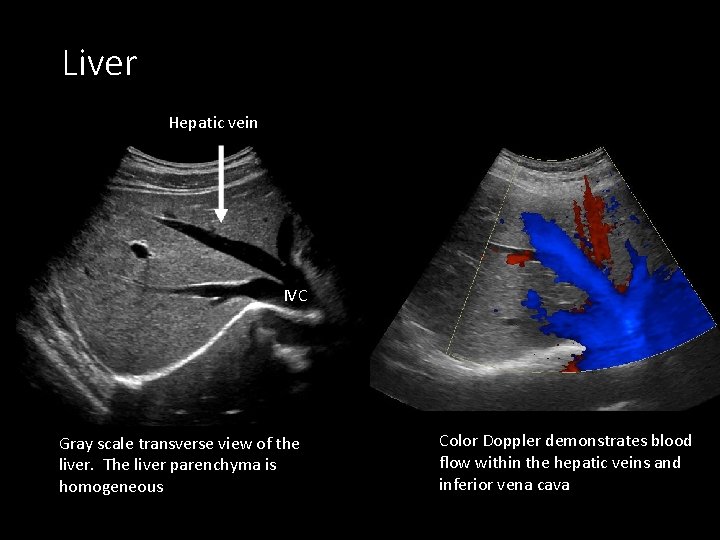
Liver Hepatic vein IVC Gray scale transverse view of the liver. The liver parenchyma is homogeneous Color Doppler demonstrates blood flow within the hepatic veins and inferior vena cava
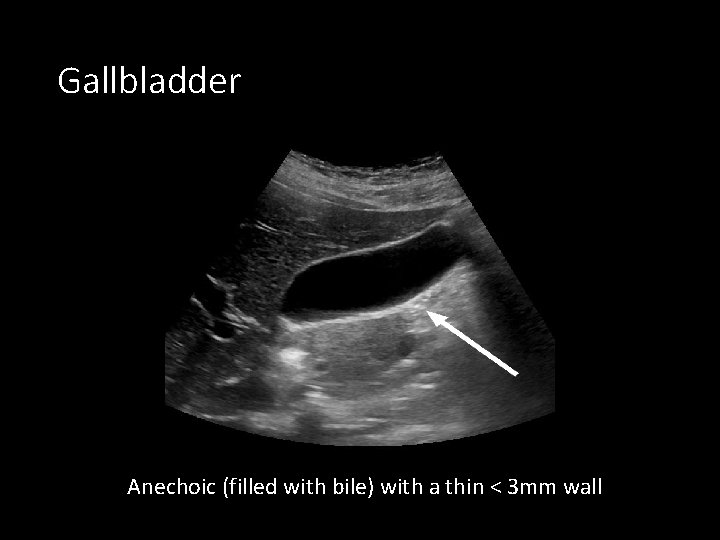
Gallbladder Anechoic (filled with bile) with a thin < 3 mm wall
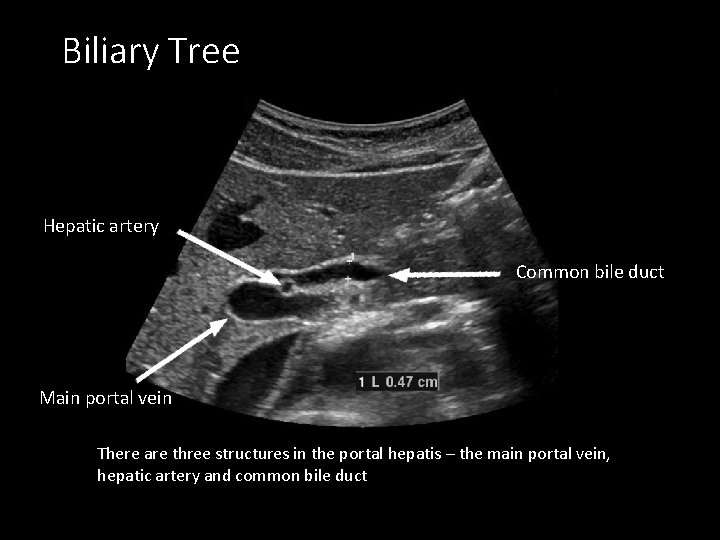
Biliary Tree Hepatic artery Common bile duct Main portal vein There are three structures in the portal hepatis – the main portal vein, hepatic artery and common bile duct
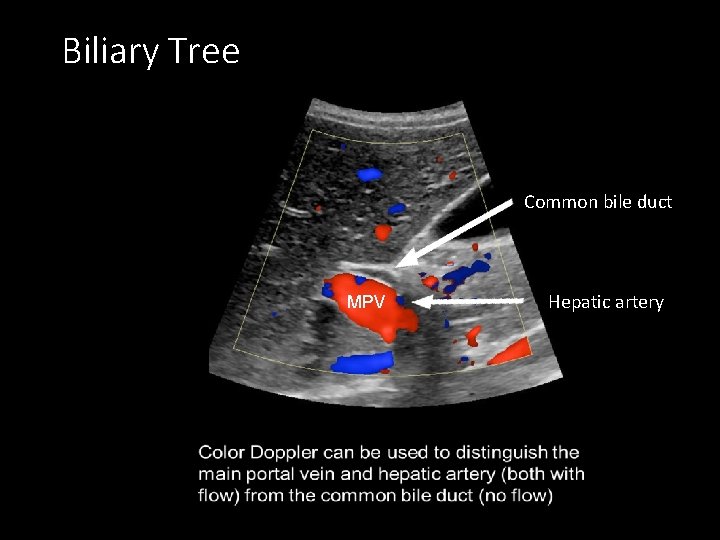
Biliary Tree Common bile duct MPV Hepatic artery
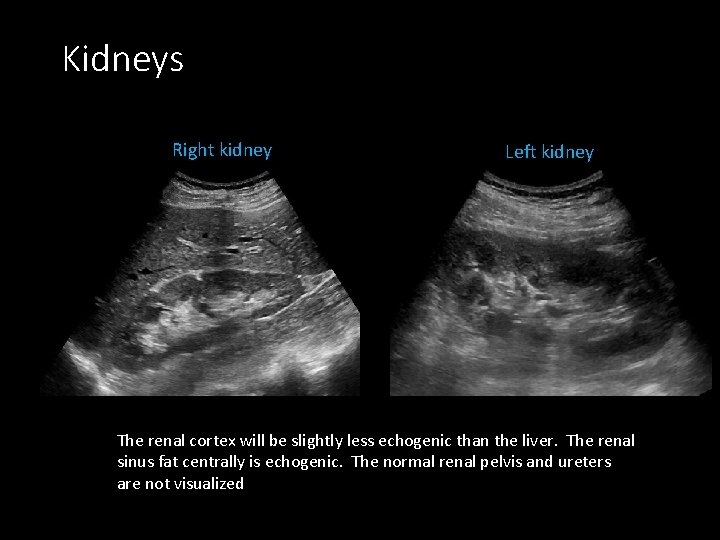
Kidneys Right kidney Left kidney The renal cortex will be slightly less echogenic than the liver. The renal sinus fat centrally is echogenic. The normal renal pelvis and ureters are not visualized
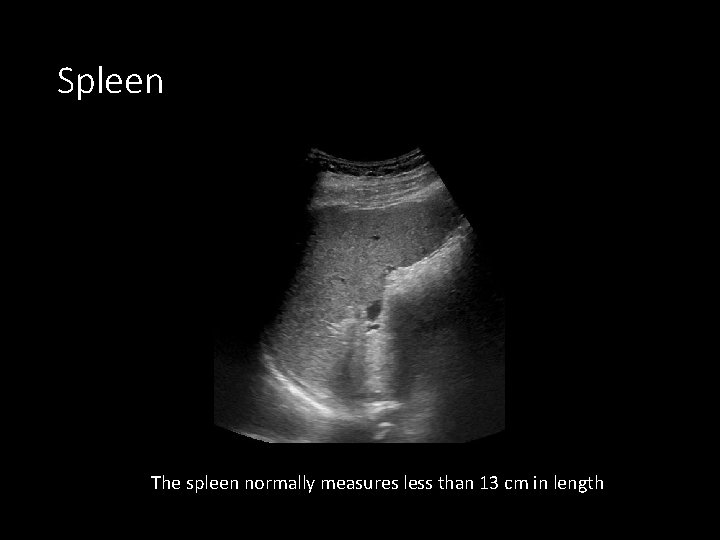
Spleen The spleen normally measures less than 13 cm in length
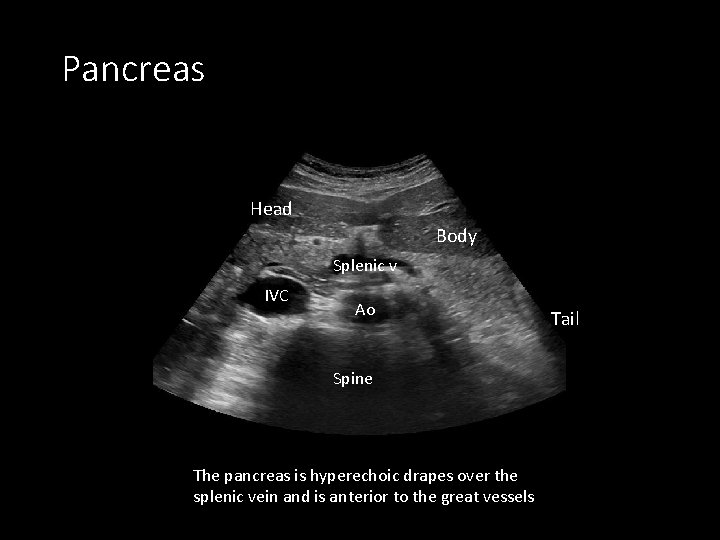
Pancreas Head Body Splenic v IVC Ao Spine The pancreas is hyperechoic drapes over the splenic vein and is anterior to the great vessels Tail
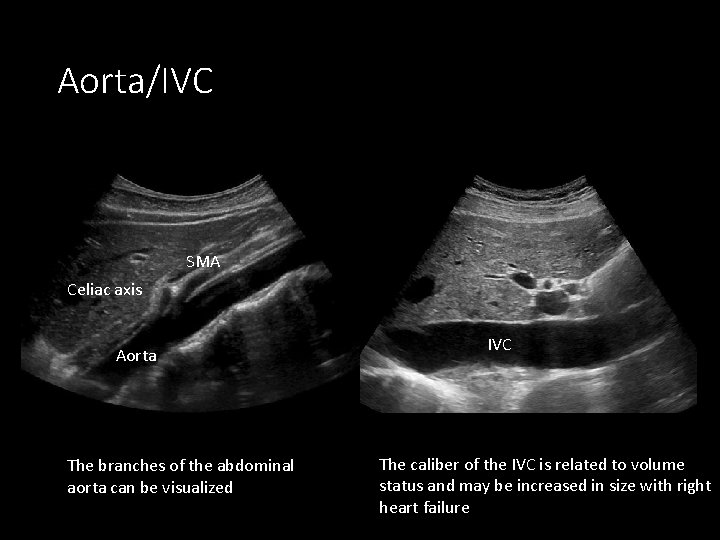
Aorta/IVC SMA Celiac axis Aorta The branches of the abdominal aorta can be visualized IVC The caliber of the IVC is related to volume status and may be increased in size with right heart failure
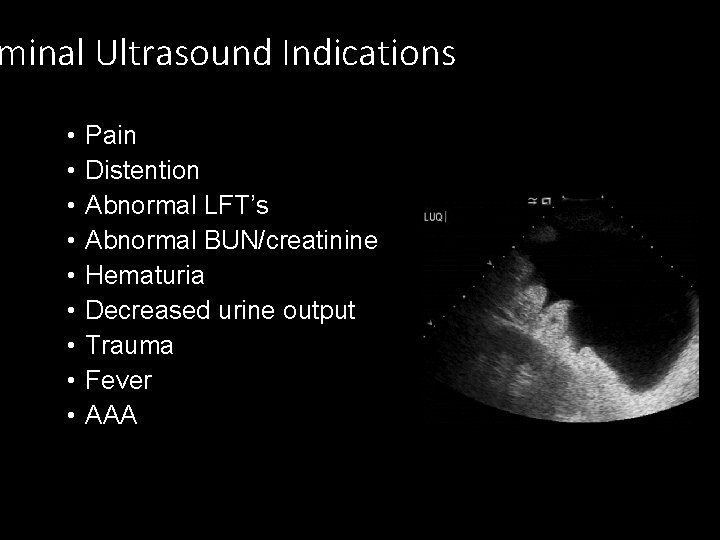
minal Ultrasound Indications • • • Pain Distention Abnormal LFT’s Abnormal BUN/creatinine Hematuria Decreased urine output Trauma Fever AAA

Patient Considerations • NPO for 6 hours • will minimize the amount of obscuring bowel gas • will allow the gallbladder to distend with bile, making detection of gallstones easier • Patient mobility • Repositioning the patient in a decubitus position can move bowel gas away from an area of interest, improving visualization • Bandages/tubes on the abdomen • will limit the areas on the abdomen (acoustic windows) through which you can image

A few examples of pathology on abdominal ultrasound

Identifying Pathology on Ultrasound Examples to Consider
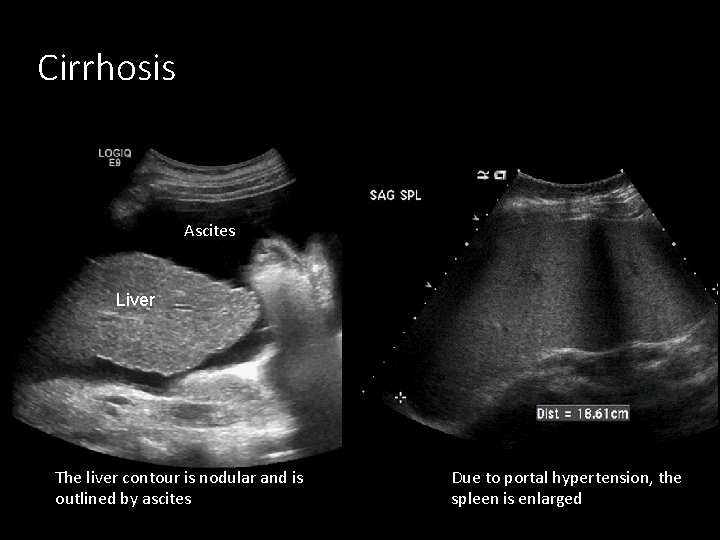
Cirrhosis Ascites Liver The liver contour is nodular and is outlined by ascites Due to portal hypertension, the spleen is enlarged
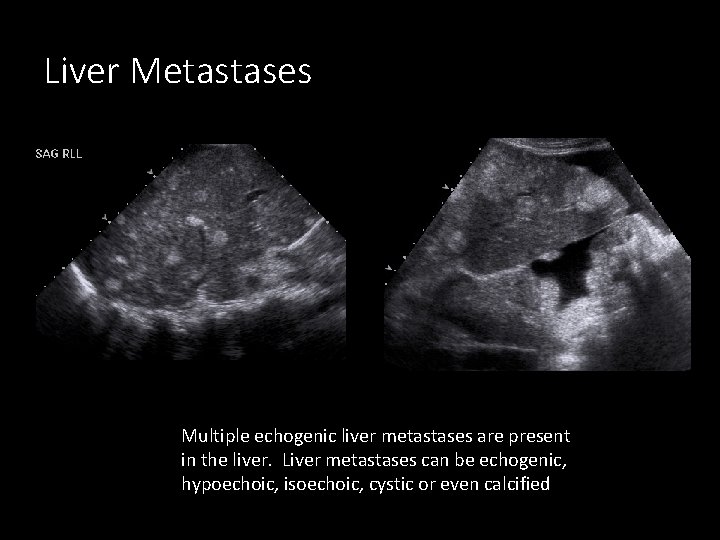
Liver Metastases Multiple echogenic liver metastases are present in the liver. Liver metastases can be echogenic, hypoechoic, isoechoic, cystic or even calcified
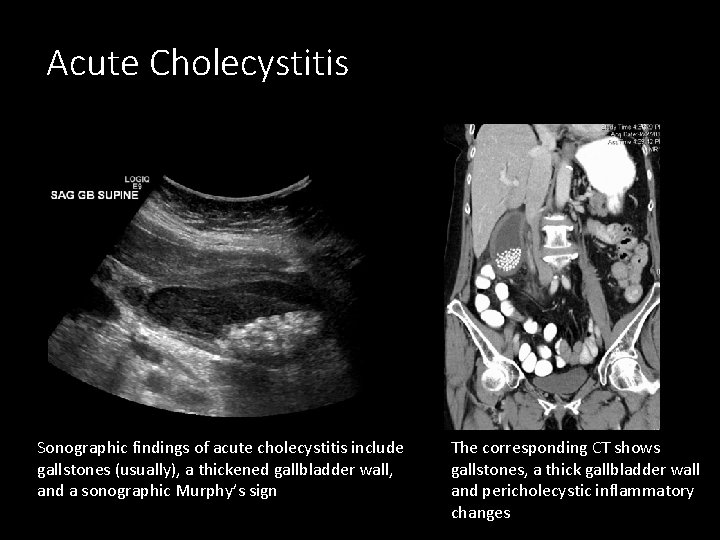
Acute Cholecystitis Sonographic findings of acute cholecystitis include gallstones (usually), a thickened gallbladder wall, and a sonographic Murphy’s sign The corresponding CT shows gallstones, a thick gallbladder wall and pericholecystic inflammatory changes
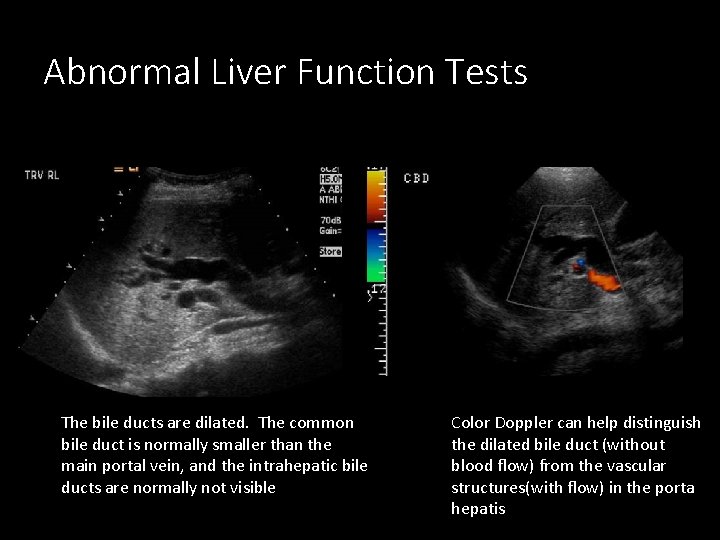
Abnormal Liver Function Tests The bile ducts are dilated. The common bile duct is normally smaller than the main portal vein, and the intrahepatic bile ducts are normally not visible Color Doppler can help distinguish the dilated bile duct (without blood flow) from the vascular structures(with flow) in the porta hepatis
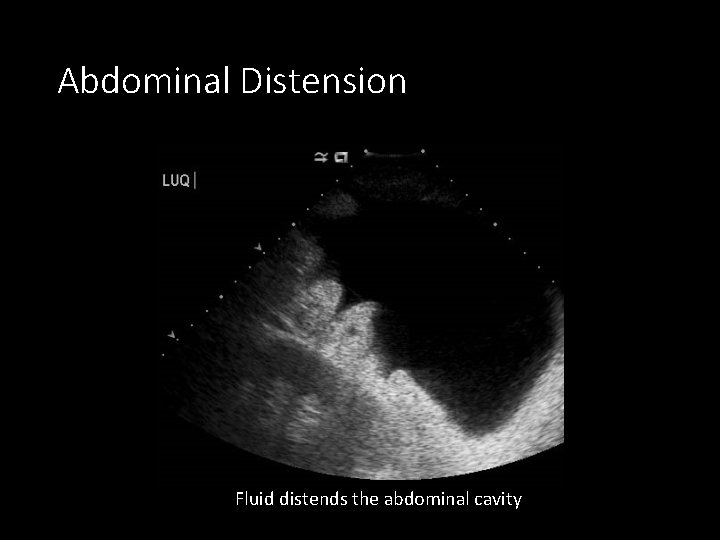
Abdominal Distension Fluid distends the abdominal cavity
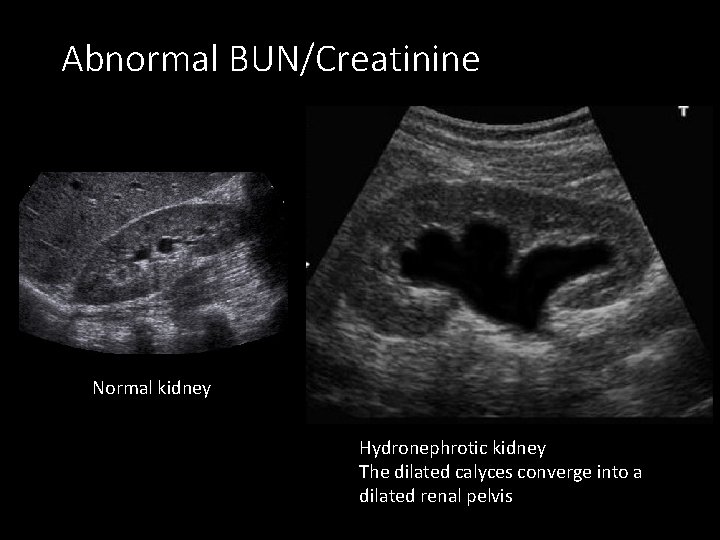
Abnormal BUN/Creatinine Normal kidney Hydronephrotic kidney The dilated calyces converge into a dilated renal pelvis
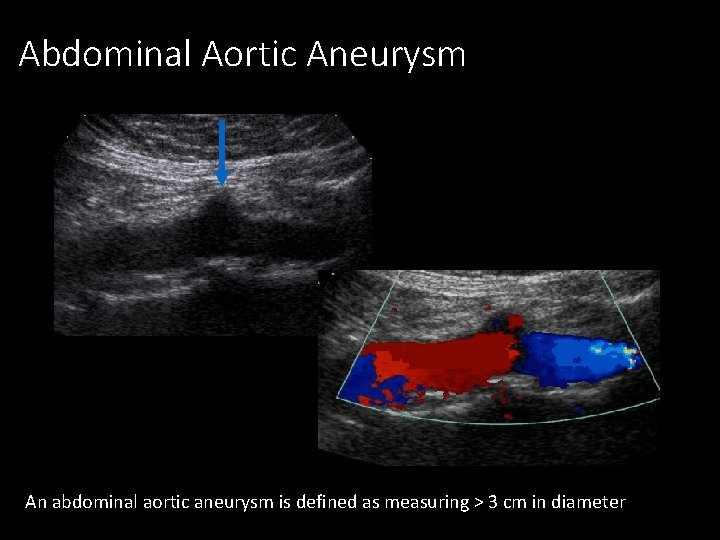
Abdominal Aortic Aneurysm An abdominal aortic aneurysm is defined as measuring > 3 cm in diameter

Summary • Advantages of ultrasound: • No radiation • Portable • Cost effective • Abdominal Ultrasound can be used to diagnose common abnormalities, including liver disease, cholecystitis, biliary obstruction, hydronephrosis, splenomegaly, ascites, and abdominal aortic aneurysm

END
- Slides: 56