Interpretation of renal biochemistry Doc Dr Mine KUCUR

Interpretation of renal biochemistry Doc. Dr. Mine KUCUR

Overview n Renal function tests n Tests for GFR n Urinalysis n Tests for Renal Tubular Acidosis n Tests of Kidney Concentrating Ability n Summary

Renal function tests n Detect renal damage n Monitor functional damage n Help determine etiology
Laboratory tests of renal function n urine protein n glomerular filtration rate n n n (GFR) plasma creatinine plasma urea urine volume urine urea minerals in urine glucose n hematuria n osmolality

Tests of renal function n glomerular filtration rate=GFR n plasma creatinine= Pcr n plasma urea-Purea n urine volume= V n urine urea- Uurea n cystatin C in plasma? n urine protein n urine glucose n hematuria n osmolality

Tests of Glomerular Filtration Rate n Urea n Creatinine Clearance n e. GFR n Cystatin C

Glomerular Filtration Rate (GFR) n Volume of blood filtered across glomerulus per unit time n Best single measure of kidney function

GFR Normally 100 -130 ml/min Determined by: • Net filtration pressure across glomerular basement membrane • Permeability and surface area of glomerular basement membrane

GFR n Patient’s remain asymptomatic until there has been a significant decline in GFR n Can be very accurately measured using “goldstandard” technique

GFR n Ideal Marker n Produced normally by the body n Produced at a constant rate n Filtered across glomerular membrane n Removed from the body only by the kidney filtered only, not reabsorbed or secreted

Candidate markers for GFR Inulin + Filtered only – Not made by body; must be injected Creatinine + An endogenous product of muscle metabolism; near-constant production – Filtered, but a bit secreted Urea + An endogenous product of protein intake – Filtered and absorbed; synthesis varies with diet 0

Urea n Used historically as marker of GFR n Freely filtered but both re-absorbed and excreted into the urine n Re-absorption into blood increased with volume depletion; therefore GFR underestimated n Diet, drugs, disease all significantly effect Urea production

Urea n Product of protein catabolism n Filtered n Reabsorbed in proximal tubule n If sodium is avidly reabsorbed, so is urea n Serum urea concentration measured as “Blood Urea Nitrogen (BUN)”

Urea n Increase n Decrease n Volume depletion n Volume Expansion n Dietary protein n Liver disease n Corticosteroids n Severe malnutrition n Tetracyclines n Blood in G-I tract

Why does BUN increase? GFR, but also: Increased renal reabsorption: n ECV depletion Increased hepatic urea synthesis n High protein feeding n Corticosteroid treatment (Prednisone, etc. ) n GI blood absorption

BUN: Uses n Imperfect marker of GFR n Marker for adequacy of protein intake n Marker for presence of uremic toxins in chronic renal failure n BUN: Cr ratio reflects ECV volume status: n n 10: 1 = normal >20: 1 if ECV contracted. Why? ? ? Proximal tubule Na and urea reabsorption!

Creatinine n Product of muscle metabolism n Some creatinine is of dietary origin n Freely filtered, but also actively secreted into urine n Secretion is affected by several drugs

Serum Creatinine n Increase n Male n Meat in diet n Muscular body type n Cimetidine & some other medications n n n Decrease Age Female Malnutrition Muscle wasting Amputation

Serum Creatinine Concentration n Normally 0. 7 -1. 4 mg/dl, depending on muscle mass n Inversely proportional to GFR n Good way to follow changes in GFR n BUT also elevated by muscle mass, tubular secretion

Creatinine Clearance n Measure serum and urine creatinine levels and urine volume and calculate serum volume cleared of creatinine n Same issues as with serum creatinine, except muscle mass n Requirements for 24 hour urine collection adds variability and inconvenience

Creatinine Clearance n Therefore, it represents the volume of serum completely cleared of creatinine per unit time n Since virtually all creatinine is cleared via glomerular filtration, it closely approximates the GFR

Creatinine Clearance EXAMPLE: UCr = 72 mg/dl SCr = 2. 0 mg/dl V = 2 liters time = 24 hours
![Limitations of Creatinine Clearance n Only valid at steady state—[Cr]serum must be stable n Limitations of Creatinine Clearance n Only valid at steady state—[Cr]serum must be stable n](http://slidetodoc.com/presentation_image/241875f52a0c62daaef8f22411e38e7b/image-23.jpg)
Limitations of Creatinine Clearance n Only valid at steady state—[Cr]serum must be stable n Trimethoprim, cimetidine lower tubular Cr secretion and lower Cr. Cl without changing GFR: n Becomes more inaccurate at low GFR

Another Problem with Creatinine Clearance n Must be done on a properly collected, timed urine sample--patient error n How can we check accuracy of any timed urine collection?

Creatinine Excretion n The amount of creatinine excreted per day is stable for a given patient n It is function of muscle mass: generally higher in men vs. women, youth vs. elderly n expressed per kg lean body mass as the creatinine index

Quick formulae for estimating GFR Include some combination of sex, weight, serum creatinine, race, and age. Use only at steady state (stable SCr) Useful screens for decreased GFR, esp. in elderly and small people, where errors in drug dosing may be major

Creatinine Test Summary

Cystatin C n Cystatin C is a 13 KD protein produced by all cells at a constant rate n Freely filtered n Re-absorbed and catabolized by the kidney and does not appear in the urine

e. GFR n Increasing requirements for dialysis and transplant (8 – 10% per year) n Shortage of transplantable kidneys n Large number at risk
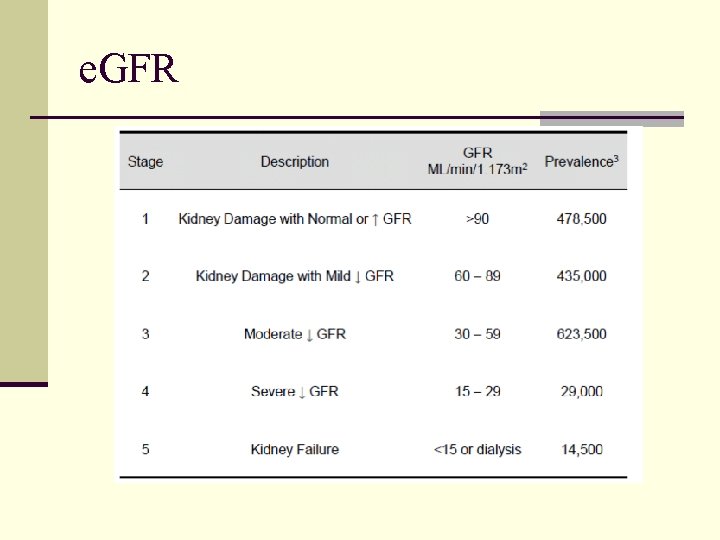
e. GFR
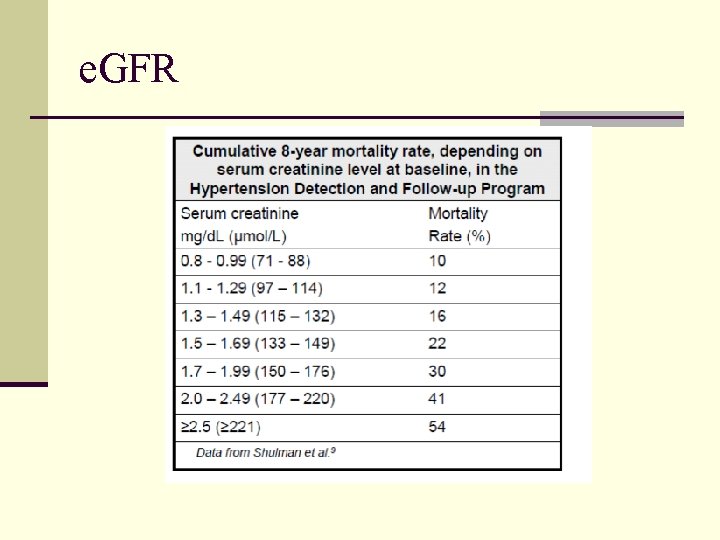
e. GFR

Problem n Need an easy test to screen for early decreases in GFR that you can apply to a large, at-risk population n Can serum creatinine be made more sensitive by adding more information?

e. GFR by MDRD Formula n Mathematically modified serum creatinine with additional information from patients age, sex and ethnicity n e. GFR = 30849. 2 x (serum creatinine)-1. 154 x (age)-0. 203 (if female x (0. 742))

e. GFR n e. GFR calculation has been recommended by National Kidney Foundation whenever a serum creatinine is performed in adults

Screen High Risk Groups n e. GFR n Urinalysis n Albumin / Creatinine Ratio

Tests that predict kidney disease n e. GFR n Albumin Creatinine Ratio (aka ACR or Microalbumin)

Proteinuria n In health: n High molecular weight proteins are retained in the circulation by the glomerular filter (Albumin, Immunoglobulins) n Low molecular weight proteins are filtered then reabsorbed by renal tubular cells

Proteinuria n Glomerular: n Mostly albumin, because of its high concentration and therefore high filtered load n Tubular: n Low molecular weight proteins not reabsorbed by tubular cells (e. g. alpha-1 microglobulin) n Overflow: n Excessive filtration of one protein exceeds reabsorbtive capacity (Bence-Jones, myoglobin)

Albumin Creatinine Ratio (Microalbumin) n Normal albumin molecule n In health, there is very little or no albumin in the urine n Most dip sticks report albumin at greater than 150 mg/L

Urinary Albumin n Detection of low levels of albumin (even if below dipstick cut-off) is predictive of future kidney disease with diabetes n Very significant biologic variation usually requires repeat collections n Treatment usually based on timed urine albumin collections

Follow-up based on Screen Results n Kidney Ultrasound n Specialist Referral n Cardiovascular Risk Assessment n Diabetes Control n Smoking cessation n Hepatitis / Influenza Management

Creatinine Standardization in British Columbia n Based on Isotope dilution /mass spectrometry measurements of creatinine standards n Permits estimation and correction of creatinine and e. GFR bias at the laboratory level

Importance of Standardization n Low bias creatinine: n Causes inappropriately increased e. GFR n Patients will not receive the benefits of more intensive investigation of treatment n High bias creatinine: n Causes inappropriately decreased e. GFR n Patients receive investigations and treatment which is not required. Wastes time, resources and increases anxiety.

Poor Creatinine Precision n Incorrect categorization of patients with both “normal” and decreased e. GFR.

Total Error n TE = % bias + 1. 96 CV n Goal is <10% (requires bias ≤ 4% and CV ≤ 3%)

Kidney Functions n Selectively secretes into or re-absorbs from the filtrate to maintain n Water Balance n n Retention of nutrients n n Tests: specific gravity, osmolarity, water deprivation testing, Antidiuretic hormone Tests: proteins, sugar, amino acids, phosphate Secretes waste products n Tests: urate, oxalate, bile salts

Kidney Functions n Selectively secretes into or re-absorbs from the filtrate to maintain n Salt Balance n n Tests: Na+, Cl-, K+ Aldosterone, Renin Acid Base Balance n Tests: p. H, HCO 3 -, NH 4+ Acid loading, Urinary Anion Gap

Kidney Functions n Target organ n Parathyroid hormone (Ca++, Mg++) n Aldosterone (salt balance) n ADH (water balance) n Production n Erythropoietin n 1, 25 dihydroxycholecalciferol

Urinalysis n Dipstick n Protein n Useful screening test Dipstick more sensitive to albumin than other proteins Large biologic variation

Urinalysis n Dipstick – cont’d n Hemoglobin n Glomerular, tubular or post-renal source Reasonably sensitive Positive dipstick and negative microscopy with lysed red cells

Urinalysis n Dipstick – cont’d n Glucose n Reasonable technically, however screening and monitoring programs for diabetes are now done by blood and Point-of-Care devices

Specific Gravity n Approximate only n Measurement of osmolarity preferred when concentrating ability being assessed

p. H n p. H changes with time in a collected urine n Calculations to determine urine ammonium levels and response to acid-loading generally required to assess for renal tubular acidosis

Microscopic Urinalysis n Epithelial Cells n Squamous, Transitional, Renal n n n All may be present in small numbers Important to recognize possible malignancy Comment on unusual numbers

Renal Tubular Epithelial

Red Cells n May originate in any part of the urinary tract n Small numbers may be normal n There is provincial protocol for the investigation of persistent hematuria

White Blood Cells n Neutrophils often present in small numbers n Lymphocytes and moncytes less often n Marker for infection or inflammation

Casts n Hyaline and granular casts not always pathologic, clinical correlation required n Red cell casts always significant, usually glomerular injury n WBC casts also always significant, usually infection, sometimes inflammation n Bacterial casts only found in pyelonephritis n Waxy casts found in significant kidney disease

Tests for Renal Tubular Acidosis n Urinary Anion Gap (Na+ + K+) – Cln In acidosis the kidney should excrete NH 4+ and the gap will be negative

RTA n If NH 4 + is not present (or if HCO 3 - is present) the gap will be neutral or positive, implying impaired kidney handling of acid load. Urine Anion Gap = (Na+ + K+) –Cl-

RTA n Ammonium Chloride Loading n Load with ammonium chloride n Hourly measurements of urine p. H n Normal at least one p. H below 5. 5

Tests of Kidney Concentrating Ability n To differentiate n Psychogenic polydipsia n Central diabetes insipidus n Nephrogenic diabetes insipidus

Overnight Water Deprivation Testing n (Serum osmolarity <295 monitor patient weight hourly) n Collect urine hourly from 0600 for osmolarity n Baseline serum osmolarity, Na+, ADH n When osmolarity plateaus repeat above tests and administer ADH

Interpretation n If urine concentrates (osmolarity >600 and serum osmolarity below <295) n Normal physiology (? Psychogenic polydipsia)

No Urine Concentration No Response to ADH n Nephrogenic diabetes insipidus

No Urine Concentration n Positive response to ADH n Central diabetes insipidus

To summarize: 1. Use the Creatinine Clearance as the best estimate of GFR 2. Use the Serum Creatinine to follow renal function over time 3. Use the Creatinine Index to check the adequacy of a urine collection 4. Use the BUN to help assess GFR, volume status, and protein intake
- Slides: 67