International Neurourology Journal 2016 20 59 68 Comparison





- Slides: 15

International Neurourology Journal 2016; 20: 59 -68 Comparison of Predictive Factors for Postoperative Incontinence of Holmium Laser Enucleation of the Prostate by the Surgeons’ Experience During Learning Curve Katsumi Shigemura, Kazushi Tanaka, Fukashi Yamamichi, Koji Chiba, Masato Fujisawa Division of Urology, Department of Organ Therapeutics, Faculty of Medicine, Kobe University Graduate School of Medicine, Kobe, Japan This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http: //creativecommons. org/licenses/by-nc/3. 0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.

International Neurourology Journal 2016; 20: 59 -68 PURPOSE • To detect predictive factors for postoperative incontinence following holmium laser enucleation of the prostate (Ho. LEP) according to surgeon experience (beginner or experienced) and preoperative clinical data.

International Neurourology Journal 2016; 20: 59 -68 Methods • Of 224 patients, a total of 203 with available data on incontinence were investigated. • The potential predictive factors for post-Ho. LEP incontinence included clinical factors, such as patient age, and preoperative urodynamic study results, including detrusor overactivity (DO). • We also classified the surgeons performing the procedure according to their Ho. LEP experience: beginner (<21 cases) and experienced (≥ 21 cases).

International Neurourology Journal 2016; 20: 59 -68 Results • Our statistical data showed DO was a significant predictive factor at the super-short period (the next day of catheter removal: odds ratio [OR], 3. 375; P=0. 000). • Additionally, patient age, surgeon mentorship (inverse correlation), and prostate volume were significant predictive factors at the 1 -month interval after Ho. LEP (OR, 1. 072; P=0. 004; OR, 0. 251; P=0. 002; and OR, 1. 008; P=0. 049, respectively). • With regards to surgeon experience, DO and preoperative International Prostate Symptom Score (inverse) at the super-short period, and patient age and mentorship (inverse correlation) at the 1 -month interval after Ho. LEP (OR, 3. 952; P=0. 002; OR, 1. 084; P=0. 015; and OR, 1. 084; P=0. 015; OR, 0. 358; P=0. 003, respectively) were significant predictive factors for beginners, and first desire to void (FDV) at 1 month after Ho. LEP (OR, 1. 009; P=0. 012) was a significant predictive factor for experienced surgeons in multivariate analysis.

International Neurourology Journal 2016; 20: 59 -68 Conclusions • Preoperative DO, IPSS, patient age, and surgeon mentorship were significant predictive factors of postoperative patient incontinence for beginner surgeons, while FDV was a significant predictive factors for experienced surgeons. • These findings should be taken into account by surgeons performing Ho. LEP to maximize the patient’s quality of life with regards to urinary continence.

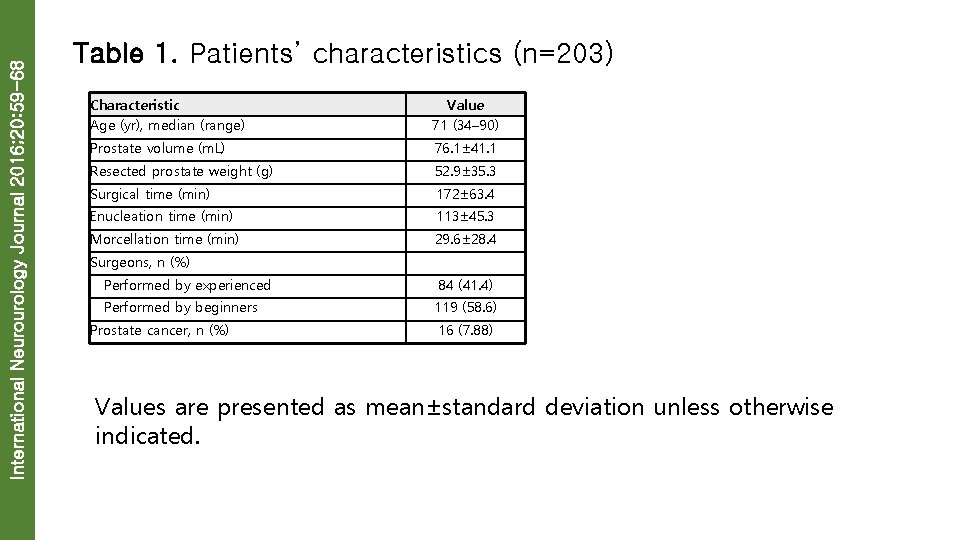
International Neurourology Journal 2016; 20: 59 -68 Table 1. Patients’ characteristics (n=203) Characteristic Age (yr), median (range) Value 71 (34– 90) Prostate volume (m. L) 76. 1± 41. 1 Resected prostate weight (g) 52. 9± 35. 3 Surgical time (min) 172± 63. 4 Enucleation time (min) 113± 45. 3 Morcellation time (min) 29. 6± 28. 4 Surgeons, n (%) Performed by experienced 84 (41. 4) Performed by beginners 119 (58. 6) Prostate cancer, n (%) 16 (7. 88) Values are presented as mean±standard deviation unless otherwise indicated.

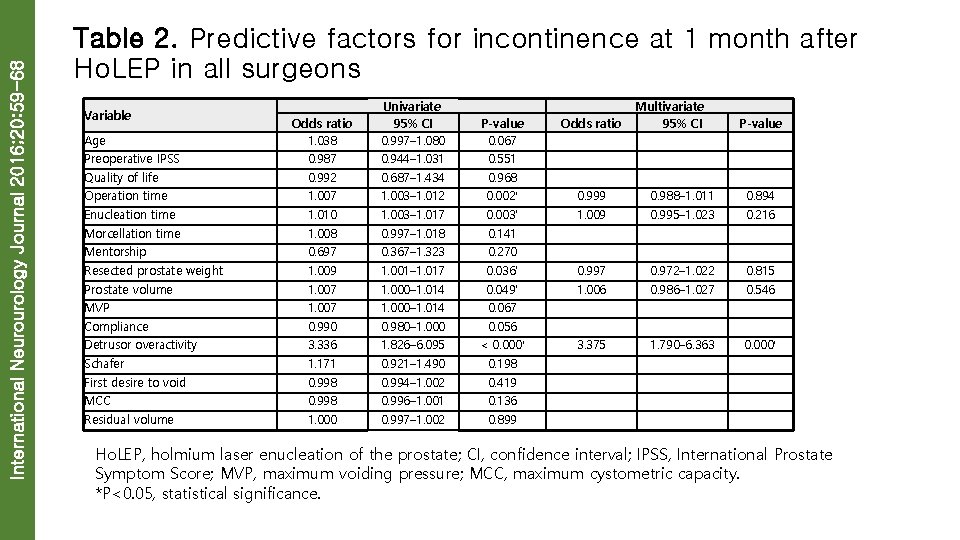
International Neurourology Journal 2016; 20: 59 -68 Table 2. Predictive factors for incontinence at 1 month after Ho. LEP in all surgeons Odds ratio 1. 038 Univariate 95% CI 0. 997– 1. 080 P-value 0. 067 Odds ratio Preoperative IPSS 0. 987 0. 944– 1. 031 0. 551 Quality of life 0. 992 0. 687– 1. 434 0. 968 Operation time 1. 007 1. 003– 1. 012 0. 002* 0. 999 0. 988– 1. 011 0. 894 1. 009 0. 995– 1. 023 0. 216 Variable Age Multivariate 95% CI P-value Enucleation time 1. 010 1. 003– 1. 017 0. 003* Morcellation time 1. 008 0. 997– 1. 018 0. 141 Mentorship 0. 697 0. 367– 1. 323 0. 270 0. 997 0. 972– 1. 022 0. 815 Resected prostate weight 1. 009 1. 001– 1. 017 0. 036* Prostate volume 1. 007 1. 000– 1. 014 0. 049* 1. 006 0. 986– 1. 027 0. 546 MVP 1. 007 1. 000– 1. 014 0. 067 Compliance 0. 990 0. 980– 1. 000 0. 056 Detrusor overactivity 3. 336 1. 826– 6. 095 < 0. 000* 3. 375 1. 790– 6. 363 0. 000* Schafer 1. 171 0. 921– 1. 490 0. 198 First desire to void 0. 998 0. 994– 1. 002 0. 419 MCC 0. 998 0. 996– 1. 001 0. 136 Residual volume 1. 000 0. 997– 1. 002 0. 899 Ho. LEP, holmium laser enucleation of the prostate; CI, confidence interval; IPSS, International Prostate Symptom Score; MVP, maximum voiding pressure; MCC, maximum cystometric capacity. *P<0. 05, statistical significance.

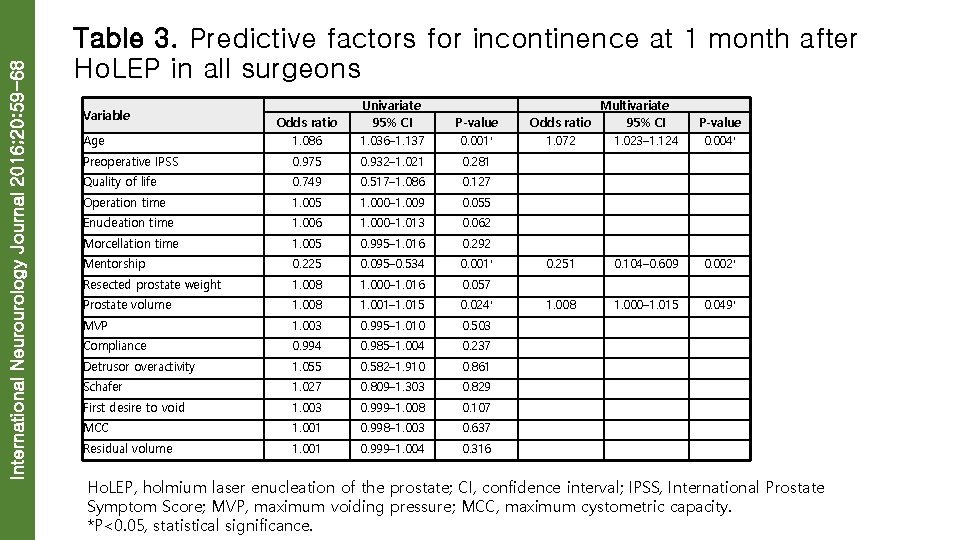
International Neurourology Journal 2016; 20: 59 -68 Table 3. Predictive factors for incontinence at 1 month after Ho. LEP in all surgeons Odds ratio 1. 086 Univariate 95% CI 1. 036– 1. 137 P-value 0. 001* Preoperative IPSS 0. 975 0. 932– 1. 021 0. 281 Quality of life 0. 749 0. 517– 1. 086 0. 127 Operation time 1. 005 1. 000– 1. 009 0. 055 Enucleation time 1. 006 1. 000– 1. 013 0. 062 Morcellation time 1. 005 0. 995– 1. 016 0. 292 Mentorship 0. 225 0. 095– 0. 534 0. 001* 0. 251 0. 104– 0. 609 0. 002* Resected prostate weight 1. 008 1. 000– 1. 016 0. 057 Prostate volume 1. 008 1. 001– 1. 015 0. 024* 1. 008 1. 000– 1. 015 0. 049* MVP 1. 003 0. 995– 1. 010 0. 503 Compliance 0. 994 0. 985– 1. 004 0. 237 Detrusor overactivity 1. 055 0. 582– 1. 910 0. 861 Schafer 1. 027 0. 809– 1. 303 0. 829 First desire to void 1. 003 0. 999– 1. 008 0. 107 MCC 1. 001 0. 998– 1. 003 0. 637 Residual volume 1. 001 0. 999– 1. 004 0. 316 Variable Age Multivariate Odds ratio 95% CI 1. 072 1. 023– 1. 124 P-value 0. 004* Ho. LEP, holmium laser enucleation of the prostate; CI, confidence interval; IPSS, International Prostate Symptom Score; MVP, maximum voiding pressure; MCC, maximum cystometric capacity. *P<0. 05, statistical significance.

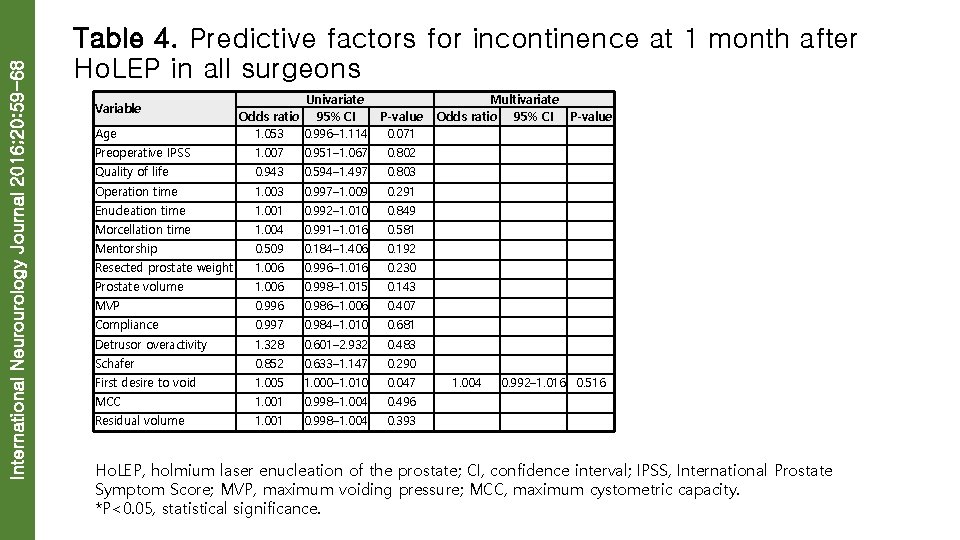
International Neurourology Journal 2016; 20: 59 -68 Table 4. Predictive factors for incontinence at 1 month after Ho. LEP in all surgeons Variable Age Univariate Odds ratio 95% CI 1. 053 0. 996– 1. 114 P-value 0. 071 Multivariate Odds ratio 95% CI P-value Preoperative IPSS 1. 007 0. 951– 1. 067 0. 802 Quality of life 0. 943 0. 594– 1. 497 0. 803 Operation time 1. 003 0. 997– 1. 009 0. 291 Enucleation time 1. 001 0. 992– 1. 010 0. 849 Morcellation time 1. 004 0. 991– 1. 016 0. 581 Mentorship 0. 509 0. 184– 1. 406 0. 192 Resected prostate weight 1. 006 0. 996– 1. 016 0. 230 Prostate volume 1. 006 0. 998– 1. 015 0. 143 MVP 0. 996 0. 986– 1. 006 0. 407 Compliance 0. 997 0. 984– 1. 010 0. 681 Detrusor overactivity 1. 328 0. 601– 2. 932 0. 483 Schafer 0. 852 0. 633– 1. 147 0. 290 First desire to void 1. 005 1. 000– 1. 010 0. 047 1. 004 MCC 1. 001 0. 998– 1. 004 0. 496 Residual volume 1. 001 0. 998– 1. 004 0. 393 0. 992– 1. 016 0. 516 Ho. LEP, holmium laser enucleation of the prostate; CI, confidence interval; IPSS, International Prostate Symptom Score; MVP, maximum voiding pressure; MCC, maximum cystometric capacity. *P<0. 05, statistical significance.

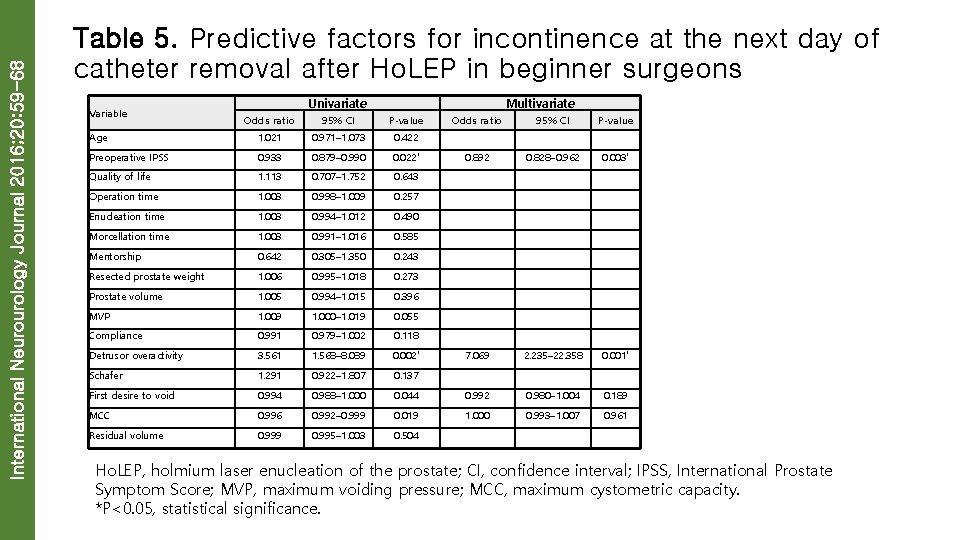
International Neurourology Journal 2016; 20: 59 -68 Table 5. Predictive factors for incontinence at the next day of catheter removal after Ho. LEP in beginner surgeons Variable Univariate Multivariate Odds ratio 95% CI P-value Age 1. 021 0. 971– 1. 073 0. 422 Preoperative IPSS 0. 933 0. 879– 0. 990 0. 022* 0. 892 0. 828– 0. 962 0. 003* Quality of life 1. 113 0. 707– 1. 752 0. 643 Operation time 1. 003 0. 998– 1. 009 0. 257 Enucleation time 1. 003 0. 994– 1. 012 0. 490 Morcellation time 1. 003 0. 991– 1. 016 0. 585 Mentorship 0. 642 0. 305– 1. 350 0. 243 Resected prostate weight 1. 006 0. 995– 1. 018 0. 273 Prostate volume 1. 005 0. 994– 1. 015 0. 396 MVP 1. 009 1. 000– 1. 019 0. 055 Compliance 0. 991 0. 979– 1. 002 0. 118 Detrusor overactivity 3. 561 1. 568– 8. 089 0. 002* 7. 069 2. 235– 22. 358 0. 001* Schafer 1. 291 0. 922– 1. 807 0. 137 First desire to void 0. 994 0. 988– 1. 000 0. 044 0. 992 0. 980– 1. 004 0. 189 MCC 0. 996 0. 992– 0. 999 0. 019 1. 000 0. 993– 1. 007 0. 961 Residual volume 0. 999 0. 995– 1. 003 0. 504 Ho. LEP, holmium laser enucleation of the prostate; CI, confidence interval; IPSS, International Prostate Symptom Score; MVP, maximum voiding pressure; MCC, maximum cystometric capacity. *P<0. 05, statistical significance.

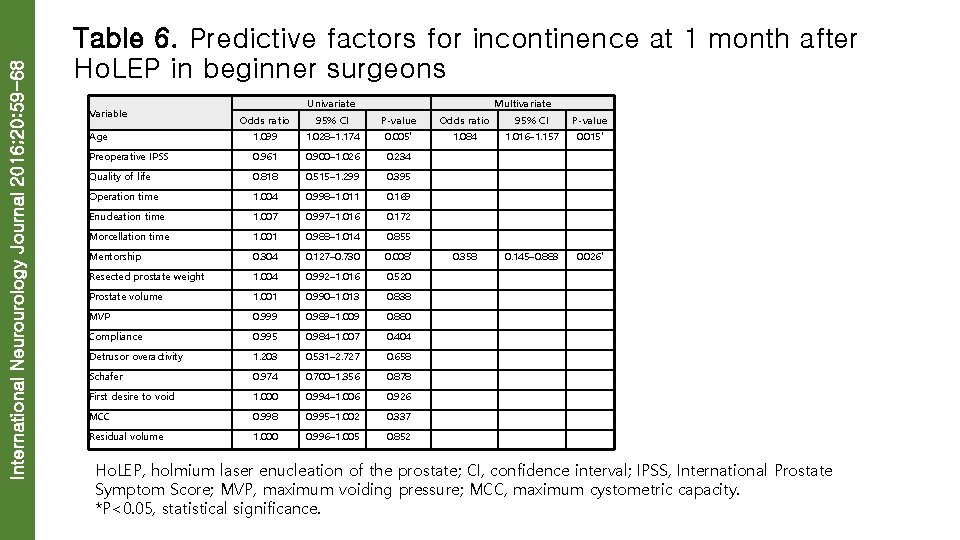
International Neurourology Journal 2016; 20: 59 -68 Table 6. Predictive factors for incontinence at 1 month after Ho. LEP in beginner surgeons Variable Univariate Odds ratio Multivariate 95% CI P-value Odds ratio 95% CI P-value 1. 084 1. 016– 1. 157 0. 015* Age 1. 099 1. 028– 1. 174 0. 005* Preoperative IPSS 0. 961 0. 900– 1. 026 0. 234 Quality of life 0. 818 0. 515– 1. 299 0. 395 Operation time 1. 004 0. 998– 1. 011 0. 169 Enucleation time 1. 007 0. 997– 1. 016 0. 172 Morcellation time 1. 001 0. 988– 1. 014 0. 855 Mentorship 0. 304 0. 127– 0. 730 0. 008* 0. 358 0. 145– 0. 883 0. 026* Resected prostate weight 1. 004 0. 992– 1. 016 0. 520 Prostate volume 1. 001 0. 990– 1. 013 0. 838 MVP 0. 999 0. 989– 1. 009 0. 880 Compliance 0. 995 0. 984– 1. 007 0. 404 Detrusor overactivity 1. 203 0. 531– 2. 727 0. 658 Schafer 0. 974 0. 700– 1. 356 0. 878 First desire to void 1. 000 0. 994– 1. 006 0. 926 MCC 0. 998 0. 995– 1. 002 0. 337 Residual volume 1. 000 0. 996– 1. 005 0. 852 Ho. LEP, holmium laser enucleation of the prostate; CI, confidence interval; IPSS, International Prostate Symptom Score; MVP, maximum voiding pressure; MCC, maximum cystometric capacity. *P<0. 05, statistical significance.

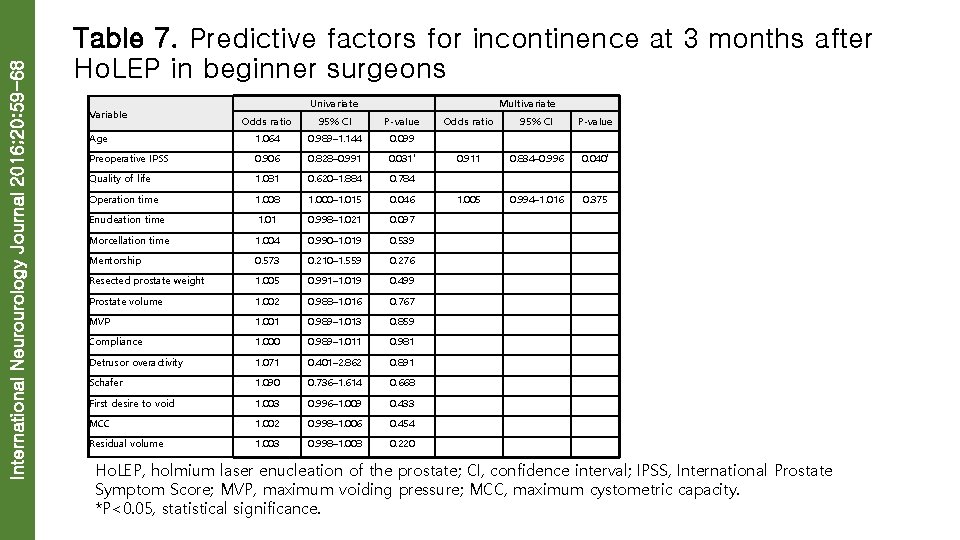
International Neurourology Journal 2016; 20: 59 -68 Table 7. Predictive factors for incontinence at 3 months after Ho. LEP in beginner surgeons Variable Univariate Multivariate Odds ratio 95% CI P-value Age 1. 064 0. 989– 1. 144 0. 099 Preoperative IPSS 0. 906 0. 828– 0. 991 0. 031* 0. 911 0. 834– 0. 996 0. 040* Quality of life 1. 081 0. 620– 1. 884 0. 784 Operation time 1. 008 1. 000– 1. 015 0. 046 1. 005 0. 994– 1. 016 0. 375 Enucleation time 1. 01 0. 998– 1. 021 0. 097 Morcellation time 1. 004 0. 990– 1. 019 0. 539 Mentorship 0. 573 0. 210– 1. 559 0. 276 Resected prostate weight 1. 005 0. 991– 1. 019 0. 499 Prostate volume 1. 002 0. 988– 1. 016 0. 767 MVP 1. 001 0. 989– 1. 013 0. 859 Compliance 1. 000 0. 989– 1. 011 0. 981 Detrusor overactivity 1. 071 0. 401– 2. 862 0. 891 Schafer 1. 090 0. 736– 1. 614 0. 668 First desire to void 1. 003 0. 996– 1. 009 0. 433 MCC 1. 002 0. 998– 1. 006 0. 454 Residual volume 1. 003 0. 998– 1. 008 0. 220 Ho. LEP, holmium laser enucleation of the prostate; CI, confidence interval; IPSS, International Prostate Symptom Score; MVP, maximum voiding pressure; MCC, maximum cystometric capacity. *P<0. 05, statistical significance.

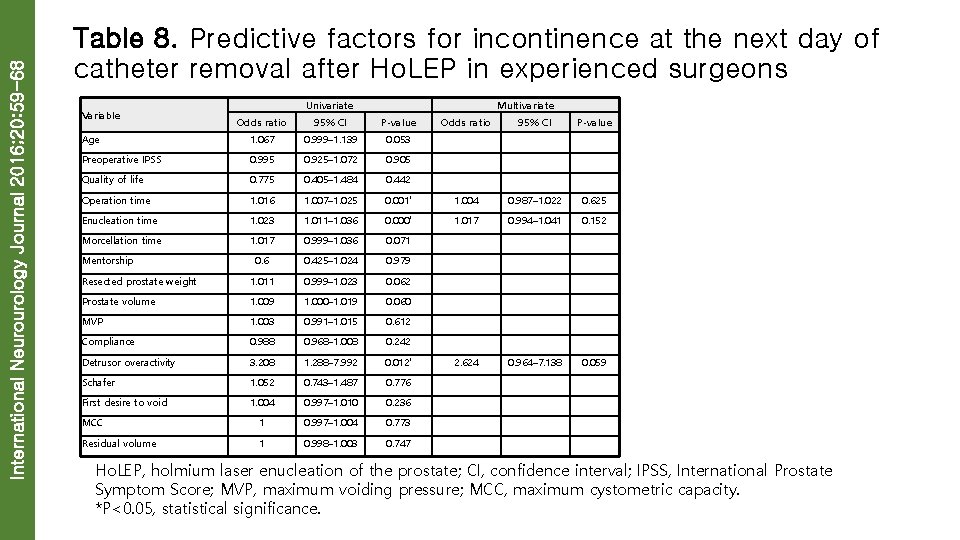
International Neurourology Journal 2016; 20: 59 -68 Table 8. Predictive factors for incontinence at the next day of catheter removal after Ho. LEP in experienced surgeons Variable Univariate Multivariate Odds ratio 95% CI P-value Age 1. 067 0. 999– 1. 139 0. 053 Preoperative IPSS 0. 995 0. 925– 1. 072 0. 905 Quality of life 0. 775 0. 405– 1. 484 0. 442 Operation time 1. 016 1. 007– 1. 025 0. 001* 1. 004 0. 987– 1. 022 0. 625 Enucleation time 1. 023 1. 011– 1. 036 0. 000* 1. 017 0. 994– 1. 041 0. 152 Morcellation time 1. 017 0. 999– 1. 036 0. 071 0. 6 0. 425– 1. 024 0. 979 Resected prostate weight 1. 011 0. 999– 1. 023 0. 062 Prostate volume 1. 009 1. 000– 1. 019 0. 060 MVP 1. 003 0. 991– 1. 015 0. 612 Compliance 0. 988 0. 968– 1. 008 0. 242 Detrusor overactivity 3. 208 1. 288– 7. 992 0. 012* 2. 624 0. 964– 7. 138 0. 059 Schafer 1. 052 0. 743– 1. 487 0. 776 First desire to void 1. 004 0. 997– 1. 010 0. 236 MCC 1 0. 997– 1. 004 0. 773 Residual volume 1 0. 998– 1. 003 0. 747 Mentorship Ho. LEP, holmium laser enucleation of the prostate; CI, confidence interval; IPSS, International Prostate Symptom Score; MVP, maximum voiding pressure; MCC, maximum cystometric capacity. *P<0. 05, statistical significance.

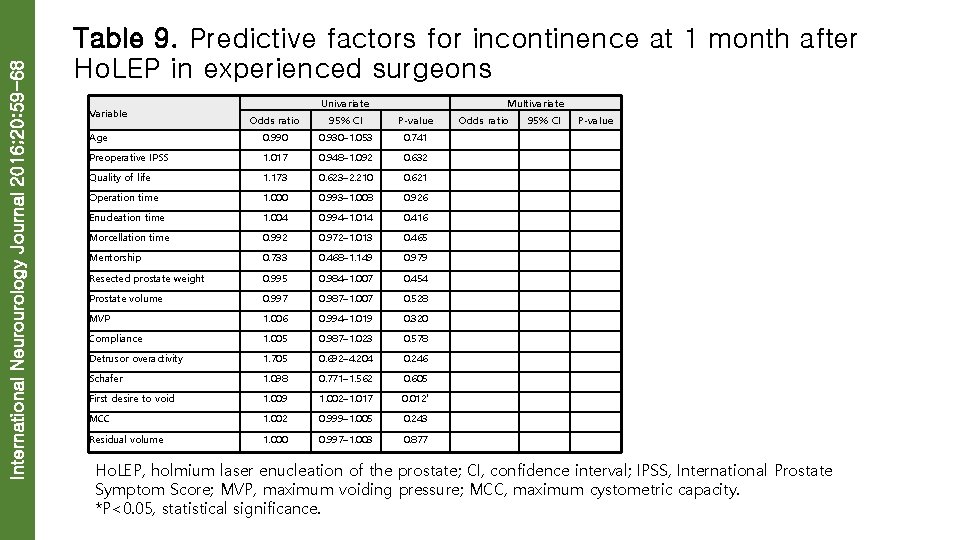
International Neurourology Journal 2016; 20: 59 -68 Table 9. Predictive factors for incontinence at 1 month after Ho. LEP in experienced surgeons Variable Univariate Multivariate Odds ratio 95% CI P-value Age 0. 990 0. 930– 1. 053 0. 741 Preoperative IPSS 1. 017 0. 948– 1. 092 0. 632 Quality of life 1. 173 0. 623– 2. 210 0. 621 Operation time 1. 000 0. 993– 1. 008 0. 926 Enucleation time 1. 004 0. 994– 1. 014 0. 416 Morcellation time 0. 992 0. 972– 1. 013 0. 465 Mentorship 0. 733 0. 468– 1. 149 0. 979 Resected prostate weight 0. 995 0. 984– 1. 007 0. 454 Prostate volume 0. 997 0. 987– 1. 007 0. 528 MVP 1. 006 0. 994– 1. 019 0. 320 Compliance 1. 005 0. 987– 1. 023 0. 578 Detrusor overactivity 1. 705 0. 692– 4. 204 0. 246 Schafer 1. 098 0. 771– 1. 562 0. 605 First desire to void 1. 009 1. 002– 1. 017 0. 012* MCC 1. 002 0. 999– 1. 005 0. 243 Residual volume 1. 000 0. 997– 1. 003 0. 877 Ho. LEP, holmium laser enucleation of the prostate; CI, confidence interval; IPSS, International Prostate Symptom Score; MVP, maximum voiding pressure; MCC, maximum cystometric capacity. *P<0. 05, statistical significance.

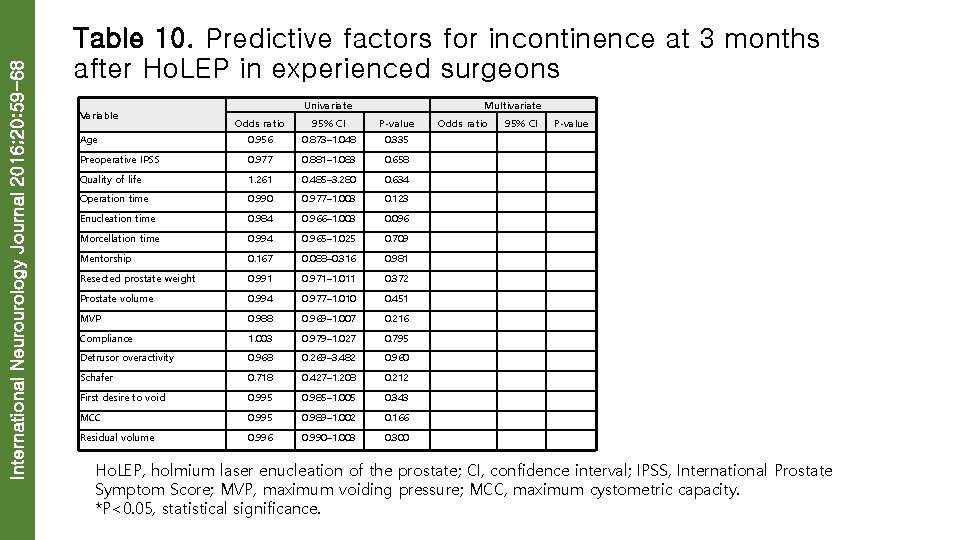
International Neurourology Journal 2016; 20: 59 -68 Table 10. Predictive factors for incontinence at 3 months after Ho. LEP in experienced surgeons Variable Univariate Multivariate Odds ratio 95% CI P-value Age 0. 956 0. 873– 1. 048 0. 335 Preoperative IPSS 0. 977 0. 881– 1. 083 0. 658 Quality of life 1. 261 0. 485– 3. 280 0. 634 Operation time 0. 990 0. 977– 1. 003 0. 123 Enucleation time 0. 984 0. 966– 1. 003 0. 096 Morcellation time 0. 994 0. 965– 1. 025 0. 709 Mentorship 0. 167 0. 088– 0. 316 0. 981 Resected prostate weight 0. 991 0. 971– 1. 011 0. 372 Prostate volume 0. 994 0. 977– 1. 010 0. 451 MVP 0. 988 0. 969– 1. 007 0. 216 Compliance 1. 003 0. 979– 1. 027 0. 795 Detrusor overactivity 0. 968 0. 269– 3. 482 0. 960 Schafer 0. 718 0. 427– 1. 208 0. 212 First desire to void 0. 995 0. 985– 1. 005 0. 343 MCC 0. 995 0. 989– 1. 002 0. 166 Residual volume 0. 996 0. 990– 1. 003 0. 300 Ho. LEP, holmium laser enucleation of the prostate; CI, confidence interval; IPSS, International Prostate Symptom Score; MVP, maximum voiding pressure; MCC, maximum cystometric capacity. *P<0. 05, statistical significance.