Intermittent Positive Pressure Breathing Incentive Spirometry IPPB Indications

Intermittent Positive. Pressure Breathing (간헐적 양압 호흡)


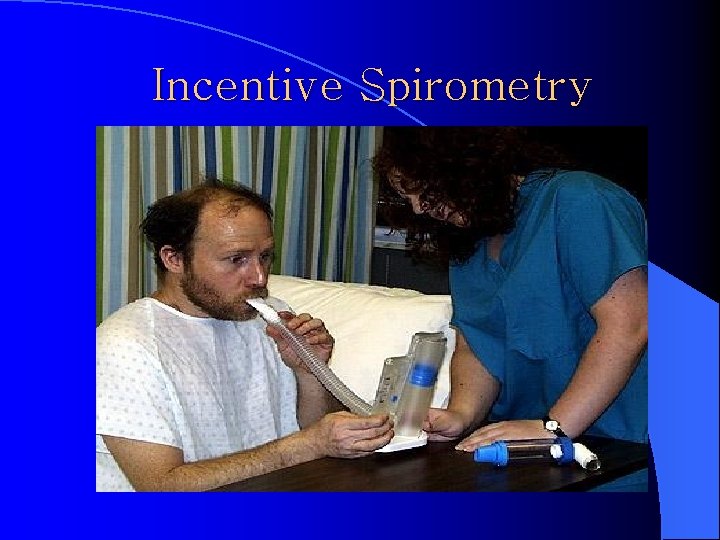
Incentive Spirometry


IPPB Indications – 폐 확장의 개선이 필요한 경우 Treatment of atelectasis not responsive to otherapies, (e. g. , IS and CPT) l 분비물이 적당하게 제거되지 않는 경우 – ventilation 제한 – 비 효과적인 기침 l

IPPB Indications – 과 탄산증 환자를 위한 Short-term nonivasive ventilatory support. l Alternative to intubation and continuous ventilatory support

IPPB Indications – The need to deliver aerosol medication When nebulizer has been unsuccessful l 호흡근육이 약하거나 피로한 경우 l
IPPB Contraindications – Tension pneumothorax – ICP > 15 mm Hg – 혈역학적 불안정 – Recent facial, oral or skull surgery

IPPB Contraindications – Tracheoesophageal fistula – Recent esophageal surgery – Active hemoptysis – Nausea – Air swallowing - 복부팽만.

IPPB Contraindications – Active, untreated TB – Radiographic evidence of bleb – 딸꾹질 (hiccups)

IPPB 위해요인 – Increase airway resistance – Barotrauma, pneumothorax – 병원감염 (Nosocomial infection) – Hyperventilation (hypocapnia) – Hemoptysis

IPPB 위해요인 – Hypoxemia의 악화 – Hypoventilation – 환기/관류 불일치(V/Q mismatch) – 공기누적(Air trapping), auto peep, overdistended alveoli

IPPB l 잠재적 결과 (Potential Outcomes) – Improved 흡기량(IC) or 폐활량(VC) – Increased FEV 1 or peak flow – Enhanced cough or secretion clearance – Improved Chest radiograph *FEV 1=Forced expiratory volume in 1 sec (1초간 노력성 호기): 폐쇄성 폐질환의 지표

IPPB l Potential Outcomes – Improved breath sounds – Improved oxygenation – 환자의 subjective response이 호전.

IPPB l Baseline Assessment – Vital signs – Patient’s appearance and 감각 – Breathing pattern – Breath sounds

IPPB l 실행 (Implementation) – Infection control – Equipment preparation l Pressure check machine/circuit

IPPB l 실행(Implementation) – Patient orientation Why MD ordered therapy l What treatment does l How it feels l Expected results(결과 기대) l
IPPB l 실행 (Implementation) – Application Mouthpiece / nose clip (initially) l Mouth seal l Face Mask l Tracheostomy/endotracheal tube adaptor l

IPPB l Implementation – Machine settings l Sensitivity of 1 – 2 cm H 2 O l Initial pressure between 10 – 15 cm H 20 l Breathing pattern of 6 breaths/min l I: E ration of 1: 3 to 1: 4 l 환자의 요구나 기대(목표)에 따라 Flow와 pressure 조절.

IPPB l Implementation – When treating atelectasis volume-oriented(지향적) Therapy l Tidal volumes (VT) 측정 필요. l VT goals must be set l VT goal of 10 – 15 m. L/kg of body weight l Pressure can be increased to reach VT goal if tolerated by patient l

IPPB l Discontinuation and Follow-Up – Treatments typically last 15 -20 – – minutes Repeat patient assessment Identify untoward effect Evaluate progress 기록 (Document)

Mark 7 Series

IPPB – Bird Series l Mark 7 Series – Pneumatically driven – Can be time, pressure, or manually TRIGGERED – Pressure CYCLED – Can be used to provide short-term ventilatory support – Primarily used for IPPB therapy

IPPB – Bird Series Inspiratory Flow Rate 1. Sensitivity Control Pressure Control Air Dilution Expiratory Timer

IPPB – Bird Series Center Body Gas Source Inlet Ambient Chamber Pressure Chamber Mainstream Hose Connection Hand Timer Pressure Manometer Nebulizer / Exhalation Valve Connection
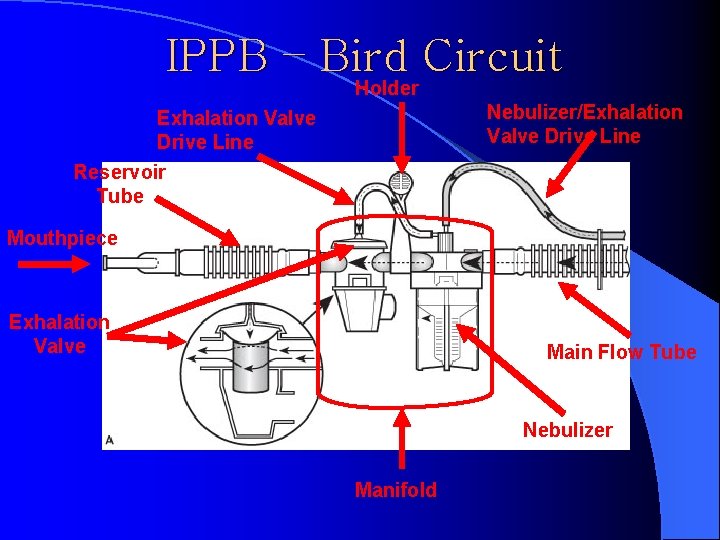
IPPB – Bird Circuit Holder Nebulizer/Exhalation Valve Drive Line Reservoir Tube Mouthpiece Exhalation Valve Main Flow Tube Nebulizer Manifold
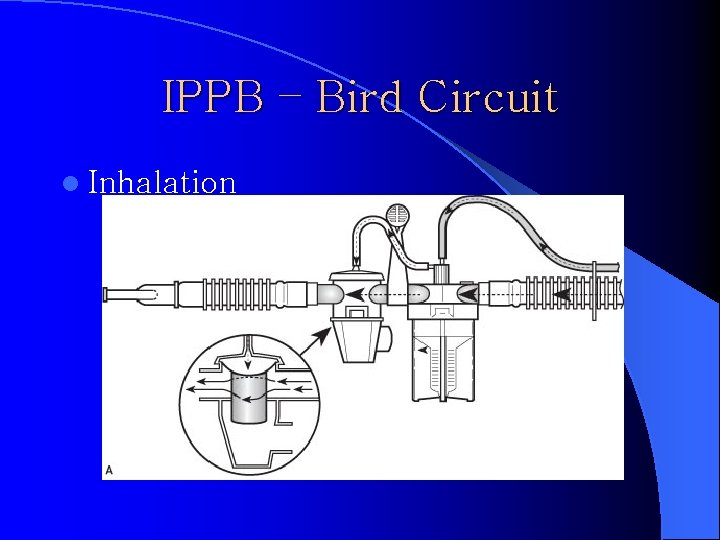
IPPB – Bird Circuit l Inhalation

IPPB – Bird Circuit l Exhalation

IPPB – Bird Circuit
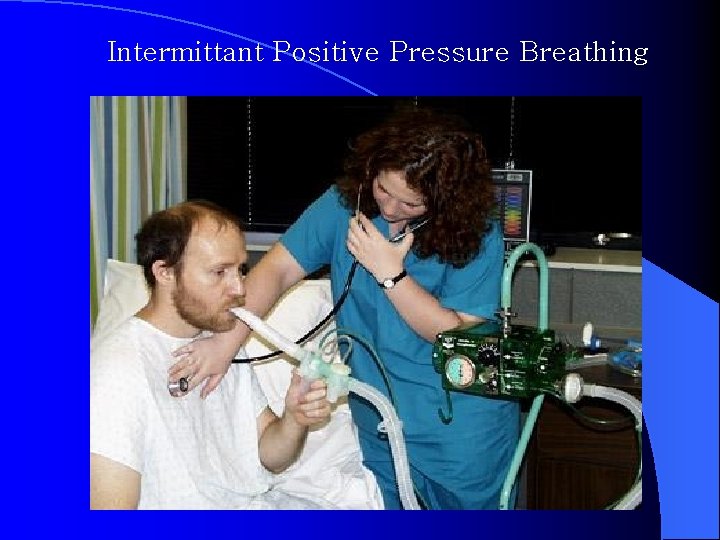
Intermittant Positive Pressure Breathing
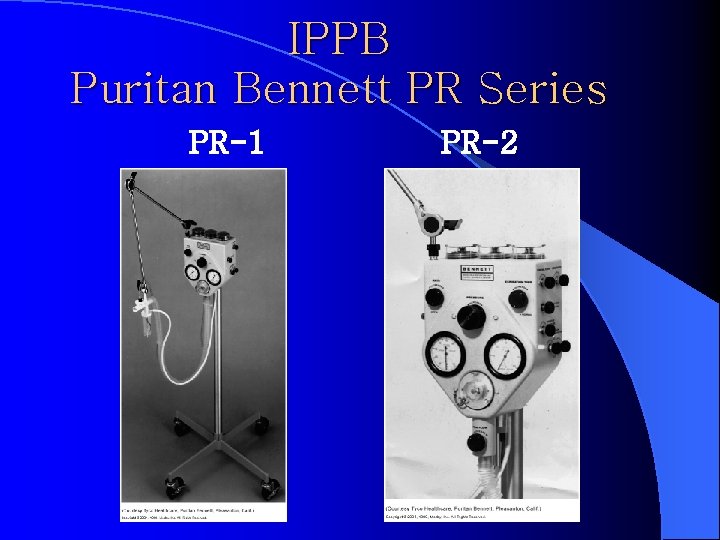
IPPB Puritan Bennett PR Series PR-1 PR-2

IPPB Puritan Bennett PR Series l PR-1 and PR-2 – Pneumatically driven – Can be time, pressure, or manually TRIGGERED – Flow CYCLED, pressure limited – Can be used to provide short-term ventilatory support – Primarily used for IPPB therapy
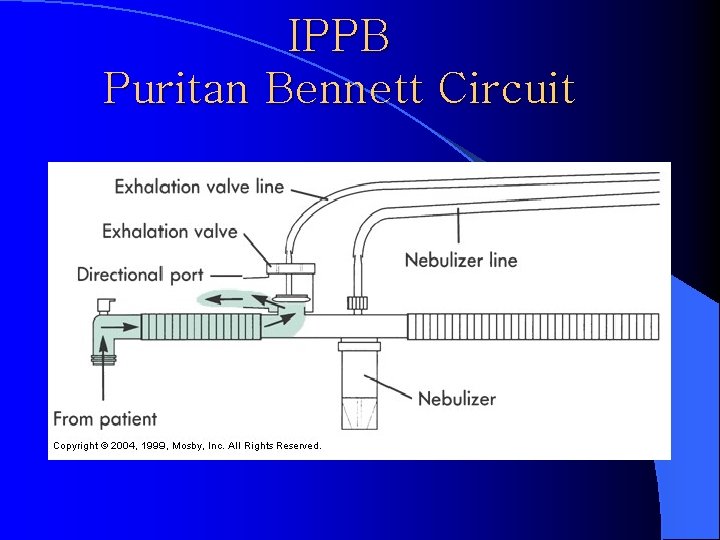
IPPB Puritan Bennett Circuit


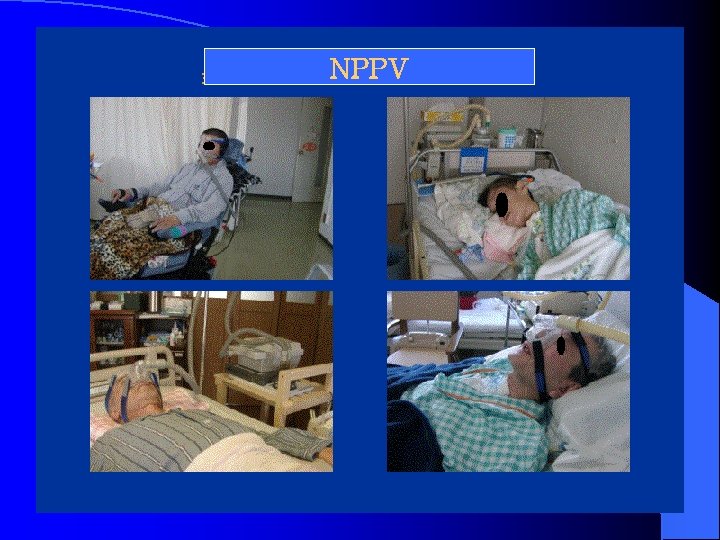
NPPV


- Slides: 39