Interdisciplinary Collaboration in a Community Based Learning Project

Inter-disciplinary Collaboration in a Community- Based Learning Project: Medical Professional Students’ Experiences in a Farmworker Health Project. A MSEDI project Sara Pullen, DPT, MPH, CHES Erin Lepp, MMSC, PA Emily Herndon MD, FAAFP.

Disclosures • No financial relationship with any commercial interest producing any health care goods or services • Will not be discussing any investigational drugs or products • Not affiliated with any speaker’s bureau

Learning Objectives 1. Describe what an academic service-learning project is and how integration of interprofessional student teams can enhance student learning 2. Discuss the advantages and disadvantages of peer teaching in an interprofessional setting 3. Adapt a similar model of interdisciplinary teams with other student-run free clinics in their own institutions.

Introduction Interprofessional collaboration among healthcare workers, especially in the academic setting, has the potential to improve patient outcomes and to train the next generation of healthcare professionals in the importance of working as a cohesive team.

Introduction Providing interdisciplinary educational opportunities and programs to students benefits both the students and the academic institution, as it fosters collaboration and prepares students for an important aspect of their future career.

Background • Current literature describes: – Pro bono clinics in context of medical students – community-academic partnerships for migrant workers • Gap in literature: – lack of research examining specifically PA, MD and PT collaboration for both pro bono clinics and migrant worker health

Project Background

Project Background • Since 2010 the project has grown to include physical therapy (PT) and medical (MD) students

Project Background • In an effort to improve student-learning outcomes during the project, Emory faculty from the 3 departments initiated an interdisciplinary care model for the 2014 SGFP in the hopes to: – foster inter-departmental collaboration – offer students a stronger leaning experience.

Methods • Teams of clinical medical (MD/PA) students paired with PT students • Integrated teams provide care to individual patients • Fosters peer teaching and allows participants to be “student experts” in their respective fields

Methods • Study tool: A one-time use, original, anonymous, written survey designed by the investigators. • One survey given pre-trip at orientation, one given 2 -weeks post-trip • Surveys collect data regarding students’ perspectives on an interdisciplinary servicelearning experience; specific knowledge gained from their non-respective field and confidence in communicating and collaborating with professionals in other fields

Methods • Exempt from Emory University IRB review • Inclusion criteria: students who volunteered with the SGFHP. • Subject recruitment: took place at SGFHP orientation. • Students voluntarily took surveys and could withdraw from study at any time without penalty. Students signed a consent form to complete the survey.

Methods • Quantitative data was analysed with SAS • Qualitative data themes were identified by two reviewers
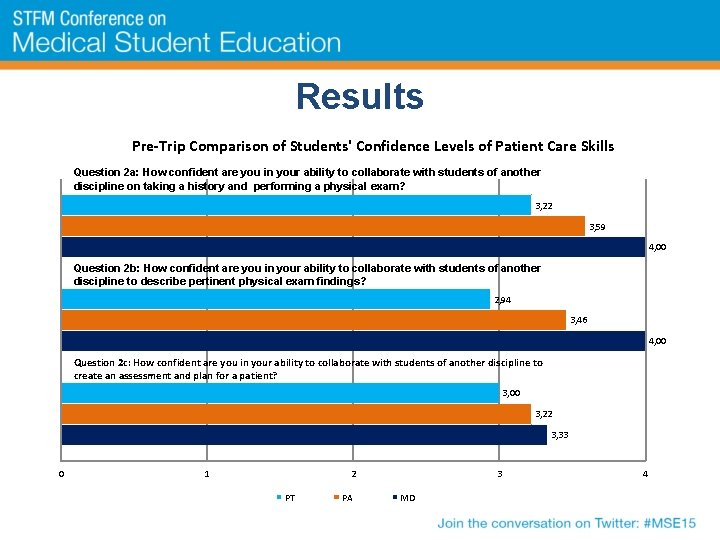
Results Pre-Trip Comparison of Students' Confidence Levels of Patient Care Skills Question 2 a: How confident are you in your ability to collaborate with students of another discipline on taking a history and performing a physical exam? 3, 22 3, 59 4, 00 Question 2 b: How confident are you in your ability to collaborate with students of another discipline to describe pertinent physical exam findings? 2, 94 3, 46 4, 00 Question 2 c: How confident are you in your ability to collaborate with students of another discipline to create an assessment and plan for a patient? 3, 00 3, 22 3, 33 0 1 2 PT PA 3 MD 4
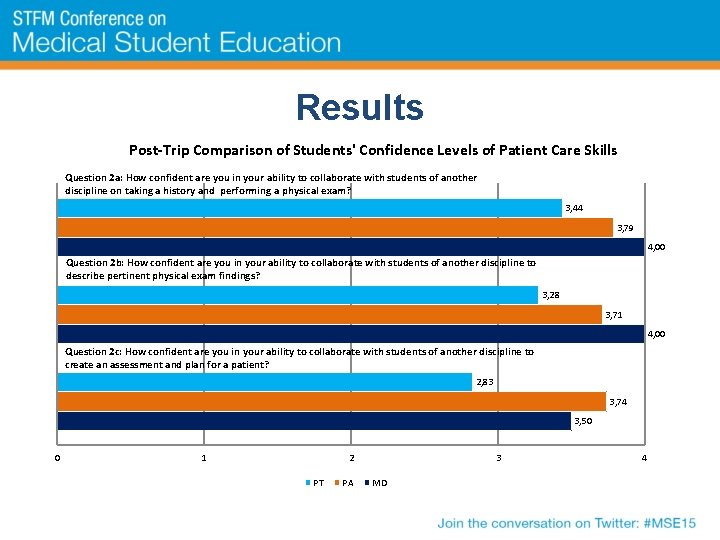
Results Post-Trip Comparison of Students' Confidence Levels of Patient Care Skills Question 2 a: How confident are you in your ability to collaborate with students of another discipline on taking a history and performing a physical exam? 3, 44 3, 79 4, 00 Question 2 b: How confident are you in your ability to collaborate with students of another discipline to describe pertinent physical exam findings? 3, 28 3, 71 4, 00 Question 2 c: How confident are you in your ability to collaborate with students of another discipline to create an assessment and plan for a patient? 2, 83 3, 74 3, 50 0 1 2 PT PA 3 MD 4
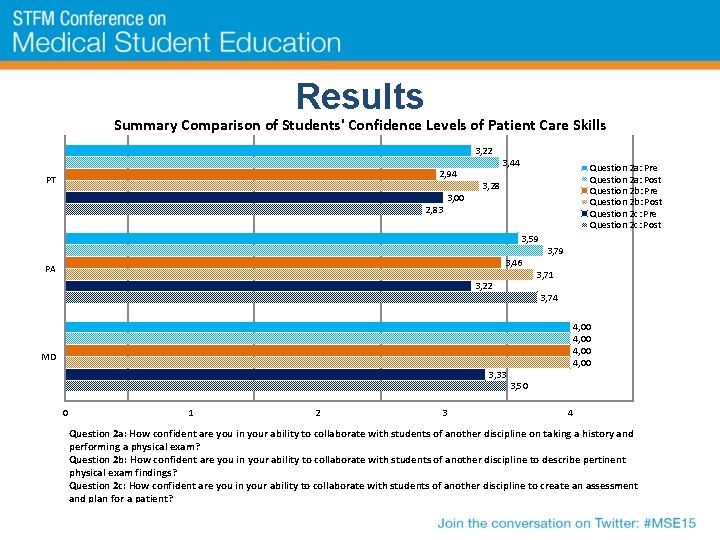
Results Summary Comparison of Students' Confidence Levels of Patient Care Skills 3, 22 2, 94 PT 2, 83 3, 00 3, 44 Question 2 a: Pre Question 2 a: Post Question 2 b: Pre Question 2 b: Post Question 2 c: Pre Question 2 c: Post 3, 28 3, 59 3, 46 PA 3, 22 3, 79 3, 71 3, 74 4, 00 MD 3, 33 0 1 2 3 3, 50 4 Question 2 a: How confident are you in your ability to collaborate with students of another discipline on taking a history and performing a physical exam? Question 2 b: How confident are you in your ability to collaborate with students of another discipline to describe pertinent physical exam findings? Question 2 c: How confident are you in your ability to collaborate with students of another discipline to create an assessment and plan for a patient?
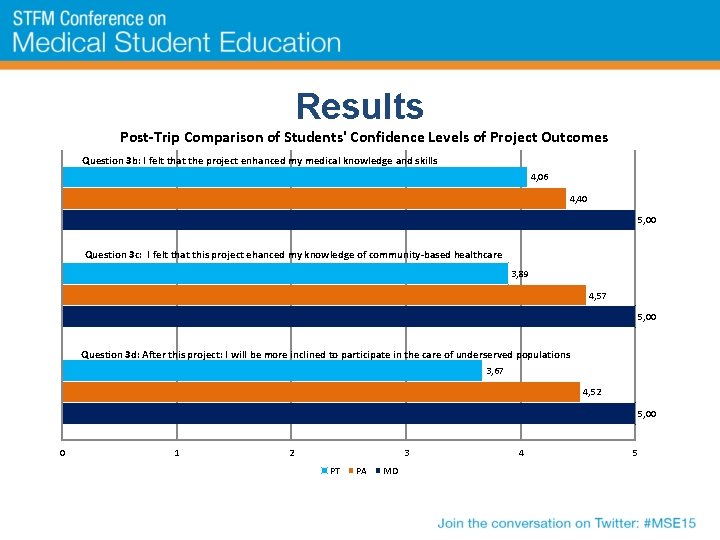
Results Post-Trip Comparison of Students' Confidence Levels of Project Outcomes Question 3 b: I felt that the project enhanced my medical knowledge and skills 4, 06 4, 40 5, 00 Question 3 c: I felt that this project ehanced my knowledge of community-based healthcare 3, 89 4, 57 5, 00 Question 3 d: After this project: I will be more inclined to participate in the care of underserved populations 3, 67 4, 52 5, 00 0 1 2 3 PT PA MD 4 5

Examples of Comments • “Meeting students from other programs and different disciplines of medicine” (PA-S) • “Collaboration among various providers” (MD-S) • “Being able to work alongside a PA student and having the chance to learn how to make a presentation to a MD” (PT-S)

Future Directions: Other Tools • Validated surveys that look at students’ perceptions and attitudes (i. e. IEPS, RIPLS) • Using focus groups to gather qualitative data about students’ experiences that can further shape other opportunities for IPE.

Future Directions: Collaboration With Students From Other Institutions • Adding Marriage and Family Therapy students to the PT/PA/MD team from Valdosta State University • Adding Pharm-D residents from Mercer University College of Pharmacy

Questions or Comments?

Please evaluate this session at: stfm. org/sessionevaluation
- Slides: 22