INTENSIVE INSULIN THERAPY J Robin Conway M D

INTENSIVE INSULIN THERAPY J. Robin Conway M. D. Diabetes Clinic, Smiths Falls, ON 1 -800 -717 -0145 www. diabetesclinic. ca 1

Objectives • Optimize diabetes management • Assist you in initiating insulin in your office – When to start insulin therapy? – Insulins, doses, delivery options – Patient training www. diabetesclinic. ca 2

Challenges in Initiating Insulin? 1. Patient attitudes – Fear of needles – Insulin viewed as a threat by patient & physician – Hypoglycemia 2. Physician Attitudes – Discomfort with insulin • Lack of knowledge and experience – Fear of needles www. diabetesclinic. ca 3

Type 1 Diabetes: • Impaired or absent ß cell function: – insulin secretion • Normal insulin action: – insulin sensitivity • The insulin deficiency results in unacceptable blood glucose control www. diabetesclinic. ca 4

Type 2 Diabetes: Double Impairment • Impaired ß cell function: – insulin secretion • Impaired insulin action: – insulin resistance • Results in unacceptable blood glucose control www. diabetesclinic. ca 5

Type 1 & 2 Diabetes: Key Concepts • Minimizing the complications of diabetes requires: – Early diagnosis and treatment of diabetes – Maintaining Hb. A 1 C level < 7% • Achieving Hb. A 1 C < 7% requires control of post-prandial and fasting hyperglycemia www. diabetesclinic. ca 6
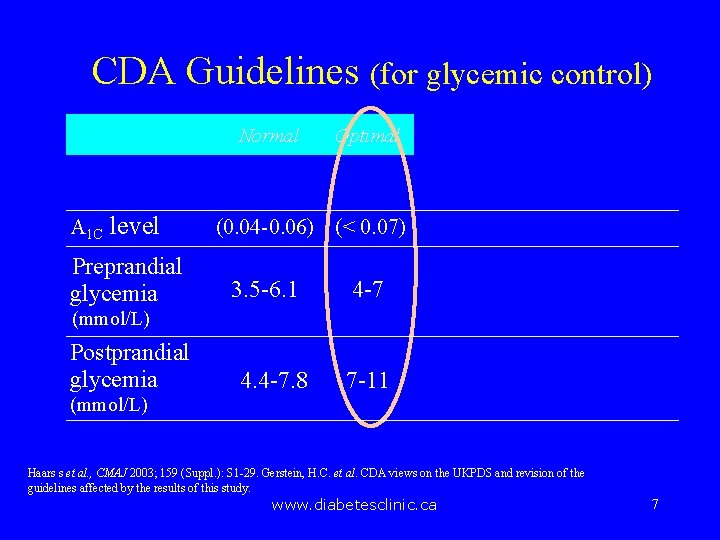

CDA Guidelines (for glycemic control) Normal A 1 C level Preprandial glycemia Optimal (0. 04 -0. 06) (< 0. 07) 3. 5 -6. 1 4 -7 (mmol/L) Postprandial glycemia (mmol/L) 4. 4 -7. 8 7 -11 Haars s et al. , CMAJ 2003; 159 (Suppl. ): S 1 -29. Gerstein, H. C. et al. CDA views on the UKPDS and revision of the guidelines affected by the results of this study. www. diabetesclinic. ca 7

Steps to Glycemic Control • Establish glycemic objectives – Target fasting and post-prandial glycemia • Diet counseling with exercise component • Diabetes education for every patient • Pharmacological treatment; oral and insulin www. diabetesclinic. ca 8

Patient Counselling Topics A. Review symptoms and treatment of hypoglycemia B. Proper training and correct use of glucose monitor C. Target desired glycemic levels for each patient www. diabetesclinic. ca 9

A. Hypoglycemia • Definition: Glycemia < 3. 8 mmol • Patients may experience hypoglycemia at different glycemic levels www. diabetesclinic. ca 10

Symptoms of Hypoglycemia Mild • < 3. 3 mmol/L • Neurovegetative symptoms – – – – Sweating Trembling Palpitations Anxiety Tingling Pallor Hunger Moderate to Severe • < 2. 8 mmol/L • Symptoms of glucopenia – – – – www. diabetesclinic. ca Confusion Visual disturbances Weakness Speech disorder Behavioural disorder Drowsiness Coma Convulsions 11

Preventing Hypoglycemia • Check BG 4 -6 times per day • Carry glucose tablets • Have Glucagon Kit available www. diabetesclinic. ca 12

Preventing Hypoglycemia • Test before driving and ideally 1 hour later (target: over 5. 5 mmol/L) • Perform two SMBG 30 minutes apart prior to bedtime (confirming rising or falling BG) • When drinking alcohol, perform SMBG hourly • With exercise, perform SMBG pre- and postexercise • If hypoglycemia episodes persist, raise target glucose levels www. diabetesclinic. ca 13

Hypoglycemia Treatment Guidelines The Rule of 15 • If BG is 4 mmol/L or below – Treat with 15 grams of carbohydrates (glucose tabs) – Check BG in 15 minutes, and if not above 4 mmol/L, repeat treatment Glucagon • Current emergency kit readily available and knowledgeable person trained to administer www. diabetesclinic. ca 14

Preventing Hyperglycemia and DKA • Monitor BG 4 -6 times per day • Use Correction Boluses when appropriate www. diabetesclinic. ca 15

Hyperglycemia Treatment Guidelines The Key to Preventing DKA 1 st BG over 14 mmol/L: • Take a correction bolus, check again in 1 hour • Call physician immediately or go to ER if nausea and vomiting are present www. diabetesclinic. ca 16

B. Patient Training • Training by a multidisciplinary team at DEC is IDEAL for: – – Diet counseling Education on the injection sites Education on the various injection devices Evaluation of the patient’s support network • Other resources may exist for training, i. e. retail pharmacy www. diabetesclinic. ca 17
C. Blood Glucose Monitoring • To adjust the insulin treatment • To detect or confirm hypoglycemia or severe hyperglycemia • To adjust treatment to the circumstances of daily life using an insulin scale prescribed by the attending physician • To improve patient safety and increase motivation to comply with treatment www. diabetesclinic. ca 18

Ideal Testing Frequency • Stable type 2 – 1 -2 readings/day • Type 1 or Unstable type 2 – 3 -8 readings/day • Important to stress the need to vary testing times – AC, PC, h. s. and prn during the night www. diabetesclinic. ca 19

Injection Tools and Options • Durable delivery devices – Novolin-Pen® 3 – Novolin-Pen® Junior – In. Duo® – Innovo® – Huma. Pen® • Insulin pumps • Syringes • Disposable: multidose, prefilled (3. 0 m. L) – Novolin. Set® (NPH, Toronto, 30/70 ) – Humulin® N www. diabetesclinic. ca 20
Advancing Insulin Therapy Through Device Innovation www. diabetesclinic. ca 21

Goal of Insulin Therapy We are trying to duplicate how the pancreas works in releasing insulin for someone who doesn’t have diabetes www. diabetesclinic. ca 22
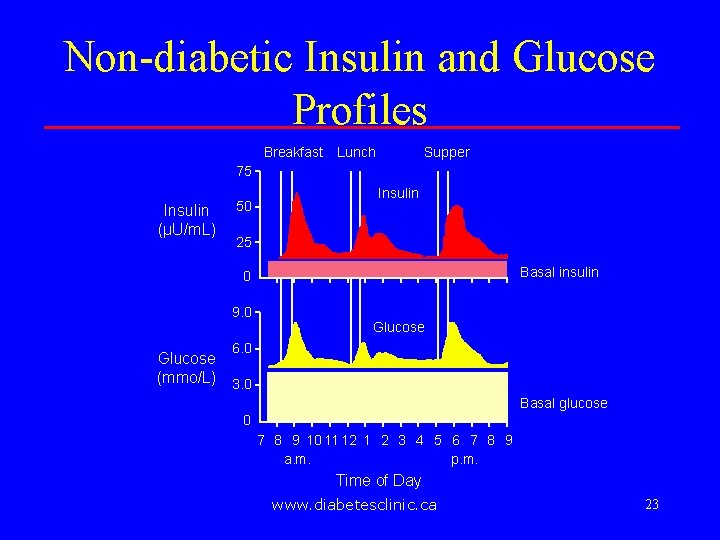
Non-diabetic Insulin and Glucose Profiles Breakfast Lunch Supper 75 Insulin (µU/m. L) 50 Insulin 25 Basal insulin 0 9. 0 Glucose 6. 0 Glucose (mmo/L) 3. 0 Basal glucose 0 7 8 9 10 11 12 1 2 3 4 5 6 7 8 9 a. m. p. m. Time of Day www. diabetesclinic. ca 23
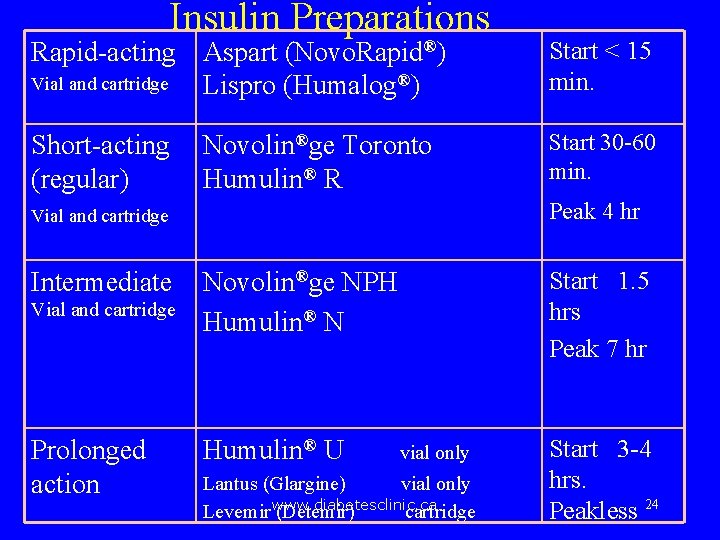
Insulin Preparations Rapid-acting Aspart (Novo. Rapid®) Vial and cartridge Lispro (Humalog®) Start < 15 min. Short-acting (regular) Start 30 -60 min. Novolin®ge Toronto Humulin® R Peak 4 hr Vial and cartridge Intermediate Vial and cartridge Prolonged action Start 1. 5 hrs Peak 7 hr Novolin®ge NPH Humulin® N Humulin® U vial only Lantus (Glargine) vial only Levemirwww. diabetesclinic. ca (Detemir) cartridge Start 3 -4 hrs. Peakless 24

Insulin Pre. Mixes • Regular + intermediate – Novolin® 10/90, 20/80, 30/70, 40/60, 50/50 – Humulin® 30/70, 20/80 • Analogue Pre-Mix – Humalog® 25/75 (insulin lispro protamine suspension) – Novo. Mix 30* (protaminated insulin aspart) * Not available www. diabetesclinic. ca 25
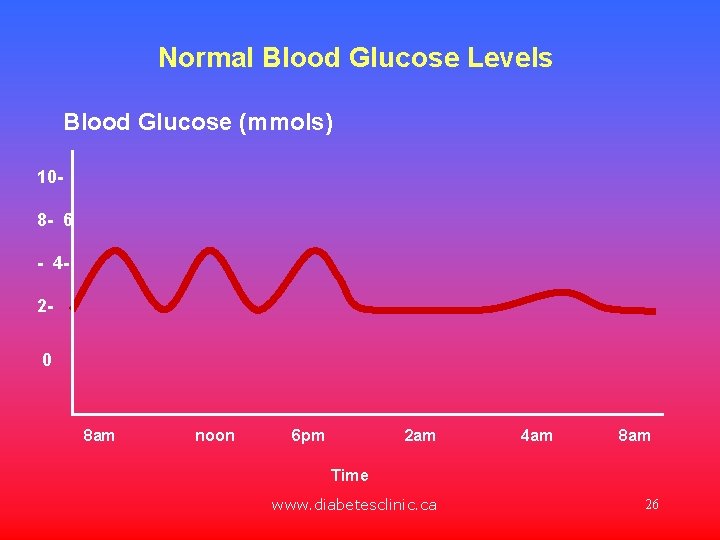
Normal Blood Glucose Levels Blood Glucose (mmols) 108 - 6 - 420 8 am noon 6 pm 2 am 4 am 8 am Time www. diabetesclinic. ca 26
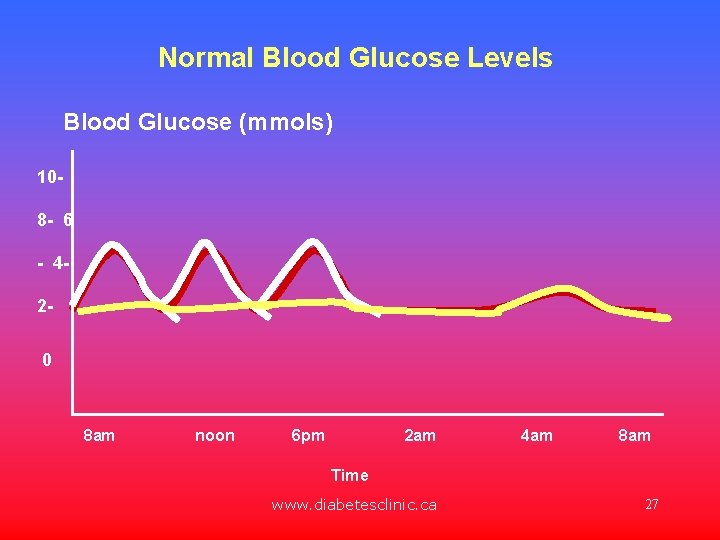
Normal Blood Glucose Levels Blood Glucose (mmols) 108 - 6 - 420 8 am noon 6 pm 2 am 4 am 8 am Time www. diabetesclinic. ca 27
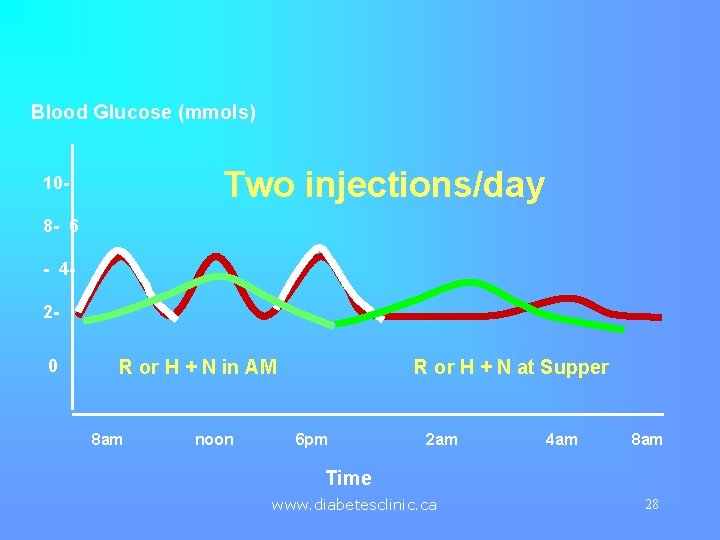
Blood Glucose (mmols) Two injections/day 108 - 6 - 420 R or H + N in AM 8 am noon R or H + N at Supper 6 pm 2 am 4 am 8 am Time www. diabetesclinic. ca 28
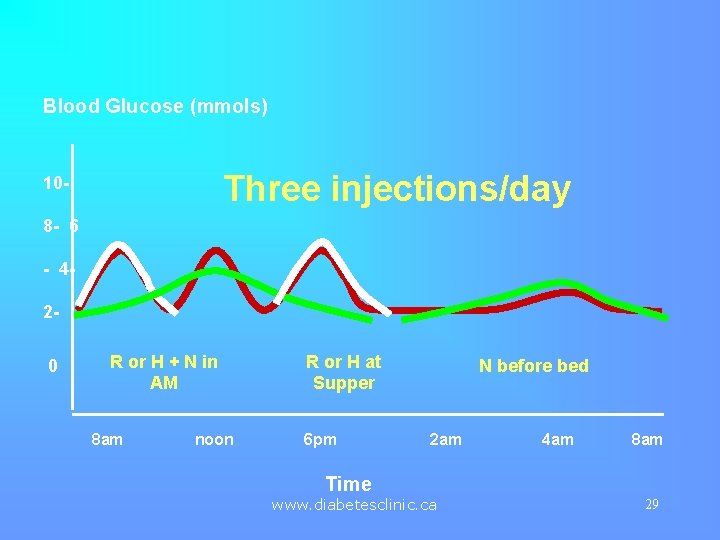
Blood Glucose (mmols) Three injections/day 108 - 6 - 420 R or H + N in AM 8 am noon R or H at Supper 6 pm N before bed 2 am 4 am 8 am Time www. diabetesclinic. ca 29
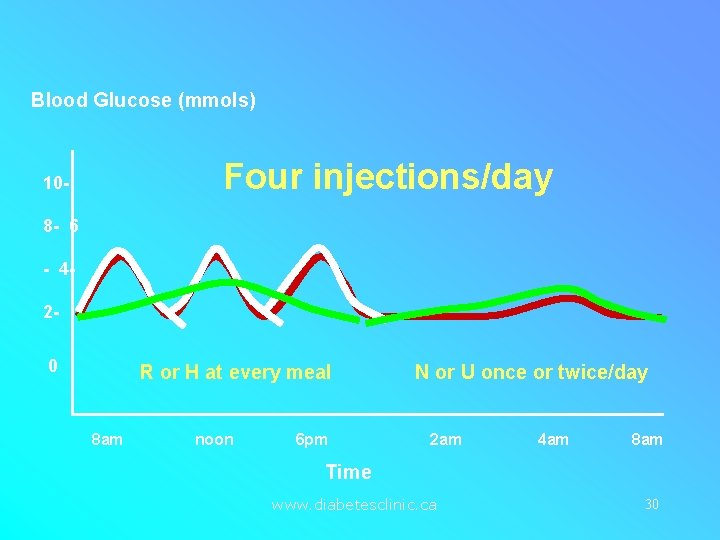
Blood Glucose (mmols) Four injections/day 108 - 6 - 420 R or H at every meal 8 am noon 6 pm N or U once or twice/day 2 am 4 am 8 am Time www. diabetesclinic. ca 30
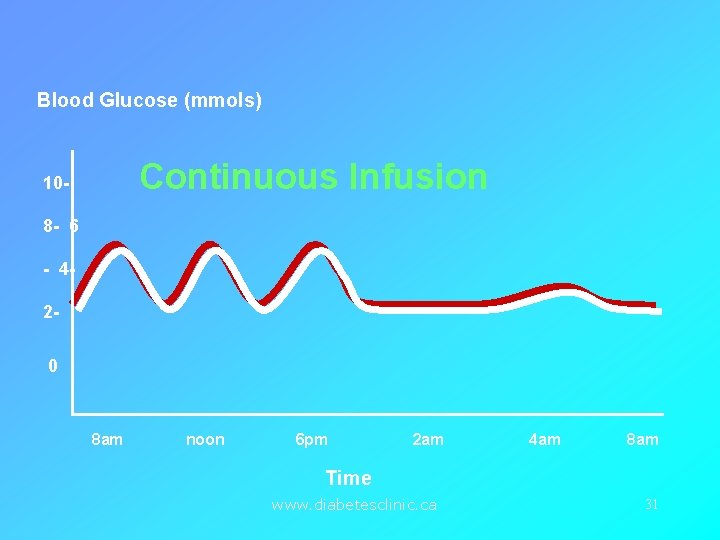
Blood Glucose (mmols) Continuous Infusion 108 - 6 - 420 8 am noon 6 pm 2 am 4 am 8 am Time www. diabetesclinic. ca 31

Limitations of Regular Human Insulin • Slow onset of activity – Should be given 30 to 45 minutes before meal • Inconvenient for patients • Long duration of activity – Lasts up to 12 hours • Potential for late postprandial hypoglycaemia (4 -6 hours) – Need for additional snack www. diabetesclinic. ca 32
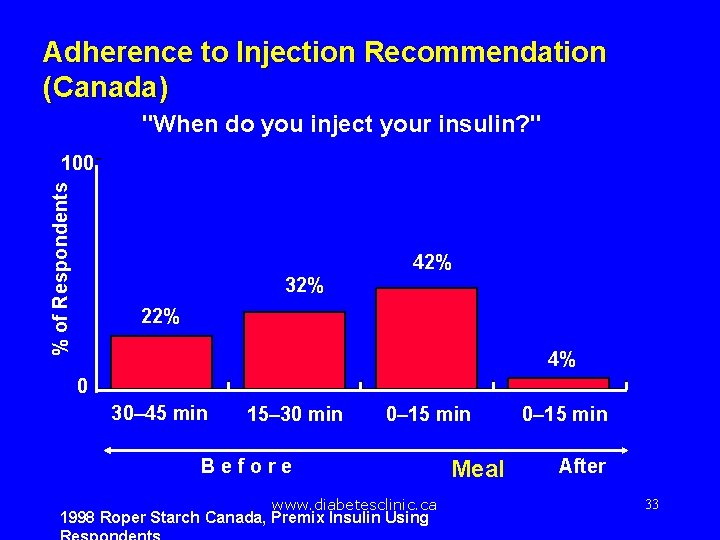
Adherence to Injection Recommendation (Canada) "When do you inject your insulin? " % of Respondents 100 42% 32% 22% 4% 0 30– 45 min 15– 30 min 0– 15 min Before www. diabetesclinic. ca 1998 Roper Starch Canada, Premix Insulin Using Meal 0– 15 min After 33
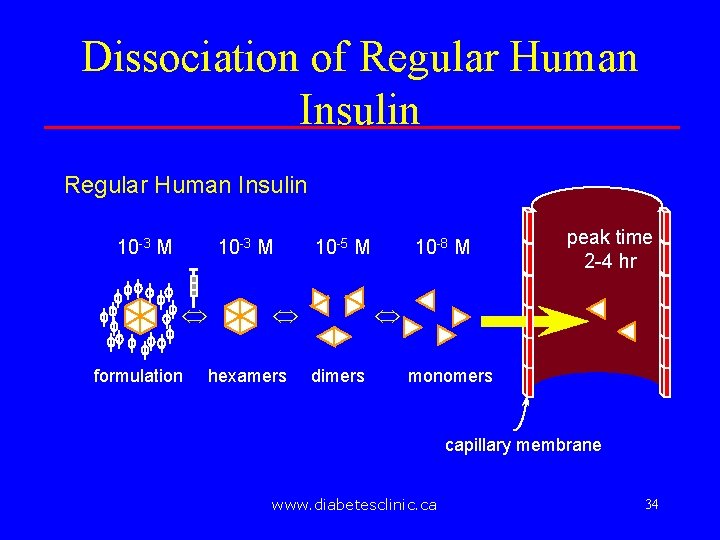
Dissociation of Regular Human Insulin 10 -3 M Û formulation 10 -5 M Û hexamers 10 -8 M peak time 2 -4 hr Û dimers monomers capillary membrane www. diabetesclinic. ca 34

Objectives for the Development of Short. Acting Insulin Analogues • Modify time action to address – Postprandial hyperglycemia – Hypoglycemia • Improve safety and convenience www. diabetesclinic. ca 35

Whats’ new in type 1 diabetes treatment? • Insulin analogues. • Physiological insulin replacement • Aggressive “intensive” management – – 4 injections per day Insulin infusion pumps Continuous glucose monitoring systems Integrated technologies for monitoring control www. diabetesclinic. ca 36
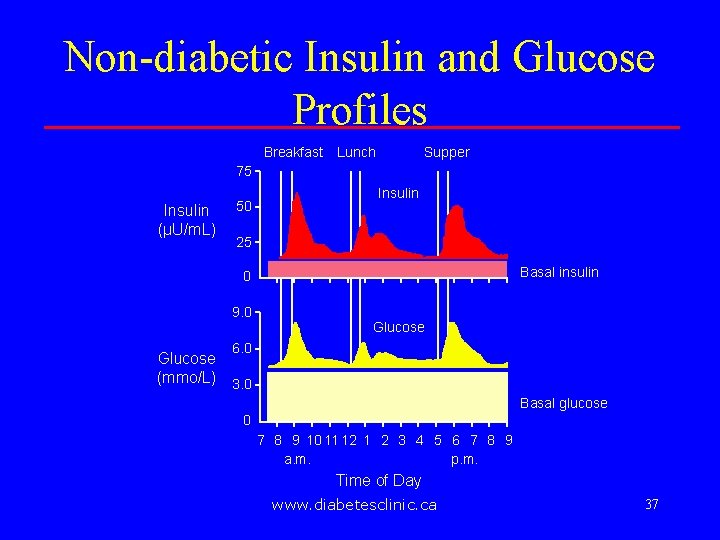
Non-diabetic Insulin and Glucose Profiles Breakfast Lunch Supper 75 Insulin (µU/m. L) 50 Insulin 25 Basal insulin 0 9. 0 Glucose 6. 0 Glucose (mmo/L) 3. 0 Basal glucose 0 7 8 9 10 11 12 1 2 3 4 5 6 7 8 9 a. m. p. m. Time of Day www. diabetesclinic. ca 37
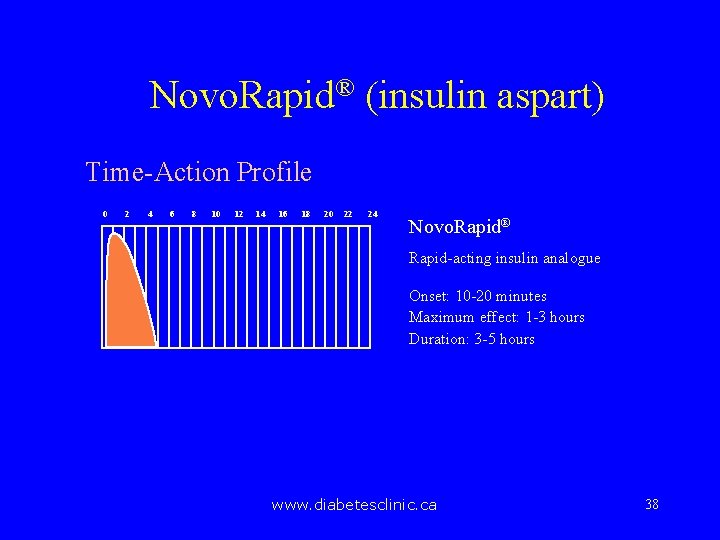
Novo. Rapid® (insulin aspart) Time-Action Profile 0 2 4 6 8 10 12 14 16 18 20 22 24 Novo. Rapid® Rapid-acting insulin analogue Onset: 10 -20 minutes Maximum effect: 1 -3 hours Duration: 3 -5 hours www. diabetesclinic. ca 38

Goal of Insulin Therapy We are trying to duplicate how the pancreas works in releasing insulin for someone who doesn’t have diabetes www. diabetesclinic. ca 39

Insulin Therapy Options • MDI therapy – 0. 5 units/kg = total daily dose – 4 x/day 40% NPH @ hs and 60% rapid acting analogue ac meals – For patients with significant complications (i. e. renal failure, foot infections, CVD, etc…) www. diabetesclinic. ca 40

Basal Insulin In someone without diabetes, the pancreas delivers a small amount of insulin continuously to cover the body’s non-food related insulin needs. www. diabetesclinic. ca 41

Bolus Insulin The amount of insulin required to cover the food you eat. Fast-acting or Short-acting (clear) insulin works as a Bolus Insulin www. diabetesclinic. ca 42

Why count carbs? • More precise way of measuring the impact of a meal on blood sugar • Lets you decide how much insulin is needed to “cover” the meal • Greater flexibility -eat what you want, when you want to eat it www. diabetesclinic. ca 43

Fine Tuning: Bolus Doses • Carbohydrate counting or pre-determined meal portion • Individualized insulin to carbohydrate dose or insulin to meal dose • Adjust bolus based on post-meal BGs or next pre-meal BG www. diabetesclinic. ca 44

Fine Tuning: Basal Rate • Monitor BG pre-meal, post-meal, bedtime, 12 am, and 2 -4 am • Test fasting BG with skipped meals • Adjust nighttime basal based on 2 -4 am and pre-breakfast BG • Adjust basal by 0. 1 u/hr to avoid over-correction www. diabetesclinic. ca 45
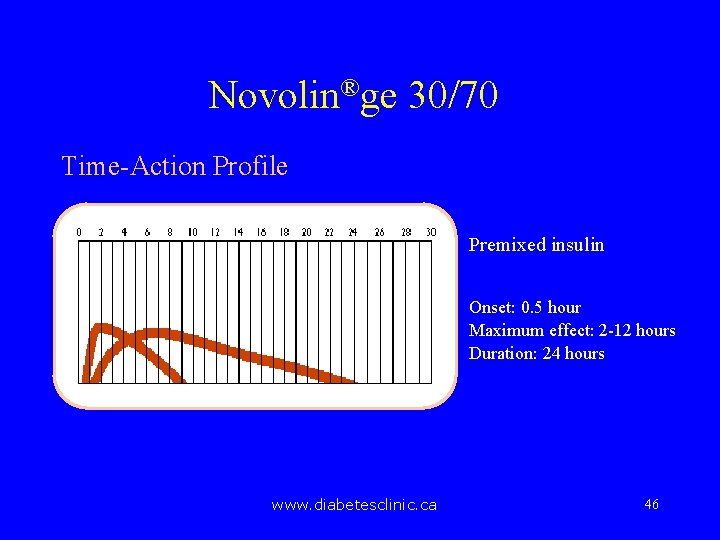
Novolin®ge 30/70 Time-Action Profile Premixed insulin Onset: 0. 5 hour Maximum effect: 2 -12 hours Duration: 24 hours www. diabetesclinic. ca 46
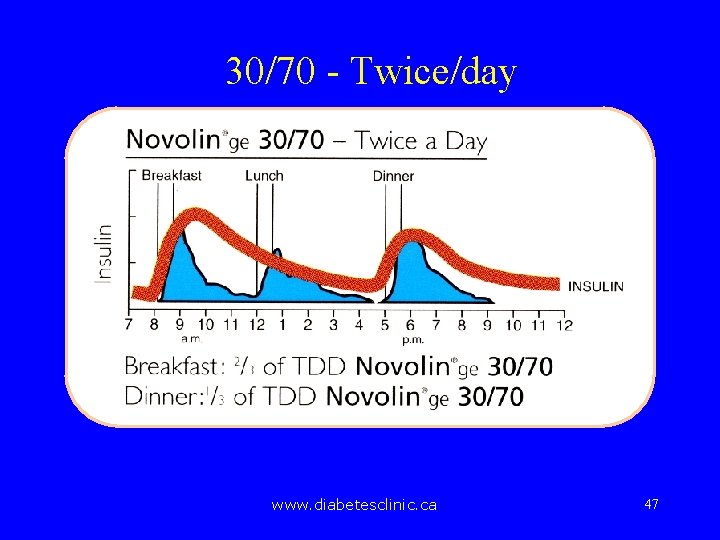
30/70 - Twice/day www. diabetesclinic. ca 47

30/70 Dose Calculation • • Weight = 80 kg x 0. 3 U/kg = 24 U 2/3 in the AM = 16 Units 1/3 at supper = 8 Units www. diabetesclinic. ca 48

Dosage Changes • Change insulin dose so that peak of action corresponds to most abnormal value (pre-meal) • If all values are abnormal - start with fasting glycemia followed by lunch, supper and bedtime • Change the dose by increments of 1 -4 U • Not more than twice/week • Monitor for PATTERNS in hypoglycemia www. diabetesclinic. ca 49
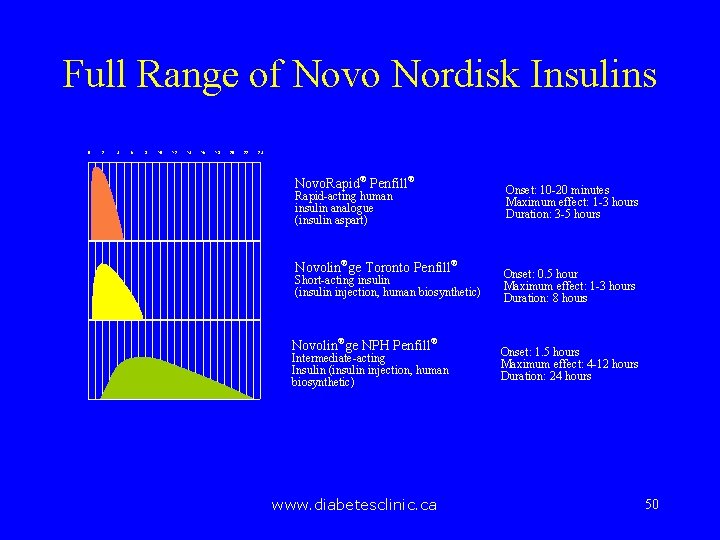
Full Range of Novo Nordisk Insulins 0 2 4 6 8 10 12 14 16 18 20 22 24 Novo. Rapid® Penfill® Rapid-acting human insulin analogue (insulin aspart) Novolin®ge Toronto Penfill® Short-acting insulin (insulin injection, human biosynthetic) Novolin®ge NPH Penfill® Intermediate-acting Insulin (insulin injection, human biosynthetic) www. diabetesclinic. ca Onset: 10 -20 minutes Maximum effect: 1 -3 hours Duration: 3 -5 hours Onset: 0. 5 hour Maximum effect: 1 -3 hours Duration: 8 hours Onset: 1. 5 hours Maximum effect: 4 -12 hours Duration: 24 hours 50

Somogyi Effect • Hyperglycemia secondary to asymptomatic hypoglycemia (especially at night) • If the insulin is increased in evening, the problem worsens • Check capillary glycemia around 3 a. m. to eliminate hypoglycemia • In this case, reduce the h. s. NPH www. diabetesclinic. ca 51

Follow-Up: The Patient’s Role Every Day Every 3 months • Check BG 4 -6 times a day, and always before bed • Follow hypoglycemia guidelines • Follow hyperglycemia guidelines • Visit healthcare provider even if feeling well • Review log book and pump settings with physician • Get an A 1 c test Every month F F Review DKA prevention Check BG - 3 am (overnight) 1 and/or 2 -hour post-meal BG for all meals on a given day www. diabetesclinic. ca 52

Case Study #1 • Patient R. M. , DM for 9 years • BMI = 34, • Meds: metformin 1000 mg BID and glyburide 10 mg BID, Avandia 8 mg OD • Hb. A 1 C is 9. 5 %, FBS 11. 8 What is the next step? www. diabetesclinic. ca 53

Case Study #2 • Patient K. G. , DM for 15 years • BMI = 23 • Meds: Metformin 1000 mg BID and Gluconorm 2 mg TID • Hb. A 1 C = 8. 5%, FBS 7. 4 • Post MI What is the next step? www. diabetesclinic. ca 54
- Slides: 54