Integration of Noncommunicable Diseases into PHC in lowresource

Integration of Noncommunicable Diseases into PHC in low-resource settings Lessons learned Dr Shanthi Mendis Chronic Disease Prevention and Management World Health Organization 1

PHC Reforms proposed (WHR 2008) l Universal coverage l Service delivery l Leadership reforms l Public policy reforms 2

WHO provides Technical support for National Health Development process (Driven by country needs) l Bhutan l Eritrea l Sri Lanka l Sudan l Syria 3

Lessons l Challenges l Opportunities l Capacity l Sustainability l Affordability l Balance l Evaluation 4
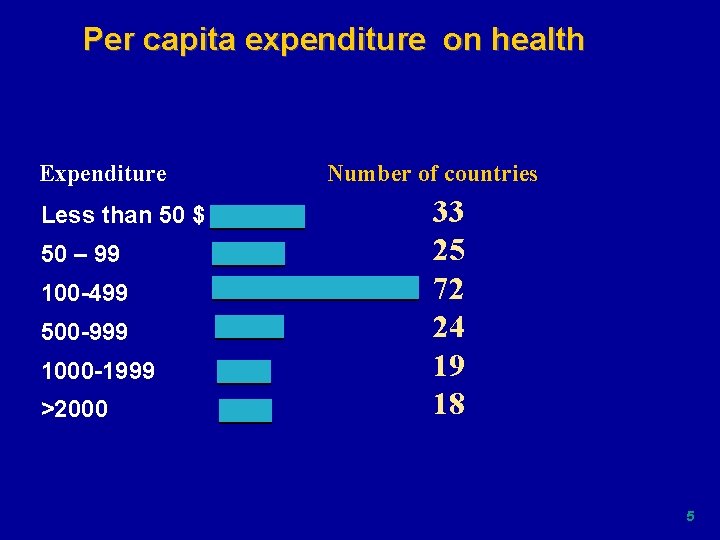
Per capita expenditure on health Expenditure Less than 50 $ 50 – 99 100 -499 500 -999 1000 -1999 >2000 Number of countries 33 25 72 24 19 18 5

Setting priorities l Contribution to morbidity and mortality (Cardiovascular diseases , diabetes, Cancer, CRD) l Availability of cost effective interventions l Feasibility of implementing in primary care 6
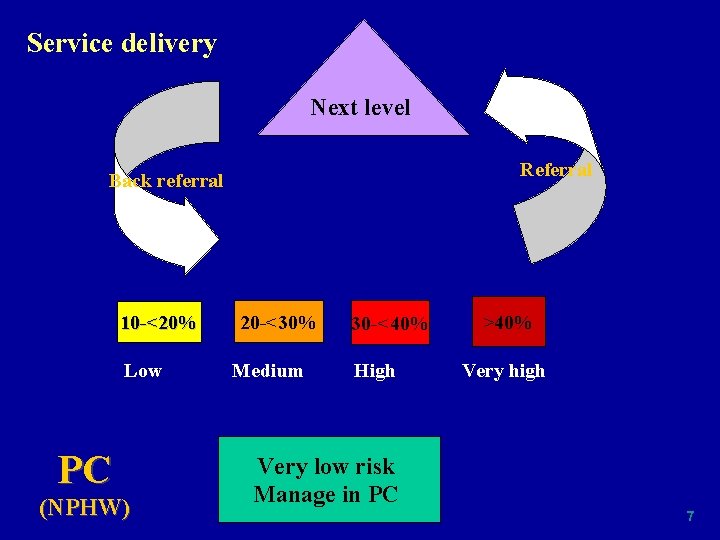
Service delivery Next level Referral Back referral 10 -<20% Low PC (NPHW) 20 -<30% Medium 30 -<40% High >40% Very high Very low risk Manage in PC 7
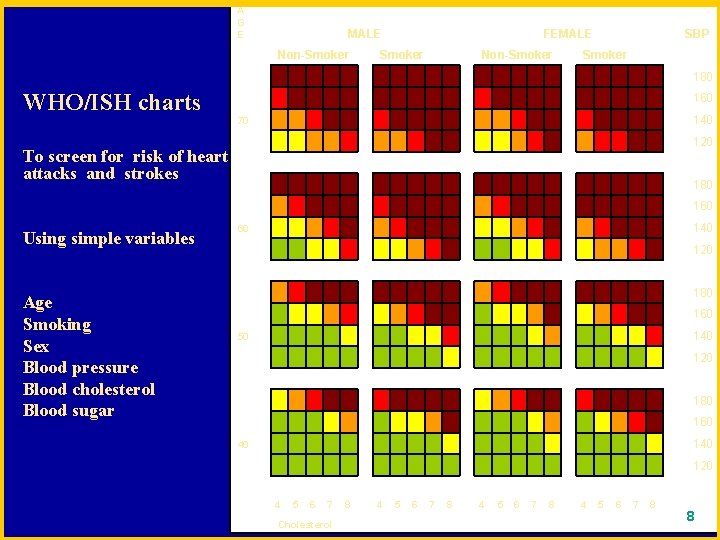
WHO/ISH charts To screen for risk of heart attacks and strokes Using simple variables Age Smoking Sex Blood pressure Blood cholesterol Blood sugar A G E Non-Smoker 70 60 MALE FEMALE SBP Non-Smoker 180 160 140 120 180 160 140 120 180 160 50 140 120 180 160 40 140 120 4 5 6 7 8 Cholesterol 8

9

PHC based Health System l Define functions of all levels of the health system based on PHC: skills, requirements, equipment, medicines, interactions between levels and sectors l Financing models for different social and economic contexts and health systems l Service delivery models that promote continuity of care across different NCDs, levels and sectors of care l Type of training, support and supervision needed for delivery of interventions by physician/ non-physician 10

Integration of NCD into PHC Per capita health expenditure in many LMIC countries is inadequate to provide universal coverage 2. Range of cost effective NCD interventions can be integrated into PHC, even in low resource settings. 3. If sustainable approaches are used they can reduce morbidity and premature mortality due to NCDs. 4. PHC has the potential to reduce suffering from preventable NCDs and reduce health-care costs. 1. 11

` 12
- Slides: 12