Integrating Structural Dissociation Theory with EMDR Therapy By

Integrating Structural Dissociation Theory with EMDR Therapy By Kathleen Martin, LCSW EMDRIA Consultant in EMDR kmartinlcsw@gmail. com www. kmccs. com

Have you treated dissociative clients? Most likely, Yes 3/3/2017 Probably more than you know! © Kathleen M. Martin 2017 2

What is Dissociation? § Even the experts don’t agree § No universal language or definition § Mistakenly judged as pathological 3/3/2017 © Kathleen M. Martin 2017 3

Overall Agreement: Dissociation is the inability to stay present with affect

Theories of Dissociation § Structural Theory (Nijenhuis, van der Hart, Steele) § Perceptual Theory (Beere) § Neodissociation Theory (Hilgard) § Ego State Theory (Federn and Watkins) § Bask Theory (Braun) § Psychobiological Theory (Krystal) § Extension of Normal Dreaming (Barrett) § Socio. Cognitive Theory (Spanos) § Behavioral States Model (Putnam) 3/3/2017 © Kathleen M. Martin 2017 5

Structural Dissociation Theory �Based on Pierre Janet’s work (1889 -1925) �Meyer (1930 -1945) added to it �Ellert Nijenhuis, Onno van der Hart and Kathy Steele expanded it since the late 1980’s 3/3/2017 © Kathleen M. Martin 2017 6

Action Systems �Human behavior is governed by evolutionally prepared, psychobiological systems �These action systems make up our personality and determine our mental and behavioral actions �Purpose of these action systems is to keep us alive and respond to our world and experience �As a psychobiological state, each action system has its own sensory, somatic, perceptual, and cognitive experience 3/3/2017 © Kathleen M. Martin 2017 7

2 Major Action Systems 1) Survival of the species: concerns mental and behavioral actions dealing with Daily Life 2) Survival of the individual: concerns Defensive actions in response to threat, injury to the body, social rejection, and attachment loss 3/3/2017 © Kathleen M. Martin 2017 8

Daily Life Action System: Survival of the Species �Exploration (work, study) �Play �Energy management: sleep, eating, preparing food, housecleaning, etc. �Attachment �Socializing �Reproduction �Care Taking (parenting, managing parents, etc) 3/3/2017 © Kathleen M. Martin 2017 9

Defensive Action System: Survival of the Individual �Fight �Flight �Freeze �Total submission (collapse) �Social submission �Attachment Cry �Recuperation (following the threat: rest, isolation, wound care, and gradual return to daily activities) 3/3/2017 © Kathleen M. Martin 2017 10

Defensive Action System handles all information from unhealed hurt Defensive Action System encodes and stores all pieces of events that are not completely processed and adaptively stored 3/3/2017 © Kathleen M. Martin 2017 11

Action Systems Before Trauma In the mentally healthy person without dissociation (before trauma is stored) these 2 action systems are open to each other: � They coordinate and cooperate with each other, doing their respective jobs �Together they metabolize and personify (integrate and synthesize) experiences as they happen and functionally store this information. 3/3/2017 © Kathleen M. Martin 2017 12

Mental Health Daily Living Defensive The Daily Living Action System and the Defensive Action System cooperate, communicate and work together. The person functions well. 3/3/2017 © Kathleen M. Martin 2017 13

Trauma Impairs this Coordination �A traumatic experience overwhelms the person’s integrative capacity �The person is flooded by the affect and somatosensory information and can not fully process, synthesize and integrate this information �The daily living action system must continue with daily activities while the defensive action system manages the unhealed affect and information �To attend to daily activities, the daily living action system must “tune out” the defensive action system �To manage the unhealed hurt, the defensive action system becomes stuck in “trauma time” and does not realize the present 3/3/2017 © Kathleen M. Martin 2017 14

Coordination of Action Systems Impaired by Trauma �This results in an alternation between Daily Living’s avoidance and Defensive’s reliving �There is an abnormal closure between the 2 action systems �System of daily life doesn’t stay fully present to assist in times of danger and doesn’t experience the full experience �System of defense is so busy reliving and managing the past that it can’t create a fresh response to the present: it sees the present through the lens of the past �Under severe or chronic stress this differentiation becomes wider 3/3/2017 © Kathleen M. Martin 2017 15

Trauma’s Impact on Avoidance and Reliving The specialization of the psychobiological “jobs” of the 2 action systems propel the alternation and co-existence of: 1) Trauma avoidance by the daily living action system that ends up experiencing “too little” (numbing, detachment, conscious and unconscious avoidance strategies) 2) Trauma fixation by the defensive action system that ends up experiencing “too much” (reliving the trauma and fixation in defense) 3/3/2017 © Kathleen M. Martin 2017 16

When Trauma Happens The 2 action systems must manage the traumatic material in their own ways, thus reducing their ability to communicate and cooperatively respond to life. A structural divide between them is created. Daily Living 3/3/2017 © Kathleen M. Martin 2017 Defensive 17

When Trauma Happens Apparently Normal Part of the Personality 3/3/2017 Emotional Part of the Personality This differentiation is the start of Dissociation. Both parts contribute to the dissociation. The Daily Living Action System’s part of the personality is now called the Apparently Normal Part and the Defensive System’s part of the personality is now called the Emotional Part. © Kathleen M. Martin 2017 18

Definition of Dissociation in Structural Dissociation Terms The structural division of the personality that occurs between these 2 action systems. There can’t be dissociation with only 1 action system. Dissociation is across the full personality. 3/3/2017 © Kathleen M. Martin 2017 19

Apparently Normal Part To keep the appearance of normality while doing daily activities it must: ü avoid the trauma üuse numbing skills (analgesia, anesthesia, amnesia, shutdown, etc) üBut it is still plagued by intrusions from the defensive system Emotional Part üEncodes and stores the trauma üRelives the trauma in emotional and sensorimotor ways üLives in “Trauma Time” and is incorrectly time oriented Therefore both parts contribute to the structural dissociation within the personality. 3/3/2017 © Kathleen M. Martin 2017 20

Why the Daily Living Action System’s part of the personality is called the The Apparently Normal Part (ANP) To pay attention to daily activities, this dissociated part of the personality must: 1) Avoid the physical and mental trauma-related cues and info held by the defensive action system 2) Become detached from the full experience 3) Appear undisturbed and able to lead a normal life 4) Can’t contribute to the integration of the event while also engaging in avoidant behavior 3/3/2017 © Kathleen M. Martin 2017 21

Why the Defensive System’s part of the Personality is called the Emotional Part The defensive action system stores, manages and relives the traumatic material An Emotional Part is like a software package that, when activated, can only relive the information that is in its program, including the vehement emotions and sensorimotor activation 2) This dissociated part views present experiences through the lens and experience of the maladaptively stored affect and information in its “software program” 1) 3/3/2017 © Kathleen M. Martin 2017 22

Why the Defensive System’s part of the Personality is called the Emotional Part 3) It is fixated in the traumatic material 4) Relives the emotional and behavioral responses used (and not used) during the traumatic event 5) Holds and relives the catastrophic beliefs and negative thoughts about self in response to the trauma; e. g. , “ It’s my fault”; “I’m not safe”; “I’m bad” 6) May be stuck in defensive actions such as fight, flight, freeze, collapse, submit, attachment cry 7) Can’t contribute to the integration of the traumatic material while stuck in “trauma time” 3/3/2017 © Kathleen M. Martin 2017 23

Differentiated Somatic & Psychobiological Experiences of the EP and ANP �Different neuroendocrine profiles �Different areas of the brain activated �ANPs avoid threat cues (internal & external) and reminders of the unhealed stored trauma �EPs selectively attend to threat cues the ANPs avoid �Numerous controlled studies support this 3/3/2017 © Kathleen M. Martin 2017 24

Growth of ANP and EP Subsystems �As more trauma occurs, more EPs are needed to store and manage the non-integrated traumatic material. �Over time these EPs can develop at least a rudimentary sense of self and, in the case of DID, develop a highly defined sense of self �Examples are: Fight, Protector, Little Girl, Teenager, Critic, Rescuer, etc. �The Daily Living Action System can also develop subsystems such as mother, student, wife, therapist, etc. 3/3/2017 © Kathleen M. Martin 2017 25

Growth of ANP and EP Subsystems �Therefore, the personality has 2 action systems who can develop any number of subsystems. �The proliferation of these subsystems is completely dependent on the chronicity and amount of nonintegrated trauma that occurs to the person. �With (early) chronicity, the more subsystems. 3/3/2017 © Kathleen M. Martin 2017 26

Levels of Structural Dissociation of the Personality �PRIMARY � Simple PTSD � Simple Dissociative Disorders (DSM-IV, ICD-10) �SECONDARY � Chronic, complex PTSD/DESNOS � BPD, DDNOS �TERTIARY � DID Van der Hart, Nijenhuis & Steele, 2000 3/3/2017 © Kathleen M. Martin 2017 27

When Integration Fails: Primary Dissociation Apparently Normal Part Emotional Part • Simple PTSD, Acute Stress Disorder • One EP holds the trauma and carries out the defensive functions • There is less communication and cooperation between the action systems than what is found in mental health (prior to the trauma) 3/3/2017 © Kathleen M. Martin 2017 28

Primary Dissociation �Alternation between single part of the personality mediated by daily life action system (ANP) and a second (rather limited and rudimentary) emotional part (EP) mediated by defense �EMDR Standard Protocol Phase 4 trauma reprocessing in primary dissociation typically goes quickly without the need of advanced strategies to treat dissociation 3/3/2017 © Kathleen M. Martin 2017 29

Secondary Dissociation Apparently Normal Part EP: fight EP: flight EP: submit EP: freeze Complex PTSD, OSDS (aka DDNOS), BPD More defensive subsystems are needed to manage the trauma 3/3/2017 © Kathleen M. Martin 2017 30

Secondary Dissociation �In Secondary Dissociation, there is one ANP with any number of EPs holding the traumatic material. �The ANP maintains executive functioning. �The EPs can be organized (fixated) around a particular memory or defensive response. Examples include: Ø Ø 3/3/2017 Attachment cry (sad, bereft part often experienced as a “child”) Fight (angry teenage part ready to fight all the time) 7 year old part caught in trauma time and reliving the event Critic part who must make all parts of self perfect to protect from being hurt © Kathleen M. Martin 2017 31

Tertiary Dissociation: DID 2 or more ANPs & numerous EP: submit EP: fight ANP 1 EP: flight ANP 2 EP: 5 yr old EP: child attachment cry 3/3/2017 © Kathleen M. Martin 2017 EP: Freeze 32

Tertiary Dissociation �More than 1 ANP, with each ANP having EPs �Integrative capacity of the individual is too low to develop or maintain a single ANP �ANP (s) looses time. The integrative capacity is too low for the ANP to stay present when a particular EP(s) is activated. �EPs can get executive functioning and “be in the driver’s seat” 3/3/2017 © Kathleen M. Martin 2017 33

The Essence of Dissociation: Non-Realization �Dissociation makes overwhelming conditions less overwhelming to the ANP and the full system �Not claiming the full experience happened “to me” makes it feel less impactful � The continuum of non-realization can range from a small piece of the event to the entire event �The non-realized pieces of the event are held by the Defensive System �Emotional Parts also participate in the nonrealization; for example, it happened to the 7 year old but not the Baby or the teenager. 3/3/2017 © Kathleen M. Martin 2017 34

Examples of Non-Realization �Narrowing of Attention: exclusion of stimuli “I didn’t notice that stop sign” “I have never noticed that picture before. ” (even though it has been in your office for years) �Minimizing: the facts are acknowledged but the impact is not acknowledged “It’s no big deal. ” “It didn’t bother me. ” �Denial: “I am not an alcoholic” �Dissociation: Division of the personality: “It happened to that girl, not me. ” “I have no memory but I keep having these sensations and images. ” 3/3/2017 © Kathleen M. Martin 2017 35

Examples of Non-Realization 1) ANP believes “the car accident where I almost died did not have an impact on me. I’m fine. It is over. It is healthy to not drive anymore because there are crazy drivers out there and it is not safe. ” 2) EP, age 14, believes that the trauma at age 7 “did not happen to me because I am too old. I was created long after that. ” 3) EP, age 5, believes she is not angry about anything and hates the 12 year old EP for being angry. 3/3/2017 © Kathleen M. Martin 2017 36

Examples of Non-Realization 1) ANP reports crying every time after sex with her husband. Even though she reported some intrusive images of childhood sexual abuse, she thinks she is just making that up and blames hormones for the crying. 2) Client’s husband died 10 years ago. Client has not grieved and says she has been too busy as a single parent to pay attention to it. She knows she is not emotionally available to her new lover and thinks she needs to finally do her grieving. Dissociative table found a 5 year old EP who did not know her husband had died. 3/3/2017 © Kathleen M. Martin 2017 37

To Recap: 1) Dissociation is the inability of the 2 action systems to stay present with each other and adaptively manage life together during or after an overwhelming event 2) Dissociation implies some degree of non-realization: “it wasn’t that bad”; “It didn’t happen to me” 3) Another way of saying this is the non-realized, maladaptively stored information is outside the person’s window of tolerance 3/3/2017 © Kathleen M. Martin 2017 38
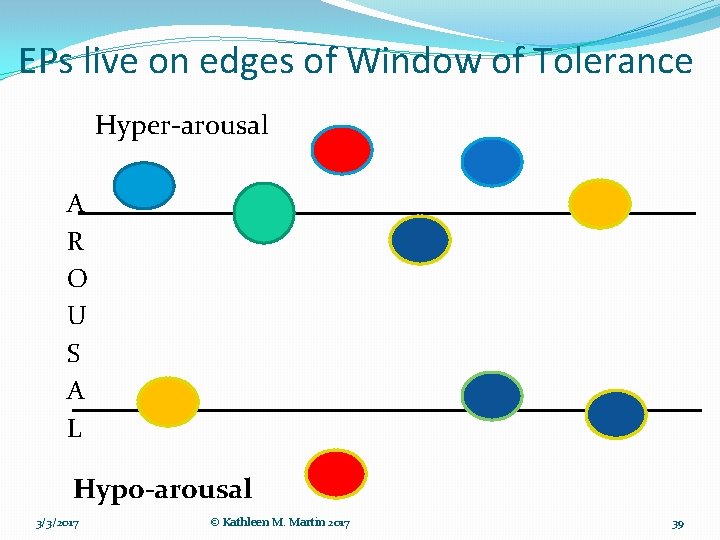
EPs live on edges of Window of Tolerance Hyper-arousal A R O U S A L Hypo-arousal 3/3/2017 © Kathleen M. Martin 2017 39

Window of Tolerance �When the maladaptively stored information/EP is inside the window of tolerance it is easily processed. �When the maladaptively stored information/EP is on the edges or outside the window of tolerance, special care must to taken so the ANP’s phobia to that information is not increased. �No integration can occur when the EP is outside the window of tolerance. �Reliving is outside the window of tolerance. Reliving implies re-dissociation/re-traumatization. 3/3/2017 © Kathleen M. Martin 2017 40

Dissociative Phobias �Hallmark of PTSD �Hallmark of Dissociation 3/3/2017 © Kathleen M. Martin 2017 41

ANP’s Selective Focus of Attention & the Growth of Dissociation ANP’s high need to avoid the trauma or reminders of the trauma: 1)Decreases the ANP’s integrative capacity to heal the trauma 2) The retraction of the field of consciousness increases with each intrusion from the unwanted maladaptively stored material held by the EP 3) Classical conditioning continues to increase the ANP’s avoidance of the Emotional Part(s) 4) This avoidance (phobia) may at times be involuntary, extreme and rigid 3/3/2017 © Kathleen M. Martin 2017 42

Reason why Dissociation Grows long after the trauma is over The ANP avoids the trauma while the EP does not realize the trauma is over. Neither part can facilitate the integration of the traumatic material. With each intrusion by the EP, the ANP must increase its avoidance behaviors, thus widening the divide between the 2 action systems. This avoidance/reenactment duality occurs simultaneously and keeps growing and intensifying. The dissociation grows over time, long after the trauma is over. The post-traumatic decline gets worse and worse. 3/3/2017 © Kathleen M. Martin 2017 43

Key Piece of Theory that informs the treatment process: The ANP’s phobia to EPs and the traumatic material they hold maintains the structural dissociation of the ANP and EPs. 3/3/2017 © Kathleen M. Martin 2017 44

Phobia grows via Classical Conditioning What fires together wires together and then: What wires together fires together 3/3/2017 © Kathleen M. Martin 2017 45

EP and Classical Conditioning �Previously neutral (internal or external) stimuli can be associated with the trauma �This expands the memory representations of the trauma and its possible triggers �EP is activated when these representations are triggered 3/3/2017 © Kathleen M. Martin 2017 46

EP and Classical Conditioning �Once activated, there is a predictable course of thinking, feeling, response and behavior �EPs do what they were programmed to do 3/3/2017 © Kathleen M. Martin 2017 47

ANP and Classical Conditioning �Exposure to the traumatic material is aversive to the ANP �Therefore ANP avoids it rather than integrates it �Each time the ANP avoids, the phobia grows �The phobia fuels a range of the ANP’s avoidance and escape reactions preventing integration of the trauma 3/3/2017 © Kathleen M. Martin 2017 48

The ANP’s phobia maintains the structural dissociation of the ANP and EPs 3/3/2017 © Kathleen M. Martin 2017 49

As ANP becomes more phobic, Dissociation Strengthens �As the ANP is intruded upon by the EP (& perhaps unaware of the stimuli that activated the EP) the ANP will associate more stimuli and information as aversive �Thus widening the ANP’s range of inner and outer events to be avoided �The ANP chronically adapts, narrows functioning, becoming less able to maintain “apparent normality” 3/3/2017 © Kathleen M. Martin 2017 50

Common Behavioral Examples of Dissociative Phobias �Client cancelling a session or coming late after or before the first trauma processing session �ANP refusal to communicate with an EP. This can grow into complete lack of coconsciousness. �Committing to work on a specific memory or issue but changing the subject repeatedly when redirected by therapist �ANP is insistent that “all is well” and “nothing phases me” �ANP refusal to admit there are emotional parts despite the clear existence of EPs 3/3/2017 © Kathleen M. Martin 2017 51

Example: Car Accident Car accident happens on a snowy day. The EP stores the trauma and relives it while at the same time the ANP must avoid cues of the trauma to do daily life tasks. EP is activated a few weeks later when it is icy and associates icy conditions into the memory network. ANP must avoid that activation and now doesn’t like driving in snow and ice. EP becomes activated on a sunny day and associates driving in sunny conditions into the memory network. ANP doesn’t like the activation when driving on a sunny day and develops avoidance of sunny-day driving. Taking this to the extreme, agoraphobia develops due to the ANP’s need to avoid. 3/3/2017 © Kathleen M. Martin 2017 52

Case Example: Jennifer Referred for treatment by a clinician who was not trained in trauma and dissociation but had worked with this client for 1 ½ years. Client destabilized early in that treatment due to going into the memories too early and not diagnosing and treating the dissociative disorder (DID). Client’s Catatonic EP became activated most of the time outside of sessions and client became non-functional. Treatment with the new clinician focused on stabilization, getting the ANP to stay present, time orientation and deactivating Catatonic. Once the phobias to the mental contents were treated, including phobias to other EPs, reprocessing the traumatic memories in a controlled, titrated way went well and she never became Catatonic again. 3/3/2017 © Kathleen M. Martin 2017 53

Spiral of ANP’s Post Traumatic Decline �ANP has less and less ability to de-activate EPs �Without the ability to de-activate EPs, the ANP can not facilitate stabilization �ANP’s “apparently normal” functioning continues to decrease �Who is in charge? 3/3/2017 © Kathleen M. Martin 2017 54

This phobia fuels a range of the ANP’s avoidance and escape reactions preventing integration of the trauma. The clinical application of this phenomenon is that as long as the ANP is phobic, there is no readiness for Phase 4 processing in the EMDR Standard Protocol. 3/3/2017 © Kathleen M. Martin 2017 55

More on the Growth of Phobia �EPs can become phobic to each other �As more trauma happens, EPs can be developed to help maintain ANP avoidance. These are called Protector Parts and function to place another barrier between the ANP and the traumatic material. 3/3/2017 © Kathleen M. Martin 2017 56

Phase-Oriented Approach to Treating Dissociation Phase 1: Engagement, Stabilization -Increase ANP’s functioning level by gradually overcoming phobias of: attachment to therapist, mental contents, EP’s, other ANP’s. Phase 2: Reprocessing Traumatic Memories Controlled and titrated processing of traumatic memories to facilitate integration without re-dissociation. Phase 3: Enhancing Daily Living - Integration of the personality, overcoming phobia of intimate attachment, and coping with life in non-dissociative/non-avoidant ways. 3/3/2017 © Kathleen M. Martin 2017 57

Phase 1 of Treating Dissociation Start with increasing ANP’s level of functioning and ability to calm EP arousal and stabilize the system This requires the ANP must: 1) Have enough positive affect tolerance for calm and skill to return self to calm (instead of shutdown) 2) Be able to stay present and communicate with EPs 3) Have compassion (instead of disgust and avoidance) toward the EPs 4) Be a leader for the full system in stabilization and the work of treatment 5) ANP has the adaptive information that PTSD means parts are stuck in trauma time and can offer time orientation skills for self 3/3/2017 © Kathleen M. Martin 2017 58

Treating ANP’s Phobia is the first order of business Always start with assessing for positive affect tolerance �The ANP must have an adequate window of tolerance for calm �Most people with complex trauma do not have enough positive affect tolerance � If the ANP can not tolerate calm then the ANP can not assist EPs to achieve calm/stabilization �Building ANP’s tolerance for calm puts the ANP back in the driver’s seat within the system �Calm must be tolerated for effective trauma reprocessing 3/3/2017 © Kathleen M. Martin 2017 59

Why is Calm so Important? Without positive affect tolerance there are only 3 options: 1) Shutdown 2) Addiction 3) Staying in the negative thoughts and behaviors (EP arousal into the maladaptively stored information) 3/3/2017 © Kathleen M. Martin 2017 60

Why Calm? �Clinically calm is the only positive affect we need to pay attention to �Of all the positive affects, calm is the one we spend the most time in �Tolerating calm will build the tolerance levels for the other positive affects of love, joy, and pride. �Tolerating calm will also build tolerance for the negative affects because the person knows he/she can come back to calm when the negative is too much 3/3/2017 © Kathleen M. Martin 2017 61

Doesn’t Everybody have Tolerance for Positive Affect? �Everybody wants to feel good but feeling good requires an emotional muscle to access and remain in that positive state �We learn our affect regulation skills from our parents �Therefore we develop a similar window of tolerance as our parents when we are young �If our parents can’t tolerate positive affect, they can’t tolerate our positive affect. Nor can they take us back to calm when we need soothing because they don’t have the skill or tolerance. So we don’t develop a strong window of tolerance for calm because the family environment can’t develop it or support it �Without the ability to calm, we only have the choices of shutdown, addiction or staying in the negative 3/3/2017 © Kathleen M. Martin 2017 62

Don’t Handicap the Treatment �Don’t pass over positive affect tolerance development �Doing so handicaps the treatment �The client misses out on developing skills to get self out of disturbance and back to calm �Without calm tolerance, the client will increase shutdown skills and perhaps addiction skills as the traumatic material is accessed �The client is not ready for Phase 4 processing if calm isn’t tolerated �Treating a client without the ability to calm is like trying to put out a fire with oxygen 3/3/2017 © Kathleen M. Martin 2017 63

Building Positive Affect Tolerance �Calm Place exercise �Spiral �Other calming skills in your bag of tricks �Your client needs MANY calming skills: don’t underestimate this. When one skill doesn’t work, they can reach for another, then another, until one works �Brief exposures to the positive (remember that when the person gets outside their window of tolerance for the positive in your office, they will either shutdown, use an addiction (imaginal or behavioral) or go into the negative) 3/3/2017 © Kathleen M. Martin 2017 64

Are Distraction Skills Calming Skills? �Maybe, Maybe not! �Distraction skills are useful and might be calming but not all distraction skills bring the client to calm �Some distraction skills are actually shutdown skills or addiction skills �Help your client know the difference 3/3/2017 © Kathleen M. Martin 2017 65

Teach the difference between Calm and Shutdown �Many people with complex trauma experience shutdown as calm �To teach the difference, get the person in a calm state and ask her/him to describe the state, using as many adjectives as possible (use calm place imagery, a recent memory of calm, etc) �Then get the person in a shutdown state and ask for as many descriptions as possible (catch them in a shutdown state in your office or use a recent memory of shutdown) �Compare them to see the differences 3/3/2017 © Kathleen M. Martin 2017 66

Have an Arsenal of Stabilization Skills to Teach the ANP �Positive Affect Tolerance �Affect Regulation Skills �DBT Skills �Distraction Skills to shift back into the present �Silly Little Questions �Pendulation �Time Orientation Skills �Adaptive Self-Care Skills including personal hygiene, exercise, eating, sleeping, energy management, routines �Good Boundaries 3/3/2017 © Kathleen M. Martin 2017 67

Arsenal of Stabilization Skills �Skills to Observe Somatic Sensations �Grounding in the Present �Hypnotic and Relaxation Skills �Mindfulness Skills �Releasing Skills (Sedona Method by Hale Dwoskin) �Resource Development and Installation �Spiritual Resources �Good Coping Mechanisms �Daily Relaxation �Friends �Satisfying Activities �Add your own to this list 3/3/2017 © Kathleen M. Martin 2017 68

Note about Systematic Relaxation and Breathing Skills: Systematic Relaxation and Breathing Skills typically do not work for this population early in treatment. Skills that call attention to the body may trigger the client rather than stabilize. Know your client. It doesn’t matter what skills work; it only matters that your client has many skills she/he likes and use to achieve stabilization. Teach your client many skills so when one skill doesn’t work, there are many skills left in the toolkit to try. 3/3/2017 © Kathleen M. Martin 2017 69

Note about mindfulness: So many people with complex trauma and affect dysregulation problems can not use mindfulness skills successfully early in treatment. They experience mindfulness as just another way to be in the negative material. They do not have enough skill to be an observer of their disturbance. Nor do they have enough skill to get themselves out of their disturbance early in treatment. So, be careful about introducing mindfulness to your complex clients early in treatment. 3/3/2017 © Kathleen M. Martin 2017 70

When Treating Dissociative Phobias, don’t use exposure to Break Down the Phobia �Doing so just grows the phobia �Exposure therapies don’t work with complex trauma until the phobia is treated �Exposing to something that isn’t tolerated is taking the person outside the window of tolerance �Do not go into the stories too soon 3/3/2017 © Kathleen M. Martin 2017 71

Topics to cover in the Treatment of Dissociation in the Stabilization Phase �Assess for dissociation (DES, MID, etc) �Strengthen the ANP �Increase ANP positive affect tolerance and the ability to bring the system to calm: this increases ANP leadership �Dissociative Table: provides a forum to access, identify and work with the system �Time Orientation �Cognitive Errors 3/3/2017 © Kathleen M. Martin 2017 72

More Topics to attend to in the Stabilization Phase as you Treat Dissociation �Increase ANP compassion, communication, cooperation, coconsciousness, ability to stay present with parts, provide stabilization and time orientation �Treat the protector parts (this also includes persecutory parts, perpetrator imitator parts, perpetrator introjects) and their contributions to nonrealization and non-personification �Do not use exposure to what is intolerable as you work on the above issues. This will only grow the phobia 3/3/2017 © Kathleen M. Martin 2017 73

How much Stabilization? The length of time spent in the stabilization phase will depend on 1) the degree of ANP (and EP) phobia 2) If the ANP can calm, soothe and time orient the EPs. 3) The strength of cognitive errors and how long it takes to systematically break them down 4) Protector parts’ process of personification and realization that the traumas happened to them too. 5) Enough time orientation to allow reprocessing as opposed to reliving If the ANP and EPs can tolerate the affect and traumatic material, are correctly time oriented and stay present with each other while the traumatic material is activated, then it is time to begin Phase 4 Desensitization (trauma reprocessing). DDNOS and DID clients will require frequent returns to the stabilization phase especially early in the reprocessing phase. 3/3/2017 © Kathleen M. Martin 2017 74

Preparing for Phase 4 Trauma Reprocessing Use normal readiness checklist and the expanded checklist for complex trauma: 1) Assessment of the ANP’s ability to stay present while EPs are activated 2) Enough EP time orientation 3) EPs are in agreement that the target can be worked on & appropriate stabilization needs have been attended to 4) There is enough co-consciousness, compassion and cooperation among the parts so the work can proceed 5) Protector Parts and Persecutory Parts have been treated enough so they can tolerate access to the traumatic material. This also means that they have developed 3/3/2017 © Kathleen M. Martin 2017 75 some personification.

The Expanded Readiness Checklist for Complex Trauma Cases Please refer to the attached training handout which includes: Page 1: The Checklist for Readiness Reprocessing as found in Shapiro’s 1995 textbook Page 2: The Expanded Readiness Checklist for Complex Trauma Page 3: How Processing Complex Trauma is different than processing simple PTSD cases 3/3/2017 © Kathleen M. Martin 2017 76

Phase 4 Trauma Reprocessing Typical Reprocessing with complex trauma & dissociation is: 1) Titrated 2) Frequently stops due to hyper/hypo arousal of an EP. When this happens, assess which EP(s) need stabilization and provide it. 3) This return to the stabilization phase may last weeks or months depending on the clinical needs of your client. 3) As more reprocessing happens over time, the window of tolerance grows and bigger chunks of material can be reprocessed and integrated more quickly. 3/3/2017 © Kathleen M. Martin 2017 77

Summary �Dissociation is the structural division between the 2 action systems of daily living and defense �Mental health (pre-trauma) is when these 2 action systems work together as a team, cooperatively and easily to respond to life events �Trauma overwhelms this cooperation and these action systems become less able to cooperate and communicate with each other �Trauma creates a differentiation and division between the 2 action systems 3/3/2017 © Kathleen M. Martin 2017 78

Summary Continued �Once trauma is stored, each action system becomes locked into their respective “jobs” �The Daily Living Action System’s dissociated part is called the ANP (Apparently Normal Part) �The ANP must avoid the trauma and trauma related cues to attend to functions of daily life �The Defensive Action System’s dissociated part is called the EP (Emotional Part) �The EP is fixated in the trauma, manages and stores the maladaptively stored information, relives and reexperiences the vehement emotions & traumatic material 3/3/2017 © Kathleen M. Martin 2017 79

Summary Continued �With each intrusion from the defensive system, the ANP must grow its need and behaviors to avoid �This alternation between the ANP’s avoidance and the EP activation in trauma time maintains the inability of the entire person to heal �As the phobia grows so does the post traumatic decline �As more trauma happens, more EPs are needed to store and manage those events �Exposure therapies are not effective in cases of secondary(DDNOS) and tertiary dissociation (DID) 80 3/3/2017 © Kathleen M. Martin 2017

Summary Continued �In cases of dissociation, time spent in the Stabilization Phase can be quite lengthy �When the trauma reprocessing phase begins, expect the need to return to stabilization often to bring all parts back into the window of tolerance �Time orientation will be necessary throughout treatment until enough reprocessing is accomplished to maintain correct EP time orientation consistently 3/3/2017 © Kathleen M. Martin 2017 81
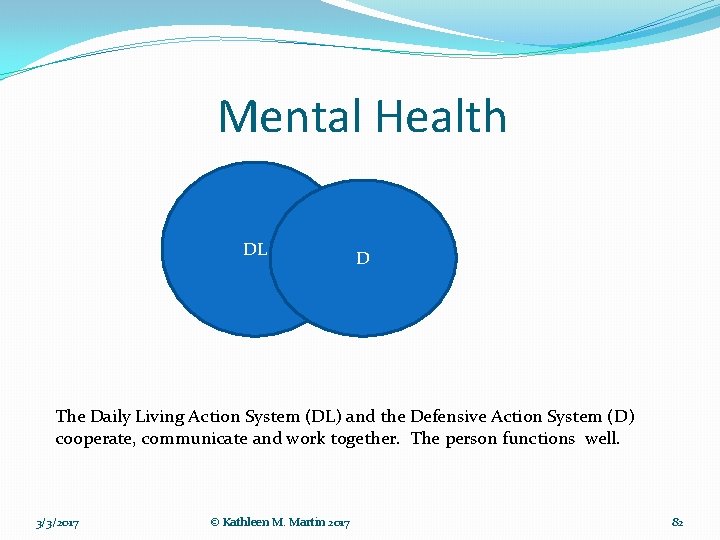
Mental Health DL D The Daily Living Action System (DL) and the Defensive Action System (D) cooperate, communicate and work together. The person functions well. 3/3/2017 © Kathleen M. Martin 2017 82

When Trauma Happens The 2 action systems must manage the traumatic material in their own ways, thus creating the structural divide between them ANP 3/3/2017 The Daily Living Action System Part is now called the ANP © Kathleen M. Martin 2017 EP The Defensive Action System Part s now called the EP 83
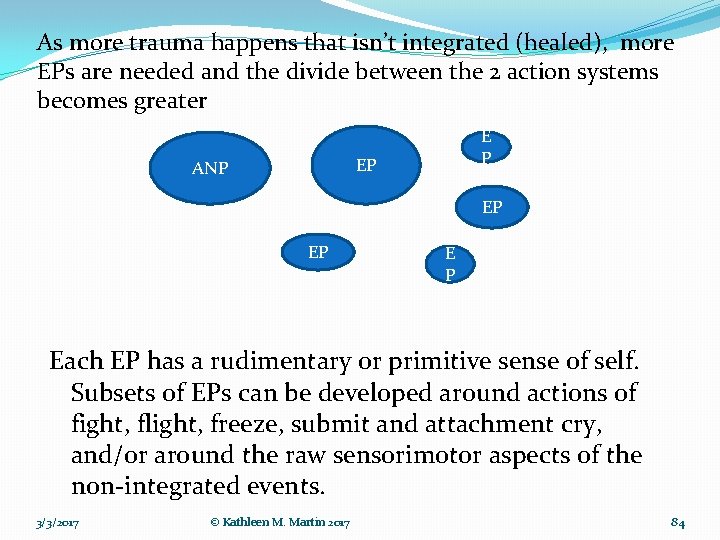
As more trauma happens that isn’t integrated (healed), more EPs are needed and the divide between the 2 action systems becomes greater E P EP ANP EP EP E P Each EP has a rudimentary or primitive sense of self. Subsets of EPs can be developed around actions of fight, flight, freeze, submit and attachment cry, and/or around the raw sensorimotor aspects of the non-integrated events. 3/3/2017 © Kathleen M. Martin 2017 84
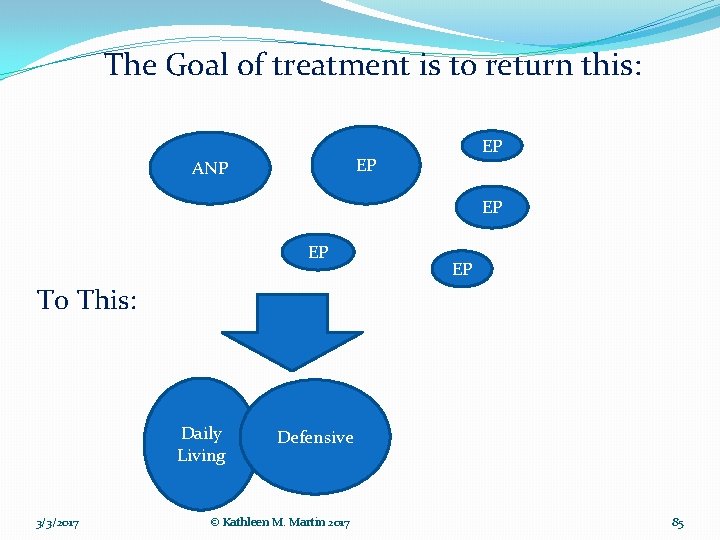
The Goal of treatment is to return this: EP EP ANP EP EP EP To This: Daily Living 3/3/2017 Defensive © Kathleen M. Martin 2017 85

References Frewen, P. , & Lanius, R. (2015). Healing the Traumatized Self. New York: Norton and Company. Gonzalez, A. & Mosquera, D. (2012). EMDR and Dissociation: The Progressive Approach. Kentucky. Gonzalez, A. & Mosquera, D. (2014). Borderline Personality Disorder and EMDR Therapy. Kentucky. Knipe, J. (2015). EMDR Toolbox Theory and Treatment of Complex PTSD and Dissociation. New York: Springer Publishing Company. Lanius, U. , Paulsen, S. , & Corrigan, F. (2014). Neurobiology and Treatment of Traumatic Dissociation Toward an Embodied Self. New York: Springer Publishing Company. Martin, K. (2012). How to Use Fraser’s Dissociative Table Technique to Access and Work with Emotional Parts of the Personality. Journal of EMDR Practice and Research, 6(4), 179186. Porges, S. (2011). The Polyvagal Theory. New York: Norton and Company. 3/3/2017 © Kathleen M. Martin 2017 86

References Van der Hart, O. , Groenendijk, M. , Gonzalez, A. , Mosquera, D. , & Solomon, R. (2013). Dissociation of the Personality and EMDR Therapy in Complex Trauma-Related Disorders: Applications in the Stabilization Phase. Journal of EMDR Practice and Research. 7(2), 8194. Van der Hart, O. , Groenendijk, M. , Gonzalez, A. , Mosquera, D. , & Solomon, R. (2014). Dissociation of the Personality and EMDR Therapy in Complex Trauma-Related Disorders: Applications in Phases 2 and 3 Treatment. Journal of EMDR Practice and Research. 8(1), 33 -48. Van der Hart, O. , Nijenhuis, E. , & Steele, K. (2006). The Haunted Self: Structural Dissociation and the Treatment of Chronic Traumatization. New York: Norton and Company. Van der Hart, O. , Nijenhuis, E. , & Solomon, R. (2010). Dissociation of the Personality in Complex Trauma-Related Disorders and EMDR: Theoretical Considerations. Journal of EMDR Practice and Research. 4(2), 76 -92. 3/3/2017 © Kathleen M. Martin 2017 87
- Slides: 87