Integrated Brain Imaging Center Structural Imaging BIC Mission

Integrated Brain Imaging Center Structural Imaging BIC

Mission To develop and apply semi-quantitative and quantitative MRI Imaging and Image Analysis Techniques

UW Epidemiological Studies • We are the imaging core for a large number of NIH funded multicenter longitudinal cohort studies to identify imaging risk factors for stroke and dementia • Cardiovascular Health Study – 18 years; 5888 subjects, identified risk predictors for stroke, USA • Atherosclerotic Risks in the Community – 13 years, 2000 subjects, USA • Strong Brain Study, 1000 subjects, USA • SABRE Stroke and Dementia Cohort, 2000 subjects, England

CHS 5888 participants Baseline 65+ (4 Centers) Medicare sample 1989 -90 “risk factor” assessment Stroke and TIA

The Cardiovascular Health Study • Assess numerous characteristics at baseline and annually • Blood pressure, weight, FEV 1, presence of atrial fibrillation, ABI, smoking • EKG, echocardiography, carotid ultrasound ENDPOINT: Stroke or TIA Surveillance of subsequent hospitalizations for event accrual

CHS • The challenge - occurrence of the endpoint, stroke and TIA, was relatively infrequent, – 6% • Diminished the power to detect correlations • Concern was that this study would require an increase in sample size or prolonged period of events accrual – $$$$$$ – BIAS DUE TO LOSSES TO FOLLOW-UP

CHS • We proposed that cerebral MRI could be used to detect a surrogate endpoint for stroke – Less expensive – Increase power to detect correlates and risk factors – Avoid “loss to follow-up” bias
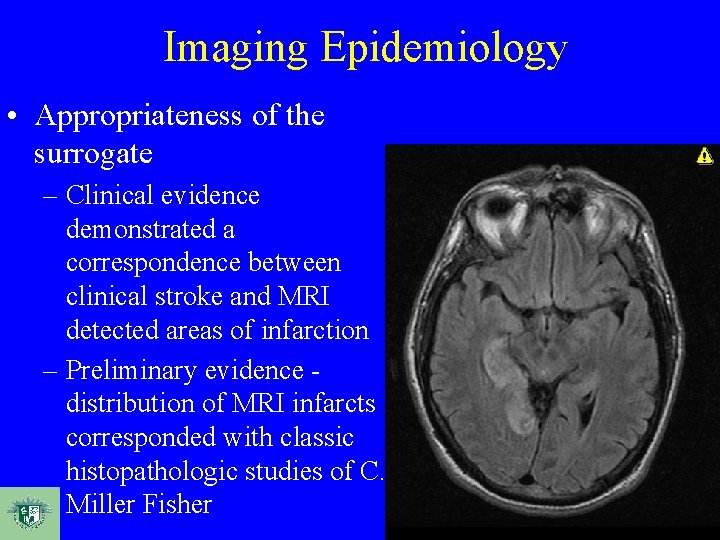
Imaging Epidemiology • Appropriateness of the surrogate – Clinical evidence demonstrated a correspondence between clinical stroke and MRI detected areas of infarction – Preliminary evidence distribution of MRI infarcts corresponded with classic histopathologic studies of C. Miller Fisher
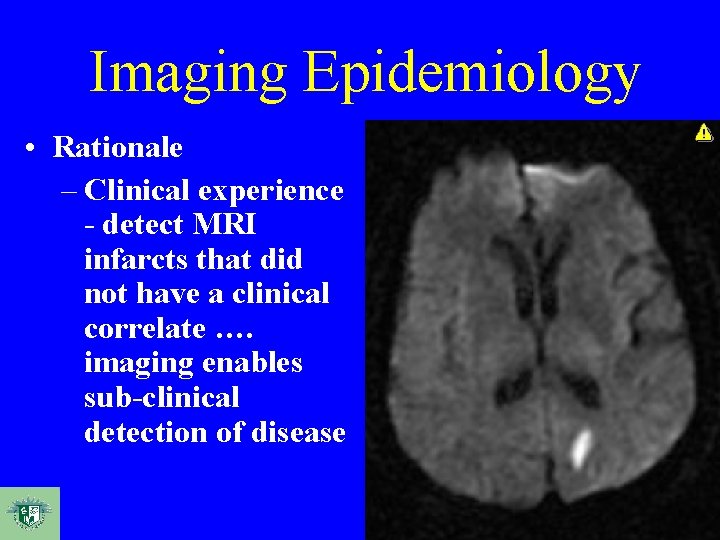
Imaging Epidemiology • Rationale – Clinical experience - detect MRI infarcts that did not have a clinical correlate …. imaging enables sub-clinical detection of disease

Methods • CHS participants underwent cerebral MRI • Pittsburgh, Pennsylvania Winston Salem, North Caroline • Sacramento, California Hagerstown, Maryland – acquired image data transferred to the MRI Reading Center

Methods -MRI Reading Center • interpreted in a standardized protocol – blinded to all clinical information including age, gender, cognitive function and race

Methods -Grading Systems • Infarcts were mapped to 23 anatomic locations – Size – Number

findings – MRI exquisitively sensitive in the detection of subclinical cerebrovascular disease – infarct-like lesions in 36% of the population – 6 fold increase in power to detect associations by incorporating imaging

Epidemiology –Enabled identification of correlates most commonly associated with stroke – Epidemiological study value • identified the correlates to address and individual most likely to benefit • Improved cost and outcome
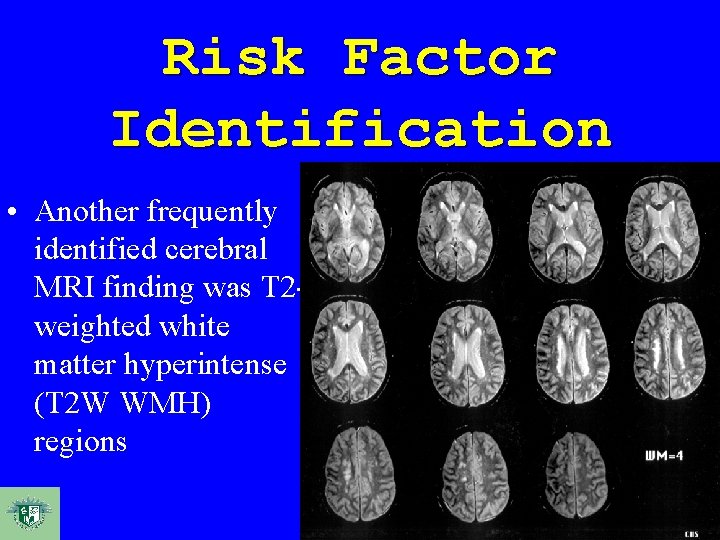
Risk Factor Identification • Another frequently identified cerebral MRI finding was T 2 weighted white matter hyperintense (T 2 W WMH) regions

Methods -Grading Systems • white matter signal changes of each individual assessed on a semi-quantitative ten-point WMG (0 -9) scale • pre-defined visual standards of 8 reference cases • total extent of periventricular and subcortical white matter signal abnormality on spin density weighted images • increased from no or barely detectable changes (grades 0 and 1 respectively) to almost all white matter involved (grade 9) Manolio TA, Stroke 1994
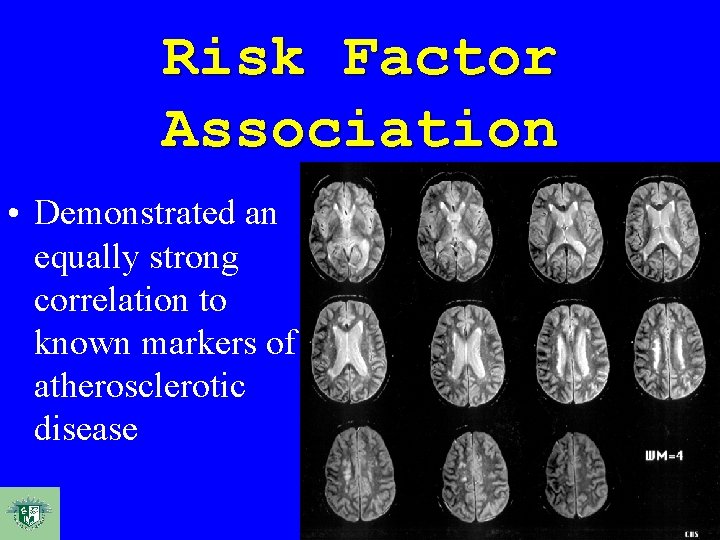
Risk Factor Association • Demonstrated an equally strong correlation to known markers of atherosclerotic disease

A new type of risk predictor • Demonstrated imaging good outcome measure • ? Value of imaging subclinical markers as predictors of disease risk • Hypothesis-T 2 W WMH is a significant subclinical predictor of stroke risk

Methods - Event Ascertainment • incident stroke the outcome of interest • participants without prevalent disease at the time of the year five MRI scan were considered “at-risk” for stroke • “possible” events ascertained every six months Price TR, AEP, 1993; Ives DG, An Epid 1995

Events • Strokes occurred in 159 -participants in the analysis incidence 12. 1/ 1000 p-yr

Risk Factor Identification • Using multiple logistic regression, stepwise increase in the hazard ratio – WMG = 2 (HR=1. 5) – WMG = 3 (HR=2. 4) – WMG = 4(HR=3. 2) – WMG > 5 (HR=3. 9) *controlling for known stroke risk factors of age, gender, race, systolic BP, diabetes, cardiovascular disease, atrial fibrillation, internal carotid wall thickness and elevated creatinine

Risk Factor Identification • combining WMG > 2 with known risk factors for cerebrovascular disease – WMG >2 with hypertension (HR = 3. 4) – WMG > 2 with diabetes (HR = 2. 4) – WMG >2 with history of MI (HR = 3. 2) – WMG >2 with history of CHF (HR = 2. 5) – WMG >2 with atrial fibrillation (HR = 7. 9)

Risk Factor Identification • Thus, imaging correlates, independent and in combination, were a better risk predictor than any previously identified risk factor from the Framingham Study – Further target the subset of individuals at greatest risk – Imaging decreasing cost and improving outcome

CHS Cognition Study: MRI Followup CHS 5888 participants 65+ (4 Centers) Medicare sample 1989 -90, 1992 -93 MRI Brain 1992 -94 3608 Measurement of incidence of dementia 2 nd MRI: 2112 1997 -99 1581 Normal 301 MCI 195 Incident dementia between MRI’s 35 Prevalent dementia at first MRI

— Odds Ratio Results of Logistic Regression Analysis for Risk of Alzheimer’s Disease vs. Normals (excludes MCIs) Among Normals and Cases Incident for AD at the 1 st MRI Who are Prevalent at the 2 nd MRI Age at MRI 2 3 MSE at HS or less Apo. E 4 MRI 1 Vs. >HS (yes vs no) Race Sex Vent. Size 5+ at 2 nd MRI Variables in the Model CHS Dementia Study

— — Odds Ratio Results of Logistic Regression Analysis for Risk of Dementia Among Non-Demented Cases and Cases Incident at MRI 1 but Prevalent at MRI 2: Controlling for Time Between MRIs Age at MRI 2 3 MSE at Grade Apo. E 4 Race Sex MRI 1 Inc. by 2+ Time MRI 1 (HS or less(yes vs no)(non-white (female Vent 5+ grades at between vs. >HS) vs. white) vs. male) vs. <5 MRI 2 MRIs (yrs) Variables in the Model CHS Dementia Study

Measurements • Quantitative – Infarct like lesions – Hippocampal volumes – White matter ischemia • Semiquantive – White matter grade – Ventricular grade – Sulcal grade – Quantitative

Acknowledgments supported by N 01 -HC-85079 to N 01 -HC 85086, N 01 -HC-35129 and N 01 -HC- 15103 from the National Heart, Lung and Blood Institute.

Acknowledgments Wake Forest University School of Medicine: Gregory L. Burke, MD, Sharon Jackson, Curt D. Furberg, David S. Lefkowitz, Mary F. Lyles, Cathy Nunn, John Chen, Beverly Tucker, Harriet Weiler; Wake Forest University – ECG Reading Center: Pentti M. Rautaharju, MD, Ph. D; University of California, Davis: John Robbins, MD, MHS; Johns Hopkins University: Linda P. Fried, MD, MPH; University of Washington Norman J Beauchamp MD MHS, Johns. Hopkins University – MRI Reading Center: Nick Bryan, MD, Ph. D, University of Pittsburgh: Lewis H. Kuller, MD, Dr. PH; University of California at Irvine – Echocardiography Reading Center (baseline): Julius M. Gardin, MD; Georgetown Medical Center – Echocardiography Reading Center (followup): John S. Gottdiener, MD; New England Medical Center Boston – Ultrasound Reading Center: Daniel H. O’Leary, MD; University of Vermont – Central Blood Analysis Laboratory: Russell P. Tracy, Ph. D; University of Arizona at Tucson – Pulmonary Reading Center: Paul Enright, MD; Retinal Reading Center – University of Wisconsin: Ronald Klein, MD; University of Washington – Coordinating Center: Richard A. Kronmal, Ph. D; NHLBI Project Office: Jean Olson, MD, MPH.
- Slides: 29