Insulin Use in Diabetes Mellitus Jennifer Beggs Introduction

Insulin Use in Diabetes Mellitus Jennifer Beggs

Introduction • • History of insulin Manufacture and secretion The insulin receptor Homeostatic role Insulin and diabetes mellitus Types of insulin in DM Rx Insulin use in Type 1 DM Insulin use in Type 2 DM

History of insulin • 1922: Bovine insulin first extracted • 1923: Nobel Prize in physiology and Medicine awarded to Toronto based team – F Banting and JJR Mac. Leod (shared with Best and Colling) • International recognition of Paulescu as the true discoverer of insulin 50 years later • 1958: Primary structure determined by British molecular biologist Frederick Sanger (Nobel Prize in Chemistry). First protein to have its sequence be determined • 1969: Tertiary structure (conformation) determined by Dorothy Crowfoot Hodgkin, using X-ray diffraction studies

Insulin Formation and Secretion Endogenous peptide hormone Coded for on chromosome 11 Controlled release of chemical energy from food Secreted by beta islet cells of pancreas Intracellular conversion: pre-proinsulin to insulin • Two pathways: constitutive and regulated • Secretion into portal circulation • Primary target is liver • • •

Insulin Receptor • Cell membrane glycoprotein • Insulin binding to alpha-subunits • Conformational change leads to cascade response • Glucose transporter moves to cell surface • Increased glucose uptake into cell • Receptor complex recycled

Glucose homeostasis • Homeostasis of blood glucose (63 -144 mg/d. L) • FASTING – Insulin secretion reduced – Regulation of glucose release by liver • POSTPRANDIAL – Insulin secretion increased – Increased glucose uptake by fat and muscle • Insulin antagonised by ‘anti-insulins’ – – Gluycagon Adrenaline Human growth hormone Cortisol

Insulin and Diabetes Mellitus • Diabetes mellitus: Syndrome of chronic hyperglycaemia due to insulin deficiency, resistance, or both • Type 1 DM: Absolute insulin deficiency • Type 2 DM: Relative insulin deficiency and/or insulin resistance

Types of Insulin Rx • Animal versus biosynthetic human insulin • Short acting insulin – Soluble insulin – Rapid acting insulin analogues • Intermediate/long acting – Protamine/zinc formulations – Long acting insulin analogues • Mixed insulin (biphasic)

Short Acting Insulins • Soluble – SC administration • Onset 30 -60 mins • Peak 2 -4 hrs • Duration <8 hrs • Rapid analogues – Lispro, Aspart – Quicker onset, shorter half-life – Reduced hypoglycaemia

Intermediate / Long acting • Addition of protamine/zinc – crystal formation • SC administration – Onset 1 -2 hrs – Peak 4 -12 hrs – Duration 16 -35 hrs • Analogues – Glargine – Reduced solubility at lower p. H

Mixed (Biphasic) • Pre-mixed insulin containing a short and intermediate/long acting insulin • Usually 30: 70 ratio • Fewer injections • Less flexibility of lifestyle

Example Regimens in Type 1 DM • Mixed insulin bd before meals • Short acting td before meals and intermediate/long od before bed • Adjustment of insulin as appropriate for blood glucose result
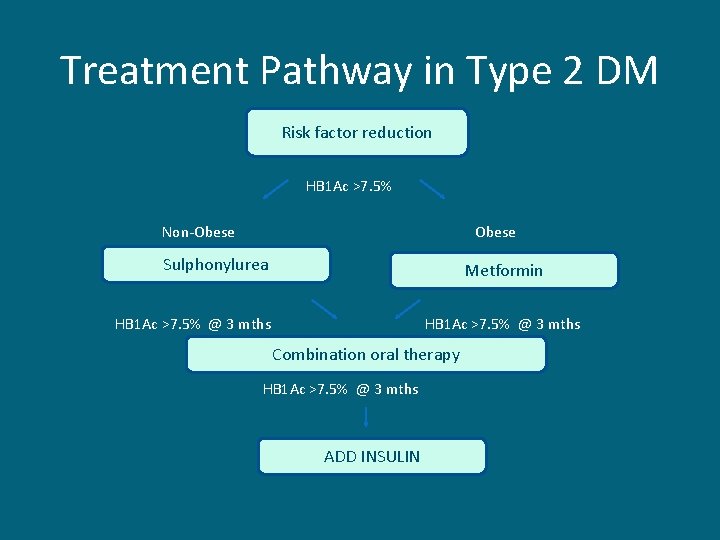
Treatment Pathway in Type 2 DM Risk factor reduction HB 1 Ac >7. 5% Non-Obese Sulphonylurea Metformin HB 1 Ac >7. 5% @ 3 mths Combination oral therapy HB 1 Ac >7. 5% @ 3 mths ADD INSULIN

Hypoglycaemia • Most common complication of insulin Rx • Precipitated by alcohol, irregular eating habit, raised exertion levels • Symptoms and signs develop over a few minutes – – – – Sweating Tremor Palpitations Drowsiness Behavioural changes Coma Rarely – convulsions, hemiparesis • Most DM sufferers experience symptoms • 1/3 with at least one episode of coma

Thank you! • Questions?
- Slides: 15