Insulin Pump Therapy Bruce W Bode MD and

Insulin Pump Therapy Bruce W. Bode, MD and Sandra Weber, MD
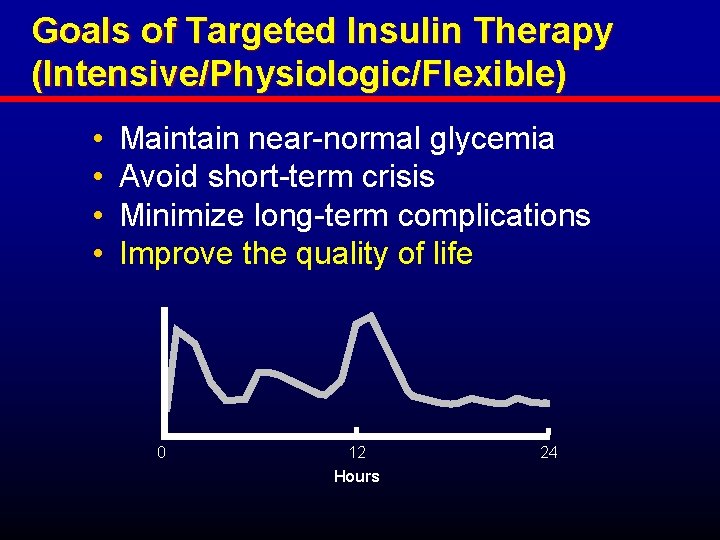
Goals of Targeted Insulin Therapy (Intensive/Physiologic/Flexible) • • Maintain near-normal glycemia Avoid short-term crisis Minimize long-term complications Improve the quality of life 0 12 Hours 24
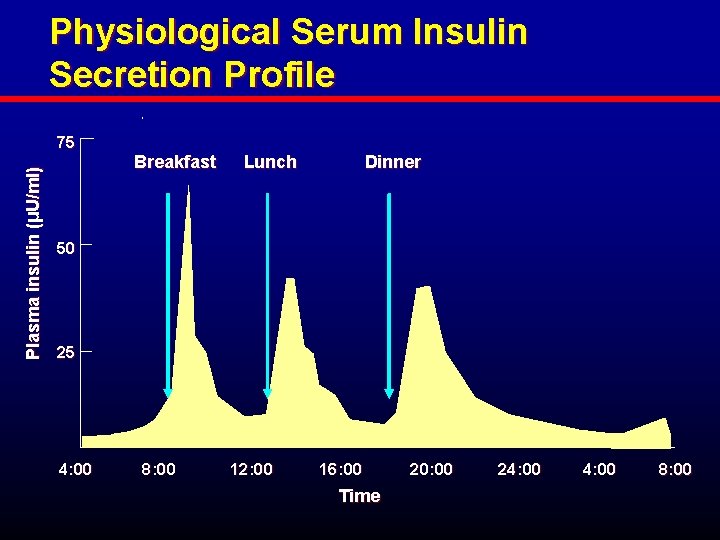
Physiological Serum Insulin Secretion Profile Plasma insulin (µU/ml) 75 Breakfast Lunch Dinner 50 25 4: 00 8: 00 12: 00 16: 00 Time 20: 00 24: 00 8: 00
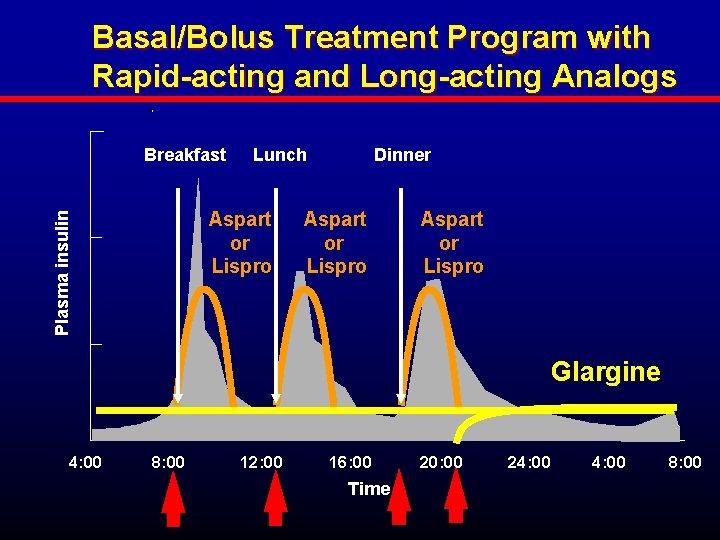
Basal/Bolus Treatment Program with Rapid-acting and Long-acting Analogs Breakfast Lunch Plasma insulin Aspart or Lispro Dinner Aspart or Lispro Glargine 4: 00 8: 00 12: 00 16: 00 Time 20: 00 24: 00 8: 00
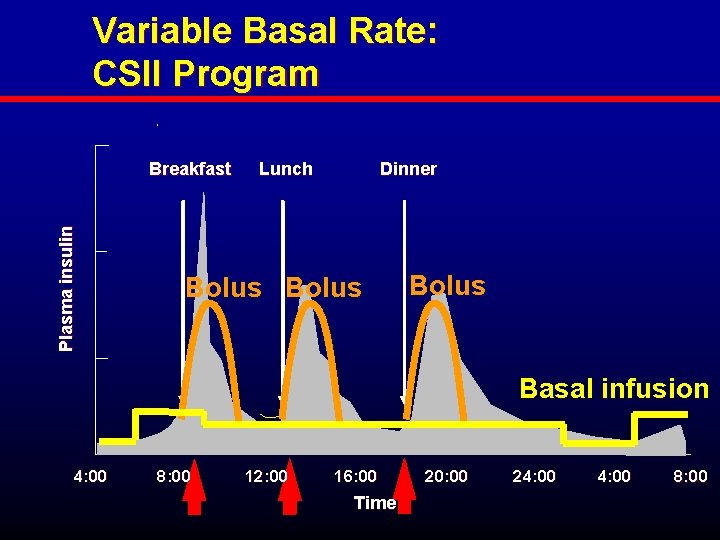
Variable Basal Rate: CSII Program Plasma insulin Breakfast Lunch Dinner Bolus Basal infusion 4: 00 8: 00 12: 00 16: 00 Time 20: 00 24: 00 8: 00

Metabolic Advantages with CSII • Improved glycemic control • Better pharmacokinetic delivery of insulin — Less hypoglycemia — Less insulin required • Improved quality of life
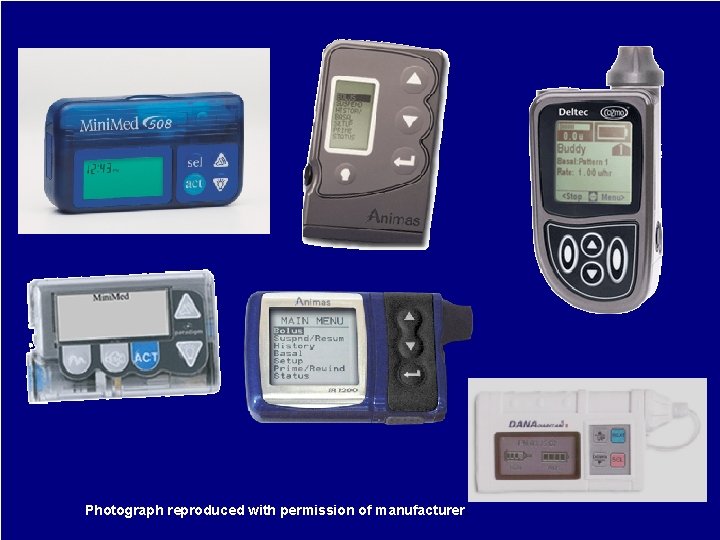
Photograph reproduced with permission of manufacturer.
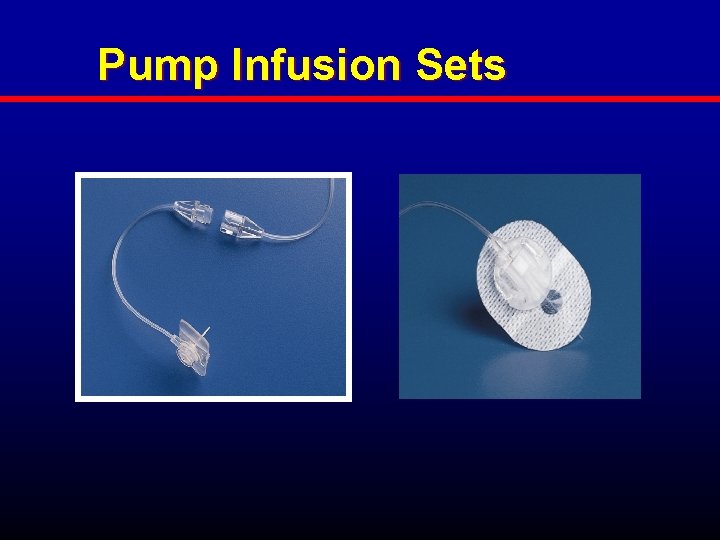
Pump Infusion Sets

Current Pump Therapy Indications • • Diagnosed with diabetes (even new-onset type 1 diabetes) Need to normalize blood glucose — A 1 C > 6. 5% — Glycemic excursions — Hypoglycemia • Need for flexible insulin program

CSII Factors Affecting A 1 C • Monitoring — A 1 C = 8. 3 - (0. 21 x BG per day) • Recording 7. 4 vs 7. 8 • Diet practiced — CHO: 7. 2 — Fixed: 7. 5 — WAG: 8. 0 • Insulin type (Aspart) Bode et al. Diabetes 1999; 48 Suppl 1: 264 Bode et al. Diabetes Care 2002; 25 439

Initial Adult Dosage: Calculations Starting doses • Based on pre-pump total daily dose (TDD) Ø reduce TDD by 25% to 30% for pump TDD • Calculated based on weight Ø 0. 24 x weight in lb (0. 53 x weight in kg) Bode BW, et al. Diabetes. 1999; 48(suppl 1): 84. Bell D, Ovalle F. Endocr Pract. 2000; 6: 357 -360. Crawford LM. Endocr Pract. 2000; 6: 239 -243.

Target BG Ranges for CSII • Normal —Preprandial: 70 - 140 mg/dl — 1 hr postprandial: <160 mg/dl • Hypoglycemic unawareness —Preprandial: 100 - 160 mg/dl • Pregnant —Preprandial: 60 - 90 mg/dl — 1 hr postprandial: <120 mg/dl Individually set for each patient Fanelli CG et al. , Diabetologia 1994, 37: 1265 -76. Jovanovich L, AMJOb. Gynec 1991, 164: 103 -11.

Initial Adult Dosage: Calculations Basal rate • 45% to 50% of pump TDD • Divide total basal by 24 hours to decide on hourly basal • Start with only 1 basal rate • See how it goes before adding basals

Basal Dose Adjustment Overnight Rule of 30: Check BG ü Bedtime ü 12 AM ü 3 AM ü 6 AM Adjust overnight basal if readings vary > 30 mg/dl

Basal Dose Adjustment Overnight • Adults often need an increase in basal rate in the “Dawn” hours (4 am to 9 am) • Children often need an increase in basal rate earlier starting at 10 pm to 2 am
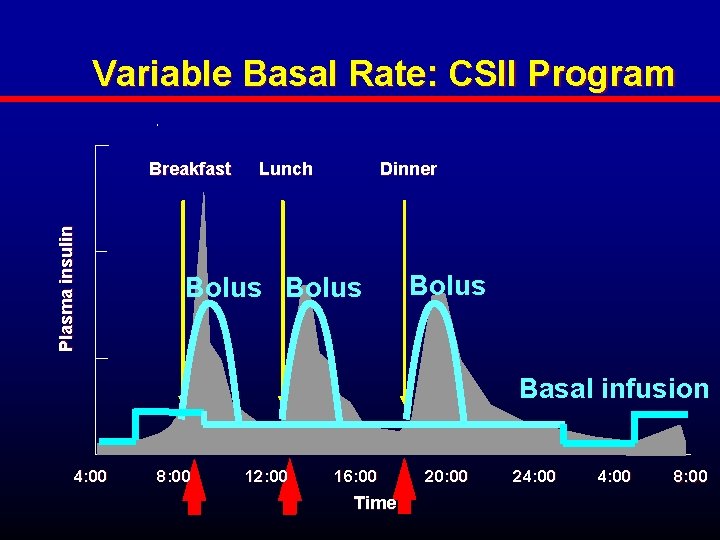
Variable Basal Rate: CSII Program Plasma insulin Breakfast Lunch Dinner Bolus Basal infusion 4: 00 8: 00 12: 00 16: 00 Time 20: 00 24: 00 8: 00

Basal Dose Adjustment Daytime Rule of 30: Check BG üBefore usual meal time üSkip meal üEvery 2 hrs (for 6 hrs) Adjust daytime basal if readings vary > 30 mg/dl

Bolus Dose Calculations Meal (food) Bolus Method 1 • Test BG before meal • Give pre-determined insulin dose for pre-determined CHO content • Test BG after meal • Goal < 60 mg/dl rise post meal or < 160 mg/dl

Estimating the Carbohydrate to Insulin Ratio (CIR) Individually determined • CIR = (2. 8 x wgt in lbs) / TDD • Anywhere from 5 to 25 g CHO is covered by 1 unit of insulin Davidson et al: Diabetes Tech & Therap. April 2003

Correction Bolus • Must determine how much glucose is lowered by 1 U of rapid-acting insulin • This number is known as the correction factor (CF) • Use the 1700 rule to estimate the CF • CF=1700 divided by TDD example: if TDD=36 U, then CF=1700/36= 50, meaning 1 U will lower the BG 50 mg/d. L

Correction Bolus Formula Current BG - Ideal BG Glucose Correction Factor Example: —Current BG: 220 mg/d. L —Ideal BG: 100 mg/d. L —Glucose CF: 50 mg/d. L 220 - 100 50 = 2. 4 U

If A 1 C is Not to Goal Must look at: • SMBG frequency and recording • Diet practiced —Do they know what they are eating? —Do they bolus for all food and snacks? • Infusion site areas —Are they in areas of lipohypertrophy? • Other factors: —Fear of low BG —Overtreatment of low BG

Case Study # 1 • • GL, male, age 39 Type 1 X 8 years A 1 C= 7%; recent increase from 6% CSII basal rates: 12 am 1. 0 u/h; 4: 30 am 1. 6 u/h; 11: 30 am 1. 0 u/h • Insulin: carbohydrate ratio =1 u : 10 grams • Correction Factor: BG - 100 divided by 40 • CGMS done to assist with improving overall glycemic control
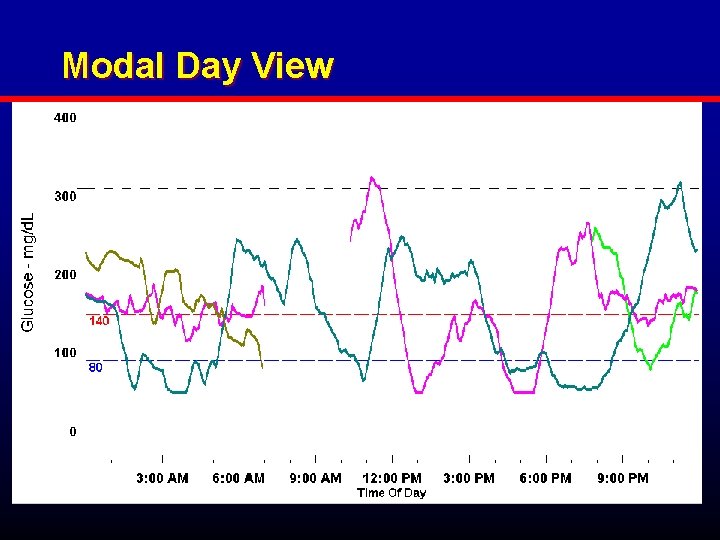
Modal Day View
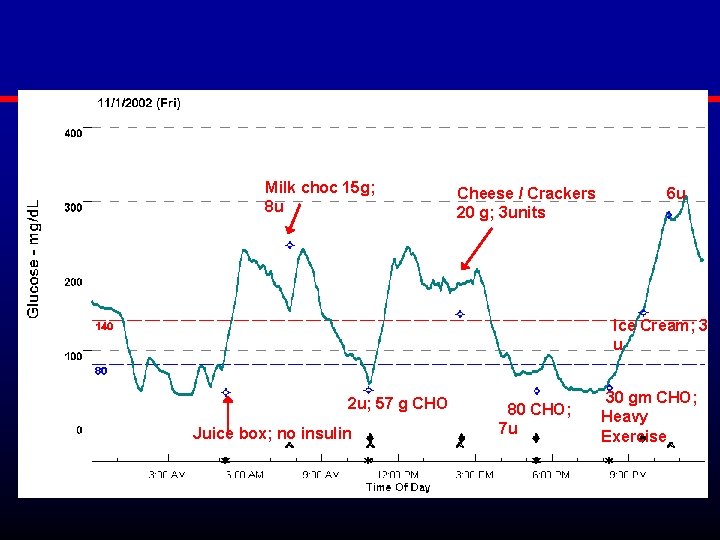
Milk choc 15 g; 8 u Cheese / Crackers 20 g; 3 units 6 u Ice Cream; 3 u 2 u; 57 g CHO Juice box; no insulin 80 CHO; 7 u 30 gm CHO; Heavy Exercise

Most common bolusing errors • Under-estimation of carbohydrates consumed (CHO bolus) • Over-correction of post-prandial elevations (CF bolus) — Remaining unused, active insulin — Stacking of boluses

Bolus: Source of Errors • “Inability” to count carbs correctly — Lack of knowledge, skill — Lack of time — Too much work • Incorrect use of SMBG number • Incorrect math in calculation • “WAG” estimations

The Major Problems ♦ Up until now we have not taken the active insulin issue into consideration ♦ The math involved with this has become too complicated, and it would be impossible to accurately calculate the active insulin without assistance

Smart Pumps

Bolus Wizard Calculator : meter-entered )))) ) ) ) )) ) Paradigm 512™ Paradigm Link™ • Monitor sends BG value to pump via radio waves : No transcribing error • Enter carbohydrate intake into pump • “Bolus Wizard” calculates suggested dose
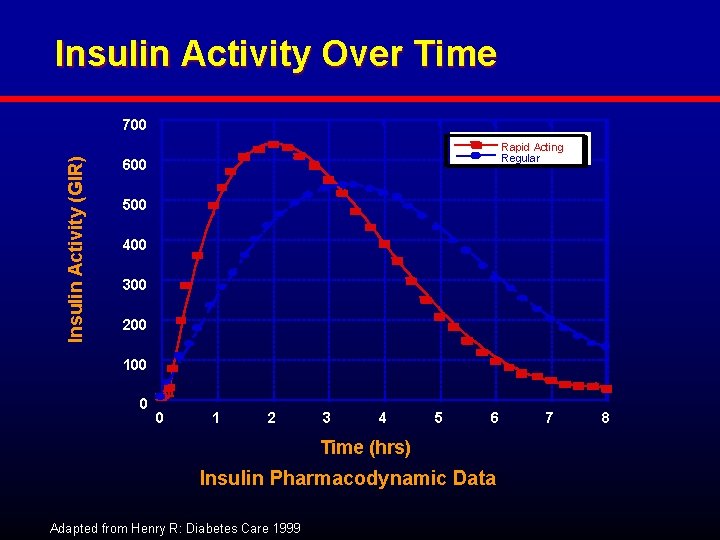
Insulin Activity Over Time Insulin Activity (GIR) 700 Rapid Acting Regular 600 500 400 300 200 100 0 0 1 2 3 4 5 6 Time (hrs) Insulin Pharmacodynamic Data Adapted from Henry R: Diabetes Care 1999 7 8
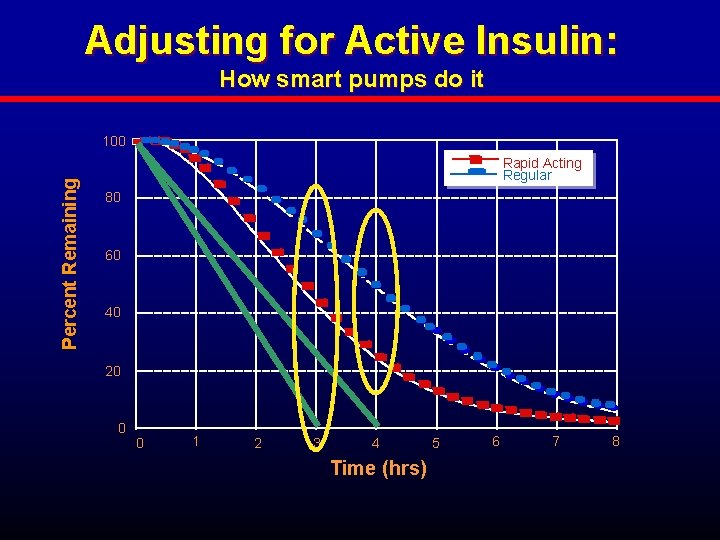
Adjusting for Active Insulin: How smart pumps do it Percent Remaining 100 Rapid Acting Regular 80 60 40 20 0 0 1 2 3 4 Time (hrs) 5 6 7 8

Bolus Wizard Set Up Screen Wizard: On Carb Units: grams Carb Ratios: 10 BG Units: mg/dl Sensitivity: 50 BG Target: 100

For This System To Work ♦ It is critical the target, basal doses, the correction doses, and the carbohydrate ratios are accurate ♦ Understanding how to match carbohydrate amounts with insulin is critical

Do Smart Pumps Enable Others To Go To CSII? • YES • All patients with diabetes not at goal are candidates for Insulin Pump Therapy - Type 1 any age - Type 2 - Diabetes in Pregnancy

Summary • Insulin pump therapy offers improved glucose control with less risk of hypoglycemia and an improvement in quality of life • Appropriate candidate selection, training, and follow-up ensures safe and effective therapy

Questions • For a copy or viewing of these slides, contact • WWW. adaendo. com
- Slides: 37