Instructions delete this slide before presenting This presentation

Instructions – delete this slide before presenting • This presentation can be used either as a complete in-service or as a practical follow-up session following staff completing the ‘Understanding radiation oncology’ rapid learning. • If using as a complete in-service start from slide 2. • If using as a follow-up session, start from slide 24. • Read through all slides and notes and adapt contents as necessary to ensure contents are consistent with local policies, procedures and models of care. • All case studies contained within this presentation are fictional. • All patient management information contained in this presentation is an examples only and is not designed to be used as a management guideline in clinical practice. • Refer to your local policies and procedures regarding the management of oncological emergencies and radiation toxicities.

Radiation therapy Introduction and practical points Developed in collaboration with the Central Coast Cancer Centre

Contents 1 Introduction to radiation therapy 2 Indications for radiation therapy 3 Side effects 4 Case studies 5 Quiz
What is radiation therapy? • Treatment of cancer with ionising radiation • Local treatment

How does it work to treat cancer? • • Stops cells from replicating Causes damage to cellular DNA Ø Direct – breaks in DNA strands Ø Indirect – free radical production • Cancer cells – more susceptible to damage, less able to repair damage Normal cells – able to repair damage and recover •
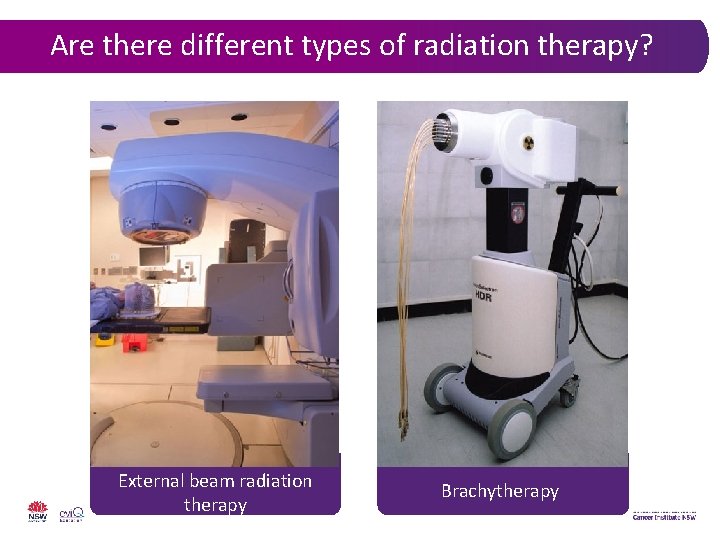
Are there different types of radiation therapy? External beam radiation therapy Brachytherapy
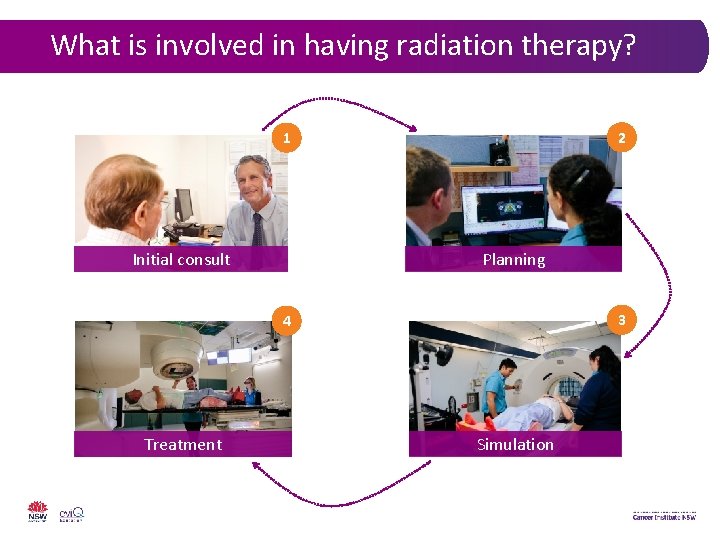
What is involved in having radiation therapy? 2 1 Planning Initial consult 3 4 Treatment Simulation
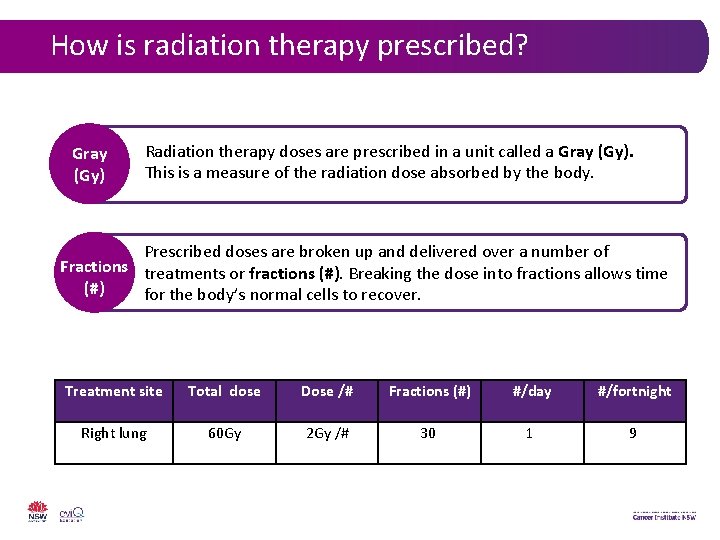

How is radiation therapy prescribed? Gray (Gy) Radiation therapy doses are prescribed in a unit called a Gray (Gy). This is a measure of the radiation dose absorbed by the body. Prescribed doses are broken up and delivered over a number of Fractions treatments or fractions (#). Breaking the dose into fractions allows time (#) for the body’s normal cells to recover. Treatment site Total dose Dose /# Fractions (#) #/day #/fortnight Right lung 60 Gy 2 Gy /# 30 1 9

Who can benefit from radiation therapy? Approximately 50% of all people diagnosed with cancer can benefit from radiation therapy in the management of their disease. Treatment intent Treatment setting • Curative • Sole treatment • Palliative • In combination with other modalities • Prophylactic • Emergency
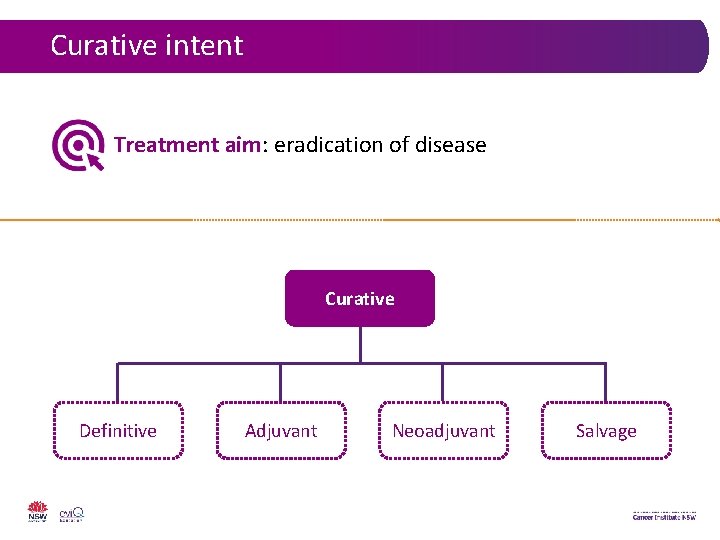
Curative intent Treatment aim: eradication of disease Curative Definitive Adjuvant Neoadjuvant Salvage
Curative - definitive • radiation therapy is the sole or primary treatment modality • Systemic anti-cancer therapies may be delivered concurrently as a radiosensitiser • Cancer types üProstate üCervical üHead and neck üLung üAnal üColorectal üOesophageal üSkin üBladder üBrain

Curative - adjuvant • radiation therapy is delivered after primary treatments • Aims to: Ø reduce the risk of the cancer returning locoregionally Ø improve survival. • Cancer types üBreast üColorectal üCervical üEndometrial üOesophageal üHead and neck üMelanoma and skin üLung

Curative - neoadjuvant • radiation therapy is delivered before surgery • Aim: improving surgical outcomes e. g. shrinking the tumour to improve operability • Cancer types üOesophageal üRectal üSarcoma üLung (Pancoast)

Curative - salvage • Delivered after primary treatments have failed • Aim: to eradicate residual disease • Cancer types üProstate bed (following removal of prostate)

Prophylactic Aim: to eradicate subclinical disease in order to prevent or delay the clinical spread of disease. • May provide benefit in those cancers where the pattern of disease failure is well recognised. • Cancer types ü Prophylactic cranial irradiation in lung cancer

Palliative Aim: control symptoms, improve quality of life Indications • Painful bone metastases • Presence of brain metastases • Skin lesion which is eroding the skin • Oesophageal tumour causing dysphagia • Shortness of breath from lung cancer • Pain, abdominal distension from liver metastases • Haematuria from bladder cancer
Emergency Aim radiation therapy is used to shrink the tumour with the aim of: • reducing pain • reducing bleeding • alleviating obstruction • reducing compression. Indications For urgent referral to radiation oncology: • moderate to severe cancer pain • spinal cord compression • uncontrolled bleeding due to cancer • superior vena cava obstruction.
Spinal cord compression • Spine metastases can compress the spinal cord • Swift intervention required • Left untreated can lead to permanent damage and functional loss Signs and symptoms: • pain that is increasing • muscle weakness • sensory loss • numbness • paraesthesia • bladder and bowel dysfunction and incontinence • ataxia.

Superior vena cava (SVC) obstruction • Some tumours may compress the SVC • May result in: • breathing compromise • cerebral oedema • death. Signs and symptoms: • oedema (head and neck region) • swelling of the upper extremities • dysphagia cough • hoarseness • dyspnoea • distorted vision • headaches • nausea.
What treatment related toxicities are possible? Sub-acute - Weeks to months following treatment Acute Late • during treatment • usually temporary • months following treatment • may be long-term or permanent

Treatment related toxicities • Localised to anatomical site or system being treated • Differ according to treatment site • Examples • Diarrhoea (pelvis) • Nausea and vomiting (abdomen or neurological) • Mucositis (head and neck) • Skin reaction (any site)
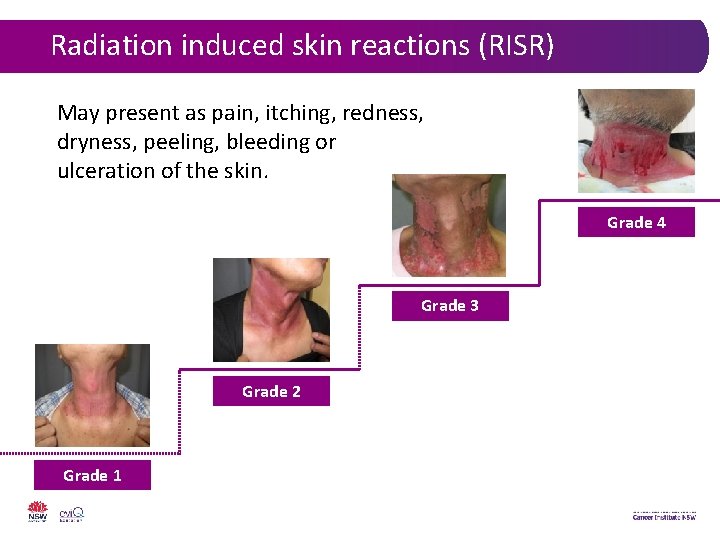
Radiation induced skin reactions (RISR) May present as pain, itching, redness, dryness, peeling, bleeding or ulceration of the skin. Grade 4 Grade 3 Grade 2 Grade 1

Management of RISR • Management differs according to grade experienced • Manage with a step up approach • Unbroken skin – maintain moisture levels • Broken skin – maintain a moist (not wet) healing environment • Manage symptoms • MDT care – grade 4

What did you remember? Quiz

Question 1 Why are radiation therapy doses delivered in fractions? The total dose is broken up and delivered in fractions to allow time for the body’s normal cells to recover between doses.

Question 2 What patients may benefit from the use of radiation therapy in the management of their disease? Radiation therapy can be used in the management of almost all cancers as a curative treatment, to palliate symptoms or as a prophylactic treatment. Radiation therapy can be used as a sole treatment or in combination with other treatment modalities.

Question 3 Some indications for radiation therapy are considered an emergency and require an urgent referral. What are they? • • • Moderate to severe cancer pain Spinal cord compression Uncontrolled bleeding due to cancer Superior vena cava obstruction Airway/bronchial obstruction

Question 4 What are the types of radiation therapy side effects? What is the pattern of onset for each of these? BONUS points if you give an example of each. Acute • start presenting after the first week or two or treatment • begin to resolve a few weeks after completing treatment • e. g. radiation induced skin reaction. Subacute • start presenting weeks or months after treatment has been completed • e. g. radiation induced pneumonitis following radiation to the chest Late • start to present months after treatment. • may be long term or permanent • e. g. cataracts following irradiation to the head and neck or brain region.

Question 5 Most side effects from radiation therapy are ‘site specific’ or localised to the anatomical site or system being treated. What acute side effects may be experienced by patients receiving radiation therapy to the following sites? Breast Abdomen Head and neck • RISR • breast oedema • rib pain. • RISR • nausea and vomiting • diarrhoea • anorexia • gastritis • enteritis. • • RISR dysphagia odynophagia xerostomia dysgeusia mucositis tinnitus.

Apply what you’ve learnt Case studies

Case study 1 Palliative Treatment - Consultation

The patient • You are the ward JMO • A 64 yo M was admitted with metastatic prostate cancer • He is now complaining of pain all over the body • Your Registrar reviews the patient and requests a Rad onc consult How will you make this consult?

What might the rad onc registrar plan/suggest? Assessment Clarifies the indication/problem Prostate • What is the primary cancer/diagnosis? Metastatic. Results of recent bone/PET scans show • Where is the cancer? sclerotic lesions at T 8 and L 5 • Where are the problem areas? Pain in lower and upper back, legs and right ribs Reviews the treatment Hx Yes - previously at another hospital Previous salvage RT following RP • Is the patient known to any Radiation oncologist? • Has the patient received radiation before? Performs a thorough clinical assessment • ECOG status 1 • Physical examination Pain likely referred from spine mets, ribs not tender to palpation

Plan • • For simulation scan today Aim to commence RT 1 -3 days 20 Gy/5# to the L and T spine mets Request previous treatment details – check overlap with L spine What members of the MDT may you need to involve/consider? Palliative care review for pain management

Case study 2 Rad onc Emergency 1

The patient • 64 yo F presents with severe back pain, lower limb weakness and incontinence. Bg breast cancer • The ED JMO is asked to assess the patient How should the JMO approach this case?

What might the JMO consider in their management plan? Assessment Physical examination and history 2 days (>few days complete recovery less likely) • What is the duration of symptoms? Motor strength of lower extremities decreased, sensory • Neurological exam function reduced • Vertebral tenderness? Yes, tenderness in lumbar spine Imaging? Urgent Whole spine MRI ordered immediately Demonstrates compression at L 3 Spinal Instability Neoplastic Score • Score of 7 – 18 – potentially unstable (consider surgical consult): patients scores 6

Plan Consider: • glucocorticoids • decompressive surgery • radiation therapy Decision: • Sim today – plan and treat • EBRT 20 Gy/5#

Case study 3 Rad onc Emergency 2

The patient • You are a nurse working on an inpatient ward. • You are performing obs for a patient with a known lung cancer. • You note that the patient is experiencing mild SOB, some difficulty swallowing and mild facial oedema What may this patient be experiencing? • Potential SVC obstruction What action should the nurse take? • Request immediate medical review, complete obs • Consider head elevation and supplementary oxygen

Plan • The patient is reviewed and sent for CT • CT confirms obstruction of the SVC caused by large mediastinal mass (NSCLC) Consider: • Symptomatic management – Head elevation, oxygen, morphine for dyspnoea, glucocorticoids • radiation therapy • Chemotherapy, endovascular stenting Decision • radiation therapy • Sim today – plan and treat • 30 Gy/10#

Case study 4 Radiation toxicity

The patient • 65 yo M with oropharyngeal ca • Completed 7 weeks of definitive radiation therapy 3 days ago • Admitted for pain and desquamation of skin over neck, painful mouth ulcers and dehydration • The ward resident is asked to review the patient and provide management advice What may the resident consider in their assessment of this patient?

Assessment What may this patient be experiencing? What grade is being experienced? Complete patient assessment Reduced oral intake, recent weight loss of 5 kg, dehydration, reduced urinary output What might the resident consider in their management plan? Acute toxicities of radiation therapy – RISR, oral mucositis, dysphagia, xerostomia, anorexia RISRAS tool, mucositis assessment scale, CTCAE grading tool • RISR – grade 3 – moist desquamation and bleeding induced by minor trauma/abrasion • Oral mucositis – grade 3 – severe pain interfering with oral intake

Plan • Admit pt – monitor weight and oral intake • Commence IV hydration RISR • Dress neck with non-adherent absorbent dressing • Monitor for signs of infection • Paracetamol prn for pain Oral mucositis • Regular sodium bicarbonate mouthwashes • Topical anaesthetic • Short active and long acting analgesia titrated to effect

Debrief • Radiation therapy can be used in the management of almost all cancers as a curative treatment, to palliate symptoms or as a prophylactic treatment. • Some indications for radiation therapy are considered an emergency and require an urgent referral. • Side effects from radiation therapy may present as acute, sub acute or late. • Radiation therapy is a local treatment and only affects the area of body being treated. Side effects will be localised.
- Slides: 46