Innovate to change the future Strategy for Innovation











- Slides: 12

Innovate to change the future Strategy for Innovation May 2018

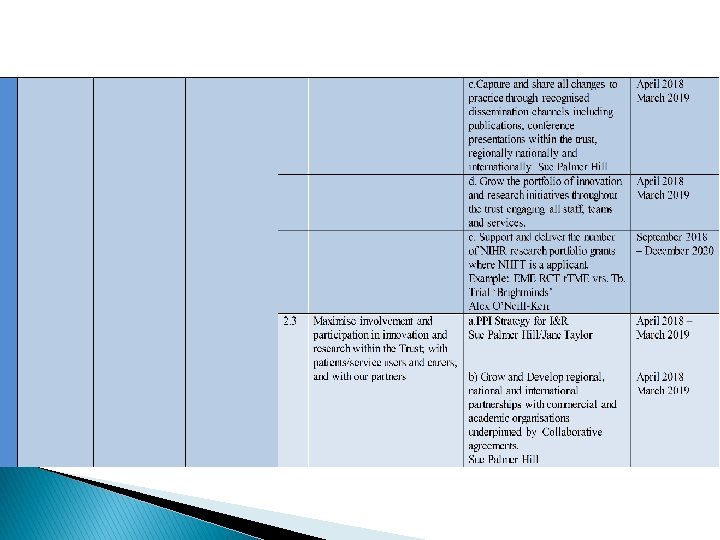
Strategic Theme 2: Innovate to change the future Outcome – what will it look/feel like in four years’ time? A diverse, contemporary organisation engaged in delivering and sharing innovations that are changing the future. Objectives – how will we achieve the outcome? 2. 1 Develop the culture, capacity and capability to support innovation and research within the Trust. 2. 2 Change practice and services whilst demonstrating improved clinical effectiveness through a programme of clinical and technological innovation and research 2. 3 Maximise involvement and participation in innovation and research within the Trust; with patients/service users and carers; and with our partners

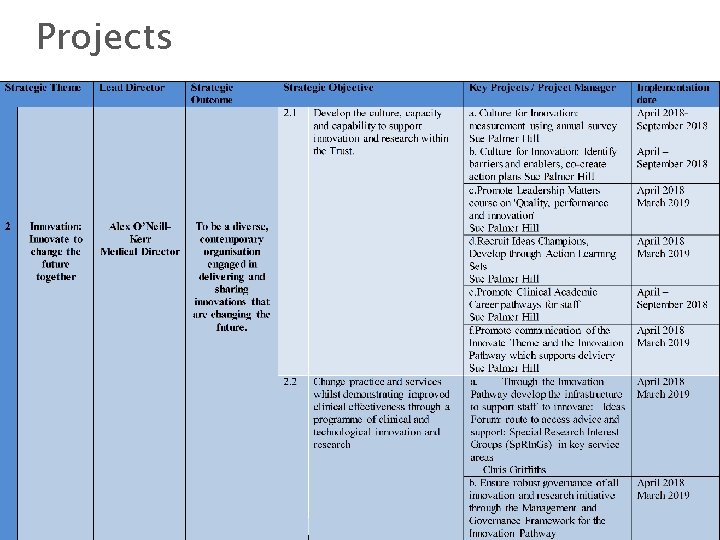
Projects


Background � Innovation Health and Wealth (DH 2011) � NHf. T outlined its rationale and business approach in ‘Research and Development Investing in the future’ Feb 2015 � Clinical Strategy, overarching aim 5. and the Quality Strategy aim 2, point 4 � Builds on areas of strength and expertise � 5 YFV 2016 � Innovation Pathway agreed to exec June 2017 � Strategy Refresh/SOFT autumn 2017 � Innovation and Creativity Conference Jan 2018 � Delivering our DIGBQ strategy together March 2018 � NHFT Clinical Strategy 2018

Objectives E Embed a culture for innovation build research capability and capacity deliver ‘What Works’ develop and strengthen collaborative partnerships build strong synergistic relationships with patients and public

Embed a culture for innovation and research Rationale: NHS trust have a duty to promote, innovation research and evidenced based practice. A vibrant innovation culture supports absorptive capacity, the ability to challenge, think creatively and adapt to new ideas. Research provides the necessary knowledge base that underpins high quality care. Actions � Develop trust innovation leadership; Senior Leadership Team engagement � Develop visible structure; Ideas Forum, Sp. RIn. Gs, Innovation Research and Clinical Effectiveness Committee � Promotion of the Innovation Pathway; individuals, teams, directorates � Visibility of Innovation across the trust; comms strategy � Access to expert advice and support; Innovation Space/I&R intranet page, Ideas Forum Measures � Recorded Innovation promotion at trust wide events � Supporting communication framework � Undertake annual ‘Innovation Culture’ Audit Mayer et al 2008 � Research ‘Innovation Culture’ within the trust (Prof Doc Thesis) � Quarterly reports to Exec. number of ideas presented and taken forward by Ideas Forum � Number of bids � Number of publications � Number of national conference presentations

Build research capacity and capability Rationale: Capacity can be defined as a process of individual and institutional development which leads to higher levels of skills and greater ability to perform: 8 elements; skill development; infrastructure, close to practice; linkages, partnerships and collaborations; dissemination; research; sustainable research activity. Research capability refers to the ability to deliver. Both have positive impacts on quality and workforce development and retention. (Sarre et al 2009) Actions � Establish links to education � Mentoring, budding and placements � Ideas Forum/Ideas champion to develop Ideas pipeline � Drop in sessions with Research Design Service � Develop and manage Intellectual Property Measures � Undertake annual Research Audit (ARC) Sarre et al 2009 � Ideas Forum metrics quarterly report � Number of people at drop in sessions � No. Masters/Ph. Ds � No. Intellectual Property output, including publications, conference presentations � Number of collaborative bids submitted; including bids with patients & carers

Deliver ‘What Works’ Rationale: Development and delivery of a blended evidence base to underpin practice. This includes the delivery of the NIHR portfolio research within the NHS contract, it also acknowledges other sources of evidence that answers the question ‘what works’ (Shepherd 2014). It includes innovations, research, service improvement, evaluation and audit. All research, evaluation and innovation projects must be delivered within a sound governance framework and to time and target. Actions: Increase productivity and capability of Innovation & Research Delivery Team � Increase number of Principal Investigators/co-applicants and collaborators � Increase the number of clinical areas engaged � Ensure robust Management & Governance Framework to manage risks � Integration across evidence areas in a blended approach, evaluation of transformational change � Develop models of share learning and mobilise knowledge � Measures Number of NHf. T projects delivered, including innovation, research, evaluation � East Midlands CRN NIHR portfolio activity report/Recruitment and time and target data � Number of commercial projects � Develop models of blended evidence � List of generated impacts � Generated income, including innovation/research grants �

Develop and strengthen collaborative partnerships Rationale: Horizontal integration. Internally NHf. T needs to ensure that all department and service are engaged with Innovation to develop the culture, capacity and increase delivery. This will include the development of innovation within service models and well and support from essential services ie pharmacy, IT, IG, comms Integration across health economy. NHf. T is a community health care trust working countywide and within an integrated health economy, this must be reflected in the Innovation Strategy it develops. Externally, NHf. T is not a university teaching hospital and has no single academic affiliation. Collaborative and crossdisciplinary partnerships, including industry influence the development of a strong innovation profile and high outputs. Action: � Development of horizontal integration of innovation across all departments and services, agreed ways of working, communication strategy � Development of horizontal integration of innovation across health economy � NIHR organisations; CLAHRC, CRN, RDS � Synergistic academic partnerships; Institute Health and Wellbeing, OU, Nottingham Northamptonshire Neuromodular Network (NX 4) � Medi. Link East Midlands, commercial & industry � Academic Health Science Network (AHSN) � Clinical Senate � Healthwatch and voluntary sector Measures � Recognition and capture of Innovation in trust and departmental strategies � Collaborative bid application � Formal collaborative agreements/memorandum of understanding in place with external partners � Attendance at partners/collaborator innovation meeting, ie Ideas Forum � Honorary posts with academic institutes

Build strong synergistic relationships with patients & public Rationale: Patient and Public Involvement (PPI) is a key part of the NHS and innovation strategy ensuring relevance and high quality outcomes for the intended end users. For the purpose of this document the term Stakeholder Involvement will be used as it is fundamental to include all stakeholders, patients, carers, public, staff, commissioners and providers to facilitate implementation and acceptability for all. Actions: � Provide better access to information regarding innovation and research opportunities, including Ideas Forum � PPI engagement on Ideas Forum and other activates � Develop models of Patient and Carer Experience and Insight � Promotion of ‘Its Ok to Ask’, Join Dementia Research � Engagement with trust PPI team, Healthwatch and voluntary sector, regional leadership in this area through CLHARC/Academic Health Science Network PPI lead Measures: � PPI representation on all groups � Annual NIHR ‘Mystery Shopper’ exercise � Formal collaborative agreements with patient groups � Number of training workshops delivered � New training packages developed

Contacts Sue Palmer Hill, RGN, MSc Head of Innovation and Research Northamptonshire Healthcare foundation Trust sue. palmer-hill@nhft. nhs. uk Tel: 01604 685563 Mob: 07827 319379