Inflammatory Bowel Diseases Ulcerative Colitis Crohns disease Are

Inflammatory Bowel Diseases

Ulcerative Colitis & Crohns disease Í Are chronic inflammatory bowel diseases with protracted relapsing & remitting coarse. Í The incidence of ( IBD ) vary between population. Í The incidence of UC is 10/ 100000, while CD is 5 -7/100000. Í CD & UC had 2 peaks 1 st in young & 2 nd in 7 th decade.

• There is dramatic increased in incidence of CD in western countries coinciding with the introduction of amore hygienic environment with the advent of domestic refrigeration & the wide use of antibiotics.

Factors associated with the development of (IBD) Genetic: o o o More common in Jews. 10% have + ve FH of IBD. High concordance between identical twins. Associated with autoimmune thyroiditis & SLE. Four regions of linkage on chromosomes 16, 12, 6 & 14 (IBD 1 -4 ). o HLA-DR 103 associated with sever UC. o UC & CD with HLA-B 27 commonly develop ankylosing spondylitis.

Environmental: o UC is more common in non-smokers & exsmokers. o CD most patients are smokers. o Associated with low residue , high refined sugar diet. o Commensal gut microbia altered ( Dysbiosis)in CD & UC. o Appendicectomy protects against UC.
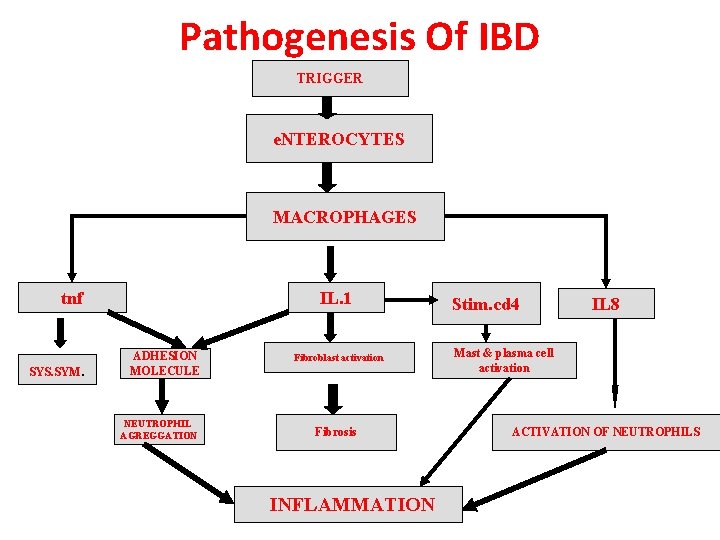
Pathogenesis Of IBD TRIGGER e. NTEROCYTES MACROPHAGES tnf SYS. SYM. IL. 1 ADHESION MOLECULE NEUTROPHIL AGREGGATION Fibroblast activation Fibrosis INFLAMMATION Stim. cd 4 IL 8 Mast & plasma cell activation ACTIVATION OF NEUTROPHILS

Common patterns of IBD distribution: Ulcerative colitis: - 40 -50% proctitis or proctosigmoiditis. - 30 -40% left sided colitis or extensive colitis. - 20% pan colitis.

, Crohns disease: - 40% Ileal or ileocolonic. - 30 -40% small intestinal. - 20% Crohns colitis. - <10% perianal disease (alone).

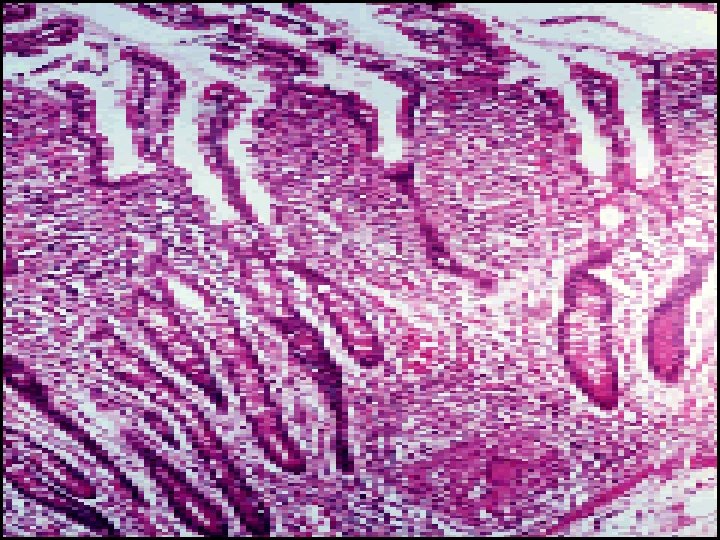
Histopathology of IBDS v. Ulcerative Colitis: -- The inflammatory process is limited to the mucosa. Acute & chronic inflammatory cells infiltrate the lamina propria & crypts ( Cryptitis ). Crypt abscesses are typical. -- Distorted Goblet cell which loss its mucus. -- Dysplasia : increased mitotic rate + nuclear atypia which herald the development of Ca colon.
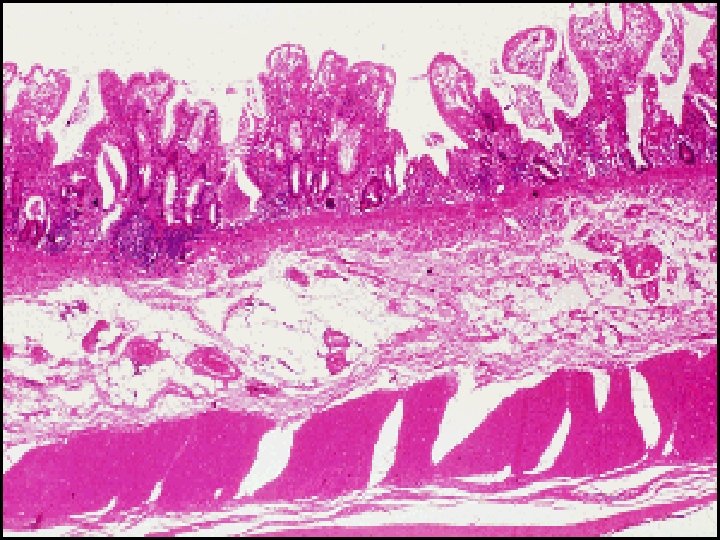
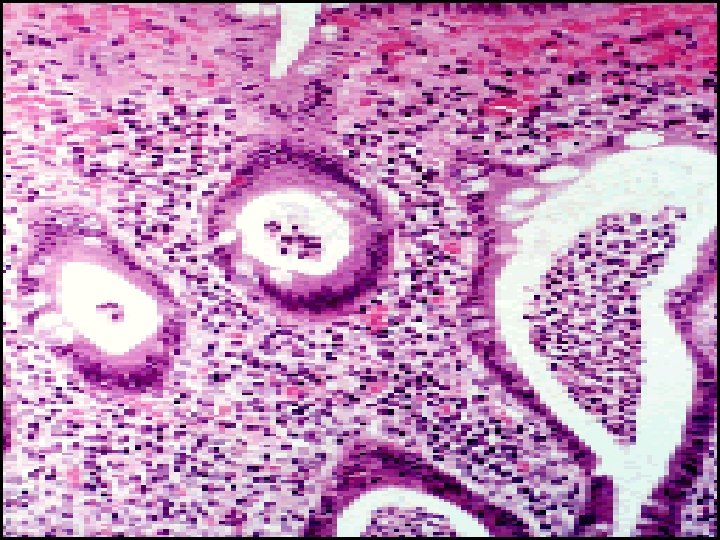
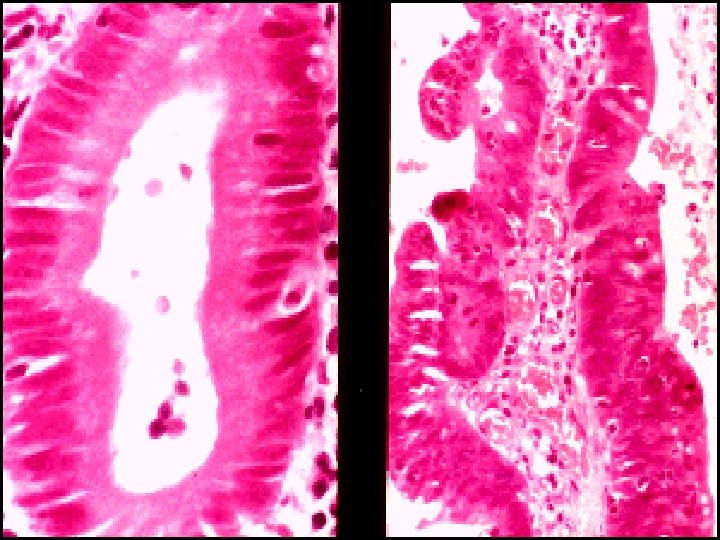

v. Crohn , s disease: --The whole wall of the intestine is oedematous & thickened , There are deep ulcers which appear as linear fissures with normal mucosa between them ( cobblestone). -- Fistulae & ulcers. -- The lesion is patchy ( skip lesion ). -- Chronic inflammatory cell infiltrate the whole layers -- Microgranuloma (aggregate of histeocytes which surrounded by lymphocytes & contain giant cells). -- Aphthus ulcer.

Clinical features of IBDS Ulcerative Colitis: -- The 1 st attack is most severe. -- Characterized by relapse & remission. -- Rarely chronic unremitting coarse.

Precipitating factors for acute relapse: Ø Gastroenteritis. Ø Antibiotic. Ø NSAIDS. Ø Emotional stress. Ø Intercurrent infection.

ÍProctitis: Rectal bleeding & mucous discharge some times with tenesmus , no constitutional symptoms. ÍProctosigmoiditis: bloody diarrhea with mucous , Small no. of patients with v. active limited disease develop fever, lethargy & abdominal discomfort. ÍExtensive colitis: bloody diarrhea with passage of mucous, in sever cases anorexia , nausea , weight loss & abdominal pain , patient is toxic with fever & tachycardia & signs of peritoneal inflammation.
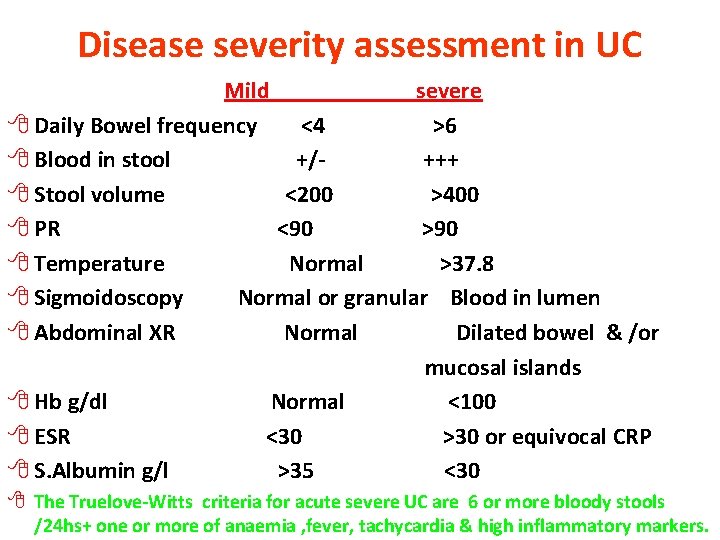
Disease severity assessment in UC Mild severe 8 Daily Bowel frequency <4 >6 8 Blood in stool +/+++ 8 Stool volume <200 >400 8 PR <90 >90 8 Temperature Normal >37. 8 8 Sigmoidoscopy Normal or granular Blood in lumen 8 Abdominal XR Normal Dilated bowel & /or mucosal islands 8 Hb g/dl Normal <100 8 ESR <30 >30 or equivocal CRP 8 S. Albumin g/l >35 <30 8 The Truelove-Witts criteria for acute severe UC are 6 or more bloody stools /24 hs+ one or more of anaemia , fever, tachycardia & high inflammatory markers.

Crohn , s disease: Ileal involvement: Abdominal pain which is associated with watery diarrhea (with out blood & mucous) + weight loss + features of protein & vitamines deficiencies. Crohn , s colitis: Like ulcerative colitis. *** Rectal sparing + Perianal disease*** Small bowel & colonic disease. Isolated Perianal disease. Severe oral ulceration.

Differences between UC & CD Ø 1 -UC involve only the colon while CD involve any part of GIT. Ø 2 -UC is continuous while CD is patchy. Ø 3 -Rectum is always involved in UC while rectal sparing in CD. Ø 4 -Histology: UC is superficial while CD affect all intestinal layers. Ø 5 -Pathology: UC there is Cryptitis & Crypt abscess While CD there is granuloma. Ø 6 -Presence of fistulae in CD > UC. Ø 7 -Presence of Perianal lesions in CD > UC. Ø 8 -Clinical presentation: bloody diarrhea in UC while in CD abdominal pain , wt. loss. Ø 9 -UC is more in non/ex-smoker while CD more in smokers. Ø 10 -Surgery is curative in UC & not in CD.

Complications of IBD v. Intestinal : § Severe colitis. § Perforation. § Hemorrhage. § Toxic megacolon. § Fistula. § Cancer of the colon.

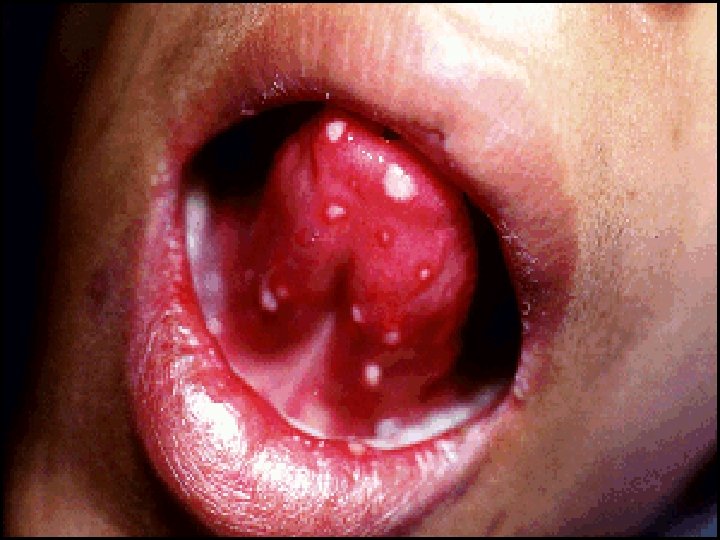
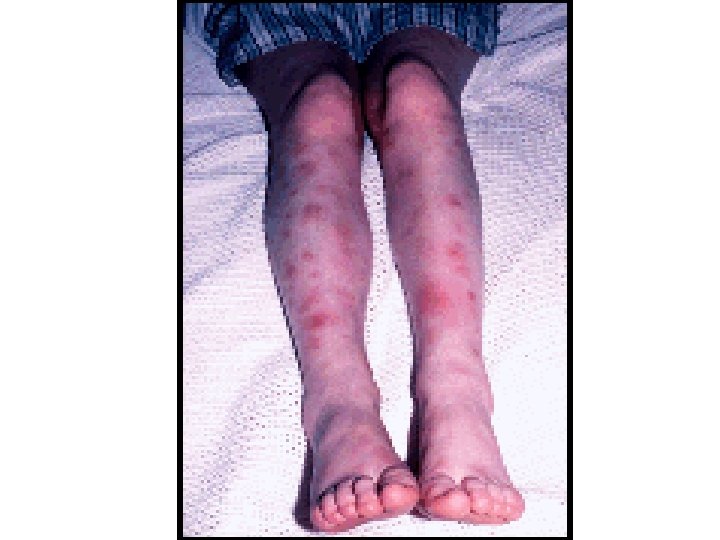
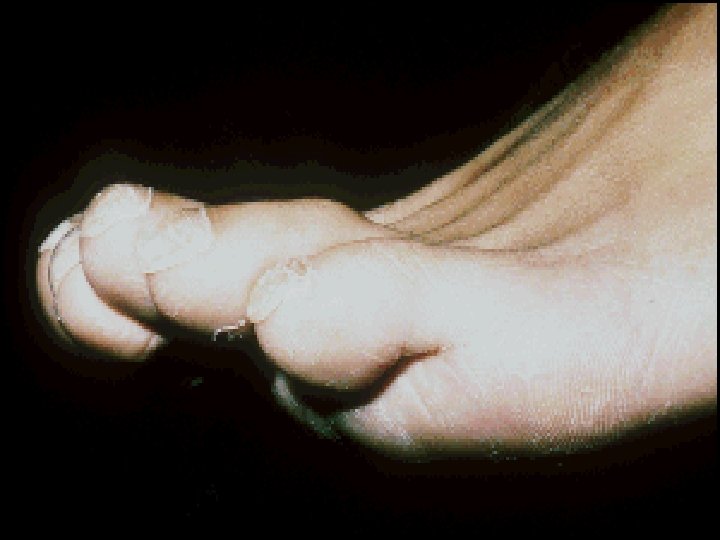
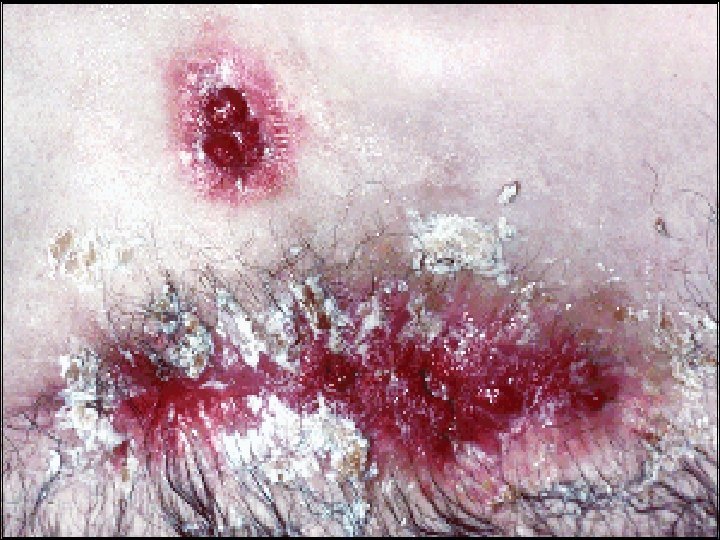
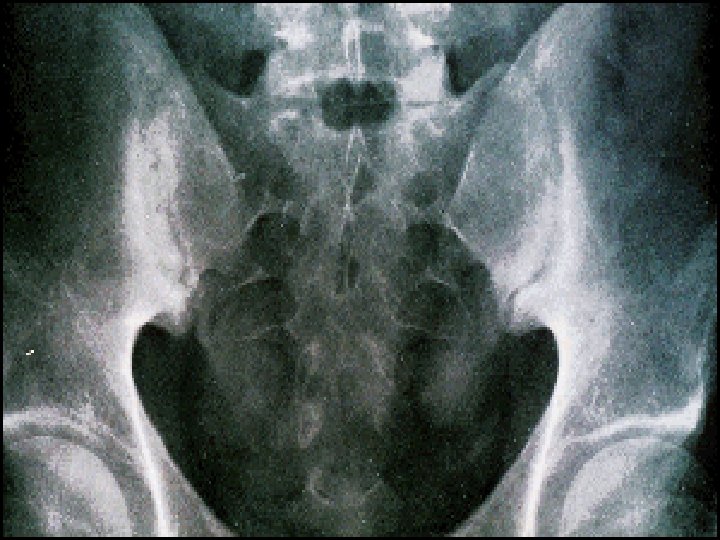
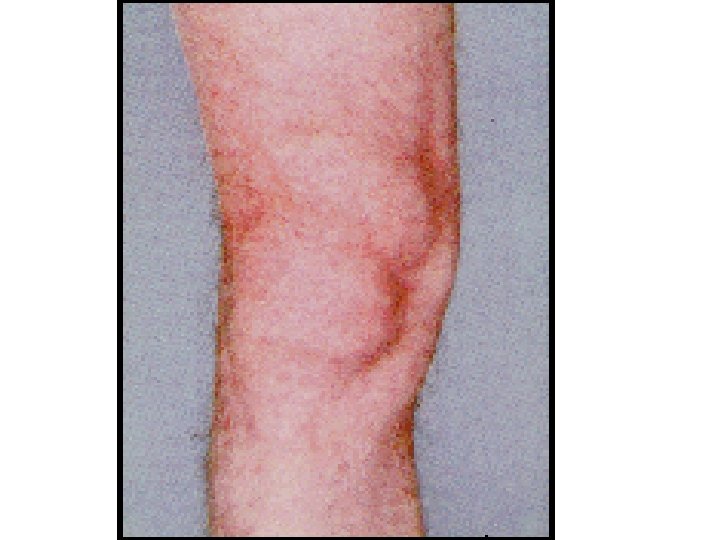
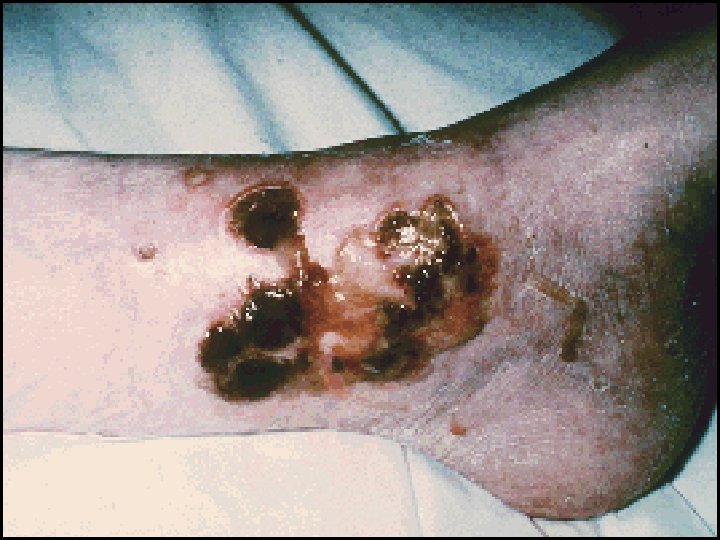
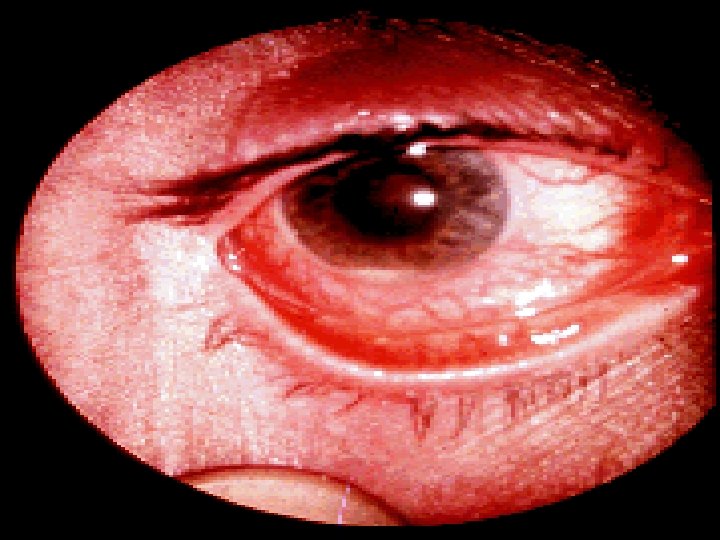
v. Extra intestinal: § Seronegative arthritis & Sacroilitis/Ankylosing spondylitis. § Ocular: *Conjunctivitis , *Iritis , *Episcleritis. § * Mouth ulcers. § Hepatic. *Fatty liver, Sclerosing cholangitis & cholangiocarcinoma, *Liver abscess & *portal pyemia § Renal. Amyloidosis & Oxalate calculi § Vascular. *DVT, *Mesenteric or *portal vein thrombosis § *Erythema nodosum, *Pyoderma gangrenosum. .

Differential diagnosis of IBD FD. D of UC & Crohn, s colitis: v. Infective: § Bacterial: Salmonella, Shegella , Campylobacter pylori , E. coli 0157, Pseudomembranous colitis, Chlamydia proctitis& Gonococcal proctitis. § Viral: Herpes simplex proctitis, Cytomegalovirus. § Protozoal: Amoebaiasis.

v. Non-Infective: § Ischemic colitis. § Collagenous colitis. § NSAIDs. § Colonic carcinoma. § Diverticulitis. § Radiation proctitis. § Behcets disease.

FD. D of small bowel CD: v. Other causes of right iliac fossa mass. Ø Caecal carcinoma Ø Appendicular mass Ø Infection ( TB , Yesinia , Actinomycosis ) v. Mesenteric adenitis. v. Pelvic inflammatory disease. v. Lymphoma.

Investigations of IBDs. z. Blood tests: HB, WBC , ESR, CRP, S. albumin. fecal calproctectin is useful for distinguishing IBD from IBS at diagnosis & for subsequent monitoring of disease activity. z. Bacteriology: Stool microscopy, culture, clostridium difficil toxin. Bl. Culture & serology.

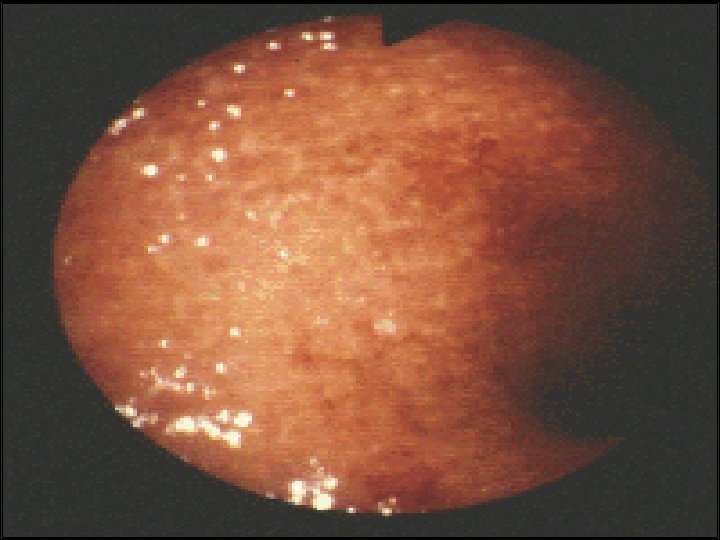
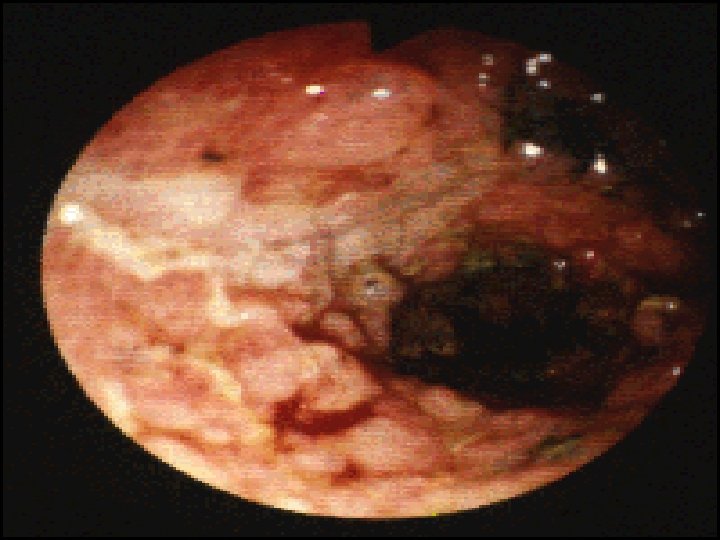
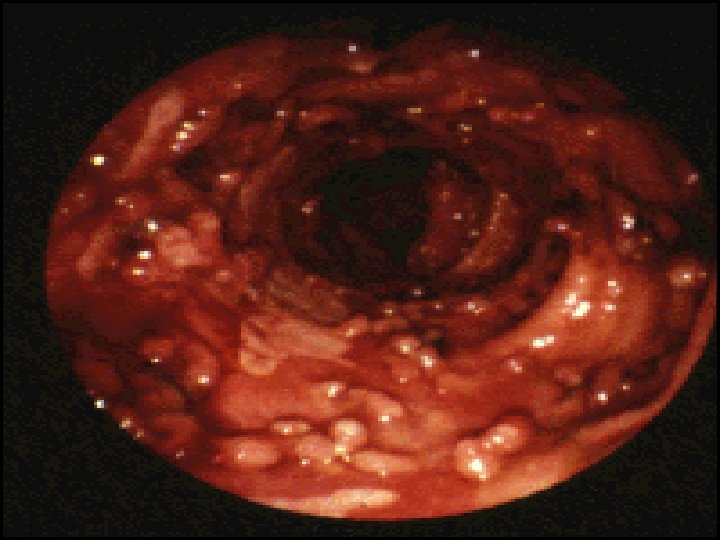
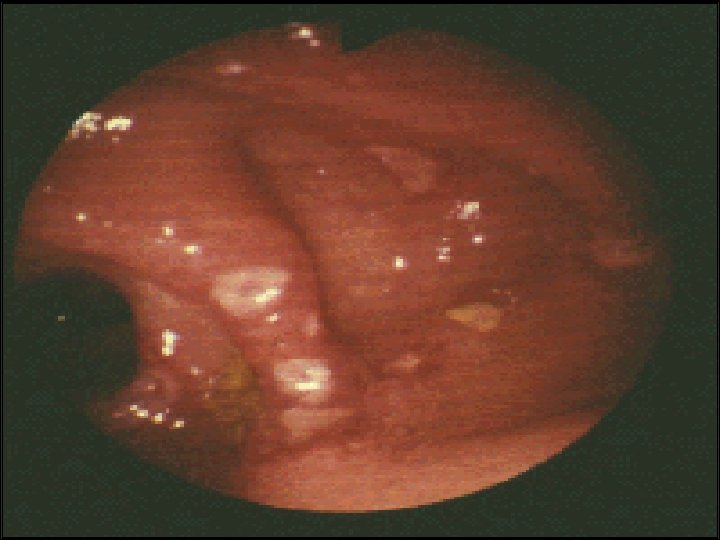
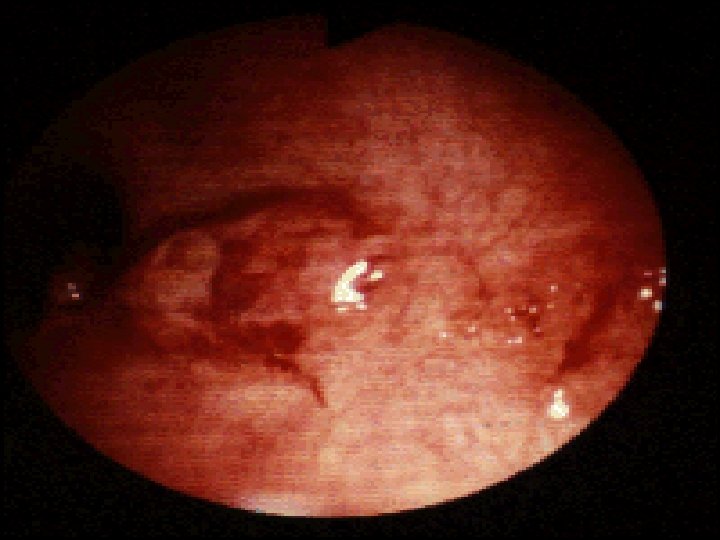
Endoscopy: Indications for endoscopy: o Disease extent. o Stricture ( biopsy ). o Filling defect. o Differentiation between UC & CD. o For follow up: Random biopsies for dysplasia or cancer for UC > 8 ys. In UC Ileocolonoscopy showed loss of vascular pattern, granularity, friability & contact bleeding with or without ulceration. In acute severe cases of UC sigmoidoscopy is done to confirm the diagnosis. In Crohns disease often there is rectal sparing , patchy inflammation , discrete deep ulcers, strictures& perianal disease

Pan colonic chromo-endoscopy : Stain the colonic mucosa by methylene blue or indigo carmine increase the chance to detect dysplasia. The procedure can classify patients into high medium & low risk groups. If high grade dysplasia found –pan proctocolectomy is recommended. In Crohns disease wireless capsule endoscopy is useful in identification of inflammation but should be avoided in presence of small intestinal stricture. Enteroscopy sometimes is required for histological diagnosis of small bowel Crohns.

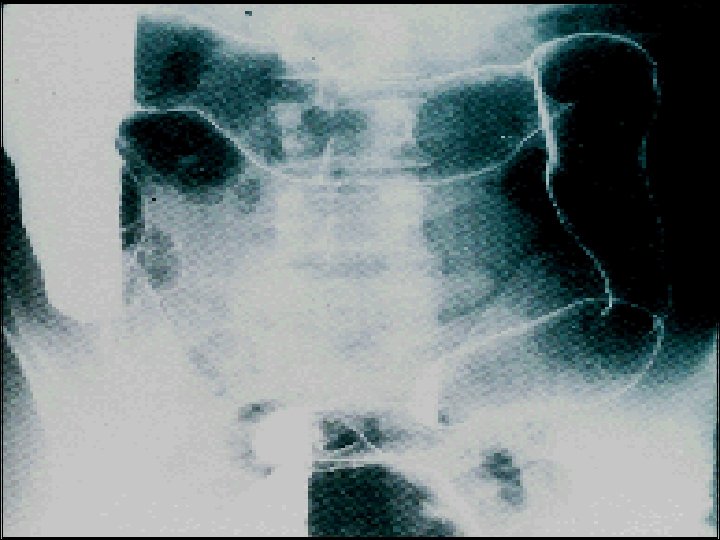
Radiology • Barium enema : is less sensitive than colonoscopy. • CT colonogram used when colonoscopy is not complete. • Barium follow through is used to visualize small bowel lesions as narrowed & ulcerated with multiple strictures. • MRI enterography: is sensitive way of detecting extraintistinal manifestations & assessing pelvic & perineal involvement. • Plain abdominal X-ray. • Ultrasound: is very powerful tool to detect small bowel inflammation & stricture formation. • CT is limited to screening for complications such as perforation or abscess formation in the acutely unwell.



Drugs used in treatment of IBDs Aminosalysilates: (( Mesalasine, Olsalazine , Balsalazide)) Modulate cytokine release from mucosa Delivered to the colon by: 1 -PH-dependent ( Asacol ) 2 -Time-dependent ( Pentasa ) 3 -Bacterial breakdown by colonic bacteria from carrier molecule ( Sulfasalazine, Olsalazine, Balsalized ).

Corticosteroid Prednisolon , Hydrocortisone , Budesonide. Anti-inflammatory ( topical, oral or I. V) Thiopurines: Azothiopurine , 6 -mercaptopurine Immunomodulation by inducing T-cell apoptosis. Is effective in 6 -8 ws after starting therapy.

Methotrexate • Anti-inflammatory • SE: Intolerance in 10 -18%, nausea , stomatitis, hepatotoxicity & pneumonitis.

Infliximab: Chimeric anti-TNF monoclonal AB. Given as I. V infusion 4 -8 weekly. Induce apoptosis of inflammatory cells Uses: Moderately-severely active CD especially fistulating. • Moderate to severe UC & Severe acute UC as rescue therapy. Ø Anaphylactic reaction after multiple infusions. Ø Contraindicated in presence of infection, reactivation of latent TB. Ø Increased risk of infection & possibly of malignancy. • •

Ciclosporine v. Suppression of T cell expansion. v. As rescue therapy to prevent surgery in UC responding poorly to corticosteroid. v. No value in CD. SE: -Nephrotoxicity. -Neurotoxicity. -Hirsutism.

Antibiotics Antibacterial. Useful in perianal CD. SE: Peripheral neuropathy in long term metronidazole. Antidiarrhoeal agents: ( Codeine phosphate , Loperamide , lomotil) Avoided in moderately or severe active UC may precipitate colonic dilatation.

Treatment of IBDs Treatment of Ulcerative Colitis: q. Treatment of acute attacks( Induction of remission ). q. Prevent relapses (Maintenance ). Sulfasalasine, Aminosalysilate. q. Detect carcinoma at early stage. q. Select patients for surgery.

• Active Proctitis: In mild to moderate disease: Mesalazine enema or suppositories combined with oral mesalazine. Topical corticosteroids are less effective& are used for patients who are intolerant of topical mesalazine. Patients who fail to respond are treated with prednisolone 40 mg daily.

Active left-sided or extensive ulcerative colitis: o In mildly active cases: High dose Aminosalysilate Topical aminosalicylat & Corticosteroid o Oral prednisolon 40 mg for more active disease & if no response to topical therapy. Sever UC: Admission& managed by physician, surgeon. 1 -Clinically: for presence of abd. Pain, Temp. , PR , stool bl. & frequency. 2 -Lab. : Hb% , WBC count , Alb. , Electrolytes , ESR & CRP. 3 -Radiologically: For colonic dilatation on plain abd.

Medical management of fulminant UC 1 -I. V fluid. 2 -Transfusion if Hb< 10 gm/L. 3 -I. V methylprednisolone ( 60 mg daily ) or Hydrocortisone. 4 -Antiboitic for proven infection. 5 -Nutritional support. 6 -Subcutanous heparin for prophylaxis of venous thromboembolism. 7 -Avoidance of Opiates & Antidiarrhoeal agents. 8 -I. V Ciclosporine ( 2 mg/kg) or Infliximab ( 5 mg/kg ) in stable patient not responding to steroid 3 -5 days

Indication for Urgent Colectomy Colonic dilatation >6 cm on plain abdominal X-Ray. Lab. & Clinical deterioration. No response after 7 -10 days.

Indications for Colectomy Impaired quality of life. -Loss of occupation or education. -Disruption of family life. Failure of medical therapy. -Dependence on corticosteroids. -Complications of drug therapy.

Indications for Colectomy Fulminant colitis. Disease complications unresponsive to medical therapy. -Arthritis. -Pyoderma Gangrenosum. Colon cancer or severe dysplasia.

Maintenance of remission in UC: -Life-long treatment for all patients with extensive disease & distal disease with more than once per year relapse. -Oral Aminosalysilate ( Mesalasine or Balsalazide ) or Salazopyrine ( for patients with arthropathy ). v If no response Thiopurine.

Medical treatment of CD Active Colitis or Iliocolitis: Like UC ( AS + Steroid ). Isolated Ileal: Corticosteroid( Budesonide) if no response surgery. Anti-TNF AB (Infliximab, Adalimumab) : v. I. V infusion 4 -8 weekly on 3 occasions induce remission in patients with CD at any site of GIT v. For refractory cases to steroid. v. Heals enterocutanous fistulae & maintains longer remissions.

v. Effective in the management of Pyoderma gangerosum & arthritis. v. It is contraindicated in presence of infection like TB. v. Relapse occur after 12 weeks so combine with Disease modifying drugs like methotrexate or thiopurine. v. It cause remarkable mucosal healing---- scaring & stricturing so used with caution in stenosing disease.

Extensive & diffuse iliocolonic: Drug therapy +Nutritional (Prolonged Parantral Nutrition )+Surgical Intervention +Endoscopic Balloon dilatation. Fistulating & Perianal disease: Ø -Metronidazole or Ciprofloxacin. Ø -Localize fistula by Ba. radiography , CT , MRI. Ø -Surgical treatment. Ø -Corticosteroid & nutritional therapy ( TPN ). Ø -Thiopurine for chronic disease. Ø -Infliximab infusion 4 -8 weekly.

Maintenance of remission in CD: 1 -Smoking cessation. 2 -Aminosalysilate have minimal efficacy. 3 -Patients with relapse more than once per year: Thiopurine. 4 -If patient intolerant to Thiopurine or 6 mercaptopurine then use once weekly methotrexate + Folic acid. 5 -More severe & aggressive disease: Combined immunomodulating agents + Infliximab.
- Slides: 63