Inflammatory Bowel Disease Definition Inflammatory bowel disease IBD

Inflammatory Bowel Disease

Definition Inflammatory bowel disease (IBD) is a term encompassing a number of chronic inflammatory disorders leading to damage of the gastrointestinal tract.

Crohns disease

Symptoms of CD The presentation depends on the site, extent, severity, and complications of intestinal and extraintestinal disease. n Fevers, night sweats, and weight loss. n Abdominal pain n Nausea and vomiting n Diarrhea n Rectal bleeding

Extraintestinal Manifestations of Inflammatory Bowel Disease n Musculoskeletal n n n n Peripheral arthritis Sacroiliitis Ankylosing spondylitis Osteoporosis Dermatologic n Erythema nodosum Pyoderma gangrenosum Aphthous stomatitis Hepatobiliary Disease n n Primary sclerosing cholangitis Ocular n n Vascular n n Uveitis Scleritis Episcleritis Thromboembolic events Renal n Nephrolithiasis

Physical Examination in CD n Weight loss and pallor. n Clubbing of the fingers. n Abdominal distension n Tenderness in the area of involvement n Abnormal bowel sounds. n Presence of an inflammatory mass are common. n Perianal abscess, fistula, skin tags, or anal stricture.

Laboratory Studies n Anemia n n n n n Deficiencies of iron, vitamin B 12, or folic acid Anemia of chronic disease. Leukocytosis Thrombocytosis Elevated ESR and C-reactive protein levels Decreased Serum albumin levels Urinalysis commonly demonstrates calcium oxalate crystals. Stoolanalysis for fecal leukocytes Serologic markers with high specificity for CD. n Anti-Saccharomyces cerevisiae antibody(ASCA) n Antibody to the outer core membrane of E. coli (Omp. C)

Imaging Studies n n Plain abdominal x- ray Barium studies n n n Small bowel enema (enteroclysis) / follow-through Large bowel enema U/S Abdomen and Pelvis / Transrectal U/S CT Abdomen and Pelvis MRI
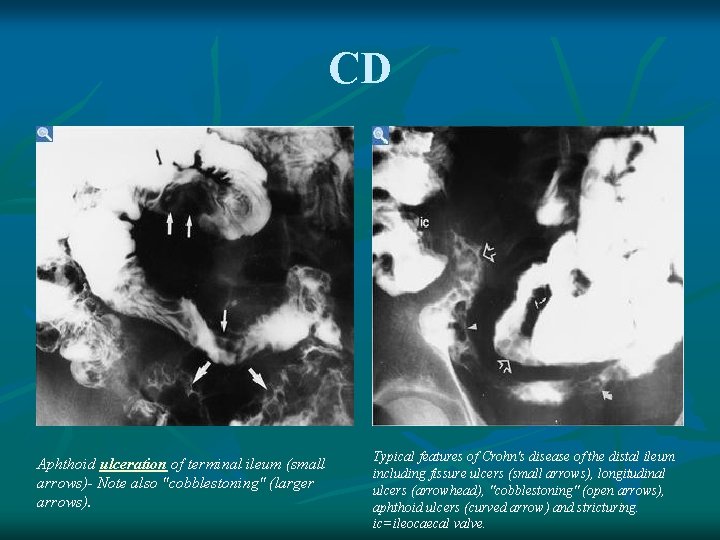
CD Aphthoid ulceration of terminal ileum (small arrows)- Note also "cobblestoning" (larger arrows). Typical features of Crohn's disease of the distal ileum including fissure ulcers (small arrows), longitudinal ulcers (arrowhead), "cobblestoning" (open arrows), aphthoid ulcers (curved arrow) and stricturing. ic=ileocaecal valve.

Endoscopy n n Upper and Lower Endoscopy Capsule Endoscopy
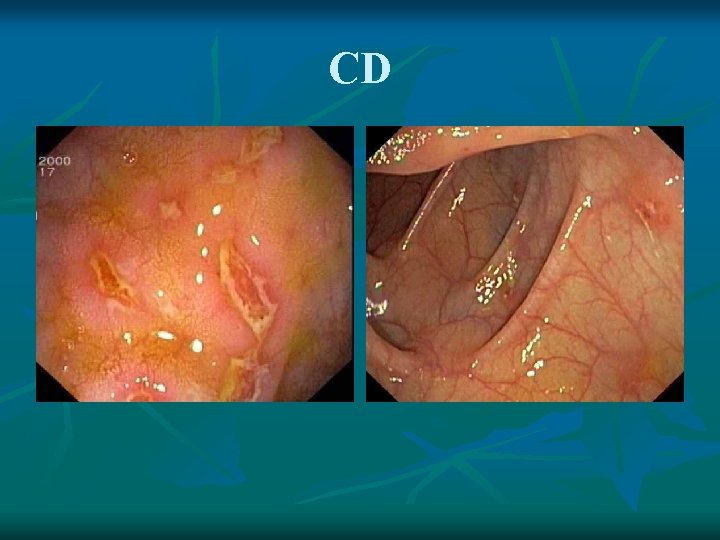
CD
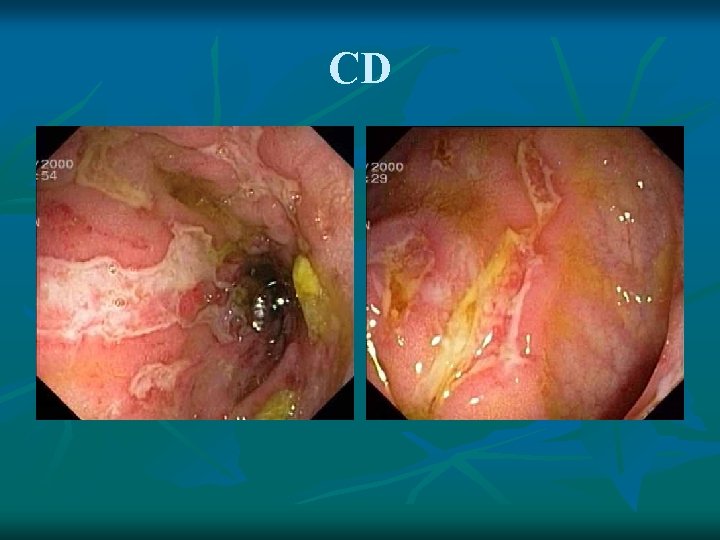
CD
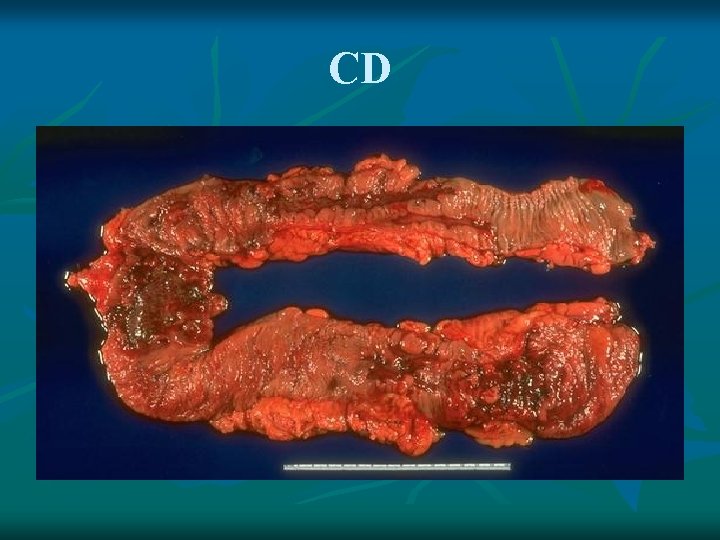
CD
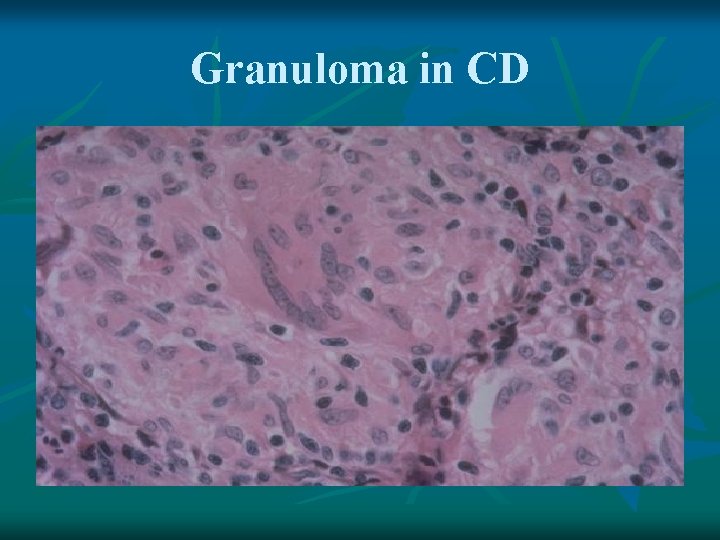
Granuloma in CD

ACG Practice Guidelines: Definitions of Disease Severity Mild – Moderate CD : n n n Ambulatory patients Patients who are able to tolerate oral alimentation Patients without manifestations of n Dehydration n Toxicity ( high fever, rigors, prostration ) n Abdominal tenderness n Painful mass n Obstruction n >10% weight loss Hanauer et al A J Gastroenterology

ACG Practice Guidelines: Definitions of Disease Severity (cont. ) Moderate-Severe CD: n n Patients who have failed to respond to treatment for mild-moderate disease Patients with more prominent symptom of: n Fever n Significant weight loss n Abdominal pain or tenderness n Intermittent nausea or vomiting (without obstructive findings) n Significant anemia Hanauer et al A J Gastroenterology

ACG Practice Guidelines: Definitions of Disease Severity (cont. ) Sever –Fulminant CD: n n Patients with persistent symptoms despite the introduction of steroids as out patient Individuals presenting with: n High fever n Persistent vomiting n Evidence of intestinal obstruction n Rebound tenterness n Cachexia, or n Evidence of abscess Hanauer et al A J Gastroenterology

ACG Practice Guidelines: Definitions of Disease activity CD in remission: n n Patients who are asymptomatic or without inflammatory sequelae Patients who have responded to acute medical intervention or have udergone surgical resection without gross evidence of residual disease NB: Patients requiring steroids to maintain well-being are considered to be “steroid-dependen”and are usually not cosidered to be “in remission. ” Hanauer et al A J Gastroenterology 2001, 96, 635
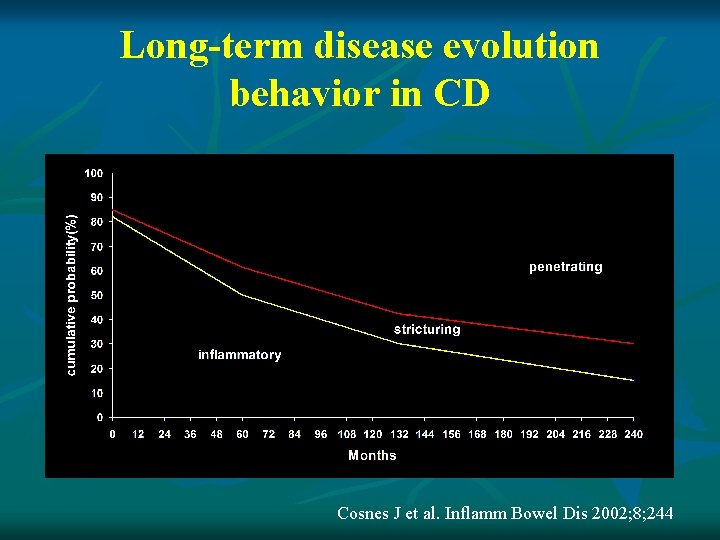
Long-term disease evolution behavior in CD Cosnes J et al. Inflamm Bowel Dis 2002; 8; 244

Medical treatment of IBD Yousef A. Qari MD, FRCPC, ABIM Consultant Gastroenterologist King Abdulaziz University Hospital Jeddah, Saudi Arabia

Current Expectations for IBD Therapy n n n Induce clinical remission Maintain clinical remission Improve quality of life Plus Heal mucosa Decrease hospitalization / surgery / overall costs Minimize disease- related and therapy-related complications

ACG Practice Guidelines: Recommended treatment Mild – Moderate CD : n Aminosalicylates n n n Sulphasalazine (3 -6 g/d) Mesalamine (3. 2 -4. 0 g/d) 40 -50% Antibiotics (CD involving colon) n n Remission Metronidasole (10 -20 mg/kg) 50% Ciprofloxacin (1 g/d) Metro+Cipro (250 mg 2 -3 times/d +500 mg 2 times/d) 76% Budesonide (CIR) (9 mg/d) n For ileal & Rt colonic disease 69%

ACG Practice Guidelines: Recommended treatment Moderate –Severe CD n n n Corticosteroids Appropriate antibiotics therapy or drainage (surgical/percutaneous) required for infection or abscess Inflximab infusion n n Effective adjunct Possible alternative to steroid therapy in selected patients in whom corticosteroids are contraindicated or ineffective.
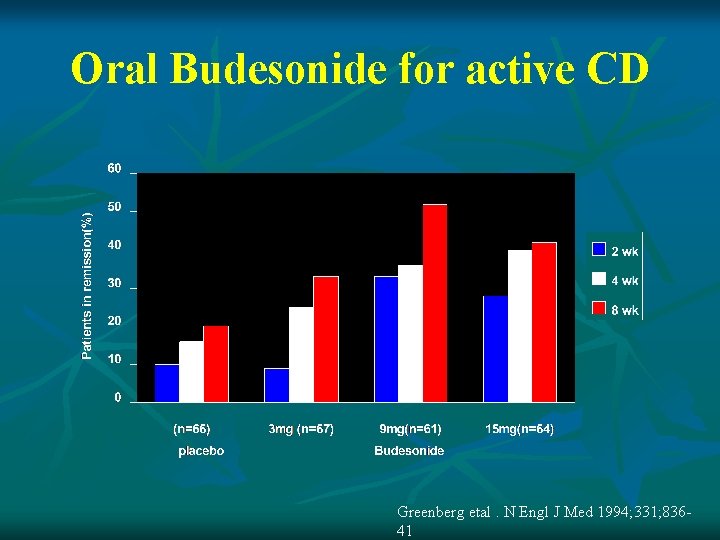
Oral Budesonide for active CD Greenberg etal. N Engl J Med 1994; 331; 83641

ACG Practice Guidelines: Recommended treatment Moderate –Severe CD: Corticosteroids Budesonide 9 mg/d or Prednisone (0. 5 -0. 75 mg/kg) or 40 mg/d n n 5 o-70% remission rate in 8 -12 weeks Until resolution of symptoms and resumption of weight gain, generally 7 -28 days. Steroid refractory & steroid dependent ≈ 50% n Smooking n Colonic disease Not effective for maintenance
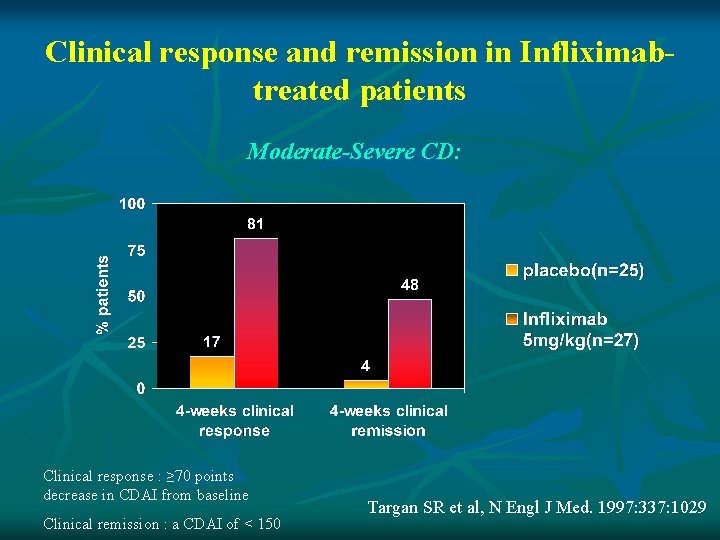
Clinical response and remission in Infliximabtreated patients Moderate-Severe CD: Clinical response : ≥ 70 points decrease in CDAI from baseline Clinical remission : a CDAI of < 150 Targan SR et al, N Engl J Med. 1997: 337: 1029

Clinical Response at Week 52* P<0. 001 P=NS P<0. 001 *Week-2 Responders
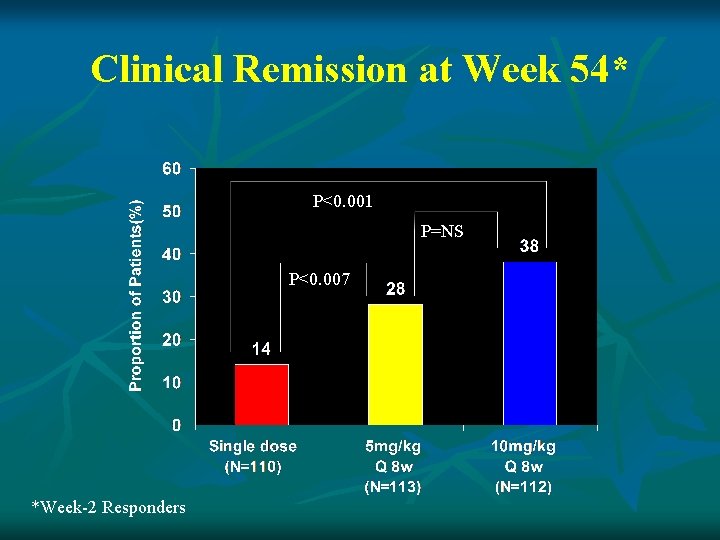
Clinical Remission at Week 54* P<0. 001 P=NS P<0. 007 *Week-2 Responders

ACG Practice Guidelines: Recommended treatment Severe-Fulminant CD: Hospitalization required for : n n patients with persistent symptoms despite introduction of oral steroids or infliximab Patients presenting with high fever, frequent vomiting, evidence of intestinal obstruction, rebound tenderness, cachexia, or an abscess Surgical consultation is warranted for patients with obstruction or tender abdominal mass. Hanaur S et al. Am J Gastroenterology; 96; 635

ACG Practice Guidelines: Recommended treatment Severe-Fulminant CD: n Exclude abscess n n n Abd US Abd CT Percutaneous Drainage Surgical Parentral corticosteroids equivalent to 40 -60 mg prednisone n n If abscess has been excluded If the patient has been receiving oral setroids

ACG Practice Guidelines: Recommended treatment n Severe-Fulminant CD: Parentral broad spectrum antibiotics n n High fever Toxic appearance Inflammatory mass Nutritional support: (Elemental or TPN) n n TPN in addition to steroids plays no specific role Indications n n n For patients unable to maintain nutritional requirments after 5 -7 days Preoperative management Pediatric age groups

Therapeutic Options for Perianal Fistulas in CD Possible efficacy n n n Proven efficacy Antibiotics n Infliximab AZT/6 -MP Cyclosporine
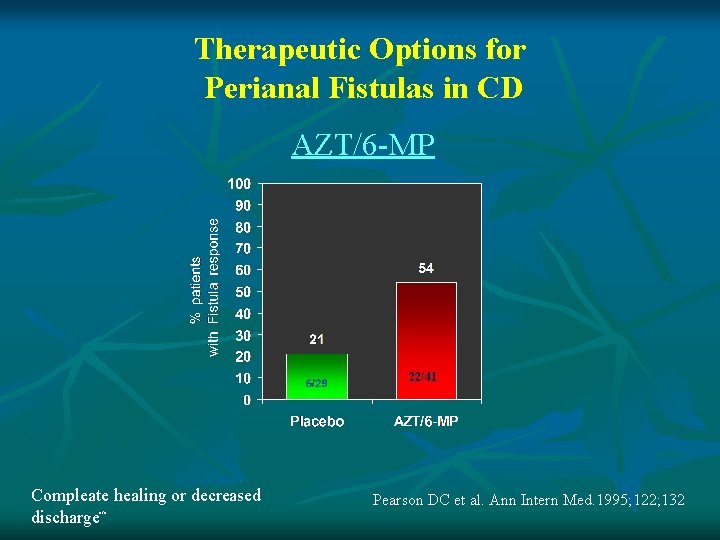
Therapeutic Options for Perianal Fistulas in CD AZT/6 -MP 22/41 Compleate healing or decreased discharge΅ Pearson DC et al. Ann Intern Med. 1995; 122; 132
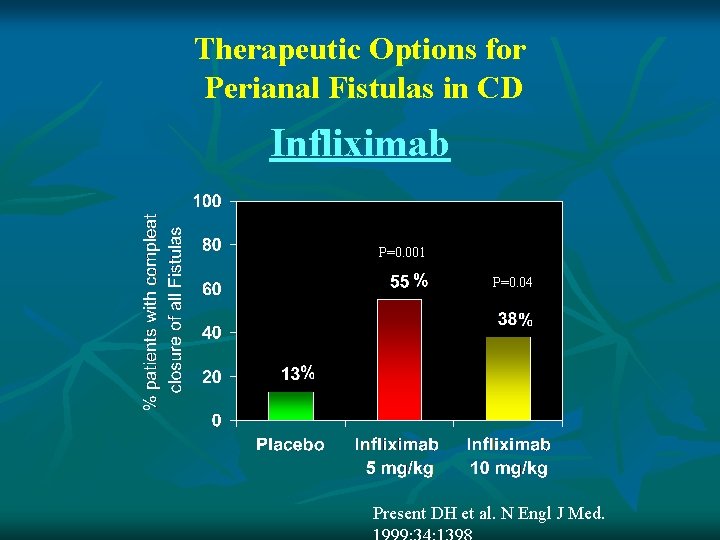
Therapeutic Options for Perianal Fistulas in CD Infliximab P=0. 001 P=0. 04 Present DH et al. N Engl J Med.
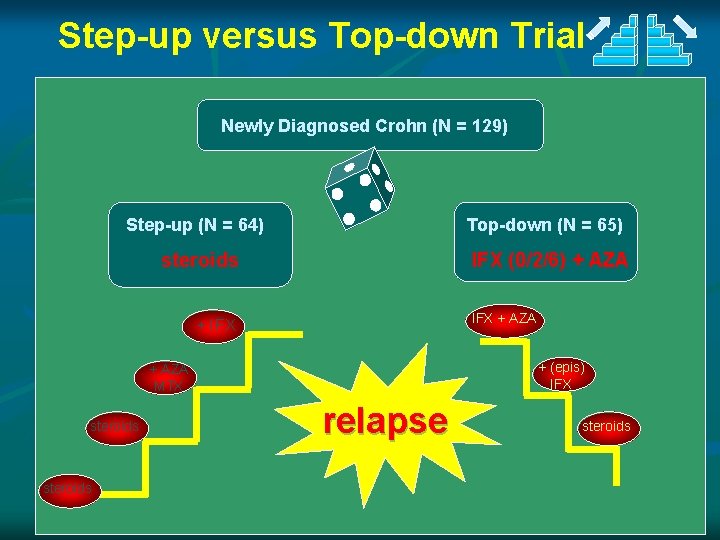
Step-up versus Top-down Trial Newly Diagnosed Crohn (N = 129) Step-up (N = 64) Top-down (N = 65) steroids IFX (0/2/6) + AZA IFX + AZA + IFX + (epis) IFX + AZA MTX steroids relapse steroids


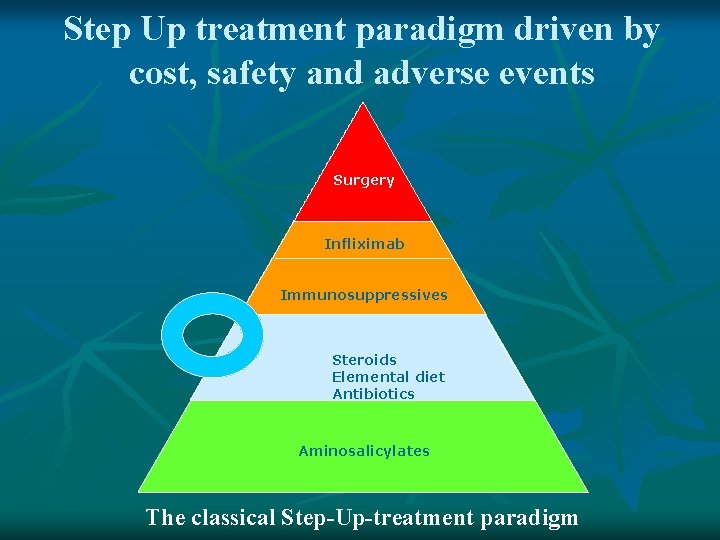
Step Up treatment paradigm driven by cost, safety and adverse events Surgery Infliximab Immunosuppressives Steroids Elemental diet Antibiotics Aminosalicylates The classical Step-Up-treatment paradigm
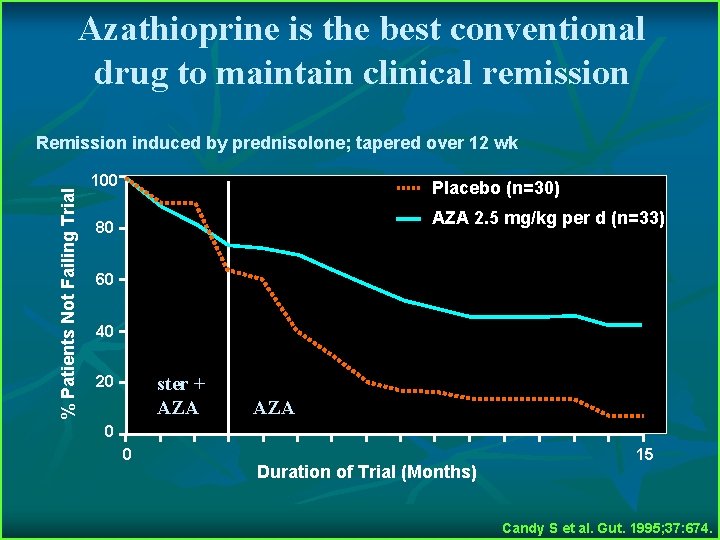
Azathioprine is the best conventional drug to maintain clinical remission % Patients Not Failing Trial Remission induced by prednisolone; tapered over 12 wk 100 Placebo (n=30) AZA 2. 5 mg/kg per d (n=33) 80 60 40 ster + AZA 20 AZA 0 0 Duration of Trial (Months) 15 Candy S et al. Gut. 1995; 37: 674.
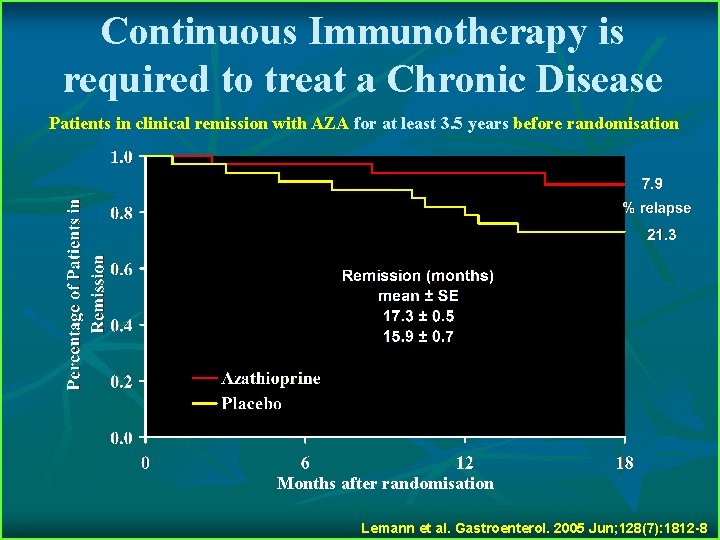
Continuous Immunotherapy is required to treat a Chronic Disease Patients in clinical remission with AZA for at least 3. 5 years before randomisation Months after randomisation Lemann et al. Gastroenterol. 2005 Jun; 128(7): 1812 -8.
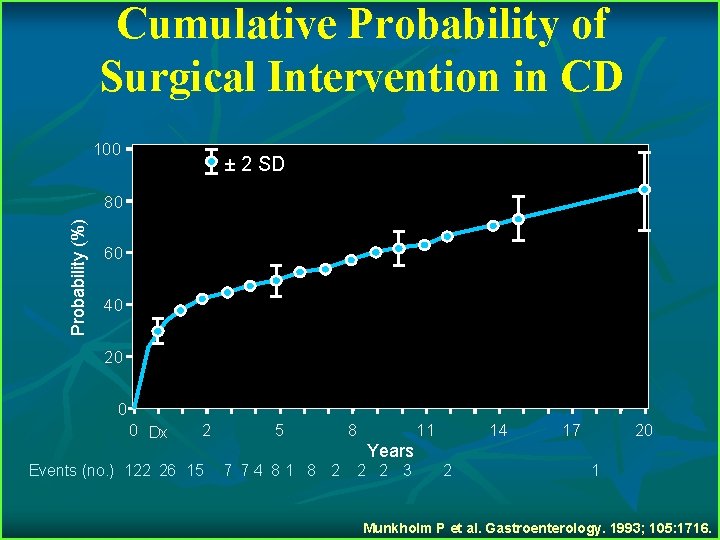
Cumulative Probability of Surgical Intervention in CD 100 ± 2 SD Probability (%) 80 60 40 20 0 0 Dx 2 Events (no. ) 122 26 15 5 8 11 14 17 20 Years 7 74 81 8 2 2 2 3 2 1 Munkholm P et al. Gastroenterology. 1993; 105: 1716.

Ulcerative colitis

Difinition A chronic disease charecterized by diffuse mucosal inflammation limited to the colon.

Age distribution of Ulcerative colitis in east and west provinces of Saudi arabia 188 CASES Age(y) at presentation 1. Qari Y et al, under publication 2. Satti M et al, Ann Saudi Med 1996; 16(6): 637 -640.
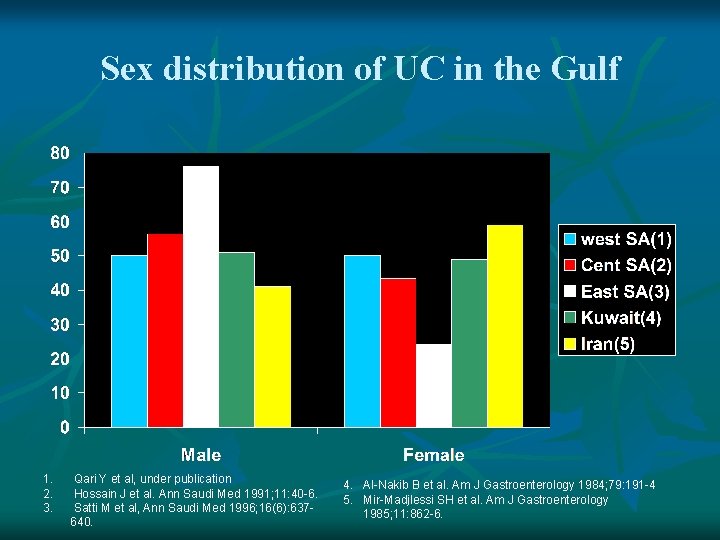
Sex distribution of UC in the Gulf 1. 2. 3. Qari Y et al, under publication Hossain J et al. Ann Saudi Med 1991; 11: 40 -6. Satti M et al, Ann Saudi Med 1996; 16(6): 637640. 4. Al-Nakib B et al. Am J Gastroenterology 1984; 79: 191 -4 5. Mir-Madjlessi SH et al. Am J Gastroenterology 1985; 11: 862 -6.

Pattern of UC in the Gulf 1. Qari Y et al, under publication 2. Hossain J et al. Ann Saudi Med 1991; 11: 40 -6. 3. Satti M et al, Ann Saudi Med 1996; 16(6): 637 -640. . 4. Al-Nakib B et al. Am J Gastroenterology 1984; 79: 191 -4 5. Mir-Madjlessi SH et al. Am J Gastroenterology 1985; 11: 862 -6.

Epidemiological figures comparing East vs West Geographic location Gulf Region Saudi Arabia West Europe and USA Incidence 0. 5 – 2. 8 / 100 000 6 -8 / 100 000 Prevalence ≈ 5 / 100 000 70 -150 /100 000
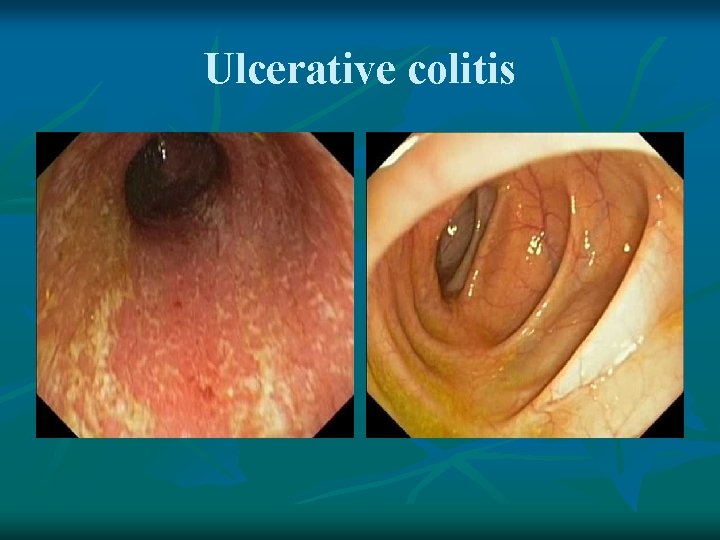
Ulcerative colitis
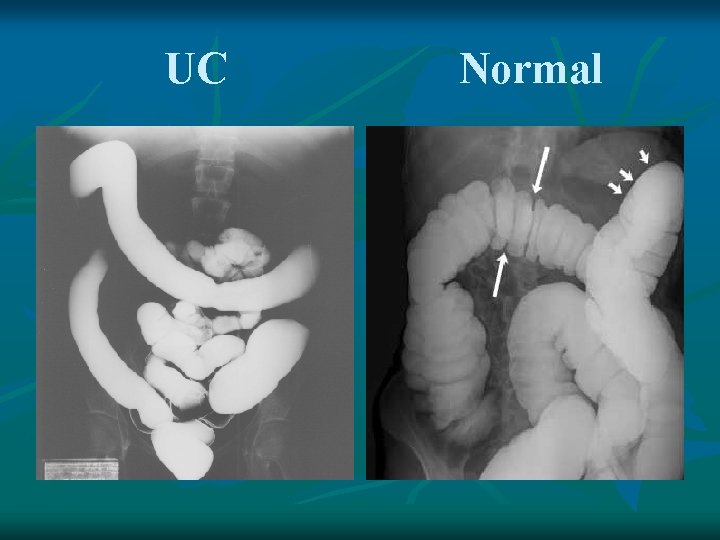
UC Normal
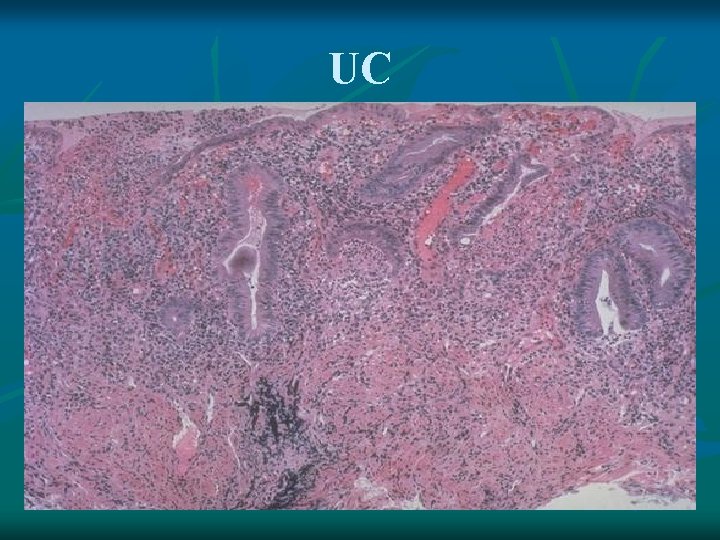
UC
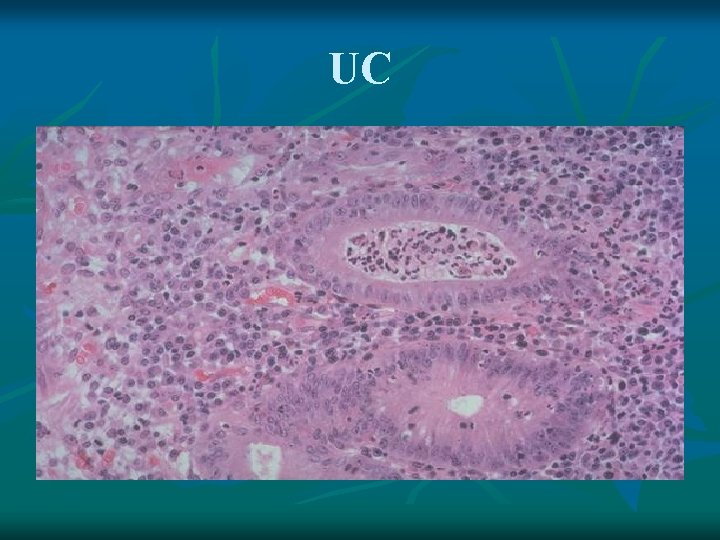
UC

The goals for the management of acute ulcerative colitis n n n Induction of remission Prevention of relapse Treatment of complications

of ? ? nt te ase Ex se Di Di Ac se tiv ase ity ? ? Therapeutic decisions

Disease Activity n n Mild Moderate Severe Fulminant
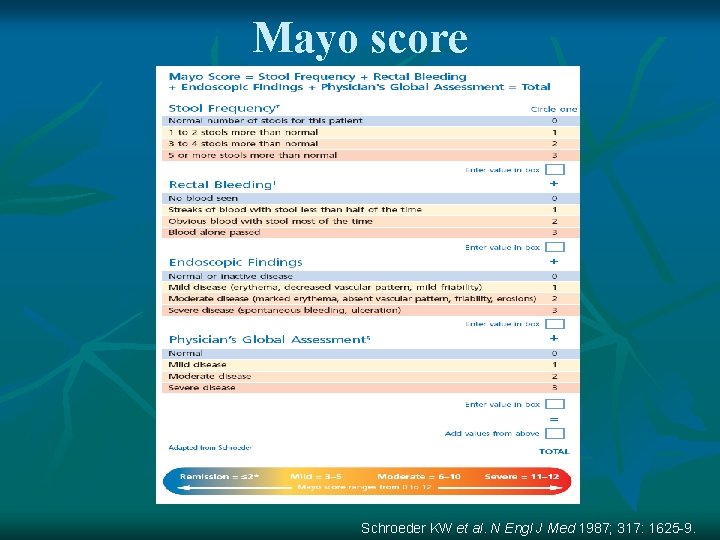
Mayo score Schroeder KW et al. N Engl J Med 1987; 317: 1625 -9.
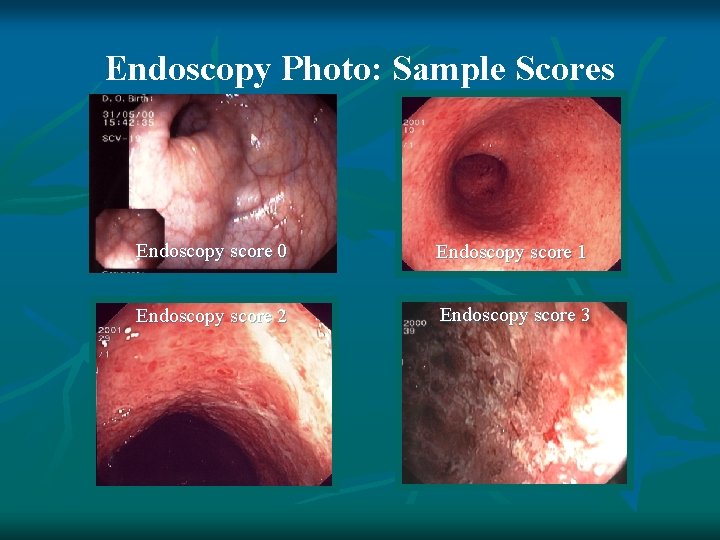
Endoscopy Photo: Sample Scores Endoscopy score 0 Endoscopy score 1 Endoscopy score 2 Endoscopy score 3
Severe colitis A bloody stool frequency of > 6/day with any one of the following: n n Tachycardia (pulse > 90 beats/min) Temperature (> 37. 8 °C) Anaemia (Hg < 10. 5 g/d. L) Raised ESR (> 30 mm/h)
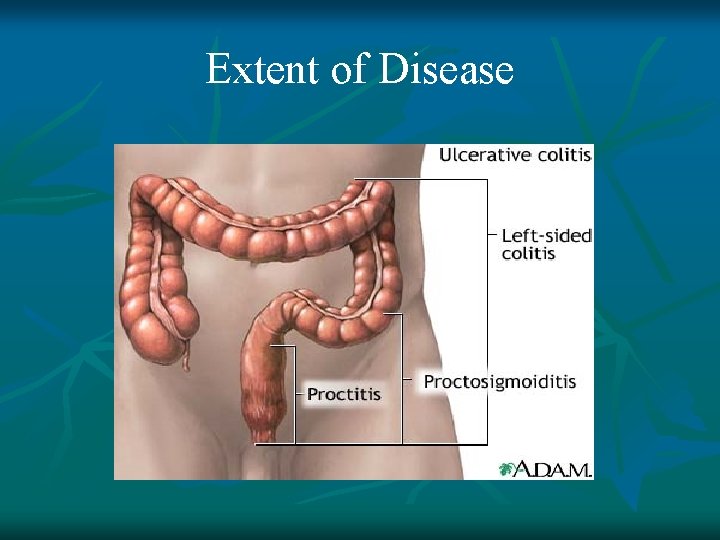
Extent of Disease
Activity Extent Medical Therapy
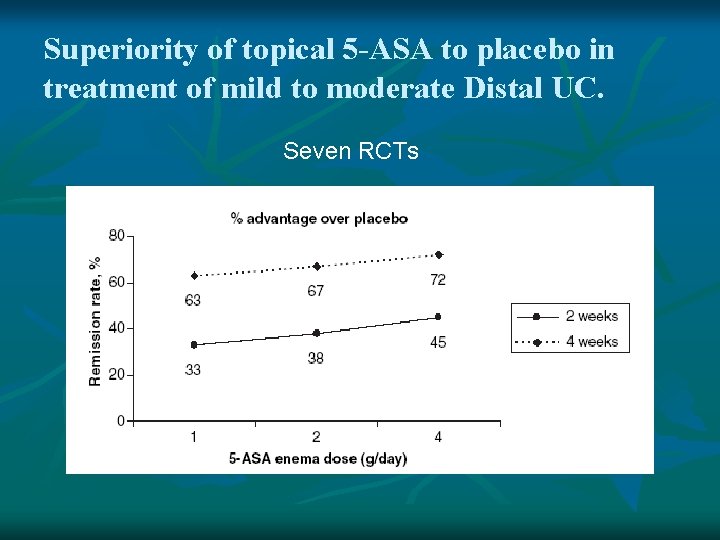
Superiority of topical 5 -ASA to placebo in treatment of mild to moderate Distal UC. Seven RCTs
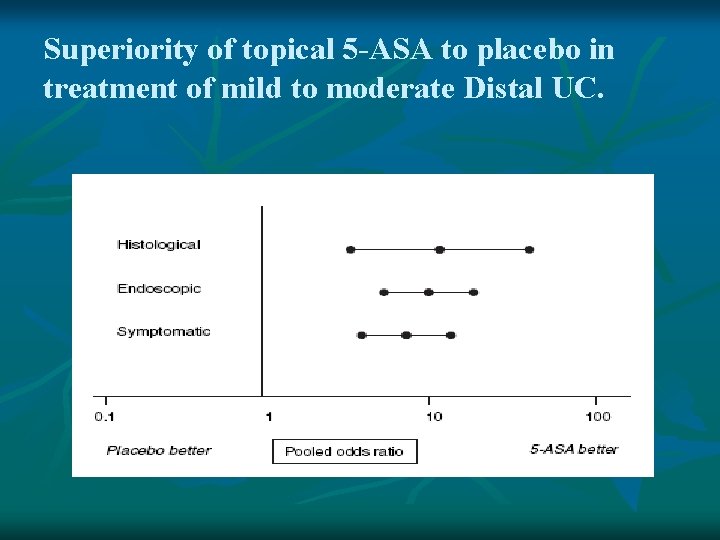
Superiority of topical 5 -ASA to placebo in treatment of mild to moderate Distal UC.
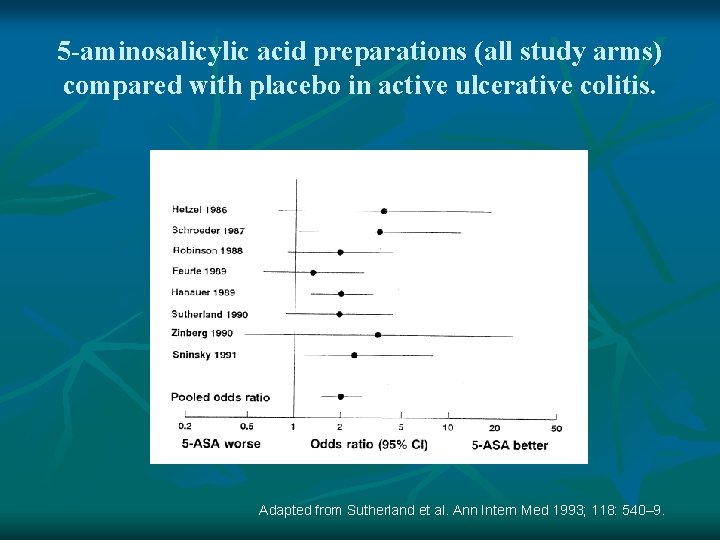
5 -aminosalicylic acid preparations (all study arms) compared with placebo in active ulcerative colitis. Adapted from Sutherland et al. Ann Intern Med 1993; 118: 540– 9.
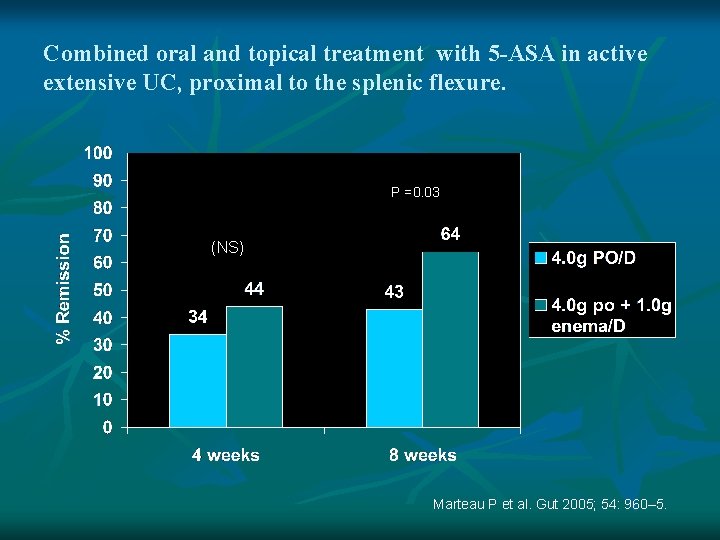
Combined oral and topical treatment with 5 -ASA in active extensive UC, proximal to the splenic flexure. P =0. 03 (NS) Marteau P et al. Gut 2005; 54: 960– 5.

Topical 5 -ASA have superior efficacy to oral mesalazine in the maintenance of remission in Distal Colitis Mantzaris GJ et al. Dis Colon Rectum 1994; 37: 58– 62 .
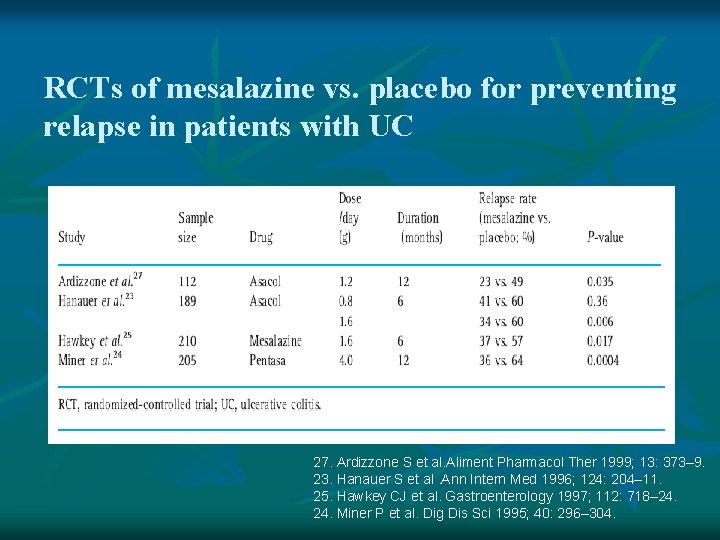
RCTs of mesalazine vs. placebo for preventing relapse in patients with UC 27. Ardizzone S et al. Aliment Pharmacol Ther 1999; 13: 373– 9. 23. Hanauer S et al. Ann Intern Med 1996; 124: 204– 11. 25. Hawkey CJ et al. Gastroenterology 1997; 112: 718– 24. Miner P et al. Dig Dis Sci 1995; 40: 296– 304.

Compliance is a problem

Patient Non-compliance with 5 -ASA Treatment Regimens Kane SV et al. Am J Gastroenterol 2001; 96: 2929 -33.
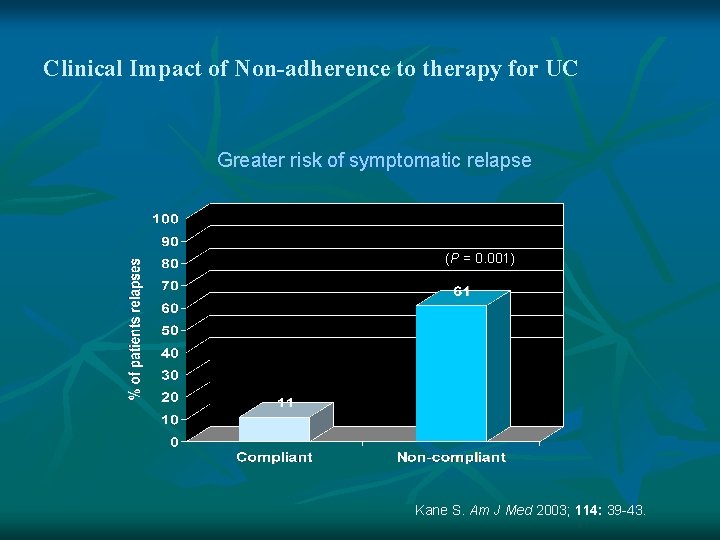
Clinical Impact of Non-adherence to therapy for UC Greater risk of symptomatic relapse (P = 0. 001) Kane S. Am J Med 2003; 114: 39 -43.
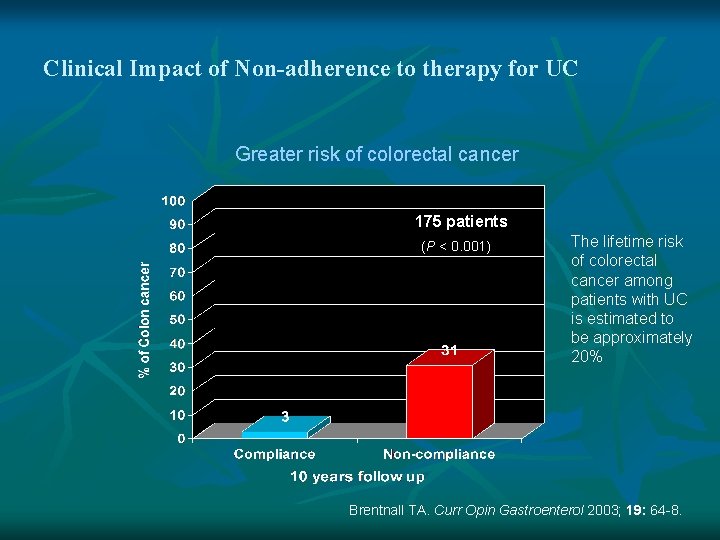
Clinical Impact of Non-adherence to therapy for UC Greater risk of colorectal cancer 175 patients (P < 0. 001) The lifetime risk of colorectal cancer among patients with UC is estimated to be approximately 20% Brentnall TA. Curr Opin Gastroenterol 2003; 19: 64 -8.

Mesalazine 2 g gel enema is as effective as and more convenient than mesalazine 2 g foam enema P<0. 005 P<0. 05 103 patients 4 weeks P<0. 05 Remission rates were comparable between the two groups. Gionchetti P. Aliment Pharmacol Ther 1999; 13: 381 -8.
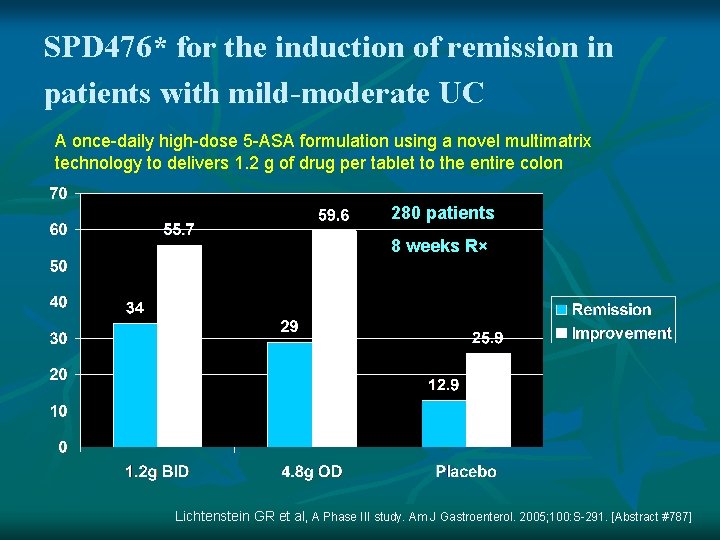
SPD 476* for the induction of remission in patients with mild-moderate UC A once-daily high-dose 5 -ASA formulation using a novel multimatrix technology to delivers 1. 2 g of drug per tablet to the entire colon 280 patients 8 weeks R× Lichtenstein GR et al, A Phase III study. Am J Gastroenterol. 2005; 100: S-291. [Abstract #787]
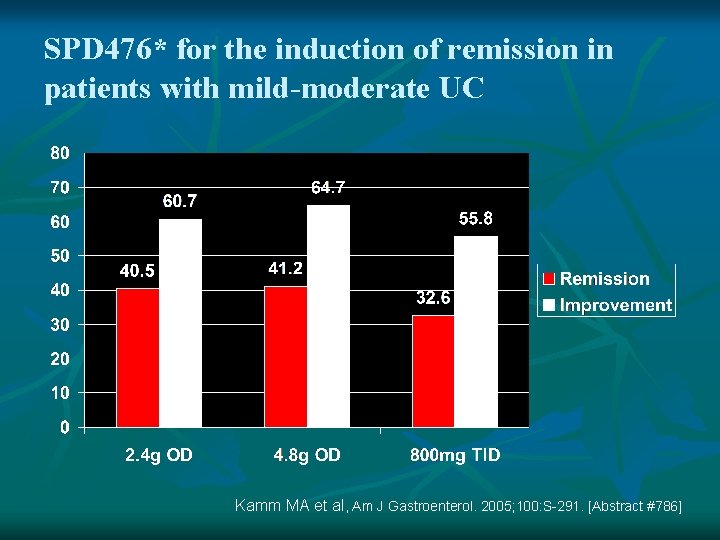
SPD 476* for the induction of remission in patients with mild-moderate UC Kamm MA et al, Am J Gastroenterol. 2005; 100: S-291. [Abstract #786]
- Slides: 72