Inflammation Dr Ahmad Hameed MBBS DCP M Phil

Inflammation Dr. Ahmad Hameed MBBS, DCP, M. Phil

Chemical Mediators and regulators of inflammation l Chemical mediators that are responsible for vascular and cellular events of inflammation. l Mediators may be produced locally by cells at inflammation, or may be derived from circulating precursors (typically synthesized by the liver) that are released at the site of inflammation. l Cell-derived mediators are § l l . Sequestered intracellular granules or synthesized de novo Plasma derived mediators are inactive which undergo proteolytic cleavage to acquire biologic activity.

Chemical Mediators and regulators of inflammation l Most mediators act by binding to specific receptors on different target cells. l l l Diverse action Direct action The actions of most mediators are tightly regulated and short lived l l Quickly decay Inactivated by enzymes Eliminated inhibited
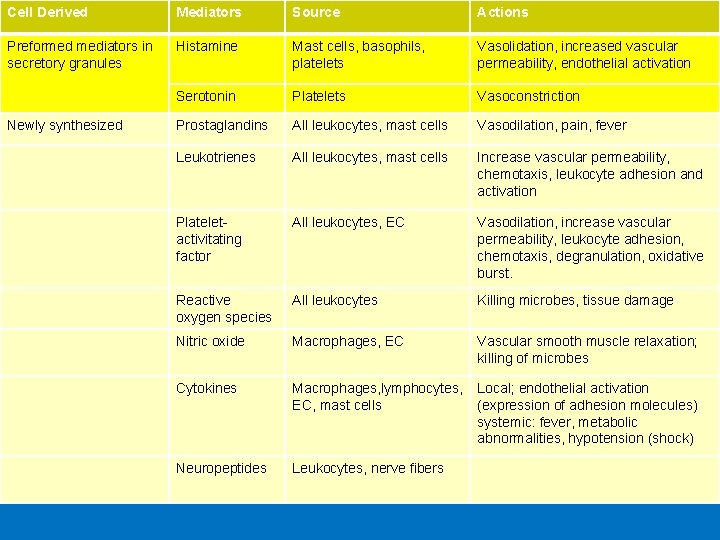
Cell Derived Mediators Source Actions Preformed mediators in secretory granules Histamine Mast cells, basophils, platelets Vasolidation, increased vascular permeability, endothelial activation Serotonin Platelets Vasoconstriction Prostaglandins All leukocytes, mast cells Vasodilation, pain, fever Leukotrienes All leukocytes, mast cells Increase vascular permeability, chemotaxis, leukocyte adhesion and activation Plateletactivitating factor All leukocytes, EC Vasodilation, increase vascular permeability, leukocyte adhesion, chemotaxis, degranulation, oxidative burst. Reactive oxygen species All leukocytes Killing microbes, tissue damage Nitric oxide Macrophages, EC Vascular smooth muscle relaxation; killing of microbes Cytokines Macrophages, lymphocytes, EC, mast cells Local; endothelial activation (expression of adhesion molecules) systemic: fever, metabolic abnormalities, hypotension (shock) Neuropeptides Leukocytes, nerve fibers Newly synthesized
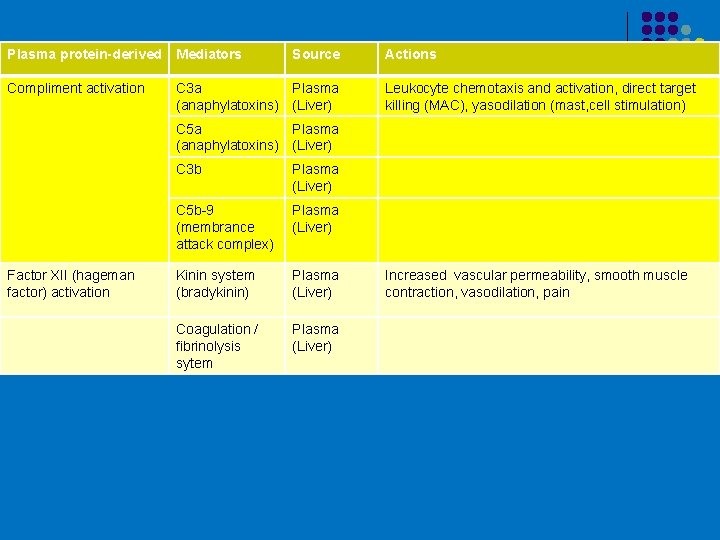
Plasma protein-derived Mediators Source Compliment activation C 3 a Plasma (anaphylatoxins) (Liver) Actions Leukocyte chemotaxis and activation, direct target killing (MAC), yasodilation (mast, cell stimulation) C 5 a Plasma (anaphylatoxins) (Liver) Factor XII (hageman factor) activation C 3 b Plasma (Liver) C 5 b-9 (membrance attack complex) Plasma (Liver) Kinin system (bradykinin) Plasma (Liver) Coagulation / fibrinolysis sytem Plasma (Liver) Increased vascular permeability, smooth muscle contraction, vasodilation, pain

Cell-Derived Mediators Tissue macrophages, mast cells, and endothelial cells, leukocytes Vasoactive Amines HISTAMINE Richest source l Mast cells ( C. T , B. V) l Basophils l Platelets Release in response to 1. Physical injury (trauma, cold, heat) 2. Immune reactions (Antibody to mast cells) 3. Anaphylatoxins (C 3 a & C 5 a) l

Histamine Releasing protein (H. R. P) from leucocytes 2. Neuropeptides (Substance P ) 3. Cytokines ( IL-1, IL-8) Action l Immediate transient response (main) l Dilatation of arterioles l Increase permeability of venules l Contricts large arteries l Acts on microcirculation / bind to H 1 receptors on endothelial cells 1.

SEROTONIN l l l 5 HT Similar action Present in platelets, entero chromaffin cells & neurons Neurotrasmitter and regulate intestinal motility When platelet aggregation occurs release serotonin Mast cells PAF platelet aggregation
Archidonic Acid Metabolites: Prostaglandins, Leukotrienes and Lipoxins Microbial Products + Mediators of Inflammation ↓ Arachidonic Acid Prostaglandins Leukotrienes

AA Metabolites l Cyclooxygenase pathway l l PGs are Produced by mast cells, macrophages, endothelium and others PGE 2, PGD 2, PGF 2α § Vasodilation § Potentiates Edema formation § Involved in pathogenesis of pain and fever PGI 2 § Produced by prostacyclin synthase in endothelial cell § Vasodilation, Inhibits Platelet aggregation TXA 2 § Produced by Thromboxane synthase in platelets § Vasoconstriction & stimulates platelets aggregation, unstable and converts to TXB 2
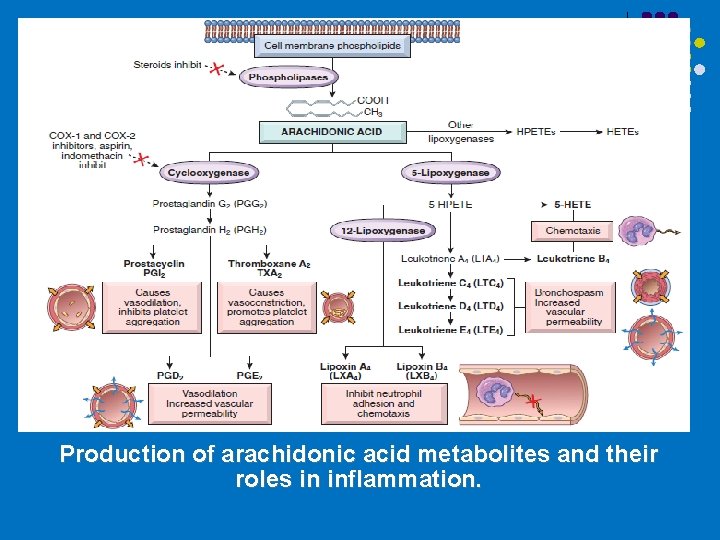
Production of arachidonic acid metabolites and their roles in inflammation.

Lipoxygenase Pathway l l LTs are secreted mainly by leukocytes and chemoattractants for leukocytes. LTA 4 LTB 4 § Produced by neutrophils & some macrophages § Chemotactic agent for neutrophils LTC 4 LTD 4 & LTE 4 § Produced by mast cells § Vasocontriction + bronchospasm + Intravascular Permeability

Anti-inflammatory Drugs that Block Prostagladin Production l l NSAID l Inhibit cyclooxygenase l Prevent biosynthesis of all PG l Treat pain and fever Cyclooxygenase inhibitor l Two isoforms - COX-1/COX-2 l COX-1 l l Expressed on most tissues produced in response to inflammation stimulate prostaglandins COX-2 l l l Absent most tissues Developed that they will not affect protective function of prostaglandins Increased risk of cerebrovascular and cardiovascular events

Lipoxygenase Pathway l Lipoxins (Anti inflammatory mediators ) § Endogenous antagonists of Leukotrienes ie inhibit neutrophil chemotaxis and adhesion to endothelium § Platelet adherent to neutrophils from LXA 4 and LXB 4

l Cortisol l Reduces vascular permeability and edema l Decreases prostglandin production by preventing release of AA by inhibiting phospholipase A 2

Platelet-Activating Factor l l l It is generated from a lipid complex stored in cell membranes; Produced by WBCs & endothelial cells induces platelet aggregation; Causes Vasoconstriction, Bronchoconstriction It activates neutrophils and is a potent eosinophil chemoattractant; It contributes to extravascularization of plasma proteins and so, to edema.
- Slides: 16