Infective Endocarditis Dr Meral SNMEZOLU Infectous Diseases Department






































































- Slides: 96

Infective Endocarditis Dr. Meral SÖNMEZOĞLU Infectous Diseases Department YEDİTEPE UNIVERSITY HOSPITAL

Learning Objectives Recognize the risk factors, signs, and symptoms of infectious endocarditis. Understand the many approaches to diagnosing infectious endocarditis. Appreciate the necessity of rapid treatment. Anticipate possible complications. Know the indications for prophylaxis of infective endocarditis

Infective Endocarditis Infective endocarditis (IE) is a deadly disease. Despite improvements in its management, IE remains associated with high mortality and severe complications

Definition IE should be suspected in a variety of very different clinical situations. It may present as an acute, rapidly progressive infection, but also as a subacute or chronic disease with lowgrade fever and non-specific symptoms that may mislead or confuse initial assessment.

Definition Up to 90% of patients present with fever, often associated with systemic symptoms of chills, poor appetite and weight loss. Heart murmurs are found in up to 85% of patients. Up to 25% of patients have embolic complications at the time of diagnosis. Therefore IE has to be suspected in any patient presenting with fever and embolic phenomena.

Definition Infectious Endocarditis (IE): an infection of the heart’s endocardial surface Classified into four groups: – Native Valve IE – Prosthetic Valve IE – Intravenous drug abuse (IVDA) IE – Nosocomial IE (HCA- IE) 1/3

Sites of lesions Mitral Valve: 85% (Left atrium/ventricle) – Common site for Strep viridans group Aortic valve: 55% (Left ventricle) – Emboli would effect systemic organs brain, kidneys, spleen Tricuspid valve: 20% (Right atrium/ventricle) – Common site for IV drug users (Staph. spp) – Emboli to lung Pulmonary valve: 1% (Right ventricle)

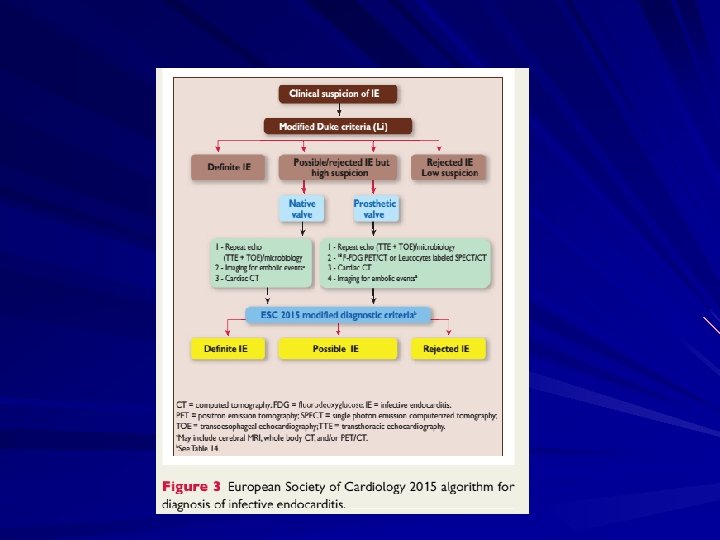
European Heart Journal (2015)

Classification Native valve endocarditis (NVE), acute and subacute Prosthetic valve endocarditis (PVE), early and late Intravenous drug abuse (IVDA) endocarditis – Other terms commonly used to classify types of IE include pacemaker IE and nosocomial IE (NIE).

Further Classification Acute – Affects normal heart valves – Rapidly destructive – Metastatic foci – Commonly Staph. – If not treated, usually fatal within 6 weeks Subacute – Often affects damaged heart valves – Indolent nature – If not treated, usually fatal by one year

Further Classification Acute Rapid progression of symptoms – Less than 6 weeks duration – Significant systemic signs/symptoms Fever Elevated systemic WBC/ left shift Subacute Slower, more chronic progression of symptoms – Low grade fevers – Vague clinical signs/symptoms weakness, anorexia, malaise, etc.

Acute NVE Frequently involves normal valves and usually has an aggressive course. Rapidly progressive illness in persons who are healthy or debilitated Virulent organisms, S aureus and group B streptococci are typically the causative agents

Subacute NVE Typically affects only abnormal valves. Its course, even in untreated patients, is usually more indolent than that of the acute form and may extend over many months. Alpha-hemolytic streptococci or enterococci, usually in the setting of underlying structural valve disease

PVE Diagnosis is more difficult in PVE than in NVE. Clinical presentation is frequently atypical, particularly in the early postoperative period, in which fever and inflammatory syndromes are common in the absence of IE. Persistent fever should trigger the suspicion of PVE.

PVE As in NVE, diagnosis of PVE is based mainly on the results of echocardiography and blood cultures. However, both are more frequently negative in PVE. Although TOE is mandatory in suspected PVE, its diagnostic value is lower than in NVE.

PVE A negative echocardiogram is frequently observed in PVE and does not rule out the diagnosis, but identification of a new periprosthetic leak is a major criterion CT or nuclear imaging is useful In PVE, staphylococcal and fungal infections are more frequent and streptococcal infection less frequent than in NVE.

PVE Staphylococci, fungi and Gram-negative bacilli are the main causes of early PVE, Staphylococci, oral streptococci, S. bovis and enterococci most frequent organisms of late PVE (community-acquired infections). Staphyloccoci and enteroccoci are the most common agents in prosthetic valve implantation endocarditis.

PVE The Duke criteria are helpful for the diagnosis of NVE (70– 80%), but are less useful in PVE Nuclear techniques, particularly 18 F-FDG PET/CT useful for the diagnosis of PVE An algorithm for evaluation of patients with suspected PVE, including echocardiography and PET/CT has been suggested

Early PVE occurs within 60 days of valve implantation. Traditionally, – coagulase-negative staphylococci, – gram-negative bacilli, and – Candida species have been the common infecting organisms.

Late PVE Early PVE is defined as IE occurring within 1 year of surgery Late PVE as IE occurring beyond 1 year, because of significant differences between the microbiological profiles

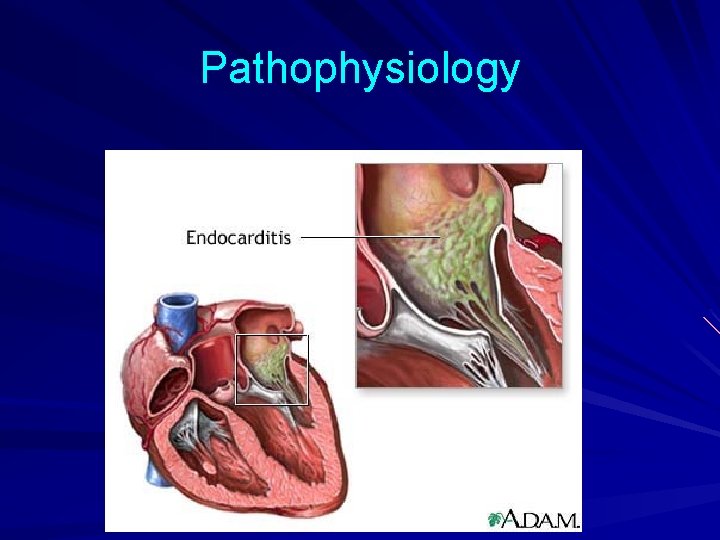
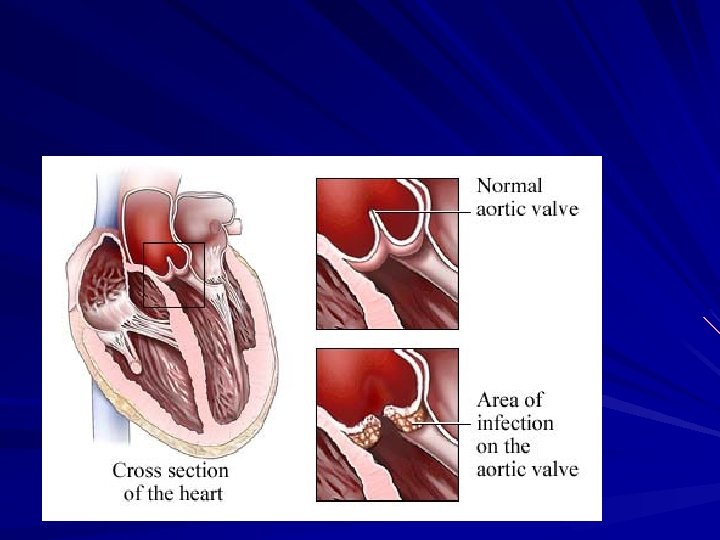
Pathophysiology 1. Turbulent blood flow disrupts the endocardium making it “sticky” 2. Bacteremia delivers the organisms to the endocardial surface 3. Adherence of the organisms to the endocardial surface 4. Eventual invasion of the valvular leaflets

Pathophysiology Formation of Non-Bacterial Thrombotic Endocarditis (NBTE) on surface of cardiac valve or site of endothelial damage – Turbulent blood flow from certain congenital cardiac lesions traumatizes endothelium – Traumatized endothelium predisposed to deposition of platelets and fibrin on endothelial surface resulting in NBTE Bacteremia with potentially pathogenic organism Adherence of bacteria in bloodstream to NBTE Proliferation of bacteria within a vegetation

Pathophysiology


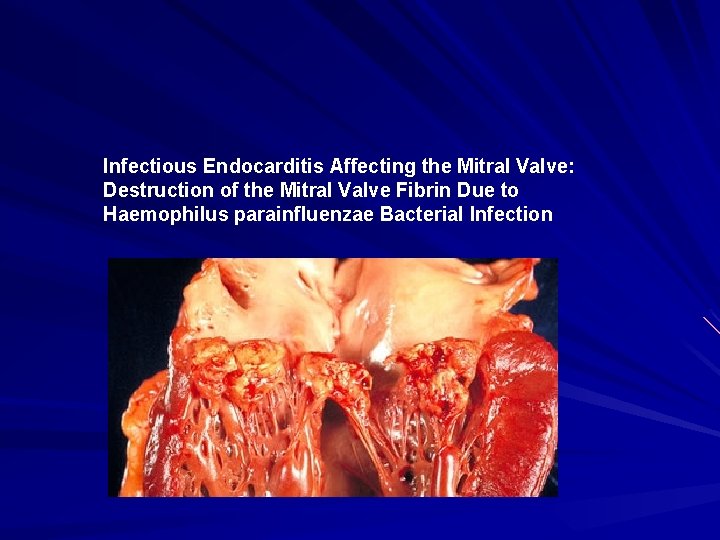
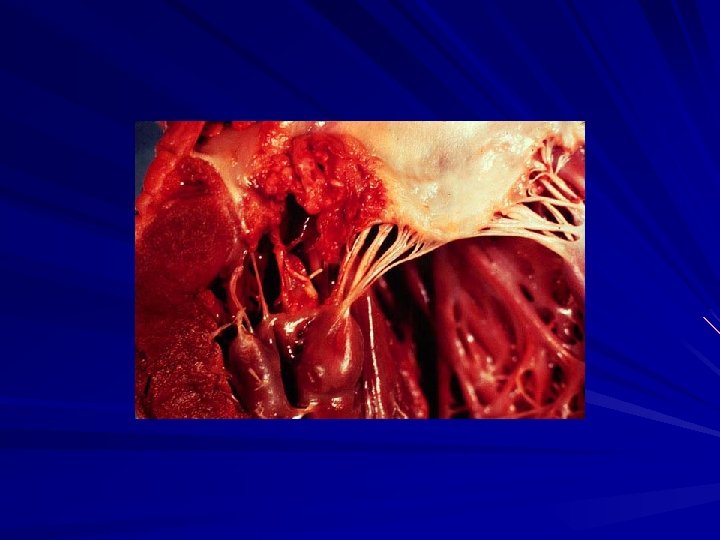
Infectious Endocarditis Affecting the Mitral Valve: Destruction of the Mitral Valve Fibrin Due to Haemophilus parainfluenzae Bacterial Infection


Pathogenesis Multiple independent pathophysiological processes – “Trauma” of the heart surfaces – Platelet/fibrin deposition over traumatized tissue (nonbacterial thrombotic endocarditis) – “Bacteremia” subsequent infection of the platelet/fibrin deposition (Bacterial endocarditis) – Bacterial multiplication (10 9, 10 cfu/gram of tissue)

Causes of Bacteremia Dental: – Procedures -Flossing/brushing Diagnostic Procedures – Respiratory Bronchoscopy – G. I. Barium enema Colonoscopy – Genitourinary Prostatectomy

Epidemiology Incidence difficult to ascertain and varies according to location 3 -9: 100. 000 in industrial countries Occurs in 1: 1000 hospital admission Much more common in males than in females (2: 1) May occur in persons of any age and increasingly common in elderly Mortality ranges from 20 -30%

Risk Factors Intravenous drug abuse Artificial heart valves and pacemakers Acquired heart defects – Calcific aortic stenosis – Mitral valve prolapse with regurgitation Congenital heart defects Intravascular catheters

Risk Factors Rheumatic heart disease – Currently accounts for 20 -25% of cases Prosthetic heart valves – 12 -33% of cases: Staph common if IE occurs within 1 year of surgery; surgery required to replace infected material IV drug use – Staph spp. most commonly isolated Intravenous catherization/shunt procedures Congenital heart defects – patent ductus arteriosus, intraventricular shunts, etc Degenerative cardiac lesions

Infecting Organisms Common bacteria – S. aureus – Streptococci – Enterococci Not so common bacteria – Fungi – Pseudomonas – HACEK

Streptococci – – Alpha-hemolytic Beta-hemolytic Enterococci Pneumococci Staphylococci – S. aureus – Coagulase negative Most common Uncommon Rare Second most common Uncommon, but increasing Gram-Negatives All Rare – Enterics, Pseudomonas species, Haemophilus, Actinobacillus, Cardiobacterium, Eikenella, Kingella, Neisseria sp Fungi – Candida species – Others Uncommon Rare

Infecting Organisms Overall, S aureus infection is the most common cause of IE, including PVE, acute IE, and IVDA IE. Approximately 35 -60. 5% of staphylococcal bacteremias are complicated by IE. More than half the cases are not associated with underlying valvular disease.

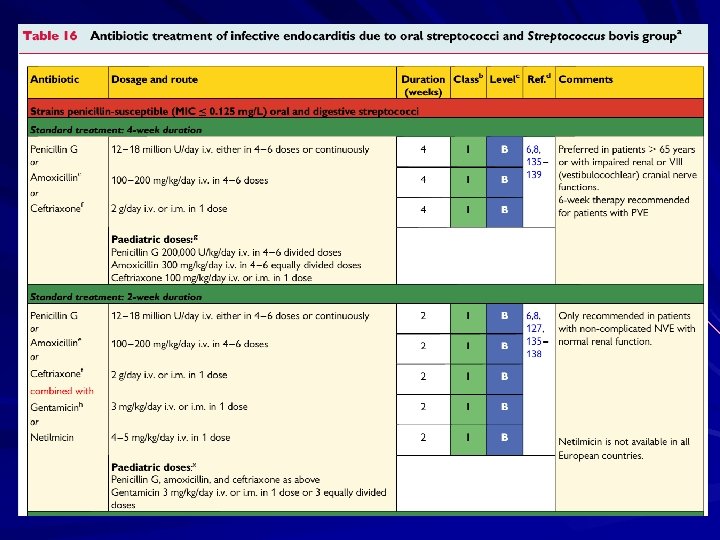
IE: Infecting organisms Bacterial(80 -90% of all causes due to strep & staph species) – Streptococci: 55 -60% Viridans strep: Strep species normally found in mouth – Strep sanguis, oralis, salivarius, or mutans Rarely caused by Group A, B, C, strep

IE: Infecting organisms Staph. species: accounts for 20 -35% of all bacterial causes – Staph aureus: (coagulase positive staph) Coagulase is an enzyme capable of causing serum proteins to clot. A. Most common bacteria isolated from IV drug users B. Most common staph species isolated from I. E. infections C. Mortality is approximately 40% D. Therapy duration based on presence/absence of prosthetic material and antibiotic sensitivity

IE: Infecting organisms – Staph epidermidis: (coagulase-negative) A. Most common staph species in patients with prosthetic valves and in neonates B. Often presents as subacute IE (SBE) – Gram Negative Bacteria HACEK group: Hemophilus spp. , Actinobacillus spp, Cardiobacterium spp, Eikenella spp, Kingella spp. Miscellaneous Gram Negative Organisms: – Typical gram negative bacilli (E. coli, Klebsiella, etc) A. Frequently part of polymicrobial infections B. IV drug users or patients with prosthetic material C. High mortality rate: >65%

Symptoms Acute – High grade fever and chills – SOB – Arthralgias/ myalgias – Abdominal pain – Pleuritic chest pain – Back pain Subacute – – – – Low grade fever Anorexia Weight loss Fatigue Arthralgias/ myalgias Abdominal pain N/V The onset of symptoms is usually ~2 weeks or less from the initiating bacteremia

Signs Fever Heart murmur Nonspecific signs – petechiae, subungal or “splinter” hemorrhages, clubbing, splenomegaly, neurologic changes More specific signs - Osler’s Nodes, Janeway lesions, and Roth Spots

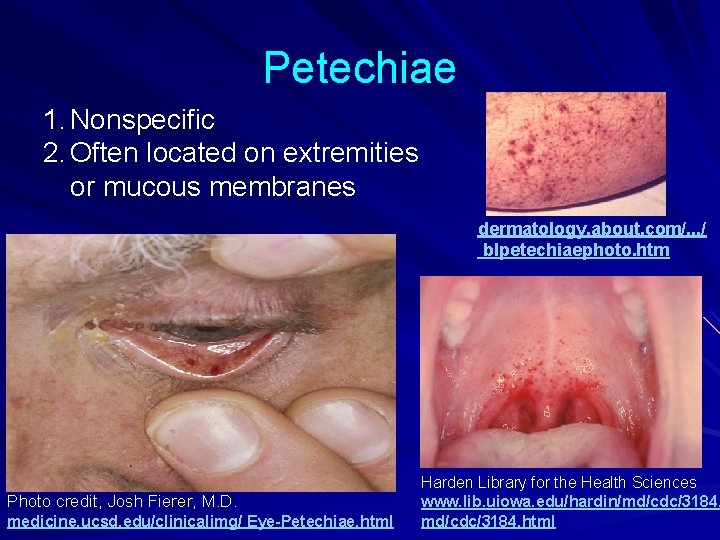
Petechiae 1. Nonspecific 2. Often located on extremities or mucous membranes dermatology. about. com/. . . / blpetechiaephoto. htm Photo credit, Josh Fierer, M. D. medicine. ucsd. edu/clinicalimg/ Eye-Petechiae. html Harden Library for the Health Sciences www. lib. uiowa. edu/hardin/md/cdc/3184. html

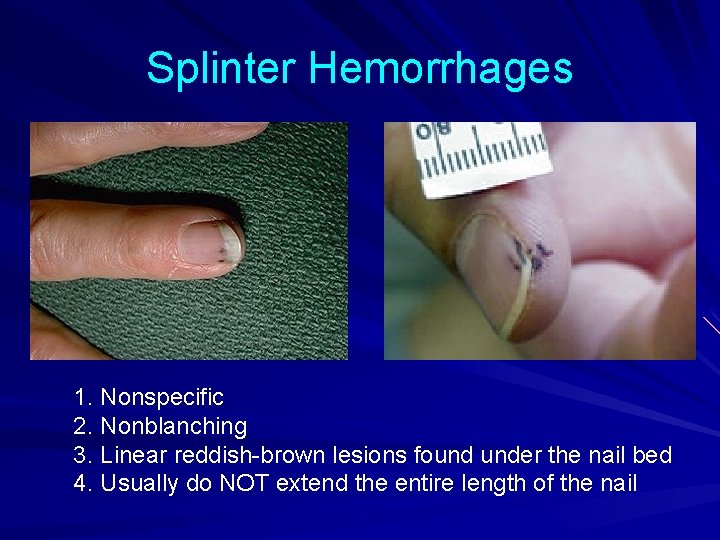
Splinter Hemorrhages 1. Nonspecific 2. Nonblanching 3. Linear reddish-brown lesions found under the nail bed 4. Usually do NOT extend the entire length of the nail

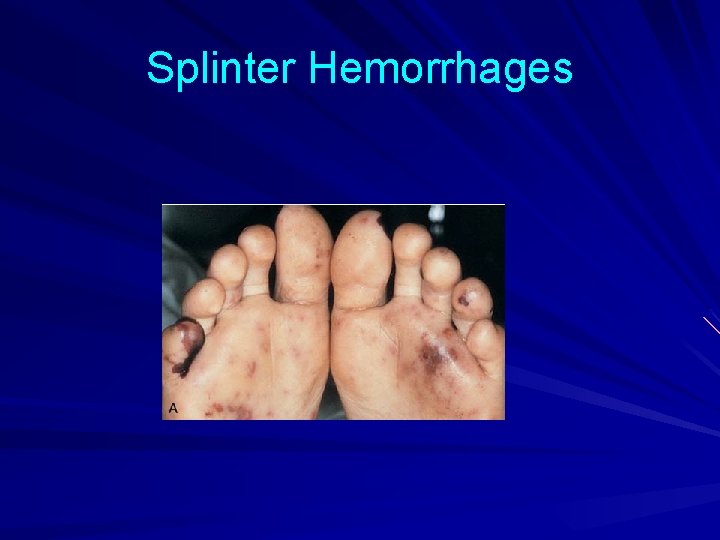
Splinter Hemorrhages

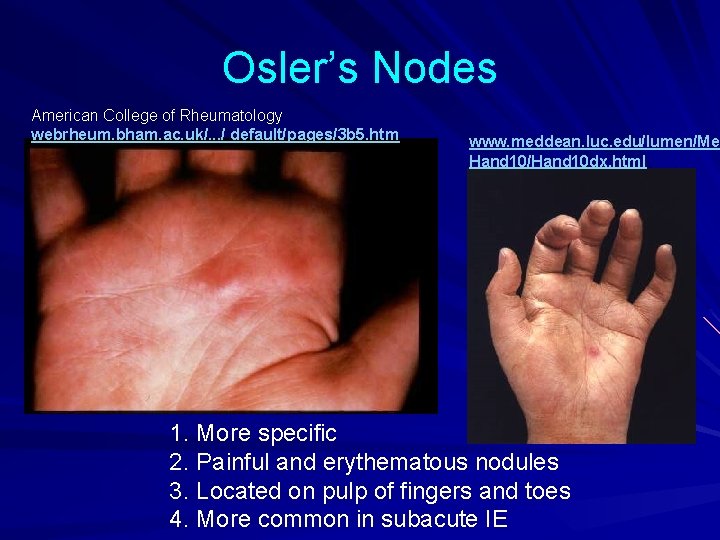
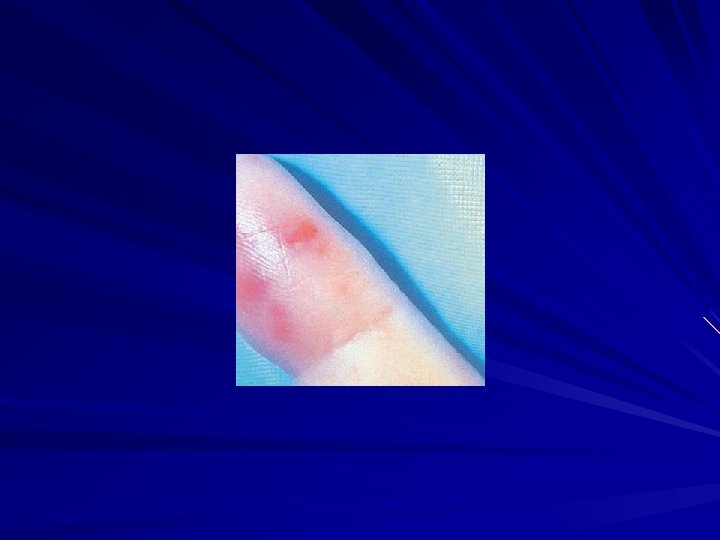
Osler’s Nodes American College of Rheumatology webrheum. bham. ac. uk/. . . / default/pages/3 b 5. htm www. meddean. luc. edu/lumen/Med Hand 10/Hand 10 dx. html 1. More specific 2. Painful and erythematous nodules 3. Located on pulp of fingers and toes 4. More common in subacute IE


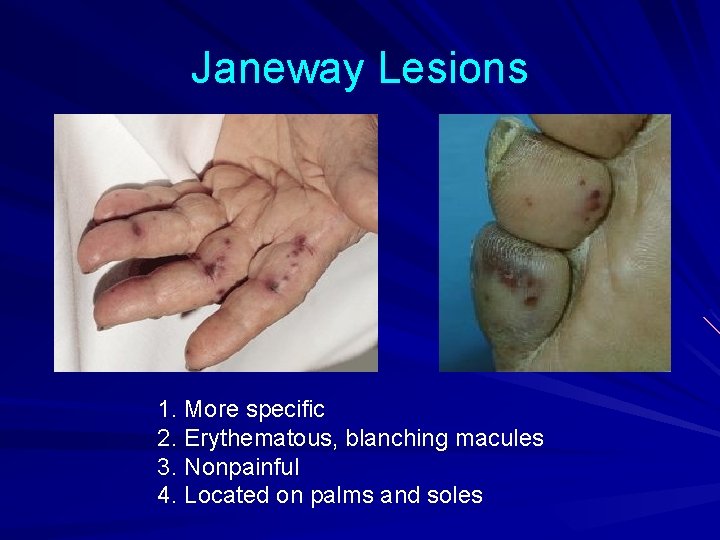
Janeway Lesions 1. More specific 2. Erythematous, blanching macules 3. Nonpainful 4. Located on palms and soles

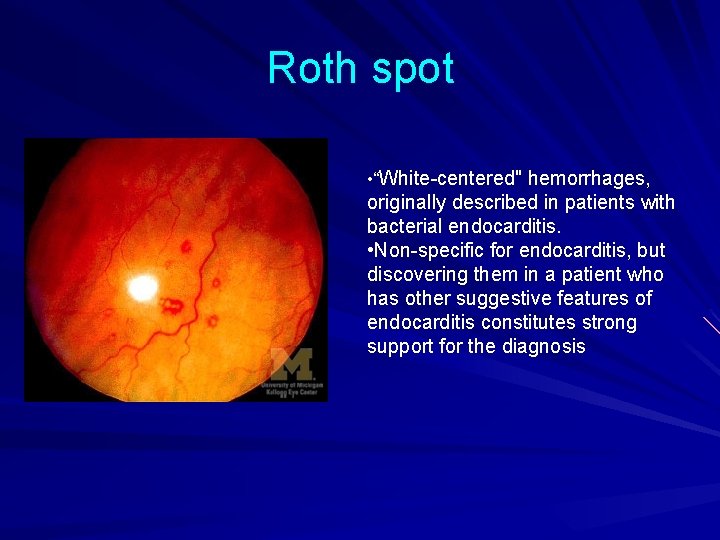
Roth spot • “White-centered" hemorrhages, originally described in patients with bacterial endocarditis. • Non-specific for endocarditis, but discovering them in a patient who has other suggestive features of endocarditis constitutes strong support for the diagnosis

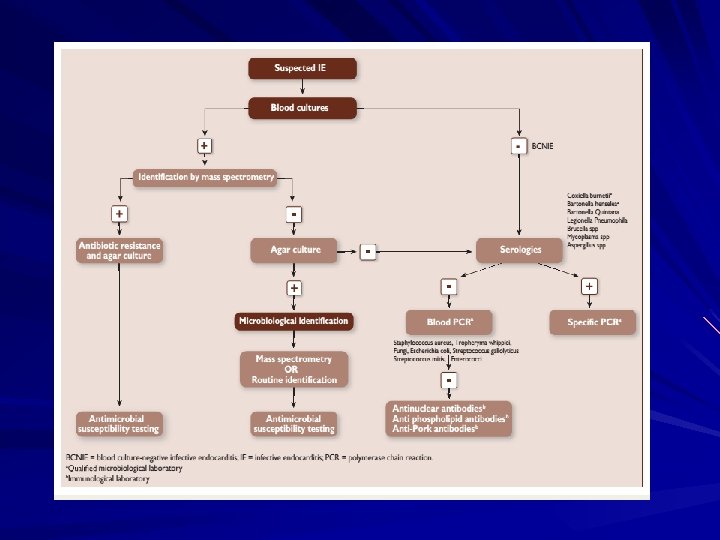
The Essential Blood Test Blood Cultures – – – Minimum of three blood cultures 1 Three separate venipuncture sites Obtain 10 -20 m. L in adults and 0. 5 -5 m. L in children 2 Positive Result – Typical organisms present in at least 2 separate samples – Persistently positive blood culture (atypical organisms) Two positive blood cultures obtained at least 12 hours apart Three or a more positive blood cultures in which the first and last samples were collected at least one hour apart

Additional Labs CBC ESR and CRP Complement levels (C 3, C 4, CH 50) RF Urinalysis Baseline chemistries and coags

Imaging Chest x-ray – Look for multiple focal infiltrates and calcification of heart valves EKG – Rarely diagnostic – Look for evidence of ischemia, conduction delay, and arrhythmias Echocardiography

Indications for Echocardiography Transthoracic echocardiography (TTE) – First line if suspected IE – Native valves Transesophageal echocardiography (TEE) – Prosthetic valves – Intracardiac complications – Inadequate TTE – Fungal or S. aureus or bacteremia

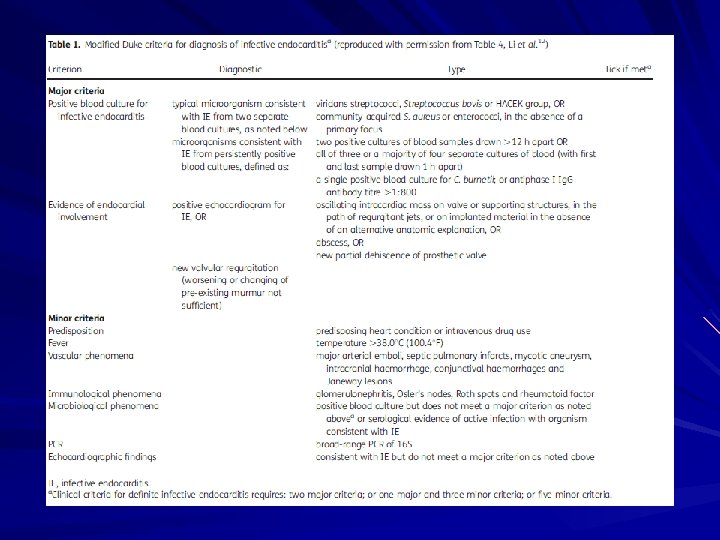
Making the Diagnosis Pelletier and Petersdorf criteria (1977) – Classification scheme of definite, probable, and possible IE – Reasonably specific but lacked sensitivity Von Reyn criteria (1981) – Added “rejected” as a category – Added more clinical criteria – Improved specificity and clinical utility Duke criteria (1994) – Included the role of echocardiography in diagnosis – Added IVDA as a “predisposing heart condition”

Modified Duke Criteria Definite IE – Microorganism (via culture or histology) in a valvular vegetation, embolized vegetation, or intracardiac abscess – Histologic evidence of vegetation or intracardiac abscess Possible IE – – – 2 major 1 major and 3 minor 5 minor Rejected IE – Resolution of illness with four days or less of antibiotics


DIAGNOSIS

Diagnosis of endocarditis is usually based on – clinical, – microbiologic, and – echocardiographic findings.



Criteria for consideration of IE

Indications for ECHO



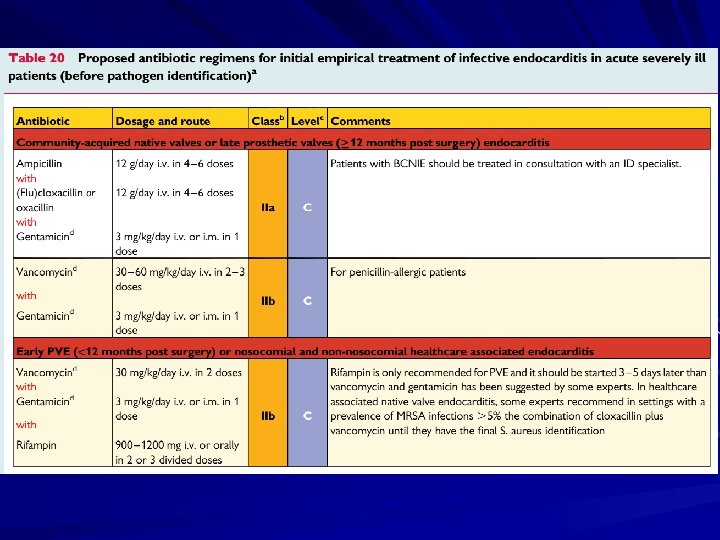
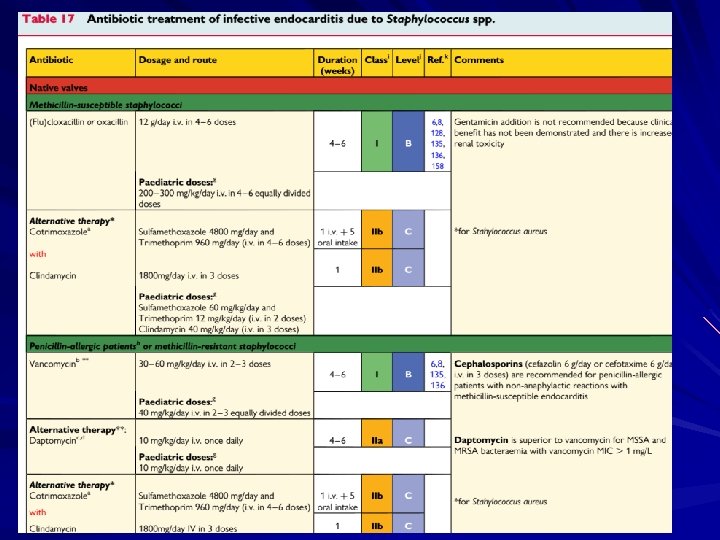
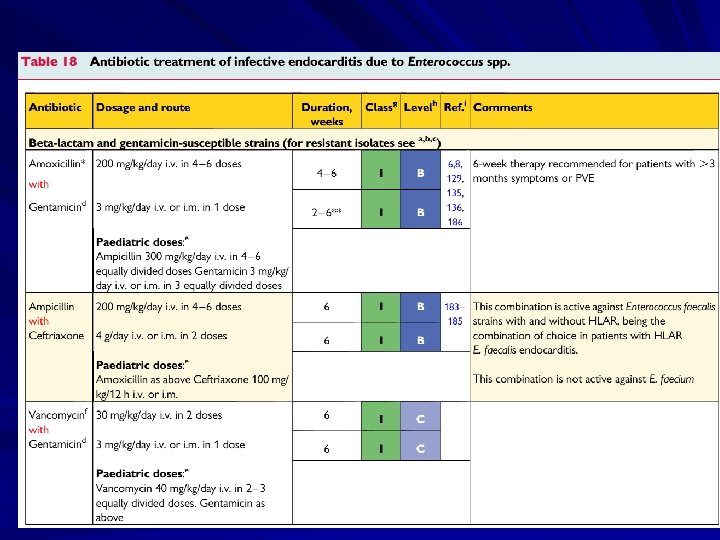
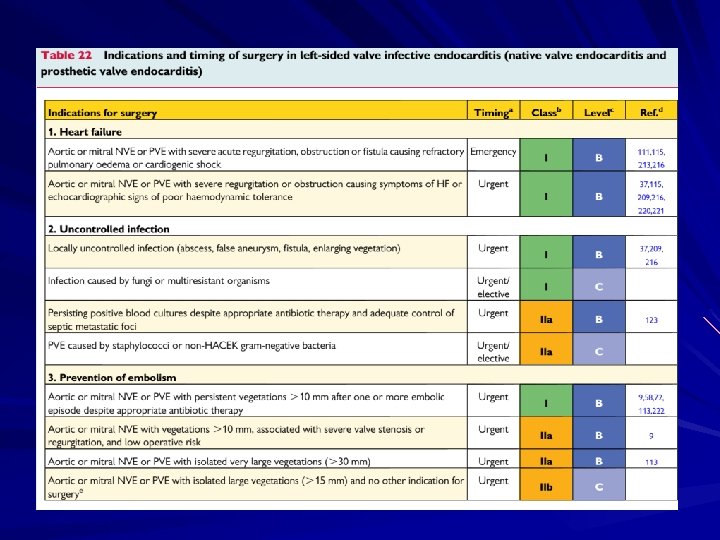
Treatment involves antimicrobial therapy targeted to the identified organism. Surgical indications include heart failure, uncontrolled infection, and prevention of embolic events.

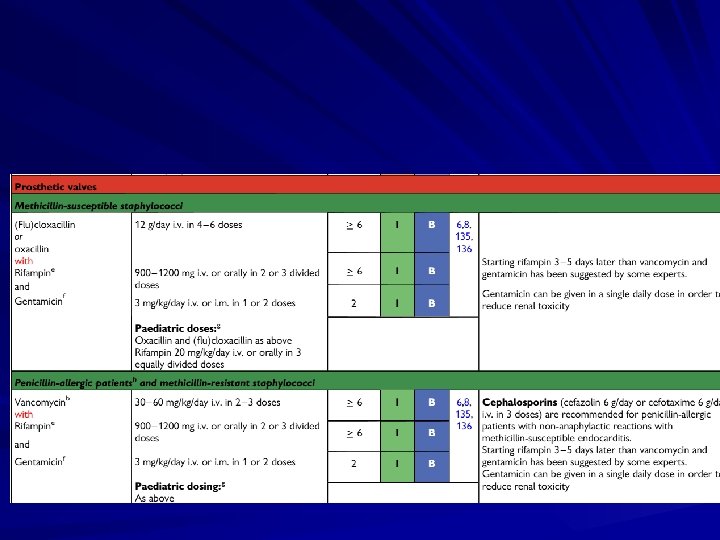
Treatment Parenteral antibiotics – High serum concentrations to penetrate vegetations – Prolonged treatment to kill dormant bacteria clustered in vegetations Surgery – Intracardiac complications Surveillance blood cultures

Treatment Multiple agents common due to synergy Duration of therapy commonly 4 -6 weeks Quick access to cardiothoracic surgery MIC’s/MBC’s determined for pathogens Effects drug selection, need for combination therapy Uncertain role for Schlicter test Unique Aminoglycoside “therapeutic” range – AG’s dosed at 1 mg/kg IV q 8 hours; Peaks of 3 acceptable







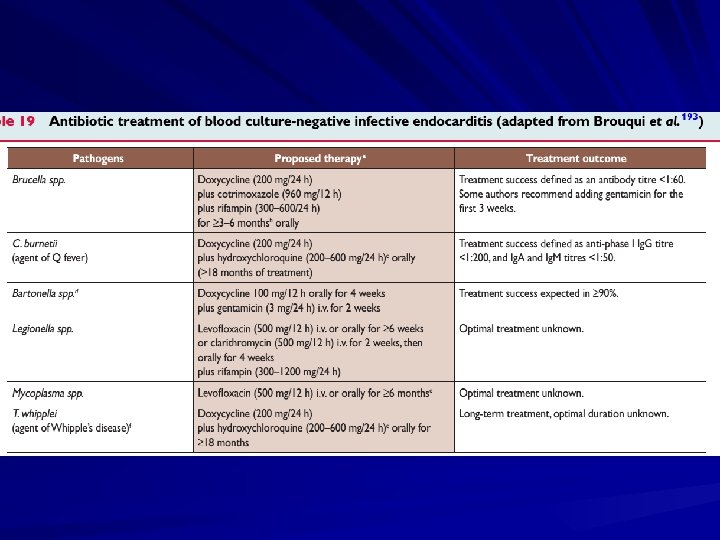
Fungal IE Fungi are most frequently observed in PVE and in IE affecting IVDAs and immunocompromised patients. Candida and Aspergillus spp. predominate, the latter resulting in BCNIE. Mortality is very high (50%), and treatment necessitates dual antifungal administration and valve replacement. Most cases are treated with various forms of Amphotericin B with or without azoles, recent case reports describe successful therapy with the new echinocandin caspofungin


Cure rates for NVE For S viridans and S bovis infection, the rate is 98%. For enterococci and S aureus infection in individuals who abuse intravenous drugs, the rate is 90%. For community-acquired S aureus infection in individuals who do not abuse intravenous drugs, the rate is 60 -70%. For infection with aerobic gram-negative organisms, the rate is 40 -60%. For infection with fungal organisms, the rate is lower than 50%.

Cure rates for NVE Rates are 10 -15% lower for each of the above categories, for both early and late PVE. Surgery is required far more frequently. Approximately 60% of early Co. NS PVE cases and 70% of late Co. NS PVE cases are curable.

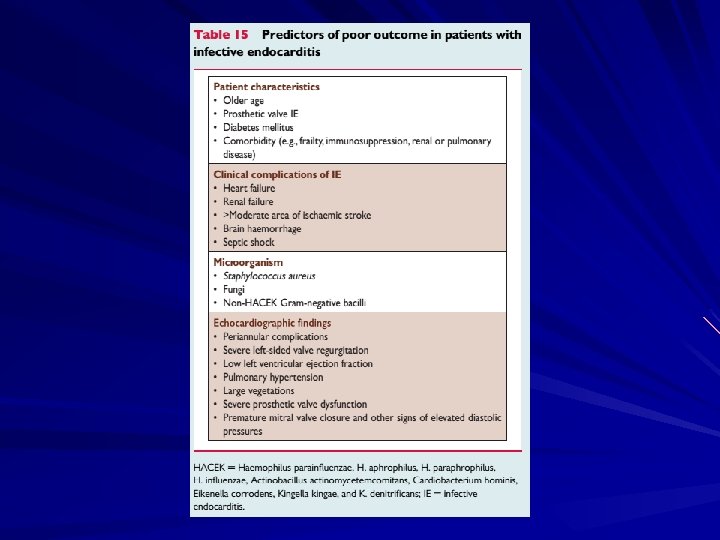
Monitoring for complications Valvular dysfunction, usually insufficiency of the mitral or aortic valves Myocardial or septal abscesses Congestive heart failure Metastatic infection Embolic phenomenon Organ dysfunction resulting from immunological processes

Complications Four etiologies – Embolic – Local spread of infection – Metastatic spread of infection – Formation of immune complexes – glomerulonephritis and arthritis

Embolic Complications Occur in up to 40% of patients with IE Predictors of embolization – Size of vegetation – Left-sided vegetations – Fungal pathogens, S. aureus, and Strep. Bovis Incidence decreases significantly after initiation of effective antibiotics

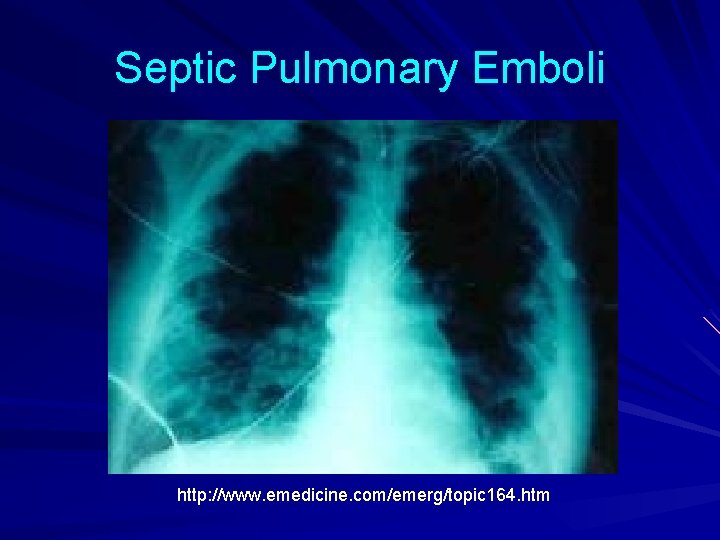
Embolic Complications Stroke Myocardial Infarction – Fragments of valvular vegetation or vegetation -induced stenosis of coronary ostia Ischemic limbs Hypoxia from pulmonary emboli Abdominal pain (splenic or renal infarction)

Septic Pulmonary Emboli http: //www. emedicine. com/emerg/topic 164. htm

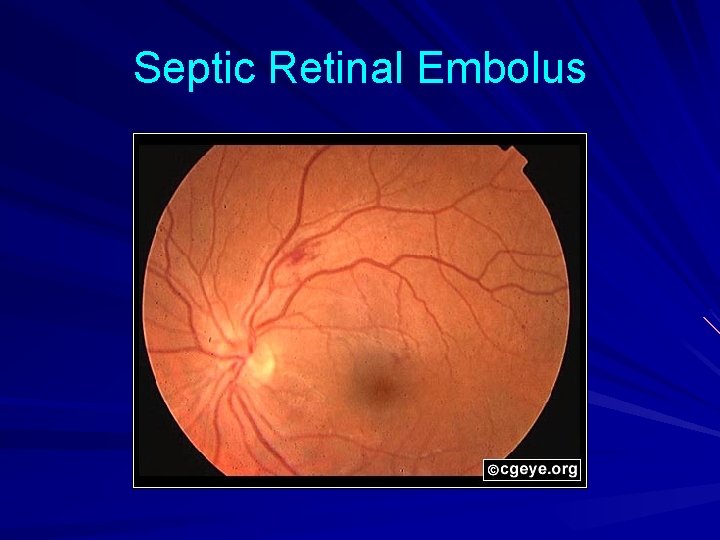
Septic Retinal Embolus

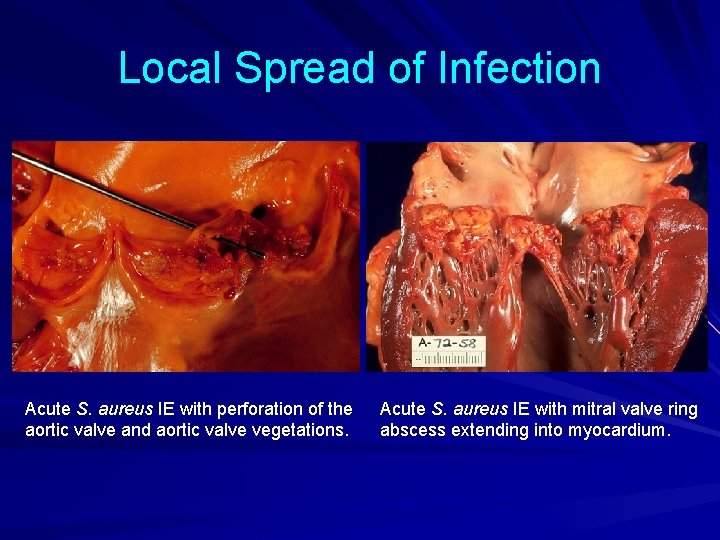
Local Spread of Infection Heart failure – Extensive valvular damage Paravalvular abscess (30 -40%) – Most common in aortic valve, IVDA, and S. aureus – May extend into adjacent conduction tissue causing arrythmias – Higher rates of embolization and mortality Pericarditis Fistulous intracardiac connections

Local Spread of Infection Acute S. aureus IE with perforation of the aortic valve and aortic valve vegetations. Acute S. aureus IE with mitral valve ring abscess extending into myocardium.

Metastatic Spread of Infection Metastatic abscess – Kidneys, spleen, brain, soft tissues Meningitis and/or encephalitis Vertebral osteomyelitis Septic arthritis


Complications requiring surgery Infected prosthetic material: less than 1 year out from original heart surgery Refractory congestive heart failure (Leading cause of death) Unresponsive infection/ continued infection despite appropriate antibiotics Pt. experiences more than 1 major emboli






TUS 2012 • Yüksek ateş şikâyetiyle başvuran 67 yaşındaki erkek hastada enfektif endokardit tanısı konulmuştur. • Kan kültürlerinde Streptococcus bovis üreyen bu hastada aşağıdaki kanserlerden hangisinin taranması gerekir? A) Meme kanseri B) Prostat kanseri C) Kolon kanseri D) Perikardiyal mezotelyom E) Akciğer kanseri

TUS 2012 • Yüksek ateş şikâyetiyle başvuran 67 yaşındaki erkek hastada enfektif endokardit tanısı konulmuştur. • Kan kültürlerinde Streptococcus bovis üreyen bu hastada aşağıdaki kanserlerden hangisinin taranması gerekir? A) Meme kanseri B) Prostat kanseri C) Kolon kanseri D) Perikardiyal mezotelyom E) Akciğer kanseri

TUS 2010 • Aşağıdakilerden hangisi en sık karşılan • • • doğal kapak endokardit etkenidir? A) Koagülaz negatif stafilokoklar B) Pnömokoklar C) Mantarlar D) Enterokoklar E) Streptokoklar

TUS 2010 • Aşağıdakilerden hangisi en sık karşılan • • • doğal kapak endokardit etkenidir? A) Koagülaz negatif stafilokoklar B) Pnömokoklar C) Mantarlar D) Enterokoklar E) Streptokoklar

TUS 2013 Aşağıdakilerden hangisi, enfektif endokardit tanısında kullanılan Duke kriterleri içerisinde minör kriterlerden biri olarak yer almaz? A) Yüksek ateş (≥ 38 °C) B) Osler nodülleri C) Roth lekeleri D) Janeway lezyonları E) Eritema marginatum

TUS 2013 Aşağıdakilerden hangisi, enfektif endokardit tanısında kullanılan Duke kriterleri içerisinde minör kriterlerden biri olarak yer almaz? A) Yüksek ateş (≥ 38 °C) B) Osler nodülleri C) Roth lekeleri D) Janeway lezyonları E) Eritema marginatum