Infectious Disease I Upper Respiratory Tract Infections Courses




























- Slides: 34

Infectious Disease I: Upper Respiratory Tract Infections Courses in Therapeutics and Disease State Management Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Learning Objectives (Slide 1 of 3) • Name the most common infectious pathogens in acute otitis media, rhinosinusitis, and pharyngitis • Identify risk factors for amoxicillin-resistant bacteria in acute otitis media • Differentiate between patients with acute otitis media and those with otitis media with effusion • Develop a treatment plan for a patient with acute otitis media • Recommend therapy for a patient with acute otitis media who fails treatment with amoxicillin Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Learning Objectives (Slide 2 of 3) • Defend the role of vaccination for the prevention of upper respiratory tract infections • Delineate viral and bacterial rhinosinusitis based on patient history • Select the proper dose of amoxicillin and amoxicillin– clavulanate for patients with upper respiratory tract infections • Determine when to refer a patient with acute bacterial rhinosinusitis to a specialist • Suggest nonprescription medications for patients with rhinosinusitis when antibiotics are not prescribed Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Learning Objectives (Slide 3 of 3) • Use a patient’s history and clinical presentation to gauge the likelihood of GABHS pharyngitis • Develop a therapeutic plan, including supportive care, for a patient with GABHS pharyngitis • Ascertain the need for GABHS diagnostic testing • Counsel a patient regarding the time frame for GABHS incubation and infectivity • Select an appropriate antibiotic and dose for recurrent GABHS in adults and children Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Required and Recommended Reading Required Reading Frei C, Frei B. Chapter 86. Upper Respiratory Tract Infections. In: Di. Piro JT, Talbert RL, Yee GC, Matzke GR, Wells BG, Posey L. eds. Pharmacotherapy: A Pathophysiologic Approach, 9 e. New York, NY: Mc. Graw-Hill; 2014. Recommended Readings • Lieberthal AS, Carroll AE, Chonmaitree T, et al. The diagnosis and management of acute otitis media. Pediatrics. 2013; 131(3): e 964 -e 999 • Chow AW, Benninger MS, Brook I, et al. IDSA clinical practice guideline for acute bacterial rhinosinusitis in children and adults. Clin Infect Dis. 2012; 54(8): 1042. • Shulman ST, Bisno AL, Clegg HW, et al. Clinical practice guideline for the diagnosis and management of group A streptococcal pharyngitis: 2012 update by the Infectious Diseases Society of America. Clin Infect Dis 2012; 55: e 86 -e 102. Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Overview: Respiratory Tract Infections • One of the most frequent infectious disease reasons of physician office and emergency room visits • Most common upper Respiratory Tract Infections • Otitis media is an inflammation of the middle ear • Rhinosinusitis is an inflammation and/or infection of the paranasal sinuses • Pharyngitis is an acute infection of the oropharynx or nasopharynx Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Anatomy of the Upper Airway Link: Figures demonstrating the anatomy of the upper airway Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Acute Otitis Media: Pathophysiology • Acute otitis media has a sudden onset of signs and symptoms • Commonly preceded by a viral upper respiratory infection that impairs the function of the Eustachian tube in the middle ear • Impaired mucociliary actions leads to the migration and build up of pathogens that colonize the nasopharynx into the middle ear • Bacteria multiply and cause infection • Anatomical differences place children at a higher risk of otitis media when compared to adults Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Acute Otitis Media: Most Common Pathogens • Virus are the most common cause • Common Bacterial causes • Streptococcus pneumoniae • Non typeable Haemophilus influenzae • Moraxella catarrhalis • Vaccination with H. influenzae type b (Hib) and the seven-valent pneumococcal conjugate (PCV 7) vaccine has decreased the rates of H. influenzae type B and S. pneumoniae Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Acute Otitis Media: Clinical Presentation Signs and Symptoms • Children present with • Irritability • Tugging on the ear • Middle Ear Inflammation • Otalgia (ear pain) • Erythema of the tympanic membrane • Middle ear effusion • Fullness/ bulging of the tympanic membrane • Limited or absent mobility of the tympanic membrane • Otorrhea Diagnosis of Acute Otitis Media • Following three criteria must be met • Acute signs of infection • Evidence of middle ear inflammation • Presence of fluid in the middle ear Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Acute Otitis Media: Treatment Overview • Differentiate acute otitis media from otitis media with effusion or chronic otitis media • Amoxicillin is the mainstay of therapy • Risk factors for amoxicillin resistant pathogens • Attendance at child care centers • Antibiotic use within the past 30 days • Age younger than 2 years Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Acute Otitis Media Treatment: Nonpharmacological / Supportive Care • Systemic pain relief • Acetaminophen • Nonsteroidal Anti-inflammatory Drugs (NSAIDs) like ibuprofen • Local pain relief (eardrops) • Amethocaine • Benzocaine • Lidocaine • Decongestants and antihistamines should not be used due to lack of benefit and increased risk of adverse effects Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Acute Otitis Media: Pharmacological Treatment (Slide 1 of 2) • Delayed therapy • Patient or caregiver receives an antibiotic prescription, but to monitor symptoms for improvement over the next 48 to 72 hours before starting antibiotics • Candidates for delayed therapy include • Children 6 months to 2 years of age without severe symptoms plus uncertain diagnosis • Children 2 years and older without severe symptoms • Children 2 years and older with an uncertain diagnosis • Amoxicillin is the drug of choice • Duration of treatment is traditionally 10 days Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

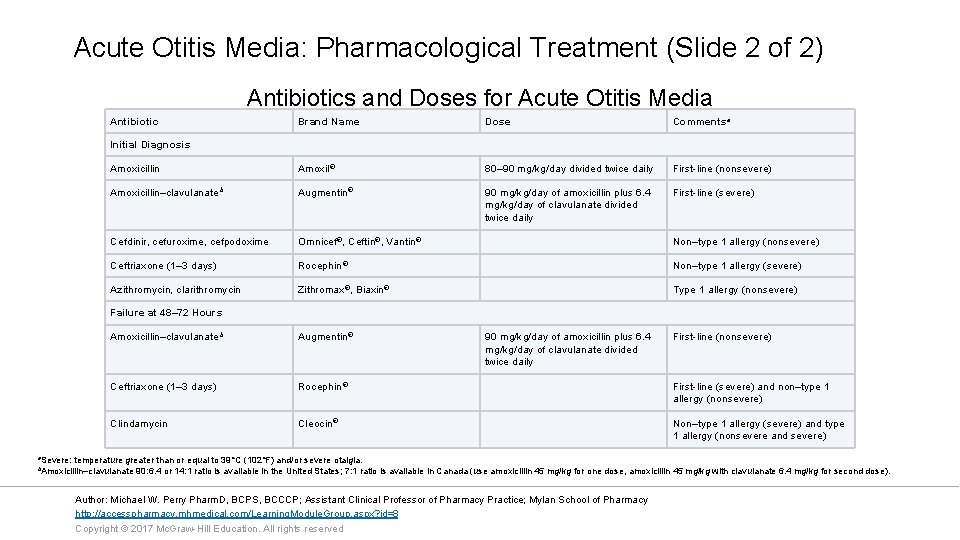
Acute Otitis Media: Pharmacological Treatment (Slide 2 of 2) Antibiotics and Doses for Acute Otitis Media Antibiotic Brand Name Dose Commentsa Amoxicillin Amoxil® 80– 90 mg/kg/day divided twice daily First-line (nonsevere) Amoxicillin–clavulanate b Augmentin® 90 mg/kg/day of amoxicillin plus 6. 4 mg/kg/day of clavulanate divided twice daily First-line (severe) Cefdinir, cefuroxime, cefpodoxime Omnicef®, Ceftin®, Vantin® Non–type 1 allergy (nonsevere) Ceftriaxone (1– 3 days) Rocephin® Non–type 1 allergy (severe) Azithromycin, clarithromycin Zithromax®, Biaxin® Type 1 allergy (nonsevere) Initial Diagnosis Failure at 48– 72 Hours Amoxicillin–clavulanate b Augmentin® 90 mg/kg/day of amoxicillin plus 6. 4 mg/kg/day of clavulanate divided twice daily First-line (nonsevere) Ceftriaxone (1– 3 days) Rocephin® First-line (severe) and non–type 1 allergy (nonsevere) Clindamycin Cleocin® Non–type 1 allergy (severe) and type 1 allergy (nonsevere and severe) a. Severe: temperature greater than or equal to 39°C (102°F) and/or severe otalgia. b. Amoxicillin–clavulanate 90: 6. 4 or 14: 1 ratio is available in the United States; 7: 1 ratio is available in Canada (use amoxicillin 45 mg/kg for one dose, amoxicillin 45 mg/kg with clavulanate 6. 4 mg/kg for second dose). Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Acute Otitis Media: Overall Monitoring • Patients should be reassessed 3 days after initial visit • Signs and symptoms of acute otitis media should be improved • Worsening symptoms • Would prompt the initiation of antibiotics if delayed therapy strategy employed • Would prompt change in antibiotic therapy if patient receiving antibiotics • Most children become asymptomatic by day 7 • Effusions in middle ear may persist even after symptom improvement • Hearing loss should warrant immediate reevaluation Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Acute Bacterial Rhinosinusitis: Pathophysiology • Rhinosinusitis is an inflammation and/or infection of the paranasal sinuses and nasal mucosa • Commonly preceded by a viral upper respiratory infection that causes inflammation of the nasal mucosa • Inflamed tissues decrease nasal drainage via the sinus ostia • Mucosal secretions build up and local defenses become impaired • Bacteria multiply and cause infection Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Anatomy of the Nasal Cavity Link: Figure demonstrating the anatomy of the nasal cavity Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Acute Bacterial Rhinosinusitis: Most Common Pathogens • Virus are the most common cause of Rhinosinusitis • Acute Bacterial Rhinosinusitis • Most common • Streptococcus pneumoniae • Haemophilus influenzae • Moraxella catarrhalis • Less Frequent • • Streptococcus pyogenes Staphylococcus aureus gram-negative bacilli anaerobes Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Acute Bacterial Rhinosinusitis: Clinical Presentation Signs and Symptoms • Sinus drainage and pressure • Purulent anterior nasal discharge • purulent or discolored posterior nasal discharge, • Nasal congestion or obstruction • Facial congestion or fullness • Facial pain or pressure • • Ear pain/pressure/fullness Dental pain Halitosis Non specific symptoms • • Fever Headache Cough Fatigue Diagnosis • Sinus puncture • Sinus radiography • Clinical Presentation • Persistent signs or symptoms ≥ 10 days without improvement • Onset of severe signs or symptoms with high fever and purulent nasal discharge or facial pain that last for 3 to 4 consecutive days • New-onset fever, headache, or increase in nasal discharge following a viral upper respiratory tract infection that lasted 5 to 6 days and with symptoms that were initially improving Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Acute Bacterial Rhinosinusitis: Treatment Overview • Reduction in the signs and symptoms of rhinosinusitis is the primary goal of treatment • • Eradicate bacterial infection with judicious use of antibiotics Minimize the duration of illness Prevent complications Prevent progression to chronic sinusitis • Amoxicillin–clavulanate is the drug of choice for acute bacterial rhinosinusitis Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Acute Bacterial Rhinosinusitis Treatment: Nonpharmacological / Supportive Care • Nonbacterial rhinosinusitis • Topical nasal decongestants • Reduce inflammation via vasoconstriction • Oxymetazoline • Phenylephrine • Oral decongestants • Reduce inflammation via vasoconstriction • Phenylephrine • Pseudoephedrine • Bacterial Rhinosinusitis • Avoid decongestants and antihistamines • Irrigation of nasal sinus • Increase mucosal moisture • Steam inhalation • Saline instillation/ irrigation • Inhaled corticosteroids can be used in patients with a history of allergic rhinitis • Irrigation of nasal sinus • Increase mucosal moisture • Steam inhalation • Saline instillation/ irrigation Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

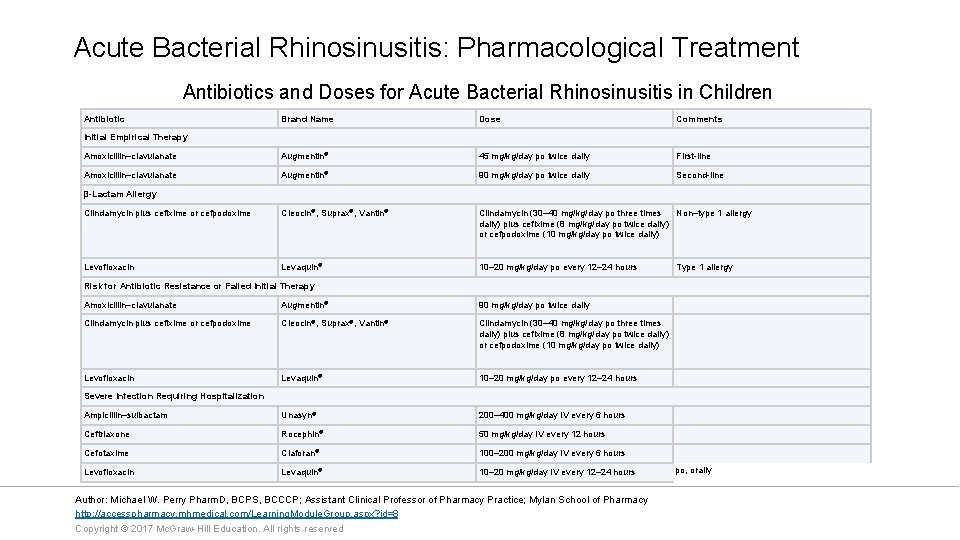
Acute Bacterial Rhinosinusitis: Pharmacological Treatment Antibiotics and Doses for Acute Bacterial Rhinosinusitis in Children Antibiotic Brand Name Dose Comments Amoxicillin–clavulanate Augmentin® 45 mg/kg/day po twice daily First-line Amoxicillin–clavulanate Augmentin® 90 mg/kg/day po twice daily Second-line Clindamycin plus cefixime or cefpodoxime Cleocin®, Suprax®, Vantin® Clindamycin (30– 40 mg/kg/day po three times Non–type 1 allergy daily) plus cefixime (8 mg/kg/day po twice daily) or cefpodoxime (10 mg/kg/day po twice daily) Levofloxacin Levaquin® 10– 20 mg/kg/day po every 12– 24 hours Initial Empirical Therapy β-Lactam Allergy Type 1 allergy Risk for Antibiotic Resistance or Failed Initial Therapy Amoxicillin–clavulanate Augmentin® 90 mg/kg/day po twice daily Clindamycin plus cefixime or cefpodoxime Cleocin®, Suprax®, Vantin® Clindamycin (30– 40 mg/kg/day po three times daily) plus cefixime (8 mg/kg/day po twice daily) or cefpodoxime (10 mg/kg/day po twice daily) Levofloxacin Levaquin® 10– 20 mg/kg/day po every 12– 24 hours Ampicillin–sulbactam Unasyn® 200– 400 mg/kg/day IV every 6 hours Ceftriaxone Rocephin® 50 mg/kg/day IV every 12 hours Cefotaxime Claforan® 100– 200 mg/kg/day IV every 6 hours Levofloxacin Levaquin® 10– 20 mg/kg/day IV every 12– 24 hours Severe Infection Requiring Hospitalization Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved po, orally

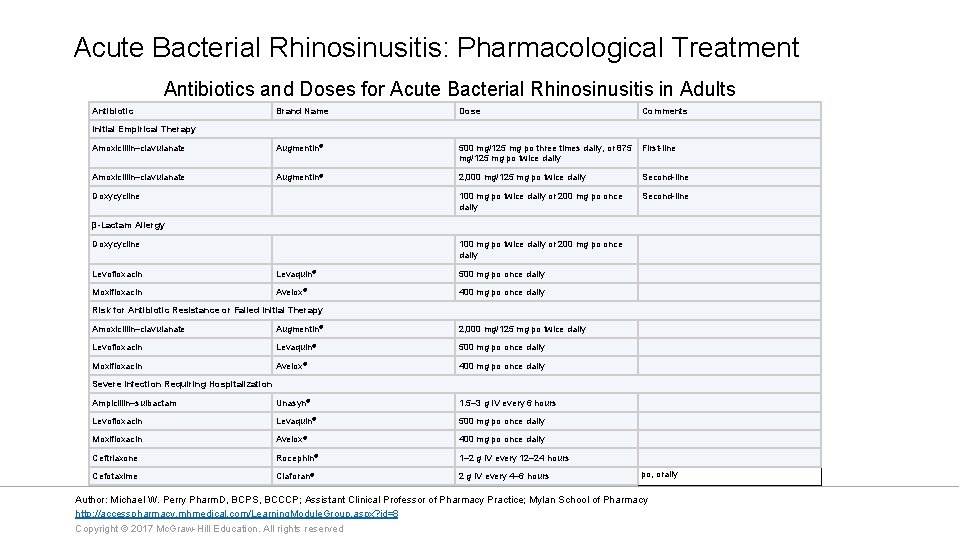
Acute Bacterial Rhinosinusitis: Pharmacological Treatment Antibiotics and Doses for Acute Bacterial Rhinosinusitis in Adults Antibiotic Brand Name Dose Comments Amoxicillin–clavulanate Augmentin® 500 mg/125 mg po three times daily, or 875 First-line mg/125 mg po twice daily Amoxicillin–clavulanate Augmentin® 2, 000 mg/125 mg po twice daily Second-line 100 mg po twice daily or 200 mg po once daily Second-line Initial Empirical Therapy Doxycycline β-Lactam Allergy Doxycycline 100 mg po twice daily or 200 mg po once daily Levofloxacin Levaquin® 500 mg po once daily Moxifloxacin Avelox® 400 mg po once daily Risk for Antibiotic Resistance or Failed Initial Therapy Amoxicillin–clavulanate Augmentin® 2, 000 mg/125 mg po twice daily Levofloxacin Levaquin® 500 mg po once daily Moxifloxacin Avelox® 400 mg po once daily Ampicillin–sulbactam Unasyn® 1. 5– 3 g IV every 6 hours Levofloxacin Levaquin® 500 mg po once daily Moxifloxacin Avelox® 400 mg po once daily Ceftriaxone Rocephin® 1– 2 g IV every 12– 24 hours Cefotaxime Claforan® 2 g IV every 4– 6 hours Severe Infection Requiring Hospitalization po, orally Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Acute Bacterial Rhinosinusitis: Overall Monitoring • Duration of therapy is generally 10 -14 days • If symptoms persist or worsen after 48 to 72 hours of antibiotic therapy, the patient should be revaluated for an alternative antibiotic • Patients with multiple treatment failures should referred to a specialist Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Acute Pharyngitis: Pathophysiology • Pharyngitis is an infection that cause pain and inflammation of the oropharynx or nasopharynx • Viral pharyngitis is more common than bacterial pharyngitis • Acute Bacterial Pharyngitis is most frequently caused by Group A βhemolytic streptococci (GABHS) • Rare but severe complications can occur with untreated GABHS infections • Rheumatic fever • Acute glomerulonephritis • Mechanism of Group A β-hemolytic streptococci is not well defined Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Acute Pharyngitis: Most Common Pathogens • Virus are the most common cause of acute pharyngitis • Acute Bacterial Pharyngitis • GABHS- most common • Less common causes • • Groups C and G Streptococcus Corynebacterium diphtheria Neisseria gonorrhoeae Mycoplasma pneumonia Arcanobacterium haemolyticum Yersinia enterocolitica Chlamydia pneumoniae Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Acute Pharyngitis: Clinical Presentation • GABHS symptoms • • • Sore throat Pain on swallowing Fever Headache GI Symptoms • Nausea • Vomiting • Abdominal pain • Erythema/inflammation of the tonsils and pharynx ± patchy exudates • Enlarged, tender lymph nodes • Red swollen uvula • Petechiae on the soft palate • Scarlatiniform rash • Viral Pathogen Symptoms • Conjunctivitis • Coryza • Cough • Laboratory Tests • Throat Swab Culture • Rapid antigen-detection test Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Acute Pharyngitis: Treatment Overview • Evaluate patients symptoms • Preform Rapid antigen-detection test and/ or throat culture in patients with high suspicion of GABHS infection • Prescribe antibiotics based on above results • Delaying antibiotic therapy for bacterial pharyngitis while awaiting culture results does not affect the risk of complications • Early initiation of antibiotics causes a faster resolution of symptoms • Penicillin and amoxicillin are the drugs of choice for GABHS pharyngitis in non allergic patients Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Acute Pharyngitis Treatment: Nonpharmacological / Supportive Care • Systemic pain relief • Acetaminophen • Nonsteroidal Anti-inflammatory Drugs (NSAIDs) like ibuprofen • Local pain relief (lozenges/ throat sprays) • Menthol • Topical anesthetics • Steroid use should be discouraged due to lack of benefit and increased risk of adverse effects Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

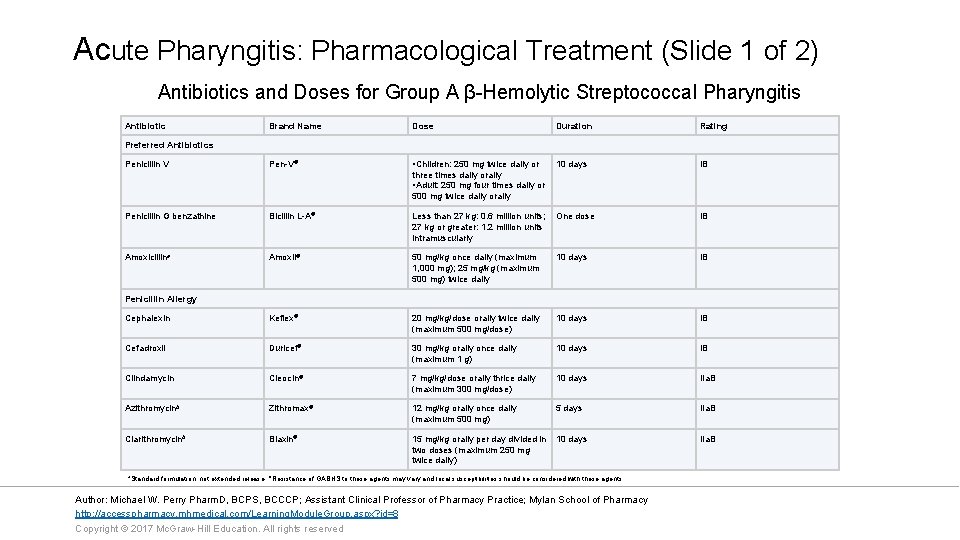
Acute Pharyngitis: Pharmacological Treatment (Slide 1 of 2) Antibiotics and Doses for Group A β-Hemolytic Streptococcal Pharyngitis Antibiotic Brand Name Dose Duration Rating Pen-V® • Children: 250 mg twice daily or 10 days IB Preferred Antibiotics Penicillin V three times daily orally • Adult: 250 mg four times daily or 500 mg twice daily orally Penicillin G benzathine Bicillin L-A® Less than 27 kg: 0. 6 million units; One dose 27 kg or greater: 1. 2 million units intramuscularly IB Amoxicillina Amoxil® 50 mg/kg once daily (maximum 1, 000 mg); 25 mg/kg (maximum 500 mg) twice daily 10 days IB Cephalexin Keflex® 20 mg/kg/dose orally twice daily (maximum 500 mg/dose) 10 days IB Cefadroxil Duricef® 30 mg/kg orally once daily (maximum 1 g) 10 days IB Clindamycin Cleocin® 7 mg/kg/dose orally thrice daily (maximum 300 mg/dose) 10 days IIa. B Azithromycinb Zithromax® 12 mg/kg orally once daily (maximum 500 mg) 5 days IIa. B Clarithromycinb Biaxin® 15 mg/kg orally per day divided in 10 days two doses (maximum 250 mg twice daily) Penicillin Allergy a. Standard formulation, not extended release. b. Resistance of GABHS to these agents may vary and local susceptibilities should be considered with these agents. Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved IIa. B

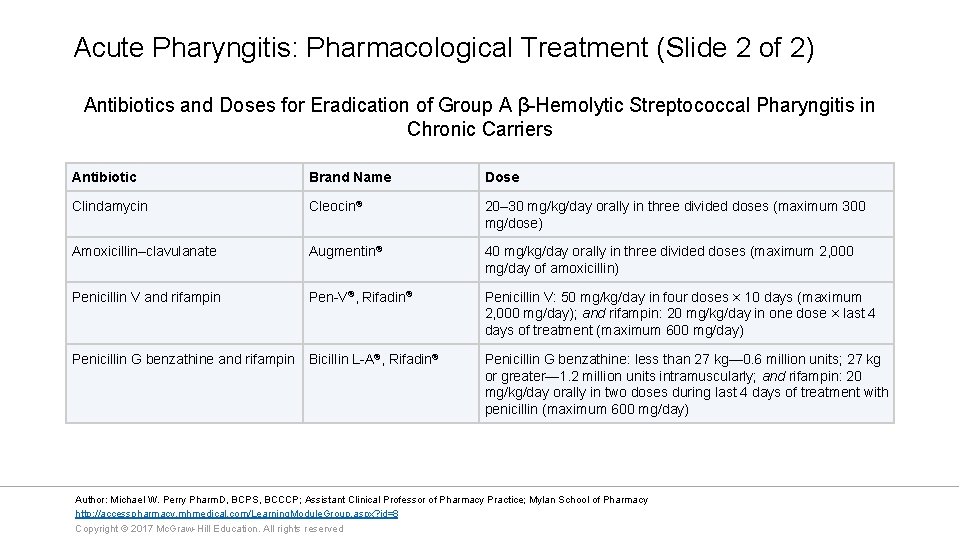
Acute Pharyngitis: Pharmacological Treatment (Slide 2 of 2) Antibiotics and Doses for Eradication of Group A β-Hemolytic Streptococcal Pharyngitis in Chronic Carriers Antibiotic Brand Name Dose Clindamycin Cleocin® 20– 30 mg/kg/day orally in three divided doses (maximum 300 mg/dose) Amoxicillin–clavulanate Augmentin® 40 mg/kg/day orally in three divided doses (maximum 2, 000 mg/day of amoxicillin) Penicillin V and rifampin Pen-V®, Rifadin® Penicillin V: 50 mg/kg/day in four doses × 10 days (maximum 2, 000 mg/day); and rifampin: 20 mg/kg/day in one dose × last 4 days of treatment (maximum 600 mg/day) Penicillin G benzathine and rifampin Bicillin L-A®, Rifadin® Penicillin G benzathine: less than 27 kg— 0. 6 million units; 27 kg or greater— 1. 2 million units intramuscularly; and rifampin: 20 mg/kg/day orally in two doses during last 4 days of treatment with penicillin (maximum 600 mg/day) Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Acute Pharyngitis: Overall Monitoring • Fever and other symptoms resolve within 3 to 4 days of onset • Resolve faster with the initiation of antibiotics in patients with bacterial infections • Duration of treatment is generally 10 days • Microbiologic eradication will occur in 48 to 72 hours, which aids in decreasing transmission • Repeat throat cultures can be ordered on patients with persistent symptoms Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Summary • Upper respiratory tract infections are a frequent and common infection that cause patients to seek help from healthcare providers • The main causative pathogens for upper respiratory tract infections are viruses • Proper identification and diagnosis of bacterial infections is required to appropriately prescribe antibiotics Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

References • Frei C, Frei B. Chapter 86. Upper Respiratory Tract Infections. In: Di. Piro JT, Talbert RL, Yee GC, Matzke GR, Wells BG, Posey L. eds. Pharmacotherapy: A Pathophysiologic Approach, 9 e. New York, NY: Mc. Graw-Hill; 2014. • Lieberthal AS, Carroll AE, Chonmaitree T, et al. The diagnosis and management of acute otitis media. Pediatrics. 2013; 131(3): e 964 -e 999 • Chow AW, Benninger MS, Brook I, et al. IDSA clinical practice guideline for acute bacterial rhinosinusitis in children and adults. Clin Infect Dis. 2012; 54(8): 1042. • Shulman ST, Bisno AL, Clegg HW, et al. Clinical practice guideline for the diagnosis and management of group A streptococcal pharyngitis: 2012 update by the Infectious Diseases Society of America. Clin Infect Dis 2012; 55: e 86 -e 102. Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved