Infectious Disease I Bone and Joint Infections Courses

Infectious Disease I: Bone and Joint Infections Courses in Therapeutics and Disease State Management Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Learning Objectives (Slide 1 of 3) • Compare the epidemiology of osteomyelitis when categorized by the mechanism of the organism reaching the bone • Differentiate the characteristics of infectious arthritis • Contrast the most common characteristics of hematogenous osteomyelitis • Compare the pathophysiology of osteomyelitis by age group • Select the most frequent organisms causing hematogenous osteomyelitis Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Learning Objectives (Slide 2 of 3) • Contrast the most common characteristics of contiguousspread osteomyelitis • Discuss the organism sources of infectious arthritis • Differentiate the risk factors for developing adult infectious arthritis • Compare the etiologies of adult infectious arthritis subgroups • Design a laboratory monitoring strategy for bone and joint infections Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Learning Objectives (Slide 3 of 3) • Contrast the usefulness of culture sites with bone and joint infections • Choose the preferred duration of therapy for patients with bone and joint infections • Discuss the patient selection characteristics for oral antibiotic regimens treating osteomyelitis • Critique the use of oral fluoroquinolones in the treatment of bone and joint infections • Construct an empiric antibiotic regimen for different patient categories with bone or joint infections Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Required Reading Armstrong EP, Shehab Z. Chapter 96. Bone and Joint Infections. In: Di. Piro JT, Talbert RL, Yee GC, Matzke GR, Wells BG, Posey L. eds. Pharmacotherapy: A Pathophysiologic Approach, 9 e. New York, NY: Mc. Graw-Hill; 2014. Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Topic Overview • Bone and Joint infections are divided into two distinct disease processes with different infecting organisms, signs and symptom • Septic or infective arthritis is the infection of a joint or synovial fluid • Osteomyelitis is the infection of a bone • Early initiation of antibiotic therapy and prolonged courses are required to reduce long term morbidity Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Osteomyelitis: Overview • Classification • Manner of a acquisition • Seeding or direct inoculation of microorganism via the blood into the bone is considered hematogenous osteomyelitis • Spread of microorganisms from adjacent soft tissues and joints is considered contiguous osteomyelitis • Direct inoculation of microorganism via puncture wounds, trauma, or surgery is considered inoculation osteomyelitis • Duration • Acute osteomyelitis has a duration of days to weeks • Chronic osteomyelitis has a duration of weeks to months Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Osteomyelitis: Pathophysiology • Hematogenous • Contiguous • Inoculation Link to figure of cross section of normal bone Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved
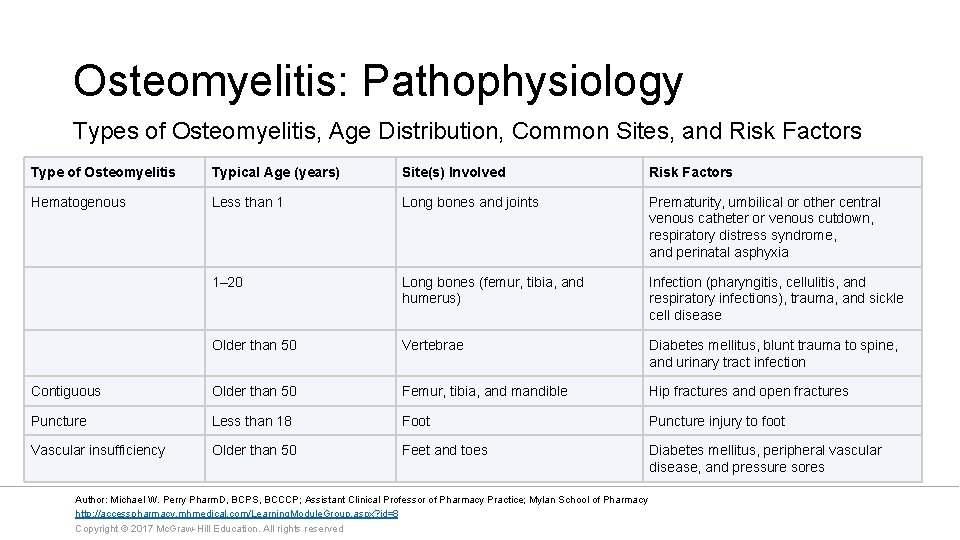
Osteomyelitis: Pathophysiology Types of Osteomyelitis, Age Distribution, Common Sites, and Risk Factors Type of Osteomyelitis Typical Age (years) Site(s) Involved Risk Factors Hematogenous Less than 1 Long bones and joints Prematurity, umbilical or other central venous catheter or venous cutdown, respiratory distress syndrome, and perinatal asphyxia 1– 20 Long bones (femur, tibia, and humerus) Infection (pharyngitis, cellulitis, and respiratory infections), trauma, and sickle cell disease Older than 50 Vertebrae Diabetes mellitus, blunt trauma to spine, and urinary tract infection Contiguous Older than 50 Femur, tibia, and mandible Hip fractures and open fractures Puncture Less than 18 Foot Puncture injury to foot Vascular insufficiency Older than 50 Feet and toes Diabetes mellitus, peripheral vascular disease, and pressure sores Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Osteomyelitis: Pathophysiology, Most Common Pathogens • Contiguous • With vascular insufficiency • Adults > 50 • • • S. aureus (MRSA) Enterobacteriaceae Pseudomonas aeruginosa Enterococcus spp. Anaerobes • without vascular insufficiency • Adult > 50 • S. aureus • Hematogenous • Neonates • S. aureus • E. coli • Group B streptococci • Pre-pubertal Children • S. aureus • Elderly • S. aureus • E. coli • Inoculation • S. aureus • Pseudomonas aeruginosa • Gram negative pathogens Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Osteomyelitis: Clinical Presentation Signs and Symptoms • Systemic • Fevers • Chills • Malaise • Localized • • • Pain or tenderness Edema Erythema Inflammation Decreased range of motion Laboratory tests • Elevated WBC • Elevated inflammatory markers • Erythrocyte sedimentation rate (ESR) • C-reactive protein (CRP) • Positive blood cultures • Bone biopsy cultures • Bone changes on radiograph • Magnetic resonance imaging • Technetium scans Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Osteomyelitis: Treatment Overview • Antibiotics must have adequate bone concentrations • Duration of Antibiotics • 4 to 6 weeks • May be able to switch to oral antibiotics • Monitoring for Efficacy • Clinical improvement of signs in symptoms in 48 to 72 hours • Reduction in CRP 1 week after therapy • Observe for adverse effects associated with long term antimicrobial therapy Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Osteomyelitis: Nonpharmacological Treatment • Surgical drainage of abscesses • Hyperbaric oxygen Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved
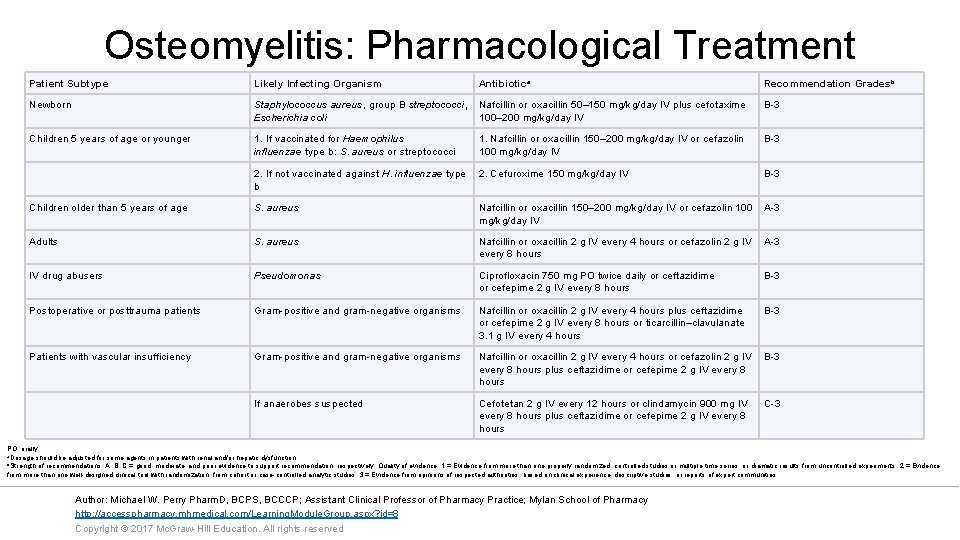
Osteomyelitis: Pharmacological Treatment Patient Subtype Likely Infecting Organism Antibiotica Newborn Staphylococcus aureus, group B streptococci, Nafcillin or oxacillin 50– 150 mg/kg/day IV plus cefotaxime Escherichia coli 100– 200 mg/kg/day IV B-3 Children 5 years of age or younger 1. If vaccinated for Haemophilus influenzae type b: S. aureus or streptococci B-3 1. Nafcillin or oxacillin 150– 200 mg/kg/day IV or cefazolin 100 mg/kg/day IV 2. If not vaccinated against H. influenzae type 2. Cefuroxime 150 mg/kg/day IV b Recommendation Gradesb B-3 Children older than 5 years of age S. aureus Nafcillin or oxacillin 150– 200 mg/kg/day IV or cefazolin 100 A-3 mg/kg/day IV Adults S. aureus Nafcillin or oxacillin 2 g IV every 4 hours or cefazolin 2 g IV A-3 every 8 hours IV drug abusers Pseudomonas Ciprofloxacin 750 mg PO twice daily or ceftazidime or cefepime 2 g IV every 8 hours B-3 Postoperative or posttrauma patients Gram-positive and gram-negative organisms Nafcillin or oxacillin 2 g IV every 4 hours plus ceftazidime or cefepime 2 g IV every 8 hours or ticarcillin–clavulanate 3. 1 g IV every 4 hours B-3 Patients with vascular insufficiency Gram-positive and gram-negative organisms Nafcillin or oxacillin 2 g IV every 4 hours or cefazolin 2 g IV B-3 every 8 hours plus ceftazidime or cefepime 2 g IV every 8 hours If anaerobes suspected Cefotetan 2 g IV every 12 hours or clindamycin 900 mg IV every 8 hours plus ceftazidime or cefepime 2 g IV every 8 hours C-3 PO, orally. a. Dosage should be adjusted for some agents in patients with renal and/or hepatic dysfunction. b. Strength of recommendations: A, B, C = good, moderate, and poor evidence to support recommendation, respectively. Quality of evidence: 1 = Evidence from more than one properly randomized, controlled studies or multiple time series; or dramatic results from uncontrolled experiments. 2 = Evidence from more than one well-designed clinical trial with randomization, from cohort or case-controlled analytic studies. 3 = Evidence from opinions of respected authorities, based on clinical experience, descriptive studies, or reports of expert communities. Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Septic Arthritis: Overview • An inflammatory reaction within the joint space • Joint Infection that can be caused by several different microorganisms • Classification by manner of a acquisition • Seeding or direct inoculation of microorganism via the blood into the bone is considered hematogenous spread • Spread of microorganisms from adjacent soft tissues and joints is considered contiguous spread • Direct inoculation of microorganism via puncture wounds, trauma, or surgery is considered inoculation spread Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved
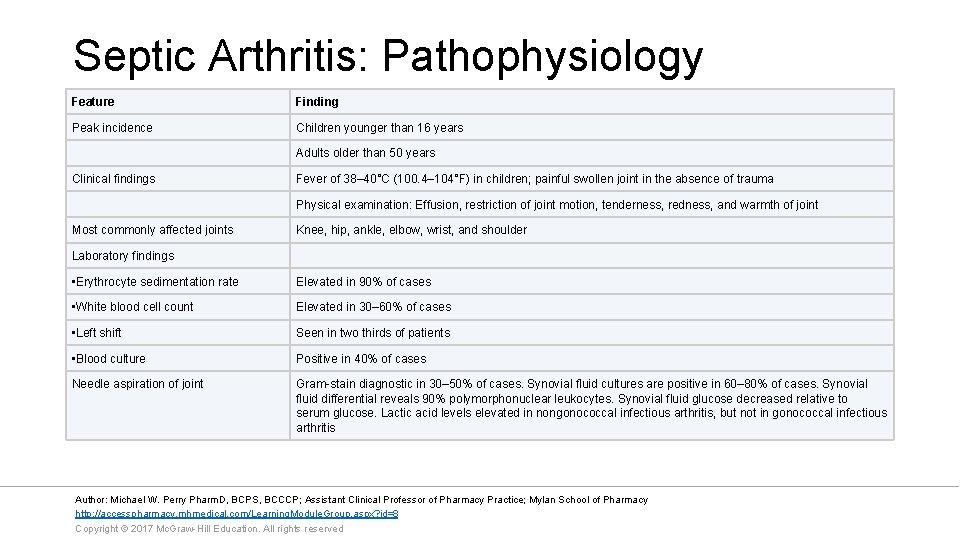
Septic Arthritis: Pathophysiology Feature Finding Peak incidence Children younger than 16 years Adults older than 50 years Clinical findings Fever of 38– 40°C (100. 4– 104°F) in children; painful swollen joint in the absence of trauma Physical examination: Effusion, restriction of joint motion, tenderness, redness, and warmth of joint Most commonly affected joints Knee, hip, ankle, elbow, wrist, and shoulder Laboratory findings • Erythrocyte sedimentation rate Elevated in 90% of cases • White blood cell count Elevated in 30– 60% of cases • Left shift Seen in two thirds of patients • Blood culture Positive in 40% of cases Needle aspiration of joint Gram-stain diagnostic in 30– 50% of cases. Synovial fluid cultures are positive in 60– 80% of cases. Synovial fluid differential reveals 90% polymorphonuclear leukocytes. Synovial fluid glucose decreased relative to serum glucose. Lactic acid levels elevated in nongonococcal infectious arthritis, but not in gonococcal infectious arthritis Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Septic Arthritis: Pathophysiology, Most Common Pathogens • Overall • Staphylococcus aureus • Streptococcal infection • Gram negative pathogens • E. coli • Pseudomonas aeruginosa • Specific Groups • Neonates • S. aureus • Group B streptococci • Gram negative pathogens • Pre-pubertal Children • S. aureus • Streptococcal infection • IV drug abusers • Pseudomonas aeruginosa Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Septic Arthritis: Clinical Presentation Signs and Symptoms • Systemic • Fevers • Chills • Malaise • Localized • • • Joint pain or tenderness Edema Erythema Inflammation Decreased range of motion Laboratory tests • Elevated WBC is rare • Elevated inflammatory markers are less common • Erythrocyte sedimentation rate (ESR) • C-reactive protein (CRP) • Positive blood cultures • Joint aspiration fluid • Presence of purulent fluid • Gram stain • Culture • Prosthetic joint material cultures Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Septic Arthritis: Treatment Overview • Antibiotics must have adequate synovial fluid concentrations • Duration of Antibiotics • 2 to 3 weeks • May be able to switch to oral antibiotics • Clinical improvement of signs in symptoms in is generally rapid after initiation of antibiotic therapy and joint aspiration Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Septic Arthritis: Nonpharmacological Treatment • Closed-needle aspiration is recommended for all infected joints except the hip • Joint rest • Passive range of motion exercises once joint pain subsides Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Septic Arthritis: Pharmacological Treatment • Infants < 1 month of age • Nafcillin or Oxacillin Plus • 3 rd generation cephalosporin • Children <5 years of age immunized for Hib • Children >5 years of age and adults • MSSA suspected • Nafcillin, Oxacillin, or Cefazolin • MRSA suspected • Clindamycin, Vancomycin, or Linezolid • Nafcillin, Oxacillin, or Cefazolin Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved
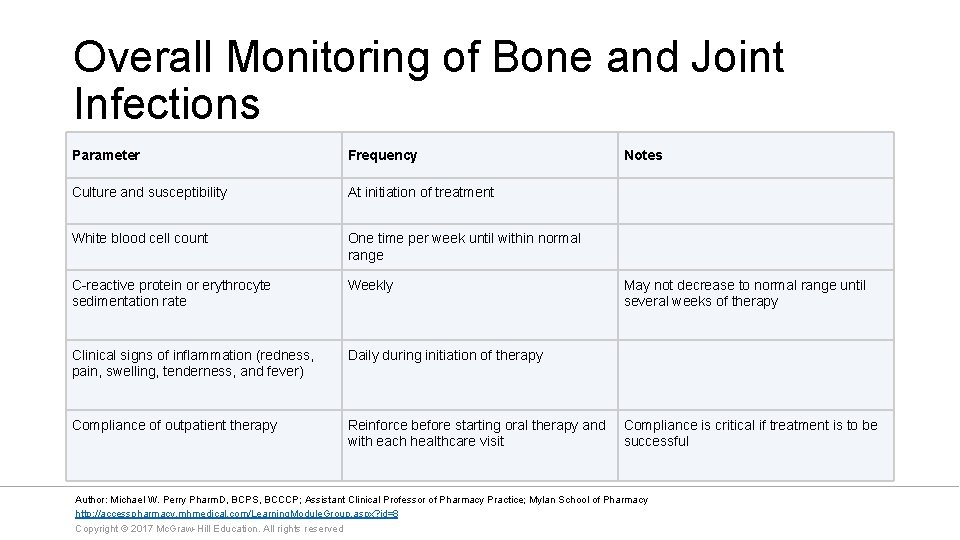
Overall Monitoring of Bone and Joint Infections Parameter Frequency Notes Culture and susceptibility At initiation of treatment White blood cell count One time per week until within normal range C-reactive protein or erythrocyte sedimentation rate Weekly Clinical signs of inflammation (redness, pain, swelling, tenderness, and fever) Daily during initiation of therapy Compliance of outpatient therapy Reinforce before starting oral therapy and Compliance is critical if treatment is to be with each healthcare visit successful May not decrease to normal range until several weeks of therapy Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Summary • Osteomyletitis and septic arthritis are infections of the bone and joints respectively • S. aureus is the most common pathogen • Intravenous Antibiotics • Bone and joint penetration must be considered • Narrow antibiotics based on cultures and sensitivities • Duration of antibiotics • Osteomyelitis 4 to 6 weeks • Septic Arthritis 2 to 3 weeks • Initiate oral antibiotics when appropriate Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Reference Armstrong EP, Shehab Z. Chapter 96. Bone and Joint Infections. In: Di. Piro JT, Talbert RL, Yee GC, Matzke GR, Wells BG, Posey L. eds. Pharmacotherapy: A Pathophysiologic Approach, 9 e. New York, NY: Mc. Graw-Hill; 2014. Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved
- Slides: 24