Infectious Agents That Cause Diarrhea Bacteria Aeromonas hydrophilia

Infectious Agents That Cause Diarrhea Bacteria Aeromonas hydrophilia Bacteroides fragilis Bacillus cerus Campylobacter jejuni Clostridium difficile Escherichia coli Mycobacterium avium complex Plesiomonos shigelloides Salmonells Shigella Staphyloccocus aureus Vibrio cholerae 01/139 Yersinia enterocolitica

Infectious Agents That Cause Diarrhea Viruses Astrovirus Calcivirus Coronavirus Cytomegalovirus Enteric adenovirus Norwalk virus Picarnovirus Rotavirus Parasites Balantidium coli Blastocystic hominis Cryptosporidium Dientamoeba fragilis Entamoeba species Enterocytozoon bieneusi Giardia lamblia Isospora belli Microsporidia species

Salmonella l l l Gram neg bacilli in Enterobacteriaceae family Three primary groups. S. typhi-enteric fever S. cholerasius S. enteritidis (>2, 000 serotypes) Transmission-poultry, water, pets, fecal-oral Incidence- <5 y >70 years immunosupression, SSD, Incubation- 6 -72 hours
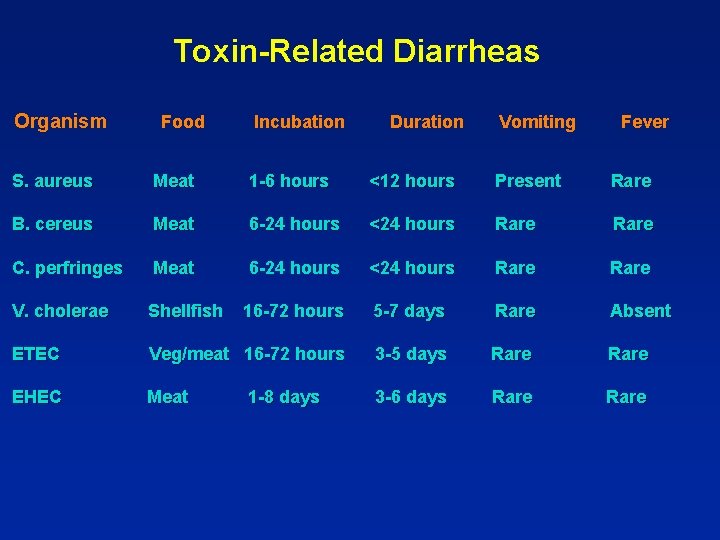
Toxin-Related Diarrheas Organism Food Incubation Duration Vomiting Fever S. aureus Meat 1 -6 hours <12 hours Present Rare B. cereus Meat 6 -24 hours <24 hours Rare C. perfringes Meat 6 -24 hours <24 hours Rare V. cholerae Shellfish 16 -72 hours 5 -7 days Rare Absent ETEC Veg/meat 16 -72 hours 3 -5 days Rare EHEC Meat 3 -6 days Rare 1 -8 days

Enteric Pathogens in HIV Children Parasites Cryptosporidium Giardia lamblia Isospora belli Entamoeba histolytica Microsporidium Fungi Candida albicans Histoplasma capsulatum

Enteric Pathogens in HIV-Children Bacteria Salmonella Shigella flexneri Campylobacter jejuni Clostridium difficile Viruses Herpes Simplex Rotavirus Adenovirus Corona virus Mycobacteria Mycobacterium avium Mycobacterium bovis Cytomegalovirus Norwalk virus Astrovirus Picarnovirus

Rotavirus l l l Major cause of severe diarrhea in children 1/3 of hospitilizations for diarrheal illnesses Peak incidence 3 -15 months, winter, west-east spread Transmission- fecal-oral route Decreased absorbtion with secondary lactose intolerance Dx- EIA/latex agglutionation kits

Rotavirus l Clinical- incubation 48 hrs (1 -7 days) frequent vomiting (67 -90%) fever (66+%) mild-profuse watery diarrhea 4 -8 days mild elevation LFT’s l Viral shedding 1 -5 days l Treatment-supportive oral immunoglobulins ?

Enteric Adenovirus l l l l l Second most common cause severe diarrhea Serotypes 40, 41 Do not cause resp symptoms Incidence- younger than 2 years, year round Fecal oral route transmission Incubation period 8 -10 days 5 -12 days diarrhea 2 -3 days low grade fever and vomiting Treatment-supportive

Norwalk Virus l l l l Small round virus Named for geographic location of outbreak Contaminated food or water Fecal-oral transmission Incubation 12 -48 hours Vomiting more prominant than diarrhea Duration less than 48 hours Treatment-supportive

Escherichia coli l Enteropathogenic E coli (EPEC) Neonates and < 2 years Severe watery diarrhea Causes chronic diarrhea/ FTT Non-invasive, non-toxin Incubation 10 hrs-6 days

Escherichia coli l Enterotoxigenic E coli (ETEC) occurs in all ages food, water contamination self limited illness, 3 -5 days watery stools and abdominal cramps enterotoxin production incubation-16 -72 hours Treatment-Septra/Cipro/Doxycycline

Escherica coli l Enteroinvasive E coli (EIEC) occurs all ages dysentary picture fever, bloody diarrhea invasion intestinal epith cells incubation-2 -4 days Treatment-TMP-SMX

Escherica coli l Enterohemorrhagic E coli (EHEC) occurs all ages nonbloody diarrhea fever, abd pain, hemorrhagic colitis Shiga-like toxin incubation 1 -8 days poorly cooked meats Treatment- +/- trimeth-sulfa

Escherica coli l E coli 0157: H 7 prototype of EHEC organisms Hemorrhagic colitis Hemolytic Uremic Syndrome 5 -10% ( anemia, dec plt, renal failure) Thrombotic thrombocytopenic purpura intussusception, IBD, ischemic colitis (does not ferment sorbitol)

Shigella l l l Gram neg bacilli in Enterobacteraceae family Four species. S. sonnei - 50% cases in US S. flexneri- 30 -40% cases in US S. dysenteriae- common in Africa/India S. boydii- uncommon Transmission via fecal oral mode Incidence- summer/fall, 1 -4 yrs, day care, Cytoxin producing and invasive

Shigella l l Clinical- 2 -4 days incubation fever, abd pain, tenesmus, systemic toxicity, seizures (10 -40%), stool-watery, mucoid, bloody duration 4 -5 days Diagnosis-culture Treatment- AMP, TMP-SMX tetra (5 d) Carriage rare outside 4 weeks Rare sequelae-HUS, Reiter’s synd, ekeri synd

Campylobacter l l Comma shaped Gram neg bacilli Two species. C. jejuni-causes gastroenteritis C. fetus- systemic illness in neonates Increasing incidence esp day care Transmission-fecal oral, contaminated poultry untreated milk, water

Campylobacter l l Clinical-incubation 1 -7 days fever, abd pain, malaise stool-bloody, watery duration 5 -7 days (10 -20% relapse) Treatment-Erythromycin (5 -7 d) Carriage 2 -3 weeks, (1 -2 days w/rx) Diagnosis-culture gram stain-motile curved rods Rare sequelae-arthritis, GBS, Reiter’s,

It Happens l l l 1. 5 Billion episodes/year worldwide 5 million deaths/year worldwide In the U. S. 21 -37 million episodes children < 5 y 10 % of these lead to HCP visits 220, 000 hospitilizations (10. 6%) 325 -425 children die (mostly <1 year) ? immunizations

Salmonella l l Clinical-asymptomatic carriage; bacteremia gastroenteritis; enteric fever, focality Gastroenteritis-watery, bloody diarrhea, abd pain, cramps, tenesmus Enteric Fever-fever, HA, malaise, abd pain, h-s megaly, rose spots, diarrhea Treatment-Gastroenteritis in <3 m, or immunosuprression, severe colitis amp, amox, TMP-SMX, cefotax

Salmonella l l Carriage- 45%+ at 12 weeks (<5 y) 1 % at 1 year prolonged with antibiotic use Vaccines-S. typhi (parental vs oral) indicated for travel to Asia, Africa

INFECTIOUS DIARRHEA Do you know what you just stepped in? It happens. . . Forrest Gump-1994

Clostridium difficile l l l Spore forming obligate anerobe, G+ bacilli Two toxins (A/B) have been found Isolated from soil, hospital environements Colonization in neonates as high as 50% Risk factorsdiminished barrier effect of normal flora Pnc, clinda, cephalosporins

Clostridium difficile l l l Clinical-incubation is unknown Pseudomembranous colitis- diarrhea abd cramps, fever, systemic toxicity Therapy-d/c antimicrobials, po vancomycin ? IV/po Flagyl, cholestyramine 10 -20% relapse-IVIG for chronic Diagnosis-isolation and toxin testing (EIA)

Evaluation of the Patient Questionfever, cramps bloody stool antibiotics mult cases immunosup Suggestscolitis, ileitis Shig, EIEC, bacteria C. difficile inc <6 h-S. aureus B. cereus inc>6 h-C. perf, Vibrio Salmonela, viral parasites

Giardia lamblia l l l Flagellate protozoa-infective cyst form Infection limited to small intestine, biliary tree Most common cause parasitic diarrhea in US Risk factors-agammoglobulinemia CF, pancreatitis, achlorhydria Transmission-water, fecal-oral

Giardia l l l Clinical acute-watery foul smelling stool, abd pain chronic-malabsorbtion, steatorrhea, FTT carrier state-asymptomatic (1 -20%) Incubation-1 -4 weeks Therapy-Furazolidine, Metronidazole, Quinacrine

Cryptosporidium parvum l l l l Coccidian protazoan-cyst form infective Transmission from infected water, birds, mammals, reptiles Incidence-inc in young, immunosuppressed Incubation-5 -21 days Usually self limited 1 -20 days Frequent watery diarrhea, fever, anorexia Immunosuppressed-chronic, FTT, dissemination, death Rx-azythro, IG, paromomycin

SINUSITIS l Clinical Diagnosis URI > 10 days Night cough > 10 days Purulent nasal discharge with fever Facial, eye pain Eye swelling w/o erythems

Sinusitis l Radiologic criteriaplain x-rays complete opacification mucosal thickening > 4 mm air-fluid levels

Sinusitis l Indications for CT Recurrent problems Persistent infection Complications-CNS/Orbital l Indications for Aspiration Clinical failure Complicated infections Immunosuppressed patient
- Slides: 32