Infections of Nervous System Encephalitis Meningitis Encephalitis Severe




























- Slides: 34

Infections of Nervous System Encephalitis Meningitis

Encephalitis • Severe inflammation of the brain • Usually caused by a mosquito-borne or a tic -borne virus • Can also be caused by: – Ingestion of infected goat’s milk – Accidental injection or inhalation of the virus

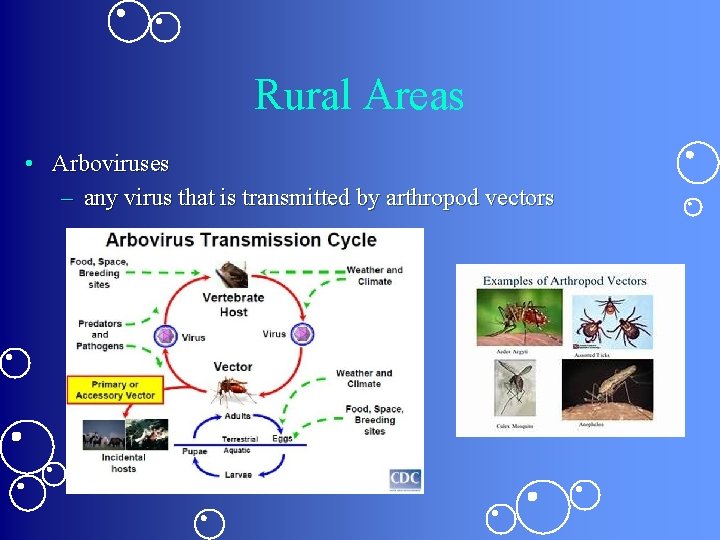
Rural Areas • Arboviruses – any virus that is transmitted by arthropod vectors

Urban Areas • Usually caused by enteroviruses – named by their transmission-route through the intestine – often found in the respiratory secretions and stool of an infected person – Types • Coxsackievirus • Echovirus • Poliovirus – Historically, poliomyelitis was the most significant disease caused by an enterovirus

Other viruses implicated • • • Herpesvirus Mumps HIV Adenoviruses Demyelinating diseases following: – Measles – Varicella – Rubella – Vaccination

Pathophysiology • Intense lymphocytic infiltration of brain tissues and leptomeninges – arachnoid and pia mater – the two innermost layers of tissue that cover the brain and spinal cord • Leads to: – Cerebral edema, degeneration of the brain’s ganglion cells, & diffuse nerve cell destruction

Signs & Symptoms • Fever of 102 -105 (38. 8 -40. 6) • Headache • Vomiting

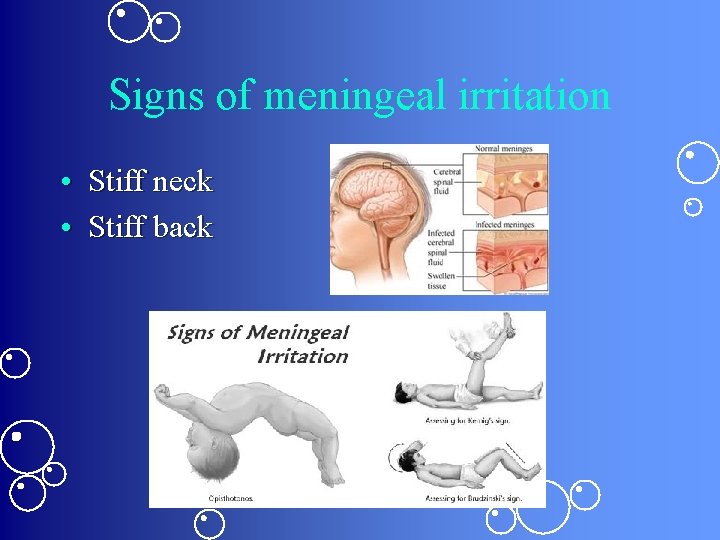
Signs of meningeal irritation • Stiff neck • Stiff back

Signs of neuron damage • • • Drowsiness Coma Paralysis Seizures Ataxia Organic psychoses

Diagnostics • CSF or blood analysis to identify the causative virus • Technetium-99 scan may show localized abnormalities • CT scan may disclose localized abnormalities

Treatment • Antiviral agents such as acyclovir • Anticonvulsants to prevent or control seizures • Furosemide or Mannitol to reduce cerebral swelling • Sedative to alleviate restlessness • ASA or Tylenol to relieve headache and reduce fever • Fluids & lytes to prevent dehydration and electrolyte imbalance • Antibiotics for secondary infections

Nursing Actions • • Frequent neuro assessments Monitor I & O Position changes to avoid joint stiffness & neck pain ROM to prevent contractures Darkened room & decreased stimulation Maintain adequate nutrition Reassure patient & family that behavior changes caused by the condition usually disappear Frequent reorientation

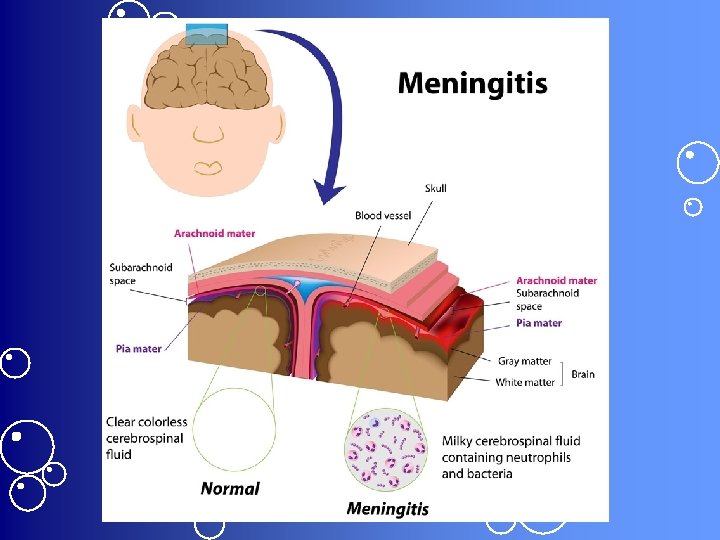
Meningitis • Brain & spinal cord become inflamed – Usually d/t bacterial infection • May involve all 3 layers of meninges – Dura mater – Arachnid mater – Pia mater


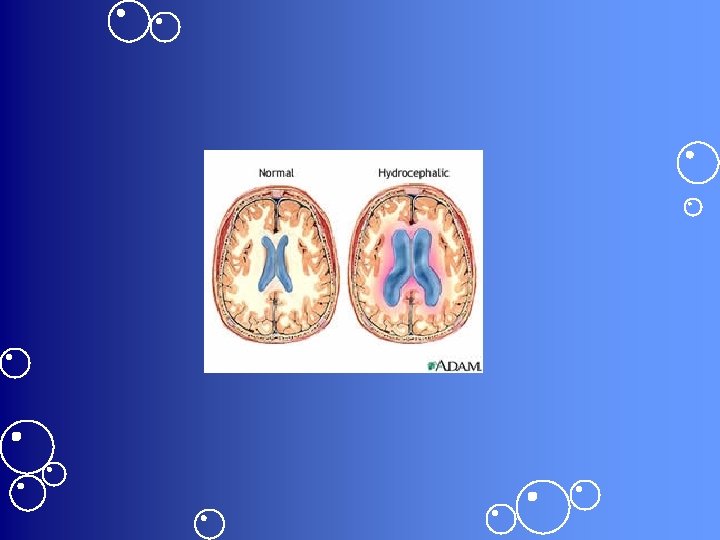
Promptness improves prognosis • If treated early, decreased risk of complications: – Increased ICP – Hydrocephalus – Cerebral infarction – Cranial nerve deficits • Optic neuritis • Deafness – Brain abscess – Seizures or coma

Etiology • Bacteremia – Pneumonia – Empyema – Osteomyelitis – Endocarditis • Aseptic – Virus or other organism • Sometimes no causative organism can be found

Other Infections Associated with Meningitis • • • Sinusitis Otitis media Encephalitis Myelitis Brain abscess – H flu – Strep Pneumonia – E Coli

Any Opening • May follow trauma or invasive procedures – Skull fx – Penetrating head wound – Lumbar puncture – Ventricular shunting

Routes of Entry 1. The blood • Most common 2. A direct opening between the CSF & the environment as a result of trauma 3. Along the cranial and peripheral nerves 4. Through the mouth or nose

Pathophysiology • Invading organism triggers an inflammatory response in the meninges • Neutrophils gather in the area & produce an exudate in the subarachnoid space – Causes the CSF to thicken • CSF flows less readily around the brain & spinal cord – Can block the arachnoid villi & further obstruct CSF flow leading to hydrocephalus


Exudate can also • Exacerbate the inflammatory response – Increases the pressure in the brain • Extend to the cranial and peripheral nerves – Triggering additional inflammation • Irritate the meninges – Disrupting their cell membranes – Causing edema

Consequences of Meningitis • • • Elevated ICP Engorged blood vessels Disrupted cerebral blood supply Possible thrombosis or rupture Cerebral infarction if ICP can’t be reduced Possible encephalitis – Secondary infection of the brain tissue

Aseptic Meningitis • Lymphocytes infiltrate the pia-arachnoid layers but usually not as severely as in bacterial meningitis – No exudate is formed • Makes this type of meningitis, self-limiting

Signs & Symptoms • Fever, chills, & malaise – d/t infection & inflammation • Headache & vomiting • Sometimes papilledema – Inflammation & edema of the optic nerve – Results from increased ICP

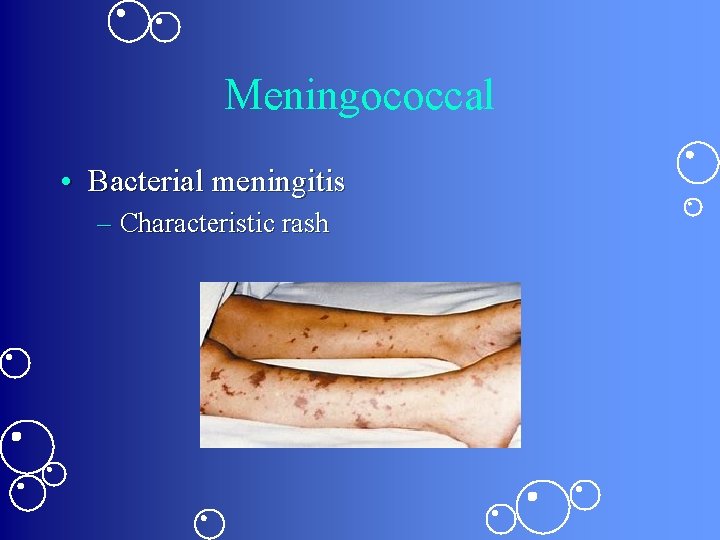
Meningococcal • Bacterial meningitis – Characteristic rash

Signs of neuron irritation • Nuchal rigidity • Positive Brudzinski’s & Kernig’s signs • Exaggerated and symmetrical deep tendon reflexes • Opisthotonos – In infants and children

You may also see these • Sinus arrhythmias d/t irritation of autonomic nerves • Irritability d/t increasing ICP • Photophobia, diplopia, and other visual problems d/t cranial nerve irritation • Delirium, deep stupor, & coma d/t increased ICP and cerebral edema

Diagnostics • LP-elevated CSF pressure from obstructed CSF outflow at the arachnoid villi • Cloudy or milky-white CSF • CSF – High protein levels – Positive Gram stain & culture • Cultures of blood, urine, and nose and throat secretions reveal the offending organism

Diagnostics, cont’d • CXR may reveal pneumonitis or lung abscess • Sinus and skull X-rays may identify paranasal sinusitis as the underlying infection or a skull fx as the mechanism for entrance of microorganisms • WBC count reveals leukocytosis

Treatment • • • Antibiotic therapy, usually for 2 weeks Digoxin to control arrhythmia Mannitol to decrease cerebral edema Anticonvulsant to prevent seizures Sedative to reduce restlessness Acetaminophen to relieve headache and fever

Supportive Measures • Bed rest • Fever reduction – Cooling blanket • Isolation if indicated – Family education

Nursing Actions • Frequent neuro assessments • Monitor for deterioration – Temperature increase, decreasing LOC, onset of seizures, altered respirations • Monitor fluid balance • Positioning • Maintain adequate nutrition & elimination • Maintain a quiet environment • Sterile technique for any dressing changes • Administer meds as indicated

Think of appropriate nursing diagnoses for patients with these infections