INFECTION PREVENTION Imarisha Maisha INFECTION PREVENTION It is






























- Slides: 34

INFECTION PREVENTION Imarisha Maisha

INFECTION PREVENTION § It is the collective effort made by health care providers and clients to prevent or minimize the risks of transmitting infections to clients or to other health care providers

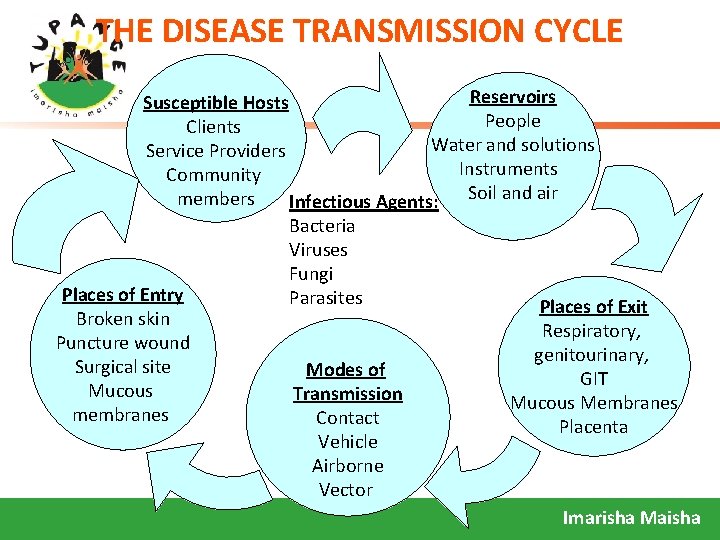
THE DISEASE TRANSMISSION CYCLE Reservoirs Susceptible Hosts People Clients Water and solutions Service Providers Instruments Community members Infectious Agents: Soil and air Bacteria Viruses Fungi Places of Entry Parasites Places of Exit Broken skin Respiratory, Puncture wound genitourinary, Surgical site Modes of GIT Mucous Transmission Mucous Membranes membranes Contact Placenta Vehicle Airborne Vector Imarisha Maisha

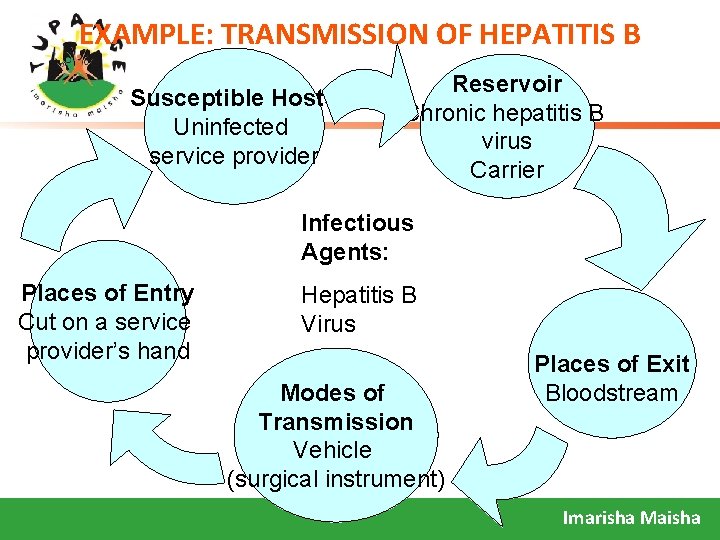
EXAMPLE: TRANSMISSION OF HEPATITIS B Susceptible Hosts Uninfected service provider Reservoir Chronic hepatitis B virus Carrier Infectious Agents: Places of Entry Cut on a service provider’s hand Hepatitis B Virus Modes of Transmission Vehicle (surgical instrument) Places of Exit Bloodstream Imarisha Maisha

ADVANTAGES OF INFECTION PREVENTION: § Prevents post procedure infections when providing clinical contraceptive methods (eg, IUCDs, implants) § Results in high-quality, safe services § Prevents infections in staff § Protects the community § Prevents the spread of antibiotic-resistant microorganisms § Lowers the cost of health care

UNIVERSAL PRECAUTIONS § A simple set of effective practices designed to protect health workers and patients from infection with a range of pathogens § Help break the disease-transmission cycle at the mode of transmission step § These practices are used when caring for all patients regardless of diagnosis.

UNIVERSAL PRECAUTIONS § Wash hands. § Decontaminate equipment and devices. § Use and dispose of needles and sharps safely (avoid recapping, especially two-handed). § Wear protective items. § Promptly clean up blood and body fluid spills. § Use safe disposal systems for waste collection and disposal.

HAND WASHING 1 Wash hands § After arriving at work § Before and after examining each client § After touching anything that might be contaminated § Before putting on gloves for clinical procedures § After removing gloves § After using the toilet or latrine § Before leaving work

HAND WASHING 2 After hand washing • Air dry hands • Dry with personal hand towel • Use electric drying machine • Avoid using a communal towel

USE OF GLOVES 1 Types of Gloves 1. Surgical gloves 2. Single-use examination gloves 3. Utility or heavy-duty household gloves

USE OF GLOVES 2 § Use separate pair of gloves for each patient § Wear correct size of gloves § Remove rings § Keep nails short

USE AND DISPOSAL OF NEEDLES AND OTHER SHARPS 1 Causes of Injuries with Sharps § Recapping hypodermic needles § Manipulating sharps before disposal § Accidentally sticking another staff member § Leaving sharps in areas where they are unexpected § Surgical procedures with limited visibility or in confined spaces § Handling or disposing of waste § Unexpected client motion during injections

USE AND DISPOSAL OF NEEDLES AND OTHER SHARPS 2 To Prevent Injuries Due to Sharps § Handle all sharps minimally after use § Use extreme care whenever sharps are handled § Dispose of sharps in puncture-resistant containers § Pass sharps using the “hands-free technique” § Do NOT recap needles

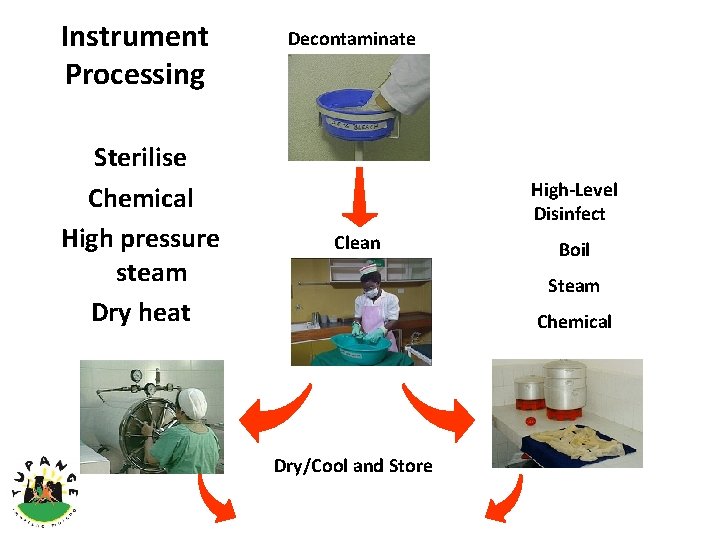
Instrument Processing Sterilise Chemical High pressure steam Dry heat Decontaminate High-Level Disinfect Clean Boil Steam Chemical Dry/Cool and Store

DECONTAMINATION § It is the first step in processing items § Makes items safer to handle and easier to clean § Soak items in a 0. 5% chlorine solution for 10 minutes immediately after use. Do not soak longer § Replace solution daily or when it becomes heavily contaminated

CLEANING § Removes blood, body fluids, tissue, and dirt § Reduces the number of microorganisms (including endospores) § Sterilization and HLD may not be effective without proper cleaning

STEPS OF CLEANING § Wear utility gloves, goggles, a mask, and protective eyewear § Scrub vigorously with a brush, detergent and water § Guard against injury from sharp objects § Hold items under the water, and be sure to get in the grooves, teeth, and joints § Rinse thoroughly to remove all detergent § Air-dry on a clean towel

STERILIZATION § Eliminate all microorganisms, including endospores § Recommended when items will come in contact with the bloodstream or tissue under the skin

DRY HEAT STERILIZATION § § § Temperatures 170 °C for 1 hour or 60 °C for 2 hours It is not necessary to open or disassemble items Start timing when the oven reaches the desired temperature

STEAM STERILIZATION (AUTOCLAVE) § Temperature: 121 °C Pressure: 106 k. Pa § Time: 20 minutes if unwrapped § 30 minutes if wrapped § Wrapped packs can be stored up to 1 week § Unwrapped items should be stored in a sterile or HLD container with a tight fitting lid

CHEMICAL STERILIZATION § Gluteraldehyde 2 -4% (e. g. cidex): soak for 10 hrs minimum § Formaldehyde 8%: soak for 24 hrs minimum After sterilization § Rinse with boiled water and air dry § Store in HLD container with a tight fitting lid

HIGH LEVEL DISINFECTION (HLD) § Eliminates all microorganisms, but does not kill all endospores § Use for items that will come in contact with broken skin or intact mucous membranes § Types: • Boiling • Use of chemicals

TIPS FOR HLD BY BOILING § Boil for 20 minutes in a cooking pot with a lid § Open or disassemble items § Do not add anything else to the pot after boiling begins § Articles must be completely immersed in water § Start timing when the water begins to boil § Store all items dry and use within one week

CHEMICALS FOR USE IN HLD Chlorine § Cheapest effective disinfectant § Effective against many microorganisms § Can be corrosive and irritating § Prepare a new solution daily § Soak instruments for 20 minutes and rinse in clean water before use

CHEMICALS FOR USE IN HLD Gluteraldehyde § Effective against many microorganisms § Not corrosive when used as directed § Irritating to people § Soak instruments for 20 minutes § Rinse in clan water before use § Use prepared solution for up to two weeks

HOUSEKEEPING General cleaning and maintenance of cleanliness • Reduces the number of microorganisms and thus, the risk of infections • Provides an appealing environment

GENERAL GUIDELINES FOR HOUSEKEEPING § Schedules should be posted and followed § Wear utility gloves and shoes when cleaning clientcare areas § Minimize scattering of dust and dirt § Scrub when cleaning § Wash from top to bottom § Change cleaning solutions when they are dirty

ROOM ARRANGEMENT • Put everything in the right place • Make all equipment and supplies needed accessible • Arrange the room so that you can move around easily and safely

WASTE DISPOSAL Types of Waste General waste – non hazardous, poses no risk of injury or infection Medical waste – material generated in a diagnosis, treatment, and/or immunization, including: Hazardous chemical waste – chemicals that are potentially toxic or poisonous

IMPORTANCE OF PROPER WASTE DISPOSAL § Minimizes spread of infection to health workers, patients and the local community § Reduced risk of accidental injury to those who handle the waste § Reduced likelihood of contamination of soil, ground water, etc. § Reduces attraction of insects and rodents § Reduced bad smell.

GUIDELINES FOR DISPOSAL OF MEDICAL WASTE § use washable, leak-proof containers § keep containers in convenient places § empty containers daily or when threequarters full § never put hands into containers § Always dispose of medical waste correctly § Wear utility gloves and shoes § Wash the gloves and your hands afterward

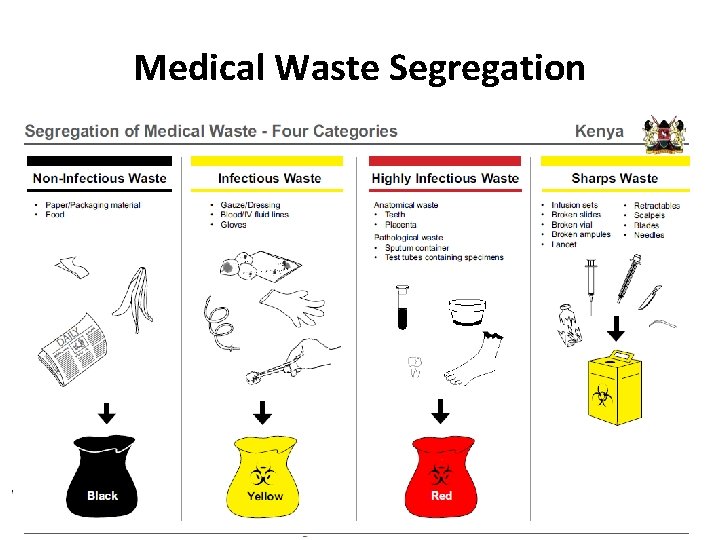
COLOUR CODING FOR WASTE SEGREGATION Category Example Colour of bin Non-infectious Papers, food cartons, Black Infectious Gloves, Yellow dressings, body fluids Highly infectious Anatomical waste Red

Medical Waste Segregation

DISPOSAL PROCEDURES FOR SHARPS § Dispose of all sharps in puncture-resistant containers § Close containers when three-quarters full § Burn or bury the container § Wash the gloves and hands afterward