Infection Prevention and Control in Primary Care Mary



















































- Slides: 55

Infection Prevention and Control in Primary Care Mary Hanrahan RGN, RM, MSc Nursing

Provide overview and update on. . Conditions SA / MSSA / MRSA / CA MRSA Clostridium difficile ESBL’s Norovirus Influenza (Pandemic) Practices / Health Care Environment Hand Hygiene PPE Sharps Decontamination / Reprocessing of equipment for minor surgery & other procedures Specimen Sampling

The waiting. . . The Adults. . . • Public health messages – leaflets / posters • Environmental furnishing & cleaning. . . • Choice of furniture • Cleaning solutions and frequencies. •

waiting cont’d. . . . The Kids…. • Ideally clean solid toys between each patient contact and weekly with detergent and water, dried and wiped with 70% alcohol wipe • Clean soiled toys between each patient contact. . . • Soft toys should be lost and never found again. • Clinical Practice & Waste Use and disposal of sharps Location of sharps boxes Disposal of nappies Blood and body fluid spills Other spills

• • • Many children in a waiting room setting may have or are incubating a community acquired infection e. g. RSV, rota virus, infected skin lesions, chicken pox Children more susceptible than adults Many have not developed immunity to common infectious fevers Sicker children less likely to play with the toys ‘Kid Incubators’ – not yet unwell will be attracted to toys.

The treatment room. . . Surfaces – ledges Medical equipment Waste Hand hygiene facilities Decontamination between patients

l. Staphylococcus aureus Found in nose of 30% of healthy people l. Can live on skin and in dust 11 days on a plastic patient chart > 12 days on a laminated tabletop - 9 days on a cloth curtain l. SA - Clinically can cause boils, abscesses, wound infections, septicaemia & food poisoning l. Susceptible conditions l. MRSA meticillin resistant staphylococcus aureus l. Screening l. MRSA patients - Burns, Post Surgery, Existing Skin for MRSA decolonisation for patients pre op / post discharge

MRSA in the GP surgery! A patient with chronic leg ulcer attends the surgery to have ulcer redressed – last laboratory report from an ulcer swab has identified – MRSA what actions do you take? A patient attends the surgery with a letter from a local hospital stating that the patient has been given a date for elective orthopaedic surgery requiring implant their preop screen denotes MRSA carrier – what actions do you take?

Primary Care Decolonisation – Oilatum Plus – Active substance - Triclosan Hospital Decolonisation - Stellisept MED Active substance and concentration in 100 g: 1. 0 g Didecyldimonium chloride This raw material is from the quaternary ammonium group (quats) -Quats are positively charged polyatomic ions with catalytic properties -Quats act by disrupting the cell membrane and proteins

PLV -SA Panton-Valentine Leukocidin (PVL) – toxin produced by <2% of S aureus. Causes recurrent skin and soft tissue infections – can be invasive e. g. necrotising haemorrhagic pneumonia – in otherwise health young people. Investigate in – recurrent boils/abscesses Nec SSTI, CA Nec H Pn. Standard swabs include anterior nares Rx – usual SA addition of Clind if PVL SA suspected.

• Spore forming bacterium - 'normal' bacteria in the gut of up to 3% of healthy adults, more common in babies - rarely causes problems. • People over 65 years are more susceptible. • Antibiotic use. • Bowel surgery. • Immunocompromised.

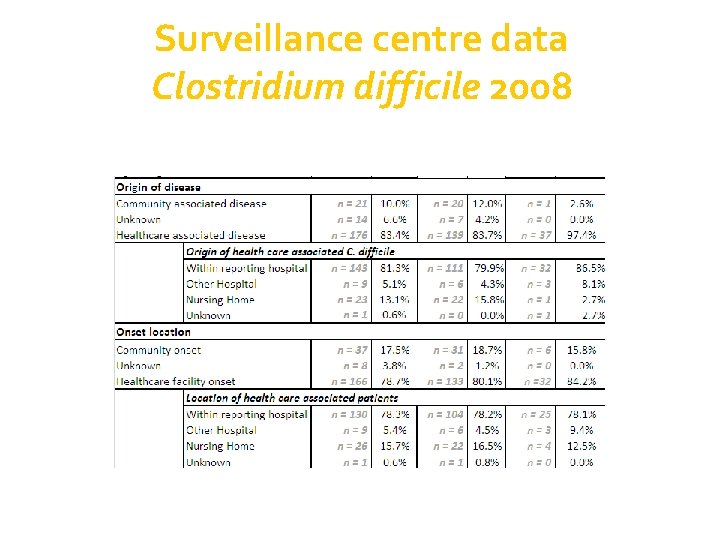
Surveillance centre data Clostridium difficile 2008

Antimicrobial Management Prescribing practices must adhere to guidance, be systematic and embedded in practice, take cognisance of patients hx Alert antimicrobials limited duration Targeted audit of use of ‘alert’ antibiotics Referral procedures to hospital

Risk Factors re Antibiotic therapy High Risk Broad spectrum antibiotics Cephalosporins Clindamycin Fluroquinalones Medium Risk Ampicillin Amoxycillin Co-trimoxazole Macrolides Tetracyclines Low Risk Aminoglycosides Metronidazole Rifampicin Vancomycin

Laboratory Specimens • Fresh is best! To avoid false negatives, transport to lab within 24 hours. • Over 24 hours- should be refrigerated at 4 C. • Over 48 hours- should be frozen at -20 C

ESBL-Producers First described in 1980 s, new class emerged early 2000 s Mostly E. Coli / Klebsiella Resistant to penicillins and cephalosporins Cross-resistance with other antibiotic classes Can be difficult to treat → only 1 oral antibiotic Colonise large bowel Concept of ‘high risk’ areas less relevant Large community reservoir (nursing homes)

ESBL Producers Most frequently causes UTI, which can progress to bacteraemia Outbreaks have occurred Risk factors and transmission mechanisms under investigation Has been detected on: Staff hands /Equipment (stethoscopes, electronic thermometers, USS probes/gel) /Cockroaches Patient long-term colonisation known

Aetiology Norovirus 80% Few particles to cause illness 2 -3 days incubation with high attack rate ( 40% or more) Spread by person – person Aerosol dissemination when vomiting Environmental contamination Water & food Secondary foodborne spread

Signs and Symptoms Vomiting, but not always Diarrhoea Nausea Abdominal cramps Headache Myalgia Chills & fever

Control of an outbreaks in an NH 2 or more cases - Report Stop people traffic / admissions Signage / Information Leaflets Isolate symptomatic patients Dedicated nursing staff for symptomatic patients Focus on hand hygiene / type of alcohol gel PPE laundry & clinical waste management environmental cleaning Obtain specimens Documentation Apply the 48 / 72 hour rule

Known outbreak of Norovirus in community what actions do you take in the surgery? Discourage attendance at the surgery. Known symptomatic patients wait is segregated area. Send sample – vomitus best if necessary. Pay particular attention to cleaning of toilet and wash hand basin used by symptomatic patients. Do not overstock toilet area.

Pandemic Influenza Modes of transmission For planning purposes it is assumed that a pandemic strain of influenza will have a similar transmission, communicability, and inactivation properties as “routine” seasonal influenza Influenza is well established to be transmitted from person-to-person through close contact

Modes of transmission influenza The most likely routes of transmission are large droplet and direct and indirect contact Airborne, or fine droplet transmission, may also occur Brankston et al (2007) Transmission of influenza A in human beings. Lancet Infect Dis. Apr; 7 (4); 257 -65

Past Pandemics in the 20 th Century Global Deaths 1918 H 1 N 1 1957 H 2 N 2 1968 H 3 N 2 Spanish Flu Asian Flu Hong Kong Flu >50 million 1 -2 million 700, 00

Unusual Features of the 1918 Influenza Pandemic 3 successive waves within ~ 9 months Unexpectedly high mortality at all ages Paradoxical mortality: low in wave 1, high in waves 2 & 3 in young/healthy, in elderly Severe bronchopneumonia; cyanotic collapse Caused by a novel H 1 N 1 virus

Staff Roles of Responsibilities and systems of working Lead person to ensure infection control issues are maintained Plan – separation/early triage Flu/non-flu patients - Cohort area large number of patients with flu symptoms - Consider entrance/exit - Consider flu/non-flu clinic - Antivirals Home visit teams Communication staff/public

Prevention of transmission Standard Infection Control Principles and Droplet Precautions are the principal infection control strategies which should be rigorously followed. In certain circumstances these control measures may need to be augmented with higher levels of respiratory protection

Prevention of transmission Hand hygiene Containment of respiratory secretions Separation or cohorting of patients Restriction of ill workers and visitors Education of staff, visitors, and patients Personal protective equipment

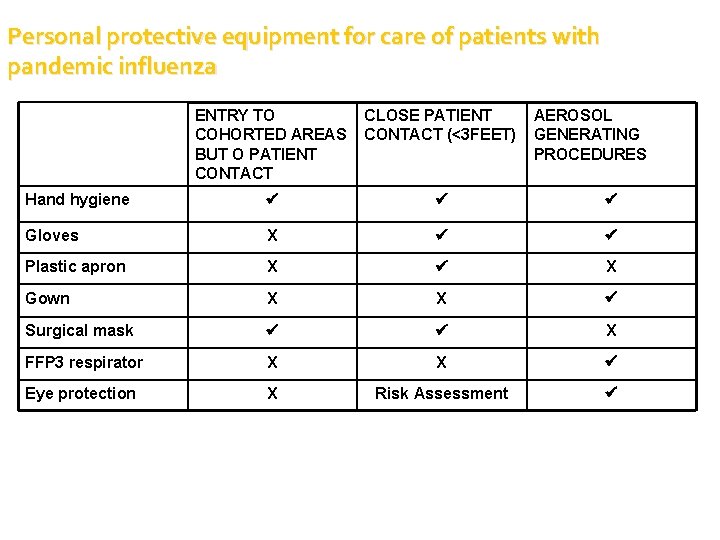
Personal protective equipment for care of patients with pandemic influenza ENTRY TO COHORTED AREAS BUT O PATIENT CONTACT CLOSE PATIENT CONTACT (<3 FEET) AEROSOL GENERATING PROCEDURES Hand hygiene Gloves X Plastic apron X X Gown X X Surgical mask X FFP 3 respirator X X Eye protection X Risk Assessment

Prevention of transmission Aerosol generating procedures nebulisers, intubation = FFP 3 mask Fit check carried out each time masks worn Seal tightly to the face (clean shaven skin) Change if breathing becomes difficult / damaged distorted or a face fit can not be achieved Eye protection – if there is a likelihood of exposure to body fluids

Within the surgery identify Cohort Area – know where to segregate waiting patients to nebulise patients if required to decontaminate equipment following use to dispose of equipment to dispose of infected materials - tissues

Telephone triage (less seriously ill reduces crowding) Access to hand washing facilities Removal of toys/soft furnishings /magazines Lidded tissue/waste bines in the areas

Infection Control Procedures Standard Infection Control principles/ Droplet precautions (Surgery/Home Visits) Hand hygiene Sinks – adequate stocks of soap and towels Hand sanitiser at points of patient care Designated Entrance/Exits with sanitisers Consider alcohol hand sanitizer for home visits Hand contact surfaces – clean regularly when designated room is in use

Respiratory Etiquette Cover mouth with disposable tissues coughing, sneezing wiping and blowing noses Dispose of used tissues Wash hands Crowded waiting areas – symptomatic patients wear masks

Hand Hygiene q. Wash/Use alcohol rub q. Expose forearms - bare below the elbow q 6 step technique + wrists q. No jewellery q. No false nails/nail polish q. Hair - off face q. Pedal bin

Hand Washing –When ! üWhen you come on duty, before & after breaks & before going home üBefore & after patient contacts üBefore & after aseptic technique/invasive procedure üBefore contact with a susceptible site üAfter contact with blood, body fluid or excreta üAfter handling contaminated equipment/waste/laundry üBefore & after contact with a patient on isolation precautions üBefore serving meals & drinks

Advantages of Cleaning Hands with Alcohol-Based Hand Rubs When compared to soap and water handwashing, alcoholbased hand rubs have the following advantages: take less time to use can be made more accessible than sinks cause less skin irritation and dryness are more effective in reducing the number of bacteria on hands making alcohol-based handrubs readily available to personnel has led to improved hand hygiene practices

When not to use alcohol gels! D&V if your product is not active against causative virus C diff – alcohol hand gels do not kill spores ! Your skin - Moisturise at appropriate times

Identify your highest risk activity in relation to the need for effective equipment decontamination! Joint and soft tissue injections Aspirations Incisions Excisions Curetting Cautery Cryotherapy Wound dressings

Guidance Facilities to provide minor surgery – DH Health Building Note 46: General Medical Practice Premises. London DH IC Guidance for General Practice IPS 2004 Cooper T (2007) IC in General Practice. Primary Health Care 14 (6) 15 -17. Health Service Circular 2000 /032 - Guidance specific to equipment decontamination.

Effective management system to cover all aspect of decontamination cycle Appropriate facilities Equipment is fit for purpose, maintained, calibrated, monitored and validated. Staff have appropriate training. Single use items are not reused Decontamination records are kept

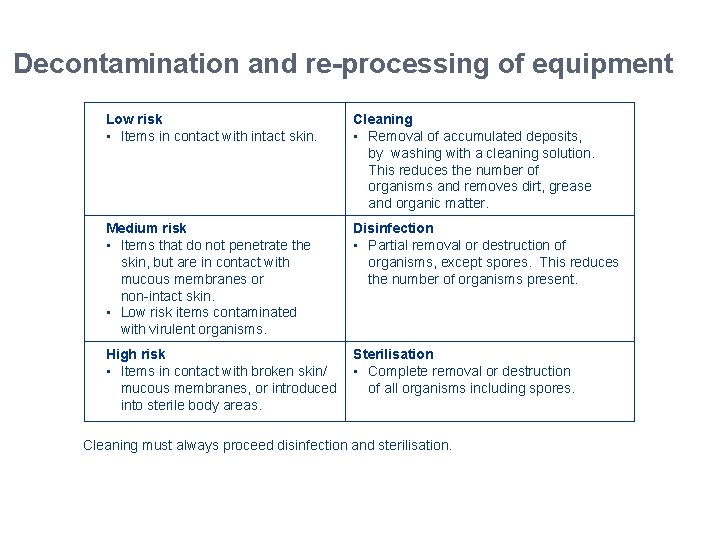
Decontamination and re-processing of equipment Low risk • Items in contact with intact skin. Cleaning • Removal of accumulated deposits, by washing with a cleaning solution. This reduces the number of organisms and removes dirt, grease and organic matter. Medium risk • Items that do not penetrate the skin, but are in contact with mucous membranes or non-intact skin. • Low risk items contaminated with virulent organisms. Disinfection • Partial removal or destruction of organisms, except spores. This reduces the number of organisms present. High risk • Items in contact with broken skin/ mucous membranes, or introduced into sterile body areas. Sterilisation • Complete removal or destruction of all organisms including spores. Cleaning must always proceed disinfection and sterilisation. 5. 7

Disinfection - 'the removal or destruction of harmful microbes, not usually including bacterial spores. (Maurer, 1974) pr. EN ISO 15883 -1) defines disinfection as 'reduction of the number of viable microorganisms on a product to a level previously specified as appropriate for its intended further handling or use'. Disinfectant compounds are required to produce a 99. 999% (log 5) reduction in bacterial population. Out of 100, 000 1, 000 survivors would remain.

Decontamination may use chemical disinfectants such as Milton or Hypochlorite. Choosing the type and concentration of a disinfectant depends on its effectiveness against specific pathogens. Hypochlorite tablets such as HAZ may also be used for Blood or body fluid spills. Actichlor Plus – combines disinfectant with detergent.

Actichlor Plus Correct dilution: Amount of available chlorine needed for the job • general environment 1, 000 ppm 1 tablet in 1 litre • blood spillage 1 tablet in 100 ml 10, 000 ppm Actichlor Plus The solution made up from the tablets will sanitise and clean at the same time. Chlorine Disinfects and Sanitises Detergent Action lifts grease and cleans

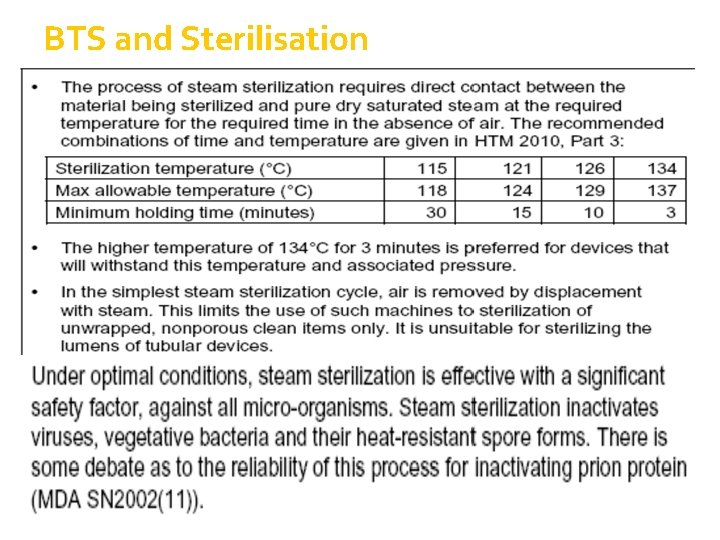
STERILISATION in CSD One means of decontamination is autoclaving. A steam autoclave destroys organisms using saturated steam under pressure. Autoclaving is used for sterilization of equipment as well as for decontamination of waste items. When autoclaving is used to sterilize reusable items, they must be soaked, cleaned, and packaged prior to the process.

BTS and Sterilisation

v. CJD Ø Effective cleaning prior to sterilization is of the utmost importance in reducing the risk of transmission of v. CJD via surgical procedures Ø Single-use instruments? HSS(MD)15/99: variant Creutzfeldt-Jakob Disease (v. CJD)

Equipment ü Before buying check decontamination requirements with manufacturer ü Use single use/single patient use equipment if possible ü Have written protocols/guidelines from manufacturer & locally for decontamination ü Have replacement policy

Specimen Taking Swabs Tissue Pus Wound Fluid/exudate Irrigate

Swabs Don’t take a swab of a wound if you don’t know what to do with the result. Before you take a swab think “Am I going to change the management of this patient based on the results of this investigation? ” If not don’t do it

Specimen Taking Which wound if any would you swab? When? How? Wet/Dry? How often? Remember swabbing may damage good tissue Communicate with laboratory Think about what you are doing and what you intend to achieve

Please Remember! Presence of micro-organisms within a wound is not necessarily indicative of infection. A diagnosis of wound infection MUST be based on the classical clinical signs together with supportive microbiology

Initiative to drive down HCAI’s • Media / Public concern • Single Rooms Policy • Unannounced Inspections of all Hospitals • Restrictions on Hospital Visiting • Dress Code • Hand Hygiene Campaign • MRSA Screening for High Risk Patients • Rapid Response Cleaning Teams • Publication of Infection Prevention and Control Performance in hospitals • Prescribing monitoring • Saving lives initiatives

Thank you Mary Hanrahan SRN, M. Sc, . Nursing. mary. hanrahan 62@googlemail. com