Infantile Vanishing White Matter Disease Kimberly Beavers MD

Infantile Vanishing White Matter Disease Kimberly Beavers MD, Miguel Flores MD, Aditi Dagli MD, Steven Messina MD

No Disclosures

Purpose • Report a unique case of infantile vanishing white matter disease • Describe important imaging findings helpful in making the appropriate diagnosis

Clinical Presentation • 6 -month-old female presenting with • Failure to thrive • Complex partial seizures • Upper extremity extensor posturing • Perioral cyanosis • Physical examination • Bilateral cataracts • Microcephaly
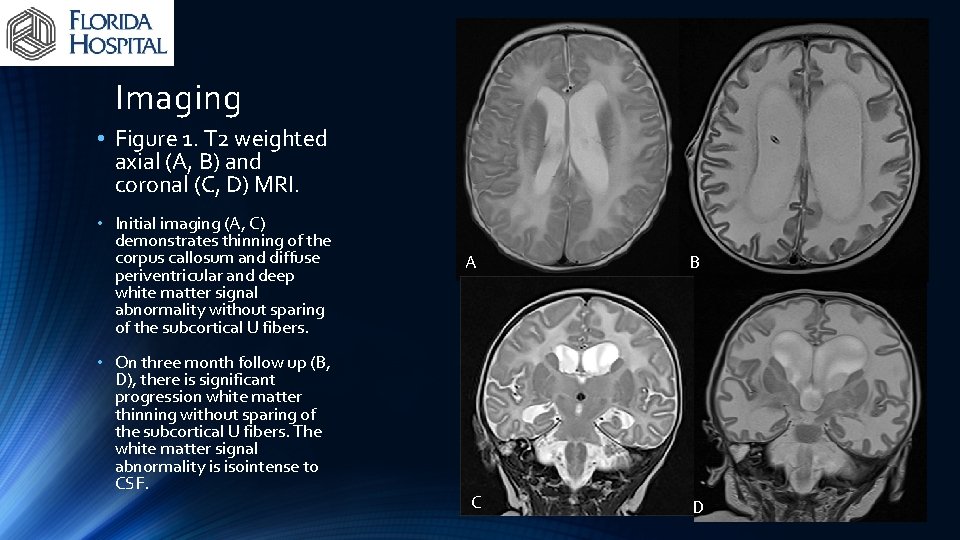
Imaging • Figure 1. T 2 weighted axial (A, B) and coronal (C, D) MRI. • Initial imaging (A, C) demonstrates thinning of the corpus callosum and diffuse periventricular and deep white matter signal abnormality without sparing of the subcortical U fibers. • On three month follow up (B, D), there is significant progression white matter thinning without sparing of the subcortical U fibers. The white matter signal abnormality is isointense to CSF. A C B D
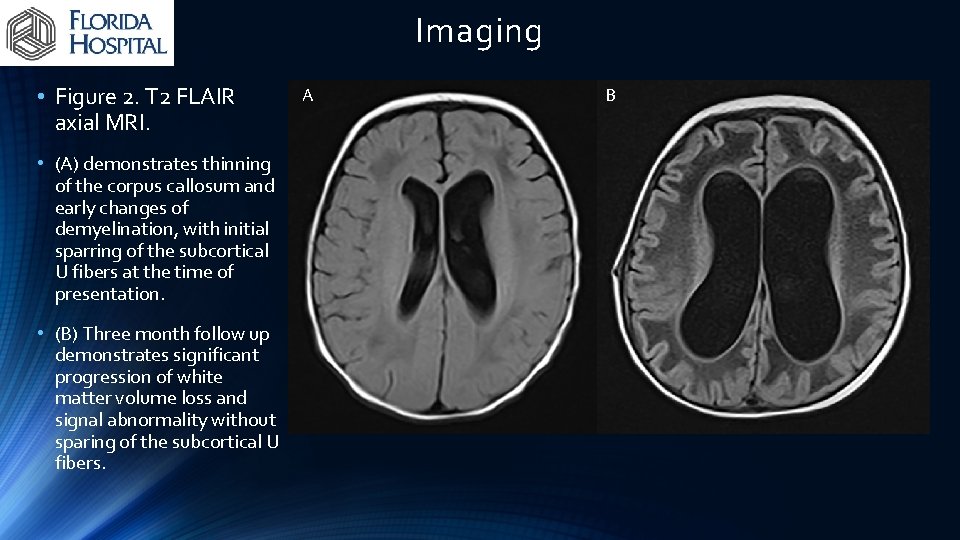
Imaging • Figure 2. T 2 FLAIR axial MRI. • (A) demonstrates thinning of the corpus callosum and early changes of demyelination, with initial sparring of the subcortical U fibers at the time of presentation. • (B) Three month follow up demonstrates significant progression of white matter volume loss and signal abnormality without sparing of the subcortical U fibers. A B

Differential Diagnosis • Leukodystrophies • Metachromatic leukodystrophy • Megalencephalic leukoencephalopathy with subcortical cysts • Alexander Disease • Krabbe Disease • Sjogren-Larsson syndrome • Canavan’s Disease (without macrocephaly)

Genetic Testing • Genetic testing revealed two mutations • EIF 2 B 2 gene from the mother and father. • The variant inherited from the mother has been reported in association with vanishing white matter disease. • The patient has since had some seizure control with Keppra, but has expectedly continued to decline clinically with significant delay of developmental milestones.

Final Diagnosis • Vanishing White Matter Disease

Metachromatic Leukodystrophy -Corollary case • 2 -year-old male presenting with epilepsy • Laboratory proven metachromatic leukodystrophy with deficient arylsulfatase-A levels. • Autosomal recessive lysosomal storage disease • Mutation of ARSA gene on chromosome 22 • Progressive central and peripheral nervous system demyelination • Symmetric, bilateral, sparing of subcortical U fibers • Slower progression of disease than Vanishing White Matter
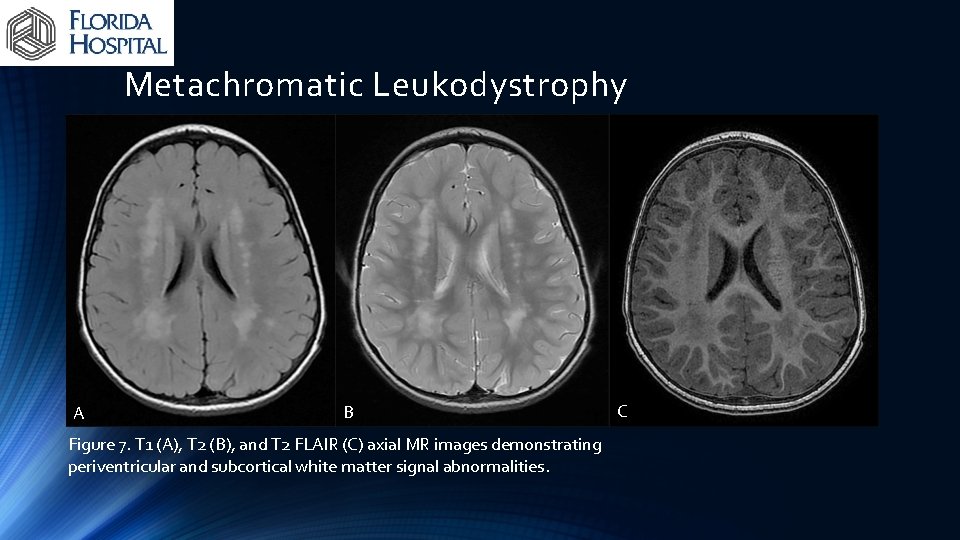
Metachromatic Leukodystrophy A B Figure 7. T 1 (A), T 2 (B), and T 2 FLAIR (C) axial MR images demonstrating periventricular and subcortical white matter signal abnormalities. C

Distinguishing Vanishing White Matter and Metachromatic Leukodystrophy • With similar appearance in the early stages, single MRI may not be able to differentiate between the two diseases. • Vanishing White Matter disease can be differentiated on MRI due to its often rapid progression. Follow up imaging is thus critical to making the correct diagnosis.

Vanishing White Matter Disease • Epidemiology • Also known as childhood ataxia with central hypomyelination • Infancy through adulthood • Mainly disease of childhood

Vanishing White Matter Disease • Etiology • Autosomal recessive genetic mutation • Chromosome 3, EIF 2 B 2 gene

Vanishing White Matter Disease • Diagnosis • Characteristic imaging findings • • Diffuse cerebral white matter signal abnormality Abnormal white matter signal intensity equal to cerebrospinal fluid on FLAIR Diffuse “melting away” pattern of vanishing white matter Sparing of subcortical U fibers (early), rapidly progressive loss of subcortical U fibers (late/severe cases) • Clinical exam • Ataxia • Epilepsy • Microcephaly Van der Knaap et al

Vanishing White Matter Disease • Management • Symptomatic management of epilepsy • Genetic counseling • Supportive care

Summary • Vanishing White Matter Disease is an uncommon leukodystrophy presenting with classical imaging findings of thinning of the corpus collosum, progressive disappearance of the periventricular and deep white matter, with sparing of subcortical U fibers in early cases. • The patient in this case had a particularly rapidly progressive case with diffuse white matter loss without sparing of subcortical U fibers. • Vanishing White Matter Disease can potentially be distinguished from other leukodystrophies on imaging by its often rapidly progressive demyelination. • Diagnosis clinically confirmed by genetic testing.

References • Bugiani, M. , Boor, I. , Powers, J. M. , Scheper, G. C. , & van der Knaap, M. S. (2010). Leukoencephalopathy with vanishing white matter: a review. J Neuropathol Exp Neurol, 69(10), 987 -996. doi: 10. 1097/NEN. 0 b 013 e 3181 f 2 eafa • Groeschel, S. , Kehrer, C. , Engel, C. , C, I. D. , Bley, A. , Steinfeld, R. , . . . Krageloh-Mann, I. (2011). Metachromatic leukodystrophy: natural course of cerebral MRI changes in relation to clinical course. J Inherit Metab Dis, 34(5), 1095 -1102. doi: 10. 1007/s 10545 -011 -9361 -1 • Lin, Y. , Pang, X. , Huang, G. , Jamison, S. , Fang, J. , Harding, H. P. , . . . Lin, W. (2014). Impaired eukaryotic translation initiation factor 2 B activity specifically in oligodendrocytes reproduces the pathology of vanishing white matter disease in mice. J Neurosci, 34(36), 12182 -12191. doi: 10. 1523/JNEUROSCI. 1373 -14. 2014 • Schiffmann, R. , Fogli, A. , van der Knaap, M. S. , & Boespflug-Tanguy, O. (1993). Childhood Ataxia with Central Nervous System Hypomyelination/Vanishing White Matter. In R. A. Pagon, M. P. Adam, H. H. Ardinger, S. E. Wallace, A. Amemiya, L. J. H. Bean, T. D. Bird, C. T. Fong, H. C. Mefford, R. J. H. Smith & K. Stephens (Eds. ), Gene. Reviews(R). Seattle (WA). • van der Knaap, M. S. , Pronk, J. C. , & Scheper, G. C. (2006). Vanishing white matter disease. Lancet Neurol, 5(5), 413 -423. doi: 10. 1016/S 1474 -4422(06)70440 -9 • Yang, E. , & Prabhu, S. P. (2014). Imaging manifestations of the leukodystrophies, inherited disorders of white matter. Radiol Clin North Am, 52(2), 279 -319. doi: 10. 1016/j. rcl. 2013. 11. 008

Contact Information • Kimberly Beavers, MD • PGY-2 • Florida Hospital Radiology, Orlando, Florida • Kimberly. Beavers. MD@flhosp. org Address • Florida Hospital Department of Radiology Specialists of Florida Hospital 601 E. Rollins Orlando, FL 32803 • Phone 407 -303 -8178 • Fax 407 -303 -7844
- Slides: 19