Infant of Diabetic Mother GDM Carb intolerance in

Infant of Diabetic Mother • • • GDM-- Carb intolerance in pregnancy affects 3 -5% of pregnancies Risk factors - ↑ maternal age , obesity ↑ BMI , strong family history southeast Asians, African Americans etc ↑ perinatal and Neonatal mortality with poor glycemic control

Introduction • Frequency: 3 -10% of pregnant women have diabetes – 88% have gestational diabetes – 12% have known diabetes • 35% with Type I diabetes • 65% with Type II diabetes

Risk of Complications • Higher with poor glucose control • Higher with pre-gestational Diabetes • ↑ risk of other compl in the mother -- eg: PIH is 2 times more common in diabetic pregnancies

LGA and SGA babies
CASE -- 1 Baby G , a 36 wk IDM with birth wt of 3. 8 kg, NVD, good APGARS was with mum, breast fed at 2 and 5 hrs of age, presented at 10 hrs of age with • H/O 1. multiple apnea • 2. severe lethargy, pale, mottled • •

Case -1 ---contd • GRBS– 30 mg% • Maternal hyperglycemia ↓ ↓ • glucose and a. a cross placenta(not insulin ) • ↓ • ↑ bl sugar in fetus →ß cell hyperplasia • ↓ • hyperinsulinemia

• • Routine monitoring in IDM is Important Glucose reqd is much higher than normal Reqr may go upto 15 mg/kg/min If not maintained on oral feeds, start IV fluids ↑ volume and conc of glucose – may need a central line for Glucose > 12% MONITORING VITAL – 48 HRS

Case --2 • 2. 1 kg Term IDM, on full feeds and normal GRBS presents on day 2 with • 1. Cyanosis • 2. lethargy, resp distress • 3. Convulsions

Case 2 ---contd • PCV– 66 % , Hb - 22 gm/dl – • Polycythemia • ↑ Hb A 1 in mother and baby –hypoxia • placental insufficiency • Needs Partial Exch transfusion to prevent CNS morbidity • Haematuria, NEC, PPHN may also occur

Preventable CNS morbidity • Hypoglycemia – microcephaly, C. P , learning disability in 30 -50% of symptomatic cases • Polycythemia -- hemiplegia, cerebral infarct • mental retardation , limb weakness • PREVENTABLE MORBIDITIES • MONITORING IS THE KEY

Case 3 • Term baby 3. 8 kg, IDM presents on day 3 with • 1. Resp Distress -80/min • H. R. – 190/min, poor pulses, s. Po 2 94% • features of CCF , Systolic murmur

Cardiac complications • H O C M - Lasix, Propranolol • Resolves by 4 -6 mos • Deposition of fat and glucose along the septum • Others-- TOGV, ASD, Coarctation
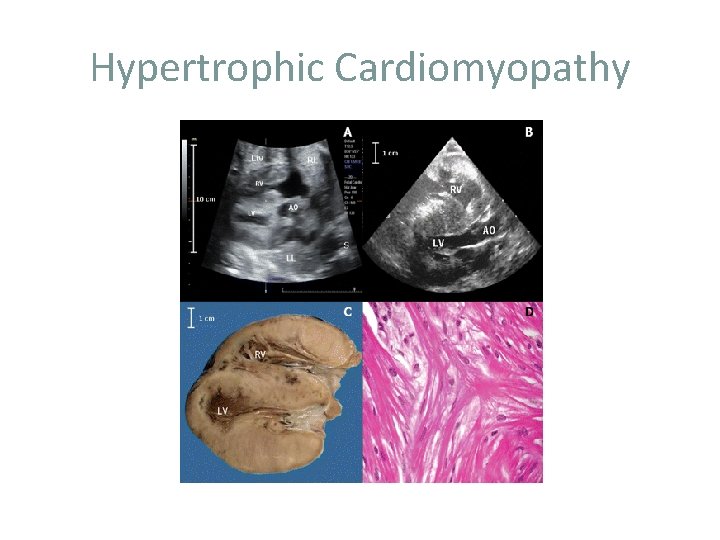
Hypertrophic Cardiomyopathy

Case 4 • Term baby 39 wks, 3. 7 kg , IDM presents with severe resp distress at 1 hr of age
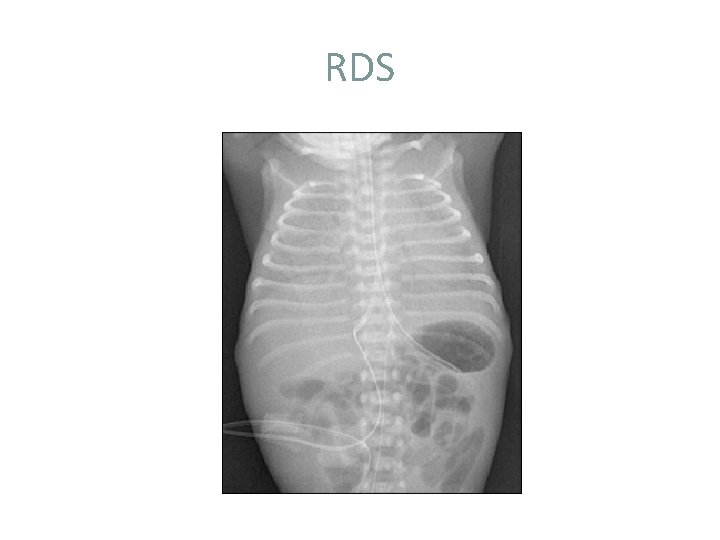
RDS
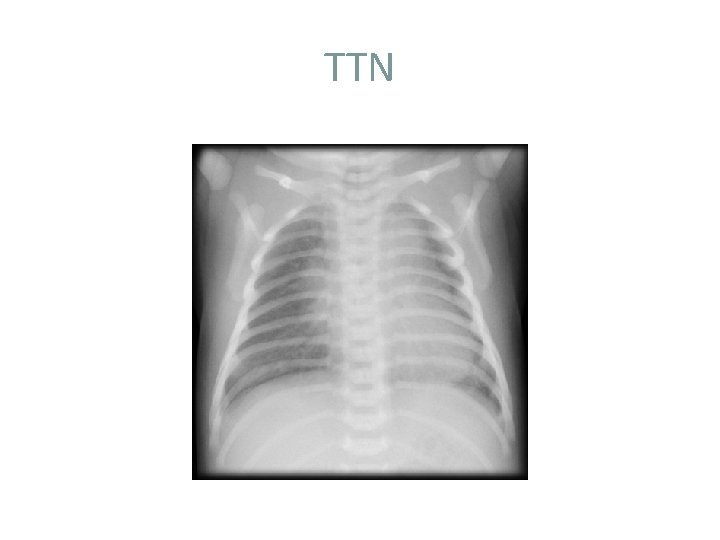
TTN

Case 5 • 4 - day old preterm IDM 36 wks- 1. 8 kg has • feed intolerance, vomiting, abd distension • bilious aspirates
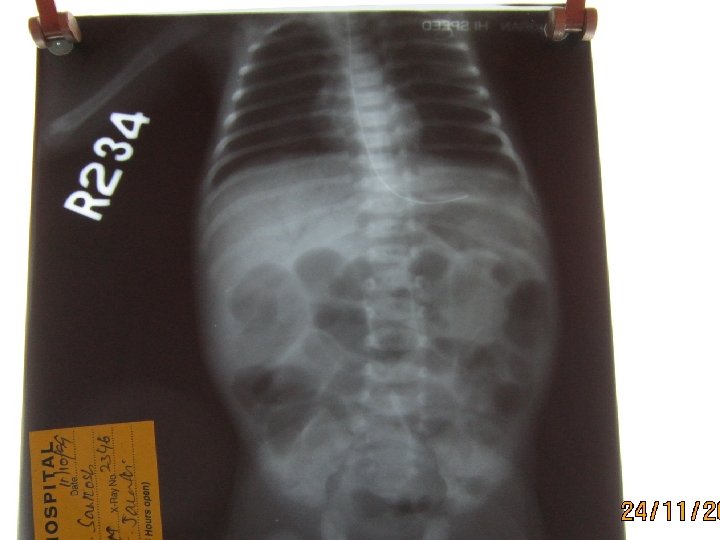
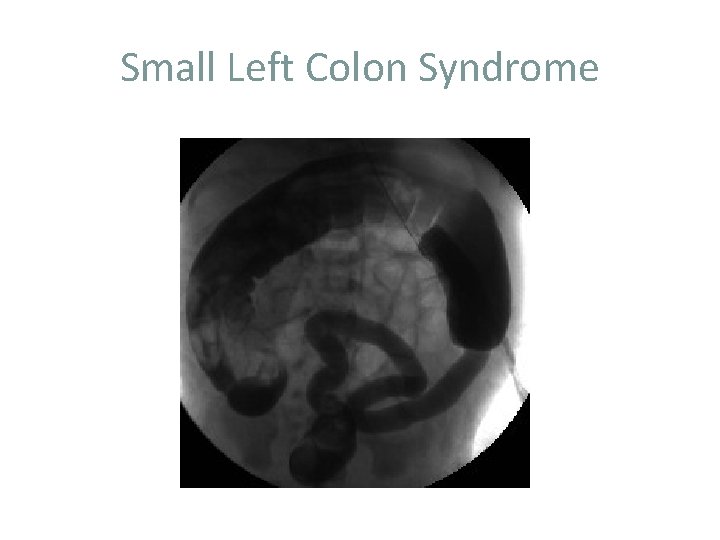
Small Left Colon Syndrome
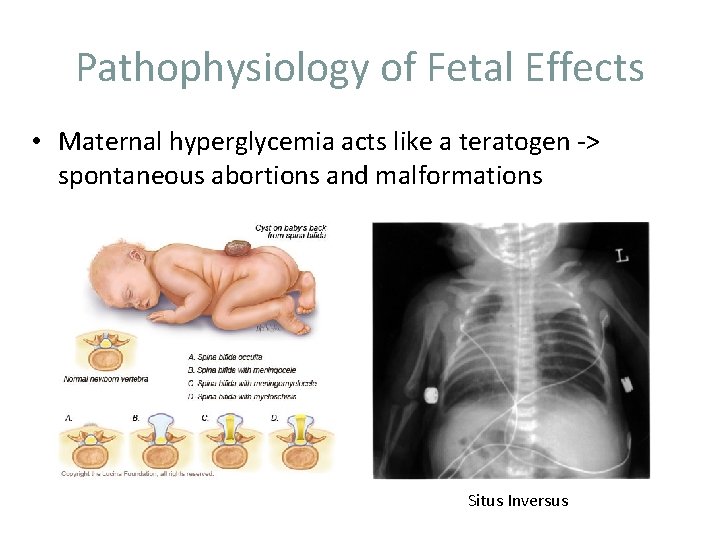
Pathophysiology of Fetal Effects • Maternal hyperglycemia acts like a teratogen -> spontaneous abortions and malformations Situs Inversus
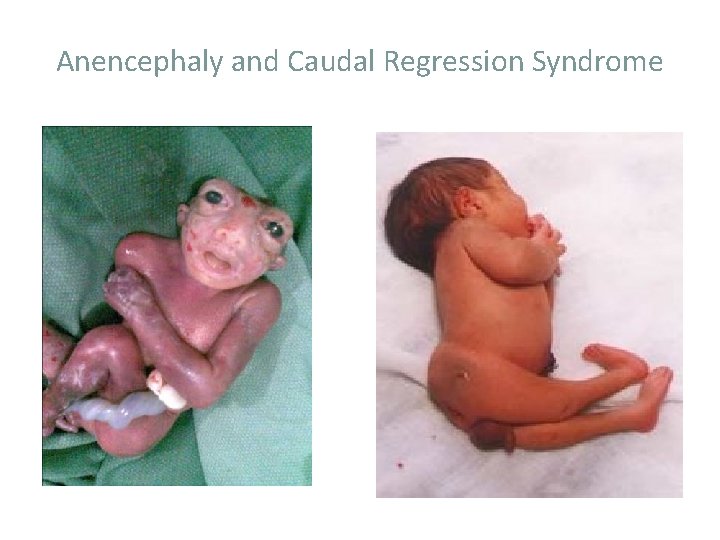
Anencephaly and Caudal Regression Syndrome
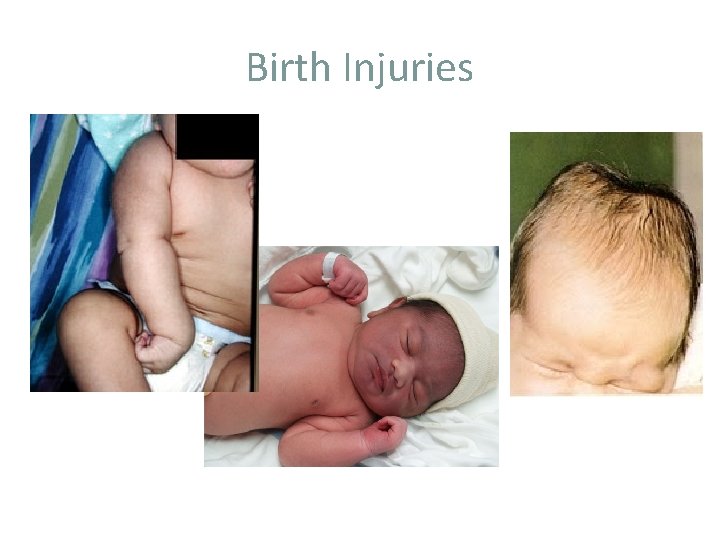
Birth Injuries

Birth Injury Macrosomia puts infant at risk for injuries during delivery Shoulder dystocia can lead to: Clavicular and/or humeral fractures Brachial plexus injuries Traumatic delivery or need for vacuum/forceps assistance can lead to: Cephalohematomas Facial bruising Facial nerve injuries

Problems of IDM babies • At Birth • • • Still birth preterm Macrosomia asphyxia birth injury
• • Problems after birth LGA SGA Hypoglycemia Hypocalcemia RDS, TTN HOCM Polycythemia Hyperbil Anomalies ( CNS, CVS GIT ) Sepsis

Role of Obstetrician • Preconception counselling • good maternal glucose control • Paediatrician • Anticipate, monitor, treat complications
- Slides: 26