Infant nutrition Care of the healthy baby Gbor

Infant nutrition. Care of the healthy baby. Gábor Veres, MD, Ph. D, Dsc Professor of Pediatrics Ist Dept. of Pediatrics Semmelweis University, Budapest

What is the most important question in infancy?

Weight gain !

Content • • • Breast feeding Composition of breast milk Eosinophilic enteropathy, Reflux (GOR) Formulas, solids Iron, vitamins

Three basic principles of infants feeding • Until 6 months exclusive breast feeding. • Demand feeding. • Milk or diluted milk can not be given even between 6 -12 months. Followon formulas are recommended.

Introduction of gluten: Until 6 months exclusive 4 -12 months (Celiac disease) breast feeding, Vriezinga, BUT: NEJM, 2014 • Introduction of gluten and solids • Between 4 -7 months (+ breast feeding) • Decrease of celiac disease and food allergy Silano M, Agostoni C, Guandalini S. Effect of the timing of gluten introduction on the development of celiac disease. World J Gastroenterol. 2010; 16: 1939 -42.

Demand feeding, BUT: • Jaundice: sleepy infant, wake-up! • Infantile colic: not every crying means baby is hungry

Energy content of the breast milk (BM) • Exclusive breast feeding covers the energy needs of infants until 6 months • Energy needs: 90 -120 kcal/kg/die • Energy of BM 60 -70 kcal/100 ml • 5000 g baby: 500 kcal BM pro day 750 ml BM / day

Advantages of breast feeding I. • Composition of breast feeding is optimal for the development of infants • PUFA content is necessary for the development of retina and brain • Breast milk is easier digestable than the different formulas

Advantages of breast feeding II. • Breast milk, especially colostrum ensures immune defense • It contains antibacterial and antiviral antibodies, as well as T-cells and macrophages • Stool p. H is lower, bacterial microflora bifidogen inhibiting enteral infections

Advantages of breast feeding III. • Frequency of obesity, hypertonia, IBD and Type I. diabetes mellitus are rare • Favourable psychological relationship between the mother and child

Immunoglobulins and cytokines in BM Tomicić et al. Pediatr Res. 2010; 68: 330 -4. • Ig. A neutralizes pathogens, does not activate complement system (oral tolerance) • TGF-beta (transforming growth factor) inhibits immune activation less allergy in breast fed infants

BUT: Breast fed infants do have: • Atopic dermatitis • Allergic-eosinophilic esophagitis • Allergic-eosinophilic colitis Foreign proteins in breast milk

Eosinophilic esophagitis • Reflux, BUT: p. H is normal, PPI therapy resistant • Dyspepsia • 75% in males • Food allergy in 50%, eosinophilia 42% • Dg: upper endoscopy • Histology: 15 eosinophils/HPF
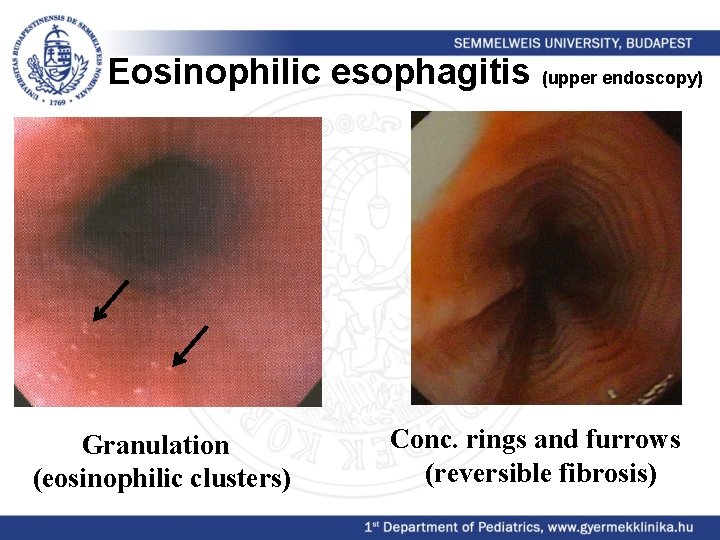
Eosinophilic esophagitis (upper endoscopy) Granulation (eosinophilic clusters) Conc. rings and furrows (reversible fibrosis)
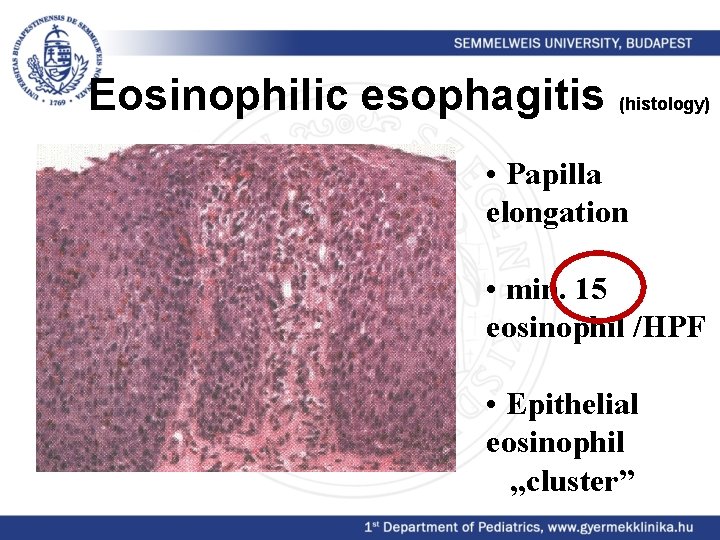
Eosinophilic esophagitis (histology) • Papilla elongation • min. 15 eosinophil /HPF • Epithelial eosinophil „cluster”

Hematochezia (fresh blood in feces) • • • 3 months old infant, breast feeding No family history for polyposis CRP, blood picture, coagulogram: normal Feces: no bacteria RDE: no fissures, no obstipation Dg: ALLERGIC COLITIS Mother’s elimination diet (cow’s milk)
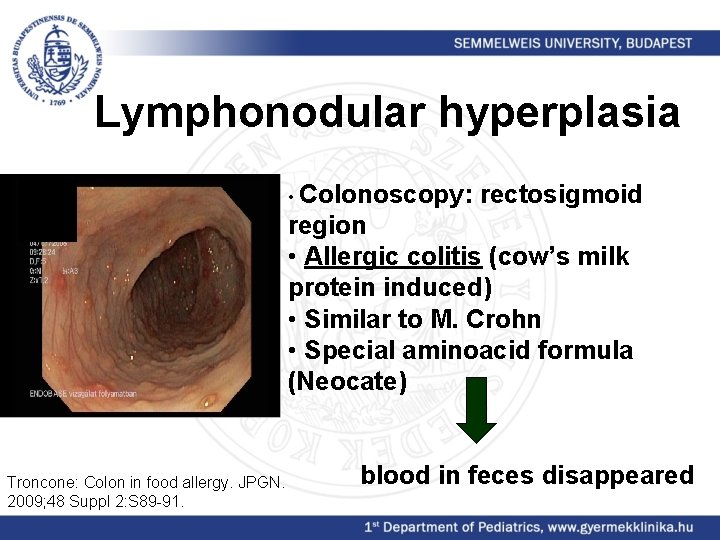
Lymphonodular hyperplasia • Colonoscopy: rectosigmoid region • Allergic colitis (cow’s milk protein induced) • Similar to M. Crohn • Special aminoacid formula (Neocate) Troncone: Colon in food allergy. JPGN. 2009; 48 Suppl 2: S 89 -91. blood in feces disappeared
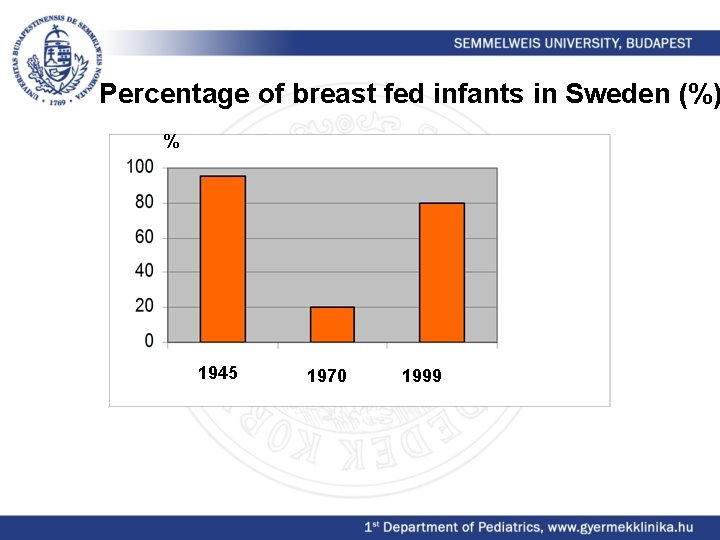
Percentage of breast fed infants in Sweden (%) % 1945 1970 1999
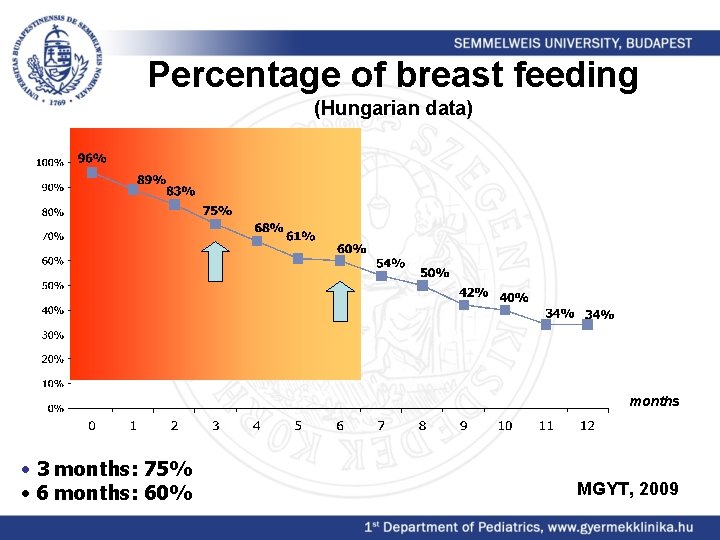
Percentage of breast feeding (Hungarian data) months • 3 months: 75% • 6 months: 60% MGYT, 2009

Composition of breast milk Newburg DS: Handbook of milk composition. Academic Press 1995; pp 273 -349 • Lactose 55 -60 g/l • Proteins 10 g/l • Lipids 40 g/l • Nucleotids, Erythropoietin, Ig. A, TGF-beta

I. Lactose in BM (55 -60 g/l) galactose • • glucose Main sugar/energy source Enzyme: lactase After 34. weeks lactase activity matures Lactase activity after the age of 3 y. • Congenital absence of lactase: very rare
II. Proteins in BM (10 g/l)

Proteins (1%=1 g/100 ml) • Protein content of colostrum and early milk is higher • Mature breast milk contains less secretory Ig. A and lactoferrin • Ratio of whey and casein is also high (80/20) which is gradually decreasing to 60/40

Whey/casein ratio (BM=60: 40) Whey: • Intestinal transport, motility • More digestable Casein: • Viscosity , anti-reflux effect

Recommended protein content of formulas ESPGHAN AAP Räihä g/100 kcal 1, 8 -2, 8 1, 8 -4, 5 1, 6 -1, 8 g/l 12 -19 12 -30 11 -12 At decreased protein content the serum urea level will be similar to that found at exclusively breast fed infants

Low protein intake in infancy is beneficial for future life • Danish survey, 631 intants • At birth, 3 months, 18 months (US, blood) Higher protein intake (formula fed infants): • Increased size of kidney • Higher urea in blood Schmidt, Pediatr Nephrol, 2004; 19: 1137 -44

Which mammals has the lowest protein in the BM ? ? ? • Human breast milk
III. Lipids in BM (40 g/l)

Importance of lipids • High energy content • Beta-palmitate trygliceride is high in BM (70%) • Significance of poly-unsaturated fatty acids (PUFA)

Structure of triglicerides ( ) CH 3 - O - R 1 | ( ) CH 2 - O - R 2 | ( ) CH 3 - O - R 3 Pancreas lipase split the palmitic acid located in position

The advantage of tryglicerides containing beta-palmitate • In this position the lipase does not split the palmitic residue • Can be absorbed !!! • Free palmitic acid forms with calcium unsoluble calcium soap which is not able to absorbe • Therefore it decreases energy and calcium supply

Significance of LC-PUFA in infant nutrition • Linolic and linolenic acid is not synthesized in the human body (essential fatty acids) • Docosahexaenoic acid is indispensable to the normal function of cell membrane

Somatic development of breast fed infants • After two months the length and weight of breast fed infants are slightly less than those of formula fed • At the preparation of reference curves a preponderance of formula fed babies occured • Not the maximal but optimal development is advantageous

Infant mortality (1000 newborns ? at 1 year) • Prehistoric man, chimpanzee infant mortality: 250 ‰ • End of XIX. is the same for men • One of the reasons: NO infant formula 1903 (Derby) infant mortality: - arteficial feeding: 230 ‰ - breast fed: 70 ‰
Infant formulas For healthy babies formulas 1. Standard formula 2. Follow-on 3. Baby’s milk Special

1. Standard formulas • Strict criteria • Range of energy: E: 60 -75 kcal/100 ml Trend toward less protein • Whey/casein = 60 : 40 • Taurin: development of retina and CNS • Carnitin: lipid metabolism

Why is not optimal to give cow’s milk to infants under one year? • It contains too much – protein – sodium • It contains too less – linolic acid – iron – vitamins (C, D, E)

Cow’s milk feeding may cause: • Iron-deficiency anaemia • Blood in feces • Atopic dermatitis • Increased osmotic load for kidneys

3. Baby’s milk • • Recommended from 7 -9 months Until 1 -3 years More expensive than cow’s milk Price: 1. 5 -2 x than cow’s milk

Special formulas Anti-reflux (AR) • Seads of Saint John’s bread-tree (Nutriton) • Corn-starch (AR) or potato-starch • Nestle HA+AR: HA: Hypoallergenic: only for prevention and anti-reflux together

Reflux, regurgitation • • • Size of stomach: 30 ml Adults: 1500 ml 5 kg infant: 200 ml BM 70 kg adult: 2. 8 litre !!! Growing well? • Exclude other causes (pyloric stenosis, intest. stenosis, CAH, infections, metabolic etc. )

Solids • Foods besides breast milk and formulas • Introduction between 4 -7 months – fruits – cereals – vegetables – meat

Iron deficiency • 1 billion people affected • Developed country: 12%, developing: 51% • Hungary: 8 -36 months: 30% 4 -6 years: 51% iron deficiency ! • Iron psychomotorial and cognitive function • In iron deficiency: lead absorption
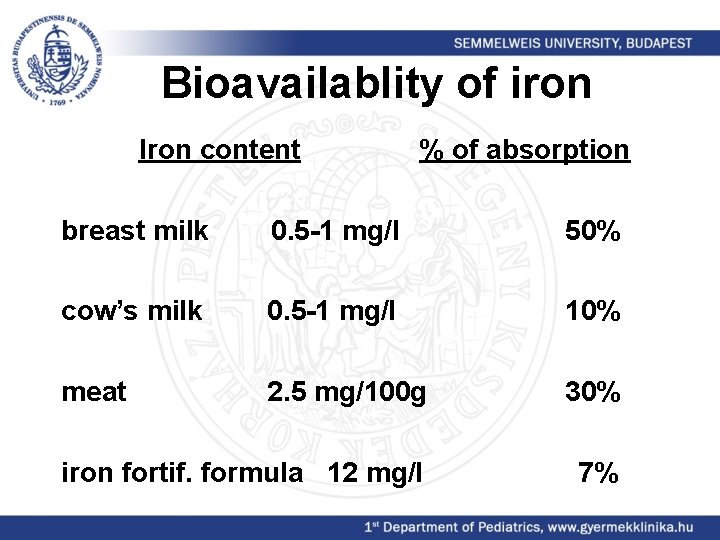

Bioavailablity of iron Iron content % of absorption breast milk 0. 5 -1 mg/l 50% cow’s milk 0. 5 -1 mg/l 10% meat 2. 5 mg/100 g 30% iron fortif. formula 12 mg/l 7%

Iron and everyday practice • First: measure iron level • Bacteria needs iron for growing • Do NOT give iron in bacterial infection! • Term baby: no supplementation in 69 months source: red blood cells • Preterm baby: 2 mg/kg after 2 months

Vitamin K • Vitamin K dependent coagulatory proteins (prothrombin, VII, IX, X) • BM contains low level, supplementation • At birth, 1 week, once/months per os, 2 mg • Formula contains vitamin K • Intestinal bacteria produce vitamin K • Liver, soybean, spinach, tomatoes, kale

Vitamin D • • Low level in BM Supplementation: 400 U/day After 2 weeks - 1 -1. 5 years or more! Formula contains vitamin D

Allergy, atopic dermatitis

Probability of atopy in positive family history • • No atopy in the family One parent / one sibling Both of parents Both p. with the same manifest. : 10% : 30% : 50% : 70%

Allergy prevention of infants • (Diet of mother during pregnacy: NO effect!!!) • Longer breast feeding • Avoid food with high allergenicity (also during breast feeding) • Hypoallergen formulas • Probiotics (Kalliomaki, Lancet, 2001)

Probiotics („Good” bacteria) • 1 -1. 5 kg bacteria in the intestinal tract • 400 bacterium species • 10 times more bacteria than cells in the body • „Good” bacteria: Bifidobacteria, Lactobacillus species
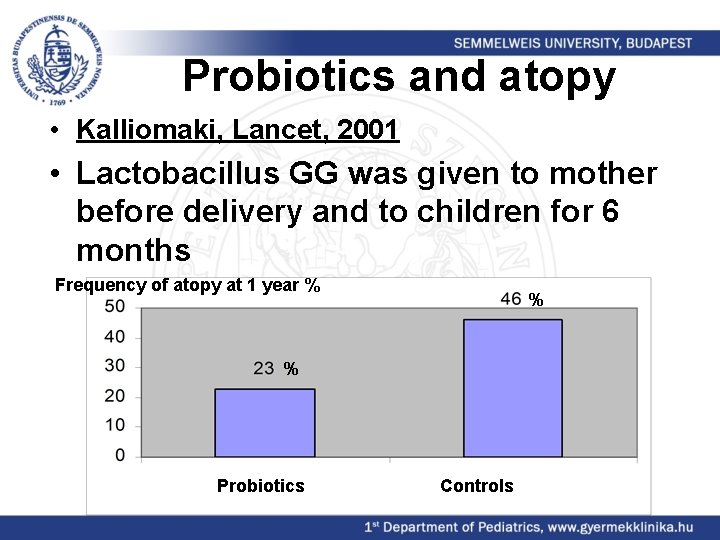
Probiotics and atopy • Kalliomaki, Lancet, 2001 • Lactobacillus GG was given to mother before delivery and to children for 6 months Frequency of atopy at 1 year % % % Probiotics Controls

Feeding of preterms • Carnitin, taurin • LC-PUFA, MCT • Phosphate crosses placenta in the last 3 months • Iodine, selenium
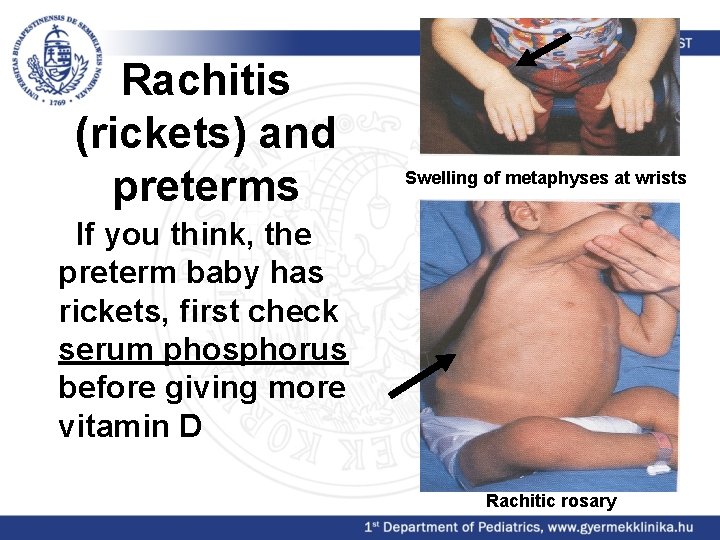
Rachitis (rickets) and preterms Swelling of metaphyses at wrists If you think, the preterm baby has rickets, first check serum phosphorus before giving more vitamin D Rachitic rosary


Somatic development of breast fed infants II. • After 3 years no difference can be detected in length of breast fed and formula fed children • The weight of formula fed babies is always higher, among them the frequency of obesity is high

Contraindications of breast feeding • From the mother’s part – Severe acut or chronic infections (typhus, erysipelas, tuberculosis, AIDS) – Sepsis – Postpartum psychosis • From the infant’s part – Some types of inborn error of metabolism (galactosaemia, some forms of glycogenosis)

Difficulties of breast feeding • Mother’s side – Mamilla rhagad – Papilla plana inverta • Infant’s side – Cleft palate – Missing sucking reflex (prematurity, cerebral impairment) – Severe rhinitis

Fruits • First apple and peach • other recommended fruits seasonal fruits – sour cherry – pealed plum – pear – orange, lemon, banana • Fruit juices and mashed form

Vegetables • First is the potato • Following with carrots, beetroot, lettuce, pumpkin, Brussels sprout, spinach, bean, green peas, asparagus • Savoy, cauliflower only after 8 months • Spinach, sorrel have high oxalate content therefore only once a week

Meats and egg • Fish is advantageous because of its fatty acid composition, but it may cause allergic reactions. • Chicken liver once a week • Egg yolk after 8 moths • Egg white after 1 year
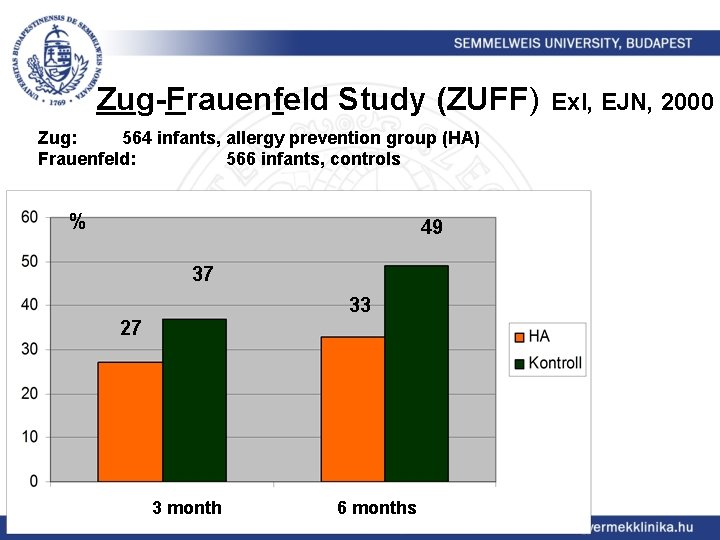
Zug-Frauenfeld Study (ZUFF) Zug: 564 infants, allergy prevention group (HA) Frauenfeld: 566 infants, controls % 49 37 33 27 3 month 6 months Exl, EJN, 2000

Ten Steps to Successful Breastfeeding(WHO/UNICEF) 1. Have a written breastfeeding policy that is routinely communicated to all health care staff 2. Train all health care staff in skills necessary to implement this policy 3. Inform all pregnant women about the benefits and management of breastfeeding

Ten Steps to Successful Breastfeeding(WHO/UNICEF) 4. Help mothers initiate breastfeeding within a half-hour of birth 5. Show mothers how to breastfeed, and how to maintain lactation even if they should be separated from their infants 6. Give newborn infants no food or drink other than breastmilk, unless medically indicated 7. Practice rooming-in: allow mothers and infants to remain together 24 hours a day

Ten Steps to Successful Breastfeeding(WHO/UNICEF) 8. Encourage breastfeeding on demand 9. Give no arteficial teats or pacifiers (also called dummies or soothers) to breastfeeding infants. 10. Foster the establishment of breastfeeding support groups and refer mothers to them on discharge from the hospital or clinic

Utilization of breast milk’s proteins • Total protein content 11 g/l, from which only 9 g/l is utilized for nutrition. • Secretory Ig. A, lactoferrin and lizozym are not used for nutrition • Only 13 % of urea can be used for aminoacid synthesis

How to decrease allergenity? • Heating, home-canning is good: apple, celery, fish BUT not good: cow’s milk, eggs • Gene technology (rice, wheat) • Enzymatic hydrolysis Special formulas: hypoallergen (HA)

Why should not be given formula instead of breast milk after birth? • Frequency of cow’s milk allergy in breast fed infants 0. 4% • But: every child was given formula in the hospital! Host, Acta Paed Scand, 1988 40 ml cow’s milk contains: -lactoglobulin (main allergen in cow’s milk) 1 litre of breast milk/day for 21 years !!!

Role of nucleotides I. • Although they can be synthetised, in infants nucleotides are semiessencial compounds as the rate of their endogen synthesis is not sufficient to the normal functions • Breast milk contains nucleotides in higher concentration than the cow’s milk and formulas

Role of nucleotides II. • Nucleotids help the development of intestinal mucosa and improve the absorption of different nutritients • They promote the growth of Bifidobacteria • Increase the cellular and humoral immune response

Erythropoietin (Epo) • Breast milk (BM): Epo (Kling, Pediatr Res, 1998) • Per os Epo can be absorbed BM protects Protease activity Intestinal permeability

What is the role of EPO in BM? • No effect on erythropoesis • Epo: trophic factor in the intestine (Juul, Gut, 2001) intestine Epo receptor EPO
- Slides: 73