Increasing Compliance of Preprocedural ABIs Megan Pepin RN

Increasing Compliance of Pre-procedural ABIs Megan Pepin, RN- Program Manager, Michelle Farneman, RN Sr. Quality Manager, Shelby Hamilton, RN, BSN, Dr. Jean Starr, Dr. Cindy Baker, Dr. Kristine Orion.

Ankle Brachial Index ABI = Ankle Brachial Index Ratio of highest systolic blood pressure at the ankle divided by the highest systolic blood pressure in the upper arm Quick, cost-effective, non-invasive test to diagnose or follow peripheral artery disease (PAD) Easily available in most medical centers
Pre-procedural ABI comparison over time

Problem Ø The acquisition of ABI studies prior to peripheral vascular interventions were below expected benchmarks for OSUMC service lines performing these interventions. The OSUMC ABI rates have been lower that national VQI rates since we began participating. The 2016 -17 Fall report rate was 68% with the VQI regional rate comparison at 90% and the VQI national rate at 78%. v According to SVS/AHA/ACC guidelines, an Ankle Brachial Index should be conducted on patients presenting with risk factors for PAD so that therapeutic interventions known to diminish their increased risk of myocardial infarction (MI), stroke, and death may be offered.
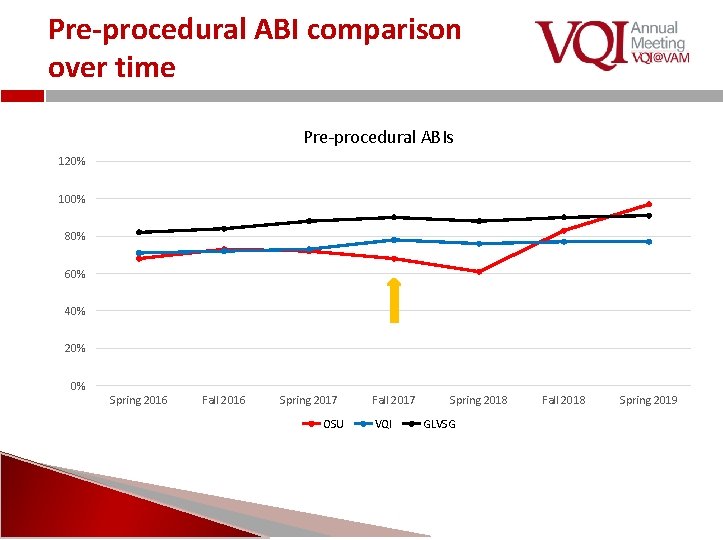
Pre-procedural ABI comparison over time Pre-procedural ABIs 120% 100% 80% 60% 40% 20% 0% Spring 2016 Fall 2016 Spring 2017 OSU Fall 2017 VQI Spring 2018 GLVSG Fall 2018 Spring 2019

Goal OSUMC will improve rate of pre-procedural ABI testing to 78% by December 31, 2018.
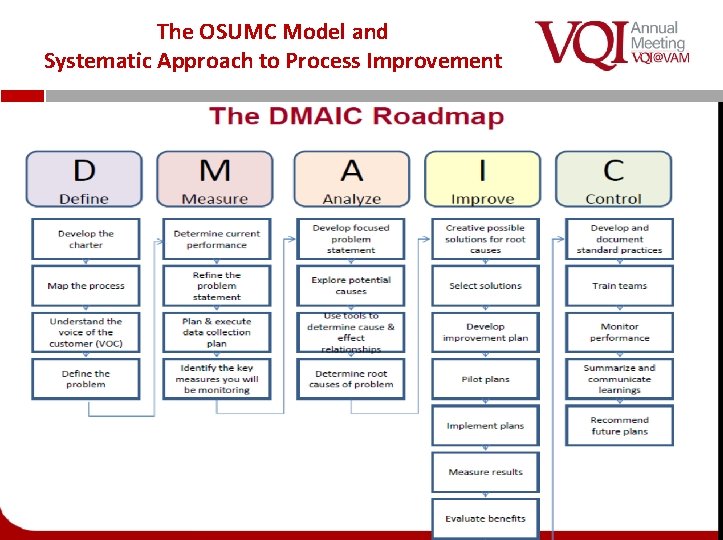
The OSUMC Model and Systematic Approach to Process Improvement

Process Using DMAIC methodology a process improvement team was developed consisting of Quality, Vascular, and Interventional Cardiology. v A retrospective analysis was completed including 2016 -2017 cases that did not have pre-procedural ABIs to identify areas for improvement.

Improvement Strategies Provide education to Interventional Cardiology and Vascular Surgery regarding importance of ABI studies and potential associated mortality/morbidity, review of current performance, and establish target benchmarks. Align clinical practices’ pre-procedural testing guidelines within all disciplines. Created a patient database Established monthly reporting process to providers with cases listed as ABI not measured.

Improvement Strategies Follow up phone calls to physician offices to obtain preprocedure testing not found in the EMR. – Educated office staff on scanning/importing offsite records and asked physicians to start dictating ABI results in their notes. Quarterly compliance reports distributed for 1 year and audit of PVI cases to evaluate effectiveness of education, identify challenges, and need for potential changes.
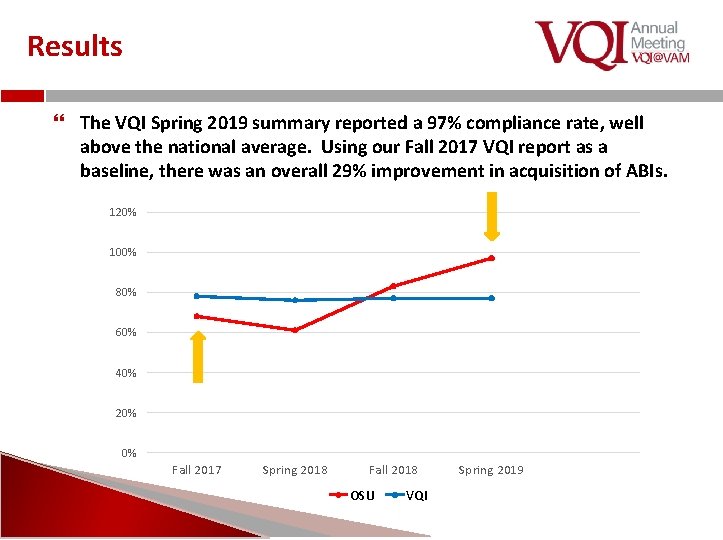
Results The VQI Spring 2019 summary reported a 97% compliance rate, well above the national average. Using our Fall 2017 VQI report as a baseline, there was an overall 29% improvement in acquisition of ABIs. 120% 100% 80% 60% 40% 20% 0% Fall 2017 Spring 2018 Fall 2018 OSU VQI Spring 2019

Challenges/Lessons Learned Variation identified between Vascular surgery and Interventional Cardiology criteria that dictated whether pre -procedural ABIs were completed within the appropriate timeframe. Limitations on outside hospital transfer patients’ records being scanned into the system or made available (i. e. Care Everywhere or being sent with the patient). Patients seen at offsite offices did not always have their ABI testing available in the EMR.

Success Factors Communication along with active engagement of the participating services and physicians. A continual quarterly report outlining current performance and opportunities for improvement. Creating a patient database to track those patients with pre-procedure ABIs captured as “not measured”. v Going forward this database will be utilized to help maintain our results along with quarterly audits and updates to make of the continuation of our success.

Success Factors Utilizing the DMAIC roadmap as a tool helped to focus our process improvement efforts. VQI charter calls-Cheryl Jackson

Questions?
- Slides: 15