Increasing colorectal cancer incidence in young adults in










- Slides: 38

Increasing colorectal cancer incidence in young adults in the US Rebecca Siegel, MPH Early-onset CRC Summit March 19, 2016

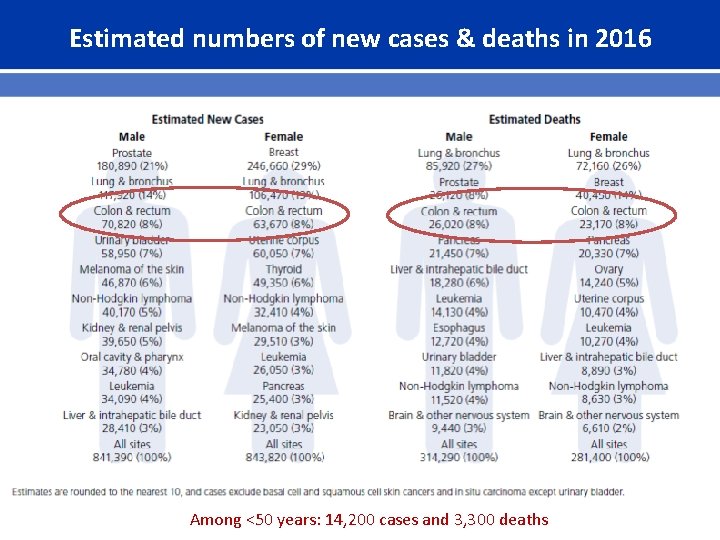
Estimated numbers of new cases & deaths in 2016 Among <50 years: 14, 200 cases and 3, 300 deaths

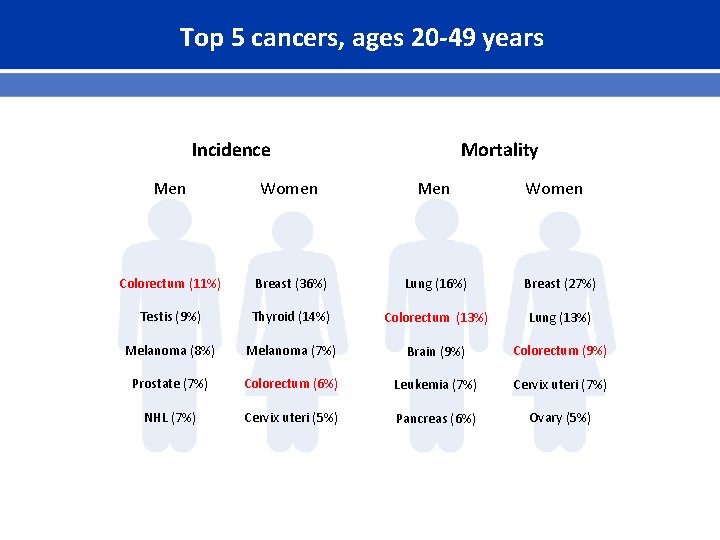
Top 5 cancers, ages 20 -49 years Incidence Mortality Men Women Colorectum (11%) Breast (36%) Lung (16%) Breast (27%) Testis (9%) Thyroid (14%) Colorectum (13%) Lung (13%) Melanoma (8%) Melanoma (7%) Brain (9%) Colorectum (9%) Prostate (7%) Colorectum (6%) Leukemia (7%) Cervix uteri (7%) NHL (7%) Cervix uteri (5%) Pancreas (6%) Ovary (5%)

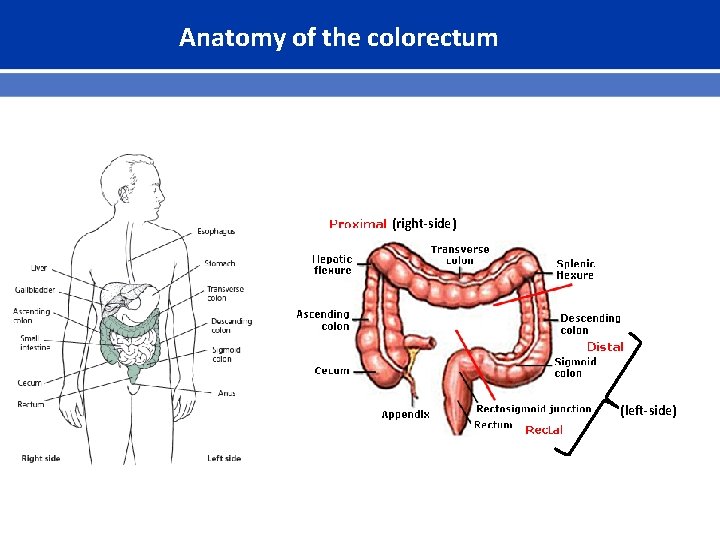
Anatomy of the colorectum (right-side) (left-side)

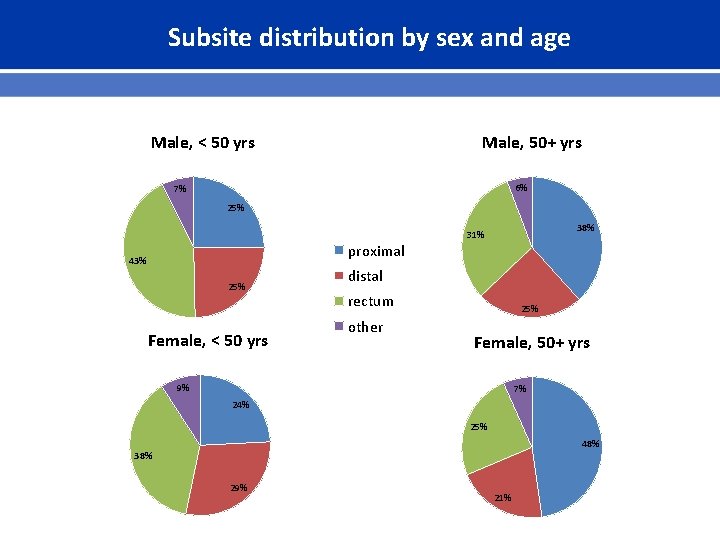
Subsite distribution by sex and age Male, < 50 yrs Male, 50+ yrs 6% 7% 25% proximal 43% 25% Female, < 50 yrs 38% 31% distal rectum other 25% Female, 50+ yrs 9% 7% 24% 25% 48% 38% 29% 21%

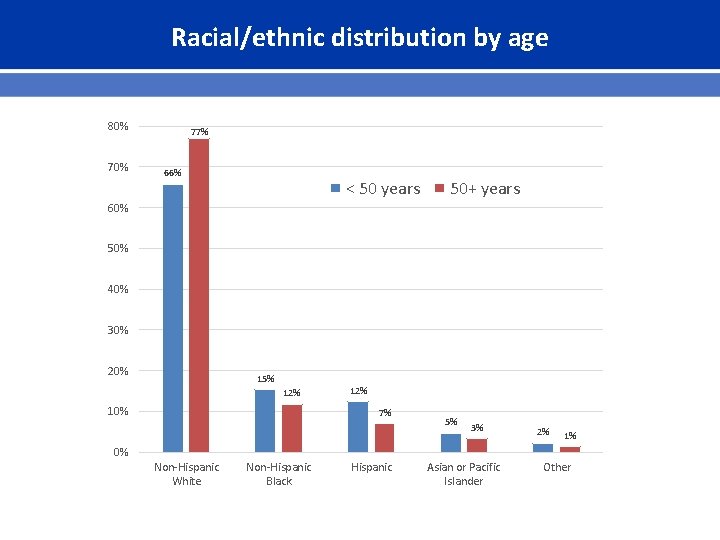
Racial/ethnic distribution by age 80% 77% 66% < 50 years 50+ years 60% 50% 40% 30% 20% 15% 12% 10% 12% 7% 5% 3% 2% 1% 0% Non-Hispanic White Non-Hispanic Black Hispanic Asian or Pacific Islander Other

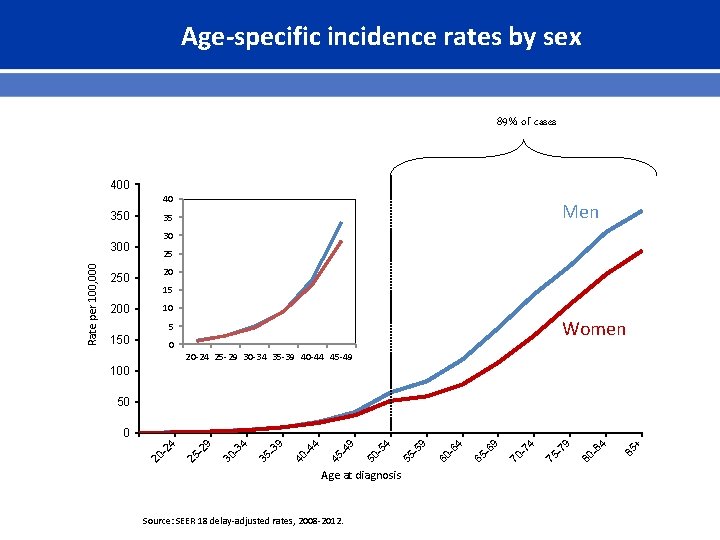
Age-specific incidence rates by sex 89% of cases 400 40 350 200 30 25 20 15 10 Women 5 150 0 20 -24 25 -29 30 -34 35 -39 40 -44 45 -49 100 50 Age at diagnosis Source: SEER 18 delay-adjusted rates, 2008 -2012. + 85 84 80 - 79 75 - 74 70 - 69 65 - 64 60 - 59 55 - 54 50 - 49 45 - 44 40 - 39 35 - 34 30 - 29 25 - 24 0 20 - Rate per 100, 000 300 Men 35

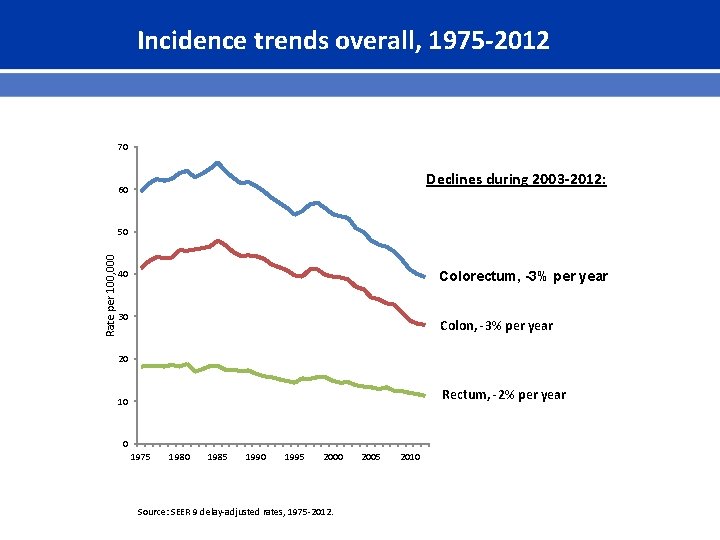
Incidence trends overall, 1975 -2012 70 Declines during 2003 -2012: 60 Rate per 100, 000 50 40 Colorectum, -3% per year 30 Colon, -3% per year 20 Rectum, -2% per year 10 0 1975 1980 1985 1990 1995 2000 Source: SEER 9 delay-adjusted rates, 1975 -2012. 2005 2010

Delayed awareness of the increasing trend The American Surgeon, Sept 1998 LSU Medical Ctr, 37 patients < 40 1976 -1997 The American Surgeon, Oct 2003 SEER 9, 5, 383 patients 20 -39 1973 -1999 Cancer Epidemiol, Biomarkers, & Prevention, June 2009 SEER 13, 20, 646 patients 20 -49 1992 -2005

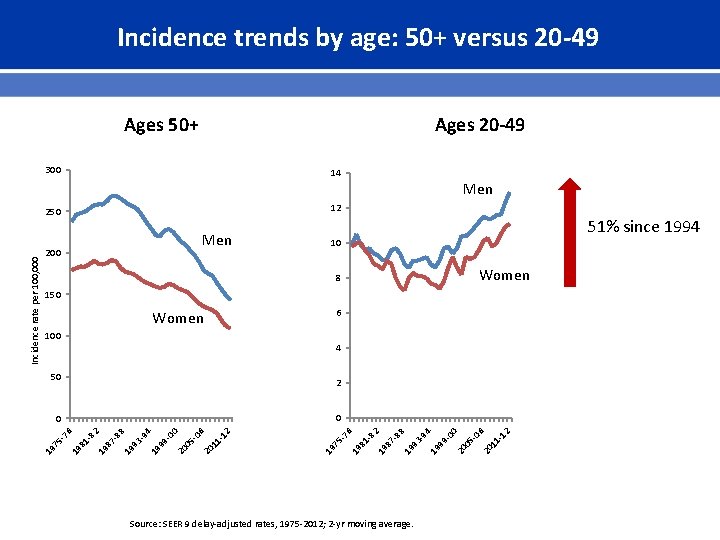
Incidence trends by age: 50+ versus 20 -49 Ages 50+ 300 14 12 250 Men 200 51% since 1994 10 Women 8 150 6 Women 100 4 50 2 Source: SEER 9 delay-adjusted rates, 1975 -2012; 2 -yr moving average. 112 20 1 506 20 0 900 19 9 394 19 9 788 19 8 182 19 8 576 19 7 576 0 0 19 7 Incidence rate per 100, 000 Men

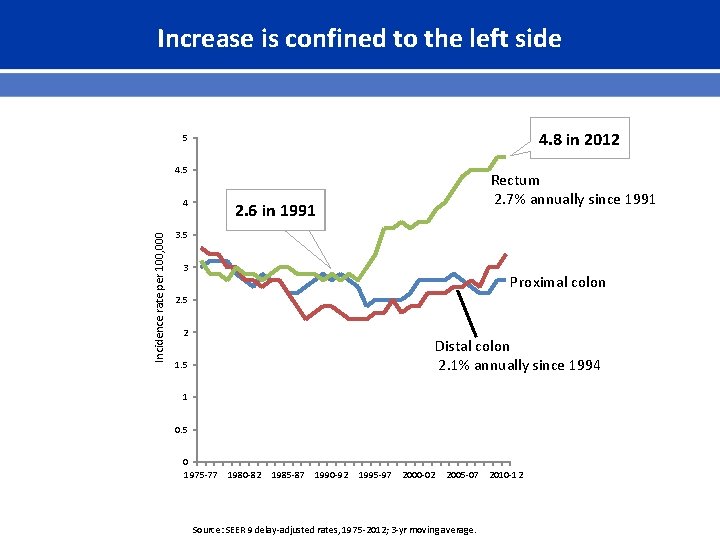
Increase is confined to the left side 4. 8 in 2012 5 4. 5 Incidence rate per 100, 000 4 Rectum 2. 7% annually since 1991 2. 6 in 1991 3. 5 3 Proximal colon 2. 5 2 Distal colon 2. 1% annually since 1994 1. 5 1 0. 5 0 1975 -77 1980 -82 1985 -87 1990 -92 1995 -97 2000 -02 2005 -07 Source: SEER 9 delay-adjusted rates, 1975 -2012; 3 -yr moving average. 2010 -12

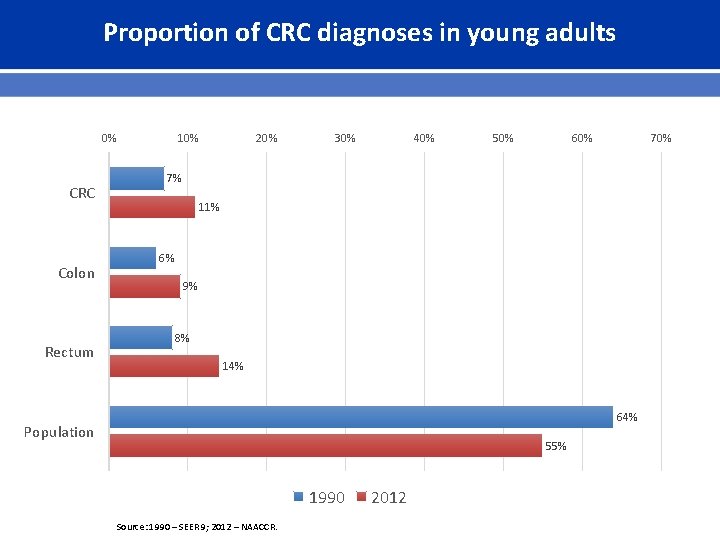
Proportion of CRC diagnoses in young adults 0% CRC Colon Rectum 10% 20% 30% 40% 50% 60% 7% 11% 6% 9% 8% 14% 64% Population 55% 1990 Source: 1990 – SEER 9; 2012 – NAACCR. 2012

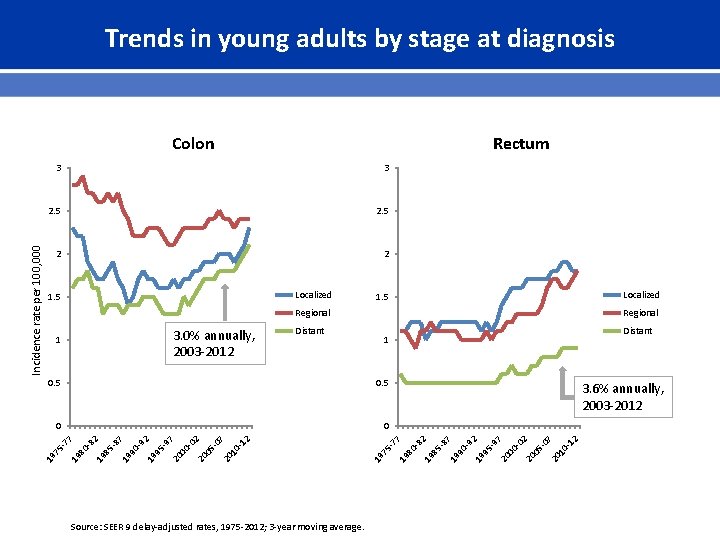
Trends in young adults by stage at diagnosis Rectum 3 3 2. 5 2 2 Localized 1. 5 Regional 012 507 20 1 20 0 002 20 0 597 092 19 9 19 8 587 3. 6% annually, 2003 -2012 577 19 7 012 507 20 1 20 0 002 20 0 19 9 19 8 19 7 597 0 092 0 587 0. 5 082 0. 5 Source: SEER 9 delay-adjusted rates, 1975 -2012; 3 -year moving average. Distant 1 082 Distant Regional 19 8 3. 0% annually, 2003 -2012 1 577 Incidence rate per 100, 000 Colon

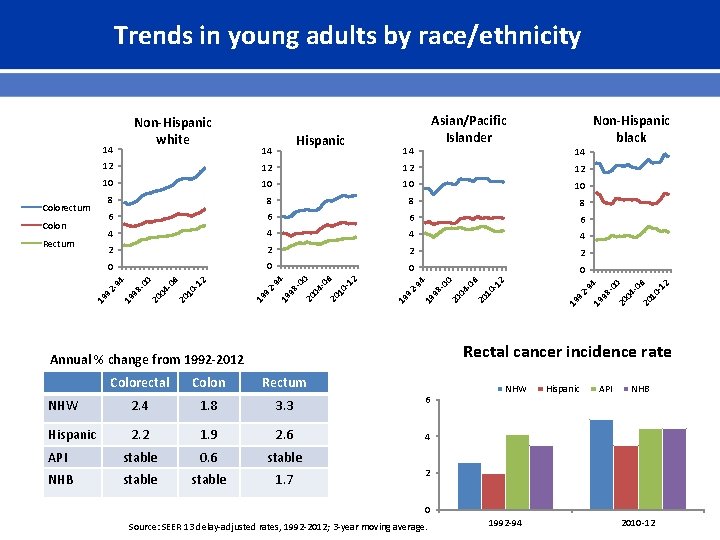
Trends in young adults by race/ethnicity 6 4 4 2 2 0 0 Colon 294 19 9 20 1 20 0 19 9 20 1 19 9 Rectal cancer incidence rate Annual % change from 1992 -2012 Colorectal 012 6 406 6 800 8 6 294 8 012 8 406 10 8 800 10 294 10 012 12 10 406 12 294 Rectum 14 12 20 0 Colon 14 12 800 Colorectum Hispanic 14 Non-Hispanic black 80 20 0 04 -0 20 6 10 -1 2 14 Asian/Pacific Islander 19 9 Non-Hispanic white Rectum NHW 2. 4 1. 8 3. 3 6 Hispanic 2. 2 1. 9 2. 6 4 API stable 0. 6 stable NHB stable 1. 7 NHW Hispanic API NHB 2 0 Source: SEER 13 delay-adjusted rates, 1992 -2012; 3 -year moving average. 1992 -94 2010 -12

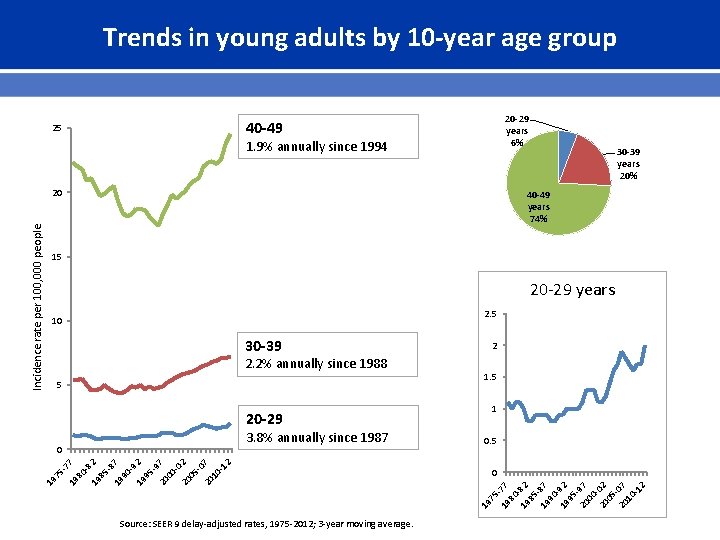
Trends in young adults by 10 -year age group 20 -29 years 6% 40 -49 25 1. 9% annually since 1994 40 -49 years 74% 15 20 -29 years 2. 5 10 30 -39 2. 2% annually since 1988 5 20 -29 3. 8% annually since 1987 1. 5 1 0. 5 0 19 7 57 19 7 80 -8 19 2 85 -8 19 7 90 -9 19 2 95 -9 20 7 00 -0 20 2 05 -0 20 7 10 -1 2 0 2 519 77 80 19 82 85 19 87 90 19 92 95 20 97 00 20 02 05 20 07 10 -1 2 Incidence rate per 100, 000 people 20 30 -39 years 20% Source: SEER 9 delay-adjusted rates, 1975 -2012; 3 -year moving average.

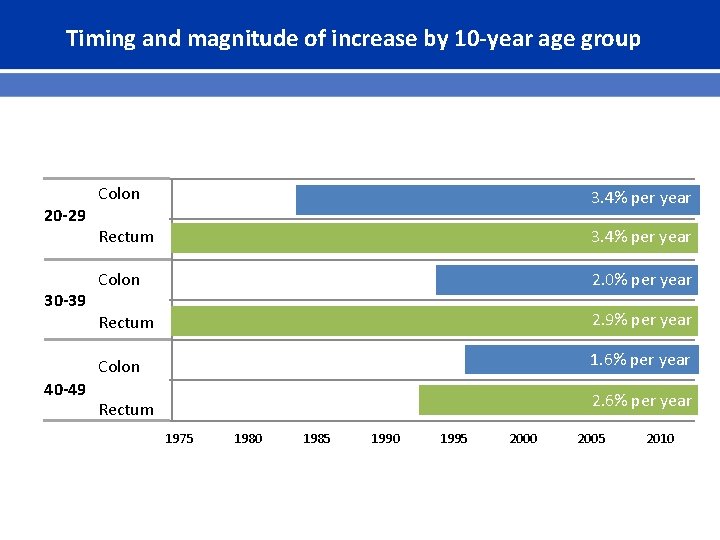
Timing and magnitude of increase by 10 -year age group 20 -29 30 -39 40 -49 Colon 3. 4% per year Rectum 3. 4% per year Colon 2. 0% per year Rectum 2. 9% per year Colon 1. 6% per year Rectum 2. 6% per year 1975 1980 1985 1990 1995 2000 2005 2010

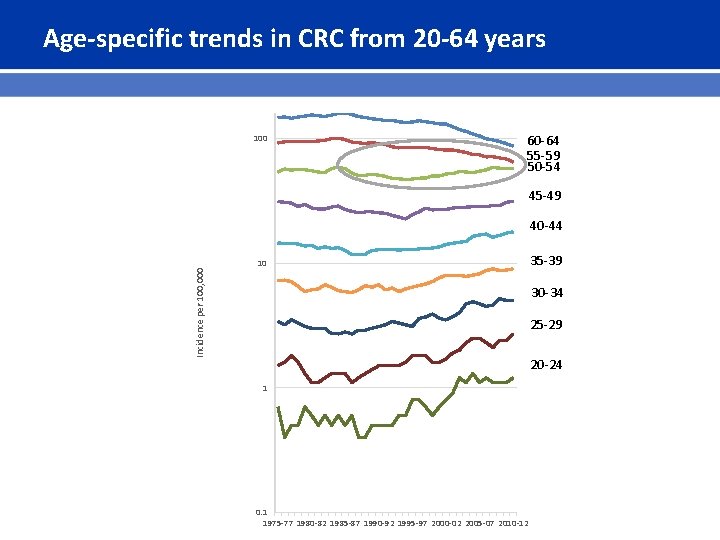
Age-specific trends in CRC from 20 -64 years 100 60 -64 55 -59 50 -54 45 -49 Incidence per 100, 000 40 -44 10 35 -39 30 -34 25 -29 20 -24 1 0. 1 1975 -77 1980 -82 1985 -87 1990 -92 1995 -97 2000 -02 2005 -07 2010 -12

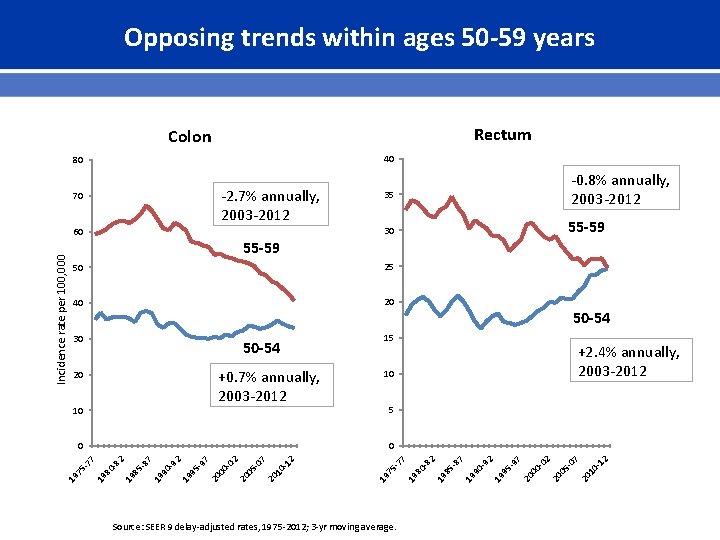
Opposing trends within ages 50 -59 years Rectum Colon 40 80 -2. 7% annually, 2003 -2012 70 55 -59 50 25 40 20 30 50 -54 +0. 7% annually, 2003 -2012 20 10 50 -54 15 +2. 4% annually, 2003 -2012 10 5 Source: SEER 9 delay-adjusted rates, 1975 -2012; 3 -yr moving average. 012 20 1 507 20 0 002 20 0 597 19 9 092 19 9 587 19 8 082 19 8 577 0 0 19 7 55 -59 30 19 7 Incidence rate per 100, 000 60 -0. 8% annually, 2003 -2012 35

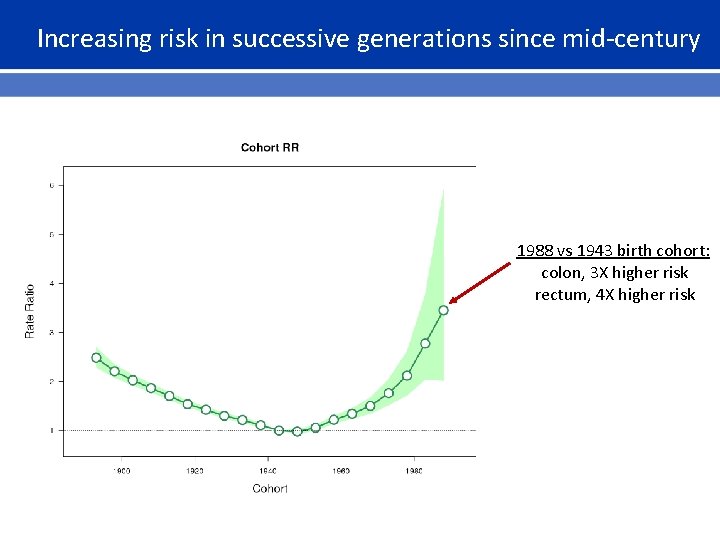
Increasing risk in successive generations since mid-century 1988 vs 1943 birth cohort: colon, 3 X higher risk rectum, 4 X higher risk

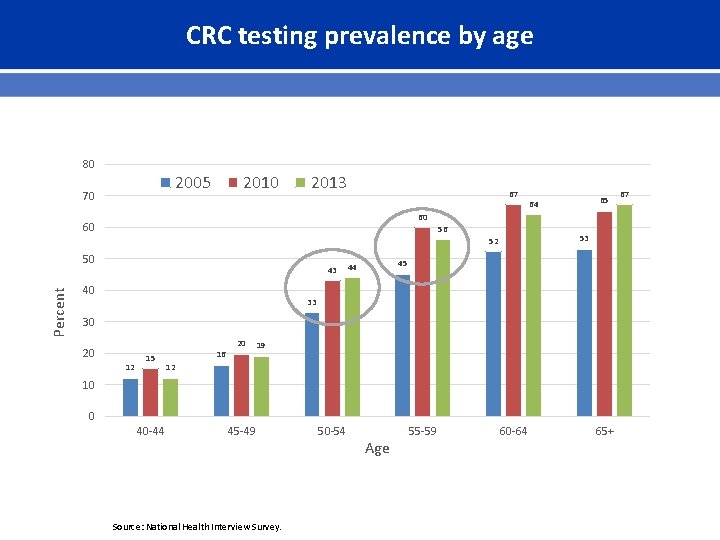
CRC testing prevalence by age 80 2005 70 2013 67 60 60 56 53 52 50 Percent 65 64 43 40 45 44 33 30 20 12 15 16 20 19 12 10 0 40 -44 45 -49 Source: National Health Interview Survey. 50 -54 Age 55 -59 60 -64 65+ 67

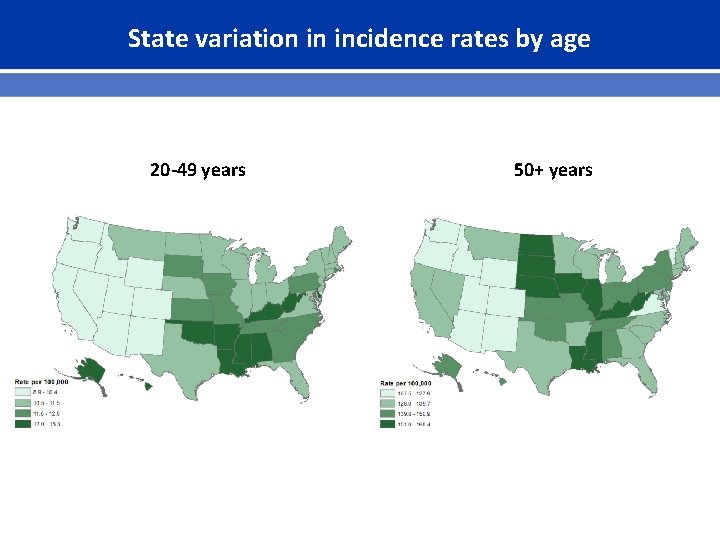
State variation in incidence rates by age 20 -49 years 50+ years

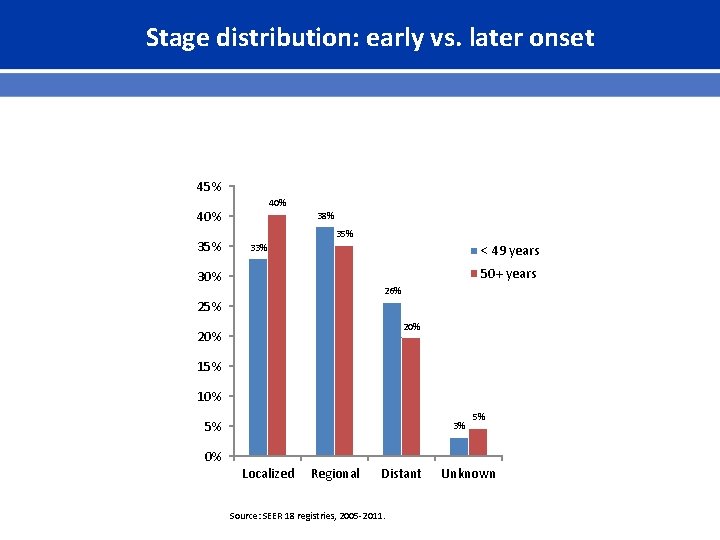
Stage distribution: early vs. later onset 45% 40% 35% 38% 35% 33% < 49 years 50+ years 30% 26% 25% 20% 15% 10% 5% 3% 5% 0% Localized Regional Distant Source: SEER 18 registries, 2005 -2011. Unknown

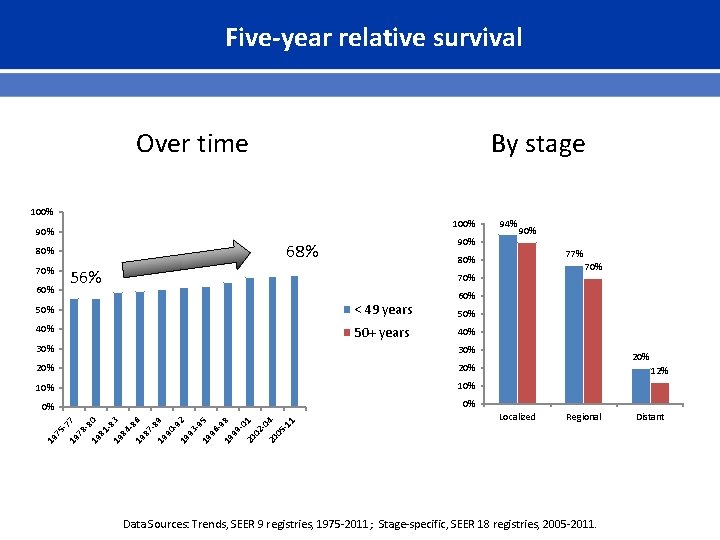
Five-year relative survival Over time By stage 100% 90% 68% 80% 70% 60% 94% 90% 77% 80% 56% 70% 50% < 49 years 40% 50+ years 60% 50% 40% 30% 20% 10% 0% 0% 19 75 -7 19 7 78 -8 19 0 81 -8 19 3 84 -8 19 6 87 -8 19 9 90 -9 19 2 93 -9 19 5 96 -9 19 8 99 -0 20 1 02 -0 20 4 05 -1 1 30% 20% 12% Localized Regional Data Sources: Trends, SEER 9 registries, 1975 -2011; Stage-specific, SEER 18 registries, 2005 -2011. Distant

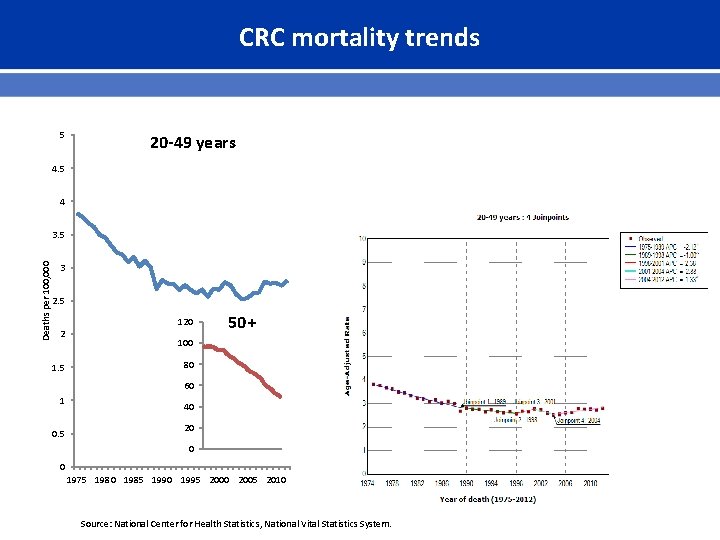
CRC mortality trends 5 20 -49 years 4. 5 4 Deaths per 100, 000 3. 5 3 2. 5 2 1. 5 120 50+ 100 80 60 1 0. 5 40 20 0 0 1975 1980 1985 1990 1995 2000 2005 2010 Source: National Center for Health Statistics, National Vital Statistics System.

Strategies for reducing colorectal cancer risk Ø Maintain a healthy weight Ø Be physically active Ø Consume a healthy diet Ø Limit alcohol consumption Ø Consume recommended levels of calcium Ø Avoid tobacco products Ø Screening at 50, OR earlier with a family history of adenomas or CRC

Who should begin screening before 50? High risk Age to begin Familial adenomatous polyposis (FAP) 10 -12 years Lynch syndrome 20 -25 years* Inflammatory bowel disease (ulcerative colitis or Crohn disease) Varies depending on age at onset *Or 10 years before youngest case in immediate family

Who else should begin screening before 50? Increased risk Age to begin Cancer/adenomas in a first-degree relative 40 years OR 10 years before youngest case Cancer in > 2 second-degree relatives 40 years

Conclusion CRC incidence rates continue to increase in young adults ACTION ITEMS Ø Early screening when appropriate Ø Increase awareness among clinicians and young adults to facilitate earlier detection Ø Know the symptoms 1. Rectal bleeding 2. Abdominal pain 3. Change in bowel habits Ø Etiologic research – known risk factors don’t explain

Thank you!

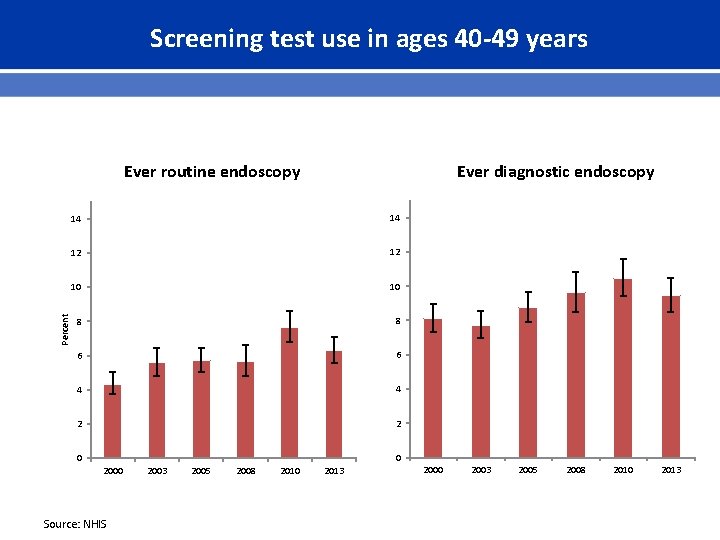
Screening test use in ages 40 -49 years Ever diagnostic endoscopy Percent Ever routine endoscopy 14 14 12 12 10 10 8 8 6 6 4 4 2 2 0 0 2000 Source: NHIS 2003 2005 2008 2010 2013 2000 2003 2005 2008 2010 2013

Why doesn’t screening begin earlier? • Increase unknown during previous evidence review (mid 2000 s) • Now in beginning stages of guideline review; independent, systematic review of the literature, including harms & benefits of screening • Screening before 50 recommended for many people; current evidence will inform guideline update • Benefits must outweigh harms at the population level Ø rare before 50 (absolute risk 0. 3% vs 5% for those 50+) Ø serious adverse events (perforation, adverse reaction to sedation, etc) Ø cost

Harms & limitations of colonoscopy screening • • • 33% of patients report at least 1 GI symptom following the procedure Serious adverse event rate: 2. 8 per 1, 000 Adverse reaction to the sedative Bleeding if a polyp or tissue sample is taken Perforation of the colon wall Screening won’t detect all cancers

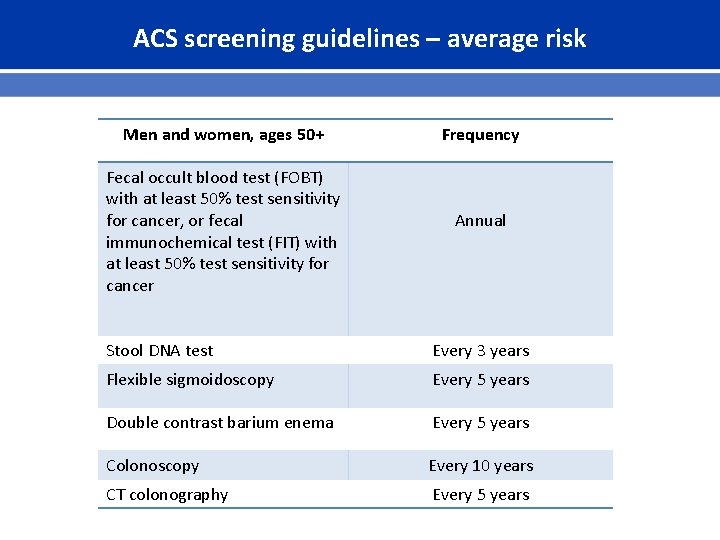
ACS screening guidelines – average risk Men and women, ages 50+ Fecal occult blood test (FOBT) with at least 50% test sensitivity for cancer, or fecal immunochemical test (FIT) with at least 50% test sensitivity for cancer Frequency Annual Stool DNA test Every 3 years Flexible sigmoidoscopy Every 5 years Double contrast barium enema Every 5 years Colonoscopy Every 10 years CT colonography Every 5 years

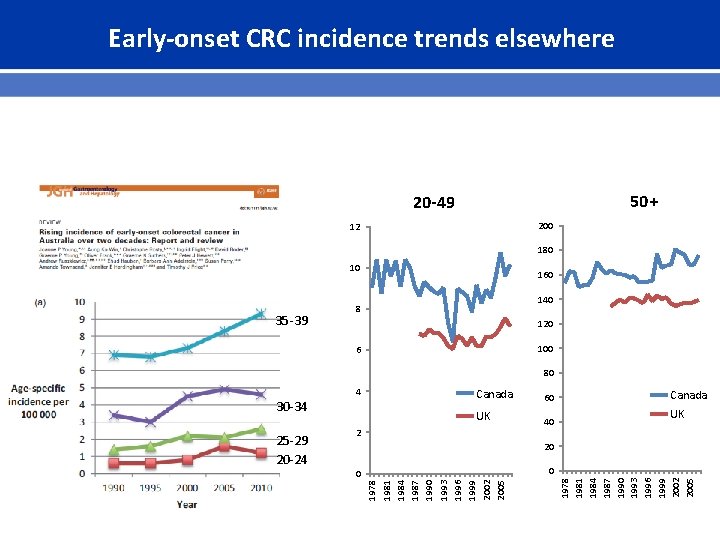
Early-onset CRC incidence trends elsewhere 50+ 20 -49 200 12 180 10 35 -39 160 140 8 120 100 6 80 60 UK 40 2 Canada UK 20 0 0 1978 1981 1984 1987 1990 1993 1996 1999 2002 2005 25 -29 20 -24 Canada 1978 1981 1984 1987 1990 1993 1996 1999 2002 2005 30 -34 4

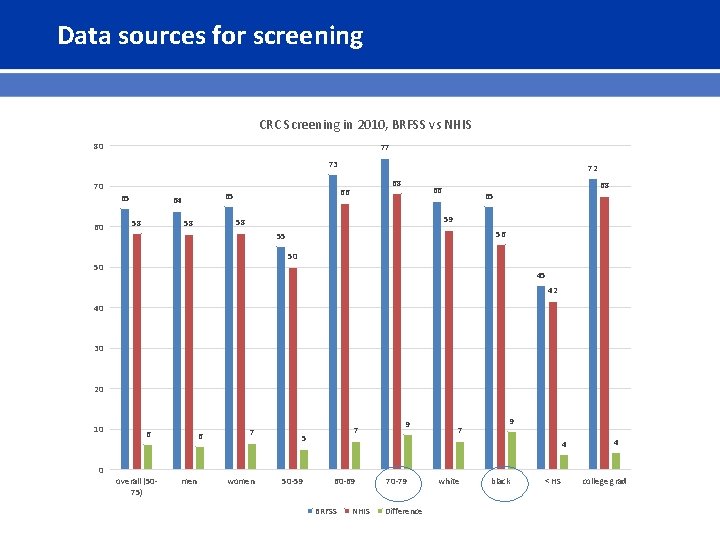
Data sources for screening CRC Screening in 2010, BRFSS vs NHIS 80 77 73 70 65 60 58 68 66 65 64 72 66 59 58 58 68 65 56 55 50 50 45 42 40 30 20 10 0 6 overall (5075) 6 men 7 women 7 5 50 -59 9 9 7 4 60 -69 BRFSS NHIS 70 -79 Difference white black < HS 4 college grad

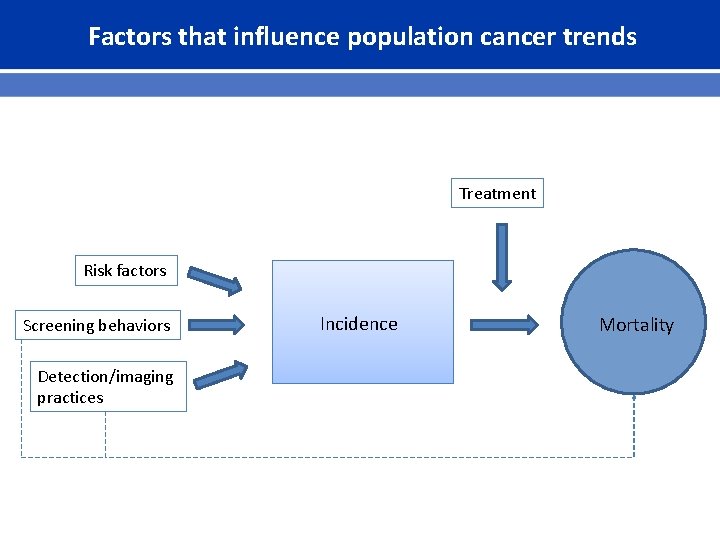
Factors that influence population cancer trends Treatment Risk factors Screening behaviors Detection/imaging practices Incidence Mortality

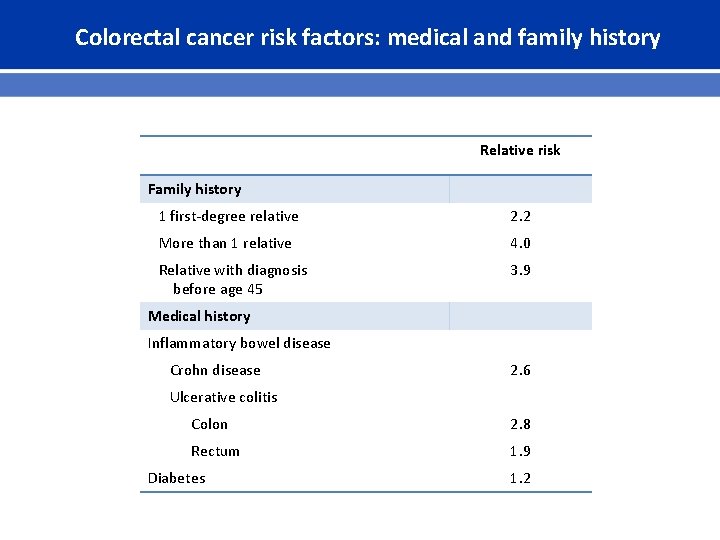
Colorectal cancer risk factors: medical and family history Relative risk Family history 1 first-degree relative 2. 2 More than 1 relative 4. 0 Relative with diagnosis before age 45 3. 9 Medical history Inflammatory bowel disease Crohn disease 2. 6 Ulcerative colitis Colon 2. 8 Rectum 1. 9 Diabetes 1. 2

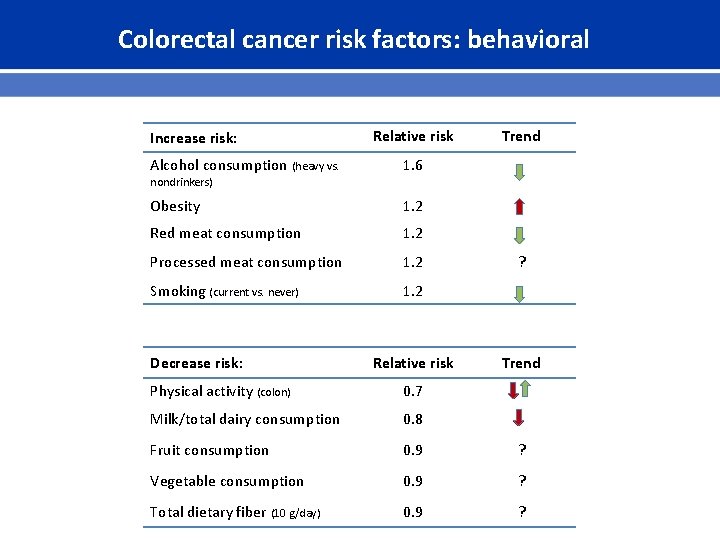
Colorectal cancer risk factors: behavioral Increase risk: Relative risk Alcohol consumption (heavy vs. 1. 6 Obesity 1. 2 Red meat consumption 1. 2 Processed meat consumption 1. 2 Smoking (current vs. never) 1. 2 nondrinkers) Decrease risk: Relative risk Trend ? Trend Physical activity (colon) 0. 7 Milk/total dairy consumption 0. 8 Fruit consumption 0. 9 ? Vegetable consumption 0. 9 ? Total dietary fiber (10 g/day) 0. 9 ?