INCONTINENCEASSOCIATED DERMATITIS Nancy Fox RN BN IIWCC OBJECTIVES

INCONTINENCE-ASSOCIATED DERMATITIS Nancy Fox RN BN IIWCC

OBJECTIVES Describe Incontinence-associated dermatitis (IAD) Differentiate IAD from other conditions Identify who is at risk Discuss assessment and categorization of IAD Identify strategies for prevention and management

DEFINING IAD Skin inflammation manifested as redness with or without blistering, erosion, or loss of the barrier function that occurs as a consequence of chronic or repeated exposure of the skin to urine or fecal matter (Gray, et al 2007)

SIGNIFICANCE OF THE PROBLEM Urinary and/or fecal incontinence reported in 19. 7% of patients in acute care; up to 78. 6% in long term care Of those incontinent patient in acute care…. ~43% have associated skin injury Precise number of patients affected by IAD is not known Prevalence of 5. 6%-50% Incidence of 3. 4%-25%
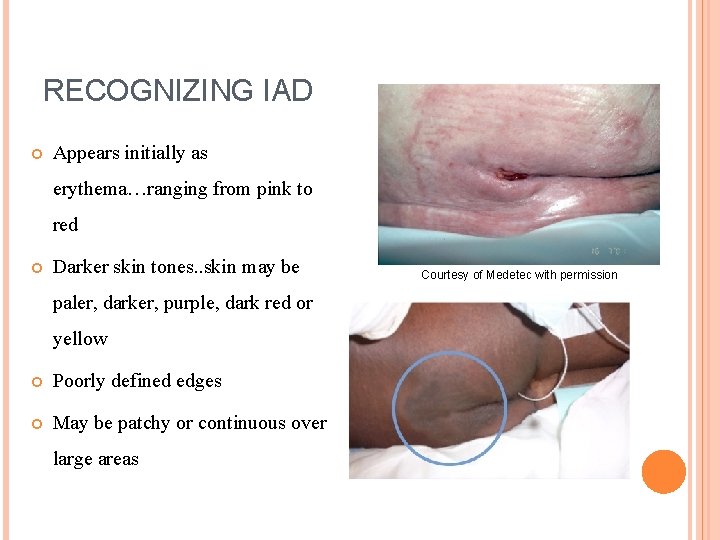
RECOGNIZING IAD Appears initially as erythema…ranging from pink to red Darker skin tones. . skin may be paler, darker, purple, dark red or yellow Poorly defined edges May be patchy or continuous over large areas Courtesy of Medetec with permission
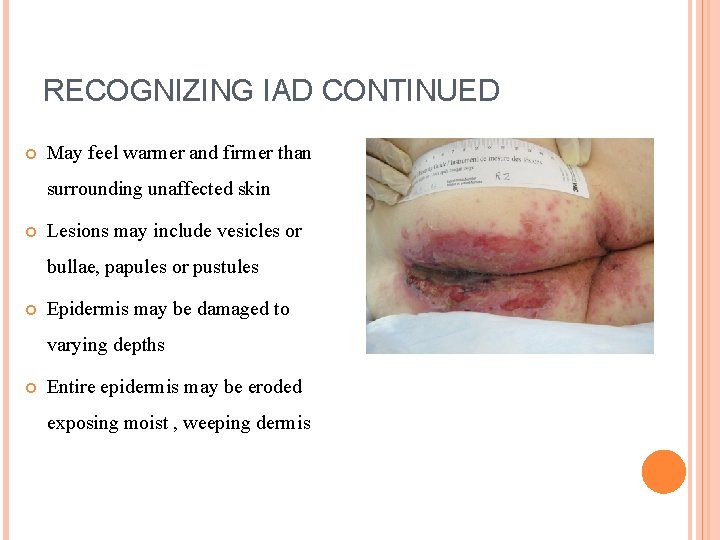
RECOGNIZING IAD CONTINUED May feel warmer and firmer than surrounding unaffected skin Lesions may include vesicles or bullae, papules or pustules Epidermis may be damaged to varying depths Entire epidermis may be eroded exposing moist , weeping dermis
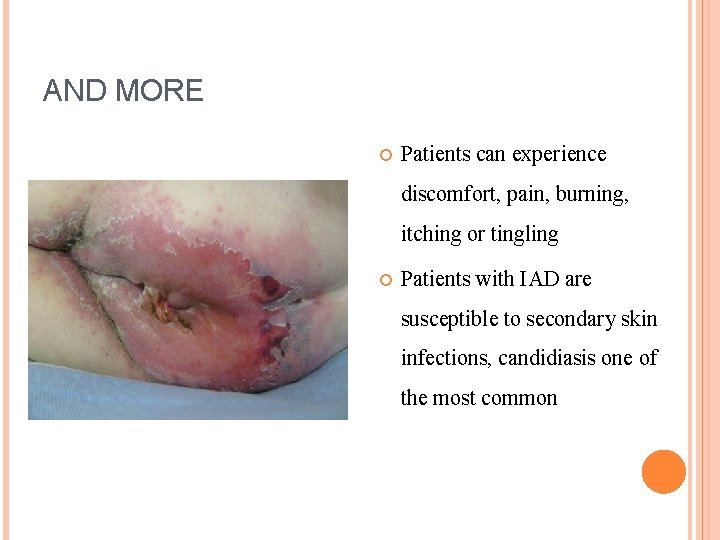
AND MORE Patients can experience discomfort, pain, burning, itching or tingling Patients with IAD are susceptible to secondary skin infections, candidiasis one of the most common
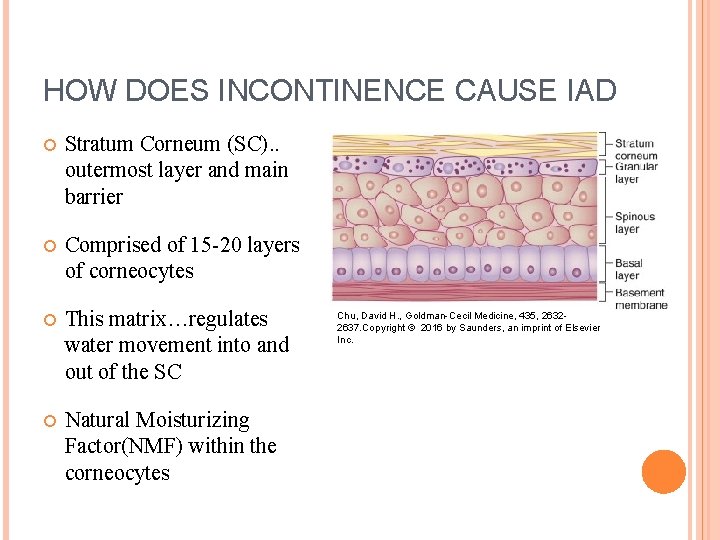
HOW DOES INCONTINENCE CAUSE IAD Stratum Corneum (SC). . outermost layer and main barrier Comprised of 15 -20 layers of corneocytes This matrix…regulates water movement into and out of the SC Natural Moisturizing Factor(NMF) within the corneocytes Chu, David H. , Goldman-Cecil Medicine, 435, 26322637. Copyright © 2016 by Saunders, an imprint of Elsevier Inc.

HOW …CONTINUED Healthy skin surface has acidic p. H 4 -6 Incontinence …water is pulled into and held in the corneocytes Overhydration →swelling and disruption of SC structure (maceration). Irritants more easily penetrate the SC→ inflammation→ more prone to injury from friction

HOW…CONTINUED Exposure to urine and feces ↑p. H. . alkaline which allows microorganisms to thrive and ↑es risk of infection. Feces contain lipid- and protein- digesting enzymes capable of damaging the SC Image provided with permission by Sage Products LLC.
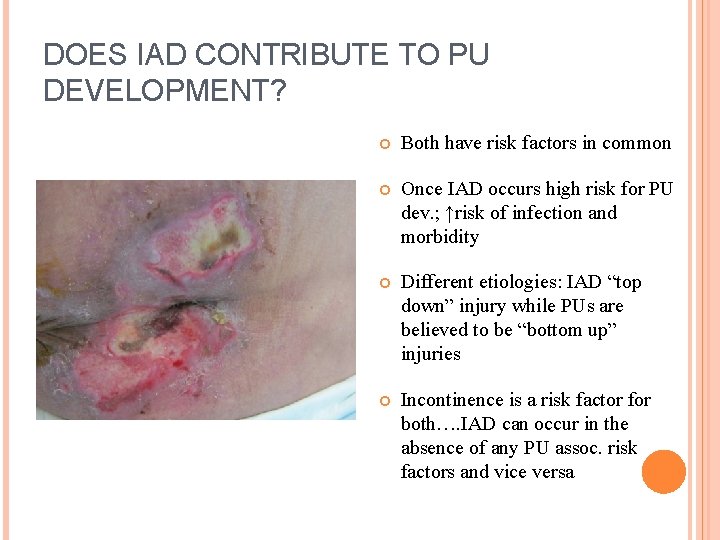
DOES IAD CONTRIBUTE TO PU DEVELOPMENT? Both have risk factors in common Once IAD occurs high risk for PU dev. ; ↑risk of infection and morbidity Different etiologies: IAD “top down” injury while PUs are believed to be “bottom up” injuries Incontinence is a risk factor for both…. IAD can occur in the absence of any PU assoc. risk factors and vice versa

DIFFERENTIATING IAD Pressure Ulcers (PU) Urinary and/or fecal incontinence Pain, burning, itching, tingling Affects perineum, perigenital area. Affected area is diffuse with poorly defined edges Exposure to pressure/shear Pain Usually over a bony prominence/assoc. with a medical device Distinct edges or margins

DIFFERENTIATING IAD Pressure Ulcers (PU) Intact skin with erythema, with/without superficial, partial thickness skin loss Secondary superficial skin infection may be present Varies from intact skin with non-blanchable erythema to full-thickness skin loss Secondary soft tissue infection may be present

KEY RISK FACTORS FOR IAD Incontinence; fecal and/or urinary Frequent episodes Use of occlusive containment products Poor skin condition (e. g. due to aging/steroid use/diabetes) Compromized mobility Pain Diminished cognitive awareness Inability to perform personal hygiene Fever Medications (antibiotics, immunosuppressants) Poor nutritional status Critical illness

RISK ASSESSMENT Perineal Assessment Tool (Nix 2002) Validated tool with 87% interrater reliability 4 item tool and assessment based on Type and intensity of irritant Duration of contact with the irritant Condition of perineal skin Presence of contributing factors e. g. low albumin, antibiotics, tube feeding Each item is rated with a score ranging from 1 -3; total scores ranging from 4 (least at risk) to 12 (most at risk)

PREVENTION OF IAD Structured skin care regimen that consists of 2 key interventions: Cleansing the skin…to remove urine and/or feces Protecting the skin…to avoid or minimize exposure to the irritants Restoring (when appropriate) to support and maintain skin barrier function

PRINCIPLES OF CLEANSE Cleanse daily and after every episode of fecal incontinence Use gentle technique with minimal friction, avoid rubbing/scrubbing the skin Avoid standard alkaline soaps Choose a gentle no-rinse liquid cleanser or pre-moistened wipe with a p. H similar to normal skin If possible use a soft, disposable non-woven cloth Gently dry skin if needed after cleansing

PRINCIPLES OF SKIN PROTECTION Apply skin protectant at a frequency consistent with its ability to protect the skin Ensure skin protectant is compatible with any other skin care products e. g. cleansers Apply the skin protectant to all skin that comes in contact with or potentially will contact urine /feces. Image provided with permission by Sage Products LLC.

CHARACTERISTICS OF THE MAIN TYPES OF SKIN PROTECTANTS Principle ingredient Description Notes Petrolatum • Derived from petroleum processing • Common base for ointments Forms occlusive layer ↑ skin hydration Dimethicone Silicone-based Non-occlusive; opaque or becomes transparent after application Acrylate terpolymer Polymer forms a transparent film Does not require removal; transparent Zinc oxide White powder mixed with a carrier to form an opaque cream, ointment or paste Can be difficult to and uncomfortable to remove

RESTORE Additional step to support and maintain the integrity of the skin barrier Use of a topical leave-on skin care product ( often termed moisturizers) Emollients. . contain lipids and are intended to reduce dryness and restore lipid matrix Humectants…function by drawing in and holding water in the SC e. g. urea, alpha hydroxyl acids, glycerin, lanolin or mineral oil Can be used by themselves or in combination with barriers
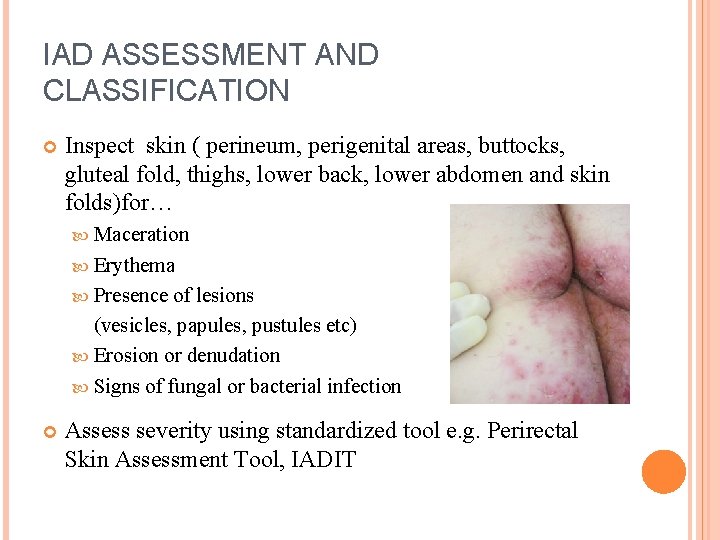
IAD ASSESSMENT AND CLASSIFICATION Inspect skin ( perineum, perigenital areas, buttocks, gluteal fold, thighs, lower back, lower abdomen and skin folds)for… Maceration Erythema Presence of lesions (vesicles, papules, pustules etc) Erosion or denudation Signs of fungal or bacterial infection Assess severity using standardized tool e. g. Perirectal Skin Assessment Tool, IADIT
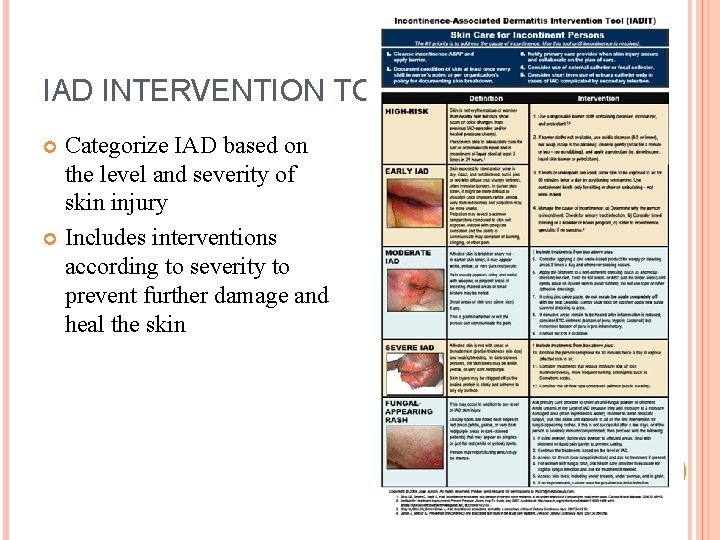
IAD INTERVENTION TOOL Categorize IAD based on the level and severity of skin injury Includes interventions according to severity to prevent further damage and heal the skin

INTERVENTIONS BASED ON SEVERITY OF IAD (IADIT, JOAN JUNKIN 2008) High Risk – skin is not red or warmer than nearby skin; person unable to self care or communicate need; incontinent of stool at least 3 x/24 hours Early or Mild IAD - skin is dry and intact but is pink or red with diffuse, often irregular borders

INTERVENTIONS FOR HIGH RISK AND EARLY IAD Use a disposable barrier cloth containing cleanser, moisturizer, and protectant Use acidic cleanser (p. H 6. 5 or lower), not soap; cleanse gently – no scrubbing; and apply protectant (i. e. dimethicone, liquid skin barrier or petrolatum) Allow skin to be exposed to air for 30 minutes twice daily by positioning semi-prone; Manage cause of incontinence
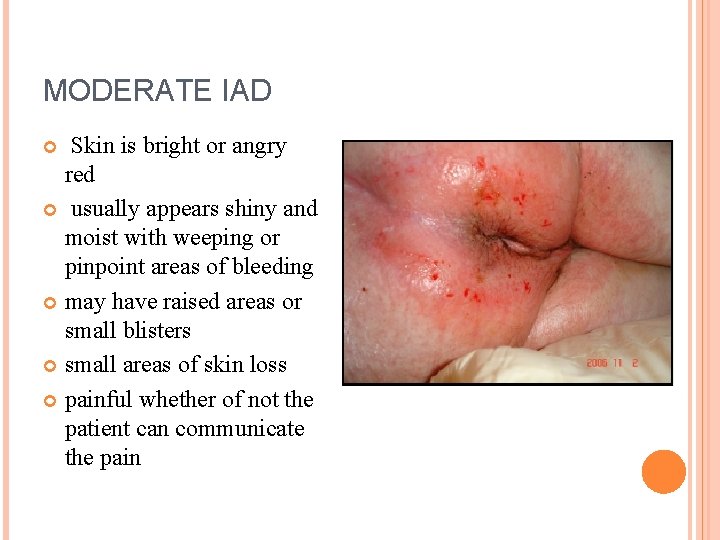
MODERATE IAD Skin is bright or angry red usually appears shiny and moist with weeping or pinpoint areas of bleeding may have raised areas or small blisters small areas of skin loss painful whether of not the patient can communicate the pain

INTERVENTIONS FOR MODERATE IAD Plus… Consider applying zinc oxide-based product for weeping or bleeding areas 3 times daily or following stool episodes May apply ointment to a non-adherent dressing and gently place on injured skin to avoid rubbing Do not scrub the paste completely off…gently soak stool off top then reapply new paste dressing to area If denuded areas remain to be healed after inflammation is reduced, consider BTC ointment (contains Balsam of Peru, trypsin, castor oil)
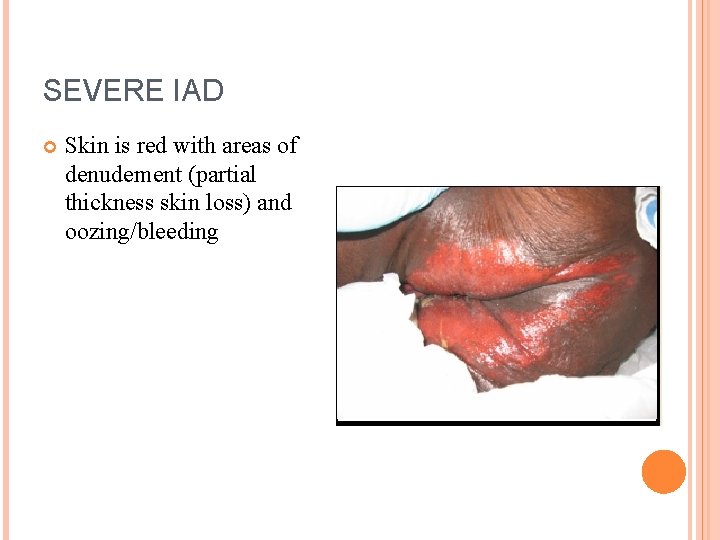
SEVERE IAD Skin is red with areas of denudement (partial thickness skin loss) and oozing/bleeding

INTERVENTIONS FOR SEVERE IAD Plus… Consider treatments that reduce moisture; low air loss mattress/overlay, more frequent turning, astringent such as Domeboro soaks. Consider the air flow type underpads Consider use of external catheter or fecal collector Consider short term use of urinary catheter in cases of IAD complicated by secondary infection
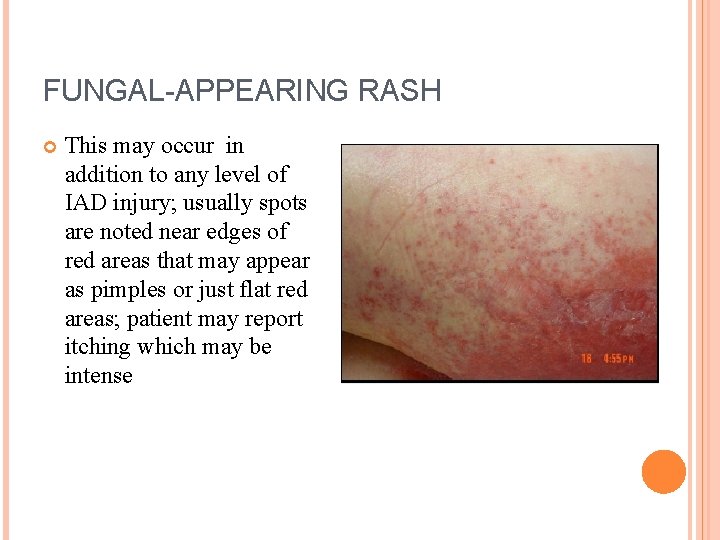
FUNGAL-APPEARING RASH This may occur in addition to any level of IAD injury; usually spots are noted near edges of red areas that may appear as pimples or just flat red areas; patient may report itching which may be intense

INTERVENTIONS FOR FUNGALAPPEARING RASH Anti-fungal powder or ointment ( avoid creams as they add moisture to an already moisture damaged area) If using powder, lightly dust powder to affected areas…seal with ointment or liquid skin barrier to prevent caking Continue treatments according to level of IAD Assess for thrush, and vaginal fungal infection in women Assess skin folds If no improvement, culture area for possible bacterial infection

TAKE HOME POINTS Identify and treat the reversible causes of incontinence Assess the risk of IAD and monitor patient Maximize nutritional intake, hydration and toileting techniques Implement a structured skin care regimen: cleanse, protect and restore Educate patients and caregivers regarding strategies.

REFERENCES Beeckman, D. , et al. Proceedings of the Global IAD Expert Panel. Incontinence –associated dermatitis: moving prevention forward. Wounds International. 2015. Available to download from www. woundsinternational. com. Gray, M. , Bliss, D. Z. , Doughty, D. B. , et al. Incontinence – Associated Dermatitis: a consensus. Journal of Wound, Ostomy, and Continence Nursing. 2007; 34(1): 45 -54. Junkin, J. , Selekof, J. L. Beyond “diaper rash”: Incontinence – associated dermatitis. Does it have you seeing red? Nursing. 2008; 38(11 Suppl. ): 1 -10. Le. Blanc, K. , Christensen, D. , Robbs, L. , et al. Best Practice Recommendations for the Prevention and Management of Incontence-associated Dermatitis. Wound Care Canada. 2010; 8(3): 6 -23.

Questions? THANK YOU!
- Slides: 33