Improving the Transition to Home Rationale Background Discharge
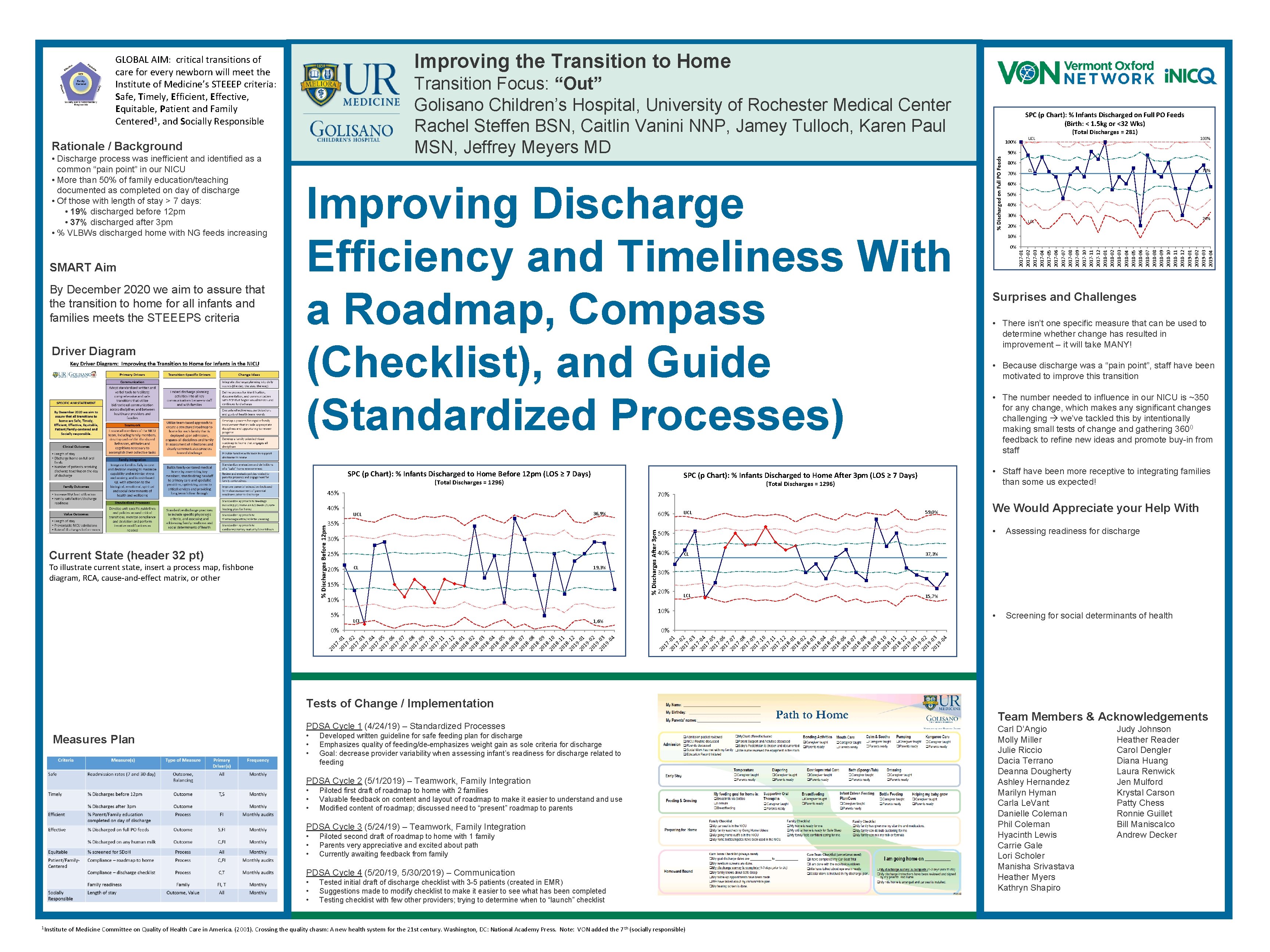
Improving the Transition to Home Rationale / Background • Discharge process was inefficient and identified as a common “pain point” in our NICU • More than 50% of family education/teaching documented as completed on day of discharge • Of those with length of stay > 7 days: • 19% discharged before 12 pm • 37% discharged after 3 pm • % VLBWs discharged home with NG feeds increasing SMART Aim By December 2020 we aim to assure that the transition to home for all infants and families meets the STEEEPS criteria Driver Diagram Improving Discharge Efficiency and Timeliness With a Roadmap, Compass (Checklist), and Guide (Standardized Processes) SPC (p Chart): % Infants Discharged to Home Before 12 pm (LOS ≥ 7 Days) (Total Discharges = 1296) 45% To illustrate current state, insert a process map, fishbone diagram, RCA, cause-and-effect matrix, or other UCL 60% 36, 9% UCL 59, 0% 35% 30% 25% 20% CL 19, 3% 15% 50% 40% 100% CL 70% 90% 80% 70% 60% 50% 40% 30% 24% LCL 10% 0% Surprises and Challenges • There isn’t one specific measure that can be used to determine whether change has resulted in improvement – it will take MANY! • Because discharge was a “pain point”, staff have been motivated to improve this transition • The number needed to influence in our NICU is ~350 for any change, which makes any significant changes challenging we’ve tackled this by intentionally making small tests of change and gathering 3600 feedback to refine new ideas and promote buy-in from staff CL 37, 3% LCL 15, 7% 20% 10% LCL 1, 6% 20 17 20 -01 17 20 -02 17 20 -03 17 20 -04 17 20 -05 17 20 -06 17 20 -07 17 20 -08 17 20 -09 17 20 -10 17 20 -11 17 20 -12 18 20 -01 18 20 -02 18 20 -03 18 20 -04 18 20 -05 18 20 -06 18 20 -07 18 20 -08 18 20 -09 18 20 -10 18 20 -11 18 20 -12 19 20 -01 19 20 -02 19 20 -03 19 -0 4 0% We Would Appreciate your Help With • Assessing readiness for discharge • Screening for social determinants of health 30% 10% 5% UCL 0% 20 17 20 -01 17 20 -02 17 20 -03 17 20 -04 17 20 -05 17 20 -06 17 20 -07 17 20 -08 17 20 -09 17 20 -10 17 20 -11 17 20 -12 18 20 -01 18 20 -02 18 20 -03 18 20 -04 18 20 -05 18 20 -06 18 20 -07 18 20 -08 18 20 -09 18 20 -10 18 20 -11 18 20 -12 19 20 -01 19 20 -02 19 20 -03 19 -0 4 Current State (header 32 pt) 100% 70% % Discharges After 3 pm % Discharges Before 12 pm 40% (Total Discharges = 281) • Staff have been more receptive to integrating families than some us expected! SPC (p Chart): % Infants Discharged to Home After 3 pm (LOS ≥ 7 Days) (Total Discharges = 1296) SPC (p Chart): % Infants Discharged on Full PO Feeds (Birth: < 1. 5 kg or <32 Wks) 2017 -01 2017 -02 2017 -03 2017 -04 2017 -05 2017 -06 2017 -07 2017 -08 2017 -09 2017 -10 2017 -11 2017 -12 2018 -01 2018 -02 2018 -03 2018 -04 2018 -05 2018 -06 2018 -07 2018 -08 2018 -09 2018 -10 2018 -11 2018 -12 2019 -01 2019 -02 2019 -03 2019 -04 Transition Focus: “Out” Golisano Children’s Hospital, University of Rochester Medical Center Rachel Steffen BSN, Caitlin Vanini NNP, Jamey Tulloch, Karen Paul MSN, Jeffrey Meyers MD % Discharged on Full PO Feeds GLOBAL AIM: critical transitions of care for every newborn will meet the Institute of Medicine’s STEEEP criteria: Safe, Timely, Efficient, Effective, Equitable, Patient and Family Centered 1, and Socially Responsible Tests of Change / Implementation PDSA Cycle 1 (4/24/19) – Standardized Processes Measures Plan • • • Developed written guideline for safe feeding plan for discharge Emphasizes quality of feeding/de-emphasizes weight gain as sole criteria for discharge Goal: decrease provider variability when assessing infant’s readiness for discharge related to feeding PDSA Cycle 2 (5/1/2019) – Teamwork, Family Integration • • • Piloted first draft of roadmap to home with 2 families Valuable feedback on content and layout of roadmap to make it easier to understand use Modified content of roadmap; discussed need to “present” roadmap to parents PDSA Cycle 3 (5/24/19) – Teamwork, Family Integration • • • Piloted second draft of roadmap to home with 1 family Parents very appreciative and excited about path Currently awaiting feedback from family PDSA Cycle 4 (5/20/19, 5/30/2019) – Communication • • • 1 Institute Tested initial draft of discharge checklist with 3 -5 patients (created in EMR) Suggestions made to modify checklist to make it easier to see what has been completed Testing checklist with few other providers; trying to determine when to “launch” checklist of Medicine Committee on Quality of Health Care in America. (2001). Crossing the quality chasm: A new health system for the 21 st century. Washington, DC: National Academy Press. Note: VON added the 7 th (socially responsible) Team Members & Acknowledgements Carl D’Angio Molly Miller Julie Riccio Dacia Terrano Deanna Dougherty Ashley Hernandez Marilyn Hyman Carla Le. Vant Danielle Coleman Phil Coleman Hyacinth Lewis Carrie Gale Lori Scholer Manisha Srivastava Heather Myers Kathryn Shapiro Judy Johnson Heather Reader Carol Dengler Diana Huang Laura Renwick Jen Mulford Krystal Carson Patty Chess Ronnie Guillet Bill Maniscalco Andrew Decker
- Slides: 1