Improving Patients Satisfaction by Improving Physicians Communication Skills

Improving Patients’ Satisfaction by Improving Physicians’ Communication Skills Stanton Hudson, MA Associate Director Nick Butler Project Director University of Missouri Center for Health Policy Health Literacy Summit Madison, WI April 14, 2015

Development Team n n n Karen Edison, MD Chair of Dermatology David Fleming, MD Chair of Internal Medicine James Campbell, Ph. D Professor Family Medicine Ioana Staiculescu, MPH Center for Health Policy Nick Butler, Center for Health Policy Stan Hudson, MA Center for Health Policy

Clinic Simulation Video https: //vimeo. com/12827349

Learning objectives n n n Identity health literacy best practices for health professionals. Understand how health literacy best practices can be used in the design and implementation of quality improvement training for health professionals. Implement health literacy quality improvement activities using the AHRQ Universal Precaution Toolkit and the CAHPS Health Literacy Item Set.

Health Literacy Quality Improvement Program n n n The Health Literacy Quality Improvement Program begins with a day-long clinical simulation workshop followed by a year-long health literacy action plan. Tailored action plan to integrate health literacy in the clinical setting Data collection protocol for baseline, 6 -month and 12 -month assessments
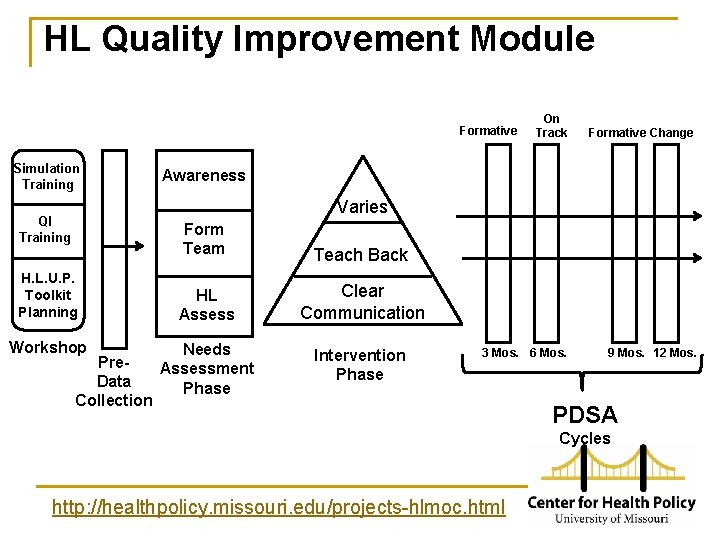
HL Quality Improvement Module On Track Formative Change 3 Mos. 6 Mos. 9 Mos. 12 Mos. Formative Simulation Training Awareness Varies QI Training H. L. U. P. Toolkit Planning Workshop Form Teach Back HL Assess Clear Communication Needs Pre. Assessment Data Phase Collection Intervention Phase PDSA Cycles http: //healthpolicy. missouri. edu/projects-hlmoc. html

Why Simulate? • Provides Standardization of Clinical Training & Assessment • Allows real-life practice of skills in a low-risk environment that encourages dialogue and feedback

Standardized Patients “A normal person who has been carefully coached to accurately portray a specific patient when given the history and physical examination. ” - Barrows, 1993, pg. 444 n Actors who will: • • • Take on characteristics of patient Be able to answer questions about history Give constructive feedback

The Exam Rooms

The Observation Room

Clinical Simulation Workshop n n n A self-reflective clinic simulation exercise to focus the physician’s attention on potential health literacy gaps or challenges encountered in his/her professional practice, A peer learning discussion of specific health literacy strategies, and Opportunities for authentic practice to reinforce knowledge and skills gained from peer learning

Health Literacy Coaching n n Ensuring clear communication and patient understanding Three mandatory tools that learners must include as part of their universal precautions plan q q q Tool 1: Form a team. Tool 2: Assess your practice. Tool 3: Raise awareness.

In addition to the three mandatory tools, learners are given the opportunity to select one additional tool to include in their plan from a list of optional tools. These tools include: q q q Tool 5 The Teach-Back Method Tool 11 Design Easy-to-Read Material Tool 12 Use Health Education Materials Effectively Tool 13 Welcome Patients: Helpful Attitude, Signs, & More Tool 14 Encourage Questions Tool 16 Improve Medication, Adherence, and Accuracy

Quality Improvement Plan n n The physician will need to survey 25 of his/her patients prior to beginning any health literacy activities, to establish baseline data, and again at six and twelve months after the health literacy plan is implemented. Plan-Do-Study-Act method

Plan-Do-Study-Act n n n Tool: Fill in the tool name you are implementing. Step: Fill in the smaller step within that tool you are trying to implement. Cycle: Fill in the cycle number of this PDSA.

Plan-Do-Study-Act- Example 1 n n n TOOL: Patient Feedback STEP: Dissemination of surveys I plan to: We are going to test a process of giving out satisfaction surveys and getting them filled out and back to us. I hope this produces: We hope to get at least 25 completed surveys per week during this campaign. Steps to execute: q q q We will display the surveys at the checkout desk. The checkout attendant will encourage the patient to fill out a survey and put it in the box next to the surveys. We will try this for 1 week.


Patient surveys n n Patient surveys are short and easy to implement Include specific items from the Item Set for Addressing Health Literacy from the Consumer Assessment of Healthcare Providers and Systems (CAHPS) Clinician & Group Survey.

Evaluation n One day workshop: q q n Pre-post survey on knowledge related to health literacy; Face-to face feedback through the session during the simulation cases review and during the coaching session Participant physicians=44
Placeholder for pre-post test results

Evaluation n One year quality improvement program: q q Tailor the survey based on the health literacy tools the provider has chosen Chose a survey methodology based on the clinic resources: n n q n Survey Monkey Paper format Patients surveyed at baseline, 6 months and 12 months Patients surveyed to date=

Sample Survey Items HL 9 – how often did this provider give you all the information you wanted about your health? HL 10 – how often did this provider encourage you to talk about all your health questions or concerns? HL 14 – how often did this provider ask you to describe how you were going to follow these instructions? HL 18 – how often were the results of your blood test, x-ray, or other test easy to understand? HL 21 – how often were these instructions about how to take your medicines easy to understand?
Place holder for patient survey results n Insert results

Lessons Learned n n n Recruitment Challenges Maintenance of Certification Challenges Learner engagement

What questions do you have? For more information please contact: Stan Hudson Center for Health Policy hudsonst@health. missouri. edu (573) 884 -7549
- Slides: 25