Improving Outcomes by Helping People Take Control The

Improving Outcomes by Helping People Take Control The theory and practice of Co -creating Health
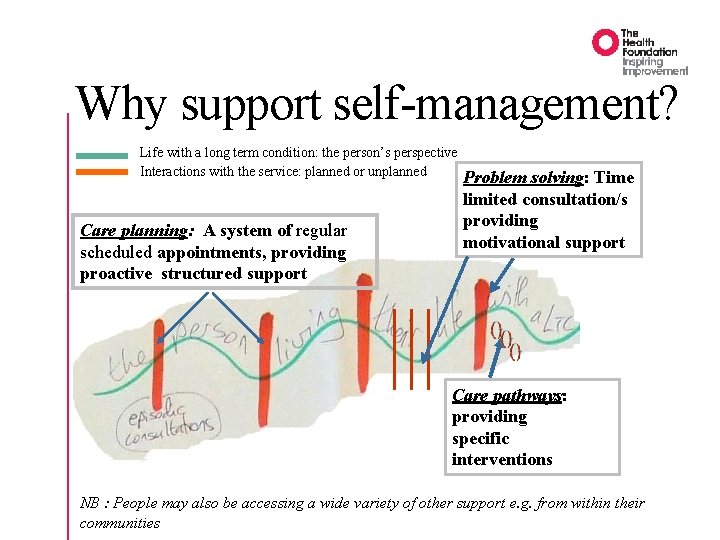
Why support self-management? Life with a long term condition: the person’s perspective Interactions with the service: planned or unplanned Care planning: A system of regular scheduled appointments, providing proactive structured support Problem solving: Time limited consultation/s providing motivational support Care pathways: providing specific interventions NB : People may also be accessing a wide variety of other support e. g. from within their communities

What is supported self-management? “Self management support can be viewed in two ways: as a portfolio of techniques and tools that help patients choose healthy behaviours; and a fundamental transformation of the patientcaregiver relationship into a collaborative partnership. ” Bodenheimer T, Mac. Gregor K, Shafiri C (2005). Helping Patients Manage Their Chronic Conditions. California: California Healthcare Foundation. 3

Co-creating Health Achieve measurable improvements in the quality of life of people living with long term conditions and improve their experience of health services by embedding self management support within mainstream health services. ©The Health Foundation 4

The Chronic Care Model Developed by the Mac. Coll Institute ACP-ASIM Journals and Books 5
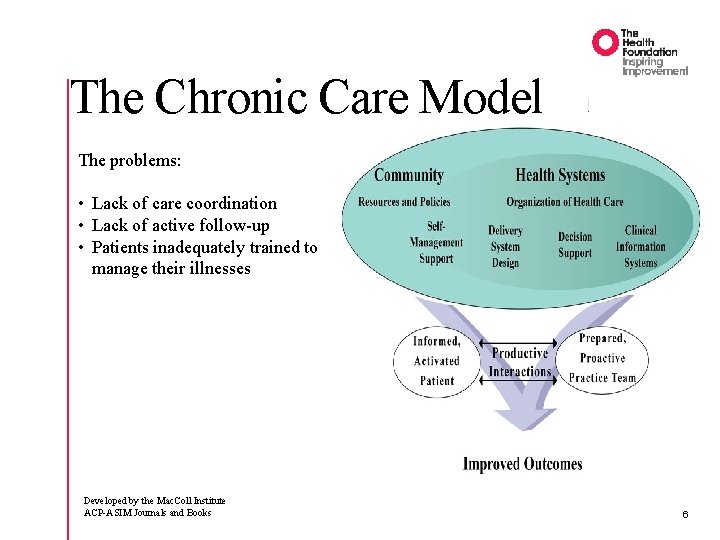
The Chronic Care Model The problems: • Lack of care coordination • Lack of active follow-up • Patients inadequately trained to manage their illnesses Developed by the Mac. Coll Institute ACP-ASIM Journals and Books 6
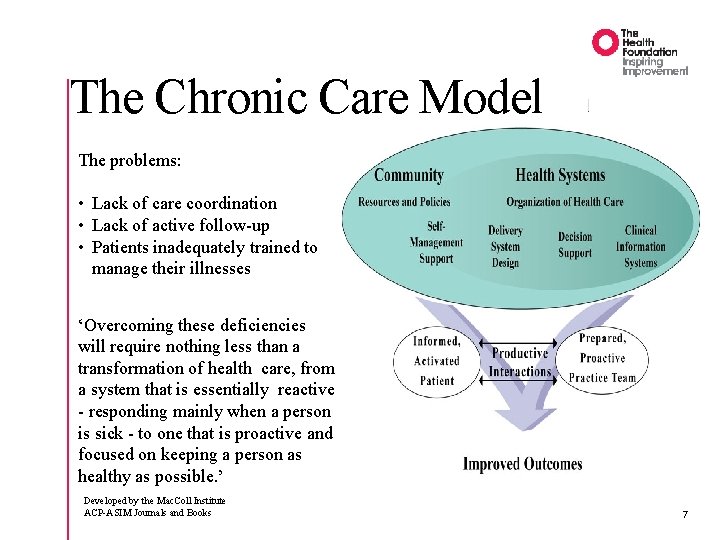
The Chronic Care Model The problems: • Lack of care coordination • Lack of active follow-up • Patients inadequately trained to manage their illnesses ‘Overcoming these deficiencies will require nothing less than a transformation of health care, from a system that is essentially reactive - responding mainly when a person is sick - to one that is proactive and focused on keeping a person as healthy as possible. ’ Developed by the Mac. Coll Institute ACP-ASIM Journals and Books 7
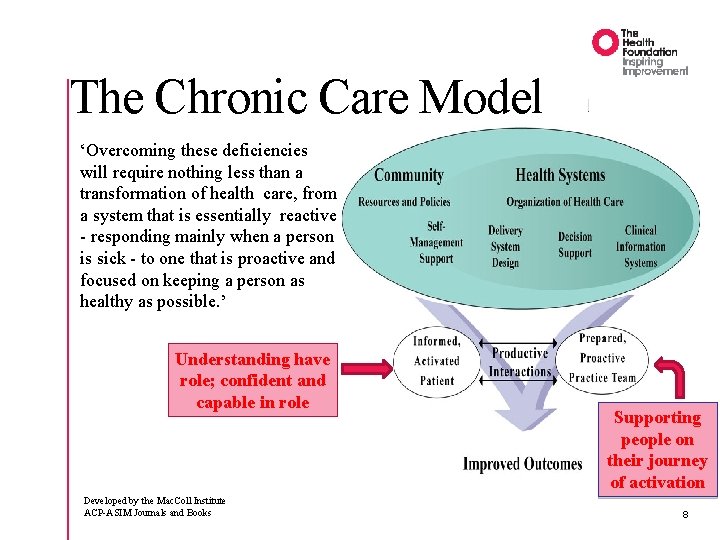
The Chronic Care Model ‘Overcoming these deficiencies will require nothing less than a transformation of health care, from a system that is essentially reactive - responding mainly when a person is sick - to one that is proactive and focused on keeping a person as healthy as possible. ’ Understanding have role; confident and capable in role Developed by the Mac. Coll Institute ACP-ASIM Journals and Books Supporting people on their journey of activation 8

The evidence Evidence for supporting self management grows every year. • Research is up to date • Internationally, studies are consistently positive • Research has used a range of methodologies. • Studies are from small to large scale. It shows that supporting self-management can improve: • • • self confidence / self efficacy self management behaviours quality of life clinical outcomes patterns of healthcare use 9
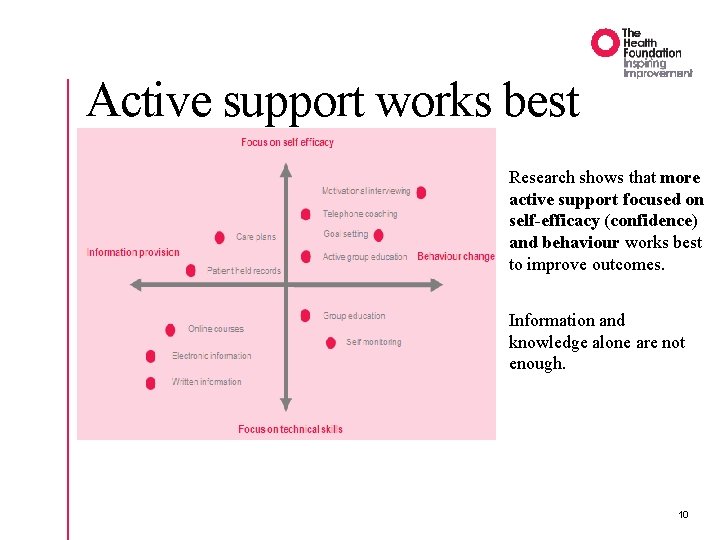
Active support works best Research shows that more active support focused on self-efficacy (confidence) and behaviour works best to improve outcomes. Information and knowledge alone are not enough. 10
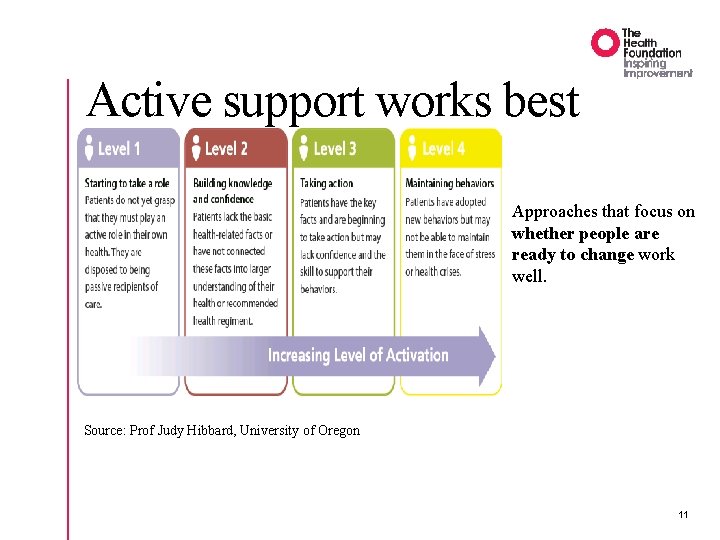
Active support works best Approaches that focus on whether people are ready to change work well. Source: Prof Judy Hibbard, University of Oregon 11

Examples of improvement • Self monitoring and agenda setting reduce hospitalisations, A&E visits, unscheduled visits to the doctor and days off work or school for people with asthma (Gibson et al 2004). • Goal setting for older women with heart conditions reduces days in hospital and overall healthcare costs (Wheeler et al 2003). • Telephone support may improve self care behaviour, glycaemic control, and symptoms among vulnerable people with diabetes (Piette et al 2000). • Motivational interviewing improve self efficacy, patient activation, lifestyle change and perceived health status (Linden et al 2010). • Individual education and group sessions improve symptoms for people with high blood pressure (Boulware et al 2001). 12
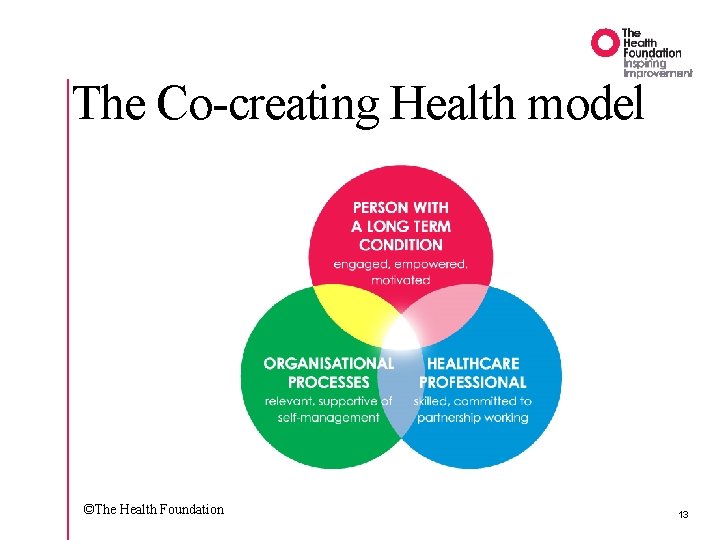
The Co-creating Health model ©The Health Foundation 13
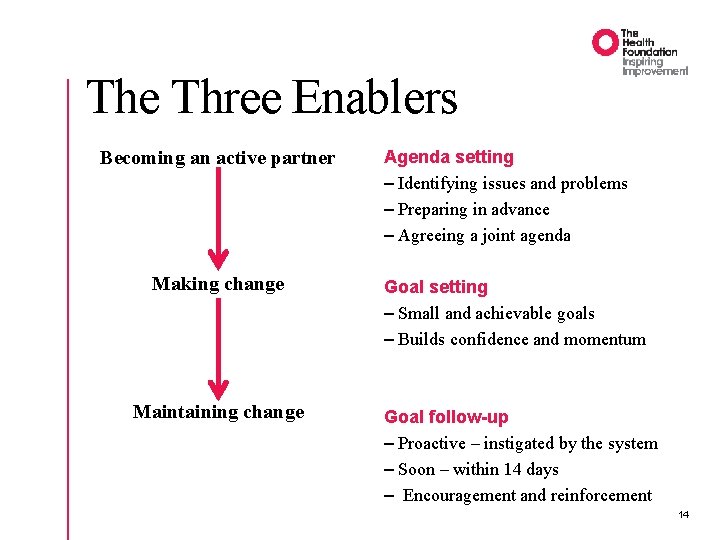
The Three Enablers Becoming an active partner Making change Maintaining change Agenda setting – Identifying issues and problems – Preparing in advance – Agreeing a joint agenda Goal setting – Small and achievable goals – Builds confidence and momentum Goal follow-up – Proactive – instigated by the system – Soon – within 14 days – Encouragement and reinforcement 14
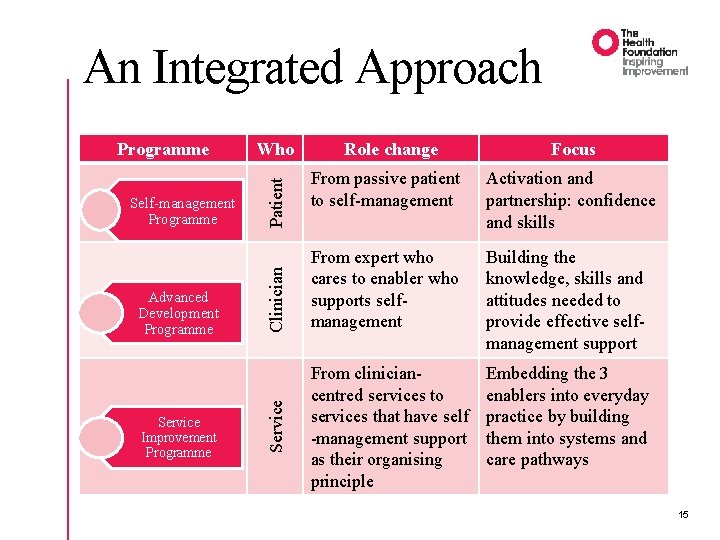
An Integrated Approach Advanced Development Programme Service Improvement Programme Patient Clinician Self-management Programme Who Service Programme Role change Focus From passive patient to self-management Activation and partnership: confidence and skills From expert who cares to enabler who supports selfmanagement Building the knowledge, skills and attitudes needed to provide effective selfmanagement support From cliniciancentred services to services that have self -management support as their organising principle Embedding the 3 enablers into everyday practice by building them into systems and care pathways 15

Self Management Programme outcomes Skills developed. . • • • Setting the agenda Setting goals Problem solving Develop the confidence Understand their condition Develop skills “I used to go to the doctor only when they summoned me, and then say ‘What are you going to do to fix my problem? ’. But now I’m saying like, ‘I’m not sure these particular painkillers are working the way we hoped, can we try something else? What could I do myself? ’ “ Person living with a long-term condition . . . producing statistically significant changes in: • positively engagement with life • constructive attitude/approach towards condition • more positive emotional well being • using self-management skills and techniques 16

Practitioner Development Programme outcomes Practice positively influenced: • • • patients’ confidence to self manage agenda setting own goals collaborative problem solving goal follow up patients’ experience “It’s a change from the traditional approach where say ‘You need to do this”, and the patient says “you’re the boss”, but doesn’t actually do it. We used to wonder why that wasn’t working” Community matron “Now I use agenda setting with my patients and I start by asking ‘what do you want us to do today? ’ Patients appreciate this different approach because you are giving them the power. You work out the goals and the steps together and they are empowered to carry on and work on it on their own. So you may need to see them a bit more at first, but in the long run you need to see them less often. ” Clinician tutor 17
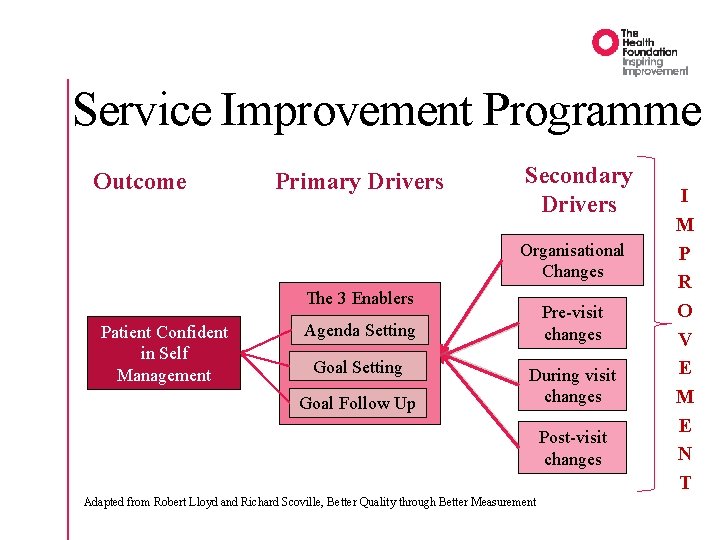
Service Improvement Programme Outcome Primary Drivers Secondary Drivers Organisational Changes The 3 Enablers Patient Confident in Self Management Pre-visit changes Agenda Setting Goal Follow Up During visit changes Post-visit changes Adapted from Robert Lloyd and Richard Scoville, Better Quality through Better Measurement I M P R O V E M E N T
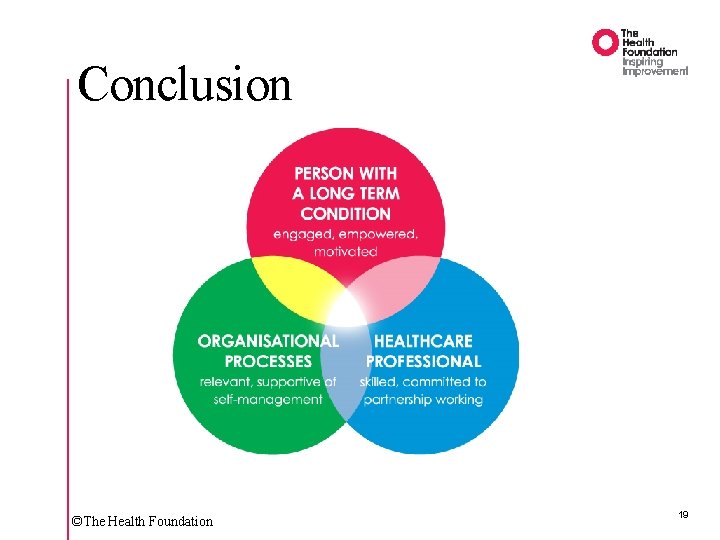
Conclusion ©The Health Foundation 19

Conclusion ‘I’d like to thank you both for giving me back the life I thought I’d lost, its made me realise I was holding myself back’ Person living with a long-term condition ©The Health Foundation 20
- Slides: 20