IMPROVING INHALER TECHNIQUE AND ADHERENCE A COMPLEX PROBLEM

IMPROVING INHALER TECHNIQUE AND ADHERENCE: A COMPLEX PROBLEM IN PRACTICE SINTHIA BOSNIC-ANTICEVICH, PHD Principal Research Fellow Sydney Medical School, University of Sydney Research Leader and Director of Development Woolcock Institute of Medical Research www. woolcock. org. au

Inhaler technique and adherence The when and how of medication management…
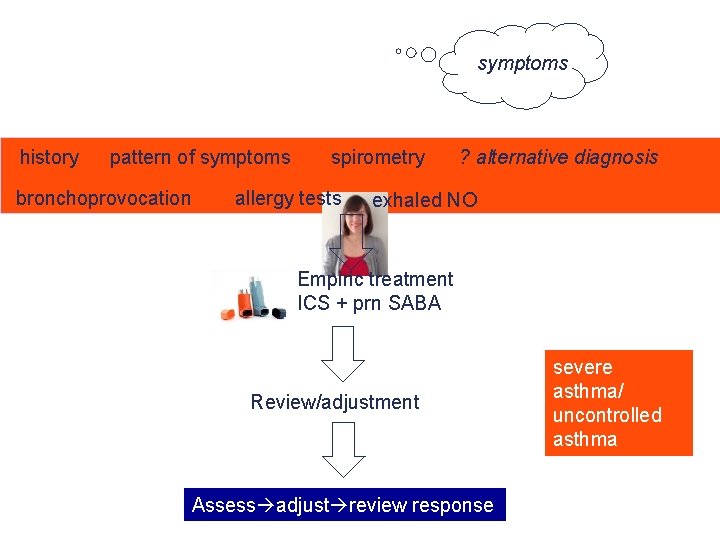
symptoms history pattern of symptoms bronchoprovocation spirometry allergy tests ? alternative diagnosis exhaled NO Empiric treatment ICS + prn SABA Review/adjustment Assess adjust review response severe asthma/ uncontrolled asthma

Implementing HARP (Helping Asthma in Real Patients): Improving asthma control through assessment and inhaler education David Price, et al.
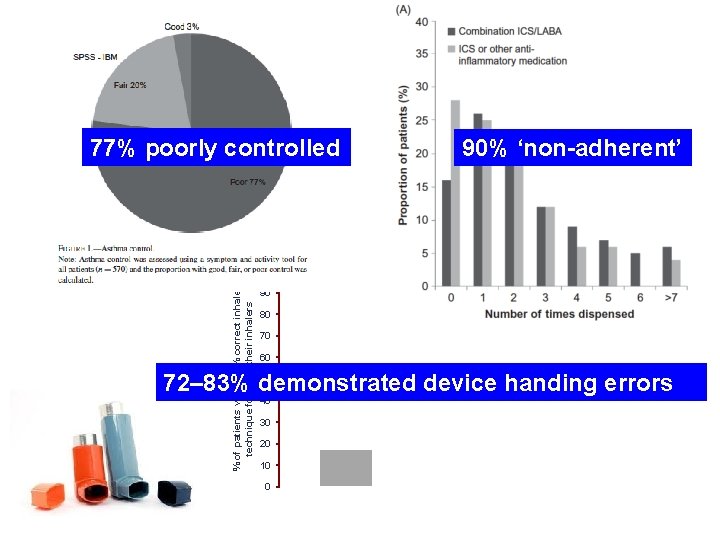
77% poorly controlled 90% ‘non-adherent’ % of patients with 100% correct inhaler technique for all of their inhalers 100 90 80 70 60 50 72– 83% demonstrated device handing errors 40 30 20 10 0
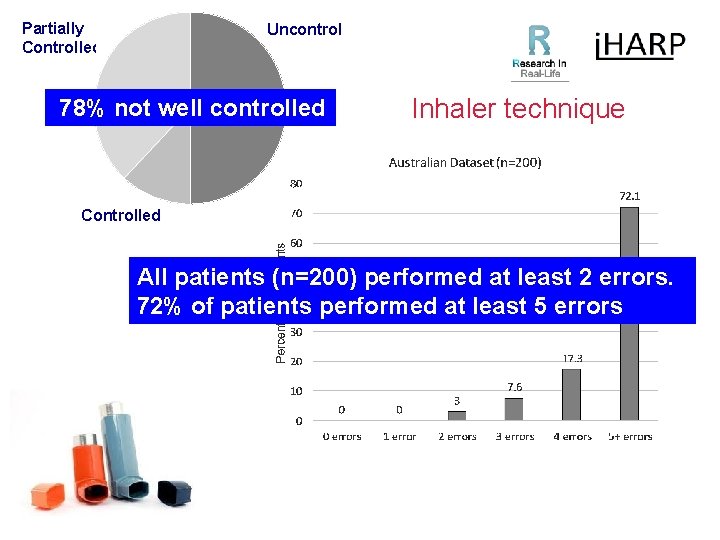
Partially Controlled Uncontrolled 78% not well controlled Inhaler technique Controlled All patients (n=200) performed at least 2 errors. 72% of patients performed at least 5 errors

GINA and medication management principles? n Control-based management n Long term goal ¡ Achieve good symptoms control ¡ Minimize § future risk of exacerbations, fixed airflow limitation and side effects n Evidence based treatment options n Patients goals should be identified a partnership n Communication skills of HCPs patient satisfaction, better health outcomes n Patient characteristics and phenotypes, patient preferences and practical issues (inhaler technique, adherence and cost to the patient) n but…. .

In practice……. n Patients have flare-ups n Severe asthma vs uncontrolled asthma ? ¡ Inhaler technique ¡ Medication adherence ¡ Incorrect diagnosis ¡ Co-morbiditites and complicated conditions ¡ Ongoing exposure to triggers n Knowing what patients should be doing required careful investigation. n Getting them to do it is difficult. ¡ Why?

Drilling down to the ‘practical issues’……. n. Adherence

n Compliance ¡ The extent to which a patient’s behaviour matches the prescriber’s advice n Adherence ¡ The extent to which the patient’s behaviour matches agreed recommendations from the prescriber n Concordance ¡ A complex idea relating to the patient/prescriber relationship and the degree to which the prescription represents shared decision.

Adherence n Up to 70% of adults with asthma do not take their medication as prescribed. n Why? ¡ Do not want to? ¡ Are not able to? ¡ Can not remember to? n It is complex and we need to understand more

There is no ‘typical’ non-adherer

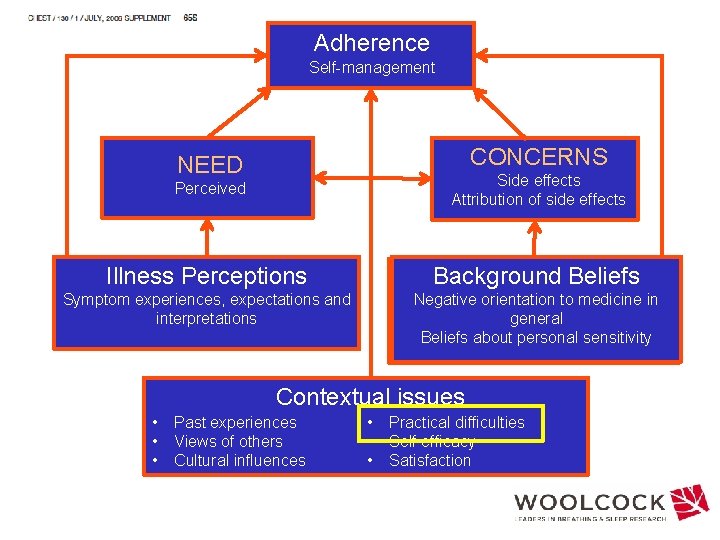
Adherence Self-management CONCERNS NEED Perceived Side effects Attribution of side effects Illness Perceptions Background Beliefs Symptom experiences, expectations and interpretations Negative orientation to medicine in general Beliefs about personal sensitivity Contextual issues • • • Past experiences Views of others Cultural influences • • • Practical difficulties Self efficacy Satisfaction

7 factors associated with poor adherence: • Perceived necessity, • safety concerns, • acceptance of chronicity and medication effectiveness, • advice from family and friends, • motivation and routing, • ease of use, • satisfaction with asthma management.

Interventions to improve adherence n Cochrane review 2008. n Randomised Controlled Trials. ¡ Adherence ¡ Clinical outcomes ¡ Minimum of 6 months n 78 trials. n 93 interventions.

Example of interventions n Increased information n Dosing dispensing charts n Counselling on specific disease, treatment etc n Appointment and prescription refill reminders n Automated telephone , CA patient n Different medication formulations monitoring and counselling n Crisis intervention conducted when n Manual telephone follow-up necessary n Family intervention n Lay health mentoring n Various ways of increasing convenience of care n Augmented pharmacy services n Simplifying dosing n Mailed communications n Involving patients more in care through home monitoring n Group meetings n Reminders e. g. programmed reminders n Special reminder pill sets n Psychological therapy (CBT)

Example of interventions n Increased information n Dosing dispensing charts n Counselling on specific disease, treatment etc n Appointment and prescription refill reminders n Automated telephone , CA patient n Different medication formulations monitoring and counselling n Crisis intervention conducted when n Manual telephone follow-up necessary n Family intervention n Lay health mentoring n Various ways of increasing convenience of care n Augmented pharmacy services n Simplifying dosing n Mailed communications n Involving patients more in care through home monitoring n Group meetings n Reminders e. g. programmed reminders n Special reminder pill sets n Psychological therapy (CBT)

What works? n 1/3 were associated with improved adherence n Reminders n Complex and in combination ¡ Information ¡ Reminders ¡ Self-monitoring ¡ Reinforcement ¡ Counseling ¡ Family therapy ¡ Psychology therapy ¡ Manual telephone follow up ¡ Supportive care

Drilling down to the other ‘practical issue’……. n. Inhaler Technique

The considerations n Up to 90% of people make handling errors. n Across all devices n Some errors are more likely to be related to poor asthma control n Some devices are more intuitive to use n Once you have learnt how to use one, the next one is easier n Should be straightforward…….

Can we improve inhaler technique? n Yes, with the right type of education ✗ ✓
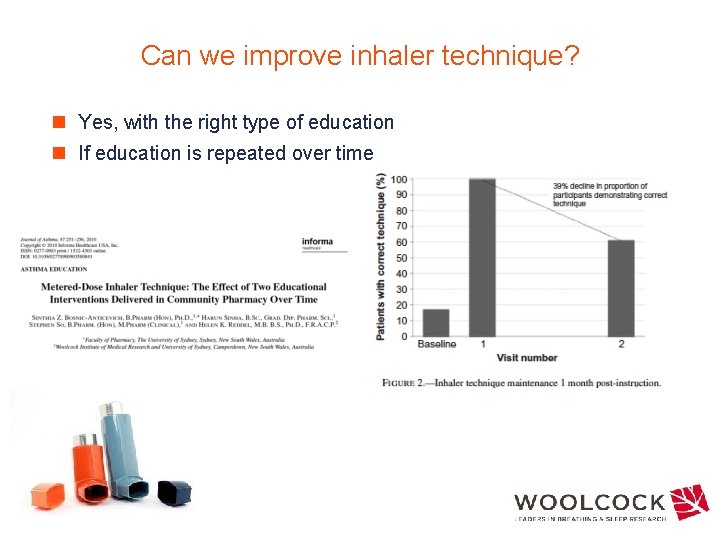
Can we improve inhaler technique? n Yes, with the right type of education n If education is repeated over time
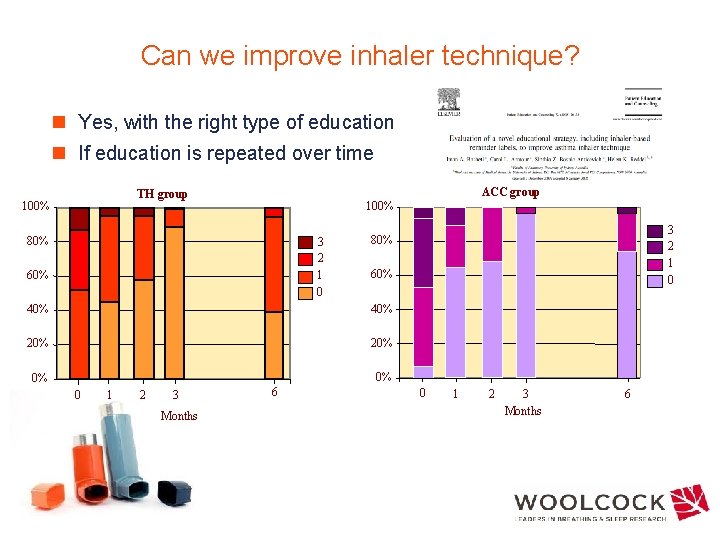
Can we improve inhaler technique? n Yes, with the right type of education n If education is repeated over time ACC group TH group 100% 80% 3 2 1 0 60% 40% 20% 0% 0% 0 1 2 3 Months 6 3 2 1 0 80% 0 1 2 3 Months 6
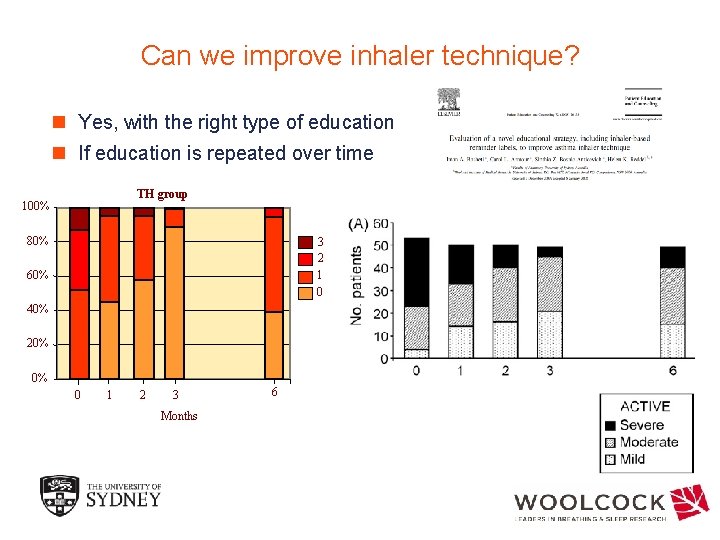
Can we improve inhaler technique? n Yes, with the right type of education n If education is repeated over time TH group 100% 80% 3 2 1 0 60% 40% 20% 0% 0 1 2 3 Months 6
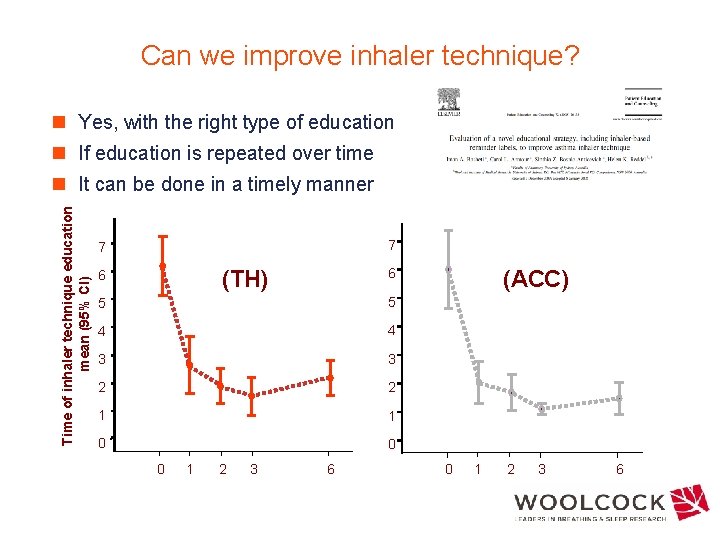
Can we improve inhaler technique? n Yes, with the right type of education n If education is repeated over time Time of inhaler technique education mean (95% CI) n It can be done in a timely manner 7 7 6 (TH) 6 5 5 4 4 3 3 2 2 1 1 0 0 0 1 2 3 6 (ACC) 0 1 2 3 6

But, it is not so simple… n 73% perceive their inhaler technique to be good or excellent n 86% find their inhalers easy to use n 95% have not had their inhaler technique checked in the last 12 months!!

WHY do patients not use their inhalers correctly, even when they are taught how?

The Inhaler Technique Maintenance Framework 1. Perceived threat of asthma 2. Self-management beliefs 3. Self-management self-efficacy

The Inhaler Technique Maintenance Framework 1. Perceived threat of asthma 2. Self-management beliefs 3. Self-management self-efficacy • Symptom experience • Witnessing asthma in others • Comorbidities • Value of health and asthma control • Emotions, e. g. fear versus complacency • Family impact • NECESSITY

The Inhaler Technique Maintenance Framework 1. Perceived threat of asthma 2. Self-management beliefs 3. Self-management self-efficacy • Overarching attitude to medication • Preventer necessity beliefs • perceived threat asthma • perceived benefits preventer • knowledge of preventer role • Preventer concerns • Side effects experienced • CONCERNS

The Inhaler Technique Maintenance Framework 1. Perceived threat of asthma 2. Self-management beliefs 3. Self-management self-efficacy • General life stresses (e. g. financial struggle) • Support from significant others • Practical and emotional • Emotions, e. g. despair and hopelessness versus caution and optimism

The Inhaler Technique Maintenance Framework A new paradigm n Is a complex process n More than just a physical skill n Intrinsically linked with other aspects of asthma management n Fixing the problem will not be so easy…

Should we be looking at them together? n Adherence and inhaler technique ¡ The co-exist ¡ Preliminary research § IT maintenance = adherence + baseline technique + device type (n=233) ¡ We have ways to measure this § INCA (INhaler Compliance Assessment) ¡ The common patient factors § Necessity § Concerns § Motivation § Overall management of asthma

Further considerations n Are some devices favoured/more intuitive, and more likely to be used properly? n Are there special populations that we should be considering? o Intellectual disability o Elderly/cognitive impairment/ physical impairment o disadvantaged n When do the problems start? o Childhood/medication taking autonomy n How can we help each other?

Solutions 1. HCP working together. 2. Understanding the patient perspective. 3. Considering special populations……

HCP working together
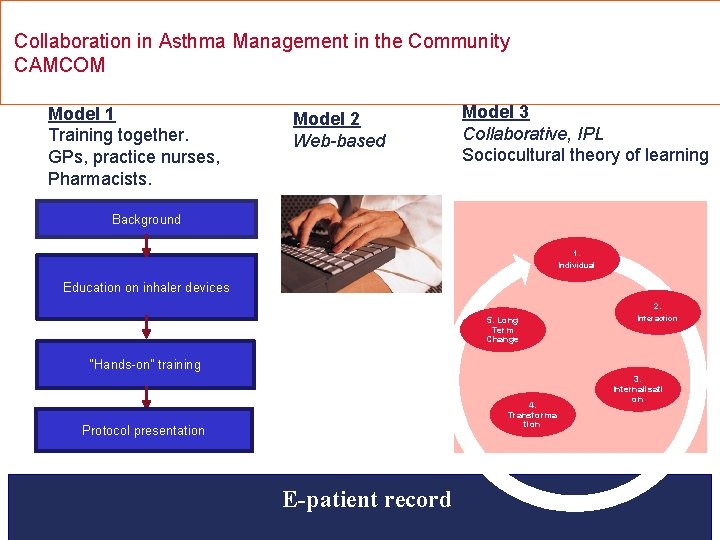
Collaboration in Asthma Management in the Community CAMCOM Model 1 Training together. GPs, practice nurses, Pharmacists. Model 2 Web-based Model 3 Collaborative, IPL Sociocultural theory of learning Background 1. Individual Education on inhaler devices 5. Long Term Change 2. Interaction “Hands-on” training 4. Transforma tion Protocol presentation E-patient record 3. Internalisati on

Understanding the patient’s networks and their influence

Understanding the patient’s networks and their influence

Individuals with Intellectual Disability

Impact and implications n It has to be based on the best science, but it needs to be relevant to the patient. n One size does not fit all. n New Asthma Management Guidelines/reports n Training of undergraduate Medical, Pharmacy and Nursing students n Continuing Professional Education courses n We need to work together n Resources. n Novel inhalers and support material for HCP and patients. n We need to make a discussion about the use of inhalers exciting….

Impact and implications n It has to be based on the bets science, but it needs to be relevant to the patient. n One size does not fit all. n New Asthma Management Guidelines/reports. n Training of undergraduate Medical, Pharmacy and Nursing students. n Continuing Professional Education courses. n Resources. n Novel inhalers and support material for HCP and patients. n We need to make a discussion about the use of inhalers exciting….
- Slides: 43