Improving Care to Geriatric Trauma Patients at Sunnybrook
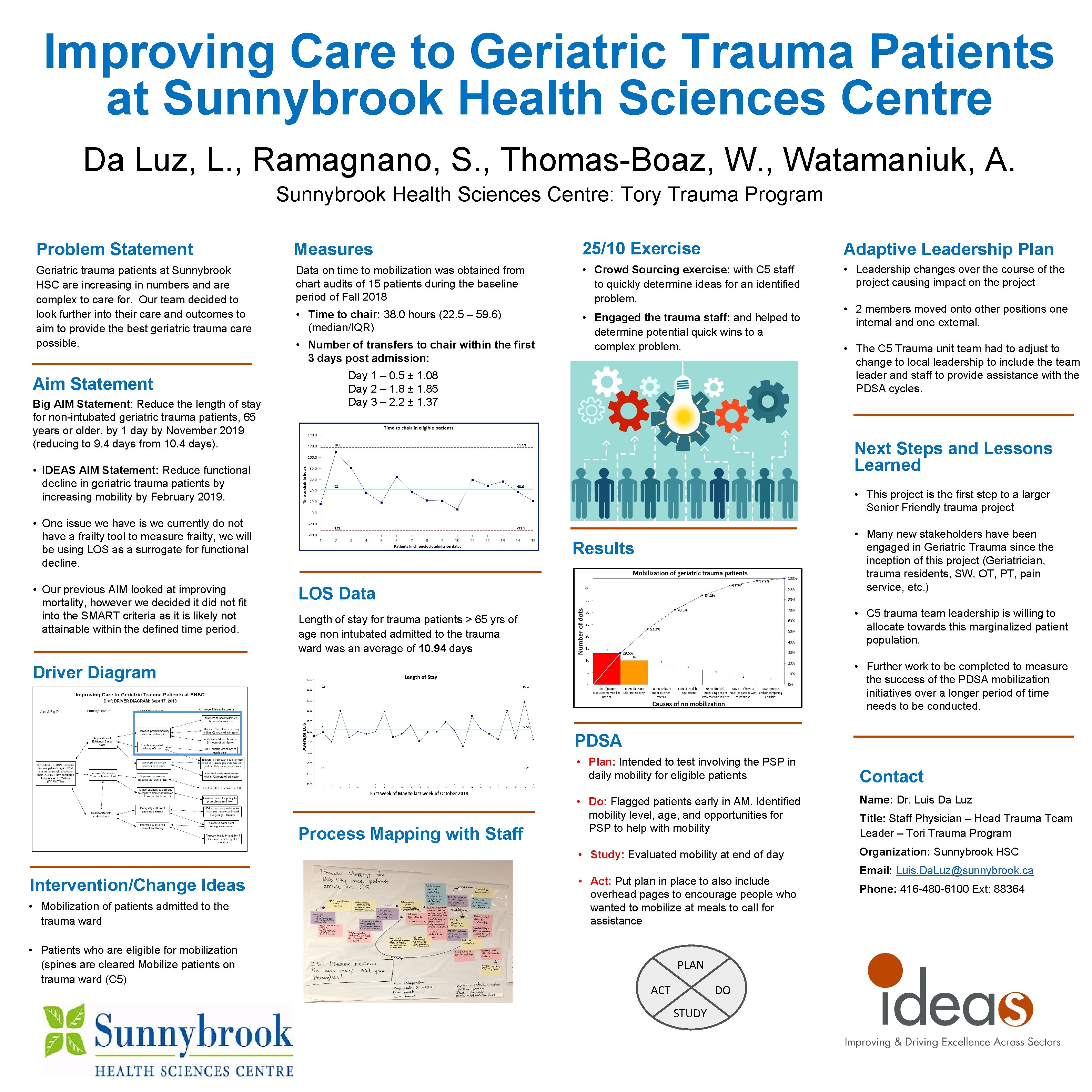
Improving Care to Geriatric Trauma Patients at Sunnybrook Health Sciences Centre Da Luz, L. , Ramagnano, S. , Thomas-Boaz, W. , Watamaniuk, A. Sunnybrook Health Sciences Centre: Tory Trauma Program Problem Statement Measures 25/10 Exercise Adaptive Leadership Plan Geriatric trauma patients at Sunnybrook HSC are increasing in numbers and are complex to care for. Our team decided to look further into their care and outcomes to aim to provide the best geriatric trauma care possible. Data on time to mobilization was obtained from chart audits of 15 patients during the baseline period of Fall 2018 • Crowd Sourcing exercise: with C 5 staff to quickly determine ideas for an identified problem. • Leadership changes over the course of the project causing impact on the project • Time to chair: 38. 0 hours (22. 5 – 59. 6) (median/IQR) • Engaged the trauma staff: and helped to determine potential quick wins to a complex problem. Aim Statement Big AIM Statement: Reduce the length of stay for non-intubated geriatric trauma patients, 65 years or older, by 1 day by November 2019 (reducing to 9. 4 days from 10. 4 days). • Number of transfers to chair within the first 3 days post admission: Day 1 – 0. 5 ± 1. 08 Day 2 – 1. 8 ± 1. 85 Day 3 – 2. 2 ± 1. 37 • The C 5 Trauma unit team had to adjust to change to local leadership to include the team leader and staff to provide assistance with the PDSA cycles. Next Steps and Lessons Learned • IDEAS AIM Statement: Reduce functional decline in geriatric trauma patients by increasing mobility by February 2019. • This project is the first step to a larger Senior Friendly trauma project • One issue we have is we currently do not have a frailty tool to measure frailty, we will be using LOS as a surrogate for functional decline. • Our previous AIM looked at improving mortality, however we decided it did not fit into the SMART criteria as it is likely not attainable within the defined time period. • 2 members moved onto other positions one internal and one external. • Many new stakeholders have been engaged in Geriatric Trauma since the inception of this project (Geriatrician, trauma residents, SW, OT, PT, pain service, etc. ) Results LOS Data • C 5 trauma team leadership is willing to allocate towards this marginalized patient population. Length of stay for trauma patients > 65 yrs of age non intubated admitted to the trauma ward was an average of 10. 94 days • Further work to be completed to measure the success of the PDSA mobilization initiatives over a longer period of time needs to be conducted. Driver Diagram PDSA • Plan: Intended to test involving the PSP in daily mobility for eligible patients Process Mapping with Staff Intervention/Change Ideas • Mobilization of patients admitted to the trauma ward • Patients who are eligible for mobilization (spines are cleared Mobilize patients on trauma ward (C 5) Contact • Do: Flagged patients early in AM. Identified mobility level, age, and opportunities for PSP to help with mobility Name: Dr. Luis Da Luz • Study: Evaluated mobility at end of day Organization: Sunnybrook HSC • Act: Put plan in place to also include overhead pages to encourage people who wanted to mobilize at meals to call for assistance PLAN ACT DO STUDY Title: Staff Physician – Head Trauma Team Leader – Tori Trauma Program Email: Luis. Da. Luz@sunnybrook. ca Phone: 416 -480 -6100 Ext: 88364
- Slides: 1