Improving CABG Surgery Amir Durrani Ben Hoagland Santosh

Improving CABG Surgery Amir Durrani Ben Hoagland Santosh Tumkur Lucas Burton Advisor: Thomas P. Ryan, Ph. D.
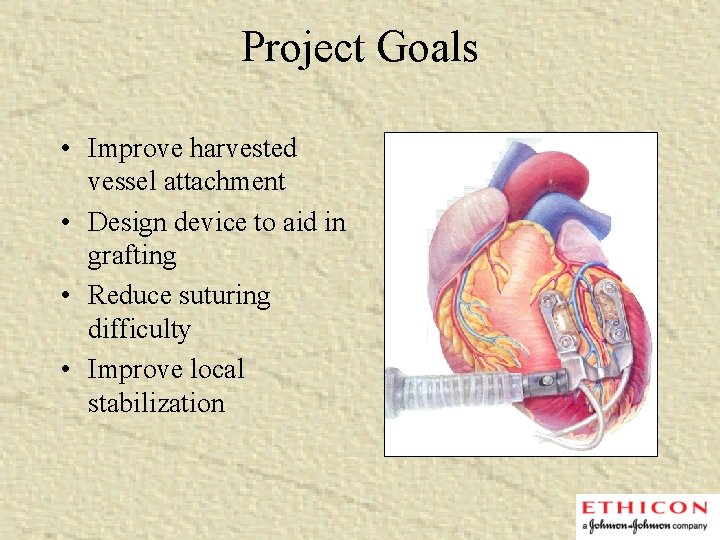
Project Goals • Improve harvested vessel attachment • Design device to aid in grafting • Reduce suturing difficulty • Improve local stabilization

Overview of Off-Pump CABG • Coronary Artery Bypass Graft • Procedure to introduce increased blood flow to occluded coronary arteries • Harvested vessels grafted to coronary arteries
Market Potential • 150, 000 Off-pump CABG surgeries performed worldwide each year • Charge for a CABG procedure ranges from $37, 000 and $72, 000 per case • $26 Billion spent per year on CABG surgeries • Use of beating heart techniques has grown more than 40% each year since 1997

Problems • Stabilization is required to perform CABG on a beating heart • Effective vessel-artery contact is imperative • Complex suturing techniques required • Current stabilizers don’t provide adequate local stabilization of graft site • Heart positioning problems • Heart hemodynamics
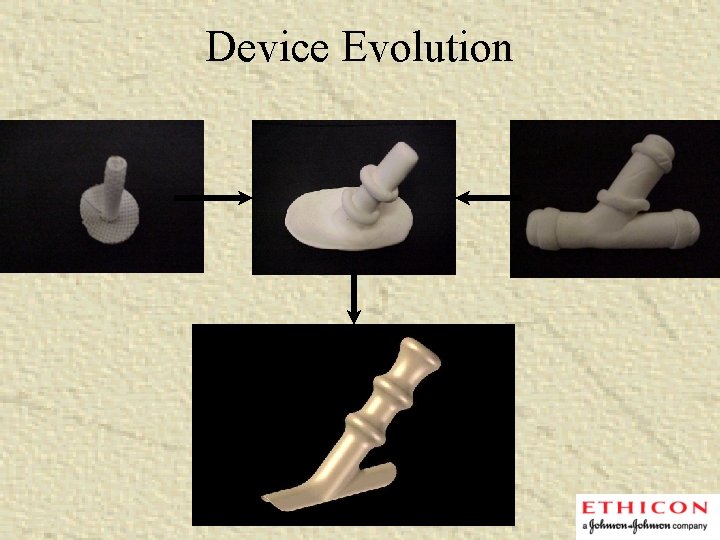
Device Evolution
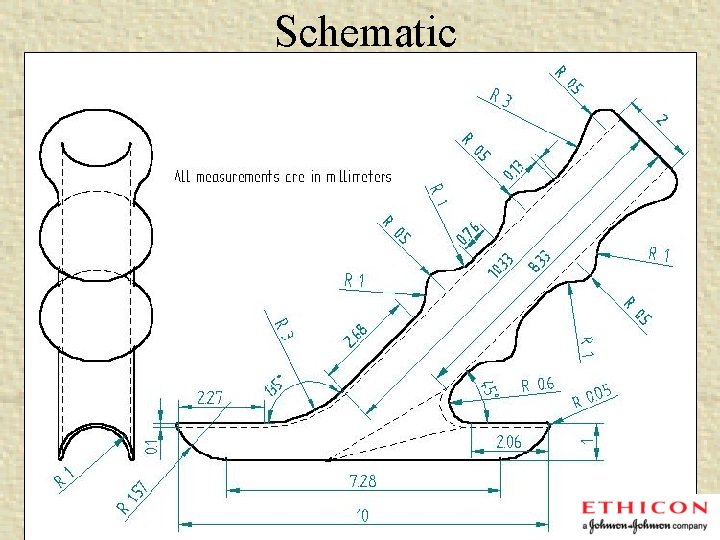
Schematic
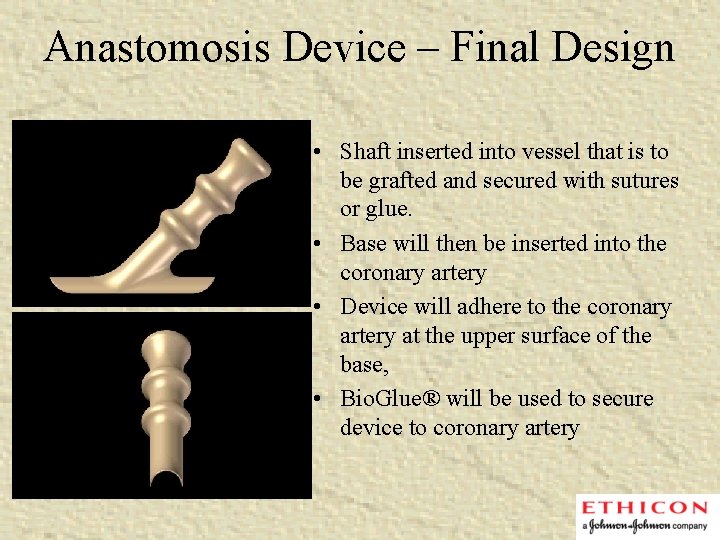
Anastomosis Device – Final Design • Shaft inserted into vessel that is to be grafted and secured with sutures or glue. • Base will then be inserted into the coronary artery • Device will adhere to the coronary artery at the upper surface of the base, • Bio. Glue® will be used to secure device to coronary artery
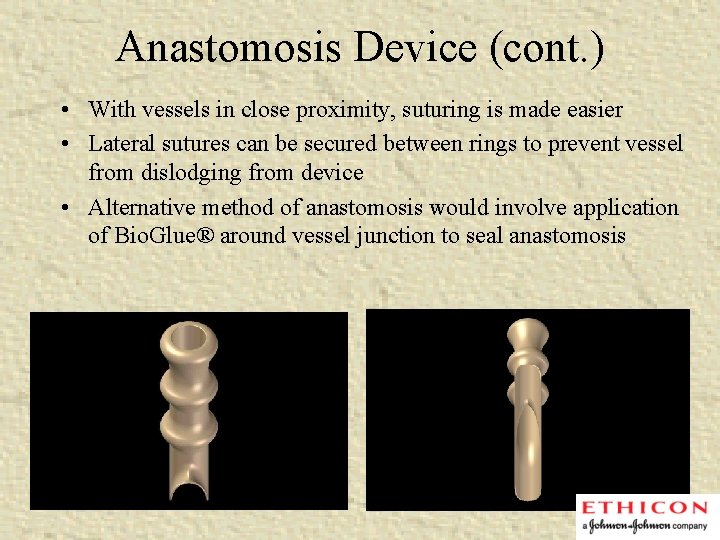
Anastomosis Device (cont. ) • With vessels in close proximity, suturing is made easier • Lateral sutures can be secured between rings to prevent vessel from dislodging from device • Alternative method of anastomosis would involve application of Bio. Glue® around vessel junction to seal anastomosis
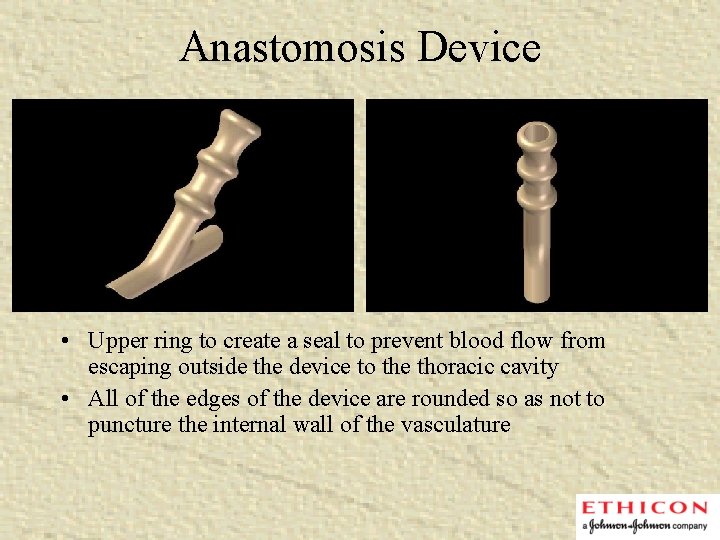
Anastomosis Device • Upper ring to create a seal to prevent blood flow from escaping outside the device to the thoracic cavity • All of the edges of the device are rounded so as not to puncture the internal wall of the vasculature

Proposed Device Materials • Currently, the device will be made entirely of polyetherketone (PEEK) • An advanced polymer that can be plastically deformed • Anastomosis will be augmented by Bio. Glue®, manufactured by Cryo. Life®, Inc. • Bio. Glue® can attach vessels and seal suture holes • Designed for use in anastomosis
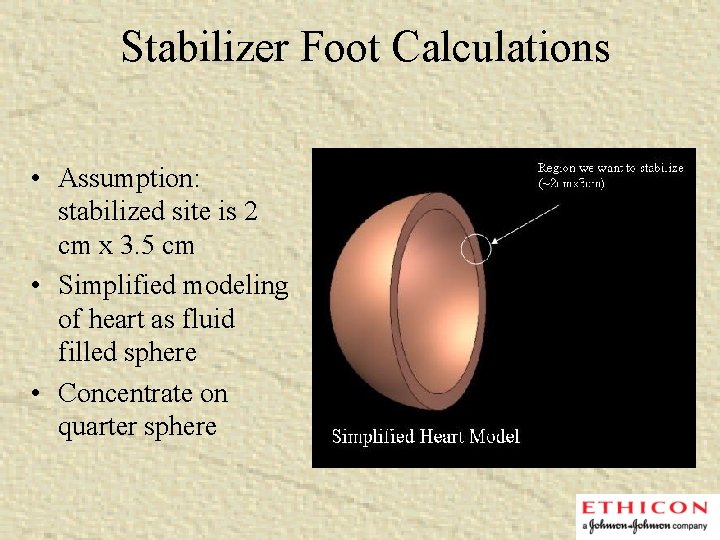
Stabilizer Foot Calculations • Assumption: stabilized site is 2 cm x 3. 5 cm • Simplified modeling of heart as fluid filled sphere • Concentrate on quarter sphere
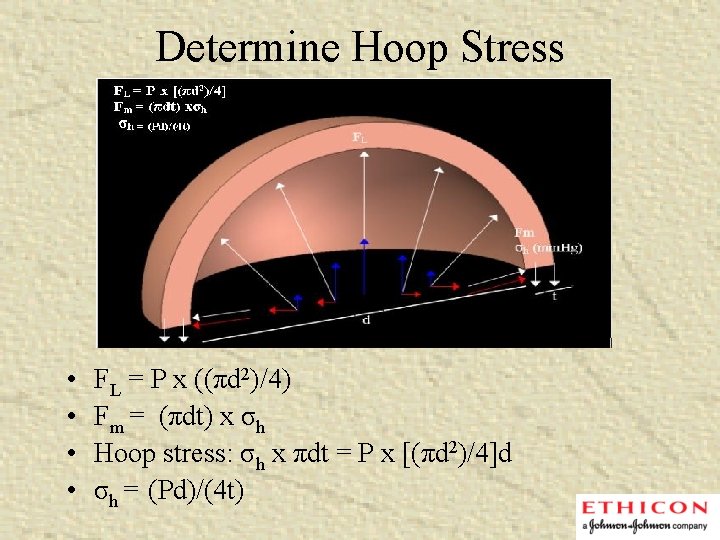
Determine Hoop Stress • • FL = P x ((πd 2)/4) Fm = (πdt) x σh Hoop stress: σh x πdt = P x [(πd 2)/4]d σh = (Pd)/(4 t)
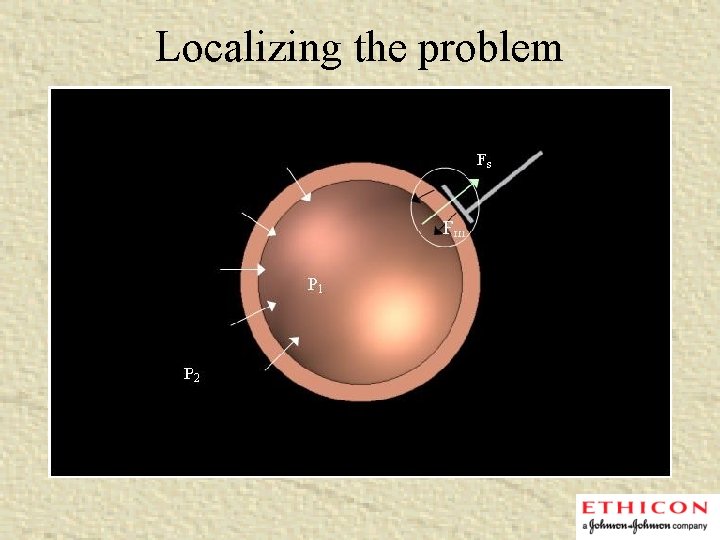
Localizing the problem
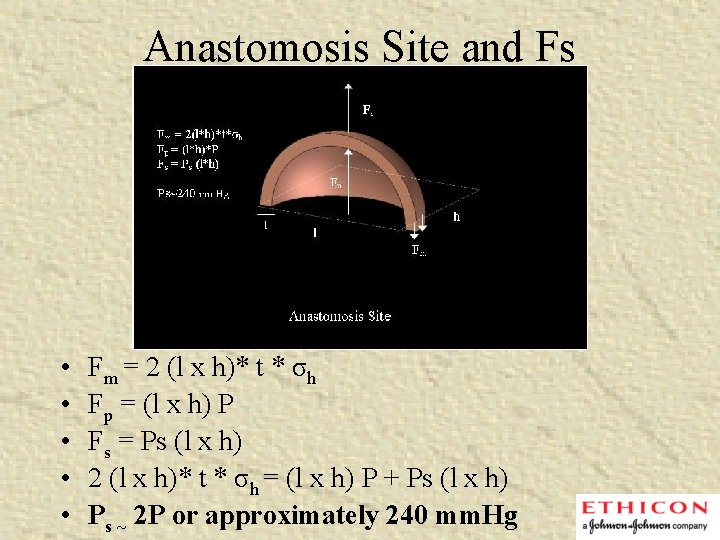
Anastomosis Site and Fs • • • Fm = 2 (l x h)* t * σh Fp = (l x h) P Fs = Ps (l x h) 2 (l x h)* t * σh = (l x h) P + Ps (l x h) Ps ~ 2 P or approximately 240 mm. Hg

Vessel Connector Material Calculations • • • Surface area of the device is 196. 1 mm 2 (1. 961 e-4 m 2) Approximated as a flat plane Maximum experimental pressure ~560 mm. Hg lower limit PEEK tensile strength 52. 5 e 4 mm. Hg/ 560 mm. Hg = 937. 5 Tensile strength well above the 560 mm. Hg pressure constraint

Bio. Glue® • Will replace sutures (or reduce number needed) • Comprised of cross-linked proteinaceous material • High strength • Strong rapid bonding between tissues • Strong rapid bonding between tissue and synthetic materials • Stronger than conventional fibrin adhesives

Bio. Glue® Composition • Cross-linking on a surface • Water soluble proteinaceous material (2753% by weight) • Di- or polyaldehydes (weight ratio: 1 part to every 20 -60 parts of protein • Water insoluble rubbery or leathery proteinaceous solids (free of aldehydes) • Tear strength of at least 75 g/cm^2

Stabilizer Improvement • Modification to suction stabilizer • Provides improved lateral stabilization • Implements a turnbuckle • Spreads tissue up to two centimeters beyond closed position • Improved vacuum system which implements four lines in parallel.

Stabilizer Foot Images

Progress Made • Completed Solid. Edge® design of our prototype • Finished Design. Safe™ Analysis • Settled on polyetherketone (PEEK) as our polymer of choice for our vessel connector device • Contacted Brian Cox of the Vanderbilt Technology Transfer Office concerning licensing and patents

Current Status • In the beginning process of obtaining a patent with help from the Tech. Transfer Office • In the process of having our vessel connector prototype built by the University of Pittsburgh • Stabilizer is currently being built by outside machine shop source • Final Report

Future Plans • Begin design of poster for final presentation • Obtain stabilizer foot from machine shop and prototype from University of Pittsburgh • Continue consultation with surgeons and engineers for feedback • Acquire Bio. Glue® sample from Cryolife®, Inc. • Finish final report

Recommendations • Perform extensive stress and material testing of anastomosis device and foot • Investigate other possible materials for anastomosis device • Explore other possible vessel connector designs or improvements • Obtain further feedback from doctors • Acquire test data with foot and anastomosis device
- Slides: 24