IMPLEMENTING A SCIENCEBASED APPROACH TO FATIGUE RISK MANAGEMENT

IMPLEMENTING A SCIENCEBASED APPROACH TO FATIGUE RISK MANAGEMENT IN NURSING Prof Philippa Gander Ph. D, FRSNZ Dr Karyn O’Keeffe Ph. D

Outline Background to the project Principles � Project Team � Fatigue risk management Legal requirements � Causes and consequences of fatigue � Managing fatigue risk � Project Aims � Processes, tools, and timeline � Discussion

Background to the project Fatigue is inevitable when 24/7 cover is required � Optimum functioning requires unrestricted sleep at night Science-based fatigue risk management � � Pooling scientific/workplace/organisational expertise to come up with better solutions Requires a collaborative approach a whole of life issue required by the Health and Safety at Work Act The project - working together to implement a new approach � Initial focus hospital based, high fatigue practice areas � child health including neonatology, emergency and trauma, in-patient mental health, intensive care/cardiac care, medical, surgical Principles and processes that are generalizable to other practice areas
Project Team Investigators � � Massey University: Prof Philippa Gander, Dr Karyn O’Keeffe (SWRC), Prof Annette Huntington, Massey School of Nursing, Dr Léonie Walker, School of Public Health New Zealand Nurses Organisation: Dr Jinny Willis Advisory Group � � � � Andrea Mc. Cance, Director of Nursing and Midwifery, Capital & Coast DHB Belinda Bennett, Operations Manager, Surgery, Women & Children, Capital & Coast DHB Toni Dal Din, Director of Nursing, Mental Health & Intellectual Disability Service, 3 DHB Pamela Doole, Manager, Strategic Policy, Nursing Council of New Zealand Michele Halford, Executive Leader Nursing, Wairarapa DHB Denise Kivell, Director of Nursing, Counties Manukau DHB Lynley Mulrine, Industrial Services Lead Organiser, Southern Region, NZNO Shannon Lake, Te Rūnanga Auckland Representative; Registered Nurse, Counties Manukau DHB Monina Gesmundo, President of the Filipino Nurses Association of New Zealand Lisa Skeet, Director, Safe Staffing, Healthy Workplaces Unit, DHB Shared Services Ted Harper, Manager, Employee Health and Safety Service, Bay of Plenty DHB Trish Walton, After Hours Duty Nurse Manager, Southern DHB Sally Houliston, Nurse Consultant, Workforce Development, Hawkes Bay DHB Professor Jeroen Douwes , Director, Centre for Public Health Research, Massey University

Health and Safety at Work Act (2015) Mental and physical fatigue can cause hazards � Hazard - ‘a person’s behaviour where that behaviour has the potential to cause death, injury, or illness to a person’ Worksafe guidance, shift work is a cause of fatigue Workplace health and safety is a shared responsibility of officers, PCBUs and workers � You cannot transfer your duty owed to another person or organisation Shift work causes fatigue contributes to hazards

What are we talking about? Fatigue is A physiological state of reduced mental or physical performance capability resulting from sleep loss or extended wakefulness, circadian phase, or workload (mental and/or physical activity) that can impair a person’s alertness and ability to work safely and efficiently International Civil Aviation Organisation (ICAO) 2011 Shift work is any work pattern that requires you to be awake when you would normally be asleep if you were free to choose your own schedule Because of the way the human brain and body are designed to function

Why sleep? Brain needs to go ‘off-line’ for essential recovery and maintenance Ignores (mostly) inputs from the senses (light, sound, smell) � complex series of processes � � dreaming (REM) and non-dreaming (non-REM) memory consolidation, learning emotional regulation repair of tissue wear-and-tear Professor William Dement growth recharge immune system regulate appetite, metabolism … wake up as an updated version of yourself! Why wake?
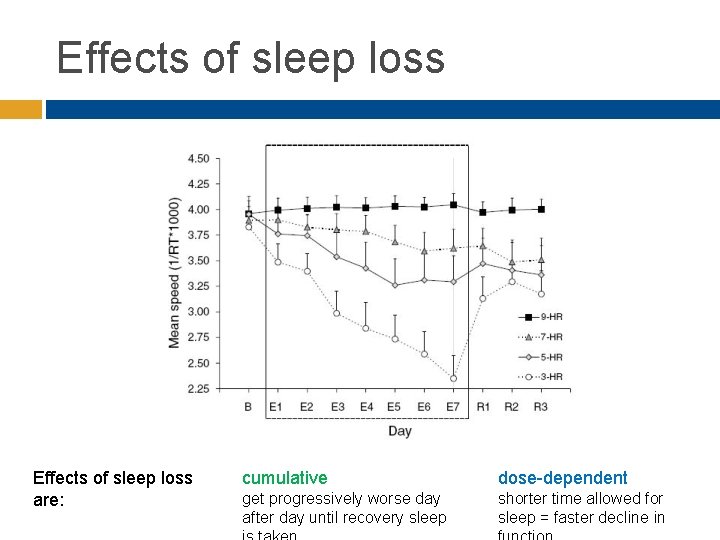
Effects of sleep loss are: cumulative dose-dependent get progressively worse day after day until recovery sleep shorter time allowed for sleep = faster decline in

Not enough sleep Restricted sleep leads to: � � feeling sleepier, irritability, degraded alertness, slower reaction times, poorer coordination, slower thinking, loss of situation awareness, less creative problem-solving uncontrolled sleep Recovering from restricted sleep � � recovery is not hour-for-hour: sleep usually gets back to normal after 2 nights of unrestricted sleep � sleepiness → microsleeps → established sleep not 48 hours off recovery of waking function can take more than 2 full nights of sleep Pressure for sleep builds up across time awake
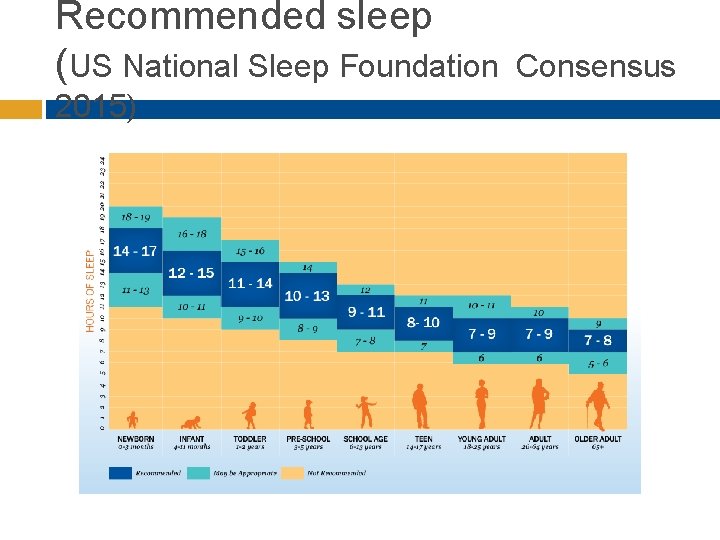
Recommended sleep (US National Sleep Foundation 2015) Consensus

Why do we sleep at night? Circadian body clock Pacemaker in the brain that drives daily cycles (circadian rhythms) in � How you function � How you feel body functions – hormones, heart rate, digestion … ability to do physical and mental work mood, sleepiness, fatigue … Tracks light intensity even through closed eye lids � � designed to keep us in step with the day/night cycle connected to sleep-promoting centres and wake-promoting centres in the brain A feature of life on earth
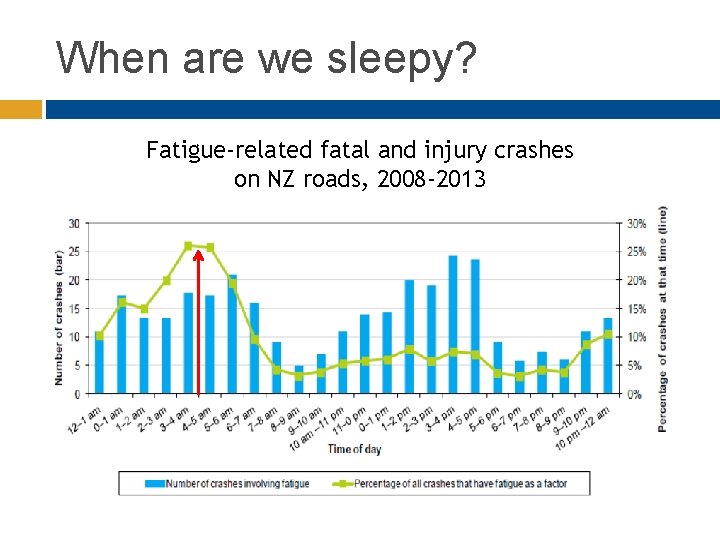
When are we sleepy? Fatigue-related fatal and injury crashes on NZ roads, 2008 -2013
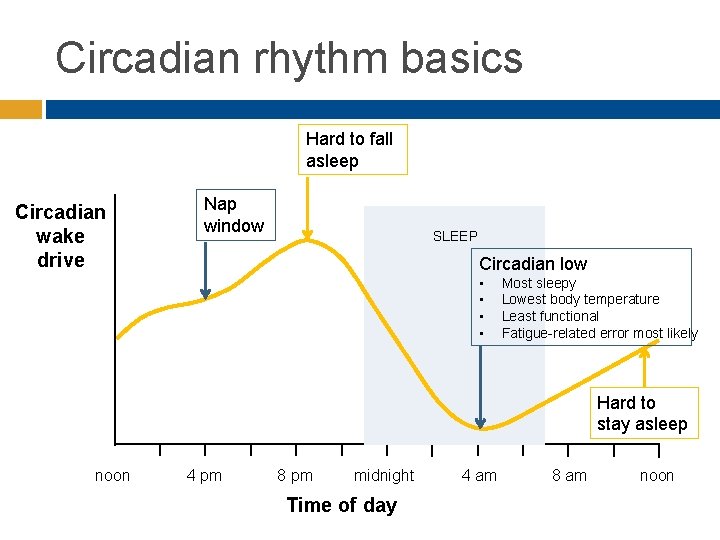
Circadian rhythm basics Hard to fall asleep Circadian wake drive Nap window SLEEP Circadian low • • Most sleepy Lowest body temperature Least functional Fatigue-related error most likely Hard to stay asleep noon 4 pm 8 pm midnight Time of day 4 am 8 am noon

Social time versus biological time Light sensitive circadian body clock doesn’t adapt to shift work Trying to work when least functional Eating at physiologically inappropriate times Trying to sleep when primed for wake � other time demands, noise, light, heat. . .

Safety of Patients and Nurses Compared to nurses who work day or evening shifts, nurses who work rotating shifts are twice as likely to � � Report clinical errors Have a motor vehicle accident Compared to nurses working shorter shifts, nurses working extended shifts (>8 hours) are � 2 -3 times more likely to � � Make clinical errors Have poorer patient outcomes, including increased patient mortality Feel drowsy while driving Have a greater likelihood of injuring themselves and others More likely to report poor quality care and poor patient safety Gold et al. , 1992; Scott et al. , 2006, 2007; Rogers et al. , 2004; Trinkoff et al. , 2007, 2011; Olds et al. ,

Nurses Health Study (90% follow-up at 22 years) Association between working rotating night shifts (defined as ≥ 3 nights/month) and: Increased all-cause and cardiovascular disease mortality (after ≥ 5 years exposure) � Increased lung cancer mortality (after ≥ 15 years exposure) � Increased risk of ischemic stroke for every 5 years of additional exposure (after ≥ 15 years exposure) � Monotonic increase risk of type 2 diabetes with increasing exposure � Partly mediated through body weight Gu et al. , 2015; Brown et al. , 2009; Pan et al. , 2011

Fatigue versus safety risk Risk depends on � What a fatigued person is doing � Other hazards present � Safety defences present Nurse travelling home after night work Driving at 100 km/hour Rural road vs Auckland motorway Airline pilot in 4 -pilot crew In-flight sleep in crew bunk Mid-cruise versus landing

Managing fatigue risk Traditional approach – limits on: � � � Maximum work hours Minimum breaks within and between shifts Frequency of 24 -h breaks Regulatory or by industrial contract Most don’t address circadian variation Don’t address risk Alternative approach – data-driven fatigue risk management systems based on: � � � New science and workplace expertise Shared responsibility Effective safety reporting culture Ongoing monitoring and management of actual risk Multiple strategies to reduce risk
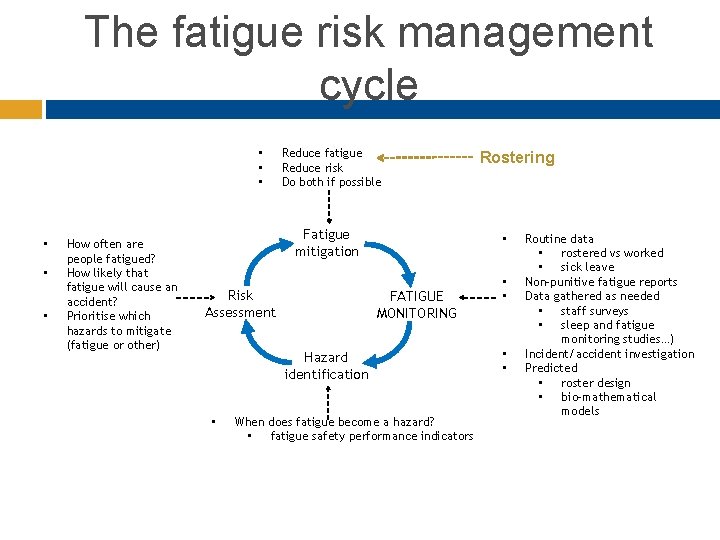
The fatigue risk management cycle • • • How often are people fatigued? How likely that fatigue will cause an accident? Prioritise which hazards to mitigate (fatigue or other) Reduce fatigue Reduce risk Do both if possible Fatigue mitigation Risk Assessment • FATIGUE MONITORING Hazard identification • Rostering When does fatigue become a hazard? • fatigue safety performance indicators • • Routine data • rostered vs worked • sick leave Non-punitive fatigue reports Data gathered as needed • staff surveys • sleep and fatigue monitoring studies…) Incident/accident investigation Predicted • roster design • bio-mathematical models

Non-punitive fatigue reporting Need to define intentional violation versus unintentional error Hazard identification; what? where? why? possible mitigations Identify hazards before they grow into accidents

Rostering The perfect roster is permanent day work with unrestricted sleep at night Better roster design � adequate sleep opportunities � limits on continuous work (time awake, time-on-task fatigue) � shift length breaks during shifts (workplace naps? ) predictable rosters, plan for covering on-call or call back � how fast is sleep debt building up? how long since 2 full nights of sleep in a row? knowing ahead of time helps people to arrive at work better-rested fair distribution of weekends off work/life balance matters

Questions to ask in your work environment(s) what are the main causes of workplace fatigue? what are safety risks posed by fatigued people? what mitigations are available to reduce fatigue? what mitigations are available to reduce the safety risks associated with fatigued people? what data do you have available for routine tracking of fatigue hazards? what other data might be useful? do you analyse for the role of fatigue in safety events? If yes, how? who is responsible for: � � � fatigue hazard identification? fatigue risk assessment? choosing and implementing fatigue mitigations? who checks that you are meeting your obligations under the HSE Act?

Implementing a Science-Based Approach to Fatigue Risk Management in Nursing Aims Processes, tools, and timeline

Project aims/steps Build fatigue awareness and knowledge across the sector � project promotional activities � comprehensive package of accessible fatigue management training materials Nationwide on-line survey of RNs and ENs work patterns in 6 practice areas � � child health including neonatology, emergency and trauma, in-patient mental health, intensive care/cardiac care, medical, surgical Outcomes � Data collection closed April 2017 Currently working on data analysis Code of Practice for shift work and fatigue management in hospital-based nursing � � � an overview of what is being worked fatigue risk assessment matrices for evaluating rosters in each practice area fatigue risk management training materials Status Website launch October 6 Social media, traditional media, stakeholder meetings … collaboration with key stakeholders broad sector consultation Parliamentary launch Identifying, or advocating for an agency with representation from all stakeholders, to take ongoing responsibility for establishing a cycle of continuous improvement in fatigue risk management.
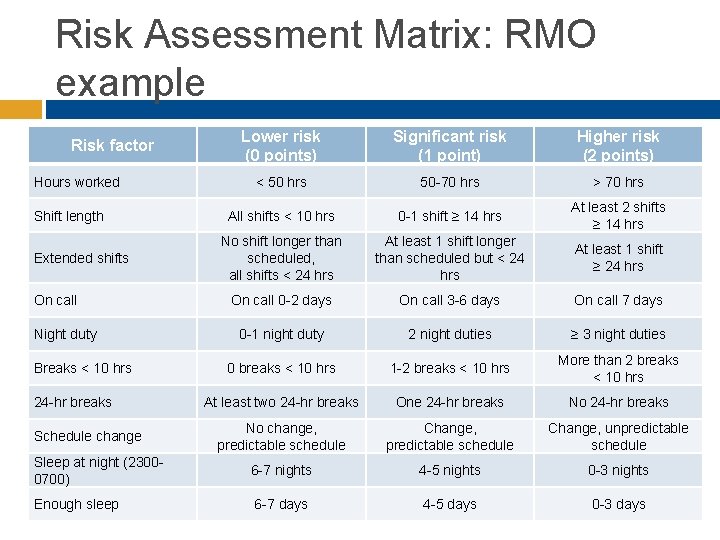
Risk Assessment Matrix: RMO example Lower risk (0 points) Significant risk (1 point) Higher risk (2 points) < 50 hrs 50 -70 hrs > 70 hrs All shifts < 10 hrs 0 -1 shift ≥ 14 hrs At least 2 shifts ≥ 14 hrs No shift longer than scheduled, all shifts < 24 hrs At least 1 shift longer than scheduled but < 24 hrs At least 1 shift ≥ 24 hrs On call 0 -2 days On call 3 -6 days On call 7 days 0 -1 night duty 2 night duties ≥ 3 night duties 0 breaks < 10 hrs 1 -2 breaks < 10 hrs More than 2 breaks < 10 hrs At least two 24 -hr breaks One 24 -hr breaks No change, predictable schedule Change, unpredictable schedule Sleep at night (23000700) 6 -7 nights 4 -5 nights 0 -3 nights Enough sleep 6 -7 days 4 -5 days 0 -3 days Risk factor Hours worked Shift length Extended shifts On call Night duty Breaks < 10 hrs 24 -hr breaks Schedule change

What makes a good Code of Practice? industry ownership having appropriate knowledge and expertise in the development of the Code providing practical, flexible, cost-effective solutions sector consultation accessibility of the Code (paper and on-line) dissemination e. g. , through sector workshops monitoring of implementation and effectiveness of the Code regular updating to reflect the current body of knowledge Pearce N, Dryson E, Gander P, Langley J, Wagstaffe M. Review of the key characteristics that determine the efficacy of OSH instruments Report to the Minister of Labour. Wellington, NZ: NOHSAC, 2008.
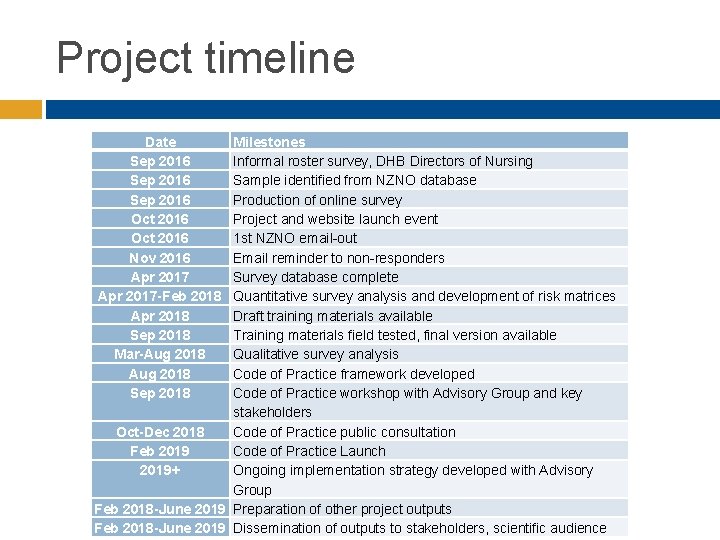
Project timeline Date Sep 2016 Oct 2016 Nov 2016 Apr 2017 -Feb 2018 Apr 2018 Sep 2018 Mar-Aug 2018 Sep 2018 Milestones Informal roster survey, DHB Directors of Nursing Sample identified from NZNO database Production of online survey Project and website launch event 1 st NZNO email-out Email reminder to non-responders Survey database complete Quantitative survey analysis and development of risk matrices Draft training materials available Training materials field tested, final version available Qualitative survey analysis Code of Practice framework developed Code of Practice workshop with Advisory Group and key stakeholders Oct-Dec 2018 Code of Practice public consultation Feb 2019 Code of Practice Launch 2019+ Ongoing implementation strategy developed with Advisory Group Feb 2018 -June 2019 Preparation of other project outputs Feb 2018 -June 2019 Dissemination of outputs to stakeholders, scientific audience

Discussion For a copy of the presentation, please email k. m. okeeffe@massey. ac. nz

Reducing fatigue Fatigue management education � � Who? - nurses, schedulers, nurse managers, OSH staff, DON, CEO What? causes of fatigue and safety issues in your workplace personal strategies to use at home (how to get better sleep) personal strategies to use at work (strategic use of caffeine, napping, …) company policies related to fatigue management (for calling in too fatigued, how to report fatigue hazards …) Reduce workload Improve skill level Healthy workforce

Reducing fatigue-related risk Policies/protocols/procedures for calling in fatigued � workplace napping (when, where, how) � managing staff with chronic sleep problems � analysis of data for monitoring fatigue � � linking fatigue management to other hazard management � acting on data, feedback to staff and management risk assessment cost of mitigations who decides about the $$? getting home safely? – risk to self and others on the road
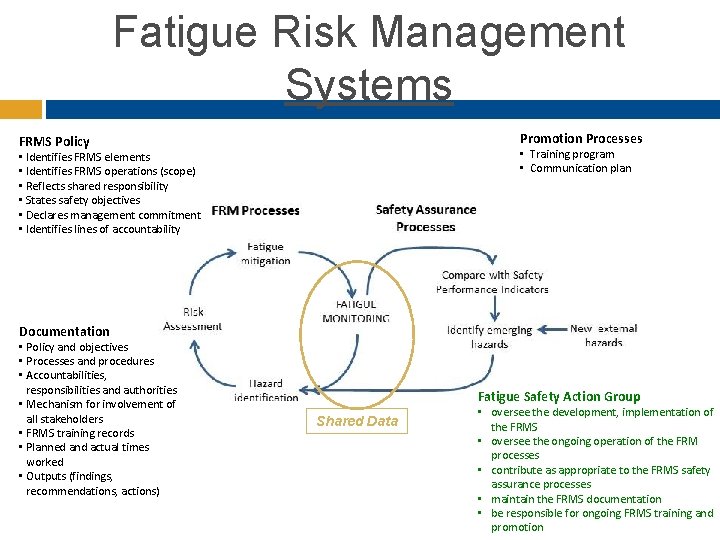
Fatigue Risk Management Systems Promotion Processes FRMS Policy • Training program • Communication plan • Identifies FRMS elements • Identifies FRMS operations (scope) • Reflects shared responsibility • States safety objectives • Declares management commitment • Identifies lines of accountability Documentation • Policy and objectives • Processes and procedures • Accountabilities, responsibilities and authorities • Mechanism for involvement of all stakeholders • FRMS training records • Planned and actual times worked • Outputs (findings, recommendations, actions) Fatigue Safety Action Group Shared Data • oversee the development, implementation of the FRMS • oversee the ongoing operation of the FRM processes • contribute as appropriate to the FRMS safety assurance processes • maintain the FRMS documentation • be responsible for ongoing FRMS training and promotion
- Slides: 31