Immunosuppressant withdrawal after renal transplant failure Allograft failure

















- Slides: 19

Immunosuppressant withdrawal after renal transplant failure 조윤주


• Allograft failure – 13 % of renal transplant pts in 2006 had undergone a previous transplant. – 100, 000 pts beginning dialysis in 2002, 4% had a failed renal allograft • Reinstitution of dialysis after transplant failure? : Optimal method of tapering?

Immunosupressive treatmet in KT • Calcineurin inhibitor (cyclosporine / tacrolimus) • Anti-metabolite (azathioprine / mycophenolate mofetil or Mycophenolate sodium) • prednisone 2009. KDIGO

Side effects Calcineurin inhibitor Antimetabolite Nephrotoxicity Hepatotoxicity Tremor DM Infection Hirsutism* Gingiva hyperplasia* Gastrointestinal toxicity BM supression Hepatotoxicity Malignancy (Skin, lymphoma) Infection *Cyclosporin

Side effects Steroids • • • Skin thinning , purpura, acne, alopecia, hypertrichosis Cataract, glaucoma IHD, Heart failure Hepatic VLDL synthesis↑ DM, Iatrogenic cushing Osteoporosis Gastritis, ulcer Fluid retention Menstrual irregularities Emotional lability, Psychosis Infection

Reasons for withdrawal • Risk of infection • Complications of corticosteroid therapy • Risk of malignancy : – Kaposi’s sarcoma , NHL, lip ca & melanoma

Complications of withdrawal • Secondary adrenal insufficiency • Loss of residual renal function • Rejection requiring transplant nephrectomy • Potential adverse immunologic effects on pts pursuing another transplantation.

2︐ adrenal insufficiency • ACTH stimulation test - "gold standard“ • Time required to recover HPA : dosage/duration (few weeks – several months) • Withdrawal in well-functioning renal transplants: Randomized trial , withdrawal over 4 month 1 year after , 1 of the 49 developed adrenal insufficiency Gradual withdrawal not associated with adrenal insufficiency. Lancet. 1996; 348(9028): 643. .

Implications of residual renal function • Renal function deteriorates rapidly after withdrawal of immunsupression • Longer tapering may permit the maintenance of some renal function while on dialysis

Rejection • Graft tenderness, fever, hematuria, localized edema, infection • Wt loss, anemia, GI symptom, Resistance to EPO stimulating agents Transplant Nephrectomy

Transplant nephrectomy • Indications : Rejection after withdrawal Hx of early graft failure • Morbidity & mortality has improved markedly • Early allograft failure: Immediate withdrawal of supression + preemptive nephrectomy • Late graft failure: Indications not defined May be considered in pts with signs of a chronic inflammatory state

• United States Renal Data System(1994 -2004) • 10, 951 dialysis pts with failed allograft, 31. 5 %underwent nephrectomy

However, • include unclear reasons for nephrectomy • not defining the comorbid conditions that prevented operation • Pts who underwent nephrectomy may have been healthier? Whether survival is truly improved with nephrectomy requires additional evidence

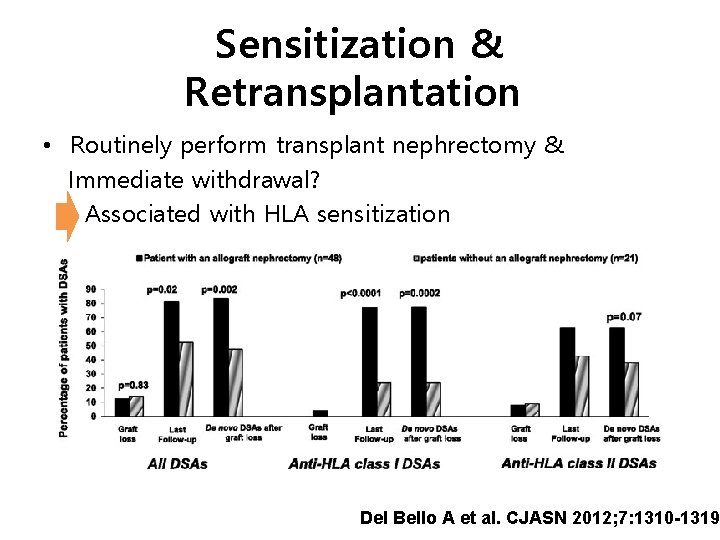
Sensitization & Retransplantation • Routinely perform transplant nephrectomy & Immediate withdrawal? Associated with HLA sensitization Del Bello A et al. CJASN 2012; 7: 1310 -1319

Effect of nephrectomy on retransplantation • Unresolved issue : Benefit for retransplantation from leaving the failed graft? • Animal models of retransplantation : To maintain tolerance & accept 2 nd graft, the presence of donor antigen is beneficial. • Rat heart transplantation model, : Graftectomy significantly reduced survival of 2 nd allograft, suggesting a tolerizing effect of residual antigen • This hypothesis has not been tested in humans

HOW? • Goal: stop the drugs without symptomatic rejection & drug withdrawal side effects • No controlled, prospective studies to determine method for tapering/withdrawing • “center-specific protocoals”

• Early allograft failure: Immediate withdrawal of immunosuppression + preemptive nephrectomy • Later allograft failure: Withdraw immunosuppression (no longer than 6 mo from the time of allograft failure) Standard protocol : Immediately withdraw cyclosporine / tacrolimus & azathioprine/mycophenolate ->subsequently taper prednisone by 1 mg/month until the drug is discontinued

• residual renal function despite allograft failure? Withdraw the anti-metabolite immediately, Reduce the CNI dose to once daily in the morning Reduce the prednisone dose to 5 mg per day CNI & steroid are tapered slowly over 3 to 6 mo. • Allograft rejection withdrawal? Prednisone 0. 3 to 1. 0 mg/kg per day for 5 – 7 days Patients are subsequently referred for surgery.